Density or Connectivity: What Are the Main Causes of the Spatial Proliferation of COVID-19 in Korea?
Abstract
1. Introduction
2. Literature Review
2.1. Cities and Pandemics
2.2. Density and Connectivity
2.3. Research Gap and Our Contribution
3. Materials and Methods
3.1. Study Area
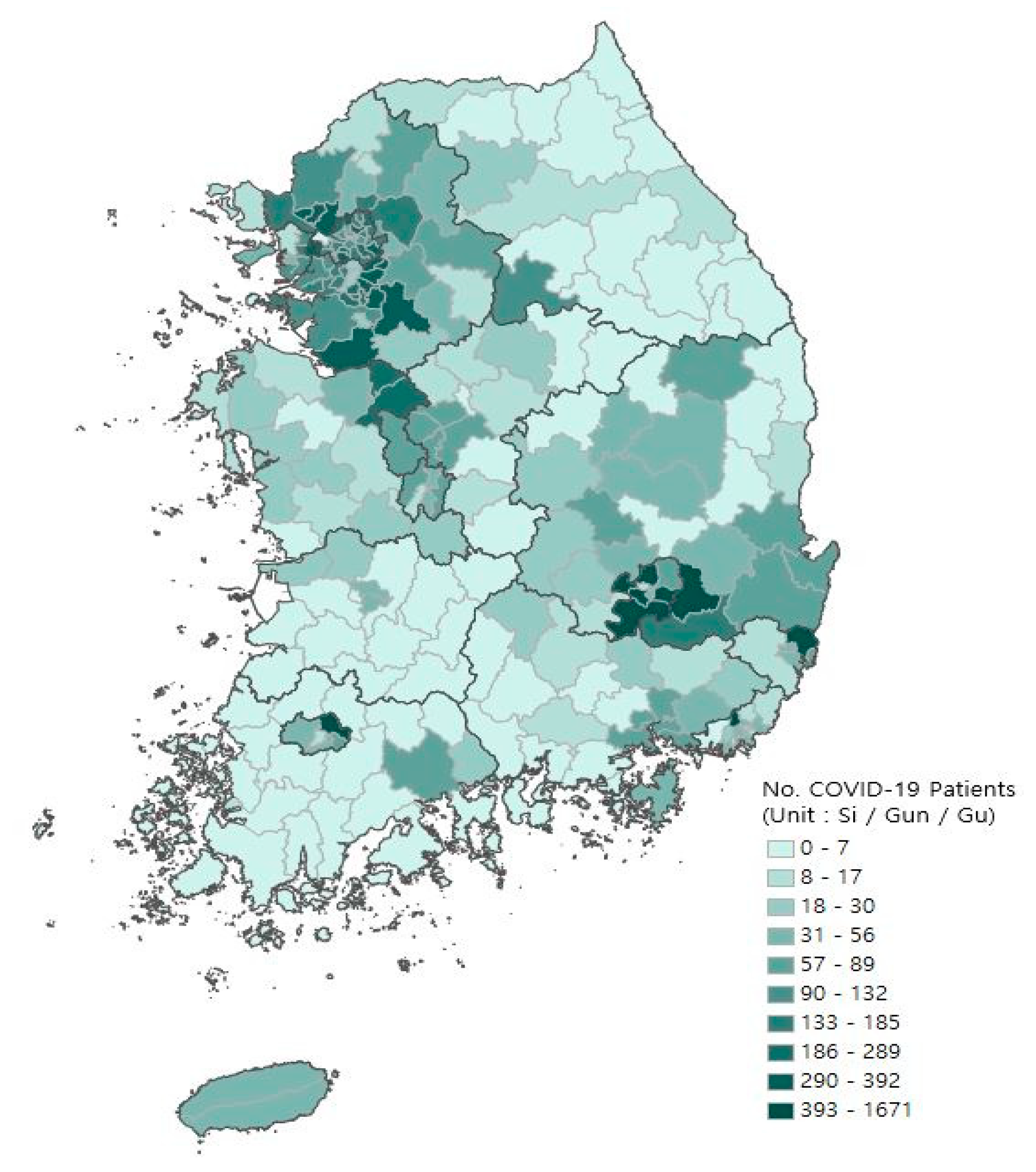
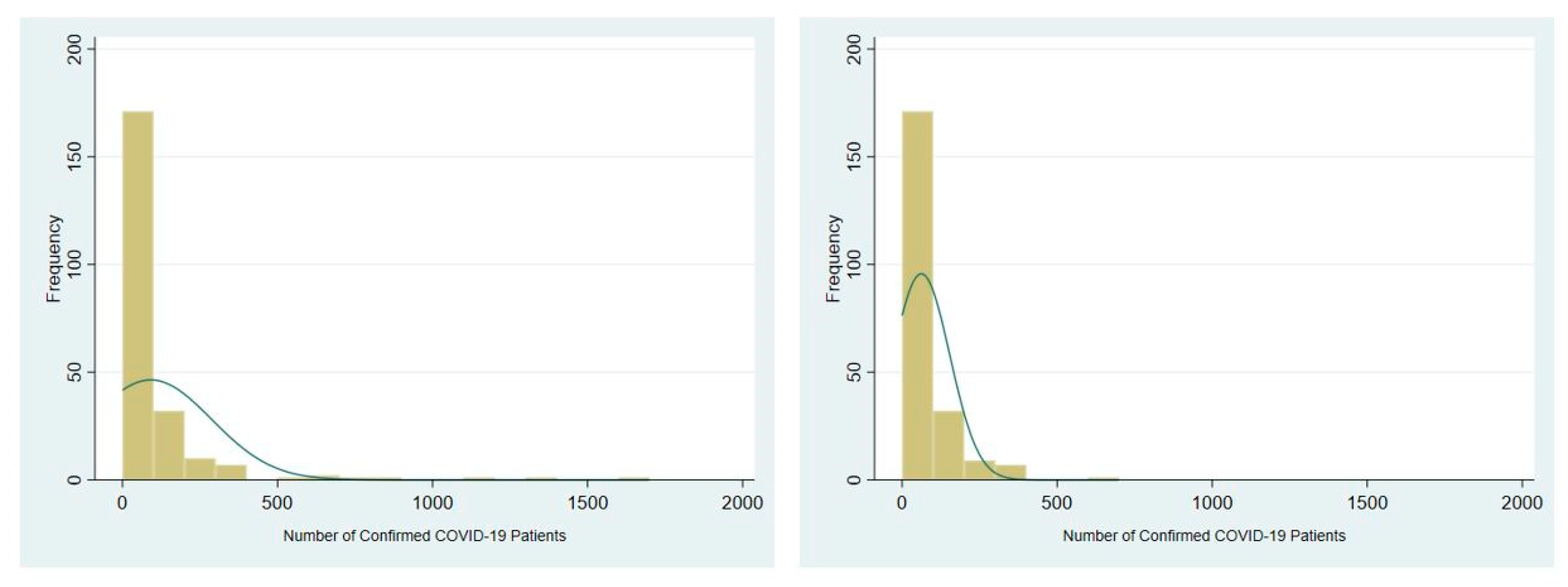
3.2. Main Outcomes
3.3. Explanatory Variables
3.4. Control Variables
3.5. Analytical Approach
4. Results
4.1. Descriptive Summary
4.2. Model Results
5. Discussion
Limitations
6. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
Appendix A. Information about the COVID-19 Dataset
References
- World Health Organization (WHO). Coronavirus Disease (COVID-19) Pandemic. 2020. Available online: https://www.who.int/emergencies/diseases/novel-coronavirus-2019 (accessed on 19 September 2020).
- Beck, U. Living in the world risk society. Econ. Soc. 2006, 35, 329–345. [Google Scholar] [CrossRef]
- Matthew, R.A.; McDonald, B. Cities under Siege: Urban Planning and the Threat of Infectious Disease. J. Am. Plan. Assoc. 2006, 72, 109–117. [Google Scholar] [CrossRef]
- Sung, H. Impacts of the Outbreak and Proliferation of the Middle East Respiratory Syndrome on Rail Transit Ridership in the Seoul Metropolitan City. J. Korea Plan. Assoc. 2016, 51, 163. [Google Scholar] [CrossRef]
- World Health Organization (WHO). Sierra Leone Stops Transmission of Ebola Virus. 2015. Available online: https://www.who.int/news/item/07-11-2015-sierra-leone-stops-transmission-of-ebola-virus (accessed on 19 September 2020).
- Glaeser, E. Cities, Productivity, and Quality of Life. Science 2011, 333, 592–594. [Google Scholar] [CrossRef] [PubMed]
- Kao, C.-L.; Chan, T.-C.; Tsai, C.-H.; Chu, K.-Y.; Chuang, S.-F.; Lee, C.-C.; Li, Z.-R.T.; Wu, K.-W.; Chang, L.-Y.; Shen, Y.-H.; et al. Emerged HA and NA Mutants of the Pandemic Influenza H1N1 Viruses with Increasing Epidemiological Significance in Taipei and Kaohsiung, Taiwan, 2009–2010. PLoS ONE 2012, 7, e31162. [Google Scholar] [CrossRef]
- Garrett, T.A. Economic Effects of the 1918 Influenza Pandemic: Implications for a Modern-Day Pandemic; Federal Reserve Bank of St. Louis: St. Louis, MO, USA, 2007. [Google Scholar]
- Nishiura, H.; Chowell, G. Rurality and pandemic influenza: Geographic heterogeneity in the risks of infection and death in Kanagawa, Japan (1918–1919). N. Z. Med. J. 2008, 121, 18–27. [Google Scholar] [PubMed]
- Parmet, W.E.; Rothstein, M.A. The 1918 Influenza Pandemic: Lessons Learned and Not—Introduction to the Special Section. Am. J. Public Health 2018, 108, 1435–1436. [Google Scholar] [CrossRef]
- Harvey, D. The Condition of Postmodernity; Blackwell: Oxford, UK, 2020; Volume 14, pp. 235–242. [Google Scholar]
- Morens, D.M.; Fauci, A.S. Emerging Infectious Diseases: Threats to Human Health and Global Stability. PLoS Pathog. 2013, 9, e1003467. [Google Scholar] [CrossRef]
- Sands, P.; Mundaca-Shah, C.; Dzau, V.J. The Neglected Dimension of Global Security—A Framework for Countering Infectious-Disease Crises. N. Engl. J. Med. 2016, 374, 1281–1287. [Google Scholar] [CrossRef]
- Morens, D.M.; Daszak, P.; Markel, H.; Taubenberger, J.K. Pandemic COVID-19 Joins History’s Pandemic Legion. mBio 2020, 11. [Google Scholar] [CrossRef]
- Brown, T.M. The COVID-19 Pandemic in Historical Perspective: An AJPH Dossier. Am. J. Public Health 2021, 111, 402–404. [Google Scholar] [CrossRef]
- Frankema, E.; Tworek, H. Pandemics that changed the world: Historical reflections on COVID-19. J. Glob. Hist. 2020, 15, 333–335. [Google Scholar] [CrossRef]
- Varlık, N. Rethinking the history of plague in the time ofCOVID-19. Centaurus 2020, 62, 285–293. [Google Scholar] [CrossRef]
- Caron, C. Are Cities a Safe Place to Live during a Pandemic? The New York Times. 7 December 2020. Available online: https://www.nytimes.com/2020/12/07/well/live/coronavirus-cities-safe.html (accessed on 14 September 2020).
- Keil, R. The density dilemma: There is always too much and too little of it. Urban Geogr. 2020, 41, 1284–1293. [Google Scholar] [CrossRef]
- Cave, B.; Kim, J.; Viliani, F.; Harris, P. Applying an equity lens to urban policy measures for COVID-19 in four cities. Cities Health 2020, 1–5. [Google Scholar] [CrossRef]
- Sharifi, A.; Khavarian-Garmsir, A.R. The COVID-19 pandemic: Impacts on cities and major lessons for urban planning, design, and management. Sci. Total Environ. 2020, 749, 142391. [Google Scholar] [CrossRef]
- UN-Habitat. Cities and Pandemics: Towards a More Just, Green and Healthy Future; UN-Habitat: Nairobi, Kenya, 2021; ISBN 978-92-1-132877-6. [Google Scholar]
- Mueller, N.; Rojas-Rueda, D.; Khreis, H.; Cirach, M.; Andrés, D.; Ballester, J.; Bartoll, X.; Daher, C.; Deluca, A.; Echave, C.; et al. Changing the urban design of cities for health: The superblock model. Environ. Int. 2020, 134, 105132. [Google Scholar] [CrossRef] [PubMed]
- Camerin, F. Open issues and opportunities to guarantee the “right to the ‘healthy’ city” in the post-Covid-19, European city. Contesti 2021. [Google Scholar] [CrossRef]
- Fabris, L.M.F.; Camerin, F.; Semprebon, G.; Balzarotti, R.M. New Healthy Settlements Responding to Pandemic Outbreaks: Approaches from (and for) the Global City. Plan J. 2021, 5. [Google Scholar] [CrossRef]
- Graziano, T. Smart Technologies, Back-to-the-Village Rhetoric, and Tactical Urbanism: Post-COVID Planning Scenarios in Italy. Int. J. E-Plan. Res. 2021, 10, 80–93. [Google Scholar] [CrossRef]
- Arbel, Y.; Fialkoff, C.; Kerner, A.; Kerner, M. Do population density, socio-economic ranking and Gini index of cities influence infection rates from coronavirus? Israel as a case study. Res. Sq. 2020. [Google Scholar] [CrossRef]
- Ehlert, A. The socioeconomic determinants of COVID-19: A spatial analysis of German county level data. medRxiv 2020. [Google Scholar] [CrossRef]
- Wong, D.W.S.; Li, Y. Spreading of COVID-19: Density matters. PLoS ONE 2020, 15, e0242398. [Google Scholar] [CrossRef] [PubMed]
- Agnoletti, M.; Manganelli, S.; Piras, F. Covid-19 and rural landscape: The case of Italy. Landsc. Urban Plan. 2020, 204, 103955. [Google Scholar] [CrossRef]
- Chowell, G.; Bettencourt, L.M.; Johnson, N.; Alonso, W.J.; Viboud, C. The 1918–1919 influenza pandemic in England and Wales: Spatial patterns in transmissibility and mortality impact. Proc. R. Soc. B Boil. Sci. 2008, 275, 501–509. [Google Scholar] [CrossRef]
- Hamidi, S.; Sabouri, S.; Ewing, R. Does Density Aggravate the COVID-19 Pandemic? J. Am. Plan. Assoc. 2020, 86, 495–509. [Google Scholar] [CrossRef]
- Teller, J. Urban density and Covid-19: Towards an adaptive approach. Build. Cities 2021, 2, 150–165. [Google Scholar] [CrossRef]
- Kissler, S.M.; Gog, J.R.; Viboud, C.; Charu, V.; Bjørnstad, O.N.; Simonsen, L.; Grenfell, B.T. Geographic transmission hubs of the 2009 influenza pandemic in the United States. Epidemics 2019, 26, 86–94. [Google Scholar] [CrossRef]
- Ljubic, B.; Gligorijevic, D.; Gligorijevic, J.; Pavlovski, M.; Obradovic, Z. Social network analysis for better understanding of influenza. J. Biomed. Inform. 2019, 93, 103161. [Google Scholar] [CrossRef]
- Cho, B.S.; Hong, S.H.; Lee, M.H. Reinterpretation of Korean Spatial Structure Based on Urban Network Approaches: Focused on Conglomerate Business Networking. J. Korean Reg. Dev. Assoc. 2015, 27, 1–13. [Google Scholar]
- Zhao, P.S.; Lee, J.H.; Lee, M.H. Characterizing the Structure of China‘s Passenger Railway Network Based on the social Network Analysis (SNA) Approaches: Focused on the 2008, 2013, and 2018 Railway Service Data, Respectively. J. Korea Contents Assoc. 2019, 19, 685–697. [Google Scholar]
- Shin, T.J.; Kim, S.; Jung, S.Y. Effects of the COVID-19 spread on the Northeast Asia Airport Network Centrality: Using Social Network Analysis. J. Digit. Converg. 2020, 18, 179–186. [Google Scholar]
- You, J. Lessons From South Korea’s Covid-19 Policy Response. Am. Rev. Public Adm. 2020, 50, 801–808. [Google Scholar] [CrossRef]
- Dighe, A.; Cattarino, L.; Cuomo-Dannenburg, G.; Skarp, J.; Imai, N.; Bhatia, S.; Gaythorpe, K.A.M.; Ainslie, K.E.C.; Baguelin, M.; Bhatt, S.; et al. Response to COVID-19 in South Korea and implications for lifting stringent interventions. BMC Med. 2020, 18, 1–12. [Google Scholar] [CrossRef]
- Lee, D.; Lee, J. Testing on the move: South Korea’s rapid response to the COVID-19 pandemic. Transp. Res. Interdiscip. Perspect. 2020, 5, 100111. [Google Scholar] [CrossRef]
- Korea Enterprises Federation (KEF). Survey on the Status of Telecommuting of Top 100 Companies in Sales According to Social Distancing, Report. 2020. Available online: http://www.kefplaza.com/labor/down.jsp?idx=14981&fileId=14709 (accessed on 2 May 2021).
- You, M.; Kim, Y.; Bak, S.; Kwon, D. Changes according to the concept of infectious production index and quarantine policy. Mag. Wkly. Health Dis. 2020, 14, 282–289. [Google Scholar]
- Kim, J.-K.; An, J.A.-R.; Oh, S.J.; Oh, J.; Lee, J.-K. Emerging COVID-19 Success Story: South Korea Learned the Lessons of MERS, Exemplars in Global Health Platform. 2021. Available online: https://ourworldindata.org/covid-exemplar-south-korea (accessed on 4 May 2021).
- Billah, A.; Miah, M.; Khan, N. Reproductive number of coronavirus: A systematic review and meta-analysis based on global level evidence. PLoS ONE 2020, 15, e0242128. [Google Scholar] [CrossRef]
- Jamshidi, S.; Baniasad, M.; Niyogi, D. Global to USA County Scale Analysis of Weather, Urban Density, Mobility, Homestay, and Mask Use on COVID-19. Int. J. Environ. Res. Public Health 2020, 17, 7847. [Google Scholar] [CrossRef]
- Kim, J.I.; Chung, H.W. The Shape of Population and Housing Density Gradients: The Case of Daegu Metropolitan City. Hous. Stud. 2006, 14, 195–214. [Google Scholar]
- Lee, Y.J. A Comparison Study on the Weighted Network Centrality Measures of tnet and WNET. J. Korean Soc. Inf. Manag. 2013, 30, 241–264. [Google Scholar] [CrossRef][Green Version]
- Block, P.; Hoffman, M.; Raabe, I.J.; Dowd, J.B.; Rahal, C.; Kashyap, R.; Mills, M.C. Social network-based distancing strategies to flatten the COVID-19 curve in a post-lockdown world. Nat. Hum. Behav. 2020, 4, 588–596. [Google Scholar] [CrossRef] [PubMed]
- Saraswathi, S.; Mukhopadhyay, A.; Shah, H.; Ranganath, T.S. Social network analysis of COVID-19 transmission in Karnataka, India. Epidemiol. Infect. 2020, 148, 1–30. [Google Scholar] [CrossRef] [PubMed]
- Jo, W.; Chang, D.; You, M.; Ghim, G.-H. A social network analysis of the spread of COVID-19 in South Korea and policy implications. Sci. Rep. 2021, 11, 1–10. [Google Scholar] [CrossRef] [PubMed]
- Yum, S. Social Network Analysis for Coronavirus (COVID-19) in the United States. Soc. Sci. Q. 2020, 101, 1642–1647. [Google Scholar] [CrossRef] [PubMed]
- Gupta, D.; Biswas, D.; Kabiraj, P. COVID-19 outbreak and Urban dynamics: Regional variations in India. GeoJournal 2021, 3, 1–19. [Google Scholar] [CrossRef]
- So, M.K.; Tiwari, A.; Chu, A.M.; Tsang, J.T.; Chan, J.N. Visualizing COVID-19 pandemic risk through network connectedness. Int. J. Infect. Dis. 2020, 96, 558–561. [Google Scholar] [CrossRef]
- Brenner, N. New Urban Spaces: Urban Theory and the Scale Question; Oxford University Press: New York, NY, USA, 2019. [Google Scholar]
- Zhong, C.; Schlapfer, M.S.; Arisona, S.M.; Batty, M.M.; Ratti, C.; Schmitt, G. Revealing centrality in the spatial structure of cities from human activity patterns. Urban Stud. 2016, 54, 437–455. [Google Scholar] [CrossRef]
- Luo, W.; Wang, Y.; Liu, X.; Gao, S. Cities as Spatial and Social Networks: Towards a Spatio-Socio-Semantic Analysis Framework. Spat. Synth. 2018, 21–37. [Google Scholar] [CrossRef]
- Lee, J.H.; Jo, S.M. Effects of Interorganizational Network Characteristics of Social Enterprises on Organizational Performance: Focusing on Network Centrality. J. Korean Soc. Welf. Adm. 2015, 17, 89–125. [Google Scholar]
- Hamidi, S.; Zandiatashbar, A. Compact development and adherence to stay-at-home order during the COVID-19 pandemic: A longitudinal investigation in the United States. Landsc. Urban Plan. 2021, 205, 103952. [Google Scholar] [CrossRef]
- Xie, J.; Luo, S.; Furuya, K.; Sun, D. Urban Parks as Green Buffers During the COVID-19 Pandemic. Sustainability 2020, 12, 6751. [Google Scholar] [CrossRef]
- Ma, A.T.; Lam, T.W.; Cheung, L.T.; Fok, L. Protected areas as a space for pandemic disease adaptation: A case of COVID-19 in Hong Kong. Landsc. Urban Plan. 2021, 207, 103994. [Google Scholar] [CrossRef] [PubMed]
- Gelman, A.; Hill, J. Data Analysis Using Regression and Multilevel/Hierarchical Models; Cambridge University Press: New York, NY, USA, 2006; ISBN 1-139-46093-5. [Google Scholar]
- Bertozzi, A.L.; Franco, E.; Mohler, G.; Short, M.B.; Sledge, D. The challenges of modeling and forecasting the spread of COVID-19. Proc. Natl. Acad. Sci. USA 2020, 117, 16732–16738. [Google Scholar] [CrossRef] [PubMed]
- Li, S.; Ma, S.; Zhang, J. Association of built environment attributes with the spread of COVID-19 at its initial stage in China. Sustain. Cities Soc. 2021, 67, 102752. [Google Scholar] [CrossRef] [PubMed]
- Yoon, D. How South Korea Put into Place the World’s Most Aggressive Coronavirus Test Program. Wall Street Journal. 16 March 2020. Available online: https://www.wsj.com/articles/how-south-korea-put-into-place-the-worlds-most-aggressive-coronavirus-testing-11584377217 (accessed on 4 May 2021).
| Indicators | Equation |
|---|---|
| Degree Centrality | : Number of connections node i has with (g − 1) nodes. |
| Closeness Centrality | : The sum of the closest distance between node i and j g: number of nodes |
| Betweenness Centrality | : the number of the closest routes between nodes j and k : the number of closest routes between nodes i and j that includes node i |
| Eigenvector Centrality | : Eigenvalue : number of nodes : the quantitative value of the connection between nodes i and j |
| Variables | Description | Mean | Std. Dev. | Min | Max | VIF |
|---|---|---|---|---|---|---|
| Dependent variables | ||||||
| Total cases | Accrued confirmed cases per city, county, district | 91.171 | 196.051 | 0 | 1671 | |
| Case rates | Accrued confirmed cases per 10,000 | 3.557 | 8.155 | 0 | 92.897 | |
| Connectivity | ||||||
| Degree centrality | Degree of centrality found using SNA | 2.13 × 10−9 | 1 | −1.101 | 4.599 | 4.59 |
| Closeness centrality | Closeness Centrality found using SNA | −3.45 × 10−9 | 1 | −5.77 | 1.361 | 1.85 |
| Betweenness centrality | Betweenness Centrality found using SNA | −1.04 × 10−9 | 1 | −0.514 | 10.257 | 1.39 |
| Eigenvector | Eigenvector found using SNA | 1.23 × 10−9 | 1 | −0.182 | 10.356 | 1.46 |
| Density | ||||||
| Net population density | Population/Land Area | −1.33 × 10−9 | 1 | −0.961 | 2.716 | 3.89 |
| Net employment density | Total # Employed/Land Area | −1.58 × 10−9 | 1 | −0.449 | 12.230 | 1.65 |
| Population characteristics | ||||||
| % Female | Total female population/total population | 0.499 | 0.013 | 0.433 | 0.523 | 1.81 |
| % 20 s years old | Total number of people between the ages of 20–29/total population | 11.633 | 5.235 | 2.508 | 66.198 | 1.70 |
| % 65+ years old | Total population of 65+/total population | 21.556 | 8.277 | 8.7 | 40.7 | 4.78 |
| Neighborhood resources | ||||||
| No. of doctors/1000 people | (Total number of doctors/total population) × 1000 | 2.778 | 2.286 | 1 | 19.6 | 1.69 |
| Availability of nursing home | Availability of nursing home (0/1) | 0.552 | 0.498 | 0 | 1 | 1.18 |
| Park area/1000 people | (Total park area/total population) × 1000 | 19,200.83 | 18,499.82 | 0 | 132,334.9 | 1.60 |
| Economic factor | ||||||
| Per capita GRDP | Growth regional domestic product (GRDP)/total population | 33.677 | 30.935 | 8.072 | 385.763 | 1.57 |
| Other Control factors | ||||||
| Land area | Area of city, county, district (km2) | 77.762 | 95.87 | 3.71 | 595.33 | 1.78 |
| Dummy for Daegu | Whether or not include Daegu (0/1) | 0.035 | 0.18 | 0 | 1 | 1.11 |
| Variables | Number of Cases | Number of Cases/10,000 Residents | ||
|---|---|---|---|---|
| Model 1: OLS | Model 2: NBR | Model 3: OLS | Model 4: NBR | |
| Connectivity | ||||
| Degree centrality | 45.62188 * (−2.34) | 0.44392 ** (3.18) | −0.50209 (−0.54) | 0.15022 (−1.35) |
| Closeness centrality | −21.27929 * (−2.58) | −0.17435 (−1.40) | −0.44005 + (−1.86) | −0.12804 (−1.48) |
| Betweenness centrality | 7.78549 (1.35) | 0.30548 (1.45) | 0.55370 (−0.75) | 0.27804 (1.28) |
| Eigenvector | −9.26285 (−1.50) | −0.10502 + (−1.91) | 0.22048 (0.68) | −0.04594 (−0.98) |
| Density | ||||
| Net population density | 29.37699 * (2.51) | 0.30569 * (−2.48) | −0.02309 (−0.05) | 0.05392 (0.48) |
| Net employment density | −4.33808 (−0.70) | −0.00395 (−0.06) | −0.45149 (−1.04) | −0.01695 (−0.34) |
| Population characteristics | ||||
| % Female | 562.86792 (−1.09) | 21.16410 ** (2.60) | 47.50386 (−1.41) | 9.38009 (1.46) |
| % 20 s years old | 2.66258 (−0.99) | 0.00978 (−0.34) | 0.22942 (−1.09) | 0.01577 (0.89) |
| % 65+ years old | 1.18664 (0.98) | −0.05200 * (−2.52) | −0.01805 (−0.29) | −0.00268 (−0.15) |
| Neighborhood resources | ||||
| No. of doctors/1000 people | −13.07725 (−1.49) | −0.05617 * (−2.12) | 0.14679 (0.77) | −0.02717 (−1.16) |
| Availability of nursing home (0/1) | 10.23637 (−0.8) | 0.45998 ** (2.73) | −0.51969 (−0.62) | 0.14658 (1.01) |
| Park area/1000 people | −0.00042 (−1.54) | −0.00001 *** (−3.69) | −0.00003 (−1.49) | −0.00001 (−1.58) |
| Economic factor | ||||
| Per capita GRDP | −0.19593 (−0.99) | −0.00176 (−1.21) | −0.002 (−0.36) | 0.00067 (−0.56) |
| Controls | ||||
| Land area (km2) | −0.00914 (−0.11) | 0.00113 (−1.43) | −0.00358 (−1.46) | −0.00139 * (−2.01) |
| Dummy for Daegu (0/1) | 800.48779 *** (5.89) | 2.45792 *** (−7.9) | 32.33786 *** (4.63) | 2.60876 *** (−10.8) |
| Constant | −228.62082 (−0.92) | −5.89396 (−1.51) | −22.74795 (−1.32) | −3.79063 (−1.24) |
| Log Likelihood | −1.37 × 103 | −1.05 × 103 | −694.8584 | −465.41374 |
| Adjusted R2 or Pseudo R2 | 0.73776 | 0.10397 | 0.57988 | 0.14277 |
| Alpha (SE) | 1.007541 *** (−0.1174) | 0.493818 *** (−0.14) | ||
| AIC | 2764.2 | 2141.95 | 1421.72 | 964.83 |
| BIC | 2819.07 | 2200.24 | 1476.59 | 1023.13 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Jo, Y.; Hong, A.; Sung, H. Density or Connectivity: What Are the Main Causes of the Spatial Proliferation of COVID-19 in Korea? Int. J. Environ. Res. Public Health 2021, 18, 5084. https://doi.org/10.3390/ijerph18105084
Jo Y, Hong A, Sung H. Density or Connectivity: What Are the Main Causes of the Spatial Proliferation of COVID-19 in Korea? International Journal of Environmental Research and Public Health. 2021; 18(10):5084. https://doi.org/10.3390/ijerph18105084
Chicago/Turabian StyleJo, Yun, Andy Hong, and Hyungun Sung. 2021. "Density or Connectivity: What Are the Main Causes of the Spatial Proliferation of COVID-19 in Korea?" International Journal of Environmental Research and Public Health 18, no. 10: 5084. https://doi.org/10.3390/ijerph18105084
APA StyleJo, Y., Hong, A., & Sung, H. (2021). Density or Connectivity: What Are the Main Causes of the Spatial Proliferation of COVID-19 in Korea? International Journal of Environmental Research and Public Health, 18(10), 5084. https://doi.org/10.3390/ijerph18105084






