Fournier’s Gangrene under Sodium–Glucose Cotransporter-2 Inhibitors Therapy in Gynecological Patients
Abstract
1. Introduction
2. Case Presentation
3. Discussion
4. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Bersoff-Matcha, S.J.; Chamberlain, C.; Cao, C.; Kortepeter, C.; Chong, W.H. Fournier gangrene associated with sodium-glucose cotransporter-2 inhibitors: A review of spontaneous postmarketing cases. Ann. Intern. Med. 2019, 170, 764–769. [Google Scholar] [CrossRef]
- Ellegård, L.; Prytz, M. Fournier’s gangrene under SGLT-2 inhibitor therapy: A literature review and case report. Int. J. Surg. Case Rep. 2020, 77, 692–694. [Google Scholar] [CrossRef]
- Sorensen, M.D.; Krieger, J.N.; Rivara, F.P.; Broghammer, J.A.; Klein, M.B.; Mack, C.D.; Wessells, H. Fournier’s gangrene: Population based epidemiology and outcomes. J. Urol. 2009, 181, 2120–2126. [Google Scholar] [CrossRef] [PubMed]
- Sorensen, M.D.; Krieger, J.N. Fournier’s gangrene: Epidemiology and outcomes in the general US population. Urol. Int. 2016, 97, 249–259. [Google Scholar] [CrossRef] [PubMed]
- Chennamsetty, A.; Khourdaji, I.; Burks, F.; Killinger, K.A. Contemporary diagnosis and management of Fournier’s gangrene. Ther. Adv. Urol. 2015, 7, 203–215. [Google Scholar] [CrossRef] [PubMed]
- Wang, T.; Patel, S.M.; Hickman, A.; Liu, X.; Jones, P.L.; Gantz, I.; Koro, C.E. SGLT2 Inhibitors and the Risk of Hospitalization for Fournier’s Gangrene: A Nested Case-Control Study. Diabetes Ther. 2020, 11, 711–723. [Google Scholar] [CrossRef] [PubMed]
- Fadini, G.P.; Sarangdhar, M.; De Ponti, F.; Avogaro, A.; Raschi, E. Pharmacovigilance assessment of the association between Fournier’s gangrene and other severe genital adverse events with SGLT-2 inhibitors. BMJ Open Diabetes Res. Care 2019, 7, e000725. [Google Scholar] [CrossRef] [PubMed]
- Anonymous. MHRA drug safety update: Risk of Fournier’s gangrene with SGLT2 inhibitors for diabetes. Drug Ther. Bull. 2019, 57, 117. [Google Scholar] [CrossRef] [PubMed]
- Kasbawala, K.; Stamatiades, G.A.; Majumdar, S.K. Fournier’s gangrene and diabetic ketoacidosis associated with Sodium glucose co-transporter 2 (SGLT2) inhibitors: Life-threatening complications. Am. J. Case Rep. 2020, 21, e921536. [Google Scholar] [CrossRef] [PubMed]
- Rodler, S.; Weig, T.; Finkenzeller, C.; Stief, C.; Staehler, M. Fournier´s gangrene under sodium-glucose cotransporter 2 inhibitor therapy as a life-threatening adverse event: A case report and review of the literature. Cureus 2019, 11, e5778. [Google Scholar] [CrossRef]
- Dave, C.V.; Schneeweiss, S.; Kim, D.; Fralick, M.; Tong, A.; Patorno, E. Sodium-Glucose Cotransporter-2 Inhibitors and the Risk for Severe Urinary Tract Infections: A Population-Based Cohort Study. Ann. Intern. Med. 2019, 171, 248–256. [Google Scholar] [CrossRef] [PubMed]
- Center for Drug Evaluation, & Research. Warning: Infection of Genital Area with SGLT2 Inhibitors for Diabetes; U.S. Food and Drug Administration: Silver Spring, MD, USA, 2018. Available online: https://www.fda.gov/drugs/drug-safety-and-availability/fda-warns-about-rare-occurrences-serious-infection-genital-area-sglt2-inhibitors-diabetes (accessed on 9 February 2019).
- Agencia Española de Medicamentos y Productos Sanitarios. Boletín Mensual de la AEMPS Sobre Medicamentos de uso Humano del mes de Enero de 2019—Agencia Española de Medicamentos y Productos Sanitarios. Available online: https://www.aemps.gob.es/informa/boletines-aemps/boletinMensual/2019-boletinMensual/boletin-mensual-de-la-aemps-sobre-medicamentos-de-uso-humano-del-mes-de-enero-de-2019/ (accessed on 20 August 2019).
- Hu, Y.; Bai, Z.; Tang, Y.; Liu, R.; Zhao, B.; Gong, J.; Mei, D. Fournier gangrene associated with sodium-glucose cotransporter-2 inhibitors: A pharmacovigilance study with data from the U.S. FDA adverse event reporting system. J. Diabetes Res. 2020, 2020, 3695101. [Google Scholar] [CrossRef]
- Beecroft, N.J.; Jaeger, C.D.; Rose, J.R.; Becerra CM, C.; Shah, N.C.; Palettas, M.S.; Lehman, A.; Posid, T.; Jenkins, L.C.; Baradaran, N. Fournier’s Gangrene in females: Presentation and management at a tertiary center. Urology 2021, 151, 113–117. [Google Scholar] [CrossRef] [PubMed]
- Czymek, R.; Frank, P.; Limmer, S.; Schmidt, A.; Jungbluth, T.; Roblick, U.; Bürk, C.; Bruch, H.-P.; Kujath, P. Fournier’s gangrene: Is the female gender a risk factor? Langenbecks Arch. Surg. 2010, 395, 173–180. [Google Scholar] [CrossRef] [PubMed]
- Hasdemir, A.O.; Büyükaşik, O.; Cöl, C. The clinical characteristics of female patients with Fournier’s gangrene. Int. Urogynecol. J. Pelvic Floor Dysfunct. 2009, 20, 1439–1443. [Google Scholar] [CrossRef] [PubMed]
- Melgar Borrego, A.B.; López Moreda, M.; Martín Méndez, L.; Julián Viñals, R. Gangrena de Fournier. A propósito de un caso. Semergen 2006, 32, 464–467. [Google Scholar] [CrossRef]
- García Morúa, A.; Acuña López, J.A.; Gutiérrez García, J.D.; Martínez Montelongo, R.; Gómez Guerra, L.S. Gangrena de Fournier: Nuestra experiencia en 5 años, revisión de la literatura y valoración del índice de severidad de la Gangrena de Fournier. Arch. Esp. Urol. 2009, 62, 532–540. [Google Scholar] [CrossRef][Green Version]
- Elbeddini, A.; Gallinger, J.; Davey, M.; Brassard, S.; Gazarin, M.; Plourde, F.; Aly, A. A case of Fournier’s Gangrene in a patient taking canagliflozin for the treatment of type II diabetes mellitus. Am. J. Case Rep. 2020, 21, e920115. [Google Scholar] [CrossRef] [PubMed]
- Muchuweti, D.; Muguti, E.; Mungazi, S.G. Spontaneous closure of an extensive postdebridement perineal wound in a newly diagnosed diabetic patient presenting with necrotizing fasciitis. Clin. Case Rep. 2020, 8, 1044–1047. [Google Scholar] [CrossRef] [PubMed]

| Case 1 | Case 2 | Case 3 | |
|---|---|---|---|
| Age | 48 | 84 | 68 |
| Medical history | obesity, poorly controlled T2DM (>15 years) and tobacco | ||
| Surgical history | No | Yes | |
| Current treatment | Metformin 850 mg-Dapagliflozin 5 mg every 12 h for 19 months | Metformin 1 g/Canagliflozin 50 mg every 12 h for 3 months | Metformin 1 g-Empagliflozin 5 mg every 12 h for 39 months |
| HbA1c level | 9% | 8% | 7.2% |
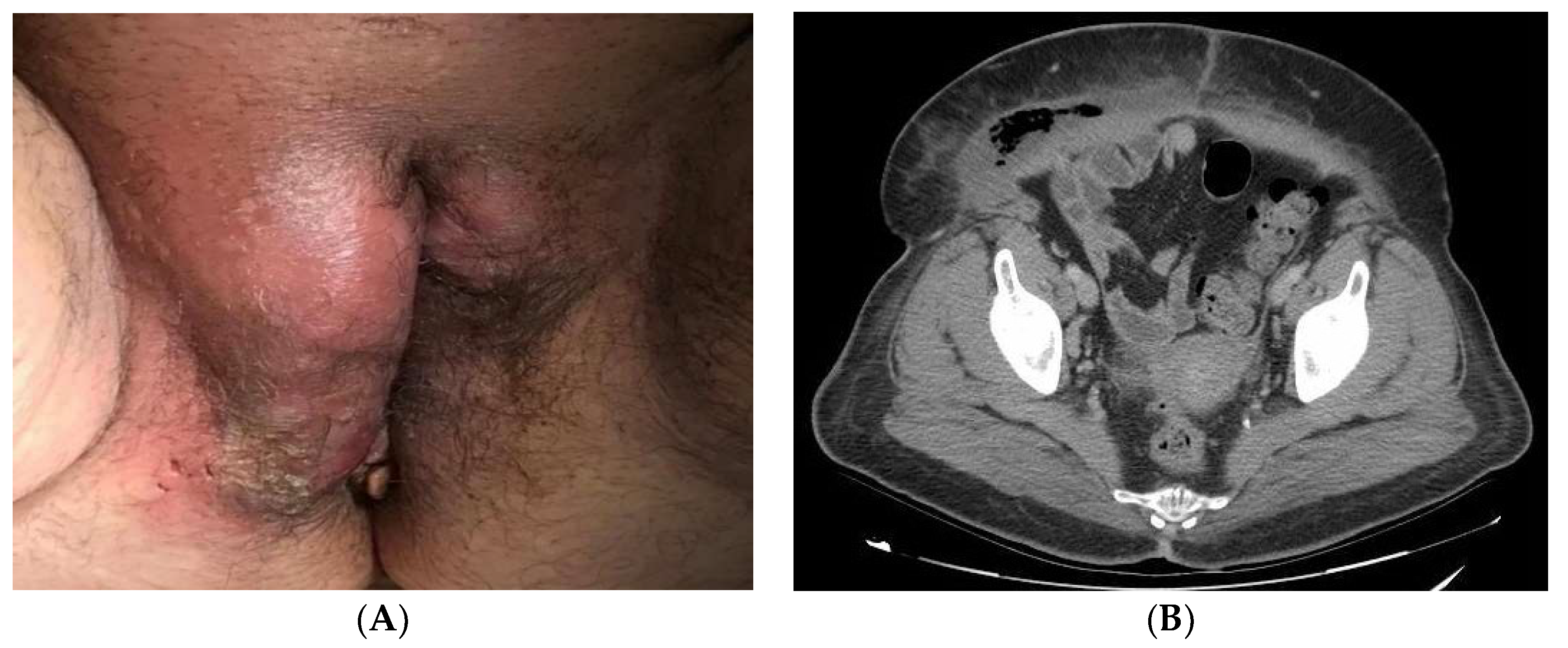
| Signs and symptoms | painful genital lump and/or fever > 38 °C | ||
| Blood analysis | leukocytosis with neutrophilia and CRP elevation | ||
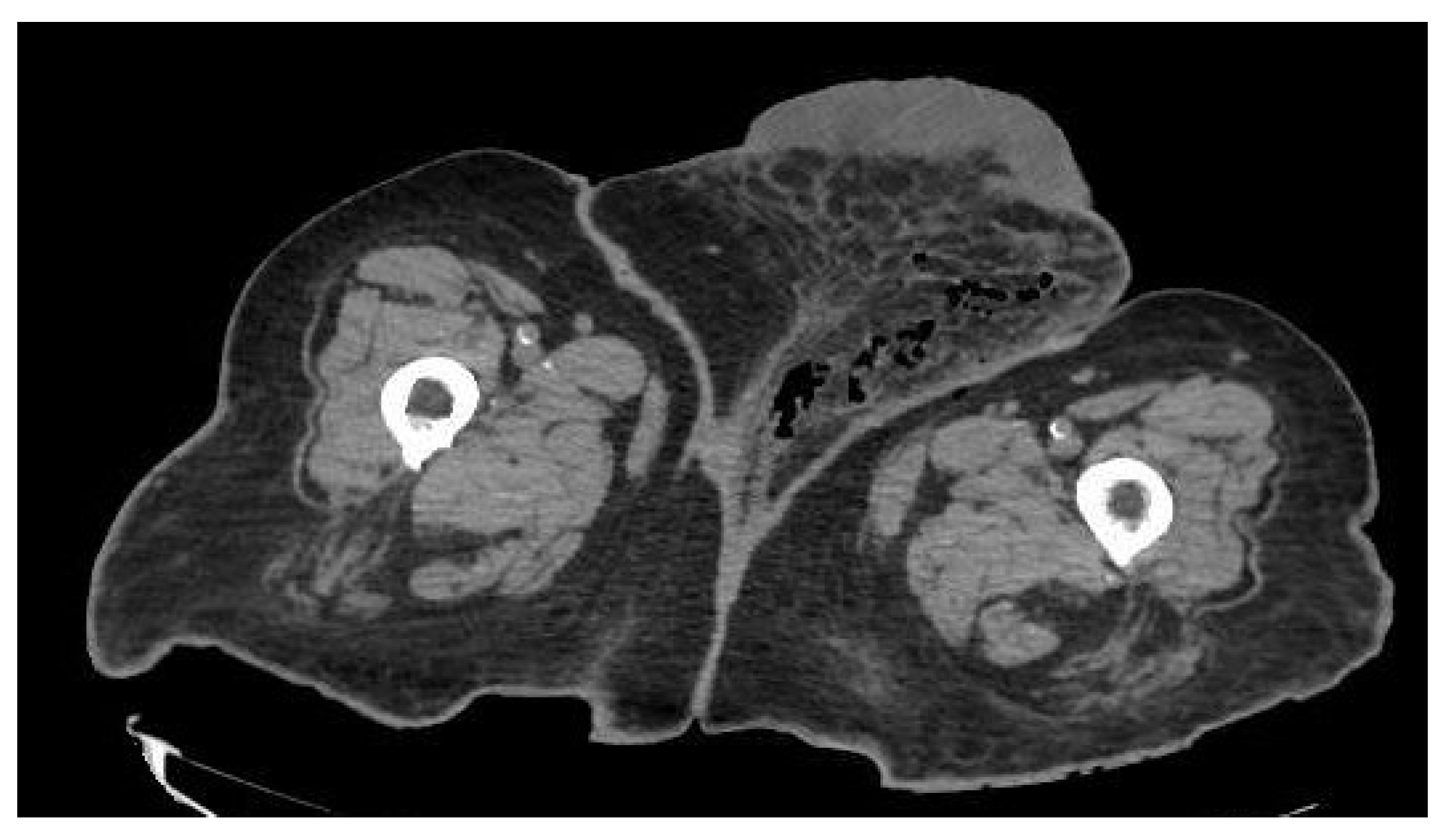
| Abdominal CT | soft tissue emphysema, subcutaneous edema and areas with gas revealing necrotic tissue from gangrene | ||
| Tissue culture | Staphylococcus auricularis and Bacteroides fragilis | Streptococcus anginosus and Prevotella bivia | Aerococcus urinae and Candida albicans |
| Blood culture | negative | ||
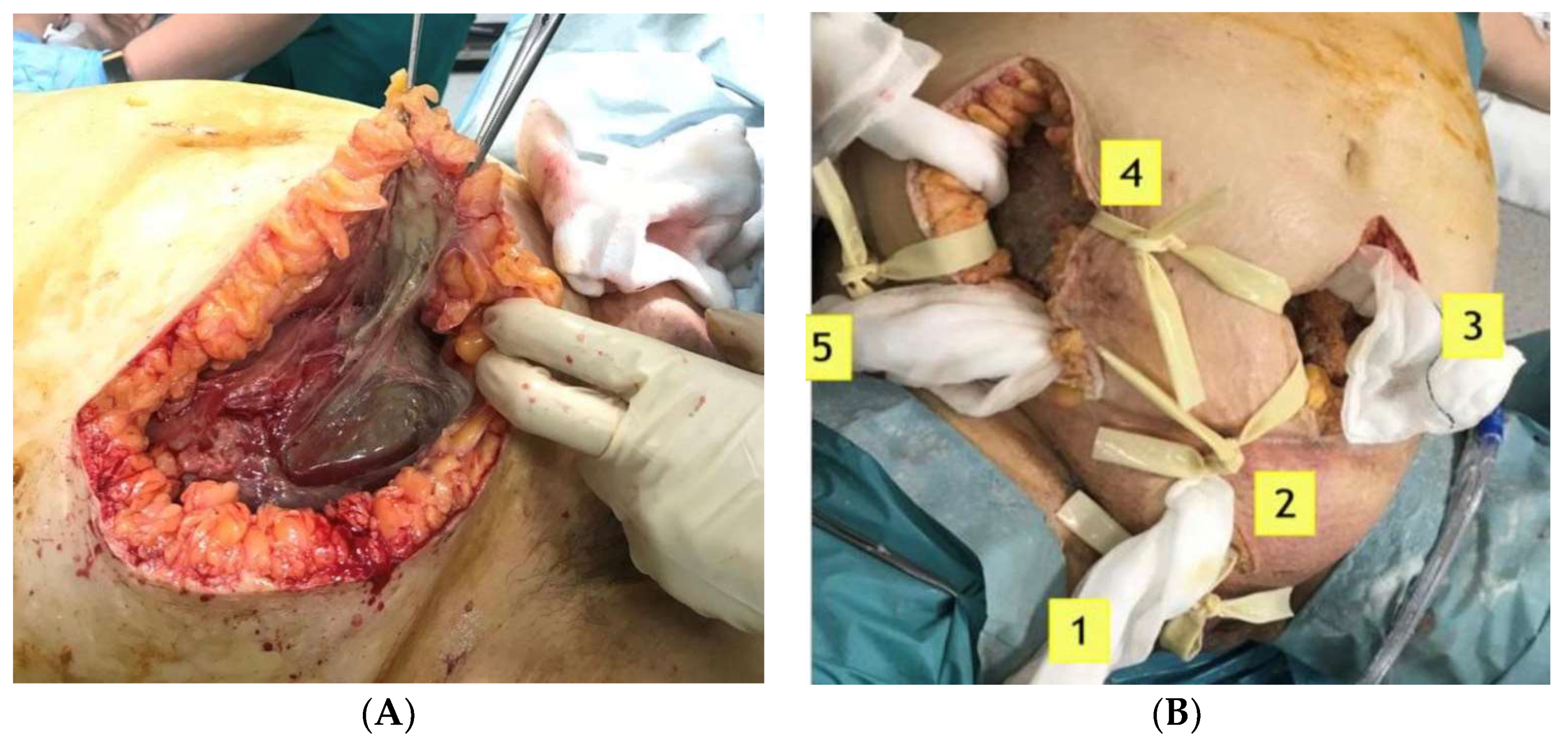
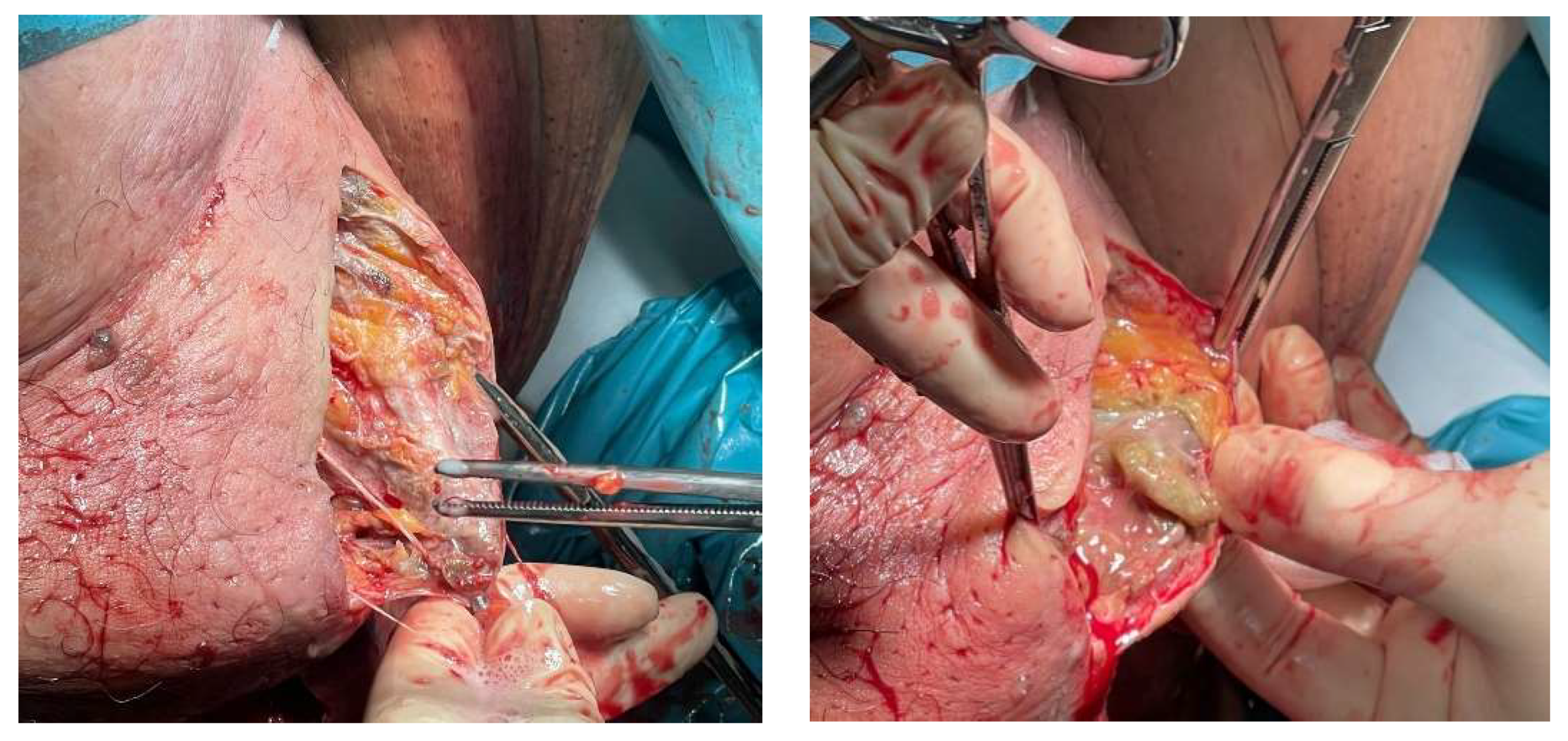
| Treatment | empirical antibiotic therapy and surgical debridement | ||
| Outcome | cured | deceased | Deceased |
| Antibiotic therapy | Meropenem + Daptomycin, later Piperacillin/Tazobactam + Clindamycin | Meropenem + Vancomycin + Clindamycin | Meropenem + Daptomycin + Clindamycin |
| Timing | 25 days | 5 days | 16 days |
| Isolate with residence | Yes | Yes | Yes |
| Surveillance swabs | Yes | ||
| Duration of the stay | 2 months | 5 days | 16 days |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Serrano Olave, A.; Bueno Moral, A.I.; Martínez Bañón, C.; González Mesa, E.; Jiménez López, J.S. Fournier’s Gangrene under Sodium–Glucose Cotransporter-2 Inhibitors Therapy in Gynecological Patients. Int. J. Environ. Res. Public Health 2022, 19, 6261. https://doi.org/10.3390/ijerph19106261
Serrano Olave A, Bueno Moral AI, Martínez Bañón C, González Mesa E, Jiménez López JS. Fournier’s Gangrene under Sodium–Glucose Cotransporter-2 Inhibitors Therapy in Gynecological Patients. International Journal of Environmental Research and Public Health. 2022; 19(10):6261. https://doi.org/10.3390/ijerph19106261
Chicago/Turabian StyleSerrano Olave, Adriana, Ana Isabel Bueno Moral, Carmen Martínez Bañón, Ernesto González Mesa, and Jesús S. Jiménez López. 2022. "Fournier’s Gangrene under Sodium–Glucose Cotransporter-2 Inhibitors Therapy in Gynecological Patients" International Journal of Environmental Research and Public Health 19, no. 10: 6261. https://doi.org/10.3390/ijerph19106261
APA StyleSerrano Olave, A., Bueno Moral, A. I., Martínez Bañón, C., González Mesa, E., & Jiménez López, J. S. (2022). Fournier’s Gangrene under Sodium–Glucose Cotransporter-2 Inhibitors Therapy in Gynecological Patients. International Journal of Environmental Research and Public Health, 19(10), 6261. https://doi.org/10.3390/ijerph19106261








