De-Sexualizing Partner Notification: A Qualitative Study on Chinese Young Adults with Chlamydia
Abstract
1. Introduction
2. Materials and Methods
2.1. Sampling and Recruitment
2.2. Procedure
2.3. Interview Schedule
2.4. Data Analysis
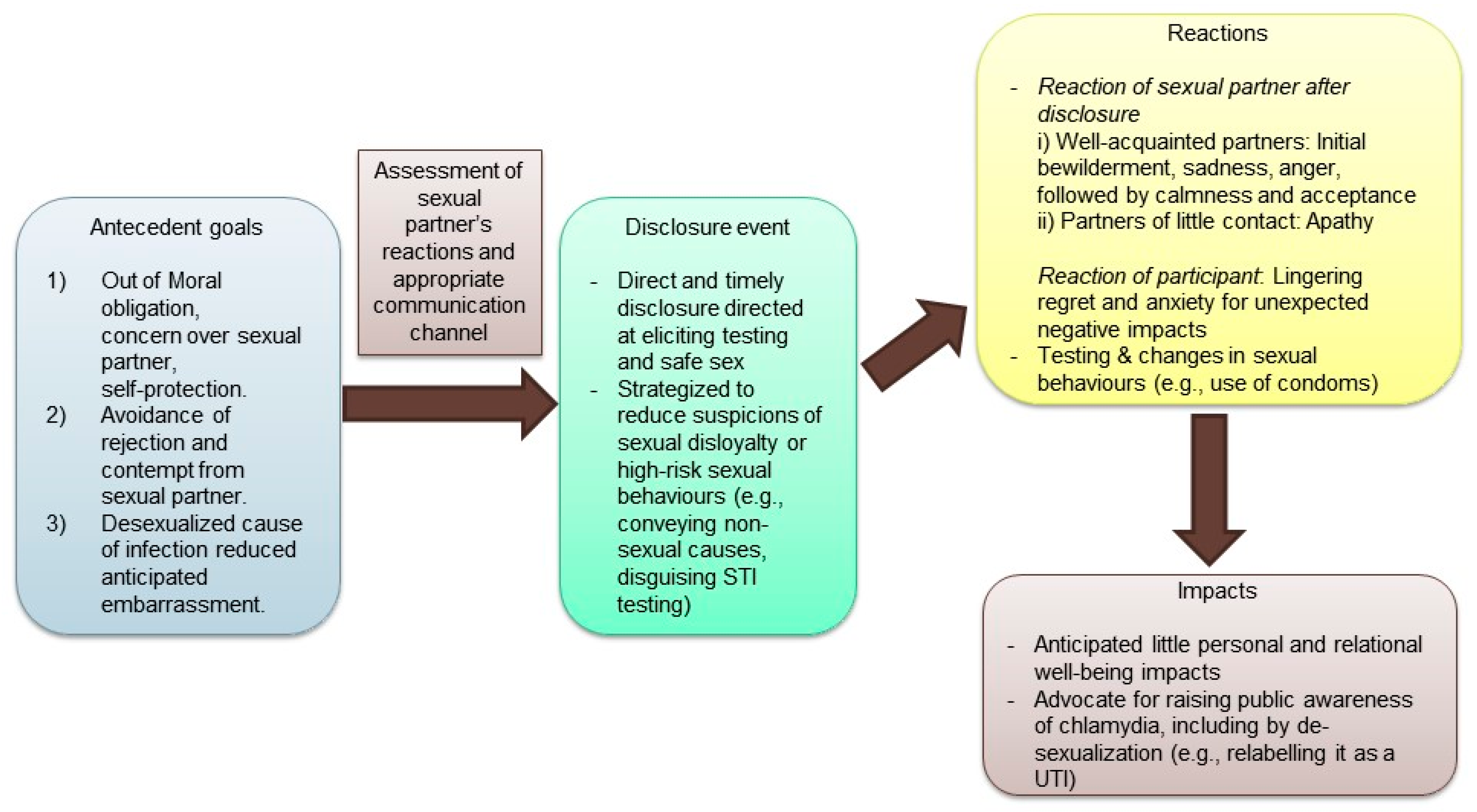
3. Results
3.1. Disclosure as a Difficult Decision But a Moral Responsibility
First, I want her (ex-girlfriend) to be well. Second, I don’t want others to have it. (Participant 007; male; disclosed).
I think this (chlamydia) is a disgrace. [Interviewer: But it might not be not your fault] But I think he (a sexual partner) anyway will mind. Likewise, if my partner tells me he has a STI, although it’s none of his fault, I won’t be all comfortable. (Participant 005; female; not disclosed)
I think I may send him (a sexual partner) a relevant website and ask what he thinks about it. If his reaction is unpleasant and it’s likely that he will gossip about me, I won’t disclose. If his reaction is OK and normal, I think there will be a better chance I will disclose. (Participant 015; female; disclosed)
3.2. Embarrassment of Disclosure Reduced with the Belief in a Non-Sexual Cause of One’s Infection
Interviewer: Okay. Was he worried about your condition?Participant: To my knowledge, not really. I think this (chlamydia) is just because of a dirty toilet.Interviewer: Did he ever thought about it might not be because of the toilet? Do you think he had ever suspected anything related to sex?Participant: To my understanding, no.Interviewer: So, are you two still together?Participant: Yes. (Participant 014; female; disclosed)
3.3. Strategizing Disclosure by De-Sexualizing the Mode of Transmission and Testing
I wrote a message on WhatsApp which said I have no bad intentions, but I want her (ex-girlfriend) to be careful (in future sex), it is for her benefits. I told her the treatment method, the antibiotics and suggested her to go and check with a doctor. (Participant 007; male; disclosed)
Our society always regard sex as such a negative thing and STI as a severe illness and is very negative. Why not call it (chlamydia) an UTI? For UTI, it might be difficult to tell (the cause), it could have come from a dirty toilet in a mall. But right now, the STI label makes it a very negative thing, but the experience of the infection itself is not too negative. (Participant 014; female; disclosed)
3.4. Lack of Relief Despite a Positive Response from Their Sexual Partner(s)
We had some conflicts. He (current boyfriend) said he thought I was a nice girl, he didn’t use the word “clean” to describe me, but he thought I was, how should I put it, safe, not possessing anything bad, etc. He said that was why he didn’t use a condom with me. I thought I didn’t know I’ve been infected too, how dare he say something so hurtful. (Participant 013; female; disclosed)
3.5. Changes in Sexual Practices
3.6. Impacts on Personal and Relational Well-Being
4. Discussion
Strength and Limitations of the Study
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Rowley, J.; Vander Hoorn, S.; Korenromp, E.; Low, N.; Unemo, M.; Abu-Raddad, L.J.; Chico, R.M.; Smolak, A.; Newman, L.; Gottlieb, S. Chlamydia, gonorrhoea, trichomoniasis and syphilis: Global prevalence and incidence estimates, 2016. Bull. World Health Organ. 2019, 97, 548. [Google Scholar] [CrossRef] [PubMed]
- Parish, W.L.; Laumann, E.O.; Cohen, M.S.; Pan, S.; Zheng, H.; Hoffman, I.; Wang, T.; Ng, K.H. Population-based study of chlamydial infection in China: A hidden epidemic. JAMA 2003, 289, 1265–1273. [Google Scholar] [CrossRef]
- Luo, Z.-Z.; Li, W.; Wu, Q.-H.; Zhang, L.; Tian, L.-S.; Liu, L.-L.; Ding, Y.; Yuan, J.; Chen, Z.-W.; Lan, L.-N. Population-based study of chlamydial and gonococcal infections among women in Shenzhen, China: Implications for programme planning. PLoS ONE 2018, 13, e0196516. [Google Scholar]
- Wong, W.C.W.; Zhao, Y.; Wong, N.S.; Parish, W.L.; Miu, H.Y.H.; Yang, L.-G.; Emch, M.; Ho, K.M.; Fong, F.Y.; Tucker, J.D. Prevalence and risk factors of chlamydia infection in Hong Kong: A population-based geospatial household survey and testing. PLoS ONE 2017, 12, e0172561. [Google Scholar] [CrossRef] [PubMed]
- Unemo, M.; Bradshaw, C.S.; Hocking, J.S.; de Vries, H.J.; Francis, S.C.; Mabey, D.; Marrazzo, J.M.; Sonder, G.J.; Schwebke, J.R.; Hoornenborg, E. Sexually transmitted infections: Challenges ahead. Lancet Infect. Dis. 2017, 17, e235–e279. [Google Scholar] [CrossRef]
- Ward, H.; Bell, G. Partner notification. Medicine 2014, 42, 314–317. [Google Scholar] [CrossRef]
- Turner, K.; Adams, E.; Grant, A.; Macleod, J.; Bell, G.; Clarke, J.; Horner, P. Costs and cost effectiveness of different strategies for chlamydia screening and partner notification: An economic and mathematical modelling study. BMJ 2011, 342, c7250. [Google Scholar] [CrossRef]
- Balfe, M.; Brugha, R.; O’Donovan, D.; O’Connell, E.; Vaughan, D. Young women’s decisions to accept chlamydia screening: Influences of stigma and doctor-patient interactions. BMC Public Health 2010, 10, 1–11. [Google Scholar] [CrossRef]
- Duncan, B.; Hart, G.; Scoular, A.; Bigrigg, A. Qualitative analysis of psychosocial impact of diagnosis of Chlamydia trachomatis: Implications for screening. BMJ 2001, 322, 195. [Google Scholar] [CrossRef]
- Kangas, I.; Andersen, B.; Olesen, F.; Møller, J.K.; Østergaard, L. Psychosocial impact of Chlamydia trachomatis testing in general practice. Br. J. Gen. Pract. 2006, 56, 587–593. [Google Scholar]
- Pimenta, J.; Catchpole, M.; Rogers, P.; Hopwood, J.; Randall, S.; Mallinson, H.; Perkins, E.; Jackson, N.; Carlisle, C.; Hewitt, G. Opportunistic screening for genital chlamydial infection. II: Prevalence among healthcare attenders, outcome, and evaluation of positive cases. Sex. Transm. Infect. 2003, 79, 22–27. [Google Scholar] [CrossRef]
- Zhang, K.-l.; Beck, E. Changing sexual attitudes and behaviour in China: Implications for the spread of HIV and other sexually transmitted diseases. AIDS Care 1999, 11, 581–589. [Google Scholar] [CrossRef] [PubMed]
- Pan, S. A sex revolution in current China. J. Psychol. Hum. Sex. 1994, 6, 1–14. [Google Scholar] [CrossRef]
- Pei, Y.; Ho, P.S.Y.; Ng, M.L. Studies on women’s sexuality in China since 1980: A critical review. J. Sex Res. 2007, 44, 202–212. [Google Scholar]
- Cao, H.; Zhou, N.; Fine, M.A.; Li, X.; Fang, X. Sexual satisfaction and marital satisfaction during the early years of Chinese marriage: A three-wave, cross-lagged, actor–partner interdependence model. J. Sex Res. 2019, 56, 391–407. [Google Scholar] [CrossRef] [PubMed]
- Zheng, W.; Zhou, X.; Zhou, C.; Liu, W.; Li, L.; Hesketh, T. Detraditionalisation and attitudes to sex outside marriage in China. Cult. Health Sex. 2011, 13, 497–511. [Google Scholar] [CrossRef]
- Chaudoir, S.R.; Fisher, J.D. The disclosure processes model: Understanding disclosure decision making and postdisclosure outcomes among people living with a concealable stigmatized identity. Psychol. Bull. 2010, 136, 236. [Google Scholar] [CrossRef] [PubMed]
- Balfe, M.; Brugha, R. Disclosure of STI testing activities by young adults: The influence of emotions and social networks. Sociol. Health Illn. 2010, 32, 1041–1058. [Google Scholar] [CrossRef]
- Liu, H.; Detels, R.; Li, X.; Ma, E.; Yin, Y. Stigma, delayed treatment, and spousal notification among male patients with sexually transmitted disease in China. Sex. Transm. Dis. 2002, 29, 335–343. [Google Scholar] [CrossRef]
- Dempsey, A.F. On the implications of desexualizing vaccines against sexually transmitted diseases: Reflections from a practicing pediatrician. Isr. J. Health Policy Res. 2017, 6, 1–3. [Google Scholar] [CrossRef]
- Velan, B.; Yadgar, Y. On the implications of desexualizing vaccines against sexually transmitted diseases: Health policy challenges in a multicultural society. Isr. J. Health Policy Res. 2017, 6, 1–12. [Google Scholar] [CrossRef]
- Bilardi, J.E.; Fairley, C.K.; Hopkins, C.A.; Hocking, J.S.; Temple-Smith, M.J.; Bowden, F.J.; Russell, D.B.; Pitts, M.; Tomnay, J.E.; Parker, R.M. Experiences and outcomes of partner notification among men and women recently diagnosed with chlamydia and their views on innovative resources aimed at improving notification rates. Sex. Transm. Dis. 2010, 37, 253–258. [Google Scholar] [CrossRef] [PubMed]
- Gottlieb, S.L.; Stoner, B.P.; Zaidi, A.A.; Buckel, C.; Tran, M.; Leichliter, J.S.; Berman, S.M.; Markowitz, L.E. A prospective study of the psychosocial impact of a positive Chlamydia trachomatis laboratory test. Sex. Transm. Dis. 2011, 38, 1004–1011. [Google Scholar] [CrossRef] [PubMed]
- Theunissen, K.A.M.; Bos, A.E.; Hoebe, C.J.; Kok, G.; Vluggen, S.; Crutzen, R.; Dukers-Muijrers, N.H. Chlamydia trachomatis testing among young people: What is the role of stigma? BMC Public Health 2015, 15, 1–8. [Google Scholar] [CrossRef] [PubMed]
- Gao, Y.; Lu, Z.; Shi, R.; Sun, X.; Cai, Y. AIDS and sex education for young people in China. Reprod. Fertil. Dev. 2001, 13, 729–737. [Google Scholar] [CrossRef]
- Pavlin, N.L.; Parker, R.; Fairley, C.K.; Gunn, J.M.; Hocking, J. Take the sex out of STI screening! Views of young women on implementing chlamydia screening in General Practice. BMC Infect. Dis. 2008, 8, 1–5. [Google Scholar] [CrossRef] [PubMed]
- Ferreira, A.; Young, T.; Mathews, C.; Zunza, M.; Low, N. Strategies for partner notification for sexually transmitted infections, including HIV. Cochrane Database Syst. Rev. 2013, 10. [Google Scholar] [CrossRef] [PubMed]
| Variable | Category | Frequency (%) |
|---|---|---|
| Gender | Male | 3 (18.7%) |
| Female | 13 (81.3%) | |
| Mean age (range) | 23.4 (20 to 31) years | |
| Education | Undergraduate or above | 10 (62.5%) |
| Higher diploma | 3 (18.8%) | |
| Senior secondary | 2 (12.5%) | |
| Junior secondary | 1 (6.2%) | |
| Occupation | Student | 1 (6.2%) |
| Full-time worker | 10 (62.5%) | |
| office administrative | 6 (37.5%) | |
| finance | 1 (6.2%) | |
| design | 1 (6.2%) | |
| healthcare professional | 1 (6.2%) | |
| social work | 1 (6.2%) | |
| Part-time worker | 4 (25.0%) | |
| Housewife | 1 (6.2%) | |
| Current relationship | Single | 6 (37.5%) |
| Stable relationship | 9 (56.3%) | |
| Divorced | 1 (6.2%) | |
| Number of sex partners in previous year | 0–1 | 7 (43.8%) |
| 2–5 | 8 (50.0%) | |
| >5 | 1 (6.2%) | |
| Sexual orientation | Heterosexual | 15 (93.8%) |
| Homosexual | 1 (6.2%) | |
| Previous urinary tract infection (UTI) or | Candidiasis | 3 (18.8%) |
| sexually transmitted infection (STI) | UTI | 1 (6.2%) |
| Unknown | 1 (6.2%) | |
| No history of UTI or STI | 11 (68.8%) |
| 1. Disguise STI testing as gynecological examination or general body check: Maybe I will make up stories about having done a body check, something like those provided by medical insurance, and the check includes a STI test and there I got the results. (Participant 010; female; disclosed) |
| 2. Emphasize the possibility of non-sexual means of transmission (e.g., contaminated underwear, sharing contaminated towels in a trip abroad, dirty toilets): I would say even if you have not had sex, you could be infected, for instance the towels, or the weather is too hot and there wasn’t thorough cleansing. (Participant 007; male; disclosed) |
| 3. Focus the conversation on the desired action (e.g., practice safe sex in the future, testing) rather than the cause or the embarrassing past: I skipped the part related to my one-night stand and only urged him (current partner) to have a check. (Participant 002; female; disclosed) |
| 4. Emphasize sexual loyalty with the current partner: I told him (current partner) directly I have not been fooling around, before I mentioned anything about the test. (Participant 002; female; disclosed) |
| 5. Nominate a distant ex-partner as the source of the infection: Even if he (current partner) kept asking I couldn’t give him an answer. I just randomly mention an ex-partner, he anyway doesn’t know my ex-partners. (Participant 013; female; disclosed) |
| 6. Make comparisons with other more severe STIs (e.g., HIV, syphilis): I asked him (current partner) to guess my diagnosis. He came up with something much scarier. Then I said no and that I had chlamydia. (Interviewer: Was he relieved?) Yes. But this is still a good thing, now he treats chlamydia more seriously. (Participant 015; female; disclosed) |
| 7. Disclose information in manageable bite-size. Do not overwhelm the sexual partner with esoteric medical terms (including the term “chlamydia”): (Interviewer: Did you tell her it is chlamydia?) No, because many people don’t know what chlamydia is. (Participant 007; male; disclosed) |
| 8. Disclose with a comfortable means for conversing private and sensitive topics: I have thought about finding a time to talk about it face-to-face. But I’m afraid I can’t kick off the conversation. (Interviewer: What about not doing it face-to-face?) A phone call then. At least a call to disclose a short version, that is roughly what I have, and then leave the details to the face-to-face meeting. With that phone call to begin with, we won’t be that embarrassed when meeting up. (Participant 013; female; disclosed) |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Lau, B.H.P.; Liu, L.; Chan, C.H.Y.; Chan, C.L.W.; Ong, J.J.; Holroyd, E.; Wong, W.C.W. De-Sexualizing Partner Notification: A Qualitative Study on Chinese Young Adults with Chlamydia. Int. J. Environ. Res. Public Health 2021, 18, 4032. https://doi.org/10.3390/ijerph18084032
Lau BHP, Liu L, Chan CHY, Chan CLW, Ong JJ, Holroyd E, Wong WCW. De-Sexualizing Partner Notification: A Qualitative Study on Chinese Young Adults with Chlamydia. International Journal of Environmental Research and Public Health. 2021; 18(8):4032. https://doi.org/10.3390/ijerph18084032
Chicago/Turabian StyleLau, Bobo H. P., Lucia Liu, Celia H. Y. Chan, Cecilia L. W. Chan, Jason J. Ong, Eleanor Holroyd, and William C. W. Wong. 2021. "De-Sexualizing Partner Notification: A Qualitative Study on Chinese Young Adults with Chlamydia" International Journal of Environmental Research and Public Health 18, no. 8: 4032. https://doi.org/10.3390/ijerph18084032
APA StyleLau, B. H. P., Liu, L., Chan, C. H. Y., Chan, C. L. W., Ong, J. J., Holroyd, E., & Wong, W. C. W. (2021). De-Sexualizing Partner Notification: A Qualitative Study on Chinese Young Adults with Chlamydia. International Journal of Environmental Research and Public Health, 18(8), 4032. https://doi.org/10.3390/ijerph18084032







