The Subjective Experience of Dyspareunia in Women with Endometriosis: A Systematic Review with Narrative Synthesis of Qualitative Research
Abstract
:1. Introduction
2. Aims of this Review
3. Materials and Methods
3.1. Quality Assessment
3.2. Data Extraction
3.3. Data Synthesis
4. Results
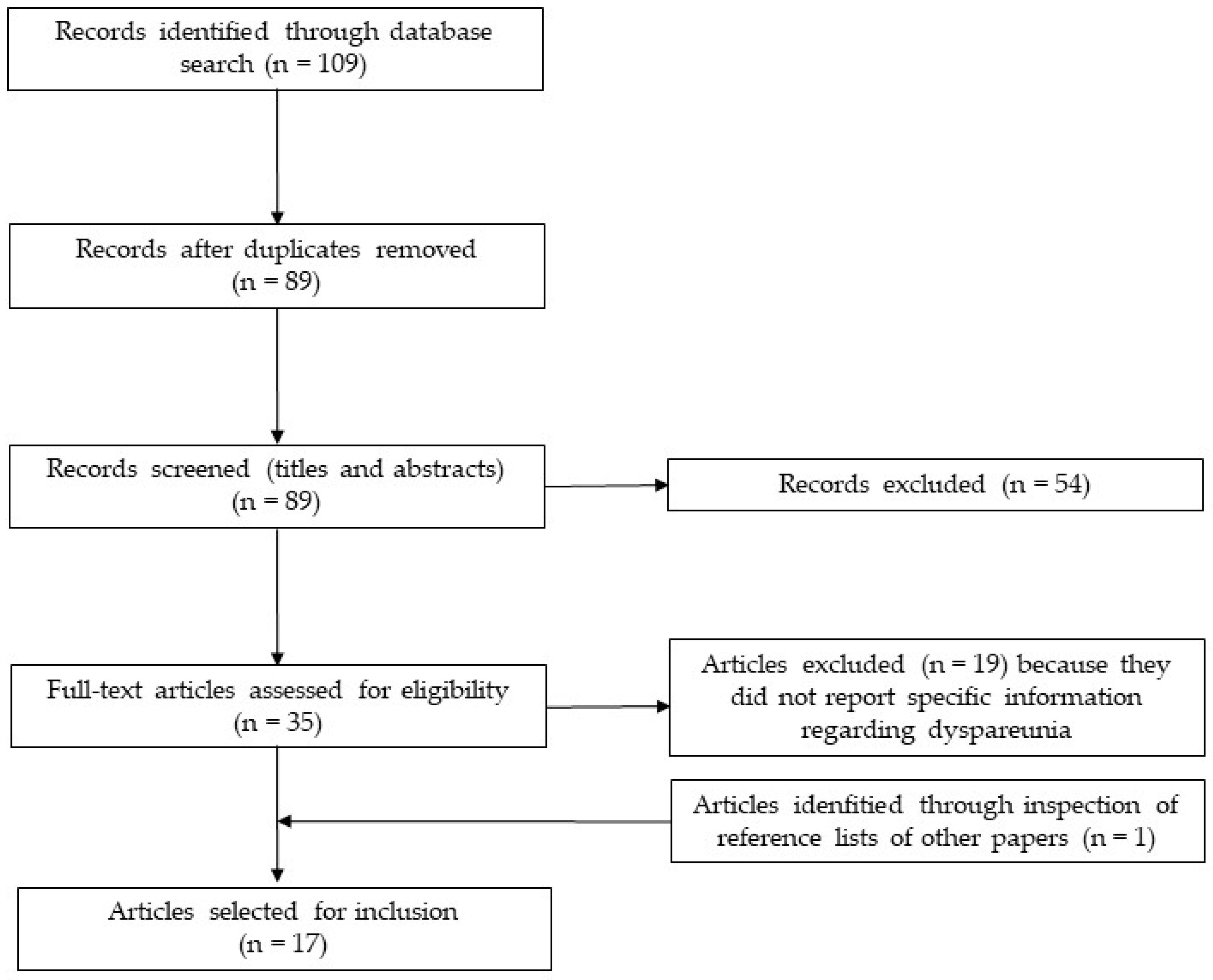
4.1. Description of the Included Studies
4.2. Narrative Synthesis
4.2.1. Women’s Perceptions of Dyspareunia
4.2.2. Coping Strategies
4.2.3. Psychological Impact
4.2.4. Impact on Intimate Relationships
4.2.5. Patient-Provider Communication
5. Discussion
Limitations and Suggestions for Future Research and Clinical Practice
6. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Schneider, M.P.; Vitonis, A.F.; Fadayomi, A.B.; Charlton, B.M.; Missmer, S.A.; DiVasta, A.D. Quality of life in adolescent and young adult women with dyspareunia and endometriosis. J. Adolesc. Health 2020, 67, 557–561. [Google Scholar] [CrossRef]
- van Poll, M.; van Barneveld, E.; Aerts, L.; Maas, J.W.; Lim, A.C.; de Greef, B.T.; Bongers, M.Y.; van Hanegem, N. Endometriosis and sexual quality of life. Sex. Med. 2020, 8, 532–544. [Google Scholar] [CrossRef]
- Acién, P.; Velasco, I. Endometriosis: A disease that remains enigmatic. ISRN Obstet. Gynecol. 2013, 2013, 242149. [Google Scholar] [CrossRef] [Green Version]
- Agarwal, S.K.; Chapron, C.; Giudice, L.C.; Laufer, M.R.; Leyland, N.; Missmer, S.A.; Singh, S.S.; Taylor, H.S. Clinical diagnosis of endometriosis: A call to action. Am. J. Obstet. Gynecol. 2019, 220, 354.e1. [Google Scholar] [CrossRef] [Green Version]
- Agarwal, S.K.; Soliman, A.M.; Pokrzywinski, R.M.; Snabes, M.C.; Coyne, K.S. Clinically meaningful reduction in dyspareunia is associated with significant improvements in health-related quality of life among women with moderate to severe pain associated with endometriosis: A pooled analysis of two phase III trials of Elagolix. J. Sex. Med. 2020, 17, 2427–2433. [Google Scholar] [CrossRef]
- Facchin, F.; Saita, E.; Barbara, G.; Dridi, D.; Vercellini, P. “Free butterflies will come out of these deep wounds”: A grounded theory of how endometriosis affects women’s psychological health. J. Health Psychol. 2018, 23, 538–549. [Google Scholar] [CrossRef]
- Soliman, A.M.; Coyne, K.S.; Zaiser, E.; Castelli-Haley, J.; Fuldeore, M.J. The burden of endometriosis symptoms on health-related quality of life in women in the United States: A cross-sectional study. J. Psychosom. Obstet. Gynecol. 2017, 38, 238–248. [Google Scholar] [CrossRef]
- Missmer, S.A.; Tu, F.F.; Agarwal, S.K.; Chapron, C.; Soliman, A.M.; Chiuve, S.; Eichner, S.; Flores-Caldera, I.; Horne, A.W.; Kimball, A.B.; et al. Impact of endometriosis on life-course potential: A narrative review. Int. J. Gen. Med. 2021, 14, 9–25. [Google Scholar] [CrossRef]
- Facchin, F.; Buggio, L.; Vercellini, P.; Frassineti, A.; Beltrami, S.; Saita, E. Quality of intimate relationships, dyadic coping, and psychological health in women with endometriosis: Results from an online survey. J. Psychosom. Res. 2021, 146, 110502. [Google Scholar] [CrossRef]
- Barbara, G.; Facchin, F.; Buggio, L.; Somigliana, E.; Berlanda, N.; Kustermann, A.; Vercellini, P. What is known and unknown about the association between endometriosis and sexual functioning: A systematic review of the literature. Reprod. Sci. 2017, 24, 1566–1576. [Google Scholar] [CrossRef]
- Bernays, V.; Schwartz, A.K.; Geraedts, K.; Rauchfuss, M.; Wölfler, M.M.; Haeberlin, F.; von Orelli, S.; Eberhard, M.; Imthurn, B.; Fink, D.; et al. Qualitative and quantitative aspects of sex life in the context of endometriosis: A multicentre case control study. Reprod. BioMed. Online 2020, 40, 296–304. [Google Scholar] [CrossRef] [PubMed]
- Shum, L.K.; Bedaiwy, M.A.; Allaire, C.; Williams, C.; Noga, H.; Albert, A.; Lisonkova, S.; Yong, P.J. Deep dyspareunia and sexual quality of life in women with endometriosis. Sex. Med. 2018, 6, 224–233. [Google Scholar] [CrossRef] [Green Version]
- Wahl, K.J.; Imtiaz, S.; Lisonek, M.; Joseph, K.S.; Smith, K.B.; Yong, P.J.; Cox, S.M. Dyspareunia in their own words: A qualitative description of endometriosis-associated sexual pain. Sex. Med. 2021, 9, 100274. [Google Scholar] [CrossRef]
- Seers, K. Qualitative systematic reviews: Their importance for our understanding of research relevant to pain. Br. J. Pain 2015, 9, 36–40. [Google Scholar] [CrossRef] [Green Version]
- Denny, E.; Khan, K.S. Systematic reviews of qualitative evidence: What are the experiences of women with endometriosis? J. Obstet. Gynaecol. 2006, 26, 501–506. [Google Scholar] [CrossRef]
- Tong, A.; Flemming, K.; McInnes, E.; Oliver, S.; Craig, J. Enhancing transparency in reporting the synthesis of qualitative research: ENTREQ. BMC Med. Res. Methodol. 2012, 12, 181. [Google Scholar] [CrossRef] [Green Version]
- Critical Appraisal Skills Programme (CASP). CASP Qualitative Research Checklist. Available online: http://media.wix.com/ugd/dded87_29c5b002d99342f788c6ac670e49f274.pdf (accessed on 25 October 2021).
- Gameiro, S.; Finnigan, A. Long-term adjustment to unmet parenthood goals following ART: A systematic review and meta-analysis. Hum. Reprod. Update 2017, 23, 322–337. [Google Scholar] [CrossRef] [Green Version]
- Dixon-Woods, M.; Agarwal, S.; Jones, D.; Young, B.; Sutton, A. Synthesising qualitative and quantitative evidence: A review of possible methods. J. Health Serv. Res. Policy 2005, 10, 45–53. [Google Scholar] [CrossRef]
- Young, K.; Fisher, J.; Kirkman, M. Women’s experiences of endometriosis: A systematic review and synthesis of qualitative research. J. Fam. Plann. Reprod. Health Care 2015, 41, 225–234. [Google Scholar] [CrossRef]
- Denny, E. Women’s experience of endometriosis. J. Adv. Nurs. 2004, 46, 641–648. [Google Scholar] [CrossRef]
- Riazi, H.; Tehranian, N.; Ziaei, S.; Mohammadi, E.; Hajizadeh, E.; Montazeri, A. Patients’ and physicians’ descriptions of occurrence and diagnosis of endometriosis: A qualitative study from Iran. BMC Women Health 2014, 14, 103. [Google Scholar] [CrossRef] [Green Version]
- Moradi, M.; Parker, M.; Sneddon, A.; Lopez, V.; Ellwood, D. Impact of endometriosis on women’s lives: A qualitative study. BMC Women Health 2014, 14, 123. [Google Scholar] [CrossRef] [Green Version]
- Seear, K. The etiquette of endometriosis: Stigmatisation, menstrual concealment and the diagnostic delay. Soc. Sci. Med. 2009, 69, 1220–1227. [Google Scholar] [CrossRef]
- Matías-González, Y.; Sánchez-Galarza, A.N.; Flores-Caldera, I.; Rivera-Segarra, E. “Es que tú eres una changa”: Stigma experiences among Latina women living with endometriosis. J. Psychosom. Obstet. Gynecol. 2021, 42, 67–74. [Google Scholar] [CrossRef] [PubMed]
- Hållstam, A.; Stålnacke, B.M.; Svensén, C.; Löfgren, M. Living with painful endometriosis—A struggle for coherence. A qualitative study. Sex. Reprod. Healthc. 2018, 17, 97–102. [Google Scholar] [CrossRef] [PubMed]
- Jones, G.; Jenkinson, C.; Kennedy, S. The impact of endometriosis upon quality of life: A qualitative analysis. J. Psychosom. Obstet. Gynecol. 2004, 25, 123–133. [Google Scholar] [CrossRef]
- Butt, F.S.; Chelsa, C. Health research chronic pelvic pain from endometriosis. Qual. Health Res. 2007, 17, 571–585. [Google Scholar] [CrossRef] [PubMed]
- Fauconnier, A.; Staraci, S.; Huchon, C.; Roman, H.; Panel, P.; Descamps, P. Comparison of patient- and physician-based descriptions of symptoms of endometriosis: A qualitative study. Hum. Reprod. 2013, 28, 2686–2694. [Google Scholar] [CrossRef] [Green Version]
- Rea, T.; Giampaolino, P.; Simeone, S.; Pucciarelli, G.; Alvaro, R.; Guillari, A. Living with endometriosis: A phenomenological study. Int. J. Qual. Stud. Health Well-Being 2020, 15, 1822621. [Google Scholar] [CrossRef]
- Denny, E.; Mann, C.H. Endometriosis-associated dyspareunia: The impact on women’s lives. J. Fam. Plann. Reprod. Health Care 2007, 33, 189–193. [Google Scholar] [CrossRef] [Green Version]
- Drabble, S.J.; Long, J.; Alele, B.; O’Cathain, A. Constellations of pain: A qualitative study of the complexity of women’s endometriosis-related pain. Br. J. Pain 2021, 15, 345–356. [Google Scholar] [CrossRef]
- Hudson, N.; Culley, L.; Law, C.; Mitchell, H.; Denny, E.; Raine-Fenning, N. ‘We needed to change the mission statement of the marriage’: Biographical disruptions, appraisals and revisions among couples living with endometriosis. Sociol. Health Illn. 2016, 38, 721–735. [Google Scholar] [CrossRef] [PubMed]
- Namazi, M.; Behboodi Moghadam, Z.; Zareiyan, A.; Jafarabadi, M. Exploring the impact of endometriosis on women’s lives: A qualitative study in Iran. Nurs. Open 2021, 8, 1275–1282. [Google Scholar] [CrossRef]
- Roomaney, R.; Kagee, A. Salient aspects of quality of life among women diagnosed with endometriosis: A qualitative study. J. Health Psychol. 2018, 23, 905–916. [Google Scholar] [CrossRef] [PubMed]
- Orr, N.; Wahl, K.; Joannou, A.; Hartmann, D.; Valle, L.; Yong, P.; Babb, C.; Kramer, C.W.; Kellogg-Spadt, S.; Renzelli-Cain, R.I. Deep dyspareunia: Review of pathophysiology and proposed future research priorities. Sex. Med. Rev. 2020, 8, 3–17. [Google Scholar] [CrossRef] [PubMed]
- Vercellini, P.; Somigliana, E.; Buggio, L.; Barbara, G.; Frattaruolo, M.P.; Fedele, L. “I can’t get no satisfaction”: Deep dyspareunia and sexual functioning in women with rectovaginal endometriosis. Fertil. Steril. 2012, 98, 1503–1511.e1. [Google Scholar] [CrossRef]
- Facchin, F.; Buggio, L.; Saita, E. Partners’ perspective in endometriosis research and treatment: A systematic review of qualitative and quantitative evidence. J. Psychosom. Res. 2020, 137, 110213. [Google Scholar] [CrossRef]
- Vercellini, P.; Meana, M.; Hummelshoj, L.; Somigliana, E.; Viganò, P.; Fedele, L. Priorities for endometriosis research: A proposed focus on deep dyspareunia. Reprod. Sci. 2011, 18, 114–118. [Google Scholar] [CrossRef]
- Fritzer, N.; Haas, D.; Oppelt, P.; Hornung, D.; Wölfler, M.; Ulrich, U.; Fischerlehner, G.; Sillem, M.; Hudelist, G. More than just bad sex: Sexual dysfunction and distress in patients with endometriosis. Eur. J. Obstet. Gynecol. Reprod. Biol. 2013, 169, 392–396. [Google Scholar] [CrossRef]
- Wahl, K.J.; Orr, N.L.; Lisonek, M.; Noga, H.; Bedaiwy, M.A.; Williams, C.; Allaire, C.; Albert, A.Y.; Smith, K.B.; Cox, S.; et al. Deep dyspareunia, superficial dyspareunia, and infertility concerns among women with endometriosis: A cross-sectional study. Sex. Med. 2020, 8, 274–281. [Google Scholar] [CrossRef] [Green Version]
- Witzeman, K.; Flores, O.A.; Renzelli-Cain, R.I.; Worly, B.; Moulder, J.K.; Carrillo, J.F.; Schneider, B. Patient–physician interactions regarding dyspareunia with endometriosis: Online survey results. J. Pain Res. 2020, 13, 1579–1589. [Google Scholar] [CrossRef] [PubMed]
| Article and Country | Aims | Participants | Women with Dyspareunia | Women’s Age Range | Type of Diagnosis | Data Collection | Data Analysis | Themes |
|---|---|---|---|---|---|---|---|---|
| Butt and Chesla, 2017 [28] (USA) | To examine the experience of couples living with endometriosis-related chronic pain | 13 heterosexual couples | Not reported | 23–48 years | Self-reported | In-depth individual and conjoint interviews | Thematic analysis; identification of exemplar and paradigm cases (interpretative phenomenology) | -Impact on intimate relationships -Patient-provider communication -Coping strategies |
| Denny, 2004 [21] (UK) | To investigate women’s experiences of living with endometriosis | 15 women | 12 women | 20–47 years | Surgical | Narratively oriented semi-structured interviews | Thematic analysis, content analysis | -Women’s perceptions of dyspareunia -Impact on intimate relationships -Patient-provider communication -Coping strategies |
| Denny and Mann, 2007 [31] (UK) | To explore the impact of dyspareunia on women’s lives | 30 women | 23 women (of 27 sexually active women) | 19–44 years | Surgical | Narratively oriented semi-structured interviews | Thematic analysis | -Women’s perceptions of dyspareunia -Psychological impact -Impact on intimate relationships -Coping strategies |
| Drabble et al., 2020 [32] (UK) | To investigate women’s experience of pain | 20 women | 14 women | 21–over 51 years | Surgical | Semi-structured interviews | Thematic analysis | -Women’s perceptions of dyspareunia -Impact on intimate relationships -Psychological impact |
| Facchin et al., 2018 [6] (Italy) | To explain how and why endometriosis affects women’s psychological health | 74 women | Not reported | 24–50 years | Surgical | Open interviews | Grounded theory | -Psychological impact -Impact on intimate relationships -Coping strategies |
| Fauconnier et al., 2013 [29] (France) | To examine the descriptions of endometriosis-related symptoms as provided by patients vs. physicians | 41 women | Up to 19 women raised themes related to dyspareunia | 21–45 years | Surgical and clinical | In-depth interviews | Thematic analysis (phenomenological approach) | -Women’s perceptions of dyspareunia -Coping strategies |
| Hållstam et al., 2018 [26] (Sweden) | To investigate women’s experience of painful endometriosis and its treatment | 13 women | Not reported | 24–48 years | ICD10 code of N 801, 803, 808, or 809 | Semi-structured interviews | Grounded theory | -Women’s perceptions of dyspareunia -Psychological impact -Impact on intimate relationship |
| Hudson et al., 2016 [33] (UK) | To explore biographical disruption in couples living with endometriosis | 22 heterosexual couples | 19 women | 25–50 years | Surgical | In-depth semi-structured interviews | Thematic analysis | -Psychological impact -Impact on intimate relationships |
| Jones et al., 2004 [27] (UK) | To investigate the impact of endometriosis on quality of life | 24 women | 18 women | 21.5–44 years | Surgical | In-depth interviews | Grounded theory | -Women’s perceptions of dyspareunia -Psychological impact -Coping strategies |
| Matías-González et al., 2020 [25] (Puerto Rico) | To investigate stigma experience in Latina women with endometriosis | 50 women | Not reported | >21 years | Surgical | Focus-group | Thematic analysis | -Impact on intimate relationships |
| Moradi et al., 2014 [23] (Australia) | To examine the impact of endometriosis on women’s lives, also comparing three age groups | 35 women | 25 women | 17–53 years | Surgical | Focus-group | Thematic analysis | -Women’s perceptions of dyspareunia -Psychological impact -Impact on intimate relationships -Coping strategies |
| Namazi et al., 2020 [34] (Iran) | To explore the impact of endometriosis among Iranian women | 20 women | Not reported | 23–43 years | Surgical | Semi-structured interviews | Content analysis | -Impact on intimate relationships |
| Rea et al., 2020 [30] (Italy) | To explore women’s lived experience of endometriosis | 25 women | Not reported | 18–54 years | Not reported | Open interviews | Cohen’s phenomenology | -Impact on intimate relationships -Psychological impact -Coping strategies |
| Riazi et al., 2014 [22] (Iran) | To explore patients’ and physicians’ experiences of occurrence and diagnosis of endometriosis | 12 women | Not reported | 22–37 years | Surgical | Semi-structured interviews | Content and thematic analysis | -Psychological impact -Women’s perceptions of dyspareunia |
| Roomaney and Kagee, 2018 [32] (South Africa) | To investigate health-related quality of life among women with endometriosis in South Africa | 25 women | Not reported | 25–42 years | Surgical | Semi-structured interviews | Thematic analysis | -Impact on intimate relationships -Psychological impact -Coping strategies |
| Seear, 2009 [24] (Australia) | To investigate stigmatizations, concealment of menstrual problems and diagnostic delay in women with endometriosis | 20 women | Not reported | 24–55 years | Not reported | Semi-structured interviews | Thematic analysis | -Impact on intimate relationships |
| Wahl et al., 2020 [13] (Canada) | To provide a qualitative description of women’s experience of endometriosis-related dyspareunia | 17 women | 17 women | 23–50 years | Clinically suspected or diagnosed endometriosis | Semi-structured interviews | Thematic analysis | -Women’s perceptions of dyspareunia -Psychological impact -Impact on intimate relationships -Coping strategies |
| Study | 1-Was There a Clear Statement of the Aims of the Research? | 2-Is a Qualitative Methodology Appropriate? | 3-Was the Research Design Appropriate to Address the Aims of the Research? | 4-Was the Recruitment Strategy Appropriate to the Aims of the Research? | 5-Was the Data Collected in a Way That Addressed the Research Issue? | 6-Has the Relationship between Researcher and Participants Been Adequately Considered? | 7-Have Ethical Issues Been Taken into Consideration? | 8-Was the Data Analysis Sufficiently Rigorous? | 9-Is there a Clear Statement of the Findings? | 10-How Valuable is the Research? | Total |
| Butt and Chesla, 2007 | Yes | Yes | Yes | Yes | Yes | No | No | Yes | Yes | Average | 7 (Moderate) |
| Denny, 2004 | Yes | Yes | Yes | Yes | Yes | No | Yes | No | Yes | Average | 7 (Moderate) |
| Denny and Mann, 2007 | Yes | Yes | Yes | Yes | Yes | No | Yes | No | Yes | High | 8 (High) |
| Drabble et al., 2020 | Yes | Yes | Yes | Yes | Yes | No | Yes | Yes | Yes | Average | 8 (High) |
| Facchin et al., 2018 | Yes | Yes | Yes | Yes | Yes | No | Yes | Yes | Yes | Average | 8 (High) |
| Fauconnier et al., 2013 | Yes | Yes | Yes | Yes | Yes | No | Yes | No | Yes | High | 8 (High) |
| Hållstam et al., 2018 | Yes | Yes | Yes | Yes | Yes | No | Yes | No | Yes | Average | 7 (Moderate) |
| Hudson et al., 2016 | Yes | Yes | Yes | Yes | Yes | No | Yes | Yes | Yes | Average | 8 (High) |
| Jones et al., 2004 | Yes | Yes | Yes | Yes | Yes | No | Yes | Yes | Yes | Average | 8 (High) |
| Matias-Gonzalez et al., 2020 | Yes | Yes | Yes | Yes | Yes | No | Yes | No | Yes | Average | 7 (Moderate) |
| Moradi et al., 2014 | Yes | Yes | Yes | Yes | Yes | No | Yes | Yes | Yes | Average | 8 (High) |
| Namazi et al., 2020 | Yes | Yes | Yes | Yes | Yes | No | Yes | Yes | Yes | Average | 8 (High) |
| Rea et al., 2020 | Yes | Yes | Yes | Yes | Yes | No | Yes | Yes | Yes | Average | 8 (High) |
| Riazi et al., 2014 | Yes | Yes | Yes | Yes | Yes | No | Yes | No | Yes | Average | 7 (Moderate) |
| Roomaney and Kagee, 2018 | Yes | Yes | Yes | Yes | Yes | No | Yes | Yes | Yes | Average | 8 (High) |
| Seear, 2009 | No | Yes | Yes | Yes | Yes | No | Yes | Yes | Yes | Average | 7 (Moderate) |
| Wahl et al., 2021 | Yes | Yes | Yes | Yes | Yes | No | Yes | Yes | Yes | High | 9 (High) |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Facchin, F.; Buggio, L.; Dridi, D.; Barbara, G.; Vercellini, P. The Subjective Experience of Dyspareunia in Women with Endometriosis: A Systematic Review with Narrative Synthesis of Qualitative Research. Int. J. Environ. Res. Public Health 2021, 18, 12112. https://doi.org/10.3390/ijerph182212112
Facchin F, Buggio L, Dridi D, Barbara G, Vercellini P. The Subjective Experience of Dyspareunia in Women with Endometriosis: A Systematic Review with Narrative Synthesis of Qualitative Research. International Journal of Environmental Research and Public Health. 2021; 18(22):12112. https://doi.org/10.3390/ijerph182212112
Chicago/Turabian StyleFacchin, Federica, Laura Buggio, Dhouha Dridi, Giussy Barbara, and Paolo Vercellini. 2021. "The Subjective Experience of Dyspareunia in Women with Endometriosis: A Systematic Review with Narrative Synthesis of Qualitative Research" International Journal of Environmental Research and Public Health 18, no. 22: 12112. https://doi.org/10.3390/ijerph182212112
APA StyleFacchin, F., Buggio, L., Dridi, D., Barbara, G., & Vercellini, P. (2021). The Subjective Experience of Dyspareunia in Women with Endometriosis: A Systematic Review with Narrative Synthesis of Qualitative Research. International Journal of Environmental Research and Public Health, 18(22), 12112. https://doi.org/10.3390/ijerph182212112







