Psychological Morbidity in Endometriosis: A Couple’s Study
Abstract
1. Introduction
2. Materials and Methods
2.1. Participants
2.2. Instruments
2.3. Procedure
2.4. Data Analysis
3. Results
3.1. The Indirect Effect of Infertility and Frequency of Sexual Activity on Women’s Psychological Morbidity—Path Analysis
3.2. Multigoup Analysis
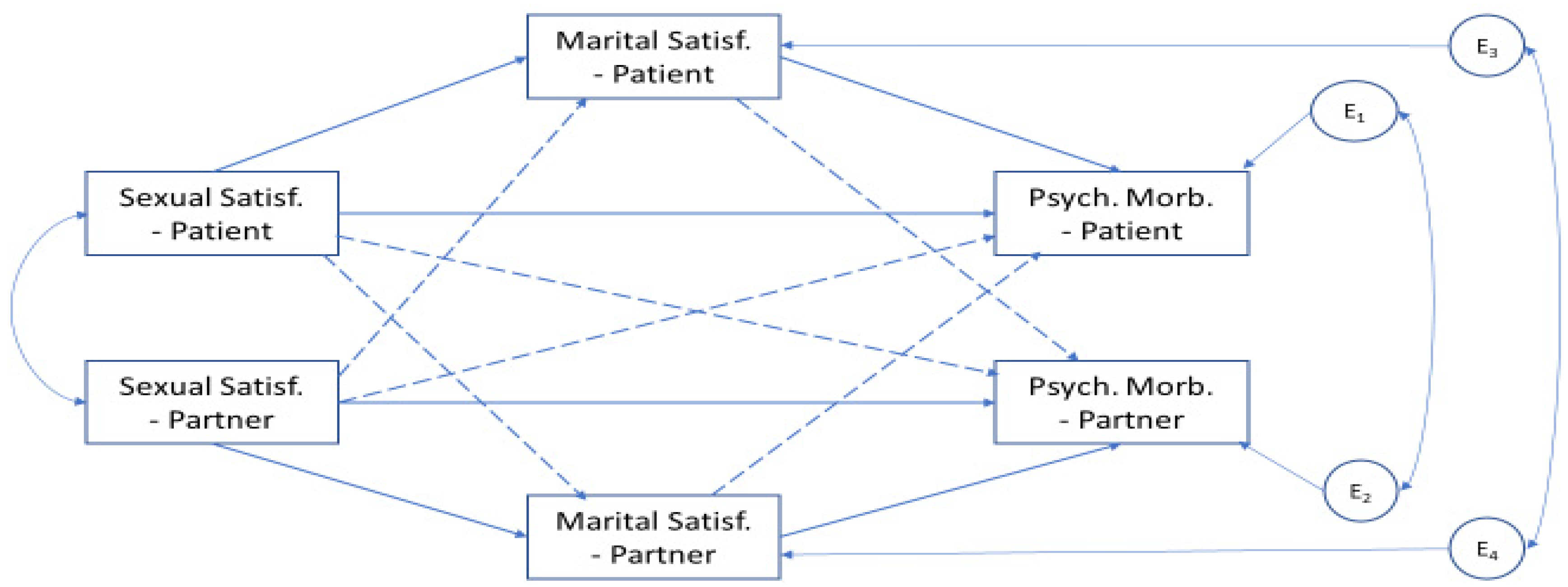
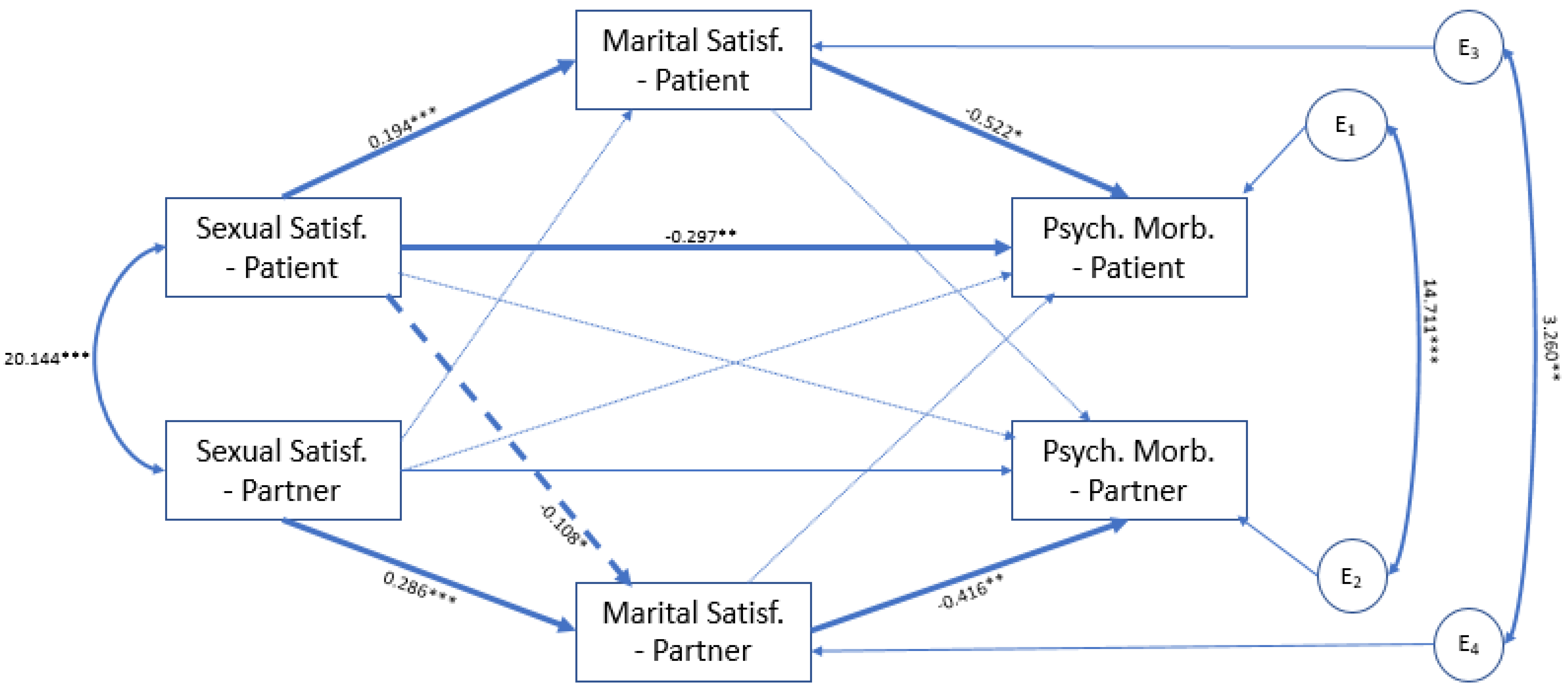
3.3. Direct and Indirect Effects in the Actor–Partner Interdependence Mediation Model (APIMeM)
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- de Marqui, A.B.T.; Silva, M.P.C.; Irie, G.R. Disfunção sexual em endometriosis: Uma revisão sistemática. [Sexual dysfunction in endometriosis: A systematic review]. Medicina (Ribeirão PretoOnline) 2015, 48, 478–490. [Google Scholar] [CrossRef][Green Version]
- Makiyan, Z. Endometriosis origin of primordial germ cells. Organogenesis 2017, 13, 95–102. [Google Scholar] [CrossRef]
- Wang, Y.; Nicholes, K.; Shih, I.M. The origin and pathogenesis of endometriosis. Annu Rev. Pathol 2020, 15, 71–95. [Google Scholar] [CrossRef] [PubMed]
- Giudice, L.C. Endometriosis. N. Engl. J. Med. 2010, 362, 2389–2398. [Google Scholar] [CrossRef] [PubMed]
- Adamson, G.D.; Kennedy, S.; Hummelshoj, L. Creating Solutions in Endometriosis: Global Collaboration through the World Endometriosis Research Foundation. J. Endometr. 2010, 2, 3–6. [Google Scholar] [CrossRef]
- de Marqui, A.B.T. Endometriosis: Do diagnóstico ao tratamento [Endometriosis from the diagnosis to the treatment]. Rev. De Enferm. E Atenção À Saúde 2016, 3, 97–105. [Google Scholar] [CrossRef]
- Hospital DA luz. Endometriose: Sintomas, Diagnóstico e Tratamentos. Available online: https://www.hospitaldaluz.pt/pt/guia-de-saude/dicionario-de-saude/E/109/endometriose-sintomas-tratamentos (accessed on 27 July 2021).
- Stratton, P.; Berkley, K.J. Chronic pelvic pain and endometriosis: Translational evidence of the relationship and implications. Hum. Reprod Update 2011, 17, 327–346. [Google Scholar] [CrossRef] [PubMed]
- Staal, A.H.J.; Van Der Zanden, M.; Nap, A.W. Diagnostic delay of endometriosis in the Netherlands. Gynecol. Obs. Investig. 2016, 81, 321–324. [Google Scholar] [CrossRef] [PubMed]
- Golfier, F.; Chanavaz-Lacheray, I.; Descamps, P.; Agostini, A.; Poilblanc, M.; Rousset, P.; Bolze, P.A.; Panel, P.; Collinet, P.; Hebert, T.; et al. The definition of Endometriosis Expert Centres. J. Gynecol Obs. Hum. Reprod 2018, 47, 179–181. [Google Scholar] [CrossRef] [PubMed]
- Revised American Society for Reproductive Medicine classification of endometriosis: 1996. Fertil Steril. 1997, 67, 817–821. [CrossRef]
- Haas, D.; Shebl, O.; Shamiyeh, A.; Oppelt, P. The rASRM score and the Enzian classification for endometriosis: Their strengths and weaknesses. Acta Obs. Gynecol. Scand. 2013, 92, 3–7. [Google Scholar] [CrossRef]
- Agarwal, S.K.; Chapron, C.; Giudice, L.C.; Laufer, M.R.; Leyland, N.; Missmer, S.A.; Singh, S.S.; Taylor, H.S. Clinical diagnosis of endometriosis: A call to action. Am. J. Abs. Gynecol 2019, 220, 354.e1–354.e12. [Google Scholar] [CrossRef]
- Porto, B.T.C.; Ribeiro, H.S.A.A.; Galvão, M.A.L.; Sekula, V.G.; Aldrigui, J.M.; Ribeiro, P.A.A. Classificação histológica e QV em mulheres portadoras de endometriose. Rev. Bras. Ginecol. Obs. 2015, 37, 87–93. [Google Scholar] [CrossRef]
- Van den Broeck, U.; Meuleman, C.; Tomassetti, C.; D’Hoore, A.; Wolthuis, A.; Van Cleynenbreugel, B.; Vergote, I.; Enzlin, P.; D’Hooghe, T. Effect of laparoscopic surgery for moderate and severe endometriosis on depression, relationship satisfaction and sexual functioning: Comparison of patients with and without bowel resection. Hum. Reprod. 2013, 28, 2389–2397. [Google Scholar] [CrossRef] [PubMed]
- Friedl, F.; Riedl, D.; Fessler, S.; Wildt, L.; Walter, M.; Richter, R.; Schüßler, G.; Böttcher, B. Impact of endometriosis on quality of life, anxiety, and depression: An Austrian perspective. Arch. Obstet. Gynaecol. 2015, 292, 1393–1399. [Google Scholar] [CrossRef] [PubMed]
- Laganà, A.S.; Condemi, I.; Retto, G.; Muscatello, M.R.A.; Bruno, A.; Zoccali, R.A.; Triolo, O.; Cedro, C. Analysis of psychopathological comorbidity behind the common symptoms and signs of endometriosis. EUR J. Abs. Gynecol. Reprod. Biol. 2015, 194, 30–33. [Google Scholar] [CrossRef] [PubMed]
- Laganà, A.S.; La Rosa, V.L.; Rapisarda, A.M.C.; Valenti, G.; Sapia, F.; Chiofalo, B.; Rosseti, D.; Frangez, H.B.; Bokal, E.V.; Vitale, S.G. Anxiety and depression in patients with endometriosis: Impact and management challenges. Int. J. Women’s Health 2017, 9, 323–330. [Google Scholar] [CrossRef] [PubMed]
- van Barneveld, E.; Manders, J.; van Osch, F.H.; van Poll, M.; Visser, L.; van Hanegem, N.; Lim, A.C.; Bongers, M.Y.; Leue, C. Depression, Anxiety, and Correlating Factors in Endometriosis: A Systematic Review and Meta-Analysis. J. Women’s Health 2021. [Google Scholar] [CrossRef] [PubMed]
- Gao, M.; Koupil, I.; Sjöqvist, H.; Karlsson, H.; Lalitkumar, S.; Dalman, C.; Kosidou, K. Psychiatric comorbidity among women with endometriosis: Nationwide cohort study in Sweden. Am J. Obstet. Gynecol. 2020, 223, 415.e1–415.e16. [Google Scholar] [CrossRef]
- Facchin, F.; Barbara, G.; Saita, E.; Mosconi, P.; Roberto, A.; Fedele, L.; Vercellini, P. Impact of endometriosis on quality of life and mental health: Pelvic pain makes the difference. J. Psychosom. Obs. Gynaecol. 2015, 36, 135–141. [Google Scholar] [CrossRef]
- Martins, J.; Ferreira, G.; Vilaça, M.; Ferreira, H.; Osório, F.; Nogueira-Silva, C.; Pereira, M.G. Quality of life and sexual satisfaction in women with endometriosis: The moderator role in symptom severity. Psychol. Sex. 2021. [Google Scholar] [CrossRef]
- Ameratunga, D.; Flemming, T.; Angstetra, D.; Ng, S.K.; Sneddon, A. Exploring the impact of endometriosis on partners. J. Obstet. Gynaecol. Res. 2017, 43, 1048–1053. [Google Scholar] [CrossRef]
- Aerts, L.; Grangier, L.; Streuli, I.; Dällenbach, P.; Marci, R.; Wenger, J.M.; Pluchino, N. Psychosocial impact of endometriosis: From co-morbidity to intervention. Best Pract. Res. Clin. Obstet. Gynaecol. 2018, 50, 2–10. [Google Scholar] [CrossRef]
- Culley, L.; Law, C.; Hudson, N.; Mitchell, H.; Denny, E.; Raine-Fenning, N. A qualitative study of the impact of endometriosis on male partners. Hum. Reprod. 2017, 32, 1667–1673. [Google Scholar] [CrossRef]
- Norinho, P.; Martins, M.M.; Ferreira, H. A systematic review on the effects of endometriosis on sexuality and couple’s relationship. Facts Views Vis. Obgyn. 2020, 12, 197–205. [Google Scholar]
- Hammerli, S.; Kohl Schwartz, A.S.; Geraedtz, K.; Imesch, P.; Rauchfuss, M.; Wölfler, M.M.; Haeberlin, F.; von Orelli, S.; Eberhard, M.; Imthurn, B.; et al. Does endometriosis affect sexual activity and satisfaction of the male partner? A comparison of partners from women diagnosed with endometriosis and controls. J. Sex. Med. 2018, 15, 853–865. [Google Scholar] [CrossRef] [PubMed]
- Moradi, M.; Parker, M.; Sneddon, A.; Lopez, V.; Ellwood, D. Impact of endometriosis on women’s lives: A qualitative study. BMC Women’s Health 2014, 14, 1–12. [Google Scholar] [CrossRef] [PubMed]
- Pluchino, N.; Wenger, J.M.; Petignat, P.; Tal, R.; Bolmont, M.; Taylor, H.S.; Bianchi-Demicheli, F. Sexual function in endometriosis patients and their partners: Effect of the disease and consequences of treatment. Hum. Reprod. Update 2016, 22, 762–774. [Google Scholar] [CrossRef] [PubMed]
- De Graaff, A.A.; D’hooghe, T.M.; Dunselman, G.A.J.; Dirksen, C.D.; Hummelshoj, L.; WERF EndoCost Consortium; Simoens, S.; Bokor, A.; Brandes, I.; Brodszky, V.; et al. The significant effect of endometriosis on physical, mental and social wellbeing: Results from an international cross-sectional survey. Hum. Reprod. 2013, 28, 2677–2685. [Google Scholar] [CrossRef]
- Camara, C.; Vos, M.C.; de Rooij, B.H.; Pijnenborg, J.M.; Boll, D.; van de Poll-Franse, L.V.; Ezendam, N.P. The role of positive psychological changes in anxiety and depression of patients with ovarian tumors and their partners: An observational study of the population-based PROFILES registry. Support. Care Cancer 2019, 27, 423–431. [Google Scholar] [CrossRef]
- Chien, C.H.; Chuang, C.K.; Liu, K.L.; Wu, C.T.; Pang, S.T.; Tsay, P.K.; Change, Y.H.; Huang, X.Y.; Liu, H.E. Effects of individual and partner factors in anxiety and depression in Taiwanese prostate cancer patients: A longitudinal study. Eur. J. Cancer Care 2018, 27, e12753. [Google Scholar] [CrossRef]
- Trudel, G.; Goldfarb, M.R. Marital and sexual functioning and dysfunctioning, depression and anxiety. Sexologies 2010, 19, 137–142. [Google Scholar] [CrossRef]
- van Poll, M.; van Barneveld, E.; Aerts, L.; Maas, J.W.; Lim, A.C.; de Greef, B.T.; Bongers, M.Y.; van Hanegem, N. Endometriosis and Sexual Quality of Life. Sex. Med. 2020, 8, 532–544. [Google Scholar] [CrossRef] [PubMed]
- Tripoli, T.M.; Sato, H.; Sartori, M.G.; de Araujo, F.F.; Girão, M.J.; Schor, E. Evaluation of quality of life and sexual satisfaction in women suffering from chronic pelvic pain with or without endometriosis. J. Sex. Med. 2011, 8, 497–503. [Google Scholar] [CrossRef] [PubMed]
- Smith, K.B.; Pukall, C.F. Sexual function, relationship adjustment, and the relational impact of pain in male partners of women with provoked vulvar pain. J. Sex. Med. 2014, 11, 1283–1293. [Google Scholar] [CrossRef]
- Muise, A.; Giang, E.; Impett, E.A. Post sex affectionate exchanges promote sexual and relationship satisfaction. Arch. Sex. Behav. 2014, 43, 1391–1402. [Google Scholar] [CrossRef]
- Rosen, N.O.; Muise, A.; Bergeron, S.; Delisle, I.; Baxter, M.L. Daily associations between partner responses and sexual and relationship satisfaction in couples coping with provoked vestibulodynia. J. Sex. Med. 2015, 12, 1028–1039. [Google Scholar] [CrossRef]
- Verit, F.F.; Verit, A.; Yeni, E. The prevalence of sexual dysfunction and associated risk factors in women with chronic pelvic pain: A cross-sectional study. Arch. Abs. Gynaecol. 2006, 274, 297–302. [Google Scholar] [CrossRef]
- Fernandez, I.; Reid, C.; Dziurawiec, S. Living with endometriosis: The perspective of male partners. J. Psychosom Res. 2006, 61, 433–438. [Google Scholar] [CrossRef]
- Northouse, L.L.; Mood, D.; Templin, T.; Mellon, S.; George, T. Couples’ patterns of adjustment to colon cancer. Soc. Sci. Med. 2000, 50, 271–284. [Google Scholar] [CrossRef]
- Centini, G.; Lazzeri, L.; Dores, D.; Pianigiani, L.; Lannone, P.; Luisi, S.; Petraglia, F.; Zupi, E. Chronic pelvic pain and quality of life in women with and without endometriosis. J. Endometrial. Pelvic Pain Disord. 2013, 5, 27–33. [Google Scholar] [CrossRef]
- Zigmond, A.S.; Snaith, R.P. The hospital anxiety and depression scale. Acta Psychiatr. Scand 1983, 67, 361–370. [Google Scholar] [CrossRef] [PubMed]
- Sousa, C.; Pereira, M.G. Morbilidade psicológica e representações da doença em pacientes com esclorese múltipla: Estudo de validação da Hospital Anxiety and Depression Scale (HADS). Psicol. Saúde Doenças 2008, 9, 283–298. [Google Scholar]
- Funk, J.L.; Rogge, R.D. Testing the ruler with item response theory: Increasing precision of measurement for relationship satisfaction with the Couples Satisfaction Index. J. Fam. Psychol. 2007, 21, 572–583. [Google Scholar] [CrossRef]
- Ferraz, A.S.; Santos, M.; Ribeiro, I.; Pereira, M.G. Validation of Portuguese version of the couples satisfaction index in women with endometriosis and their partners. Sex. Relation. Ther. 2021. Submitted manuscript. [Google Scholar]
- Lawrance, K.-A.; Byers, E.S. Sexual satisfaction in long-term heterosexual relationships: The interpersonal exchange model of sexual satisfaction. Pears. Relatsh. 1995, 2, 267–285. [Google Scholar] [CrossRef]
- Pascoal, P.M.; Narciso, I.D.S.B.; Pereira, N.M.; Ferreira, A.S. Processo de validação da Global Measure of Sexual Satisfaction em três amostras da população portuguesa. Psicol. Reflexão E Crítica 2013, 26, 691–700. [Google Scholar] [CrossRef][Green Version]
- Brown, T. Confirmatory Factor Analysis for Applied Research; Guilford Press: New York, NY, USA, 2006. [Google Scholar]
- Ledermann, T.; Macho, S.; Kenny, D.A. Assessing mediation in dyadic data using the actor-partner interdependence model. Struct. Equ. Model. 2011, 18, 595–612. [Google Scholar] [CrossRef]
- Cook, W.; Kenny, D.A. The actor-partner interdependence model: A model of bidirectional effects in developmental studies. Int. J. Behav. Dev. 2005, 29, 101–109. [Google Scholar] [CrossRef]
- Schweizer, K. Some guidelines concerning the modeling of traits and abilities in test construction. EUR J. Psychol. Assess. 2010, 26, 1–2. [Google Scholar] [CrossRef]
- Hayes, A. Introduction to Mediation, Moderation, and Conditional Process Analysis: A Regression-Based Approach; Guilford Press: New York, NY, USA, 2013. [Google Scholar]
- Roomaney, R.; cage, A. Salient aspects of quality of life among women diagnosed with endometriosis: A qualitative study. J. Health Psychol. 2018, 23, 905–916. [Google Scholar] [CrossRef]
- Knowles, S.R.; Austin, D.W.; Sivanesan, S.; Tye-Din, J.; Leung, C.; Wilson, J.; Castle, D.; Kamm, M.A.; Macrae, F.; Hebbard, G. Relations between symptom severity, illness perceptions, visceral sensitivity, coping strategies and well-being in irritable bowel syndrome guided by the common sense model of illness. Psychol. Health Med. 2017, 22, 524–534. [Google Scholar] [CrossRef] [PubMed]
- Knowles, S.R.; Castle, D.J.; Biscan, S.M.; Salzberg, M.; O’Flaherty, E.B.; Langham, R. Relationships between illness perceptions, coping and psychological morbidity in kidney transplant patients. Am. J. Med. Sci. 2016, 351, 233–238. [Google Scholar] [CrossRef] [PubMed]
- De Graaff, A.A.; Van Lankveld, J.; Smits, L.J.; Van Beek, J.J.; Dunselman, G.A.J. Dyspareunia and depressive symptoms are associated with impaired sexual functioning in women with endometriosis, whereas sexual functioning in their male partners is not affected. Hum. Reprod. 2016, 31, 2577–2586. [Google Scholar] [CrossRef] [PubMed]

| Sociodemographic Characterization | N (%) | Mean (SD) | Minimum | Maximum |
|---|---|---|---|---|
| Age | 105 | 36.08 (6.11) | 23 | 51 |
| Years of Education | 105 | 14.52 (3.46) | 6 | 21 |
| Frequency of sexual activity/month | 105 | 6.63 (5.59) | 0 | 30 |
| Duration of the relationship | 105 | 11.26 (6.65) | 1 | 29 |
| Nationality | ||||
| Portuguese | 103 (98.1) | |||
| Brazilian | 2 (1.9) | |||
| Marital Status | ||||
| Married/Cohabiting | 88 (83.8) | |||
| Single | 11 (10.5) | |||
| Divorced | 6 (5.7) | |||
| Professional Status | ||||
| Actively employed | 61 (93.8) | |||
| Unemployed | 3 (4.6) | |||
| Retired | 1 (1.5) | |||
| Absence from work | 78 (74.3) | |||
| Clinical Characterization | ||||
| Dysmenorrhea intensity | 105 | 5.10 (4.11) | 0 | 10 |
| Dysuria intensity | 105 | 0.85 (2.34) | 0 | 10 |
| Dyschezia intensity | 105 | 2.51 (3.67) | 0 | 10 |
| Dyspareunia intensity | 105 | 3.90 (3.84) | 0 | 10 |
| Chronic pelvic pain intensity | 105 | 2.81 (3.37) | 0 | 10 |
| Duration of diagnosis (months) | 105 | 60.00(60.53) | 2 | 360 |
| Having Surgery | 75 (71.4) | 33.37 (37.66) | ||
| Infertility | 37.1(37.1) | |||
| Perception of Symptom Severity | ||||
| Light | 19 (18.4) | |||
| Moderate | 38 (36.9) | |||
| Severe | 46 (44.7) | |||
| Stage of disease | ||||
| I | 1 (1.0) | |||
| II | 13 (12.4) | |||
| III | 29 (27.6) | |||
| IV | 62 (59.0) |
| Sociodemographic Characterization | N (%) | Mean (SD) | Minimum | Maximum |
|---|---|---|---|---|
| Age | 105 | 37.73 (7.43) | 20 | 59 |
| Years of Education | 105 | 12.81 (3.62) | 4 | 22 |
| Nationality | ||||
| Portuguese | 103 (98.1) | |||
| Brazilian | 2 (1.9) | |||
| Professional Status | ||||
| Actively employed | 101 (96.2) | |||
| Unemployed | 4 (3.8) |
| Predictor | Indirect Effect | Outcome | β | SE | 95% CI | p | |
|---|---|---|---|---|---|---|---|
| LL | UL | ||||||
| Sexual Satisfaction | Sexual Activity | Psychological Morbidity | −0.083 | 0.028 | −0.142 | −0.029 | 0.002 |
| Diagnosis Duration | Infertility | Psychological Morbidity | −0.062 | 0.032 | −0.139 | −0.015 | 0.009 |
| 1 | 2 | 3 | 4 | 5 | 6 | |
|---|---|---|---|---|---|---|
| 1. Sexual Satisfaction—Women | --- | |||||
| 2. Sexual Satisfaction—Sexual Partner | 0.431 *** | --- | ||||
| 3. Marital Satisfaction—Women | 0.390 *** | 0.262 ** | --- | |||
| 4. Marital Satisfaction—Sexual Partner | 0.007 | 0.453 *** | 0.306 ** | --- | ||
| 5. Psychological Morbidity—Women | −0.365 *** | −0.270 ** | −0.357 *** | -023 | --- | |
| 6. Psychological Morbidity—Sexual Partner | −0.072 | −0.233 * | −0.187 | −0.242 * | 0.354 *** | --- |
| Mean | 27.83 | 27.41 | 15.76 | 15.44 | 15.04 | 10.38 |
| SD | 7.23 | 6.53 | 3.59 | 3.61 | 8.42 | 5.77 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Pereira, M.G.; Ribeiro, I.; Ferreira, H.; Osório, F.; Nogueira-Silva, C.; Almeida, A.C. Psychological Morbidity in Endometriosis: A Couple’s Study. Int. J. Environ. Res. Public Health 2021, 18, 10598. https://doi.org/10.3390/ijerph182010598
Pereira MG, Ribeiro I, Ferreira H, Osório F, Nogueira-Silva C, Almeida AC. Psychological Morbidity in Endometriosis: A Couple’s Study. International Journal of Environmental Research and Public Health. 2021; 18(20):10598. https://doi.org/10.3390/ijerph182010598
Chicago/Turabian StylePereira, Maria Graça, Inês Ribeiro, Hélder Ferreira, Filipa Osório, Cristina Nogueira-Silva, and Ana C. Almeida. 2021. "Psychological Morbidity in Endometriosis: A Couple’s Study" International Journal of Environmental Research and Public Health 18, no. 20: 10598. https://doi.org/10.3390/ijerph182010598
APA StylePereira, M. G., Ribeiro, I., Ferreira, H., Osório, F., Nogueira-Silva, C., & Almeida, A. C. (2021). Psychological Morbidity in Endometriosis: A Couple’s Study. International Journal of Environmental Research and Public Health, 18(20), 10598. https://doi.org/10.3390/ijerph182010598






