Effects of a Short Daytime Nap on the Cognitive Performance: A Systematic Review and Meta-Analysis
Abstract
1. Introduction
2. Methods
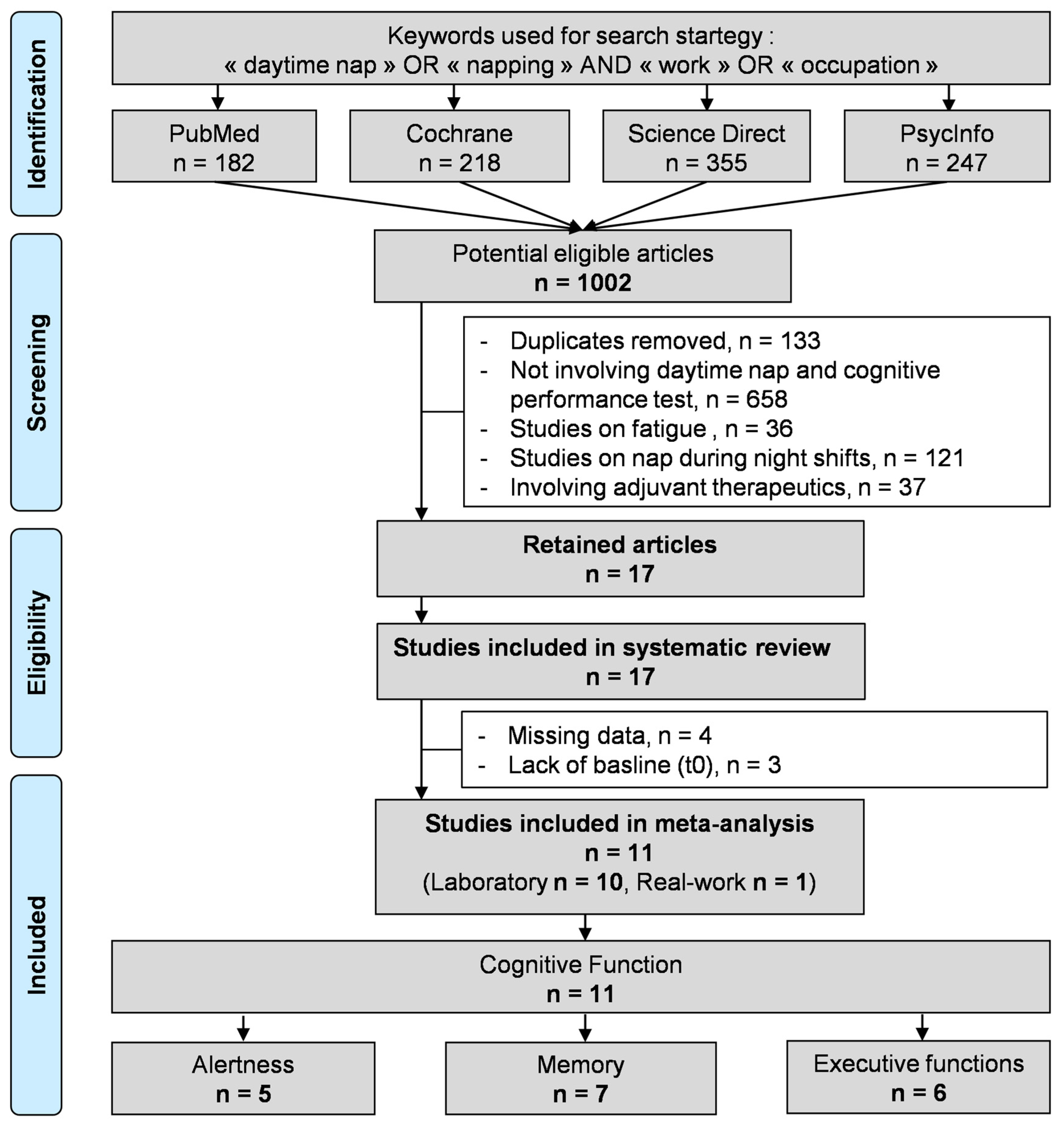
2.1. Literature Search
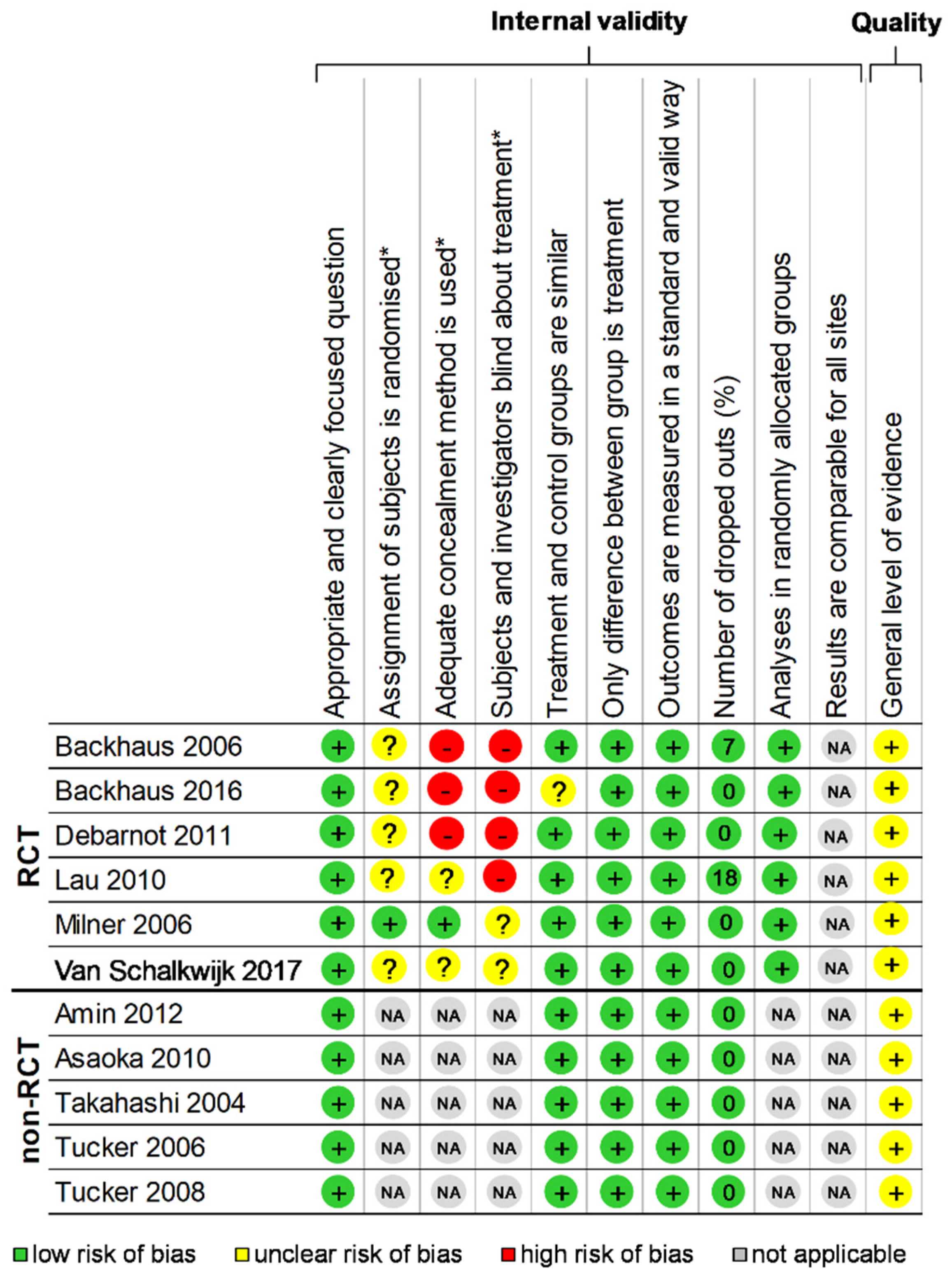
2.2. Quality of Assessment
2.3. Statistical Considerations
3. Results
3.1. Quality of Articles
3.2. Inclusion Criteria of Participants
3.3. Population
3.3.1. Sample Size
3.3.2. Sex
3.3.3. Age
3.3.4. Other
3.4. Aims and Outcomes of Included Articles
3.5. Study Designs
3.6. Characteristics of Intervention
3.7. Measurements of Cognitive Performance
3.8. Meta-Analysis on Performance between Groups at Baseline (t0) by Activity
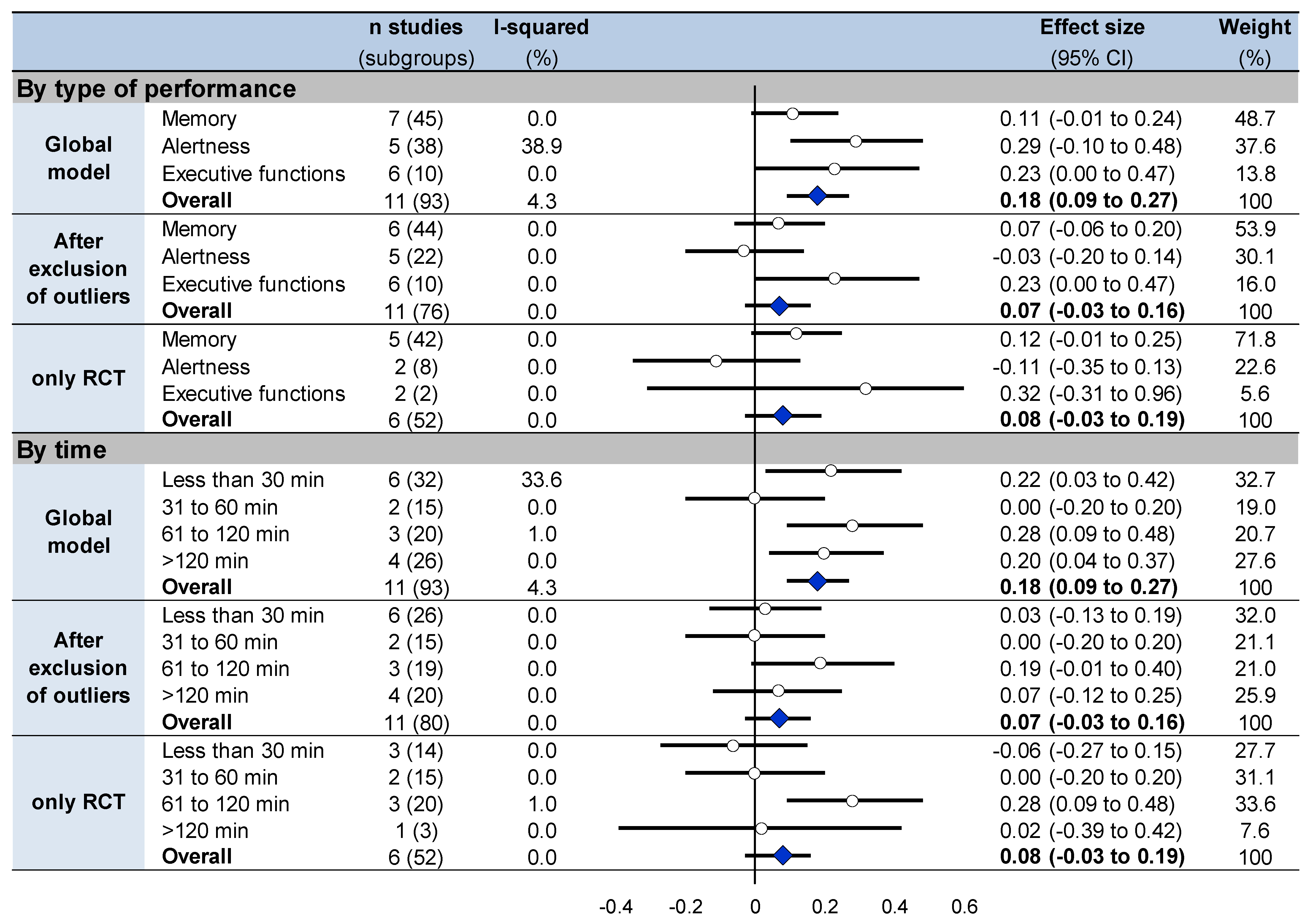
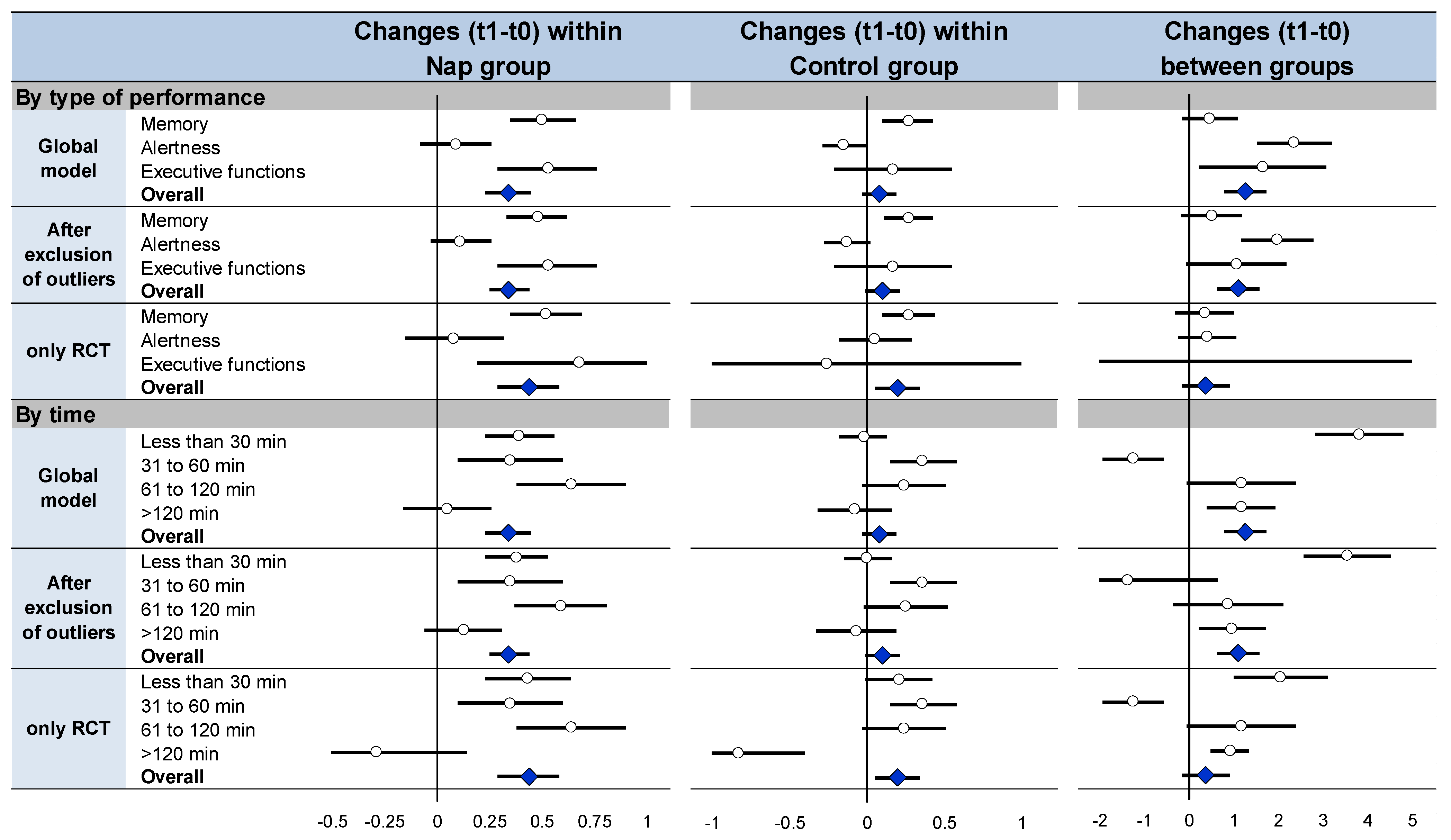
3.9. Meta-Analysis on Overall Effects of Nap between Groups
3.10. Sensitivity Analysis
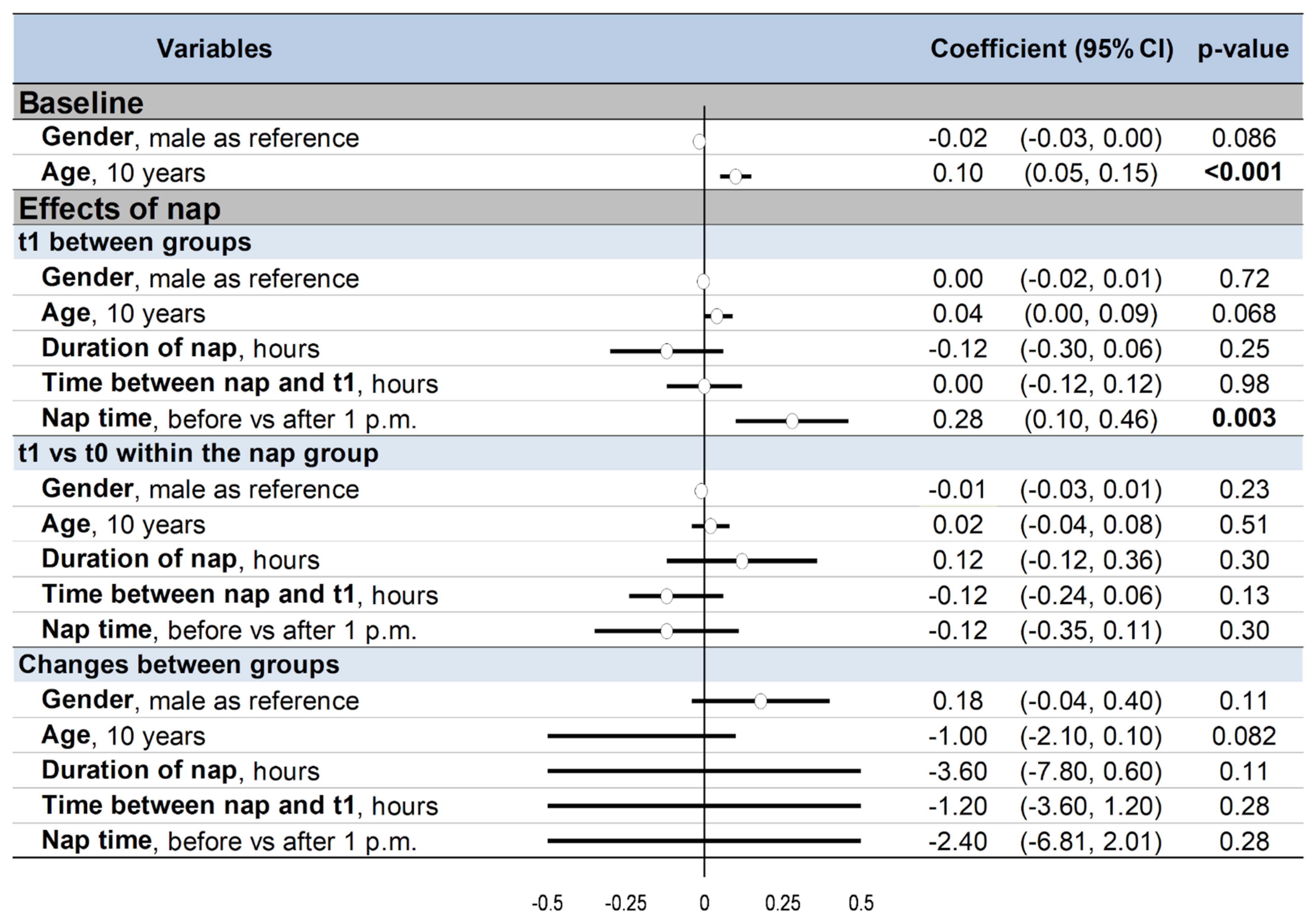
3.11. Metaregressions
4. Discussion
4.1. Nap and Cognitive Performance
4.2. Duration of Benefits and Sleep Inertia
4.3. Environmental and Individual Characteristics
4.4. Limitations
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Edenred. Baromètre Edenred-Ipsos 2016. In Comprendre et Améliorer le Bien-Être au Travail; Edenred: Malakoff, France, 2016. [Google Scholar]
- Organisation de Coopération et de Développement Economiques Level of GDP per Capita and Productivity. Available online: https://stats.oecd.org/Index.aspx?DataSetCode=PDB_LV (accessed on 18 February 2020).
- Kessler, R.C.; Berglund, P.A.; Coulouvrat, C.; Hajak, G.; Roth, T.; Shahly, V.; Shillington, A.C.; Stephenson, J.J.; Walsh, J.K. Insomnia and the Performance of US Workers: Results from the America Insomnia Survey. Sleep 2011, 34, 1161–1171. [Google Scholar] [CrossRef] [PubMed]
- Webb, W.; Dinges, D. Cultural perspectives on napping and the siesta. In Sleep and Alertness: Chronobiological, Behavioral and Medical Aspects of Napping; Raven Press: New York, NY, USA, 1989; pp. 247–265. [Google Scholar]
- Mullens, E. Apprendre à Faire la Sieste: Et si C’était un Médicament, 2nd ed.; Trédaniel: Paris, France, 2011. [Google Scholar]
- Lau, H.; Tucker, M.A.; Fishbein, W. Daytime Napping: Effects on Human Direct Associative and Relational Memory. Neurobiol. Learn Mem. 2010, 93, 554–560. [Google Scholar] [CrossRef] [PubMed]
- Comby, B. Préface de Jacques Chirac. In Eloge de la Sieste; J’ai lu: Paris, France, 2005. [Google Scholar]
- Faraut, B.; Andrillon, T.; Vecchierini, M.-F.; Leger, D. Napping: A Public Health Issue. From Epidemiological to Laboratory Studies. Sleep Med. Rev. 2017, 35, 85–100. [Google Scholar] [CrossRef] [PubMed]
- Maury, J.-P. République Populaire Chine, Constitution Chinoise. 1982. Available online: https://mjp.univ-perp.fr/constit/cn1982-0.htm (accessed on 23 October 2019).
- Williams, N.J.; Grandne, M.A.; Snipes, A.; Rogers, A.; Williams, O.; Airhihenbuwa, C.; Jean-Louis, G. Racial/Ethnic Disparities in Sleep Health and Health Care: Importance of the Sociocultural Context. Sleep Health 2015, 1, 28–35. [Google Scholar] [CrossRef]
- Rosekind, M.R.; Smith, R.M.; Miller, D.L.; Co, E.L.; Gregory, K.B.; Webbon, L.L.; Gander, P.H.; Lebacqz, J.V. Alertness Management: Strategic Naps in Operational Settings. J. Sleep Res. 1995, 4, 62–66. [Google Scholar] [CrossRef]
- Mednick, S.; Ehrman, M. Take Nap! Change Your Life; Workman Publishing: New York, NY, USA, 2006. [Google Scholar]
- Lahl, O.; Wispel, C.; Willigens, B.; Pietrowsky, R. An Ultra Short Episode of Sleep Is Sufficient to Promote Declarative Memory Performance. J. Sleep Res. 2008, 17, 3–10. [Google Scholar] [CrossRef]
- Igloi, K.; Gaggioni, G.; Sterpenich, V.; Schwartz, S. A Nap to Recap or How Reward Regulates Hippocampal-Prefrontal Memory Networks during Daytime Sleep in Humans. Elife 2015, 4, e07093. [Google Scholar] [CrossRef]
- Bonnet, M.H. The Effect of Varying Prophylactic Naps on Performance, Alertness and Mood throughout a 52-Hour Continuous Operation. Sleep 1991, 14, 307–315. [Google Scholar] [CrossRef]
- Dutheil, F.; Bessonnat, B.; Pereira, B.; Baker, J.S.; Moustafa, F.; Fantini, M.L.; Mermillod, M.; Navel, V. Napping and Cognitive Performance during Night Shifts: A Systematic Review and Meta-Analysis. Sleep 2020, 43, zsaa109. [Google Scholar] [CrossRef]
- Kubo, T.; Takeyama, H.; Matsumoto, S.; Ebara, T.; Murata, K.; Tachi, N.; Itani, T. Impact of Nap Length, Nap Timing and Sleep Quality on Sustaining Early Morning Performance. Ind. Health 2007, 45, 552–563. [Google Scholar] [CrossRef]
- Tietzel, A.J.; Lack, L.C. The Short-Term Benefits of Brief and Long Naps Following Nocturnal Sleep Restriction. Sleep 2001, 24, 293–300. [Google Scholar] [CrossRef]
- Lovato, N.; Lack, L. The effects of napping on cognitive functioning. In Progress in Brain Research; Kerkhof, G.A., van Dongen, H.P.A., Eds.; Elsevier: Amsterdam, The Netherlands, 2010; Volume 185, pp. 155–166. [Google Scholar]
- Huffington, A. The Sleep Revolution: Transforming Your Life, One Night at a Time; Harmony Hill: New York, NY, USA, 2017. [Google Scholar]
- Travers, J. Would You Like to Use a Sleep Pod at Work? Available online: https://www.labroots.com/trending/technology/7472/video-sleep-pod-work (accessed on 23 October 2019).
- La Siestoune Jacques. Available online: http://www.lasiestoune.com/jacques (accessed on 18 February 2020).
- Moher, D.; Hopewell, S.; Schulz, K.F.; Montori, V.; Gøtzsche, P.C.; Devereaux, P.J.; Elbourne, D.; Egger, M.; Altman, D.G. CONSORT 2010 Explanation and Elaboration: Updated Guidelines for Reporting Parallel Group Randomised Trials. BMJ 2010, 340, c869. [Google Scholar] [CrossRef] [PubMed]
- Vandenbroucke, J.P.; von Elm, E.; Altman, D.G.; Gøtzsche, P.C.; Mulrow, C.D.; Pocock, S.J.; Poole, C.; Schlesselman, J.J.; Egger, M. STROBE Initiative Strengthening the Reporting of Observational Studies in Epidemiology (STROBE): Explanation and Elaboration. Int. J. Surg. 2014, 12, 1500–1524. [Google Scholar] [CrossRef] [PubMed]
- Scottish Intercollegiate Guidelines Network (SIGN) Critical Appraisal Notes and Checklists. Available online: https://www.sign.ac.uk/checklists-and-notes (accessed on 23 October 2019).
- Benoist d’Azy, C.; Pereira, B.; Chiambaretta, F.; Dutheil, F. Efficacy of Different Procedures of Intra-Corneal Ring Segment Implantation in Keratoconus: A Systematic Review and Meta-Analysis. Transl. Vis. Sci. Technol. 2019, 8, 38. [Google Scholar] [CrossRef] [PubMed]
- Benoist d’Azy, C.; Pereira, B.; Naughton, G.; Chiambaretta, F.; Dutheil, F. Antibioprophylaxis in Prevention of Endophthalmitis in Intravitreal Injection: A Systematic Review and Meta-Analysis. PLoS ONE 2016, 11, e0156431. [Google Scholar] [CrossRef]
- Benoist d’Azy, C.; Pereira, B.; Chiambaretta, F.; Dutheil, F. Oxidative and Anti-Oxidative Stress Markers in Chronic Glaucoma: A Systematic Review and Meta-Analysis. PLoS ONE 2016, 11, e0166915. [Google Scholar] [CrossRef]
- Courtin, R.; Pereira, B.; Naughton, G.; Chamoux, A.; Chiambaretta, F.; Lanhers, C.; Dutheil, F. Prevalence of Dry Eye Disease in Visual Display Terminal Workers: A Systematic Review and Meta-Analysis. BMJ Open 2016, 6, e009675. [Google Scholar] [CrossRef] [PubMed]
- Lanhers, C.; Pereira, B.; Naughton, G.; Trousselard, M.; Lesage, F.-X.; Dutheil, F. Creatine Supplementation and Lower Limb Strength Performance: A Systematic Review and Meta-Analyses. Sports Med. 2015, 45, 1285–1294. [Google Scholar] [CrossRef]
- Lanhers, C.; Pereira, B.; Naughton, G.; Trousselard, M.; Lesage, F.-X.; Dutheil, F. Creatine Supplementation and Upper Limb Strength Performance: A Systematic Review and Meta-Analysis. Sports Med. 2017, 47, 163–173. [Google Scholar] [CrossRef]
- Navel, V.; Mulliez, A.; Benoist d’Azy, C.; Baker, J.S.; Malecaze, J.; Chiambaretta, F.; Dutheil, F. Efficacy of Treatments for Demodex Blepharitis: A Systematic Review and Meta-Analysis. Ocul. Surf. 2019, 17, 655–669. [Google Scholar] [CrossRef]
- Ollier, M.; Chamoux, A.; Naughton, G.; Pereira, B.; Dutheil, F. Chest CT Scan Screening for Lung Cancer in Asbestos Occupational Exposure: A Systematic Review and Meta-Analysis. Chest 2014, 145, 1339–1346. [Google Scholar] [CrossRef]
- DerSimonian, R.; Laird, N. Meta-Analysis in Clinical Trials. Control Clin. Trials 1986, 7, 177–188. [Google Scholar] [CrossRef]
- Russo, M.W. How to Review a Meta-Analysis. Gastroenterol. Hepatol. 2007, 3, 637–642. [Google Scholar]
- Christy, A.; Divya, M.; Saravanan, A.; Vadivel, S.; Jaiganesh, K. A Study on the Impact of Daytime Nap on Declarative Memory in Young Adults. Asian J. Pharm. Clin. Res. 2015, 1, 161–163. [Google Scholar]
- Hayashi, M.; Watanabe, M.; Hori, T. The Effects of a 20 Min Nap in the Mid-Afternoon on Mood, Performance and EEG Activity. Clin. Neurophysiol. 1999, 110, 272–279. [Google Scholar] [CrossRef]
- Hayashi, M.; Ito, S.; Hori, T. The Effects of a 20-Min Nap at Noon on Sleepiness, Performance and EEG Activity. Int. J. Psychophysiol. 1999, 32, 173–180. [Google Scholar] [CrossRef]
- Abdessalem, R.; Boukhris, O.; Hsouna, H.; Trabelsi, K.; Ammar, A.; Taheri, M.; Irandoust, K.; Hill, D.W.; Chtourou, H. Effect of Napping Opportunity at Different Times of Day on Vigilance and Shuttle Run Performance. Chronobiol. Int. 2019, 36, 1334–1342. [Google Scholar] [CrossRef]
- Lau, H.; Alger, S.E.; Fishbein, W. Relational Memory: A Daytime Nap Facilitates the Abstraction of General Concepts. PLoS ONE 2011, 6, e27139. [Google Scholar] [CrossRef]
- Amin, M.M.; Graber, M.; Ahmad, K.; Manta, D.; Hossain, S.; Belisova, Z.; Cheney, W.; Gold, M.S.; Gold, A.R. The Effects of a Mid-Day Nap on the Neurocognitive Performance of First-Year Medical Residents: A Controlled Interventional Pilot Study. Acad. Med. 2012, 87, 1428–1433. [Google Scholar] [CrossRef]
- Asaoka, S.; Masaki, H.; Ogawa, K.; Murphy, T.I.; Fukuda, K.; Yamazaki, K. Performance Monitoring during Sleep Inertia after a 1-h Daytime Nap. J. Sleep Res. 2010, 19, 436–443. [Google Scholar] [CrossRef]
- Backhaus, J.; Junghanns, K. Daytime Naps Improve Procedural Motor Memory. Sleep Med. 2006, 7, 508–512. [Google Scholar] [CrossRef]
- Backhaus, W.; Braass, H.; Renné, T.; Gerloff, C.; Hummel, F.C. Motor Performance Is Not Enhanced by Daytime Naps in Older Adults. Front. Aging Neurosci. 2016, 8, 125. [Google Scholar] [CrossRef] [PubMed]
- Debarnot, U.; Castellani, E.; Valenza, G.; Sebastiani, L.; Guillot, A. Daytime Naps Improve Motor Imagery Learning. Cogn. Affect. Behav. Neurosci. 2011, 11, 541–550. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Milner, C.E.; Fogel, S.M.; Cote, K.A. Habitual Napping Moderates Motor Performance Improvements Following a Short Daytime Nap. Biol. Psychol. 2006, 73, 141–156. [Google Scholar] [CrossRef] [PubMed]
- Takahashi, M.; Nakata, A.; Haratani, T.; Ogawa, Y.; Arito, H. Post-Lunch Nap as a Worksite Intervention to Promote Alertness on the Job. Ergonomics 2004, 47, 1003–1013. [Google Scholar] [CrossRef] [PubMed]
- Tucker, M.A.; Hirota, Y.; Wamsley, E.J.; Lau, H.; Chaklader, A.; Fishbein, W. A Daytime Nap Containing Solely Non-REM Sleep Enhances Declarative but Not Procedural Memory. Neurobiol. Learn Mem. 2006, 86, 241–247. [Google Scholar] [CrossRef]
- Tucker, M.A.; Fishbein, W. Enhancement of Declarative Memory Performance Following a Daytime Nap Is Contingent on Strength of Initial Task Acquisition. Sleep 2008, 31, 197–203. [Google Scholar] [CrossRef]
- Van Schalkwijk, F.J.; Sauter, C.; Hoedlmoser, K.; Heib, D.P.J.; Klösch, G.; Moser, D.; Gruber, G.; Anderer, P.; Zeitlhofer, J.; Schabus, M. The Effect of Daytime Napping and Full-Night Sleep on the Consolidation of Declarative and Procedural Information. J. Sleep Res. 2019, 28, e12649. [Google Scholar] [CrossRef]
- Dinges, D. Napping patterns and effects in human adults. In Sleep and Alertness: Chronobiological, Behavioural, and Medical Aspects of Napping; Raven Press: New York, NY, USA, 1989; pp. 171–204. [Google Scholar]
- Broughton, R.; Dinges, D. Napping: A ubiquitous enigma. In Sleep and Alertness: Chronobiological, Behavioural, and Medical Aspects of Napping; Raven Press: New York, NY, USA, 1989; pp. 1–7. [Google Scholar]
- Horne, J.A.; Reyner, L.A. Counteracting Driver Sleepiness: Effects of Napping, Caffeine, and Placebo. Psychophysiology 1996, 33, 306–309. [Google Scholar] [CrossRef]
- Taub, J.M.; Tanguay, P.E.; Rosa, R.R. Effects of Afternoon Naps on Physiological Variables Performance and Self-Reported Activation. Biol. Psychol. 1977, 5, 191–210. [Google Scholar] [CrossRef]
- Milner, C.E.; Cote, K.A. Benefits of Napping in Healthy Adults: Impact of Nap Length, Time of Day, Age, and Experience with Napping. J. Sleep Res. 2009, 18, 272–281. [Google Scholar] [CrossRef]
- Cajochen, C.; Knoblauch, V.; Wirz-Justice, A.; Kräuchi, K.; Graw, P.; Wallach, D. Circadian Modulation of Sequence Learning under High and Low Sleep Pressure Conditions. Behav. Brain Res. 2004, 151, 167–176. [Google Scholar] [CrossRef]
- Ficca, G.; Axelsson, J.; Mollicone, D.J.; Muto, V.; Vitiello, M.V. Naps, Cognition and Performance. Sleep Med. Rev. 2010, 14, 249–258. [Google Scholar] [CrossRef]
- Sugawara, S.K.; Koike, T.; Kawamichi, H.; Makita, K.; Hamano, Y.H.; Takahashi, H.K.; Nakagawa, E.; Sadato, N. Qualitative Differences in Offline Improvement of Procedural Memory by Daytime Napping and Overnight Sleep: An FMRI Study. Neurosci. Res. 2018, 132, 37–45. [Google Scholar] [CrossRef]
- Cai, D.J.; Mednick, S.A.; Harrison, E.M.; Kanady, J.C.; Mednick, S.C. REM, Not Incubation, Improves Creativity by Priming Associative Networks. Proc. Natl. Acad. Sci. USA 2009, 106, 10130–10134. [Google Scholar] [CrossRef]
- Whitehurst, L.N.; Cellini, N.; McDevitt, E.A.; Duggan, K.A.; Mednick, S.C. Autonomic Activity during Sleep Predicts Memory Consolidation in Humans. Proc. Natl. Acad. Sci. USA 2016, 113, 7272–7277. [Google Scholar] [CrossRef]
- Baxter, V.; Kroll-Smith, S. Normalizing the Workplace Nap: Blurring the Boundaries between Public and Private Space and Time. Curr. Sociol. 2005, 53, 33–55. [Google Scholar] [CrossRef]
- Boukhris, O.; Abdessalem, R.; Ammar, A.; Hsouna, H.; Trabelsi, K.; Engel, F.A.; Sperlich, B.; Hill, D.W.; Chtourou, H. Nap Opportunity During the Daytime Affects Performance and Perceived Exertion in 5-m Shuttle Run Test. Front. Physiol. 2019, 10, 779. [Google Scholar] [CrossRef] [PubMed]
- Macchi, M.M.; Boulos, Z.; Ranney, T.; Simmons, L.; Campbell, S.S. Effects of an Afternoon Nap on Nighttime Alertness and Performance in Long-Haul Drivers. Accid. Anal. Prev. 2002, 34, 825–834. [Google Scholar] [CrossRef]
- Purnell, M.T.; Feyer, A.-M.; Herbison, G.P. The Impact of a Nap Opportunity during the Night Shift on the Performance and Alertness of 12-h Shift Workers. J. Sleep Res. 2002, 11, 219–227. [Google Scholar] [CrossRef] [PubMed]
- Takahashi, M.; Arito, H. Maintenance of Alertness and Performance by a Brief Nap after Lunch under Prior Sleep Deficit. Sleep 2000, 23, 813–819. [Google Scholar] [CrossRef] [PubMed]
- Brindle, R.C.; Conklin, S.M. Daytime Sleep Accelerates Cardiovascular Recovery after Psychological Stress. Int. J. Behav. Med. 2012, 19, 111–114. [Google Scholar] [CrossRef] [PubMed]
- Naska, A.; Oikonomou, E.; Trichopoulou, A.; Psaltopoulou, T.; Trichopoulos, D. Siesta in Healthy Adults and Coronary Mortality in the General Population. Arch. Intern. Med. 2007, 167, 296–301. [Google Scholar] [CrossRef] [PubMed]
- Brooks, A.; Lack, L. A Brief Afternoon Nap Following Nocturnal Sleep Restriction: Which Nap Duration Is Most Recuperative? Sleep 2006, 29, 831–840. [Google Scholar] [CrossRef]
- Tietzel, A.J.; Lack, L.C. The Recuperative Value of Brief and Ultra-Brief Naps on Alertness and Cognitive Performance. J. Sleep Res. 2002, 11, 213–218. [Google Scholar] [CrossRef]
- Dinges, D. Sleep inertia. In Encyclopedia of Sleep and Dreaming; Greenwood: Toronto, ON, Canada, 1993; pp. 553–554. [Google Scholar]
- Hilditch, C.J.; Dorrian, J.; Banks, S. A Review of Short Naps and Sleep Inertia: Do Naps of 30 Min or Less Really Avoid Sleep Inertia and Slow-Wave Sleep? Sleep Med. 2017, 32, 176–190. [Google Scholar] [CrossRef]
- Tassi, P.; Muzet, A. Sleep Inertia. Sleep Med. Rev. 2000, 4, 341–353. [Google Scholar] [CrossRef]
- Ogilvie, R.; Broughton, R. Sleep, Arousal and Performance: Problems and Promises; Birkhauser: Boston, MA, USA, 1991. [Google Scholar]
- Dinges, D.; Orne, M.; Orne, E. Sleep Depth and Other Factors Associated with Performance upon Abrupt Awakening. Sleep Res. 1985, 14, 92. [Google Scholar]
- Muzet, A.; Nicolas, A.; Tassi, P.; Dewasmes, G.; Bonneau, A. Implementation of Napping in Industry and the Problem of Sleep Inertia. J. Sleep Res. 1995, 4, 67–69. [Google Scholar] [CrossRef]
- Scheer, F.; Shea, T.; Hilton, M.; Shea, S. An Endogenous Circadian Rhythm in Sleep Inertia Results in Greatest Cognitive Impairment up on Awakening during the Biological Night. J. Biol. Rythms 2008, 23, 353–361. [Google Scholar] [CrossRef]
- Dinges, D.; Whitehouse, W.; Orne, E.; Orne, M. The Benefits of a Nap during Prolonged Work and Wakefulness. Work Stress 1988, 2, 139–153. [Google Scholar] [CrossRef]
- Blackwell, T.; Yaffe, K.; Ancoli-Israel, S.; Schneider, J.L.; Cauley, J.A.; Hillier, T.A.; Fink, H.A.; Stone, K.L. Study of Osteoporotic Fractures Group Poor Sleep Is Associated with Impaired Cognitive Function in Older Women: The Study of Osteoporotic Fractures. J. Gerontol. A Biol. Sci. Med. Sci. 2006, 61, 405–410. [Google Scholar] [CrossRef]
- McCrae, C.S.; Rowe, M.A.; Dautovich, N.D.; Lichstein, K.L.; Durrence, H.H.; Riedel, B.W.; Taylor, D.J.; Bush, A.J. Sleep Hygiene Practices in Two Community Dwelling Samples of Older Adults. Sleep 2006, 29, 1551–1560. [Google Scholar] [CrossRef]
- Stone, K.L.; Ewing, S.K.; Lui, L.-Y.; Ensrud, K.E.; Ancoli-Israel, S.; Bauer, D.C.; Cauley, J.A.; Hillier, T.A.; Cummings, S.R. Self-Reported Sleep and Nap Habits and Risk of Falls and Fractures in Older Women: The Study of Osteoporotic Fractures. J. Am. Geriatr. Soc. 2006, 54, 1177–1183. [Google Scholar] [CrossRef]
- Vitiello, M.; Foley, D. Predictors of Planned and Unplanned Napping in Older Adults. Sleep 2007, 30, 105–106. [Google Scholar]
- Liu, X.; Liu, L. Sleep Habits and Insomnia in a Sample of Elderly Persons in China. Sleep 2006, 28, 1579–1587. [Google Scholar] [CrossRef]
- Brassington, G.S.; King, A.C.; Bliwise, D.L. Sleep Problems as a Risk Factor for Falls in a Sample of Community-Dwelling Adults Aged 64-99 Years. J. Am. Geriatr. Soc. 2000, 48, 1234–1240. [Google Scholar] [CrossRef]
- Bursztyn, M.; Ginsberg, G.; Hammerman-Rozenberg, R.; Stessman, J. The Siesta in the Elderly: Risk Factor for Mortality? Arch. Intern. Med. 1999, 159, 1582–1586. [Google Scholar] [CrossRef] [PubMed]
- Newman, A.B.; Spiekerman, C.F.; Enright, P.; Lefkowitz, D.; Manolio, T.; Reynolds, C.F.; Robbins, J. Daytime Sleepiness Predicts Mortality and Cardiovascular Disease in Older Adults. The Cardiovascular Health Study Research Group. J. Am. Geriatr. Soc. 2000, 48, 115–123. [Google Scholar] [CrossRef] [PubMed]
- Bursztyn, M.; Ginsberg, G.; Stessman, J. The Siesta and Mortality in the Elderly: Effect of Rest without Sleep and Daytime Sleep Duration. Sleep 2002, 25, 187–191. [Google Scholar] [CrossRef] [PubMed]
- Bursztyn, M.; Stessman, J. The Siesta and Mortality: Twelve Years of Prospective Observations in 70-Year-Olds. Sleep 2005, 28, 345–347. [Google Scholar] [PubMed]
- Naitoh, P.; Angus, R. Napping and human functioning during prolonged work. In Sleep and Alertness: Chronobiological, Behavioral and Medical Aspects of Napping; Raven Press: New York, NY, USA, 1989; pp. 221–246. [Google Scholar]
- Taub, J.; Hawkins, D.; van de Castle, R. Temporal Relationships of Napping Behaviour to Performance, Mood States and Sleep Physiology. Sleep Res. 1978, 7, 164. [Google Scholar]
- Mullens, E. Physiologie de La Somnolence. Available online: http://eric.mullens.free.fr/somn_f.htm (accessed on 23 October 2019).
- Blake, M.J.F. Time of Day Effects on Performance in a Range of Tasks. Psychon. Sci. 1967, 9, 349–350. [Google Scholar] [CrossRef]
- Broughton, R. Chronobiological aspects and models of sleep and napping. In Sleep and Alertness: Chronobiological, Behavioral and Medical Aspects of Napping; Raven Press: New York, NY, USA, 1989; pp. 71–98. [Google Scholar]
- Lavie, P. To nap, perchance to sleep-ultradian aspects Ž. of napping. In Sleep and Alertness: Chronobiological, Behavioral, and Medical Aspects of Napping; Raven Press: New York, NY, USA, 1989; pp. 99–120. [Google Scholar]
- Ohayon, M.M.; Zulley, J. Prevalence of Naps in the General Population. Sleep Hypn. 1999, 1, 88–97. [Google Scholar]
- Buysse, D.J.; Browman, K.E.; Monk, T.H.; Reynolds, C.F.; Fasiczka, A.L.; Kupfer, D.J. Napping and 24-Hour Sleep/Wake Patterns in Healthy Elderly and Young Adults. J. Am. Geriatr. Soc. 1992, 40, 779–786. [Google Scholar] [CrossRef]
- Foley, D.J.; Vitiello, M.V.; Bliwise, D.L.; Ancoli-Israel, S.; Monjan, A.A.; Walsh, J.K. Frequent Napping Is Associated with Excessive Daytime Sleepiness, Depression, Pain, and Nocturia in Older Adults: Findings from the National Sleep Foundation “2003 Sleep in America” Poll. Am. J. Geriatr. Psychiatry 2007, 15, 344–350. [Google Scholar] [CrossRef]
- Ohayon, M.M. Epidemiology of Insomnia: What We Know and What We Still Need to Learn. Sleep Med. Rev. 2002, 6, 97–111. [Google Scholar] [CrossRef]
- Ohayon, M.M.; Carskadon, M.A.; Guilleminault, C.; Vitiello, M.V. Meta-Analysis of Quantitative Sleep Parameters from Childhood to Old Age in Healthy Individuals: Developing Normative Sleep Values across the Human Lifespan. Sleep 2004, 27, 1255–1273. [Google Scholar] [CrossRef]
- Monk, T.H. Aging Human Circadian Rhythms: Conventional Wisdom May Not Always Be Right. J. Biol. Rhythm. 2005, 20, 366–374. [Google Scholar] [CrossRef]
- Wang, B.; Fu, X. Gender Difference in the Effect of Daytime Sleep on Declarative Memory for Pictures. J. Zhejiang Univ. Sci. B 2009, 10, 536–546. [Google Scholar] [CrossRef] [PubMed]
- Van Dongen, H.P.A. Sleep Deprivation, Stimulant Medications, and Cognition. Sleep 2015, 38, 1145–1146. [Google Scholar] [CrossRef][Green Version]
- Stone, D.; Rosopa, P. The Advantages and Limitations of Using Meta-Analysis in Human Resource Management Research. Hum. Resour. Manag. Rev. 2017, 27, 1–7. [Google Scholar] [CrossRef]
- Rosenthal, R. Meta-Analytic Procedures for Social Research; Sage Publications, Inc.: Thousand Oaks, CA, USA, 1991; ISBN 978-0-8039-4245-5. [Google Scholar]
- Cooper, H.; Hedges, L.V. The Handbook of Research Synthesis, 2nd ed.; Russell Sage Foundation: New York, NY, USA, 2008; ISBN 978-0-87154-163-5. [Google Scholar]
- Bobko, P.; Stone-Romero, E. Meta-Analysis May Be another Useful Research Tool, but It Is Not a Panacea. Res. Pers. Hum. Resour. Manag. 1998, 16, 359–397. [Google Scholar]
- Sterne, J.; Harbord, R. Funnel Plots in Meta-Analysis. Stata J. 2004, 4, 127–141. [Google Scholar] [CrossRef]
- Patino, C.M.; Ferreira, J.C. Internal and External Validity: Can You Apply Research Study Results to Your Patients? J. Bras. Pneumol. 2018, 44, 183. [Google Scholar] [CrossRef]

Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Dutheil, F.; Danini, B.; Bagheri, R.; Fantini, M.L.; Pereira, B.; Moustafa, F.; Trousselard, M.; Navel, V. Effects of a Short Daytime Nap on the Cognitive Performance: A Systematic Review and Meta-Analysis. Int. J. Environ. Res. Public Health 2021, 18, 10212. https://doi.org/10.3390/ijerph181910212
Dutheil F, Danini B, Bagheri R, Fantini ML, Pereira B, Moustafa F, Trousselard M, Navel V. Effects of a Short Daytime Nap on the Cognitive Performance: A Systematic Review and Meta-Analysis. International Journal of Environmental Research and Public Health. 2021; 18(19):10212. https://doi.org/10.3390/ijerph181910212
Chicago/Turabian StyleDutheil, Frédéric, Benjamin Danini, Reza Bagheri, Maria Livia Fantini, Bruno Pereira, Farès Moustafa, Marion Trousselard, and Valentin Navel. 2021. "Effects of a Short Daytime Nap on the Cognitive Performance: A Systematic Review and Meta-Analysis" International Journal of Environmental Research and Public Health 18, no. 19: 10212. https://doi.org/10.3390/ijerph181910212
APA StyleDutheil, F., Danini, B., Bagheri, R., Fantini, M. L., Pereira, B., Moustafa, F., Trousselard, M., & Navel, V. (2021). Effects of a Short Daytime Nap on the Cognitive Performance: A Systematic Review and Meta-Analysis. International Journal of Environmental Research and Public Health, 18(19), 10212. https://doi.org/10.3390/ijerph181910212








