Adolescent Menstrual Health Literacy in Low, Middle and High-Income Countries: A Narrative Review
Abstract
1. Introduction
2. Materials and Methods
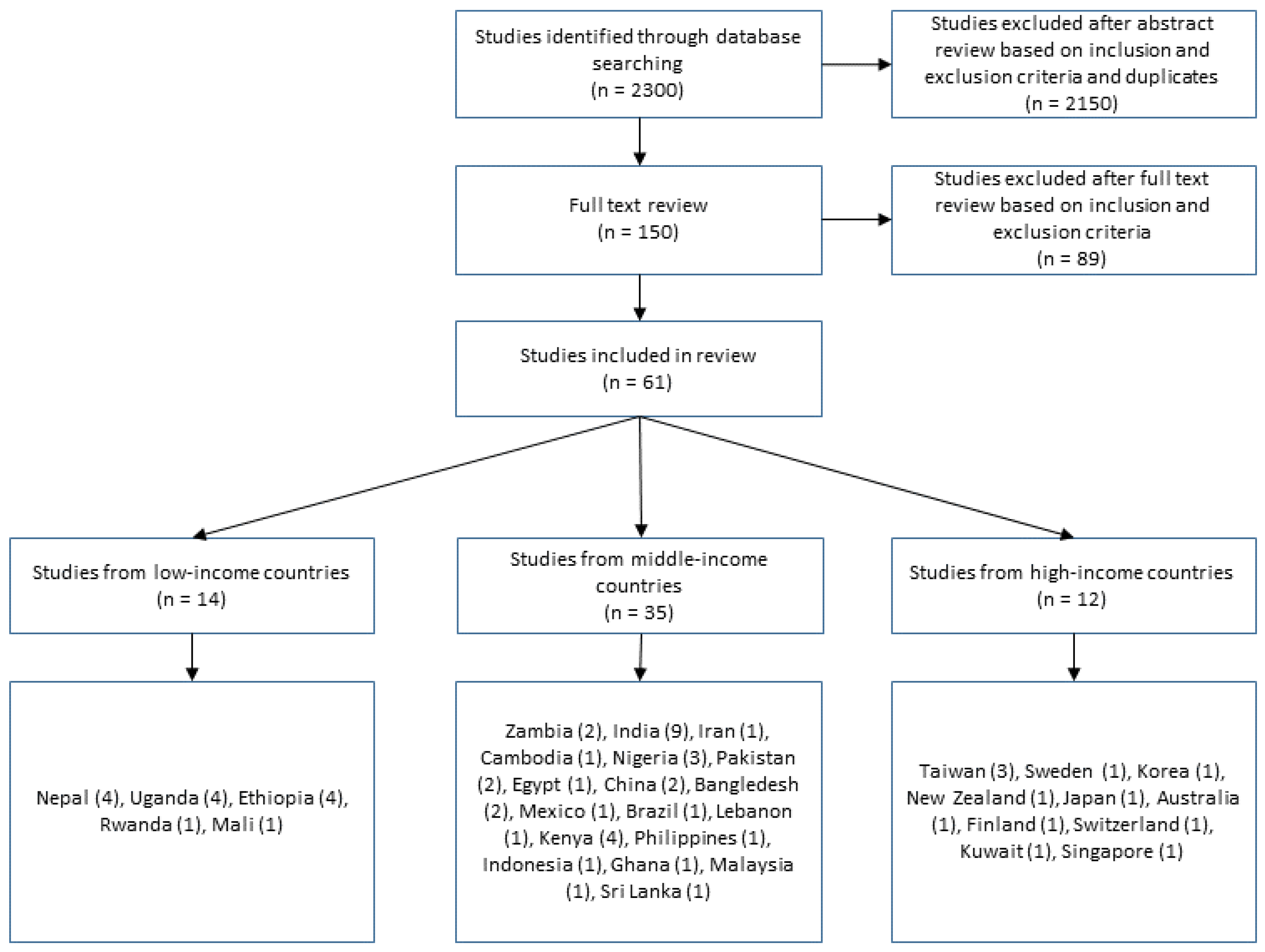
2.1. Search Strategy and Results
2.2. Inclusion and Exclusion Criteria
- Delivery of menstrual health education in schools;
- Policies and reports related to menstrual health literacy in schools;
- Attitudes and biases towards menstrual health literacy impacting school-going adolescents;
- Assessing menstrual hygiene management within schools;
- Intervention studies of menstrual health education programs in schools;
- Dysmenorrhea education and treatment in schools.
- Articles that were excluded:
- Those that focused on menstrual health literacy beyond schools, i.e., colleges, universities and the general community;
- Those that were published before 2008.
2.3. Thematic Analysis
- Menstrual hygiene management;
- Menstrual health issues;
- Attitudes towards menstruation.
3. Results and Discussion
3.1. Menstrual Hygiene Management
Low and Middle-Income Countries (LMICs)
3.2. Menstrual Health Issues
3.2.1. Low and Middle-Income Countries (LMICs)
3.2.2. High-Income Countries (HICs)
3.3. Attitudes towards Menstruation
3.3.1. Low and Middle-Income Countries (LMICs)
3.3.2. High-Income Countries (HICs)
3.4. Limitations
4. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Puberty Education & Menstrual Hygiene Management—UNESCO Digital Library; United Nations Educational, Scientific and Cultural Organization: Paris, France, 2014.
- Armour, M.; Parry, K.; Manohar, N.; Holmes, K.; Ferfolja, T.; Curry, C.; MacMillan, F.; Smith, C.A. The Prevalence and Academic Impact of Dysmenorrhea in 21,573 Young Women: A Systematic Review and Meta-Analysis. J. Womens Health 2019, 28, 1161–1171. [Google Scholar] [CrossRef]
- Keith, B. Girls’ and Women’s Right to Menstrual Health: Evidence and Opportunities; PATH: Seattle, WA, USA, 2016. [Google Scholar]
- Kane-Hartnett, L. Integrating Menstrual Hygiene Management to Achieve the SDGs; International Women’s Health Coalition: New York, NY, USA, 2018. [Google Scholar]
- Hawkey, A.J.; Ussher, J.M.; Perz, J.; Metusela, C. Experiences and Constructions of Menarche and Menstruation Among Migrant and Refugee Women. Qual. Health Res. 2017, 27, 1473–1490. [Google Scholar] [CrossRef]
- Metusela, C.; Ussher, J.; Perz, J.; Hawkey, A.; Morrow, M.; Narchal, R.; Estoesta, J.; Monteiro, M. “In My Culture, We Don’t Know Anything about That”: Sexual and Reproductive Health of Migrant and Refugee Women. Int. J. Behav. Med. 2017, 24, 836–845. [Google Scholar] [CrossRef]
- Bellis, E.K.; Li, A.D.; Jayasinghe, Y.L.; Girling, J.E.; Grover, S.R.; Peate, M.; Marino, J.L. Exploring the Unmet Needs of Parents of Adolescent Girls with Heavy Menstrual Bleeding and Dysmenorrhea: A Qualitative Study. J. Pediatr. Adolesc. Gynecol. 2020, 33, 271–277. [Google Scholar] [CrossRef] [PubMed]
- Li, A.D.; Bellis, E.K.; Girling, J.E.; Jayasinghe, Y.L.; Grover, S.R.; Marino, J.L.; Peate, M. Unmet Needs and Experiences of Adolescent Girls with Heavy Menstrual Bleeding and Dysmenorrhea: A Qualitative Study. J. Pediatr. Adolesc. Gynecol. 2020, 33, 278–284. [Google Scholar] [CrossRef]
- Armour, M.; Hyman, M.S.; Al-Dabbas, M.; Parry, K.; Ferfolja, T.; Curry, C.; MacMillan, F.; Smith, C.A.; Holmes, K. Menstrual Health Literacy and Management Strategies in Young Women in Australia: A National Online Survey of Young Women Aged 13-25 Years. J. Pediatr. Adolesc. Gynecol. 2020. [Google Scholar] [CrossRef]
- Hennegan, J.; Shannon, A.K.; Rubli, J.; Schwab, K.J.; Melendez-Torres, G.J. Women’s and Girls’ Experiences of Menstruation in Low- and Middle-Income Countries: A Systematic Review and Qualitative Metasynthesis. PLOS Med. 2019, 16, e1002803. [Google Scholar] [CrossRef]
- Menstruation; Plan International: Surrey, UK, 2019.
- Kilfoyle, K.A.; Vitko, M.; O’Conor, R.; Bailey, S.C. Health Literacy and Women’s Reproductive Health: A Systematic Review. J. Womens Health 2016, 25, 1237–1255. [Google Scholar] [CrossRef] [PubMed]
- Chandra-Mouli, V.; Patel, S.V. Mapping the Knowledge and Understanding of Menarche, Menstrual Hygiene and Menstrual Health among Adolescent Girls in Low- and Middle-Income Countries. Reprod. Health 2017, 14. [Google Scholar] [CrossRef]
- Armour, M.; Ferfolja, T.; Curry, C.; Hyman, M.S.; Parry, K.; Chalmers, K.J.; Smith, C.A.; MacMillan, F.; Holmes, K. The Prevalence and Educational Impact of Pelvic and Menstrual Pain in Australia: A National Online Survey of 4202 Young Women Aged 13–25 Years. J. Pediatr. Adolesc. Gynecol. 2020, 33, 511–518. [Google Scholar] [CrossRef] [PubMed]
- Parker, M.; Sneddon, A.; Arbon, P. The Menstrual Disorder of Teenagers (MDOT) Study: Determining Typical Menstrual Patterns and Menstrual Disturbance in a Large Population-Based Study of Australian Teenagers: The MDOT Study. BJOG Int. J. Obstet. Gynaecol. 2010, 117, 185–192. [Google Scholar] [CrossRef]
- Nur Azurah, A.G.; Sanci, L.; Moore, E.; Grover, S. The Quality of Life of Adolescents with Menstrual Problems. J. Pediatr. Adolesc. Gynecol. 2013, 26, 102–108. [Google Scholar] [CrossRef] [PubMed]
- Armour, M.; Parry, K.; Al-Dabbas, M.A.; Curry, C.; Holmes, K.; MacMillan, F.; Ferfolja, T.; Smith, C.A. Self-Care Strategies and Sources of Knowledge on Menstruation in 12,526 Young Women with Dysmenorrhea: A Systematic Review and Meta-Analysis. PLoS ONE 2019, 14, e0220103. [Google Scholar] [CrossRef]
- Bush, D.; Brick, E.; East, M.C.; Johnson, N. Endometriosis Education in Schools: A New Zealand Model Examining the Impact of an Education Program in Schools on Early Recognition of Symptoms Suggesting Endometriosis. Aust. N. Z. J. Obstet. Gynaecol. 2017, 57, 452–457. [Google Scholar] [CrossRef]
- Schoep, M.E.; Nieboer, T.E.; van der Zanden, M.; Braat, D.D.M.; Nap, A.W. The Impact of Menstrual Symptoms on Everyday Life: A Survey among 42,879 Women. Am. J. Obstet. Gynecol. 2019, 220, 569.e1–569.e7. [Google Scholar] [CrossRef] [PubMed]
- Iacovides, S.; Avidon, I.; Baker, F.C. What We Know about Primary Dysmenorrhea Today: A Critical Review. Hum. Reprod. Update 2015, 21, 762–778. [Google Scholar] [CrossRef]
- Hillen, T.I.J.; Grbavac, S.L.; Johnston, P.J.; Straton, J.A.Y.; Keogh, J.M.F. Primary Dysmenorrhea in Young Western Australian Women: Prevalence, Impact, and Knowledge of Treatment. J. Adolesc. Health 1999, 25, 40–45. [Google Scholar] [CrossRef]
- Donovan, S.; Telfar-Barnard, L. Age of First Menstruation in New Zealand: Findings from First Ever National-Level Data and Implications for Age-Appropriate Education and Support. N. Z. Med. J. 2019, 132, 1500. [Google Scholar]
- World Bank Country & Lending Groups; The World Bank: Washington, DC, USA, 2019.
- Braun, V.; Clarke, V. Using Thematic Analysis in Psychology. Qual. Res. Psychol. 2006, 3, 77–101. [Google Scholar] [CrossRef]
- Maguire, M.; Delahunt, B. Doing a Thematic Analysis: A Practical, Step-by-Step Guide for Learning and Teaching Scholars. Irel. J. Teach. Learn. High. Educ. 2017, 9. [Google Scholar]
- Chinyama, J.; Chipungu, J.; Rudd, C.; Mwale, M.; Verstraete, L.; Sikamo, C.; Mutale, W.; Chilengi, R.; Sharma, A. Menstrual Hygiene Management in Rural Schools of Zambia: A Descriptive Study of Knowledge, Experiences and Challenges Faced by Schoolgirls. BMC Public Health 2019, 19. [Google Scholar] [CrossRef]
- Tegegne, T.K.; Sisay, M.M. Menstrual Hygiene Management and School Absenteeism among Female Adolescent Students in Northeast Ethiopia. BMC Public Health 2014, 14, 1–14. [Google Scholar] [CrossRef]
- Boosey, R.; Prestwich, G.; Deave, T. Menstrual Hygiene Management amongst Schoolgirls in the Rukungiri District of Uganda and the Impact on Their Education: A Cross-Sectional Study. Pan Afr. Med. J. 2014, 19. [Google Scholar] [CrossRef] [PubMed]
- Naeem, K.; Klawitter, S.; Aziz, A. Learning, Acting, and Learning (LAL) Research on Schools’ Menstrual Hygiene Management (MHM): Pakistan. Waterlines 2015, 34, 103–112. [Google Scholar] [CrossRef]
- Vashisht, A.; Pathak, R.; Agarwalla, R.; Patavegar, B.N.; Panda, M. School Absenteeism during Menstruation amongst Adolescent Girls in Delhi, India. J. Fam. Community Med. 2018, 25, 163–168. [Google Scholar] [CrossRef]
- Yadav, R.N.; Joshi, S.; Poudel, R.; Pandeya, P. Knowledge, Attitude, and Practice on Menstrual Hygiene Management among School Adolescents. J. Nepal Health Res. Counc. 2018, 15, 212–216. [Google Scholar] [CrossRef]
- Connolly, S.; Sommer, M. Cambodian Girls’ Recommendations for Facilitating Menstrual Hygiene Management in School. J. Water Sanit. Hyg. Dev. 2013, 3, 612–622. [Google Scholar] [CrossRef]
- Lahme, A.M.; Stern, R.; Cooper, D. Factors Impacting on Menstrual Hygiene and Their Implications for Health Promotion. Glob. Health Promot. 2018, 25, 54–62. [Google Scholar] [CrossRef]
- Srivastava, S.; Chandra, M. Study on the Knowledge of School Girls Regarding Menstrual and Reproductive Health and Their Perceptions about Family Life Education Program. Int. J. Reprod. Contracept. Obstet. Gynecol. 2017, 6, 688. [Google Scholar] [CrossRef][Green Version]
- Mahajan, A.; Kaushal, K. A Descriptive Study to Assess the Knowledge and Practice Regarding Menstrual Hygiene among Adolescent Girls of Government School of Shimla, Himachal Pradesh. CHRISMED J. Health Res. 2017, 4, 99. [Google Scholar] [CrossRef]
- Sivakami, M.; van Maria Eijk, A.; Thakur, H.; Kakade, N.; Patil, C.; Shinde, S.; Surani, N.; Bauman, A.; Zulaika, G.; Kabir, Y.; et al. Effect of Menstruation on Girls and Their Schooling, and Facilitators of Menstrual Hygiene Management in Schools: Surveys in Government Schools in Three States in India, 2015. J. Glob. Health 2019, 9. [Google Scholar] [CrossRef]
- Alam, M.-U.; Luby, S.P.; Halder, A.K.; Islam, K.; Opel, A.; Shoab, A.K.; Ghosh, P.K.; Rahman, M.; Mahon, T.; Unicomb, L. Menstrual Hygiene Management among Bangladeshi Adolescent Schoolgirls and Risk Factors Affecting School Absence: Results from a Cross-Sectional Survey. BMJ Open 2017, 7, e015508. [Google Scholar] [CrossRef]
- Korir, E.; Okwara, F.N.; Okumbe, G. Menstrual Hygiene Management Practices among Primary School Girls from a Pastoralist Community in Kenya: A Cross Sectional Survey. Pan Afr. Med. J. 2018, 31. [Google Scholar] [CrossRef]
- Ellis, A.; Haver, J.; Villasenor, J.; Parawan, A.; Venkatesh, M.; Freeman, M.C.; Caruso, B.A. WASH Challenges to Girls’ Menstrual Hygiene Management in Metro Manila, Masbate, and South Central Mindanao, Philippines. Waterlines 2016, 35, 306–323. [Google Scholar] [CrossRef]
- Chothe, V.; Khubchandani, J.; Seabert, D.; Asalkar, M.; Rakshe, S.; Firke, A.; Midha, I.; Simmons, R. Students’ Perceptions and Doubts About Menstruation in Developing Countries: A Case Study From India. Health Promot. Pract. 2014, 15, 319–326. [Google Scholar] [CrossRef] [PubMed]
- Fakhri, M.; Hamzehgardeshi, Z.; Hajikhani Golchin, N.A.; Komili, A. Promoting Menstrual Health among Persian Adolescent Girls from Low Socioeconomic Backgrounds: A Quasi-Experimental Study. BMC Public Health 2012, 12. [Google Scholar] [CrossRef] [PubMed]
- Ajah, L.; Onubogu, E.; Anozie, O.; Lawani, L.; Iyoke, C.; Onwe, E.; Ajah, M. Adolescent Reproductive Health Challenges among Schoolgirls in Southeast Nigeria: Role of Knowledge of Menstrual Pattern and Contraceptive Adherence. Patient Prefer. Adherence 2015, 1219. [Google Scholar] [CrossRef] [PubMed]
- Adinma, E.D.; Adinma, J.I.B. Perceptions and Practices on Menstruation amongst Nigerian Secondary School Girls. Afr. J. Reprod. Health 2008, 12, 74–83. [Google Scholar]
- Gultie, T.; Hailu, D.; Workineh, Y. Age of Menarche and Knowledge about Menstrual Hygiene Management among Adolescent School Girls in Amhara Province, Ethiopia: Implication to Health Care Workers & School Teachers. PLoS ONE 2014, 9, e108644. [Google Scholar] [CrossRef]
- Sandhya, S.; Mondol, J.; Thapa, R.; Shrestha, A. A Study to Determine the Effectiveness of Planned Teaching Program on Adolescence Girl’s Knowledge, Attitude and Practices Towards Menstrual Hygiene in Selected Schools of Hemja, Kaski, Nepal. Int. J. Nurs. Educ. 2013, 5, 167. [Google Scholar] [CrossRef]
- Upashe, S.P.; Tekelab, T.; Mekonnen, J. Assessment of Knowledge and Practice of Menstrual Hygiene among High School Girls in Western Ethiopia. BMC Womens Health 2015, 15. [Google Scholar] [CrossRef] [PubMed]
- Miiro, G.; Rutakumwa, R.; Nakiyingi-Miiro, J.; Nakuya, K.; Musoke, S.; Namakula, J.; Francis, S.; Torondel, B.; Gibson, L.J.; Ross, D.A.; et al. Menstrual Health and School Absenteeism among Adolescent Girls in Uganda (MENISCUS): A Feasibility Study. BMC Womens Health 2018, 18. [Google Scholar] [CrossRef]
- Karkada, E.; Jatanna, S.; Abraham, S. Menstrual Beliefs and Practices among Adolescent Girls in Rural High Schools of South India. Int. J. Child Adolesc. Health 2012, 5, 317–323. [Google Scholar]
- Haque, S.E.; Rahman, M.; Itsuko, K.; Mutahara, M.; Sakisaka, K. The Effect of a School-Based Educational Intervention on Menstrual Health: An Intervention Study among Adolescent Girls in Bangladesh. BMJ Open 2014, 4, e004607. [Google Scholar] [CrossRef]
- Morrison, J.; Basnet, M.; Bhatt, A.; Khimbanjar, S.; Chaulagain, S.; Sah, N.; Baral, S.; Mahon, T.; Hodgkin, M. Girls’ Menstrual Management in Five Districts of Nepal: Implications for Policy and Practice. Stud. Soc. Justice 2018, 12, 251–272. [Google Scholar] [CrossRef]
- Girod, C.; Ellis, A.; Andes, K.L.; Freeman, M.C.; Caruso, B.A. Physical, Social, and Political Inequities Constraining Girls’ Menstrual Management at Schools in Informal Settlements of Nairobi, Kenya. J. Urban Health 2017, 94, 835–846. [Google Scholar] [CrossRef]
- Montgomery, P.; Hennegan, J.; Dolan, C.; Wu, M.; Steinfield, L.; Scott, L. Menstruation and the Cycle of Poverty: A Cluster Quasi-Randomised Control Trial of Sanitary Pad and Puberty Education Provision in Uganda. PLoS ONE 2016, 11, e0166122. [Google Scholar] [CrossRef] [PubMed]
- Hennegan, J.; Dolan, C.; Wu, M.; Scott, L.; Montgomery, P. Measuring the Prevalence and Impact of Poor Menstrual Hygiene Management: A Quantitative Survey of Schoolgirls in Rural Uganda. BMJ Open 2016, 6, e012596. [Google Scholar] [CrossRef] [PubMed]
- Rastogi, S.; Khanna, A.; Mathur, P. Uncovering the Challenges to Menstrual Health: Knowledge, Attitudes and Practices of Adolescent Girls in Government Schools of Delhi. Health Educ. J. 2019, 78, 839–850. [Google Scholar] [CrossRef]
- Blake, S.; Boone, M.; Yenew Kassa, A.; Sommer, M. Teaching Girls About Puberty and Menstrual Hygiene Management in Rural Ethiopia: Findings From a Pilot Evaluation. J. Adolesc. Res. 2018, 33, 623–646. [Google Scholar] [CrossRef]
- Su, J.; Lindell, D. Promoting the Menstrual Health of Adolescent Girls in China. Nurs. Health Sci. 2016, 18, 481–487. [Google Scholar] [CrossRef] [PubMed]
- Ortiz, M.I.; Rangel-Flores, E.; Carrillo-Alarcón, L.C.; Veras-Godoy, H.A. Prevalence and Impact of Primary Dysmenorrhea among Mexican High School Students. Int. J. Gynecol. Obstet. 2009, 107, 240–243. [Google Scholar] [CrossRef]
- Pitangui, A.G.; Gomes, M.R.A.; Lima, A.S.; Schwingel, P.A.; Albuquerque, A.P.S.; de Araújo, R.C. Menstruation Disturbances: Prevalence, Characteristics and Effects on the Activities of Daily Living among Adolescents Girls from Brazil. J. Pediatr. Adolesc. Gynecol. 2012, 26, 148–152. [Google Scholar] [CrossRef]
- Santina, T.; Wehbe, N.; Ziade, F. Exploring dysmenorrhoea and menstrual experiences among Lebanese female adolescents/Etude de la dysmenorrhee et du vecu des menstruations chez des adolescents libanaises. Rep. East. Mediterr. Health J. 2012, 18, 863. [Google Scholar]
- Davis, J.; Macintyre, A.; Odagiri, M.; Suriastini, W.; Cordova, A.; Huggett, C.; Faiqoh, P.A.A.; Budiyani, A.E.; Quillet, C.; Cronin, A.A.; et al. Menstrual Hygiene Management and School Absenteeism among Adolescent Students in Indonesia: Evidence from a Cross-Sectional School-Based Survey. Trop. Med. Int. Health 2018, 23, 1350–1363. [Google Scholar] [CrossRef]
- Chang, Y.-T.; Chen, Y.-C.; Hayter, M.; Lin, M.-L. Menstrual and Menarche Experience among Pubescent Female Students in Taiwan: Implications for Health Education and Promotion Practice. J. Clin. Nurs. 2009, 18, 2040–2048. [Google Scholar] [CrossRef]
- Wong, L.P. Premenstrual Syndrome and Dysmenorrhea: Urban-Rural and Multiethnic Differences in Perception, Impacts, and Treatment Seeking. J. Pediatr. Adolesc. Gynecol. 2011, 24, 272–277. [Google Scholar] [CrossRef] [PubMed]
- Agarwal, A.; Venkat, A. Questionnaire Study on Menstrual Disorders in Adolescent Girls in Singapore. J. Pediatr. Adolesc. Gynecol. 2009, 22, 365–371. [Google Scholar] [CrossRef]
- Abdelmoty, H.I.; Youssef, M.; Abdallah, S.; Abdel-Malak, K.; Hashish, N.M.; Samir, D.; Abdelbar, M.; Hosni, A.N.; Ghafar, M.A.-E.; Khamis, Y.; et al. Menstrual Patterns and Disorders among Secondary School Adolescents in Egypt. A Cross-Sectional Survey. BMC Womens Health 2015, 15. [Google Scholar] [CrossRef] [PubMed]
- Chan, S.; Yiu, K.; Yuen, P.; Sahota, D.; Chung, T. Menstrual problems and health-seeking behaviour in Hong Kong Chinese girls. Hong Kong Med. J. 2009, 15, 18–23. [Google Scholar] [PubMed]
- Wijesiri, H.S.M.S.; Suresh, T.S. Knowledge and Attitudes towards Dysmenorrhea among Adolescent Girls in an Urban School in Sri Lanka: Dysmenorrhea in Adolescence. Nurs. Health Sci. 2013, 15, 58–64. [Google Scholar] [CrossRef] [PubMed]
- Jeon, G.E.; Cha, N.H.; Sok, S.R. Factors Influencing the Dysmenorrhea among Korean Adolescents in Middle School. J. Phys. Ther. Sci. 2014, 26, 1337–1343. [Google Scholar] [CrossRef] [PubMed]
- Ambresin, A.-E.; Belanger, R.E.; Chamay, C.; Berchtold, A.; Narring, F. Body Dissatisfaction on Top of Depressive Mood among Adolescents with Severe Dysmenorrhea. J. Pediatr. Adolesc. Gynecol. 2012, 25, 19–22. [Google Scholar] [CrossRef]
- Bodén, E.; Wendel, C.; Adolfsson, A. Adolescents with Endometriosis: Their Experience of the School Health Care System in Sweden. Br. J. Sch. Nurs. 2013, 8, 81–87. [Google Scholar] [CrossRef]
- Kazama, M.; Maruyama, K.; Nakamura, K. Prevalence of Dysmenorrhea and Its Correlating Lifestyle Factors in Japanese Female Junior High School Students. Tohoku J. Exp. Med. 2015, 236, 107–113. [Google Scholar] [CrossRef] [PubMed]
- Suvitie, P.A.; Hallamaa, M.K.; Matomäki, J.M.; Mäkinen, J.I.; Perheentupa, A.H. Prevalence of Pain Symptoms Suggestive of Endometriosis Among Finnish Adolescent Girls (TEENMAPS Study). J. Pediatr. Adolesc. Gynecol. 2016, 29, 97–103. [Google Scholar] [CrossRef]
- Chang, Y.; Chen, Y. And Associated Factors Among Female Elementary Students in the Hualien Region. Menstrual. Health Care Behav. 2008, 16, 8–16. [Google Scholar] [CrossRef]
- Al-Matouq, S.; Al-Mutairi, H.; Al-Mutairi, O.; Abdulaziz, F.; Al-Basri, D.; Al-Enzi, M.; Al-Taiar, A. Dysmenorrhea among High-School Students and Its Associated Factors in Kuwait. BMC Pediatr. 2019, 19. [Google Scholar] [CrossRef]
- Mumtaz, Z.; Sivananthajothy, P.; Bhatti, A.; Sommer, M. “How Can We Leave the Traditions of Our Baab Daada” Socio-Cultural Structures and Values Driving Menstrual Hygiene Management Challenges in Schools in Pakistan. J. Adolesc. 2019, 76, 152–161. [Google Scholar] [CrossRef] [PubMed]
- McMahon, S.A.; Winch, P.J.; Caruso, B.A.; Obure, A.F.; Ogutu, E.A.; Ochari, I.A.; Rheingans, R.D. “The Girl with Her Period Is the One to Hang Her Head” Reflections on Menstrual Management among Schoolgirls in Rural Kenya. BMC Int. Health Hum. Rights 2011, 11. [Google Scholar] [CrossRef] [PubMed]
- Amatya, P.; Ghimire, S.; Callahan, K.E.; Baral, B.K.; Poudel, K.C. Practice and Lived Experience of Menstrual Exiles (Chhaupadi) among Adolescent Girls in Far-Western Nepal. PLoS ONE 2018, 13, e0208260. [Google Scholar] [CrossRef] [PubMed]
- Trinies, V.; Caruso, B.; Sogoré, A.; Toubkiss, J.; Freeman, M. Uncovering the Challenges to Menstrual Hygiene Management in Schools in Mali. Waterlines 2015, 34, 31–40. [Google Scholar] [CrossRef]
- Mason, L.; Nyothach, E.; Alexander, K.; Odhiambo, F.O.; Eleveld, A.; Vulule, J.; Rheingans, R.; Laserson, K.F.; Mohammed, A.; Phillips-Howard, P.A. ‘We Keep It Secret So No One Should Know’—A Qualitative Study to Explore Young Schoolgirls Attitudes and Experiences with Menstruation in Rural Western Kenya. PLoS ONE 2013, 8, e79132. [Google Scholar] [CrossRef] [PubMed]
- Rheinländer, T.; Gyapong, M.; Akpakli, D.E.; Konradsen, F. Secrets, Shame and Discipline: School Girls’ Experiences of Sanitation and Menstrual Hygiene Management in a Peri-Urban Community in Ghana. Health Care Women Int. 2019, 40, 13–32. [Google Scholar] [CrossRef] [PubMed]
- Janoowalla, H.; Keppler, H.; Asanti, D.; Xie, X.; Negassa, A.; Benfield, N.; Rulisa, S.; Nathan, L.M. The Impact of Menstrual Hygiene Management on Adolescent Health: The Effect of Go! Pads on Rate of Urinary Tract Infection in Adolescent Females in Kibogora, Rwanda. Int. J. Gynecol. Obstet. 2020, 148, 87–95. [Google Scholar] [CrossRef]
- Elledge, M.; Muralidharan, A.; Parker, A.; Ravndal, K.; Siddiqui, M.; Toolaram, A.; Woodward, K. Menstrual Hygiene Management and Waste Disposal in Low and Middle Income Countries-A. Rev. Lit. Int. J. Environ. Res. Public Health 2018, 15, 2562. [Google Scholar] [CrossRef] [PubMed]
- Sommer, M.; Chandraratna, S.; Cavill, S.; Mahon, T.; Phillips-Howard, P. Managing Menstruation in the Workplace: An Overlooked Issue in Low- and Middle-Income Countries. Int. J. Equity Health 2016, 15, 86. [Google Scholar] [CrossRef] [PubMed]
- Nielsen-Bohlman, L.; Panzer, A.; Kindig, D. Health Literacy: A Prescription to End Confusion; National Academies Press: Washington, DC, USA, 2004. [Google Scholar]
- South Australia Department of Education Menstrual Management. Available online: https://www.education.sa.gov.au/supporting-students/health-e-safety-and-wellbeing/health-support-planning/managing-health-education-and-care/personal-care/menstrual-management (accessed on 25 February 2019).
| Inadequate Hygiene Practices and School Infrastructure | Lack of Information | Pain |
|---|---|---|
| No access to sanitary napkins Use of alternate material instead of disposable napkins WASH issues No management help * | Source of information: mother, sister, friend etc. No management information in school * Skipped the reproductive biology chapter | Fatigue Headaches Not going to doctor Home remedies Normalization Dysmenorrhea Diagnosis of disorders |
| Cultural Taboos | Impact | Males |
| Menstrual blood is dirty Menstruating females are impure Restricted participation in daily activities Keep it a secret * Becoming a woman * | Absenteeism * Anxiety * Embarrassment * Discomfort * Depression * Shame * | Sexualizing menstruation Prefer female teachers Harassment by boys Male teacher issue Keep it a secret * Becoming a woman * |
| Menstrual Hygiene Management | Menstrual Health Issues | Attitudes Towards Menstruation |
|---|---|---|
| No access to sanitary napkins Use of alternate material instead of disposable napkins WASH issues No management information and help in school Source of information: mother, sister, friend etc. Skipped the reproductive biology chapter Absenteeism, anxiety, embarrassment and discomfort due to hygiene management issues | Fatigue Headaches Not going to doctor Home remedies Normalization Dysmenorrhea Diagnosis of disorders Absenteeism, discomfort and mental health issues due to menstrual health issues/disorders | Menstrual blood is dirty Menstruating females are impure Restricted participation in daily activities Keep it a secret Becoming a woman Sexualizing menstruation Prefer female teachers Harassment by boys Male teacher issue Absenteeism, anxiety, embarrassment, discomfort, depression and shame due to attitudes towards menstruation |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Holmes, K.; Curry, C.; Sherry; Ferfolja, T.; Parry, K.; Smith, C.; Hyman, M.; Armour, M. Adolescent Menstrual Health Literacy in Low, Middle and High-Income Countries: A Narrative Review. Int. J. Environ. Res. Public Health 2021, 18, 2260. https://doi.org/10.3390/ijerph18052260
Holmes K, Curry C, Sherry, Ferfolja T, Parry K, Smith C, Hyman M, Armour M. Adolescent Menstrual Health Literacy in Low, Middle and High-Income Countries: A Narrative Review. International Journal of Environmental Research and Public Health. 2021; 18(5):2260. https://doi.org/10.3390/ijerph18052260
Chicago/Turabian StyleHolmes, Kathryn, Christina Curry, Sherry, Tania Ferfolja, Kelly Parry, Caroline Smith, Mikayla Hyman, and Mike Armour. 2021. "Adolescent Menstrual Health Literacy in Low, Middle and High-Income Countries: A Narrative Review" International Journal of Environmental Research and Public Health 18, no. 5: 2260. https://doi.org/10.3390/ijerph18052260
APA StyleHolmes, K., Curry, C., Sherry, Ferfolja, T., Parry, K., Smith, C., Hyman, M., & Armour, M. (2021). Adolescent Menstrual Health Literacy in Low, Middle and High-Income Countries: A Narrative Review. International Journal of Environmental Research and Public Health, 18(5), 2260. https://doi.org/10.3390/ijerph18052260








