How People with Lived Experiences of Substance Use Understand and Experience User Involvement in Substance Use Care: A Synthesis of Qualitative Studies
Abstract
1. Introduction
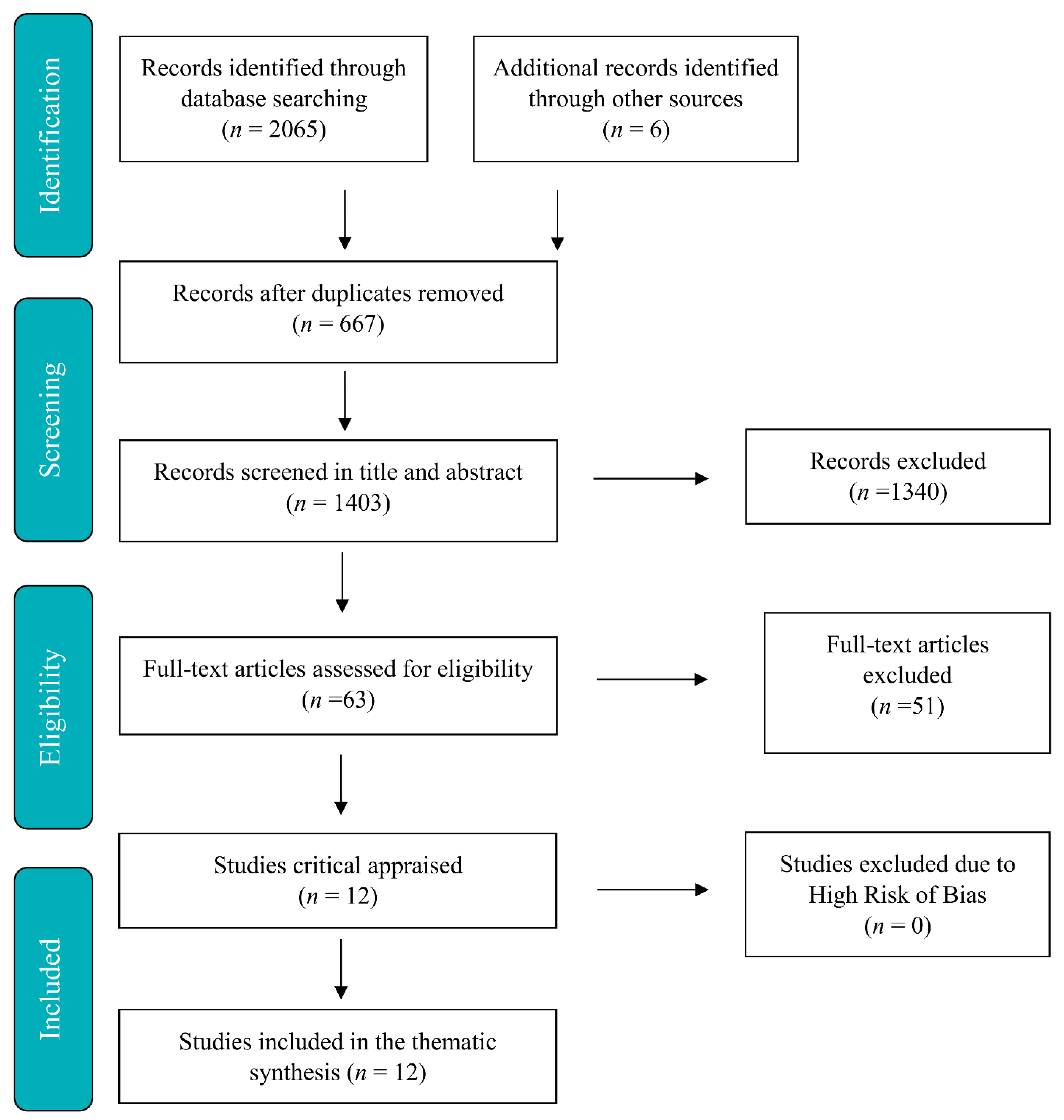
2. Materials and Methods
2.1. Data Collection
- (1)
- The study was an empirical study, written in English, and published in a peer-reviewed journal;
- (2)
- The study included qualitative data that explored the understandings and experiences of user involvement in substance use care from the perspective of people with lived experiences of substance use. In cases of mixed-method studies, only the qualitative results were included;
- (3)
- The study sample consisted of people who were 18 years old or older, had lived experiences of substance use, and were receiving help from the welfare system to reduce any difficulties resulting from drug use;
- (4)
- The study was published between January 2008 and June 2021.
2.2. Characteristics of the Primary Studies
2.3. Analytic Methods
3. Results
3.1. The Fluid Concept of User Involvement
3.1.1. User Involvement as Joint Meaning Production
3.1.2. User Involvement as a Point of View That Is Heard
3.1.3. User Involvement as Representation in the Welfare Services
3.2. Key Practices
3.2.1. To Been Seen and Respected as a Unique Person
3.2.2. Quality of the Interaction Process
3.2.3. Scope of Action
4. Discussion
Strength and Limitations
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Goodhew, M.; Stein-Parbury, J.; Dawson, A. Consumer participation in drug treatment: A systematic review. Drugs Alcohol Today 2019, 19, 97–112. [Google Scholar] [CrossRef]
- Laitila, M.; Nikkonen, M.; Pietilä, A.-M. Involvement in mental health and substance abuse work: Conceptions of service users. Nurs. Res. Pract. 2011, 11, 20. [Google Scholar] [CrossRef]
- Tambuyzer, E.; Pieters, G.; Van Audenhove, C. Patient involvement in mental health care: One size does not fit all. Health Expect. 2014, 17, 138–150. [Google Scholar] [CrossRef] [PubMed]
- Hyshka, E.; Karekezi, K.; Tan, B.; Slater, L.G.; Jahrig, J.; Wild, T.C. The role of consumer perspectives in estimating population need for substance use services: A scoping review. BMC Health Serv. Res. 2017, 17, 217. [Google Scholar] [CrossRef] [PubMed]
- Ti, L.; Tzemis, D.; Buxton, J.A. Engaging people who use drugs in policy and program development: A review of the literature. Subst. Abus. Treat. Prev. Policy 2012, 7, 47. [Google Scholar] [CrossRef] [PubMed]
- Marshall, T.; Kinnard, E.N.; Hancock, M.; King-Jones, S.; Olson, K.; Abba-Aji, A.; Rittenbach, K.; Vohra, S. Patient engagement, treatment preferences and shared decision-making in the treatment of opioid use disorder in adults: A scoping review protocol. BMJ Open 2018, 8, e022267. [Google Scholar] [CrossRef]
- Greer, A.M.; Amlani, A.; Burmeister, C.; Scott, A.; Newman, C.; Lampkin, H.; Pauly, B.; Buxton, J.A. Peer engagement barriers and enablers: Insights from people who use drugs in British Columbia, Canada. Can. J. Public Health 2019, 110, 227–235. [Google Scholar] [CrossRef]
- Crawford, M.J.; Rutter, D.; Manley, C.; Weaver, T.; Bhui, K.; Fulop, N.; Tyrer, P. Systematic review of involving patients in the planning and development of health care. BMJ 2002, 325, 1263. [Google Scholar] [CrossRef] [PubMed]
- Marchand, K.; Beaumont, S.; Westfall, J.; MacDonald, S.; Harrison, S.; Marsh, D.C.; Schechter, O.; Joekes, E. Conceptualizing patient-centered care for substance use disorder treatment: Findings from a systematic scoping review. Subst. Abus. Treat. Prev. Policy 2019, 14, 37. [Google Scholar] [CrossRef]
- Marchand, K.; Foreman, J.; MacDonald, S.; Harrison, S.; Schechter, M.T.; Oviedo-Joekes, E. Building healthcare provider relationships for patient-centered care: A qualitative study of the experiences of people receiving injectable opioid agonist treatment. Subst. Abus. Treat. Prev. Policy 2020, 15, 7. [Google Scholar] [CrossRef]
- Arnstein, S.R. A ladder of citizen participation. J. Am. Inst. Plan. 1969, 35, 216–224. [Google Scholar] [CrossRef]
- Burns, D.; Taylor, M. Auditing Community Participation; Policy Press: Bristol, UK, 2000. [Google Scholar]
- Cornwall, A. Unpacking Participation: Models, meanings and practices. Community Dev. J. 2008, 43, 269–283. [Google Scholar] [CrossRef]
- Hart, R.A. Children’s Participation: The Theory and Practice of Involving Young Citizens in Community Development and Environmental Care; Routledge: New York, NY, USA, 2013. [Google Scholar]
- Pretty, J. The many interpretations of participation. Focus 1995, 16, 4–5. [Google Scholar]
- Tritter, J.Q.; McCallum, A. The snakes and ladders of user involvement: Moving beyond Arnstein. Health Policy 2006, 76, 156–168. [Google Scholar] [CrossRef]
- White, D. Consumer and community participation: A reassessment of process, impact and value. In The Handbook of Social Studies in Health and Medicine; Albrecht, I.G.L., Fitzpatrick, R., Scrimshaw, S.C., Eds.; SAGE: London, UK, 2003. [Google Scholar]
- Wilcox, D. The Guide to Effective Participation; Partnership Books: Brighton, UK, 1994. [Google Scholar]
- Beresford, P. The theory and philosophy behind user involvement. In Social Care, Service Users and User Involvement; Beresford, I.P., Carr, S., Eds.; Jessica Kingley: London, UK, 2012; pp. 21–36. [Google Scholar]
- Bochel, C.; Bochel, H.; Somerville, P.; Worley, C. Marginalised or enabled voices? ‘User participation’ in policy and practice. Soc. Policy Soc. 2008, 7, 201–210. [Google Scholar] [CrossRef][Green Version]
- Askheim, O.P. Brukermedvirkningsdiskurser i den norske velferdspolitikken [User involvement discourses in Norwegian welfare policy]. Tidsskr. Velferdsforskning 2017, 20, 134–149. [Google Scholar] [CrossRef]
- Bee, P.; Price, O.; Baker, J.; Lovell, K. Systematic synthesis of barriers and facilitators to service user-led care planning. Br. J. Psychiatry 2015, 207, 104–114. [Google Scholar] [CrossRef]
- Trujols, J.; Siñol, N.; Iraurgi, I.; Batlle, F.; Guàrdia, J.; de los Cobos, J.P. Patient and clinician’s ratings of improvement in methadone-maintained patients: Differing perspectives? Harm Reduct. J. 2011, 8, 23. [Google Scholar] [CrossRef] [PubMed]
- Trujols, J.; Iraurgi, I.; Oviedo-Joekes, E.; Guàrdia-Olmos, J. A critical analysis of user satisfaction surveys in addiction services: Opioid maintenance treatment as a representative case study. Patient Prefer. Adherence 2014, 8, 107. [Google Scholar] [CrossRef]
- Noblit, G.W.; Hare, R.D. Meta-Ethnography: Synthesizing Qualitative Studies; Sage: London, UK, 1988; Volume 11. [Google Scholar]
- Malterud, K. Qualitative Metasynthesis: A Research Method for Medicine and Health Sciences; Routledge: New York, NY, USA, 2019. [Google Scholar]
- King, A. Service user involvement in methadone maintenance programmes: The philosophy, the ideal and the reality. Drugs: Educ. Prev. Policy 2011, 98, 276–284. [Google Scholar] [CrossRef]
- Patterson, S.; Weaver, T.; Agath, K.; Albert, E.; Rhodes, T.; Rutter, D.; Crawford, M. “They can’t solve the problem without us”: Qualitative study of stakeholder perspective on user involvement in drug treatment services in England. Health Care Community 2009, 17, 54–62. [Google Scholar] [CrossRef]
- Fischer, J.; Neale, J. Involving drug users in treatment decisions: An exploration of potential problems. Drugs Educ. Prev. Policy 2009, 15, 161–175. [Google Scholar] [CrossRef]
- Fischer, J.; Neale, J.; Bloor, M.; Jenkins, N. Conflict and user involvement in drugs misuse treatment decision-making: A qualitative study. Subst. Treat. Prev. Policy 2008, 3, 21. [Google Scholar] [CrossRef] [PubMed]
- Hansen, I.L. User’s Choices in Providing Services to the Most Vulnerable Homeless People. Soc. Incl. 2018, 6, 319–326. [Google Scholar] [CrossRef]
- Ness, O.; Kvello, Ø.; Borg, M.; Semb, R.; Davidson, L. “Sorting things out together:” Young Adults’ Experiences of Collaborative Practices in Mental Health and Substance Use Care. Am. J. Psychiatr. Rehabil. 2017, 20, 126–142. [Google Scholar] [CrossRef]
- Rance, J.; Treloar, C. “We are people too”: Consumer participation and the potential transformation of therapeutic relations within drug treatment. Int. J. Drug Policy 2015, 26, 30–36. [Google Scholar] [CrossRef]
- Larsen, T.; Sagvaag, H. Empowerment and pathologisation: A case study in Norwegian mental health and substance abuse services. Health Expect. 2018, 21, 1231–1240. [Google Scholar] [CrossRef] [PubMed]
- Patterson, S.; Weaver, T.; Crawford, M. Drug service user groups: Only a partial solution to the problem of developing user involvement. Drugs Educ. Prev. Policy 2010, 17, 84–97. [Google Scholar] [CrossRef]
- Van Hout, M.C.; McElrath, K. Service user involvement in drug treatment programmes: Barriers to implementation and potential benefits for client recovery. Drugs Educ. Prev. Policy 2012, 19, 474–483. [Google Scholar] [CrossRef]
- Page, M.J.; Moher, D.; Bossuyt, P.M.; Boutron, I.; Hoffmann, T.C.; Mulrow, C.D.; Shamseer, L.; Tetzlaff, J.M.; Akl, E.A.; Brennan, S.E.; et al. PRISMA 2020 explanation and elaboration: Updated guidance and exemplars for reporting systematic reviews. BMJ 2021, 29, 372. [Google Scholar]
| Concepts | Terms |
|---|---|
| Concept I: service user perspectives | “user participat*” OR rights OR cooperation OR co?production OR involvement OR participation OR engagement OR “take part” OR patient satisfaction OR patient?centered evaluation OR service user perspective OR patient perception OR shared decision-making. |
| Concept II: substance use problems | “drug-related” OR “drug abuse*” OR “drug misuse*” OR “illicit drug*” OR “substance abuse*” OR “problematic substance use” OR addiction. |
| Concept III: user involvement | participation OR involvement OR user involvement OR engag* OR patient activat* OR empowerment OR shared decision* OR partnership OR consumer participation OR experience* OR opinion* OR view* OR meaning* OR knowledge* OR understand* OR attitude OR satisfaction OR voices. |
| Concept IV: substance use services | “social service” OR support* OR counsel* OR “social work” OR practitioner OR “health service” OR therap* OR “mental health” OR “social care” OR “local service” OR “welfare service” OR postvention OR treatment OR harm reduction service OR health care OR substance use services OR drug treatment service. |
| Concept V: qualitative research | focus group* OR qualitative research OR qualitative study OR qualitative studies OR qualitative method* OR interviews OR phenomenolog* OR interpretive OR interpretative OR hermeneutic* OR “first person” OR “self-report*” OR narrativ* OR “grounded theory” OR “field stud*” |
| Article | Country | Data | Theoretical Concept | Relevant Sample | Analytical Approach | Research Question/Aim |
|---|---|---|---|---|---|---|
| Fischer, J., Neale, J., Bloor, M., & Jenkins, N. (2008). Conflict and user involvement in drug misuse treatment decision-making: a qualitative study. Substance abuse treatment, prevention, and policy, 3(1), 21. | UK | Individual interviews | User involvement | 79 clients in residential and community drug treatment agencies; 53 men and 26 women. | Thematic analysis | Develop our understanding of user involvement by examining the extent, causes, responses to, and outcomes of conflicts occurring between the clients and staff of drug treatment services. |
| Fischer, J., & Neale, J. (2008). Involving drug users in treatment decisions: An exploration of potential problems. Drugs: education, prevention and policy, 15(2), 161–175. | UK | Individual interviews | User involvement | Same as the above. | Thematic analysis | To investigate the problems that might specifically arise when involving drug users in making their ‘own’ treatment decisions. |
| Greer, A. M., Amlani, A., Burmeister, C., Scott, A., Newman, C., Lampkin, H., … & Buxton, J.A. (2019). Peer engagement barriers and enablers: insights from people who use drugs in British Columbia. Canadian Journal of Public Health 110(2), 227–235 | Canada | Peer-facilitated focus groups | Peer engagement | 83 participants who used illicit drugs, aged 18–64; 38 males, 30 females, 2 trans, and 13 unknown. | Thematic analysis, participatory coding | Examining the perspectives of people who use or have used illicit drugs (PWUD) on peer engagement in health and harm reduction settings across British Columbia (BC), Canada. |
| Hansen, I. L. S. (2018). Users’ choice in providing services to the most vulnerable homeless people. Social Inclusion, 6(3), 319–326. | Norway | Individual interviews | User’s choice/ self-determination | 16 participants in Housing First with severe substance use problems and mental illness; 13 men and 3 women, 9 aged 30–49, 6 over 50, and 1 under 30. | Thematic analysis | Discuss users’ experiences from participating in Housing First programs in Norway (provide a broad range of services, including various forms of practical assistance, help with personal finances, counselling, help establishing and maintaining contact with other social and health services, and coordination of service provision on an individual basis). |
| King, A. (2011). Service user involvement in methadone maintenance programmes: The ‘philosophy, the ideal and the reality’. Drugs: education, prevention and policy, 18(4), 276–284. | Ireland | Individual interviews | Service user involvement | 8 service users from different clinics, aged over 18. | Thematic content analysis | To explore user involvement processes within methadone maintenance programs, aiming to establish the degree to which partnership and collaboration exists between the users and providers of Irish drug treatment services. |
| Larsen, T., & Sagvaag, H. (2018). Empowerment and pathologization: A case study in Norwegian mental health and substance abuse services. Health Expectations, 21(6), 1231–1240. | Norway | Minutes, dialogue meetings, multistage focus group, individual interviews | Empowerment/decision-making | 6 patients in opioid maintenance treatment, (+ 5 co-researchers). | Content analysis, member-checking | To explore what may hinder patients’ voices being heard when collaborating with staff and leaders to improve services. |
| Laitila, M., Nikkonen, M., & Pietilä, A. M. (2011). Involvement in mental health and substance abuse work: conceptions of service users. Nursing research and practice, 2011. | Finland | Individual interviews | Service user involvement | 27 service users with experience from mental health and/or substance abuse services. (Snowball sample); 10 women and 17 men, 9 aged 31–50, 5 under 30, and 4 over 50. | Phenomenographic analysis | What are service users’ conceptions of SUI in mental health and substance abuse work? |
| Ness, O., Kvello, Ø., Borg, M., Semb, R., & Davidson, L. (2017). “Sorting things out together”: Young adults’ experiences of collaborative practices in mental health and substance use care. American Journal of Psychiatric Rehabilitation, 20(2), 126–142. | Norway | Individual interviews | Collaborative practice | 7 service users, 2 females and 5 males aged 20–30. | Thematic analysis | How do young adult service users with co-occurring mental health and substance use problems understand and describe collaborative practice with community mental health practitioners? |
| Patterson, S., Weaver, T., & Crawford, M. (2010). Drug service user groups: Only a partial solution to the problem of developing user involvement. Drugs: education, prevention and policy, 17(1), 84–97. | UK | Focus group interviews | User involvement | 78 participants in “user groups” aged 20 to 50, approximately 1/3 female. | Grounded theory | To investigate and describe the role of drug service user groups in local service user involvement (UI). |
| Patterson, S., Weaver, T., Agath, K., Albert, E., Rhodes, T., Rutter, D., & Crawford, M. (2009). ‘They can’t solve the problem without us’: a qualitative study of stakeholder perspectives on user involvement in drug treatment services in England. Health & social care in the community, 17(1), 54–62. | UK | Focus group interviews and individual interviews | User involvement | Same as the above. | Grounded theory | To develop a contextualised description of UI in drug treatment based upon an analysis of the experiences and perspectives of those commissioning, managing, providing and using services. |
| Rance, J., & Treloar, C. (2015). “We are people too”: Consumer participation and the potential transformation of therapeutic relations within drug treatment. International Journal of Drug Policy, 26(1), 30–36. | Australia | Individual interviews | Consumer participation | 30 consumers in three drug treatment facilities undergoing a participation project, aged 25–69. | Adaptive coding | What made such transformation possible? |
| Van Hout, M. C., & McElrath, K. (2012). Service user involvement in drug treatment programmes: Barriers to implementation and potential benefits for client recovery. Drugs: Education, Prevention and Policy, 19(6), 474–483. | Ireland/ UK | Individual interviews and field notes | Service user involvement | 12 service users from organizations providing services to individuals experiencing problem drug misuse. Age 20–60, reported 9 females and 2 males (!) | Thematic analysis | To investigate user and treatment provider perspectives of the nature and extent of service user involvement in the region, and explore the perceived benefits and limitations of implementing service user forum(s) in the region. |
| Hansen (2018) | Statements from Informants | Rance and Treloar (2015) | Statements from Informants | Næss et al. (2017) | Statements from Informants | Our Translation | Second-Order Analyses |
|---|---|---|---|---|---|---|---|
| Respect and acceptance | They have to listen to me! They see behind your behaviours, see the person in this. You feel worthy when you meet them, that you are of importance. | Recognized and acknowledged humanness, subjectivity | They can see that you know, you are human | Don’t fix me or judge me | It is crucial that I am met with respect and that the practitioner show that she care about me, not seeing me as merely a “number in the system.” | To be respected and recognized as a subject | User involvement as joint meaning-production |
| Joint reflection work (The analysis shows that the staff contribute with advice, guidance, questions, and opinions.) | Collaborative ethos | Everyone working together | Trusted partner to make stimulating reflections. | If the practitioners don’t know me, and they don’t ask me questions, but just give me advice or tell me what to do, that always make me do the opposite. | Joint meaning–production | ||
| Engaging in making choices is not always easy-appreciate the staff as partners or co-producers of decisions. | I think they can decide a little too, I am not very good at deciding. | Interaction | Enhanced opportunities for interaction | Someone to sort issues out with | Having good conversations with the practitioners helped me to clear my mind. If this didn’t happen, I just got stuck and overwhelmed with everything. | User involvement is about shared decisions |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Selseng, L.B.; Follevåg, B.-M.; Aaslund, H. How People with Lived Experiences of Substance Use Understand and Experience User Involvement in Substance Use Care: A Synthesis of Qualitative Studies. Int. J. Environ. Res. Public Health 2021, 18, 10219. https://doi.org/10.3390/ijerph181910219
Selseng LB, Follevåg B-M, Aaslund H. How People with Lived Experiences of Substance Use Understand and Experience User Involvement in Substance Use Care: A Synthesis of Qualitative Studies. International Journal of Environmental Research and Public Health. 2021; 18(19):10219. https://doi.org/10.3390/ijerph181910219
Chicago/Turabian StyleSelseng, Lillian Bruland, Brit-Marie Follevåg, and Håvard Aaslund. 2021. "How People with Lived Experiences of Substance Use Understand and Experience User Involvement in Substance Use Care: A Synthesis of Qualitative Studies" International Journal of Environmental Research and Public Health 18, no. 19: 10219. https://doi.org/10.3390/ijerph181910219
APA StyleSelseng, L. B., Follevåg, B.-M., & Aaslund, H. (2021). How People with Lived Experiences of Substance Use Understand and Experience User Involvement in Substance Use Care: A Synthesis of Qualitative Studies. International Journal of Environmental Research and Public Health, 18(19), 10219. https://doi.org/10.3390/ijerph181910219






