Analysis of the Readability of Questionnaires on Symptoms of Pelvic Floor Dysfunctions Adapted to Spanish
Abstract
1. Introduction
2. Materials and Methods
2.1. Sample Selection
2.1.1. Inclusion Criteria
- - Questionnaires that evaluate the symptoms of urinary incontinence, fecal incontinence, overactive bladder and benign prostate hyperplasia, as well as global questionnaires of pelvic floor dysfunctions;
- - Questionnaires adapted to and validated in Spanish.
2.1.2. Exclusion Criteria
- - Questionnaires developed exclusively in Spanish;
- - Questionnaires aimed at other pathologies that do not belong to the sphere of pelvic floor dysfunctions and that include those symptoms.
2.2. Selected Questionnaires
- - A questionnaire for benign prostatic hyperplasia: IPSS [21];
2.3. Readability Indexes
2.3.1. Readability of Fernández Huerta
2.3.2. The Szigriszt-Pazos Perspicuity Index
2.3.3. The Inflesz Readability Scale
2.3.4. Readability µ (mu)
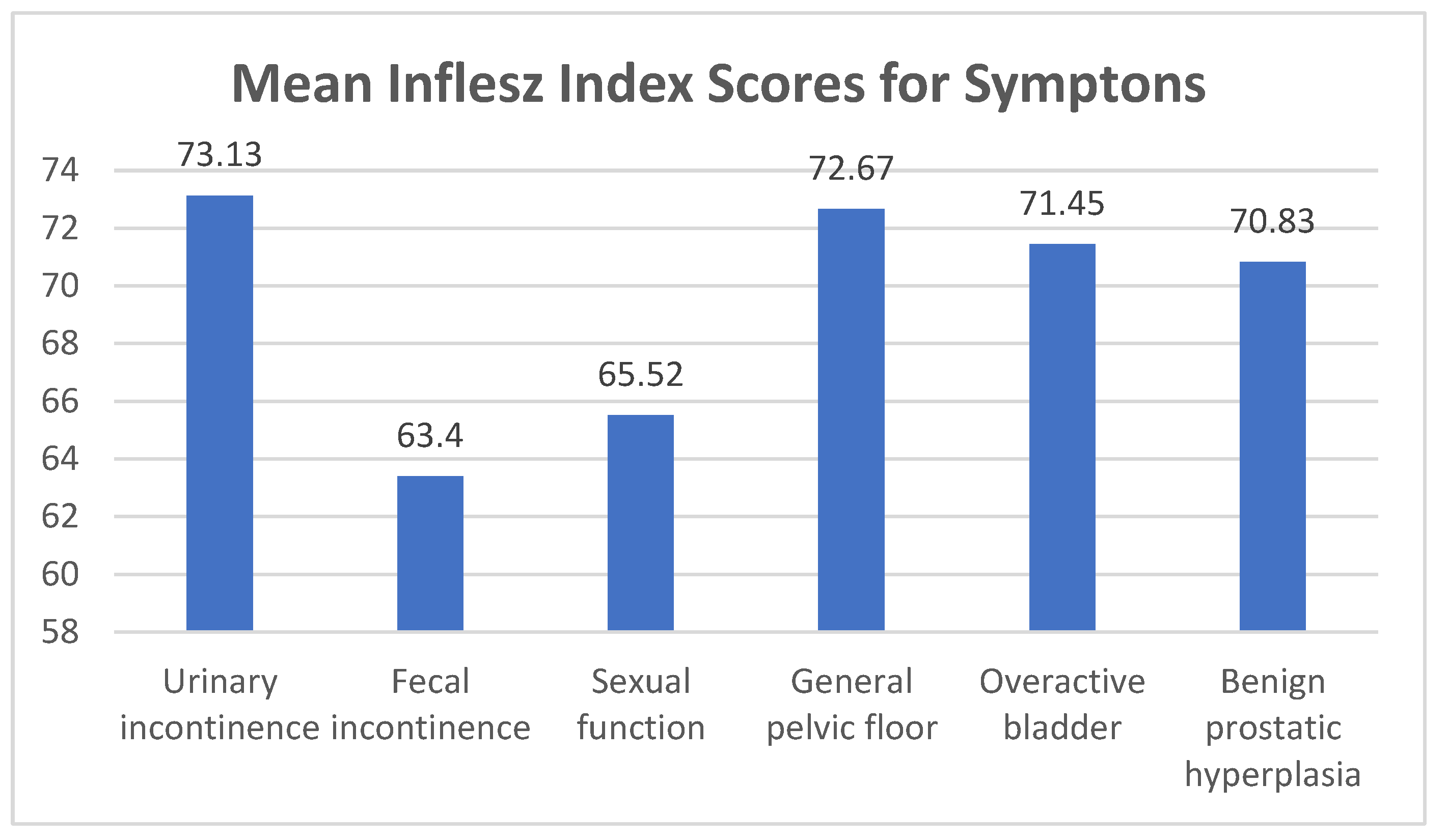
3. Results
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Martí-Ragué, J. Trastornos del suelo pélvico. Cir. Esp. 2005, 77, 254–257. [Google Scholar] [CrossRef]
- Rajkowska-Labon, E.; Bakuła, S.; Kucharzewski, M.; Śliwiński, Z. Efficacy of Physiotherapy for Urinary Incontinence following Prostate Cancer Surgery. BioMed Res. Int. 2014, 2014, 785263. Available online: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4017841/ (accessed on 9 January 2021).
- Yount, S.M. The Impact of Pelvic Floor Disorders and Pelvic Surgery on Women’s Sexual Satisfaction and Function. J. Midwifery Womens Health 2013, 58, 538–545. [Google Scholar] [CrossRef] [PubMed]
- Wiebe, S.; Guyatt, G.; Weaver, B.; Matijevic, S.; Sidwell, C. Comparative responsiveness of generic and specific quality-of-life instruments. J. Clin. Epidemiol. 2003, 56, 52–60. [Google Scholar] [CrossRef]
- Gaines, T.; Malik, R.D. Readability of pelvic floor dysfunction questionnaires. Neurourol. Urodyn. 2020, 39, 813–818. [Google Scholar] [CrossRef] [PubMed]
- Universidad de Oviedo; Martínez-González, M.C.; Martínez-González, R.-A.; Guerra-Tapia, A. La importancia de los cuestionarios en salud. Más Dermatol. 2014, 23, 15–18. [Google Scholar] [CrossRef]
- Hernández-Sampieri, R.; Fernández, C.; Baptista, P. Metodología de la Investigación, 5th ed.; McGraw-Hill: New York, NY, USA, 2010. [Google Scholar]
- Alas, A.N.; Bergman, J.; Dunivan, G.C.; Rashid, R.; Morrisroe, S.N.; Rogers, R.G.; Anger, J.T. Readability of Common Health-Related Quality-of-Life Instruments in Female Pelvic Medicine. Female Pelvic Med. Reconstr. Surg. 2013, 19, 293–297. [Google Scholar] [CrossRef]
- Espuña Pons, M.; Rebollo Álvarez, P.; Puig Clota, M. Validación de la versión española del International Consultation on Incontinence Questionnaire-Short Form. Un cuestionario para evaluar la incontinencia urinaria. Med. Clín. 2004, 122, 288–292. [Google Scholar] [CrossRef]
- Bouallalene-Jaramillo, K.; Bagur-Calafat, M.C.; Girabent-Farrés, M. Validation of the Spanish version of the Urogenital Distress Inventory short form and Incontinence Impact Questionnaire short form for women between the ages of 18 and 65. Actas Urol. Esp. 2015, 39, 511–517. [Google Scholar] [CrossRef]
- Treszezamsky, A.D.; Karp, D.; Dick-Biascoechea, M.; Ehsani, N.; Dancz, C.; Montoya, T.I.; Olivera, C.; Smith, A.L.; Cardenas, R.; Fashokun, T.; et al. Spanish translation and validation of four short pelvic floor disorders questionnaires. Int. Urogynecol. J. 2013, 24, 655–670. [Google Scholar] [CrossRef]
- Sandvik, H.; Espuna, M.; Hunskaar, S. Validity of the incontinence severity index: Comparison with pad-weighing tests. Int. Urogynecol. J. 2006, 17, 520–524. [Google Scholar] [CrossRef]
- Flández, J.; Monrroy, H. Escalas de Evaluación en Incontinencia Fecal. Gastroenterol. Latinoam. 2016, 27, 226–230. Available online: https://gastrolat.org/escalas-de-evaluacion-en-incontinencia-fecal/ (accessed on 16 November 2020).
- Maestre González, Y. Prevalencia de la Incontinencia Fecal en Un Sector de la Ciudad de Barcelona Y Análisis de SU Impacto en la Calidad de Vida Y la Salud Mental; Facultad de Medicina, Departamento de Cirugía: Autónoma de Barcelona, Spain, 2013. [Google Scholar]
- Sánchez-Sánchez, B.; Navarro-Brazález, B.; Arranz-Martín, B.; Sánchez-Méndez, Ó.; de la Rosa-Díaz, I.; Torres-Lacomba, M. The Female Sexual Function Index: Transculturally Adaptation and Psychometric Validation in Spanish Women. Int. J. Environ. Res. Public Health 2020, 17, 994. [Google Scholar] [CrossRef]
- Mestre, M.; Lleberia, J.; Pubill, J.; Espuña-Pons, M. Spanish version of the Pelvic Organ Prolapse/Urinary Incontinence Sexual Questionnaire IUGA-Revised (PISQ-IR): Transcultural validation. Int. Urogynecol. J. 2017, 28, 1865–1873. [Google Scholar] [CrossRef] [PubMed]
- Espuña Pons, M.; Puig Clota, M.; González Aguilón, M.; Zardain, P.C.; Rebollo Álvarez, P. Cuestionario para evaluación de la función sexual en mujeres con prolapso genital y/o incontinencia: Validación de la versión española del “Pelvic Organ Prolapse/Urinary Incontinence Sexual Questionnaire (PISQ-12)”. Actas Urol. Esp. 2008, 32, 211–219. Available online: http://scielo.isciii.es/scielo.php?script=sci_arttext&pid=S0210-48062008000200009&lng=es (accessed on 16 November 2020). [CrossRef]
- Weinberg, A.C.; Brandeis, G.H.; Bruyere, J.; Tsui, J.F.; Weiss, J.P.; Rutman, M.P.; Blaivas, J.G. Reliability and validity of the overactive bladder symptom score in spanish (OABSS-S): Validation of the OABSS in Spanish. Neurourol. Urodyn. 2012, 31, 664–668. [Google Scholar] [CrossRef] [PubMed]
- Espuña Pons, M.; Puig Clota, M.; Rebollo Álvarez, P. Validación de la versión en español del Cuestionario de Autoevaluación del Control de la Vejiga (CACV): Un nuevo instrumento para detectar pacientes con disfunción del tracto urinario inferior. Actas Urol. Esp. 2006, 30, 1017–1024. Available online: http://scielo.isciii.es/scielo.php?script=sci_arttext&pid=S0210-48062006001000008&lng=es (accessed on 2 November 2020). [CrossRef][Green Version]
- Brenes, F.J.; Angulo, J.C.; Ochayta, D.; Rejas, J.; Arumí, D.; Cañadas, A.; Lizarraga, I. Validación psicométrica de las escalas OAB-V8 y OAB-V3 para la detección de pacientes con probable vejiga hiperactiva en la población española. Med. Clín. 2014, 143, 521–529. [Google Scholar] [CrossRef]
- Carballido Rodríguez, J.; Grunfeld Abellán, A.; Escudero Callen, A.; Gil Bermejo, F.J.; Regadera-Anechina, L.; Badía Llach, X. Validación de la versión española del Cuestionario Benign Prostatic Hyperplasia Impact Index. “Estudio Validart”. Actas Urol. Esp. 2008, 32, 230–239. [Google Scholar] [CrossRef][Green Version]
- Espuña Pons, M.; Fillol Crespo, M.; Pascual Amorós, M.A.; Rebollo Álvarez, P.; Prieto Soto, M. Validación de la versión en español del cuestionario “Epidemiology of Prolapse and Incontinence Questionnaire-EPIQ”. Actas Urol. Esp. 2009, 33, 646–653. [Google Scholar] [CrossRef]
- Sánchez-Sánchez, B.; Torres-Lacomba, M.; Yuste-Sánchez, M.J.; Navarro-Brazález, B.; Pacheco-da-Costa, S.; Gutiérrez-Ortega, C.; Zapico-Goñi, Á. Cultural adaptation and validation of the Pelvic Floor Distress Inventory Short Form (PFDI-20) and Pelvic Floor Impact Questionnaire Short Form (PFIQ-7) Spanish versions. Eur. J. Obstet. Gynecol. Reprod. Biol. 2013, 170, 281–285. [Google Scholar] [CrossRef]
- Fernández Huerta, J. Medidas sencillas de lecturabilidad. Consigna 1959, 214, 29–32. [Google Scholar]
- Szigriszt Pazos, F. Sistemas Predictivos de Legibilidad Del Mensaje Escrito: Fórmula de Perspicuidad. Ph.D. Thesis, Facultad de Ciencias de la Información, Universidad Complutense de Madrid, Madrid, Spain, 1993. [Google Scholar]
- Barrio Cantalejo, I.M. Legibilidad Y Salud: Los Métodos de Medición de La Legibilidad Y SU Aplicación al Diseño de Folletos Educativos Sobre Salud; Autónoma de Madrid: Madrid, Spain, 2007; Available online: http://hdl.handle.net/10486/2488 (accessed on 10 July 2021).
- Barrio-Cantalejo, I.M.; Simón-Lorda, P.; Melguizo, M.; Escalona, I.; Marijuán, M.I.; Hernando, P. Validación de la Escala INFLESZ para evaluar la legibilidad de los textos dirigidos a pacientes. An. Sis. San. Navar. 2008, 31, 135–152. Available online: http://scielo.isciii.es/scielo.php?script=sci_arttext&pid=S1137-66272008000300004&lng=en&nrm=iso&tlng=en (accessed on 11 April 2021). [CrossRef] [PubMed]
- Legibilidad Mμ. Available online: https://legibilidadmu.cl/ (accessed on 10 July 2021).
- Stossel, L.M.; Segar, N.; Gliatto, P.; Fallar, R.; Karani, R. Readability of Patient Education Materials Available at the Point of Care. J. Gen. Intern. Med. 2012, 27, 1165–1170. [Google Scholar] [CrossRef] [PubMed]
| Lecturability Fernández Huerta | Level | Perspicuity Szigriszt-Pazos | Level | Perspicuity Inflesz | Level | Legibility µ | Level |
|---|---|---|---|---|---|---|---|
| 90–100 | Very easy | 86–100 | Very easy | 80–100 | Very easy | 91–100 | Very easy |
| 80–90 | Easy | 76–85 | Easy | 65–80 | Somewhat easy | 81–90 | Easy |
| 70–80 | Some easy | 66–75 | Somewhat easy | 55–65 | Normal | 71–80 | Somewhat easy |
| 60–70 | Normal | 51–65 | Normal | 40–55 | Somewhat difficult | 61–70 | Adequate |
| 50–60 | Somewhat difficult | 36–50 | Somewhat difficult | 0–40 | Very difficult | 51–60 | Somewhat difficult |
| 30–50 | Difficult | 16–35 | Difficult | 31–50 | Difficult | ||
| 0–30 | Very difficult | 0–15 | Very difficult | 0–30 | Very difficult |
| Questionnaire | Dysfunction | Number of Questions | Characteristics |
|---|---|---|---|
| ICIQ-SF [9] | Urinary incontinence | 3 | Measures the frequency, quantity and affectation |
| UDI-6 [10] | Urinary incontinence | 6 | Grade of recommendation A; measures the degree of severity |
| 3IQ [11] | Urinary incontinence | 3 | Classifies urge or stress incontinence in primary care settings |
| QUID [11] | Urinary incontinence | 6 | Has two subscales: stress and urgency |
| Severity test of Sandvik [12] | Urinary incontinence | 2 | Measures aspects of frequency and quantity |
| WEXNER [13] | Fecal incontinence | 3 | Collects data on the type of leak, use of dressings and lifestyle alteration |
| Browning y Parks [13] | Fecal incontinence | 1 | Divided into four degrees |
| FISI [13] | Fecal incontinence | 1 | A table is obtained with values between 0 and 61 points |
| St Mark’s Hospital [14] | Fecal incontinence | 5 | Evaluates use of astringent medication, diapers, or degree of urgency |
| FSFI [15] | Sexual function | 19 | Evaluates six domains: desire, arousal, lubrication, orgasm, satisfaction and pain |
| PISQ-IR [16] | Sexual function | 12/21 | 12 items for sexually inactive women; 21 items for sexually active women |
| PISQ-12 [17] | Sexual function | 12 | Evaluates women with POP and/or urinary incontinence |
| OABSS [18] | Overactive bladder | 7 | Five items for urinary urgency and two for daily and nocturnal frequency |
| B-SAQ [19] | Overactive bladder | 8 | Divided into two scales that report discomfort and symptoms |
| OAB-V8 [20] | Overactive bladder | 8 | Measures the magnitude of affectation of the symptoms; a dichotomous item assesses the gender of the patient |
| OAB-V3 [20] | Overactive bladder | 3 | Neutral with respect to the gender of the patient |
| IPSS [21] | Benign prostatic hyperplasia | 8 | Seven items measure frequency and severity of symptoms and one item measures the general impact on quality of life |
| EPIQ [22] | General pelvic floor symptoms | 22 | Seven dimensions: Overactive bladder, stress urinary incontinence, quality of life, pelvic prolapse, incontinence, emptying pain and difficulty and defecatory dysfunction |
| PFDI-20 [23] | General pelvic floor symptoms | 20 | Divided into three scales: prolapse, colorectal–anal and urinary symptoms. |
| Questionnaires | Fernández Huerta | Szigriszt-Pazos | Inflesz | Legibility µ |
|---|---|---|---|---|
| Normal readability limit | 61 | 51 | 56 | 61 |
| Urinary incontinence | 77.68 | 73.13 | 73.13 | 68.62 |
| ICIQ-SF | 81.39 | 77.08 | 77.08 | 71.51 |
| UDI-6 | 61.89 | 56.50 | 56.50 | 58.57 * |
| 3 IQ | 75.50 | 70.87 | 70.87 | 61.63 |
| QUID | 77.15 | 72.80 | 72.80 | 66.29 |
| Severity test of Sandvik | 92.47 | 88.41 | 88.41 | 85.11 |
| Fecal incontinence | 67.90 | 63.40 | 63.40 | 58.17 |
| Wexner | 99.92 | 95.96 | 95.96 | 76.24 |
| Browning and Parks | 44.12 * | 38.98 * | 38.98 * | 47.34 * |
| FISI | 73.49 | 69.43 | 69.43 | 63.36 |
| St Mark´s Hospital | 54.08 * | 49.24 * | 49.24 * | 45.73 * |
| Sexual Function | 70.03 | 65.52 | 65.52 | 59.64 |
| FSFI | 68.65 | 63.87 | 63.87 | 55.23 * |
| PISQ-IR | 71.56 | 67.42 | 67.42 | 54.75 * |
| PISQ 12 | 69.87 | 65.26 | 65.26 | 68.94 |
| Overactive bladder | 76.07 | 71.45 | 71.45 | 72.72 |
| B-SAQ | 72.09 | 67.01 | 67.01 | 59.44 * |
| OAB-V8 | 74.45 | 69.82 | 69.82 | 71.53 |
| OAB-V3 | 77.69 | 73.17 | 73.17 | 86.52 |
| OABSS-S | 80.05 | 75.79 | 75.79 | 73.39 |
| Benign prostatic hyperplasia | 75.30 | 70.83 | 70.83 | 55.94 |
| IPSS | 75.30 | 70.83 | 70.83 | 55.94 * |
| General pelvic floor symptoms | 77.20 | 72.67 | 72.67 | 51.62 |
| EPIQ | 72.36 | 67.69 | 67.69 | 56.87 * |
| PFDI-20 | 82.04 | 77.65 | 77.65 | 46.36 * |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Checa-Moreno, V.; Díaz-Mohedo, E.; Suárez-Serrano, C. Analysis of the Readability of Questionnaires on Symptoms of Pelvic Floor Dysfunctions Adapted to Spanish. Int. J. Environ. Res. Public Health 2021, 18, 10320. https://doi.org/10.3390/ijerph181910320
Checa-Moreno V, Díaz-Mohedo E, Suárez-Serrano C. Analysis of the Readability of Questionnaires on Symptoms of Pelvic Floor Dysfunctions Adapted to Spanish. International Journal of Environmental Research and Public Health. 2021; 18(19):10320. https://doi.org/10.3390/ijerph181910320
Chicago/Turabian StyleCheca-Moreno, Víctor, Esther Díaz-Mohedo, and Carmen Suárez-Serrano. 2021. "Analysis of the Readability of Questionnaires on Symptoms of Pelvic Floor Dysfunctions Adapted to Spanish" International Journal of Environmental Research and Public Health 18, no. 19: 10320. https://doi.org/10.3390/ijerph181910320
APA StyleCheca-Moreno, V., Díaz-Mohedo, E., & Suárez-Serrano, C. (2021). Analysis of the Readability of Questionnaires on Symptoms of Pelvic Floor Dysfunctions Adapted to Spanish. International Journal of Environmental Research and Public Health, 18(19), 10320. https://doi.org/10.3390/ijerph181910320






