Of Pandemics and Zombies: The Influence of Prior Concepts on COVID-19 Pandemic-Related Behaviors
Abstract
1. Introduction
1.1. Research on Human Concepts
1.2. Concepts in the Time of COVID-19
1.3. The Current Experiment
2. Methods
2.1. Participants
2.2. Materials
2.2.1. Category Similarity Measures
2.2.2. COVID-19 Behavioral Response Measures
2.2.3. Controls for COVID-19 Behavioral Response Measures
2.3. Procedure
3. Results
3.1. Analysis Plan
3.2. Political Orientation and Perceived Self-Risk Control Measures
3.3. Relationship between Categories and Health Behaviors
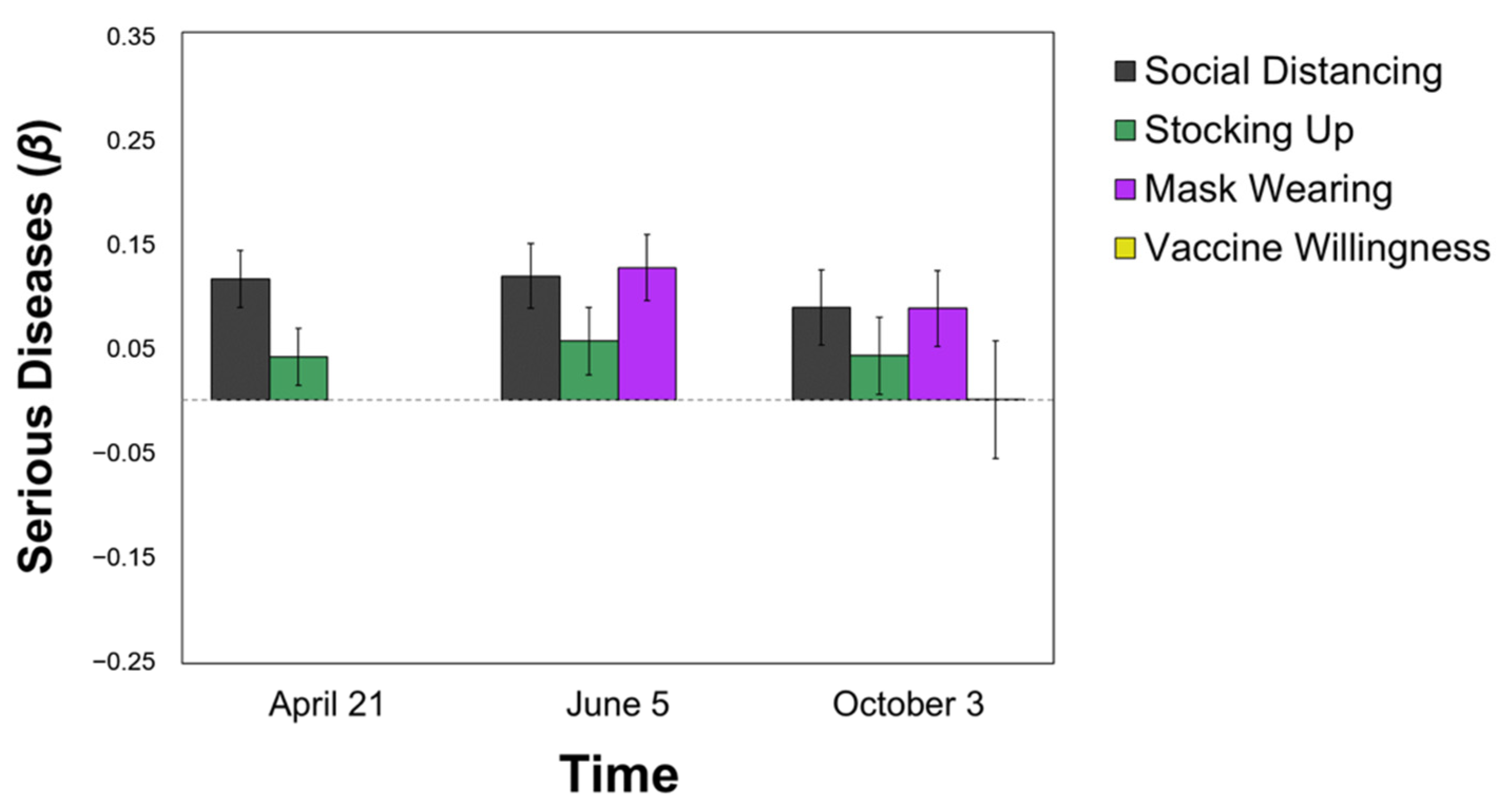
3.3.1. Serious Diseases
3.3.2. Normal Flu
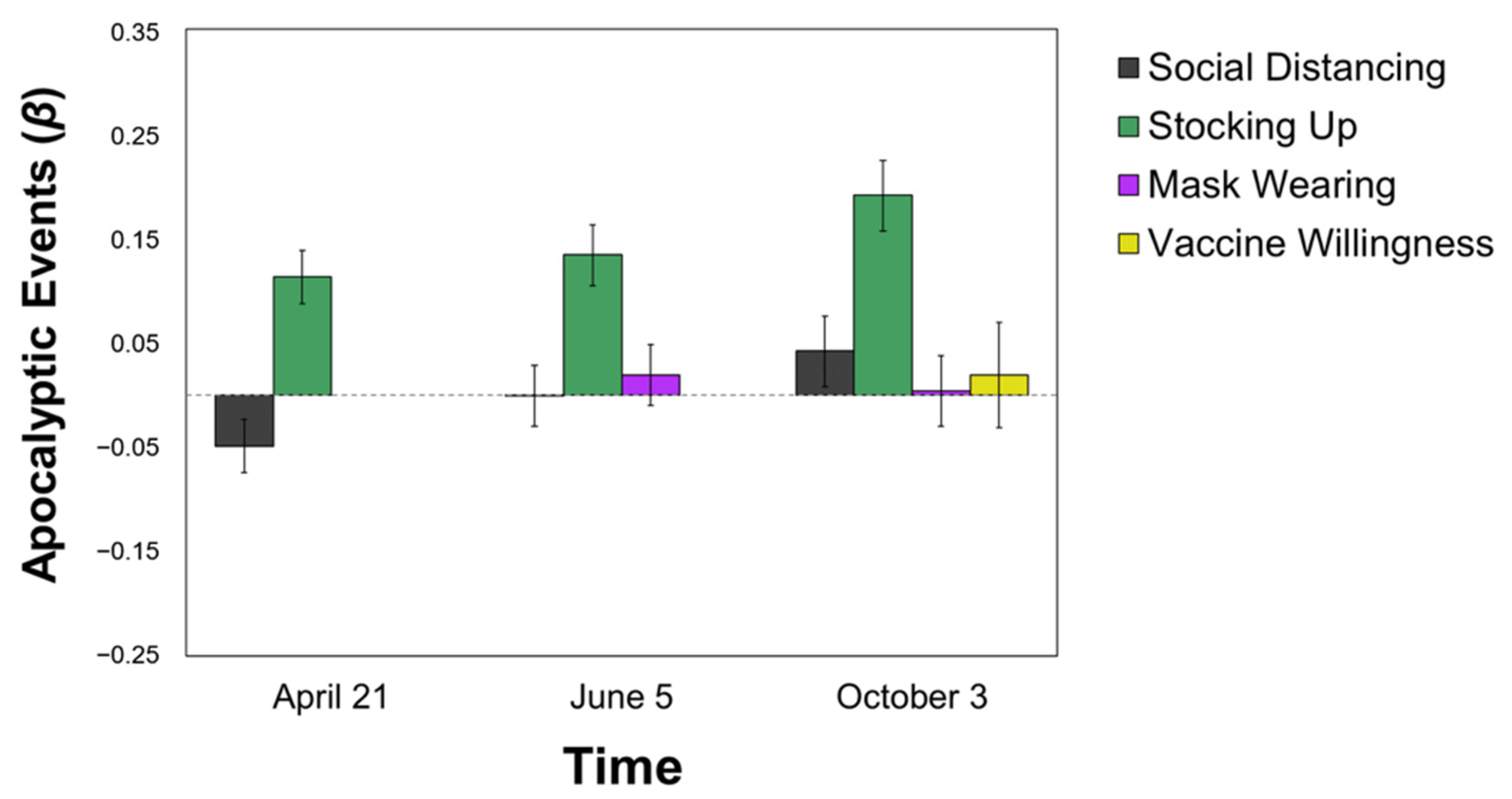
3.3.3. Apocalyptic Events
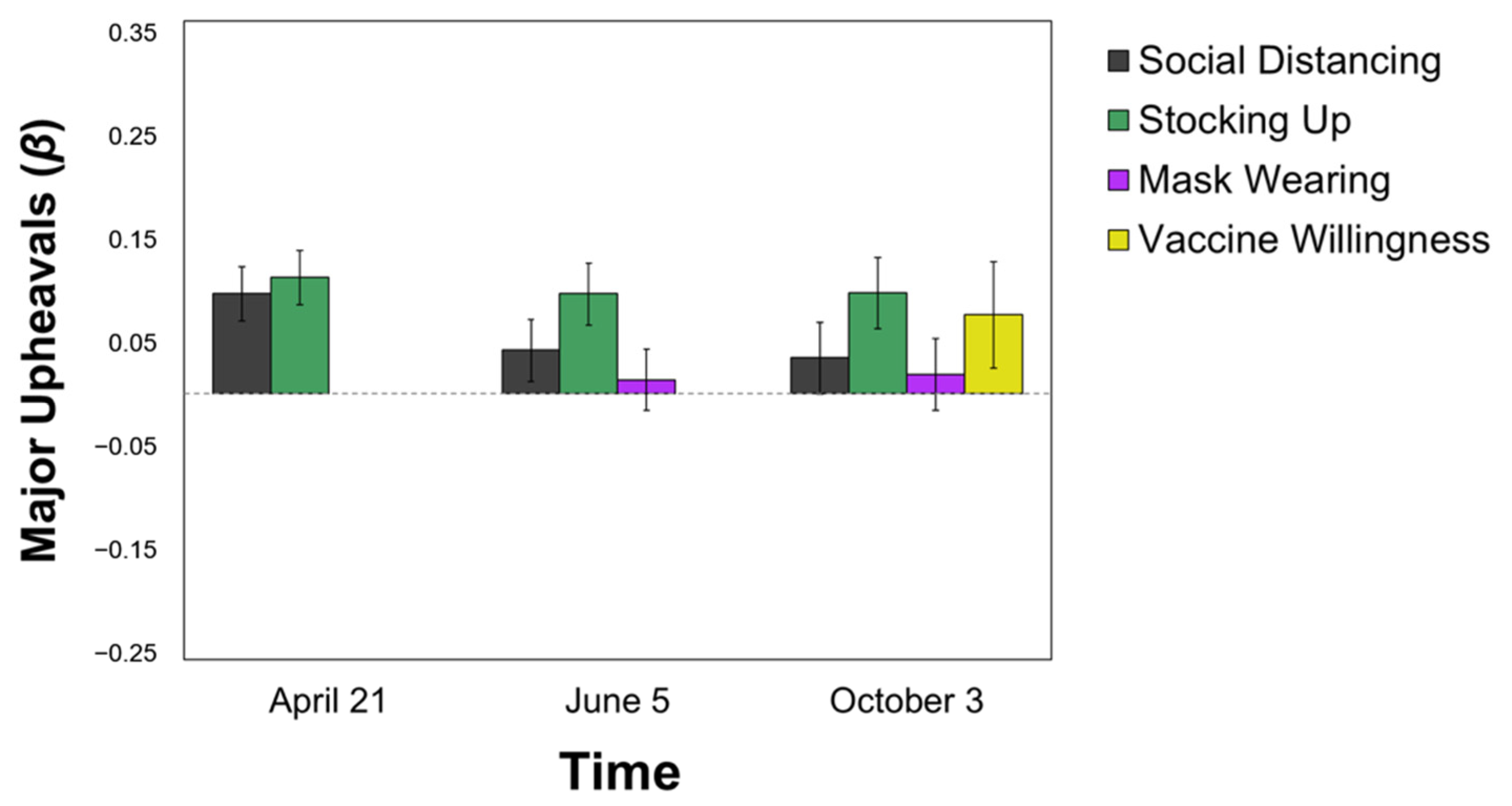
3.3.4. Major Upheavals
4. Discussion
4.1. Implications for Research on Human Concepts
4.2. Implications for Public Health
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
Appendix A. Creation of Category Similarity Scales
Appendix A.1. Selecting Category Comparisons
Appendix A.2. Supporting Factor Analysis
References
- World Health Organization Listings of WHO’s Response to COVID-19. Available online: https://www.who.int/news/item/29-06-2020-covidtimeline (accessed on 21 January 2021).
- Beer, T. All the Times Trump Compared COVID-19 to the Flu, Even after He Knew COVID-19 Was Far More Deadly. Available online: https://www.forbes.com/sites/tommybeer/2020/09/10/all-the-times-trump-compared-covid-19-to-the-flu-even-after-he-knew-covid-19-was-far-more-deadly/?sh=2cb54bdef9d2 (accessed on 10 September 2020).
- Lovelace, B., Jr. Medical Historian Compares the Coronavirus to the 1918 Flu Pandemic: Both Were Highly Political. Available online: https://www.cnbc.com/2020/09/28/comparing-1918-flu-vs-coronavirus.html (accessed on 29 September 2020).
- Goldstone, R.L.; Kersten, A.; Carvalho, P.F. Categorization and Concepts. In Stevens’ Handbook of Experimental Psychology and Cognitive Neuroscience; Wixted, J., Ed.; Wiley: New York, NY, USA, 2018; Volume 3, pp. 275–317. ISBN 978-1-119-17017-4. [Google Scholar]
- Murphy, G.L. What are categories and concepts. In The Making of Human Concepts; Mareschal, D., Quinn, P., Lea, S., Eds.; Oxford University Press: Oxford, UK, 2010; pp. 11–28. [Google Scholar]
- Ashby, F.G.; Maddox, W.T. Human category learning. Annu. Rev. Psychol. 2004, 56, 149–178. [Google Scholar] [CrossRef]
- Kruschke, J.K. Category learning. In The Handbook of Cognition; Lamberts, K., Goldstone, R.L., Eds.; Sage: London, UK, 2005; pp. 183–201. [Google Scholar]
- Heit, E. Models of the effects of prior knowledge on category learning. J. Exp. Psychol. Learn. Mem. Cogn. 1994, 20, 1264–1282. [Google Scholar] [CrossRef]
- Tenenbaum, J.B.; Griffiths, T.L.; Kemp, C. Theory-based bayesian models of inductive learning and reasoning. Trends Cogn. Sci. 2006, 10, 309–318. [Google Scholar] [CrossRef] [PubMed]
- Barsalou, L.W. The human conceptual system. In The Cambridge Handbook of Psycholinguistics; Cambridge University Press: New York, NY, USA, 2012; pp. 239–258. ISBN 978-0-521-67792-9. [Google Scholar]
- Markman, A.B.; Ross, B.H. Category use and category learning. Psychol. Bull. 2003, 129, 592–613. [Google Scholar] [CrossRef]
- Chen, S.Y.; Ross, B.H.; Murphy, G.L. Implicit and explicit processes in category-based induction: Is induction best when we don’t think? J. Exp. Psychol. Gen. 2014, 143, 227–246. [Google Scholar] [CrossRef]
- Gelman, S.A.; Davidson, N.S. Conceptual influences on category-based induction. Cognit. Psychol. 2013, 66, 327–353. [Google Scholar] [CrossRef]
- Osherson, D.N.; Smith, E.E.; Wilkie, O.; López, A.; Shafir, E. Category-based induction. Psychol. Rev. 1990, 97, 185–200. [Google Scholar] [CrossRef]
- Waldmann, M.R.; Hagmayer, Y. Categories and causality: The neglected direction. Cognit. Psychol. 2006, 53, 27–58. [Google Scholar] [CrossRef]
- Markman, A.B.; Wisniewski, E.J. Similar and different: The differentiation of basic-level categories. J. Exp. Psychol. Learn. Mem. Cogn. 1997, 23, 54–70. [Google Scholar] [CrossRef]
- Rosch, E.; Mervis, C.B.; Gray, W.D.; Johnson, D.M.; Boyes-Braem, P. Basic objects in natural categories. Cognit. Psychol. 1976, 8, 382–439. [Google Scholar] [CrossRef]
- Johnson, K.E.; Mervis, C.B. Effects of varying levels of expertise on the basic level of categorization. J. Exp. Psychol. Gen. 1997, 126, 248–277. [Google Scholar] [CrossRef]
- Tanaka, J.W.; Taylor, M. Object categories and expertise: Is the basic level in the eye of the beholder? Cognit. Psychol. 1991, 23, 457–482. [Google Scholar] [CrossRef]
- Murphy, G.L.; Ross, B.H. Induction with cross-classified categories. Mem. Cognit. 1999, 27, 1024–1041. [Google Scholar] [CrossRef]
- Ross, B.H.; Murphy, G.L. Food for thought: Cross-classification and category organization in a complex real-world domain. Cognit. Psychol. 1999, 38, 495–553. [Google Scholar] [CrossRef]
- Frank, S.M.; Durden, T.E. Two approaches, one problem: Cultural constructions of Type II Diabetes in an indigenous community in Yucatán, Mexico. Soc. Sci. Med. 2017, 172, 64–71. [Google Scholar] [CrossRef]
- Marsh, J.K.; Ahn, W. Spontaneous assimilation of continuous values and temporal information in causal induction. J. Exp. Psychol. Learn. Mem. Cogn. 2009, 35, 334–352. [Google Scholar] [CrossRef]
- Medin, D.L.; Goldstone, R.L.; Gentner, D. Respects for similarity. Psychol. Rev. 1993, 100, 254–278. [Google Scholar] [CrossRef]
- Davis, T.; Lacour, M.; Goldwater, M.; Hughes, B.; Ireland, M.E.; Worthy, D.A.; Gaylord, N.; Van Allen, J. Communicating about diseases that originate in animals: Lessons from the psychology of inductive reasoning. Behav. Sci. Policy 2020, 6, 1–11. [Google Scholar]
- Hirani, S.P.; Newman, S.P. Patients’ beliefs about their cardiovascular disease. Heart 2005, 91, 1235–1239. [Google Scholar] [CrossRef]
- Senior, V.; Marteau, T.M.; Peters, T.J. Will genetic testing for predisposition for disease result in fatalism? A qualitative study of parents responses to neonatal screening for familial hypercholesterolaemia. Soc. Sci. Med. 1999, 48, 1857–1860. [Google Scholar] [CrossRef]
- Iselin, M.-G.; Addis, M.E. Effects of etiology on perceived helpfulness of treatments for depression. Cogn. Ther. Res. 2003, 27, 205–222. [Google Scholar] [CrossRef]
- Marsh, J.K.; Romano, A.L. Lay judgments of mental health treatment options: The mind versus body problem. Med. Decis. Mak. Policy Pract. 2016, 1, 2381468316669361. [Google Scholar] [CrossRef] [PubMed]
- Peters, D.; Menendez, D.; Rosengren, K. Reframing mental illness: The role of essentialism on perceived treatment efficacy and stigmatization. Mem. Cognit. 2020, 48, 1317–1333. [Google Scholar] [CrossRef] [PubMed]
- Colman, L.; Delaruelle, K.; Luypaert, C.; Verniest, R.; Bracke, P. Burdens in mental health recovery: Causal beliefs and their relation to stigma and help seeking recommendations. Int. J. Soc. Psychiatry 2020, 17, 0020764020973249. [Google Scholar] [CrossRef] [PubMed]
- Haslam, N.; Kvaale, E.P. Biogenetic explanations of mental disorder: The mixed-blessings model. Curr. Dir. Psychol. Sci. 2015, 24, 399–404. [Google Scholar] [CrossRef]
- Marsh, J.K.; Shanks, L.L. Thinking you can catch mental illness: How beliefs about membership attainment and category structure influence interactions with mental health category members. Mem. Cognit. 2014, 42, 1011–1025. [Google Scholar] [CrossRef]
- Ashby, F.G.; Valentin, V.V. Multiple systems of perceptual category learning: Theory and cognitive tests. In Handbook of Categorization in Cognitive Science; Cohen, H., Lefebvre, C., Eds.; Elsevier: San Diego, CA, USA, 2017; pp. 157–188. ISBN 978-0-08-101107-2. [Google Scholar]
- Murphy, G. The Big Book of Concepts; MIT Press: Cambridge, MA, USA, 2002; ISBN 0-262-25006-3. [Google Scholar]
- Seger, C.A.; Miller, E.K. Category learning in the brain. Annu. Rev. Neurosci. 2010, 33, 203–219. [Google Scholar] [CrossRef]
- Murphy, G.L.; Medin, D.L. The role of theories in conceptual coherence. Psychol. Rev. 1985, 92, 289–316. [Google Scholar] [CrossRef]
- Ziori, E.; Dienes, Z. How does prior knowledge affect implicit and explicit concept learning? Q. J. Exp. Psychol. 2008, 61, 601–624. [Google Scholar] [CrossRef]
- Davis, T.; Love, B.C.; Maddox, W.T. Two pathways to stimulus encoding in category learning? Mem. Cognit. 2009, 37, 394–413. [Google Scholar] [CrossRef][Green Version]
- Goldwater, M.B.; Don, H.J.; Krusche, M.J.F.; Livesey, E.J. Relational discovery in category learning. J. Exp. Psychol. Gen. 2018, 147, 1–35. [Google Scholar] [CrossRef] [PubMed]
- Heit, E. Knowledge and concept learning. In Knowledge, Concepts and Categories.; The MIT Press: Cambridge, MA, USA, 1997; pp. 7–41. ISBN 0-262-62118-5. [Google Scholar]
- Piroth, L.; Cottenet, J.; Mariet, A.-S.; Bonniaud, P.; Blot, M.; Tubert-Bitter, P.; Quantin, C. Comparison of the characteristics, morbidity, and mortality of covid-19 and seasonal influenza: A nationwide, population-based retrospective cohort study. Lancet Respir. Med. 2021, 9, 251–259. [Google Scholar] [CrossRef]
- Krewski, D.; Lemyre, L.; Turner, M.C.; Lee, J.E.C.; Dallaire, C.; Bouchard, L.; Brand, K.; Mercier, P. Public perception of population health risks in canada: Health hazards and sources of information. Hum. Ecol. Risk Assess. Int. J. 2006, 12, 626–644. [Google Scholar] [CrossRef]
- Ma, Z.; Ma, R. Predicting intentions to vaccinate against COVID-19 and seasonal flu: The role of consideration of future and immediate consequences. Health Commun. 2021, 1–10. [Google Scholar] [CrossRef]
- Betz, N.; Coley, J.D. Development of conceptual flexibility in intuitive biology: Effects of environment and experience. Front. Psychol. 2020, 11, 2454. [Google Scholar] [CrossRef]
- Goldstone, R.L.; Lippa, Y.; Shiffrin, R.M. Altering object representations through category learning. Cognition 2001, 78, 27–43. [Google Scholar] [CrossRef]
- Ahn, W.; Flanagan, E.H.; Marsh, J.K.; Sanislow, C.A. Beliefs about essences and the reality of mental disorders. Psychol. Sci. 2006, 17, 759–766. [Google Scholar] [CrossRef]
- Cooper, J.A.; Marsh, J.K. The influence of expertise on essence beliefs for mental and medical disorder categories. Cognition 2015, 144, 67–75. [Google Scholar] [CrossRef]
- Lynch, E.B.; Coley, J.D.; Medin, D.L. Tall Is typical: Central tendency, ideal dimensions, and graded category structure among tree experts and novices. Mem. Cognit. 2000, 28, 41–50. [Google Scholar] [CrossRef][Green Version]
- Medin, D.L.; Lynch, E.B.; Coley, J.D.; Atran, S. Categorization and reasoning among tree experts: Do all roads lead to Rome? Cognit. Psychol. 1997, 32, 49–96. [Google Scholar] [CrossRef]
- Shafto, P.; Coley, J.D. Development of categorization and reasoning in the natural world: Novices to experts, naive similarity to ecological knowledge. J. Exp. Psychol. Learn. Mem. Cogn. 2003, 29, 641–649. [Google Scholar] [CrossRef]
- Lin, E.L.; Murphy, G.L. Effects of background knowledge on object categorization and part detection. J. Exp. Psychol. Hum. Percept. Perform. 1997, 23, 1153–1169. [Google Scholar] [CrossRef]
- Wisniewski, E.J.; Medin, D.L. On the interaction of theory and data in concept learning. Cogn. Sci. 1994, 18, 221–281. [Google Scholar] [CrossRef]
- Moreau, C.P.; Markman, A.B.; Lehmann, D.R. “What Is It?” categorization flexibility and consumers’ responses to really new products. J. Consum. Res. 2001, 27, 489–498. [Google Scholar] [CrossRef]
- Bruine de Bruin, W.; Saw, H.-W.; Goldman, D.P. Political polarization in us residents’ covid-19 risk perceptions, policy preferences, and protective behaviors. J. Risk Uncertain. 2020, 46, 270–277. [Google Scholar] [CrossRef] [PubMed]
- Brewer, N.T.; Chapman, G.B.; Gibbons, F.X.; Gerrard, M.; McCaul, K.D.; Weinstein, N.D. Meta-analysis of the relationship between risk perception and health behavior: The example of vaccination. Health Psychol. Off. J. Div. Health Psychol. Am. Psychol. Assoc. 2007, 26, 136–145. [Google Scholar] [CrossRef]
- Sheeran, P.; Harris, P.R.; Epton, T. Does heightening risk appraisals change people’s intentions and behavior? A meta-analysis of experimental studies. Psychol. Bull. 2014, 140, 511–543. [Google Scholar] [CrossRef] [PubMed]
- Bruine de Bruin, W.; Bennett, D. Relationships between initial COVID-19 risk perceptions and protective health behaviors: A national survey. Am. J. Prev. Med. 2020, 59, 157–167. [Google Scholar] [CrossRef]
- Marsh, J.K.; Ungson, N.D.; Packer, D.J. Bring out Your Experts: The Influence of Perceived Expert Causal Understanding on Pandemic Behaviors. Unpublished manuscript, last modified, 27 April 2021. (under review).
- Packer, D.J.; Ungson, N.D.; Marsh, J.K. Conformity and reactions to deviance in the time of COVID-19. Group Process. Intergroup Relat. 2021, 24, 311–317. [Google Scholar] [CrossRef]
- Asch, S.E. Forming impressions of personality. J. Abnorm. Soc. Psychol. 1946, 41, 258–290. [Google Scholar] [CrossRef] [PubMed]
- Baiocchi, M.C.; Waxman, S.; Pérez, É.M.; Pérez, A.; Taverna, A. Social-ecological relations among animals serve as a conceptual framework among the Wichi. Cogn. Dev. 2019, 52, 100807. [Google Scholar] [CrossRef]
- López, A.; Atran, S.; Coley, J.D.; Medin, D.L.; Smith, E.E. The tree of life: Universal and cultural features of folkbiological taxonomies and inductions. Cognit. Psychol. 1997, 32, 251–295. [Google Scholar] [CrossRef]
- Lindgren, E.; Andersson, Y.; Suk, J.E.; Sudre, B.; Semenza, J.C. Monitoring EU emerging infectious disease risk due to climate change. Science 2012, 336, 418. [Google Scholar] [CrossRef]
- Schmeller, D.S.; Courchamp, F.; Killeen, G. Biodiversity loss, emerging pathogens and human health risks. Biodivers. Conserv. 2020, 29, 3095–3102. [Google Scholar] [CrossRef]
- Angermeyer, M.C.; Holzinger, A.; Carta, M.G.; Schomerus, G. Biogenetic explanations and public acceptance of mental illness: Systematic review of population studies. Br. J. Psychiatry 2011, 199, 367–372. [Google Scholar] [CrossRef]
- Phelan, J.C. Genetic bases of mental illness—A Cure for stigma? Trends Neurosci. 2002, 25, 430–431. [Google Scholar] [CrossRef]
- Phelan, J.C. Geneticization of Deviant Behavior and Consequences for Stigma: The Case of Mental Illness. J. Health Soc. Behav. 2005, 46, 307–322. [Google Scholar] [CrossRef]
- Iuliano, A.D.; Roguski, K.M.; Chang, H.H.; Muscatello, D.J.; Palekar, R.; Tempia, S.; Cohen, C.; Gran, J.M.; Schanzer, D.; Cowling, B.J.; et al. Estimates of global seasonal influenza-associated respiratory mortality: A modelling study. The Lancet 2018, 391, 1285–1300. [Google Scholar] [CrossRef]
- Center for Disease Control National Pandemic Strategy. Available online: https://www.cdc.gov/flu/pandemic-resources/national-strategy/index.html (accessed on 9 February 2021).
- Kain, T.; Fowler, R. Preparing intensive care for the next pandemic influenza. Crit. Care 2019, 23, 337. [Google Scholar] [CrossRef]
- Jorgensen, P.; Mereckiene, J.; Cotter, S.; Johansen, K.; Tsolova, S.; Brown, C. How close are countries of the WHO European Region to achieving the goal of vaccinating 75% of key risk groups against influenza? results from national surveys on seasonal influenza vaccination programmes, 2008/2009 to 2014/2015. Vaccine 2018, 36, 442–452. [Google Scholar] [CrossRef] [PubMed]
- Luckhurst, R. Zombies: A Cultural History; Reaktion Books: London, UK, 2015. [Google Scholar]

| Scale | Item | Time |
|---|---|---|
| Serious Diseases (α = 0.71) | The 1918 flu pandemic (a.k.a, the Spanish Flu) | T1 |
| The rise of HIV/AIDS in the 1980s | T1 | |
| The spread of SARS in 2002–2003 | T1 | |
| Bubonic plague/black death | T2 | |
| Swine flu/H1N1 | T2 | |
| Ebola | T2 | |
| Normal Flu | The spread of the flu in any normal year | T1 |
| Apocalyptic Events (α = 0.70) | Zombie movies like World War Z, I Am Legend, or 28 Days Later | T1 |
| Zombie TV shows such as The Walking Dead | T1 | |
| Video and board games (e.g., Plague Inc., Pandemic, Fallout) | T2 | |
| Major Upheavals (α = 0.80) | 11 September 2001 | T2 |
| Economic upheaval (e.g., the Great Depression, the 2008 recession) | T2 | |
| Societal upheaval (e.g., the LA riots) | T2 | |
| War (e.g., WWII) | T2 |
| Predictor | Time 2 (β) | Time 3 (β) | Time 4 (β) |
|---|---|---|---|
| Serious Diseases | 0.115 *** | 0.118 *** | 0.088 * |
| Normal Flu | −0.123 *** | −0.114 *** | −0.059 |
| Apocalyptic Event | −0.049 | <0.001 | 0.042 |
| Major Upheavals | 0.094 *** | 0.041 | 0.034 |
| Political Ideology | −0.144 *** | −0.276 *** | −0.320 *** |
| Perceived Self-Risk | 0.056 * | 0.120 *** | 0.103 *** |
| R2 | 0.071 *** | 0.134 *** | 0.152 *** |
| Predictor | Time 2 (β) | Time 3 (β) | Time 4 (β) |
|---|---|---|---|
| Serious Diseases | 0.041 | 0.056 | 0.042 |
| Normal Flu | −0.063 * | −0.056 | −0.045 |
| Apocalyptic Event | 0.113 *** | 0.134 *** | 0.191 *** |
| Major Upheavals | 0.109 *** | 0.094 ** | 0.095 ** |
| Political Ideology | 0.018 | −0.050 | −0.057 |
| Perceived Self-Risk | 0.054 * | 0.075 ** | 0.099 ** |
| R2 | 0.046 *** | 0.058 *** | 0.086 *** |
| Predictor | Time 3 (β) | Time 4 (β) |
|---|---|---|
| Serious Diseases | 0.126 *** | 0.087 * |
| Normal Flu | −0.088 ** | −0.072 * |
| Apocalyptic Event | 0.019 | 0.004 |
| Major Upheavals | 0.013 | 0.018 |
| Political Ideology | −0.240 *** | −0.282 *** |
| Perceived Self-Risk | 0.119 *** | 0.083 ** |
| R2 | 0.106 *** | 0.118 *** |
| Predictor | Time 4 (β) |
|---|---|
| Serious Diseases | <0.001 |
| Normal Flu | 0.034 |
| Apocalyptic Event | 0.019 |
| Major Upheavals | 0.074 |
| Political Ideology | 0.180 *** |
| Perceived Self-Risk | 0.046 |
| R2 | 0.047 ** |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Marsh, J.K.; Ungson, N.D.; Packer, D.J. Of Pandemics and Zombies: The Influence of Prior Concepts on COVID-19 Pandemic-Related Behaviors. Int. J. Environ. Res. Public Health 2021, 18, 5207. https://doi.org/10.3390/ijerph18105207
Marsh JK, Ungson ND, Packer DJ. Of Pandemics and Zombies: The Influence of Prior Concepts on COVID-19 Pandemic-Related Behaviors. International Journal of Environmental Research and Public Health. 2021; 18(10):5207. https://doi.org/10.3390/ijerph18105207
Chicago/Turabian StyleMarsh, Jessecae K., Nick D. Ungson, and Dominic J. Packer. 2021. "Of Pandemics and Zombies: The Influence of Prior Concepts on COVID-19 Pandemic-Related Behaviors" International Journal of Environmental Research and Public Health 18, no. 10: 5207. https://doi.org/10.3390/ijerph18105207
APA StyleMarsh, J. K., Ungson, N. D., & Packer, D. J. (2021). Of Pandemics and Zombies: The Influence of Prior Concepts on COVID-19 Pandemic-Related Behaviors. International Journal of Environmental Research and Public Health, 18(10), 5207. https://doi.org/10.3390/ijerph18105207






