Effects of Meditation on Mental Health and Cardiovascular Balance in Caregivers
Abstract
1. Introduction
2. Materials and Methods
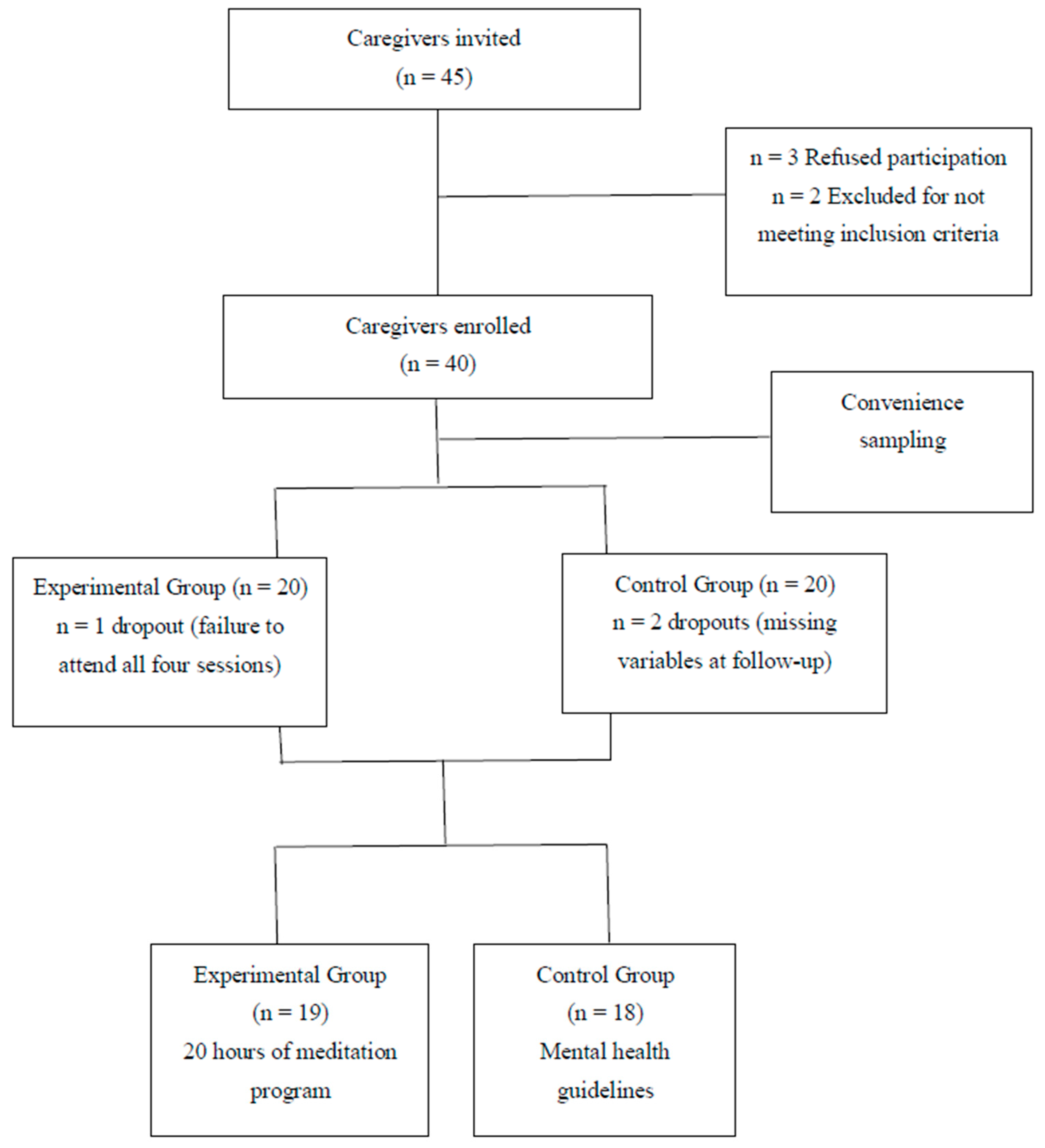
2.1. Study Design
2.2. Setting and Selection of Participants
2.3. Control Group
2.4. Experimental Group
2.5. Meditation Training Program
Sample Size Calculation
2.6. Outcome Measures
2.7. Statistical Analysis
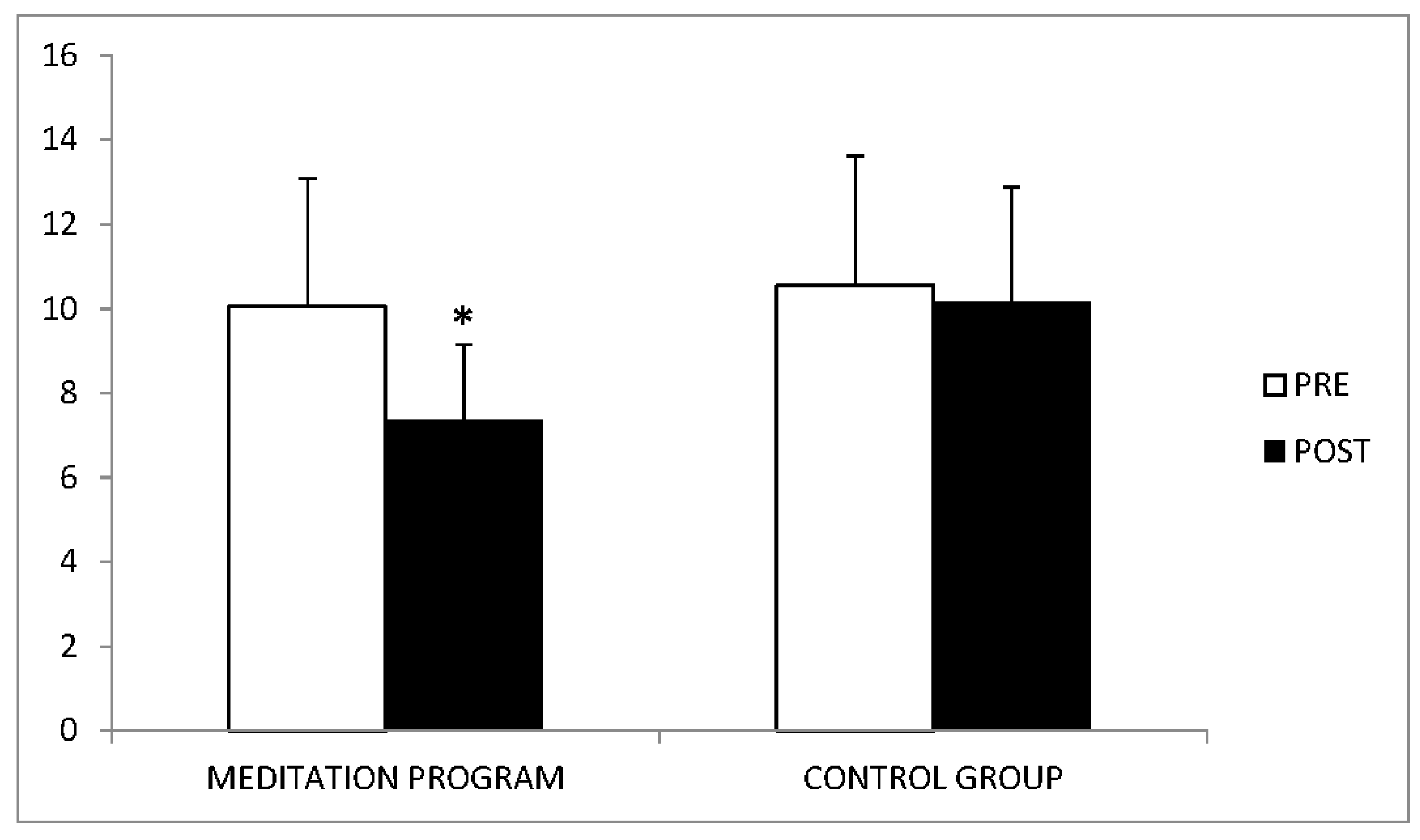
3. Results
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Grant, J.S.; Graven, L.J. Problems experienced by informal caregivers of individuals with heart failure: An integrative review. Int. J. Nurs. Stud. 2018, 80, 41–66. [Google Scholar] [CrossRef] [PubMed]
- Meléndez, J.C.; Tomás, J.M.; Navarro, E. Everyday life activities and well-being: Their relationships with age and gender in the elderly. Ann. Psychol. 2011, 27, 164–169. [Google Scholar]
- Hsu, T.; Loscalzo, M.; Ramani, R.; Forman, S.; Popplewell, L.; Clark, K.; Katheria, V.; Feng, T.; Strowbridge, R.; Rinehart, R.; et al. Factors associated with high burden in caregivers of older adults with cancer. Cancer 2014, 120, 2927–2935. [Google Scholar] [CrossRef] [PubMed]
- Liew, T.M.; Tai, B.C.; Yap, P.; Koh, G.C. Comparing the Effects of Grief and Burden on Caregiver Depression in Dementia Caregiving: A Longitudinal Path Analysis over 2.5 Years. J. Am. Med. Dir. Assoc. 2019, 20, 977–983. [Google Scholar] [CrossRef] [PubMed]
- Marfil-Gómez, R.; Morales-Puerto, M.; León-Campos, Á.; Morales-Asencio, J.M.; Morilla-Herrera, J.C.; Timonet-Andreu, E.; Cuevas-Fernández, G.M.; Martí-García, C.; López-Leiva, I.; García-Mayor, S. Quality of Life, Physical and Mental Health of Family Caregivers of Dependent People with Complex Chronic Disease: Protocol of a Cohort Study. Int. J. Environ. Res. Public Health 2020, 17, 7489. [Google Scholar] [CrossRef]
- Ruisoto, P.; Ramírez, M.; Paladines-Costa, B.; Vaca, S.; Clemente-Suárez, V.J. Predicting Caregiver Burden in Informal Caregivers for the Elderly in Ecuador. Int. J. Environ. Res. Public Health 2020, 17, 7338. [Google Scholar] [CrossRef]
- Sallim, A.B.; Sayampanathan, A.; Cuttilan, A.; Ho, R. Prevalence of Mental Health Disorders Among Caregivers of Patients with Alzheimer Disease. J. Am. Med. Dir. Assoc. 2015, 16, 1034–1041. [Google Scholar] [CrossRef]
- Torres Lima, A.G.; Da Silva Sales, C.C.; De Lima Serafim, W.F. Burden, depression and anxiety in primary caregivers of children and adolescents in renal replacement therapy. J. Bras. Nefrol. 2019, 41, 356–363. [Google Scholar] [CrossRef] [PubMed]
- de Camargos, M.G.; Paiva, B.S.R.; de Almeida, C.S.L.; Paiva, C.E. What Is Missing for You to Be Happy? Comparison of the Pursuit of Happiness among Cancer Patients, Informal Caregivers, and Healthy Individuals. J. Pain Symptom Manag. 2019, 58, 417–426. [Google Scholar] [CrossRef] [PubMed]
- Javalkar, K.; Rak, E.; Phillips, A.; Haberman, C.; Ferris, M.; Van Tilburg, M. Predictors of Caregiver Burden among Mothers of Children with Chronic Conditions. Children 2017, 4, 39. [Google Scholar] [CrossRef] [PubMed]
- Bouchard, K.; Greenman, P.S.; Pipe, A.; Johnson, S.M.; Tulloch, H. Reducing Caregiver Distress and Cardiovascular Risk: A Focus on Caregiver-Patient Relationship Quality. Can. J. Cardiol. 2019, 35, 1409–1411. [Google Scholar] [CrossRef] [PubMed]
- Teixeira, R.J.; Remondes-Costa, S.; Graça Pereira, M.; Brandão, T. The impact of informal cancer caregiving: A literature review on psychophysiological studies. Eur. J. Cancer Care 2019, 28, e13042. [Google Scholar] [CrossRef] [PubMed]
- Mulcahy, J.S.; Larsson, D.E.O.; Garfinkel, S.N.; Critchley, H.D. Heart rate variability as a biomarker in health and affective disorders: A perspective on neuroimaging studies. Neuroimage 2019, 202, 116072. [Google Scholar] [CrossRef]
- Malik, M.; Bigger, J.T.; Camm, A.J.; Kleiger, R.E.; Malliani, A.; Moss, A.J.; Schwartz, P.J. Heart rate variability. Standards of measurement, physiological interpretation, and clinical use. Task Force of the European Society of Cardiology and the North American Society of Pacing and Electrophysiology. Eur. Heart J. 1996, 17, 354–381. [Google Scholar] [CrossRef]
- Díaz-Rodríguez, L.; Arroyo-Morales, M.; Fernández-de-las-Peñas, C.; García-Lafuente, F.; García-Royo, C.; Tomás-Rojas, I. Immediate effects of reiki on heart rate variability, cortisol levels, and body temperature in health care professionals with burnout. Biol. Res. Nurs. 2011, 13, 376–382. [Google Scholar] [CrossRef] [PubMed]
- Díaz-Rodríguez, L.; Fernández-Pérez, A.M.; Galiano-Castillo, N.; Cantarero-Villanueva, I.; Fernández-Lao, C.; Martín-Martín, L.M.; Arroyo-Morales, M. Do Patient Profiles Influence the Effects of Massage? A Controlled Clinical Trial. Biol. Res. Nurs. 2016, 18, 489–497. [Google Scholar] [CrossRef] [PubMed]
- Gandhi, S.; Palled, V.K.; Sahu, M.; Jagannathan, A.; Khanna, M.; Jose, A. Effectiveness of Caregivers’ Yoga Module on Psychological Distress and Mental Well-Being among Caregivers of Patients Admitted to Neurological Rehabilitation Wards of a Tertiary Care Institute, Bengaluru, Karnataka, India. J. Neurosci. Rural Pract. 2019, 10, 657–665. [Google Scholar] [CrossRef]
- Lopez, G.; Chaoul, A.; Powers-James, C.; Eddy, C.A.; Mallaiah, S.; Gomez, T.I.; Williams, J.L.; Wei, Q.; Bruera, E.; Cohen, L. Group Yoga Effects on Cancer Patient and Caregiver Symptom Distress: Assessment of Self-reported Symptoms at a Comprehensive Cancer Center. Integr. Cancer Ther. 2018, 17, 1087–1094. [Google Scholar] [CrossRef]
- National Center for Complementary and Integrative Health. 2016. Available online: https://www.nccih.nih.gov/health/meditation-in-depth (accessed on 25 March 2020).
- Hölzel, B.K.; Lazar, S.W.; Gard, T.; Schuman-Olivier, Z.; Vago, D.R.; Ott, U. How Does Mindfulness Meditation Work? Proposing Mechanisms of Action from a Conceptual and Neural Perspective. Perspect. Psychol. Sci. 2011, 6, 537–559. [Google Scholar] [CrossRef]
- Lippelt, D.P.; Hommel, B.; Colzato, L.S. Focused attention, open monitoring and loving kindness meditation: Effects on attention, conflict monitoring, and creativity—A review. Front. Psychol. 2014, 5, 1083. [Google Scholar] [CrossRef] [PubMed]
- Magan, D.; Yadav, R.K. Physiological persona differences based on stress and inflammation between meditators and healthy controls. J. Complement. Integr. Med. 2019, 17. [Google Scholar] [CrossRef]
- Kwak, S.; Kim, S.Y.; Bae, D.; Hwang, W.J.; Cho, K.I.K.; Lim, K.O.; Park, H.Y.; Lee, T.Y.; Kwon, J.S. Enhanced Attentional Network by Short-Term Intensive Meditation. Front. Psychol. 2020, 10, 3073. [Google Scholar] [CrossRef]
- Magan, D.; Yadav, R.K.; Bal, C.S.; Mathur, R.; Pandey, R.M. Brain Plasticity and Neurophysiological Correlates of Meditation in Long-Term Meditators: A 18Fluorodeoxyglucose Positron Emission Tomography Study Based on an Innovative Methodology. J. Altern. Complement. Med. 2019, 25, 1172–1182. [Google Scholar] [CrossRef]
- Pagliaro, G.; Bernardini, F. A Specific Type of Tibetan Medicine Meditation for Women with Breast Cancer: A Pilot Survey. Oncology 2019, 97, 119–124. [Google Scholar] [CrossRef]
- Levine, G.N.; Lange, R.A.; Bairey-Merz, C.N.; Davidson, R.J.; Jamerson, K.; Mehta, P.K.; Michos, E.D.; Norris, K.; Ray, I.B.; Saban, K.L.; et al. American Heart Association Council on Clinical Cardiology; Council on Cardiovascular and Stroke Nursing; and Council on Hypertension. Meditation and Cardiovascular Risk Reduction: A Scientific Statement from the American Heart Association. J. Am. Heart Assoc. 2017, 6, e002218. [Google Scholar] [CrossRef]
- Lau, S.; Chong, M.S.; Ali, N.; Chan, M.; Chua, K.C.; Lim, W.S. Caregiver Burden: Looking Beyond the Unidimensional Total Score. Alzheimer Dis. Assoc. Disord. 2015, 29, 338–346. [Google Scholar] [CrossRef]
- Danucalov, M.A.; Kozasa, E.H.; Afonso, R.F.; Galduroz, J.C.; Leite, J.R. Yoga and compassion meditation program improve quality of life and self-compassion in family caregivers of Alzheimer’s disease patients: A randomized controlled trial. Geriatr. Gerontol. Int. 2017, 17, 85–91. [Google Scholar] [CrossRef]
- Alarcón, R. Desarrollo de una Escala Factorial para medir Felicidad. Interam. J. Psychol. 2006, 40, 99–106. [Google Scholar]
- Sánchez-López, M.P.; Limiñana-Gras, R.M.; Colodro-Conde, L.; Cuéllar-Flores, I. Use of the Hospital Anxiety and Depression Scale in Spanish caregivers. Scand. J. Caring Sci. 2015, 29, 751–759. [Google Scholar] [CrossRef]
- Kuppusamy, M.; Kamaldeen, D.; Pitani, R.; Amaldas, J.; Ramasamy, P.; Shanmugam, P.; Vijayakumar, V. Effects of yoga breathing practice on heart rate variability in healthy adolescents: A randomized controlled trial. Integr. Med. Res. 2020, 9, 28–32. [Google Scholar] [CrossRef]
- Cohen, J. Statistical Power Analysis for the Behavioral Sciences, 2nd ed.; Elsevier Science: Burlington, NJ, USA, 2013; Available online: http://www.utstat.toronto.edu/~brunner/oldclass/378f16/readings/CohenPower.pdf (accessed on 27 December 2020).
- Saeed, S.A.; Cunningham, K.; Bloch, R.M. Depression and Anxiety Disorders: Benefits of Exercise, Yoga, and Meditation. Am. Fam. Physician 2019, 99, 620–627. [Google Scholar] [PubMed]
- Hearn, J.H.; Cotter, I.; Finlay, K.A. Efficacy of Internet-Delivered Mindfulness for Improving Depression in Caregivers of People with Spinal Cord Injuries and Chronic Neuropathic Pain: A Randomized Controlled Feasibility Trial. Arch. Phys. Med. Rehabil. 2019, 100, 17–25. [Google Scholar] [CrossRef] [PubMed]
- Klamut, M.K. The promotion of happiness. Ann. Univ. Mariae Curie Sklodowska Med. 2002, 57, 1–9. [Google Scholar] [PubMed]
- Dunne, S.; Sheffield, D.; Chilcot, J. Brief report: Self-compassion, physical health and the mediating role of health-promoting behaviours. J. Health Psychol. 2018, 23, 993–999. [Google Scholar] [CrossRef]
- Dambrun, M.; Ricard, M.; Després, G.; Drelon, E.; Gibelin, E.; Gibelin, M.; Loubeyre, M.; Py, D.; Delpy, A.; Garibbo, C.; et al. Measuring happiness: From fluctuating happiness to authentic-durable happiness. Front. Psychol. 2012, 3, 16. [Google Scholar] [CrossRef]
- Dambrun, M. When the dissolution of perceived body boundaries elicits happiness: The effect of selflessness induced by a body scan meditation. Conscious. Cogn. 2016, 46, 89–98. [Google Scholar] [CrossRef]
- Liu, I.; Ni, S.; Peng, K. Happiness at Your Fingertips: Assessing Mental Health with Smartphone Photoplethysmogram-Based Heart Rate Variability Analysis. Telemed. J. e-Health 2020, 26, 1483–1491. [Google Scholar] [CrossRef]
- Fernández-Lao, C.; Cantarero-Villanueva, I.; Díaz-Rodríguez, L.; Cuesta-Vargas, A.I.; Fernández-Delas-Peñas, C.; Arroyo-Morales, M. Attitudes towards massage modify effects of manual therapy in breast cancer survivors: A randomised clinical trial with crossover design. Eur. J. Cancer Care 2012, 21, 233–241. [Google Scholar] [CrossRef]
- Yuen, A.W.; Sander, J.W. Can natural ways to stimulate the vagus nerve improve seizure control? Epilepsy Behav. 2017, 67, 105–110. [Google Scholar] [CrossRef]
- Arya, N.K.; Singh, K.; Malik, A.; Mehrotra, R. Effect of Heartfulness cleaning and meditation on heart rate variability. Indian Heart J. 2018, 70, S50–S55. [Google Scholar] [CrossRef]
- Chu, I.H.; Lin, Y.J.; Wu, W.L.; Chang, Y.K.; Lin, I.M. Effects of Yoga on Heart Rate Variability and Mood in Women: A Randomized Controlled Trial. J. Altern. Complement. Med. 2015, 21, 789–795. [Google Scholar] [CrossRef] [PubMed]
- Chang, K.M.; Chueh, M.T.W.; Lai, Y.J. Meditation Practice Improves Short-Term Changes in Heart Rate Variability. Int. J. Environ. Res. Public Health 2020, 17, 2128. [Google Scholar] [CrossRef] [PubMed]
- Landry, J.M. Physiological and psychological effects of a Himalayan singing bowl in meditation practice: A quantitative analysis. Am. J. Health Promot. 2014, 28, 306–309. [Google Scholar] [CrossRef] [PubMed]
| Variables | Meditation Program (n = 19) | Control Group (n = 18) | p |
|---|---|---|---|
| Age (y) Mean (SD) ** | 44.42 ± 8.17 | 43.61 ± 6.46 | |
| (33–64) | (34–56) | 0.74 | |
| Gender (%) * | |||
| Female | 73.7 | 77.8 | |
| Male | 26.3 | 22.2 | 0.77 |
| Ethnicity (%) * | |||
| Caucasian | 94.7 | 100 | |
| Black | 5.3 | 0.0 | |
| Gypsy | 0.0 | 0.0 | |
| Arab | 0.0 | 0.0 | 0.32 |
| Marital status (%) * | |||
| Single | 5.3 | 0.0 | |
| Married | 73.7 | 72.2 | |
| Divorced | 15.8 | 16.7 | |
| Widow | 5.3 | 11.1 | 0.71 |
| Educational level (%) * | |||
| Primary studies | 26.3 | 0.0 | |
| Secondary studies | 42.1 | 27.8 | |
| Higher Education | 31.6 | 72.2 | 0.01 * |
| Occupational status (%) * | |||
| Homemaker | 31.6 | 11.1 | |
| Employed | 68.4 | 88.9 | |
| Unemployed | 0.0 | 0.0 | |
| Retired | 0.0 | 0.0 | 0.13 |
| Smoking status (%) * | |||
| Non-smoker | 57.9 | 55.6 | |
| Smoker | 15.8 | 22.2 | |
| Ex-smoker | 26.3 | 22.2 | 0.87 |
| Alcohol status(%) * | |||
| Don’t consume | 68.4 | 50.0 | |
| Consume monthly | 10.5 | 22.2 | |
| Consume weekly | 21.1 | 27.8 | |
| Consume daily | 0.0 | 0.0 | 0.47 |
| Menopausal status (%) * | |||
| NO | 84.2 | 94.4 | |
| YES | 15.8 | 5.6 | 0.31 |
| Duration of caring (%) * | |||
| 1–5 years | 26.3 | 33.0 | |
| 6–10 years | 47.4 | 38.9 | |
| >11 years | 26.3 | 27.8 | 0.85 |
| Caregiver relationship with care receiver (%) * | |||
| Partner | 5.3 | 5.6 | |
| Parent | 52.6 | 55.6 | |
| Child | 42.1 | 38.9 | 0.98 |
| Weight (Kg) Mean (SD) ** | 70.60 ± 12.78 | 68.63 ± 14.38 | |
| (53–110) | (56–105) | 0.66 | |
| Height (cm) Mean (SD) ** | 165.78 ± 7.08 | 165.66 ± 6.80 | |
| (155–180) | (158–179) | 0.95 | |
| Body Mass Index Mean ** (Kg/m2) (SD) | 25.73 ± 4.77 | 24.76 ± 3.30 | |
| (20.20–39.56) | (21.01–32.77) | 0.48 |
| Outcomes | Meditation Program (n = 19) | Control Group (n = 18) | F |
|---|---|---|---|
| Heart rate (beat * min−1) | |||
| Baseline | 75.05 ± 10.01 | 73.89 ± 6.41 | |
| Post-treatment | 63.42 ± 1035 | 72.72 ± 6.93 | 17.90 * |
| Systolic Pressure Blood (mm Hg) | |||
| Baseline | 127.21 ± 16.00 | 128.16 ± 9.83 | |
| Post-treatment | 115.63 ± 14.01 | 127.22 ± 10.54 | 16.23 ** |
| Diastolic Pressure Blood (mm Hg) | |||
| Baseline | 74.05 ± 9.57 | 73.16 ± 3.22 | |
| Post-treatment | 67.57 ± 7.50 | 72.05 ± 3.36 | 34.39 ** |
| Heart Rate Variability | |||
| SDNN | |||
| Baseline | 45.08 ± 28.83 | 52.47 ± 16.04 | |
| Post-treatment | 90.33 ± 50.65 | 55.65 ± 16.42 | 13.59 * |
| RMSSD | |||
| Baseline | 41.78 ± 30.16 | 49.64 ± 17.39 | |
| Post-treatment | 91.04 ± 63.81 | 54.58 ± 17.85 | 10.72 * |
| HRV índex | |||
| Baseline | 4.93 ± 2.56 | 6.02 ± 1.55 | |
| Post-treatment | 6.72 ± 2.70 | 5.91 ± 1.34 | 8.40 * |
| LF | |||
| Baseline | 171.08 ± 60.09 | 137.82 ± 41.97 | |
| Post-treatment | 169.00 ± 69.33 | 144.64 ± 46.41 | 0.25 |
| HF | |||
| Baseline | 141.86 ± 61.25 | 140.88 ± 31.49 | |
| Post-treatment | 167.34 ± 65.13 | 137.90 ± 31.48 | 4.82 * |
| LF/HF Ratio | |||
| Baseline | 1.39 ± 0.76 | 1.04 ± 0.45 | |
| Post-treatment | 1.38 ± 1.44 | 1.10 ± 0.52 | 0.06 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Díaz-Rodríguez, L.; Vargas-Román, K.; Sanchez-Garcia, J.C.; Rodríguez-Blanque, R.; Cañadas-De la Fuente, G.A.; De La Fuente-Solana, E.I. Effects of Meditation on Mental Health and Cardiovascular Balance in Caregivers. Int. J. Environ. Res. Public Health 2021, 18, 617. https://doi.org/10.3390/ijerph18020617
Díaz-Rodríguez L, Vargas-Román K, Sanchez-Garcia JC, Rodríguez-Blanque R, Cañadas-De la Fuente GA, De La Fuente-Solana EI. Effects of Meditation on Mental Health and Cardiovascular Balance in Caregivers. International Journal of Environmental Research and Public Health. 2021; 18(2):617. https://doi.org/10.3390/ijerph18020617
Chicago/Turabian StyleDíaz-Rodríguez, Lourdes, Keyla Vargas-Román, Juan Carlos Sanchez-Garcia, Raquel Rodríguez-Blanque, Guillermo Arturo Cañadas-De la Fuente, and Emilia I. De La Fuente-Solana. 2021. "Effects of Meditation on Mental Health and Cardiovascular Balance in Caregivers" International Journal of Environmental Research and Public Health 18, no. 2: 617. https://doi.org/10.3390/ijerph18020617
APA StyleDíaz-Rodríguez, L., Vargas-Román, K., Sanchez-Garcia, J. C., Rodríguez-Blanque, R., Cañadas-De la Fuente, G. A., & De La Fuente-Solana, E. I. (2021). Effects of Meditation on Mental Health and Cardiovascular Balance in Caregivers. International Journal of Environmental Research and Public Health, 18(2), 617. https://doi.org/10.3390/ijerph18020617










