Development and Psychometric Properties of a Questionnaire Assessing Self-Reported Generic Health Literacy in Adolescence
Abstract
1. Introduction
2. Materials and Methods
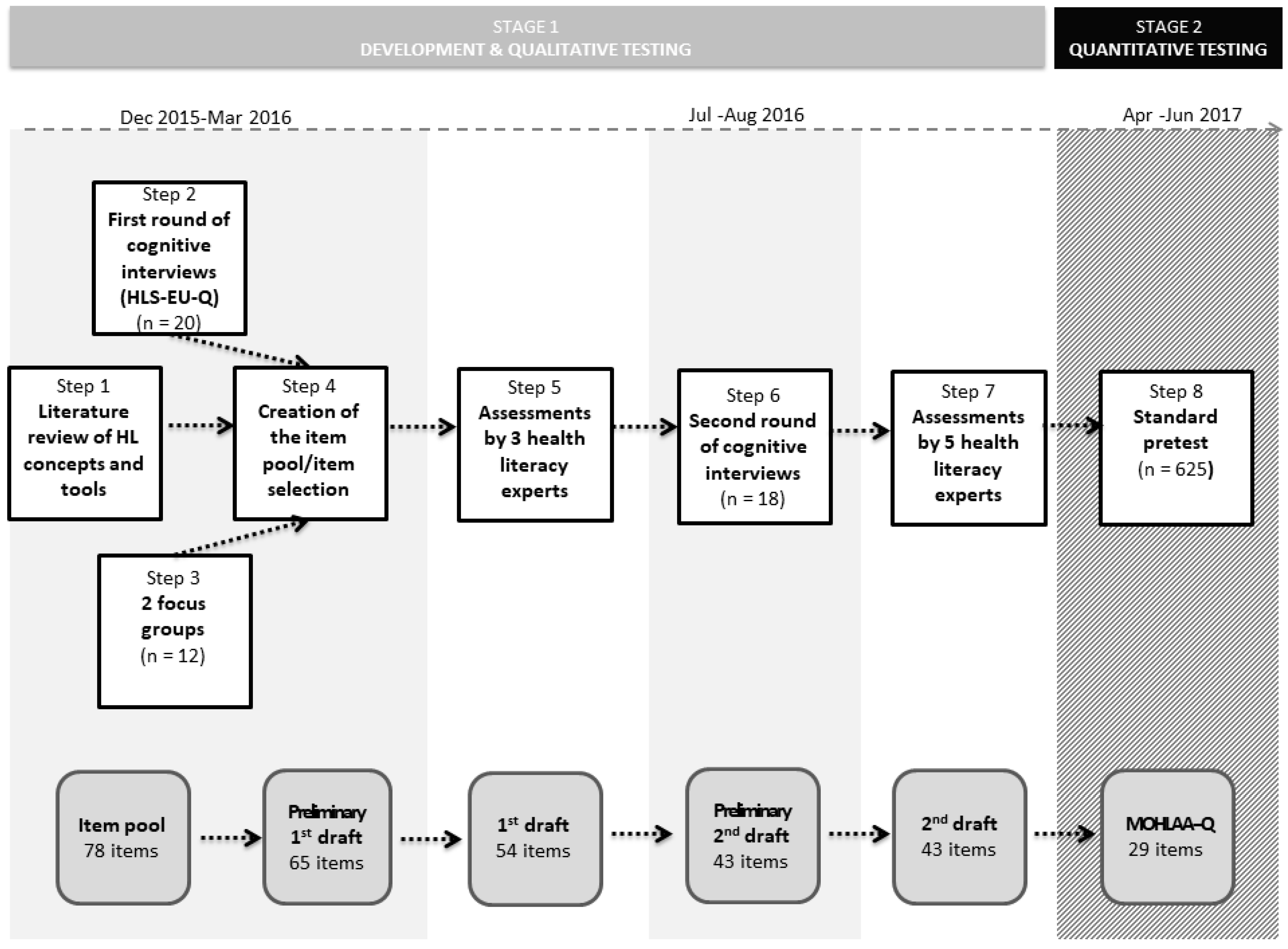
2.1. Stage 1: Development and Qualitative Testing
2.2. Stage 2: Quantitative Testing
2.2.1. Pretest Design and Data Collection
2.2.2. Measures
2nd Draft of the MOHLAA-Q
Further Scales for Validation
Sociodemographic Questions
2.2.3. Psychometric Analyses
3. Results
3.1. Stage 1 Development and Qualitative Testing
3.2. Stage 2: Quantitative Testing
3.2.1. Item and Reliability Analysis
Missing Values and Item Distribution
Discrimination and Difficulty Index
Reliability Analysis before the CFA
3.2.2. Structural Validity
3.2.3. Convergent and Concurrent Validity
4. Discussion
4.1. Structural Validity
4.2. Internal Consistency
4.3. Testing of Health-Related Knowledge (Scale D)
4.4. Consideration of the Role of Social Agents (Scale E)
4.5. Strengths and Limitations
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
Abbreviations
| CFA | Confirmatory Factor Analysis |
| CFI | Comparative Fit Index |
| CI | Cognitive Interview |
| df | Degrees of Freedom |
| EAs | Expert Assessments |
| FAS | Family Affluence Scale |
| FGs | Focus Groups |
| HLCA | Health Literacy in Childhood and Adolescence |
| HLS-EU-Q47-GER | German version of the European Health Literacy Survey Questionnaire, 47-item version |
| ITC | Corrected Item-Total Correlation |
| LR | Literature Review |
| MOHLAA-Q | Measurement of Health Literacy Among Adolescents Questionnaire |
| MSPSS | Multidimensional Scale of Perceived Social Support |
| NVS | Newest Vital Sign |
| HLAT-8 | Health Literacy Assessment |
| RMSEA | Root Mean Square Error of Approximation |
| TLI | Tucker-Lewis Index |
| WHO | World Health Organization |
| WLSM | Robust Weighted Least Square Mean-Adjusted |
| WRMR | Weighted Root Mean Square Residual |
References
- Berkman, N.D.; Sheridan, S.L.; Donahue, K.E.; Halpern, D.J.; Crotty, K. Low health literacy and health outcomes: An updated systematic review. Ann. Intern. Med. 2011, 155, 97–107. [Google Scholar] [CrossRef] [PubMed]
- Bitzer, E.M.; Sørensen, K. Gesundheitskompetenz – Health Literacy. Gesundheitswesen 2018, 80, 754–766. [Google Scholar] [CrossRef] [PubMed]
- Speros, C. Health literacy: Concept analysis. J. Adv. Nurs. 2005, 50, 633–640. [Google Scholar] [CrossRef] [PubMed]
- World Health Organization Regional Office for Europe (WHO Europe). Health Literacy. The Solid Facts. Available online: https://apps.who.int/iris/bitstream/handle/10665/128703/e96854.pdf (accessed on 17 November 2019).
- Sørensen, K.; Van den Broucke, S.; Fullam, J.; Doyle, G.; Pelikan, J.; Slonska, Z.; Brand, H.; Consortium Health Literacy Project European. Health literacy and public health: A systematic review and integration of definitions and models. BMC Public Health 2012, 12, 1–13. [Google Scholar] [CrossRef]
- World Health Organization (WHO). Shanghai declaration on promoting health in the 2030 Agenda for Sustainable Development. In Health Promotion International; WHO: Geneva, Switzerland, 2017; Volume 32, pp. 7–8. [Google Scholar]
- Mantwill, S.; Monestel-Umaña, S.; Schulz, P.J. The Relationship between Health Literacy and Health Disparities: A Systematic Review. PLoS ONE 2015, 10, e0145455. [Google Scholar] [CrossRef]
- Hurrelmann, K.; Quenzel, G. Lebensphase Jugend. Eine Einführung in die sozialwissenschaftliche Jugendforschung, 13th ed.; Beltz Juventa: Weinheim, Germany, 2016; ISBN 978-3-7799-2619-1. [Google Scholar]
- Silbereisen, R.K.; Weichold, K. Jugend (12–19 Jahre). In Entwicklungspsychologie, 7th ed.; Schneider, W., Lindenberger, U., Eds.; Beltz Verlag: Weinheim, Basel, 2012; pp. 235–258. ISBN 978-3-621-27768-6. [Google Scholar]
- Berk, E.L. Entwicklungspsychologie, 5th ed.; Pearson Education Deutschland GmbH: Munich, Germany, 2011; ISBN 978-3-86-894-049-7. [Google Scholar]
- Franzkowiak, P. Risikoverhalten und Gesundheitsbewusstsein bei Jugendlichen. Der Stellenwert von Rauchen und Alkoholkonsum im Alltag von 15-bis 20jährigen; Springer: Berlin, Germany, 1986; ISBN 3540165908. [Google Scholar]
- Institute of Medicine National Research Council. Adolescent Risk and Vulnerability: Concepts and Measurement; The National Academies Press: Washington, DC, USA, 2001; ISBN 978-0-309-07620-3. [Google Scholar]
- Wartella, E.; Rideout, V.; Montague, H.; Beaudoin-Ryan, L.; Lauricella, A. Teens, Health and Technology: A National Survey. Media Commun. 2016, 4, 13–23. [Google Scholar] [CrossRef]
- Paakkari, L.; Paakkari, O. Health literacy as a learning outcome in schools. Health Educ. 2012, 112, 133–152. [Google Scholar] [CrossRef]
- Fleary, S.A.; Joseph, P.; Pappagianopoulos, J.E. Adolescent health literacy and health behaviors: A systematic review. J. Adolesc. 2018, 62, 116–127. [Google Scholar] [CrossRef]
- Sanders, L.M.; Federico, S.; Klass, P.; Abrams, M.A.; Dreyer, B. Literacy and child health: A systematic review. Arch. Pediatr Adolesc Med. 2009, 163. [Google Scholar] [CrossRef]
- Bröder, J.; Okan, O.; Bauer, U.; Bruland, D.; Schlupp, S.; Bollweg, T.M.; Saboga-Nunes, L.; Bond, E.; Sorensen, K.; Bitzer, E.M.; et al. Health literacy in childhood and youth: A systematic review of definitions and models. BMC Public Health 2017, 17, 1–25. [Google Scholar] [CrossRef]
- Guo, S.; Armstrong, R.; Waters, E.; Sathish, T.; Alif, S.M.; Browne, G.R.; Yu, X. Quality of health literacy instruments used in children and adolescents: A systematic review. BMJ Open 2018, 8, 1–18. [Google Scholar] [CrossRef]
- Okan, O.; Lopes, E.; Bollweg, T.M.; Bröder, J.; Messer, M.; Bruland, D.; Bond, E.; Carvalho, G.S.; Sørensen, K.; Saboga-Nunes, L.; et al. Generic health literacy measurement instruments for children and adolescents: A systematic review of the literature. BMC Public Health 2018, 18, 1–19. [Google Scholar] [CrossRef] [PubMed]
- Ormshaw, M.J.; Paakkari, L.T.; Kannas, L.K. Measuring child and adolescent health literacy: A systematic review of literature. Health Educ. 2013, 113, 433–455. [Google Scholar] [CrossRef]
- Perry, E.L. Health literacy in adolescents: An integrative review. J. Spec. Pediatr. Nurs. 2014, 19, 210–218. [Google Scholar] [CrossRef] [PubMed]
- Wallmann, B.; Gierschner, S.; Froböse, I. Health literacy: What do our students know about health? Präv. Gesundheitsf. 2011, 7, 5–10. [Google Scholar] [CrossRef]
- Steckelberg, A.; Hülfenhaus, C.; Kasper, J.; Mühlhauser, I. Ebm@school--a curriculum of critical health literacy for secondary school students: Results of a pilot study. Int. J. Public Health 2009, 54, 158–165. [Google Scholar] [CrossRef]
- Steckelberg, A.; Hülfenhaus, C.; Kasper, J.; Rost, J.; Mühlhauser, I. How to measure critical health competences: Development and validation of the Critical Health Competence Test (CHC Test). Adv. Health Sci. Educ. 2009, 14, 11–22. [Google Scholar] [CrossRef]
- Schmidt, C.O.; Fahland, R.A.; Franze, M.; Splieth, C.; Thyrian, J.R.; Plachta-Danielzik, S.; Hoffmann, W.; Kohlmann, T. Health-related behaviour, knowledge, attitudes, communication and social status in school children in Eastern Germany. Health Educ. Res. 2010, 25, 542–551. [Google Scholar] [CrossRef]
- Berens, E.M.; Vogt, D.; Messer, M.; Hurrelmann, K.; Schaeffer, D. Health literacy among different age groups in Germany: Results of a cross-sectional survey. BMC Public Health 2016, 16, 1151. [Google Scholar] [CrossRef]
- Quenzel, G.; Schäffer, D.; Messer, M.; Vogt, D. Health literacy among less well-educated young people: Influencing factors and consequences. Bundesgesundheitsbl Gesundheitsforsch Gesundheitsschut 2015, 58, 951–957. [Google Scholar] [CrossRef]
- Richter, D.; Mehnert, A.; Forstmeyer, D.; Ernst, J.; Geue, K. Health Literacy in Adolescent and Young Adult Cancer Patients and Its Association with Health Outcomes. J. Adolesc. Young Adult Oncol. 2019, 451–457. [Google Scholar] [CrossRef]
- Zamora, P.; Pinheiro, P.; Okan, O.; Bitzer, E.-M.; Jordan, S.; Bittlingmayer, U.H.; Kessl, F.; Lenz, A.; Wasem, J.; Jochimsen, M.A.; et al. “Health Literacy” in childhood and adolescence. Structure and subject of a new interdisciplinary research network (HLCA research network). Präv. Gesundheitsf. 2015, 10, 167–172. [Google Scholar] [CrossRef]
- Hopker, T.; Lampert, T.; Spallek, J. Identification and characterisation of health behaviours in 11- to 17-year-old adolescents: A cluster analysis based on the german health interview and examination survey for children and adolescents. Gesundheitswesen 2014, 76, 453–461. [Google Scholar] [CrossRef] [PubMed]
- Richter, M.; Settertobulte, W. Gesundheits- und Freizeitverhalten von Jugendlichen. In Jugendgesundheitssurvey. Internationale Vergleichsstudie im Auftrag der Weltgesundheitsorganisation WHO; Hurrelmann, K., Klocke, A., Melzer, W., Ravens-Sieberer, U., Eds.; Juventa Verlag: Weinheim/München, Germany, 2003; pp. 99–157. ISBN 377991199X. [Google Scholar]
- Domanska, O.; Firnges, C.; Bollweg, T.M.; Sørensen, K.; Holmberg, C.; Jordan, S. Do adolescents understand the items of the European Health Literacy Survey Questionnaire (HLS-EU-Q47) - German version? Findings from cognitive interviews of the project “Measurement of Health Literacy Among Adolescents” (MOHLAA) in Germany. Arch. Public Health 2018, 76, 1–14. [Google Scholar] [CrossRef] [PubMed]
- Firnges, C.; Domanska, O.; Jordan, S. Developing an instrument for measuring the health literacy of adolescents: Lessons learned. In International Handbook of Health Literacy. Research, Practice and Policy Across the Lifespan; Okan, O., Bauer, U., Levin-Zamir, D., Pinheiro, P., Sørensen, K., Eds.; Policy Press University of Bristol: Great Britain, UK, 2019; pp. 99–114. ISBN 978-1447344513. [Google Scholar]
- Sørensen, K.; Van den Broucke, S.; Pelikan, J.M.; Fullam, J.; Doyle, G.; Slonska, Z.; Kondilis, B.; Stoffels, V.; Osborne, R.H.; Brand, H.; et al. Measuring health literacy in populations: Illuminating the design and development process of the European Health Literacy Survey Questionnaire (HLS-EU-Q). BMC Public Health 2013, 13, 1–10. [Google Scholar] [CrossRef]
- Duong, T.V.; Aringazina, A.; Baisunova, G.; Nurjanah; Pham, T.V.; Pham, K.M.; Truong, T.Q.; Nguyen, K.T.; Oo, W.M.; Mohamad, E.; et al. Measuring health literacy in Asia: Validation of the HLS-EU-Q47 survey tool in six Asian countries. J. Epidemiol. 2017, 27, 80–86. [Google Scholar] [CrossRef]
- Nakayama, K.; Osaka, W.; Togari, T.; Ishikawa, H.; Yonekura, Y.; Sekido, A.; Matsumoto, M. Comprehensive health literacy in Japan is lower than in Europe: A validated Japanese-language assessment of health literacy. BMC Public Health 2015, 15, 505. [Google Scholar] [CrossRef]
- Pelikan, J.M.; Ganahl, K. Measuring Health Literacy in General Populations: Primary Findings from the HLS-EU Consortium’s Health Literacy Assessment Effort. Stud. Health Technol Inform. 2017, 240, 34–59. [Google Scholar]
- Toci, E.; Burazeri, G.; Sorensen, K.; Kamberi, H.; Brand, H. Concurrent validation of two key health literacy instruments in a South Eastern European population. Eur. J. Public Health 2015, 25, 482–486. [Google Scholar] [CrossRef]
- Bröder, J.; Okan, O.; Bauer, U.; Schlupp, S.; Pinheiro, P. Advancing perspectives on health literacy in childhood and youth. Health Promot. Int. 2019, 1–11. [Google Scholar] [CrossRef]
- Prüfer, P.; Rexroth, M. Zwei-Phasen-Pretesting. Available online: http://www.gesis.org/fileadmin/upload/forschung/publikationen/gesis_reihen/zuma_arbeitsberichte/00_08.pdf (accessed on 23 April 2015).
- Abel, T.; Hofmann, K.; Ackermann, S.; Bucher, S.; Sakarya, S. Health literacy among young adults: A short survey tool for public health and health promotion research. Health Promot. Int. 2015, 30, 725–735. [Google Scholar] [CrossRef]
- Weiss, B.D.; Mays, M.Z.; Martz, W.; Castro, K.M.; DeWalt, D.A.; Pignone, M.P.; Mockbee, J.; Hale, F.A. Quick assessment of literacy in primary care: The newest vital sign. Ann. Fam Med. 2005, 3, 514–522. [Google Scholar] [CrossRef]
- Weiss, B.D. The Newest Vital Sign: Frequently Asked Questions. HLRP Health Lit. Res. Pract. 2018, 2, e125–e127. [Google Scholar] [CrossRef] [PubMed]
- Linnebur, L.A.; Linnebur, S.A. Self-Administered Assessment of Health Literacy in Adolescents Using the Newest Vital Sign. Health Promot. Pract. 2018, 19, 119–124. [Google Scholar] [CrossRef] [PubMed]
- Warsh, J.; Chari, R.; Badaczewski, A.; Hossain, J.; Sharif, I. Can the Newest Vital Sign Be Used to Assess Health Literacy in Children and Adolescents? Clin. Pediatrics 2013. [Google Scholar] [CrossRef] [PubMed]
- Schwarzer, R.; Jerusalem, M.H. Scales for Recording Teacher and Student Characteristics. Documentation of the Psychometric Procedures within the Framework of the Scientific Monitoring of the Pilot Project Self-Effective Schools; Berlin, 1999, ISBN 3-00-003708-X. Available online: http://www.psyc.de/skalendoku.pdf (accessed on 20 April 2020).
- Zimet, G.D.; Powell, S.S.; Farley, G.K.; Werkman, S.; Berkoff, K.A. Psychometric characteristics of the Multidimensional Scale of Perceived Social Support. J. Pers. Assess. 1990, 55, 610–617. [Google Scholar]
- Hartley, J.E.; Levin, K.; Currie, C. A new version of the HBSC Family Affluence Scale - FAS III: Scottish Qualitative Findings from the International FAS Development Study. Child. Indic. Res. 2016, 9, 233–245. [Google Scholar] [CrossRef] [PubMed]
- Bucksch, J.; Finne, E.; Gohres, H.; Bilz, L.; Moor, I.; Richter, M.; Kolip, P. Die Methodik des HBSC-Surveys 2013/14. In Schule und Gesundheit. Ergebnisse des WHO-Jugendgesundheitssurveys “Health Behaviour in School-aged Children”; Bilz, L., Sudeck, G., Bucksch, J., Klocke, A., Kolip, P., Melzer, W., Ravens-Sieberer, U., Richter, M., Deutschland, H.-S., Eds.; Beltz Juventa: Weinheim, Germany, 2016; pp. 35–46. ISBN 978-3-7799-1991-9. [Google Scholar]
- Bildungsinstitut Bildungsforschung (BIFIE). Materials. PISA 2015. Student Questionnaire. [Materialien. PISA 2015. Schülerfragebogen]. Available online: https://www.bifie.at/wp-content/uploads/2017/04/Schuelerfragebogen.pdf (accessed on 14 August 2018).
- Bühner, M. Einführung in die Test.-und Fragebogenkonstruktion, 3rd ed.; Pearson Deutschland GmbH: Hallbergmoos, Germany, 2011; ISBN 3868940332. [Google Scholar]
- Kelava, A.; Moosbrugger, H. Deskriptivstatistische Evaluation von Items (Itemanalyse) und Testwertverteilungen. In Testtheorie und Fragebogenkonstruktion, 2nd ed.; Moosbrugger, H., Kelava, A., Eds.; Springer: Heidelberg, Germany, 2012; pp. 73–98. ISBN 978-3-540-71635-8. [Google Scholar]
- Terwee, C.B.; Bot, S.D.; de Boer, M.R.; van der Windt, D.A.; Knol, D.L.; Dekker, J.; Bouter, L.M.; de Vet, H.C. Quality criteria were proposed for measurement properties of health status questionnaires. J. Clin. Epidemiol. 2007, 60, 34–42. [Google Scholar] [CrossRef] [PubMed]
- West, S.G.; Finch, J.F.; Curran, P.J. Structural equation models with nonnormal variables: Problems and remedies. In Structural Equation Modeling: Concepts, Issues, and Applications; Sage Publications, Inc.: Thousand Oaks, CA, USA, 1995; pp. 56–75, ISBN 0-8039-5317-8 (Hardcover); 0-8039-5318-6 (Paperback). [Google Scholar]
- Edwards, J.R.; Bagozzi, R.P. On the Nature and Direction of Relationship Betwenn Costructs and Measures. Psychol. Methods 2000, 5, 155–174. [Google Scholar] [CrossRef]
- Bollen, K.A. Multiple indicators: Internal consistency or no necessary relationship? Quality Quant. 1984, 18, 377–385. [Google Scholar] [CrossRef]
- Lane, H.G.; Aldoory, L. Recommendations for Measurment of Child Health Literacy: A Pragmatic Approach. Health Literacy Res. Pract. 2019, 3, e165–e169. [Google Scholar] [CrossRef] [PubMed]
- Gellert, P.; Tille, F. What do we know so far? The role of health knowledge withhin theories of halth literacy. Eur. Health Psychl. 2015, 17, 266–274. [Google Scholar]
- Brown, T.A. Confirmatory Factor Analysis for Applied Research, 2nd ed.; The Guilford Press: New York, NY, USA, 2015; ISBN 978-1-4625-1536-3. [Google Scholar]
- Schreiber, J.B.; Nora, A.; Stage, F.K.; Barlow, E.A.; King, J. Reporting Structural Equation Modeling and Confirmatory Factor Analysis Results: A Review. J. Educ. Res. 2006, 99, 323–338. [Google Scholar] [CrossRef]
- Hu, L.T.; Bentler, P.M. Cutoff Criteria for Fit Indexes in Covariance Structure Analysis: Conventional Criteria Versus New Alternatives. Structural Equation Modeling—A Multidisciplinary Journal 1999, 6, 1–55. [Google Scholar] [CrossRef]
- Yu, C.-Y. Evaluating Cutoff Criteria of Model Fit Indices for Latent Variable Models with Binary and Continuous Outcomes. Doctoral Dissertation, University of California, Los Angeles, CA, USA, 2002. [Google Scholar]
- Browne, M.W.; Cudeck, R. Alternative Ways of Assessing Model Fit. Sociol. Methods Res. 1992, 21, 230–258. [Google Scholar] [CrossRef]
- Röthlin, F.; Pelikan, J.M.; Ganahl, K. Die Gesundheitskompetenz von 15-jährigen Jugendlichen in Österreich. Abschlussbericht der österreichischen Gesundheitskompetenz Jugendstudie im Auftrag des Hauptverbands der österreichischen Sozialversicherungsträger (HVSV); Ludwig Boltzmann Institut Health Promotion Research (LBIHPR): Wien, Austria, 2013. [Google Scholar]
- HLS-EU Consortium. Comparative report on health litercy in eight EU members states. The European Health Literacy Survey HLS-EU (Second Reviesed and Extended Version, Date July 22th, 2014). Available online: https://cdn1.sph.harvard.edu/wp-content/uploads/sites/135/2015/09/neu_rev_hls-eu_report_2015_05_13_lit.pdf (accessed on 3 December 2019).
- Berkman, N.D.; Sheridan, S.L.; Donahue, K.E.; Halpern, D.J.; Viera, A.; Crotty, K.; Holland, A.; Brasure, M.; Lohr, K.N.; Harden, E.; et al. Health literacy interventions and outcomes: An updated systematic review. Evid Rep. Technol Assess. (Full Rep.) 2011, 1–941. [Google Scholar]
- Driessnack, M.; Chung, S.; Perkhounkova, E.; Hein, M. Using the "Newest Vital Sign" to assess health literacy in children. J. Pediatr. Health Care 2014, 28, 165–171. [Google Scholar] [CrossRef]
- Yu, X.; Yang, T.; Wang, S.; Zhang, X. Study on student health literacy gained through health education in elementary and middle schools in China. Health Educ. J. 2012, 71, 452–460. [Google Scholar] [CrossRef]
- Chinn, D.; McCarthy, C. All Aspects of Health Literacy Scale (AAHLS): Developing a tool to measure functional, communicative and critical health literacy in primary healthcare settings. Patient Educ. Couns. 2013, 90, 247–253. [Google Scholar] [CrossRef]
- Ghanbari, S.; Ramezankhani, A.; Montazeri, A.; Mehrabi, Y. Health Literacy Measure for Adolescents (HELMA): Development and Psychometric Properties. PLoS ONE 2016, 11, e0149202. [Google Scholar] [CrossRef]
- Massey, P.; Prelip, M.; Calimlim, B.; Afifi, A.; Quiter, E.; Nessim, S.; Wongvipat-Kalev, N.; Glik, D. Findings toward a multidimensional measure of adolescent health literacy. Am. J. Health Behav. 2013, 37, 342–350. [Google Scholar] [CrossRef]
- Vardavas, C.I.; Kondilis, B.K.; Patelarou, E.; Akrivos, P.D.; Falagas, M.E. Health literacy and sources of health education among adolescents in Greece. Int. J. Adolesc. Med. Health 2009, 21, 179–186. [Google Scholar] [CrossRef] [PubMed]
- Messer, M.; Vogt, D.; Quenzel, G.; Schaeffer, D. Health Literacy bei vulnerablen Zielgruppen. Präv. Gesundheitsf. 2016, 11, 110–116. [Google Scholar] [CrossRef]
- Messer, M.V.D.; Quenzel, G.; Schaeffer, D. Fragebogen HLS-NRW-Q. Anlage zur Publikation: Health Literacy bei vulnerablen Zielgruppen: Entwicklung und Konzeption des HLS-NRW-Q Fragebogens. Prävention und Gesundheitsförderung. 2016. Available online: https://www.uni-bielefeld.de/gesundhw/ag6/downloads/Fragebogen_HLS-NRW-Q.pdf (accessed on 20 May 2016).
- Gould, S.J. Health consciousness and health behavior: The application of a new health consciousness scale. Am. J. Prev. Med. 1990, 6, 228–237. [Google Scholar] [CrossRef]
- Bundeszentrale für gesundheitliche Aufklärung (BZgA). drugcom.de. Available online: http://www.drugcom.de/wissenstests/ (accessed on 12 May 2016).
- Bundesministerium für Ernährung und Landwirtschaft (BMEL). Quiz zur Lebensmittelkennzeichnung. Available online: https://www.bmel-durchblicker.de/fileadmin/user_upload/Kinderquiz-IGW-2015.pdf (accessed on 12 May 2016).
- Statistisches Bundesamt (Destatis). Bevölkerung und Erwerbstätigkeit. Bevölkerung mit Migrationshintergrund - Ergebnisse des Mikrozensus - 2016. Fachserie 1 Reihe 2.2; Statistisches Bundesamt (Destatis): Wiesbaden, Germany, 2017. [Google Scholar]
- Paek, H.J.; Reber, B.H.; Lariscy, R.W. Roles of interpersonal and media socialization agents in adolescent self-reported health literacy: A health socialization perspective. Health Educ. Res. 2011, 26, 131–149. [Google Scholar] [CrossRef] [PubMed]
- Schmidt-Denter, U.; Schick, H. Kurzform des Fragebogens zur personalen und sozialen Identität von Jugendlichen und Erwachsenen (FPSI-K); Universität zu Köln: Köln, Germany, 2005. [Google Scholar]
- Lohaus, A.; Schmitt, G.M. Kontrollüberzeugungen zu Krankheit und Gesundheit (KKG): Bericht über die Entwicklung eines Testverfahrens. Diagnostica 1989, 35, 59–72. [Google Scholar]
- Paek, H.J.; Hove, T. Social cognitive factors and perceived social influences that improve adolescent eHealth literacy. Health Commun. 2012, 27, 727–737. [Google Scholar] [CrossRef]
- ABDA - Bundesvereinigung Deutscher Apothekerverbände e.V. Aponet.de. Wissenstest: Sind Sie Erste-Hilfe-tauglich? Available online: https://www.aponet.de/service/checklisten-und-tests/wissenstests/erste-hilfe.html (accessed on 20 February 2016).
- Bax, C. Beipackzettel lesen und verstehen. Arbeitseinheit im Rahmen des ESF - Projekts, “Alphabetisierung- Grundbildung- Gesundheit”. 2008. Available online: http://docplayer.org/28681859-Arbeitseinheit-im-rahmen-des-esf-projekts-alphabetisierung-grundbildung-gesundheit-beipackzettel-lesen-und-verstehen.html (accessed on 20 April 2020).
- Jessor, R.; Turbin, M.S.; Costa, F.M. Predicting developmental change in healthy eating and regular exercise among adolescents in China and the United States: The role of psychosocial and behavioral protection and risk. J. Res. Adolesc. 2010, 20, 707–725. [Google Scholar] [CrossRef]
- Bollweg, T.M.; Okan, O.; Fretian, A.M.; Bröder, J.; Domanska, O.; Jordan, S.; Bruland, D.; Pinheiro, P.; Bauer, U. Adapting the European Health Literacy Survey Questionnaire for 4th-Grade students in Germany: Validation and Psychometric Analysis. Health Literacy Res. Pract. (in press).
- Manganello, J.A.; DeVellis, R.F.; Davis, T.C.; Schottler-Thal, C. Development of the Health Literacy Assessment Scale for Adolescents (HAS-A). J. Commun. Healthc. 2015, 8, 172–184. [Google Scholar] [CrossRef]
- Finbraten, H.S.; Pettersen, K.S.; Wilde-Larsson, B.; Nordstrom, G.; Trollvik, A.; Guttersrud, O. Validating the European Health Literacy Survey Questionnaire in people with type 2 diabetes: Latent trait analyses applying multidimensional Rasch modelling and confirmatory factor analysis. J. Adv. Nurs 2017. [Google Scholar] [CrossRef] [PubMed]
- Nunnally, J.C. Psychometric Theory, 2nd ed.; McGraw-Hill.: New York, NY, USA, 1978. [Google Scholar]
- Danner, D. Reliabilität - die Genauigkeit einer Messung; GESIS - Leibniz-Instiut für Sozialwissenschaften (GESIS Survey Guidelines): Mannheim, Germany, 2015; pp. 1–12. [Google Scholar]
- Cortina, J.M. What is coefficient alpha? An examination of theory and applications. J. Appl. Psychol. 1993, 78, 98–104. [Google Scholar] [CrossRef]
- McCormack, L.; Haun, J.; Sorensen, K.; Valerio, M. Recommendations for advancing health literacy measurement. J. Health Commun 2013, 18 (Suppl. 1), 9–14. [Google Scholar] [CrossRef]
- Basch, C.H.; MacLean, S.A.; Romero, R.-A.; Ethan, D. Health Information Seeking Behavior Among College Students. J. Commun. Health 2018, 43, 1094–1099. [Google Scholar] [CrossRef] [PubMed]
- Chang, F.C.; Chiu, C.H.; Chen, P.H.; Miao, N.F.; Lee, C.M.; Chiang, J.T.; Pan, Y.C. Relationship Between Parental and Adolescent eHealth Literacy and Online Health Information Seeking in Taiwan. Cyberpsychol. Behav. Soc. Netw. 2015, 18, 618–624. [Google Scholar] [CrossRef]
- Chisolm, D.J.; Sarkar, M.; Kelleher, K.J.; Sanders, L.M. Predictors of Health Literacy and Numeracy Concordance Among Adolescents With Special Health Care Needs and Their Parents. J. Health Commun. 2015, 20 (Suppl. 2), 43–49. [Google Scholar] [CrossRef]
- Abel, T.; Sommerhalder, K. Gesundheitskompetenz/Health Literacy: Das Konzept und seine Operationalisierung. Bundesgesundheitsblatt Gesundheitsforschung Gesundheitsschutz 2015, 58, 923–929. [Google Scholar] [CrossRef]
- Guo, S.; Davis, E.; Yu, X.; Naccarella, L.; Armstrong, R.; Abel, T.; Browne, G.; Shi, Y. Measuring functional, interactive and critical health literacy of Chinese secondary school students: Reliable, valid and feasible? Glob. Health Promot. 2018. [Google Scholar] [CrossRef]
- Olyani, S.; Tehrani, H.; Esmaily, H.; Rezaii, M.M.; Vahedian-Shahroodi, M. Assessment of health literacy with the Newest Vital Sign and its correlation with body mass index in female adolescent students. Int. J. Adolesc. Med. Health 2017. [Google Scholar] [CrossRef]
- Senatsverwaltung für Gesundheit; Pflege und Gleichstellung Berlin Brandenburg. Amt für Statistik Berlin-Brandenburg. Gender Datenreport Berlin 2017. Available online: https://www.statistik-berlin-brandenburg.de/gender/kapitel/pdf/Gender_datenreport_2017.pdf (accessed on 8 August 2019).

| Topic of the Scale (No. of items) | Theoretical Key Dimension | Specified, Evaluated Health Literacy Attributes |
|---|---|---|
| A Dealing with health-related information (16 items) | cognitive | understanding, appraising, critical thinking, and functional literacy skills |
| behavioral | information seeking, application of health information | |
| B Communication and interaction skills (5 items) | behavioral /communicative | skills to communicate and interact about health information |
| C Attitudes toward one’s own health and health information (7 items) | affective/conative | self-awareness, self-control, self-efficacy, motivation, interest |
| D Health-related knowledge (10 items) | cognitive | knowledge about physical activity; the health risks of alcohol use, cannabis use and smoking; the emergency number; first aid measures in case of skin burns; medication leaflets; nutrition labels; patient rights; ways of transmitting HIV/AIDS |
| E Support for health-related issues by social agents (5 items) | contextual factor affecting individual health literacy | competencies of social agents, including doctors, parents, and friends, for communication and provision of support related to health topics |
| 43 items |
| Total | Percentage | Missing Values | |
|---|---|---|---|
| (n) | % | (n)% | |
| Demographic characteristics | |||
| Sex | (0) 0.00 | ||
| Girl | (367) | 58.72 | |
| Boy | (258) | 41.28 | |
| Age | (0) 0.00 | ||
| 14 years | (159) | 25.44 | |
| 15 years | (165) | 26.40 | |
| 16 years | (145) | 23.20 | |
| 17 years | (156) | 24.96 | |
| Socioeconomic characteristics | |||
| Are you going to school? | (4) 0.64 | ||
| Yes | (586) | 93.76 | |
| No | (35) | 5.60 | |
| Educational level | (9) 1.44 | ||
| No high school certificate | (120) | 19.20 | |
| High school certificate | (467) | 74.72 | |
| I do not know yet | (29) | 4.64 | |
| Family affluence | (5) 0.80 | ||
| Low | (136) | 21.76 | |
| Medium | (379) | 60.64 | |
| High | (105) | 16.80 | |
| Migration background | (7) 1.12 | ||
| None/German | (347) | 55.52 | |
| One-sided | (109) | 17.44 | |
| Two-sided | (162) | 25.92 |
| Var. Name | Scale A Dealing with Health-Related Information * How Easy or Difficult Is It for You to? | Source of Item | N | Missing [%] (n) | Mean | Skewness | Kurtosis | Variance | Cronbach’s α | ITC | Excluded in Step |
|---|---|---|---|---|---|---|---|---|---|---|---|
| info1 | …find information about what to do when you feel ill to make yourself get better? | HLS-EU-Q47 [34] (Q1) | 622 | 0.48 (3) | 3.37 | −0.50 | 3.11 | 0.36 | 0.775 | 0.46 | |
| info2 | …find information about what you can do in case of a medical emergency? e.g., an accident, severe skin burn, alcohol poisoning | HLS-EU-Q47 [34] (Q3) | 623 | 0.32 (2) | 3.15 | −0.30 | 2.74 | 0.44 | 0.780 | 0.40 | 2 |
| info3 | …understand a medication leaflet | HLS-EU-Q47 [34] (Q6) | 616 | 1.44 (9) | 3.03 | −0.38 | 2.58 | 0.60 | 0.783 | 0.36 | |
| info4 | …judge which information about an illness in the media you can trust and which you cannot? media: internet, TV, radio, press | HLS-EU-Q47 [34] (Q12) | 622 | 0.48 (3) | 2.58 | 0.09 | 2.59 | 0.58 | 0.776 | 0.44 | |
| info5 | ...follow the instructions of your doctor or pharmacist? | HLS-EU-Q47 [34] (Q16) | 622 | 0.48 (3) | 3.48 | −0.80 | 3.39 | 0.35 | 0.781 | 0.39 | |
| info6 | ...find information about how you can deal with mental problems? e.g., permanent stress, depression, being bullied, eating disorder | HLS-EU-Q47 [34] (Q18) | 618 | 1.12 (7) | 2.84 | −0.19 | 2.39 | 0.66 | 0.773 | 0.48 | |
| info7 | ...understand how you can protect yourself against sexually transmitted diseases? By sexually transmitted diseases we mean diseases such as HIV/AIDS, chlamydia infection, or herpes. | HLS-EU-Q47 [34] (Q19) | 620 | 0.80 (5) | 3.53 | −1.17 | 4.17 | 0.39 | 0.778 | 0.43 | |
| info8 | ...judge whether you can trust the media when they warn you of health risks? | HLS-EU-Q47 [34] (Q28) | 619 | 0.96 (6) | 2.69 | 0.10 | 2.51 | 0.53 | 0.779 | 0.42 | |
| info9 | …implement advice from your family so you do not get sick? | HLS-EU-Q47 [34] (Q30) | 620 | 0.80 (5) | 3.12 | −0.47 | 2.79 | 0.54 | 0.789 | 0.29 | |
| info10 | …ask your friends for health tips? | HLS-EU-Q47 [34] (Q30) | 619 | 0.96 (6) | 2.94 | −0.38 | 2.79 | 0.60 | 0.783 | 0.37 | 2 |
| info11 | ...find information about healthy behavior such as exercise and nutrition? | HLS-EU-Q47 [34] (Q32) | 623 | 0.32 (2) | 3.41 | −0.63 | 2.40 | 0.42 | 0.774 | 0.47 | |
| info12 | ...understand information on food packaging? | HLS-EU-Q47 [34] (Q38) | 624 | 0.16 (1) | 3.13 | −0.53 | 2.33 | 0.69 | 0.775 | 0.46 | |
| info13 | ...judge how what you do daily affects your health? e.g., eating, drinking, exercise, relaxation, body care | HLS-EU-Q47 [34] (Q43) | 622 | 0.48 (3) | 3.02 | −0.28 | 2.21 | 0.64 | 0.770 | 0.52 | |
| info14 | ...get involved in promoting a healthier life in your neighborhood? e.g., more parks and sports grounds, less noise and traffic, better air quality | HLS-EU-Q47 [34] (Q47) | 620 | 0.80 (5) | 1.95 | 0.59 | 2.90 | 0.66 | 0.794 | 0.23 | 1 |
| Test scale A (without item 15 and 16) | 0.792 a | ||||||||||
| info15girls | ...understand information about the vaccination against cervical cancer (HPV)? | HLS-EU-Q47 [34] (Q23) | 367 | 1.09 (4) | 3.07 | −0.54 | 2.90 | 0.61 | NC | NC | 1 |
| info16 boys | ...understand how to use condoms? | HLS-EU-Q47 [34] (Q23) | 258 | 5.81 (15) | 3.50 | −1.57 | 5.89 | 0.47 | NC | NC | 1 |
| B Interactions and communication skills To what extent do you agree with the following sentences? | Source of item | N | Missing [%] (n) | Mean | Skewness | Kurtosis | Variance | Cronbach’s α | ITC | Excluded in step | |
| com1 | When you think about your last visit to the doctor, did you ask all the questions that interested you? | HELMA [70] (Q37) | 621 | 0.64 (4) | 3.01 | −0.41 | 2.43 | 0.69 | 0.514 | 0.39 | |
| com2 | I chat with my friends about how one can avoid unhealthy behavior, e.g., smoking, drinking over the limit. | HELMA [70] (Q41) | 621 | 0.64 (4) | 2.75 | −0.17 | 2.18 | 0.82 | 0.546 | 0.33 | |
| com3 | If my friends or siblings have questions about health, I can help them. | HLAT-8 [41] (Q5) | 620 | 0.80 (5) | 3.04 | −0.35 | 3.05 | 0.47 | 0.495 | 0.42 | |
| com4 | It is easy for me to talk with my parents about topics about health. | Peak et al. 2011 [79] | 622 | 0.48 (3) | 3.31 | −0.93 | 3.27 | 0.60 | 0.515 | 0.39 | |
| com5 | I talk to people at school or at the workplace if I have stress or problems, e.g., with a school social worker/school teacher. | Peak et al. 2011 [79] | 619 | 0.96 (6) | 2.24 | 0.33 | 2.00 | 1.03 | 0.604 | 0.22 | 1 |
| Test scale B | 0.591 a | ||||||||||
| C Attitudes toward one’s own health and health information To what extent do you agree with the following sentences? | Source of item | N | Missing [%] (n) | Mean | Skewness | Kurtosis | Variance | Cronbach’s α | ITC | Excluded in step | |
| att1 | How much in general do you pay attention to your health? | Health Consciousness Scale [75] | 621 | 0.64 (4) | 3.38 | −0.03 | 3.28 | 0.60 | 0.548 | 0.34 | |
| att2 | I am aware of my physical condition throughout the day. | Health Consciousness Scale [75] | 623 | 0.32 (2) | 4.31 | −0.88 | 4.54 | 0.44 | 0.541 | 0.36 | 1 |
| att3 | I feel very quickly when my mood is changing. | FPSI-K [80] | 623 | 0.32 (2) | 4.35 | −1.37 | 5.11 | 0.64 | 0.582 | 0.24 | 1 |
| att4 | I seek advice from others when I am ill. | Locus of Control about illness and health [81] | 623 | 0.32 (2) | 3.62 | −0.56 | 2.47 | 1.18 | 0.575 | 0.26 | |
| att5 | It is up to me to protect myself from diseases. | Locus of Control about illness and health [81] | 618 | 1.12 (7) | 4.14 | −1.05 | 4.52 | 0.67 | 0.549 | 0.34 | |
| att6 | I can influence whether or not I feel well. | Locus of Control about illness and health [81] | 621 | 0.64 (4) | 3.77 | −0.64 | 2.84 | 1.06 | 0.575 | 0.26 | |
| att7 | It is important to me to know about health issues. | Health Motivation [82] | 623 | 0.32 (2) | 3.64 | −0.44 | 2.45 | 1.04 | 0.530 | 0.39 | |
| 7 | Test scale C | 0.595 a | |||||||||
| D Health-related knowledge | Source of item | N | Missing [%] (n) | Mean/item difficulty | Skewness | Kurtosis | Variancea | KR-20 | ITCa | Excluded in step | |
| know1 | How often should a young person at your age to be physically active? | Health quiz [22] | 624 | 0.16 (1) | 0.32 | n.a. | n.a. | 0.22 | n.a. | 0.05 | |
| know2 | How does it affect the body if you regularly drink a lot of alcohol? | Quiz drug com [76] | 625 | 0.00 (0) | 0.43 | n.a. | n.a. | 0.25 | n.a. | 0.09 | |
| know3 | What are the health effects for young people of consuming cannabis (marijuana, hashish) often? | Quiz drug com [76] | 625 | 0.00 (0) | 0.45 | n.a. | n.a | 0.25 | n.a. | 0.08 | |
| know4 | What is not one of the possible effects of smoking? | Quiz drug com [76] | 622 | 0.48 (3) | 0.56 | n.a. | n.a. | 0.25 | n.a. | 0.10 | |
| know5 | What phone number do you need to dial if you need an ambulance? | HLS-NRW-Q [74] | 620 | 0.80 (5) | 0.97 | n.a. | n.a. | 0.03 | n.a. | −0.04 | 1 |
| know6 | How can small burns be treated? | Quiz aponet [83] | 624 | 0.16 (1) | 0.66 | n.a. | n.a. | 0.23 | n.a. | 0.13 | |
| know7 | Under which keyword does a medication package leaflet describe the undesirable effect of the medicine? | Educational material about medication leaflet [84] | 624 | 0.16 (1) | 0.95 | n.a. | n.a. | 0.05 | n.a. | 0.27 | 1 |
| know8 | Which ingredient is contained in the highest amount in a cocoa drink powder with the ingredients listed on the package as follows: sugar, dextrose, low-fat cocoa drink powder, emulsifying agent (lecithin), salt? | Food label quiz [77] | 623 | 0.16 (2) | 0.80 | n.a. | n.a. | 0.16 | n.a. | 0.17 | |
| know8 | We want to know if you know what your rights are. Which of the above statements is incorrect? | Massey et al. [71] (Q14) | 622 | 0.16 (3) | 0.39 | n.a. | n.a. | 0.24 | n.a. | 0.07 | |
| know 10 | How can HIV/AIDS be transmitted? | self-developed | 622 | 0.16 (3) | 0.70 | n.a. | n.a. | 0.21 | n.a. | 0.06 | |
| Test scale D | 0.63 | 0.263 b | |||||||||
| E Support for health-related issues by social agents | N | Missing [%] (n) | Mean | Skewness | Kurtosis | Variance | Cronbach’s α | ITC | Excluded in step | ||
| cont1 | Thinking about your last visit to the doctor, did your doctor explain everything to you so that you understood it? | Massey [71] (Q2) | 621 | 0.64 (4) | 3.52 | −1.21 | 4.24 | 0.41 | 0.332 | 0.13 | 1 |
| cont2 | At school/work, there are people who help me if I have stress or problems. | self-developed | 622 | 0.48 (3) | 3.08 | −0.55 | 2.50 | 0.73 | 0.247 | 0.23 | 1 |
| cont4 | My family helps me when I have questions about health. | HLAT-8 [41](Q6) | 621 | 0.64 (4) | 3.59 | −1.55 | 5.40 | 0.39 | 0.245 | 0.23 | 1 |
| cont4 | If you do something that harms your health, would your friends try to dissuade you of that? | Jessor et al. [85] | 621 | 0.64 (4) | 3.31 | −0.85 | 3.15 | 0.57 | 0.286 | 0.18 | 1 |
| cont5 | I usually can use the internet alone and undisturbed. | Peak et al. 2011 [84] | 620 | 0.80 (5) | 3.80 | −2.61 | 9.82 | 0.25 | 0.362 | 0.09 | 1 |
| Test scale E | 0.345 a |
| MOHLAA-Q Scale | Specified Measurement Model/Factor | No. | x2WLSMV(df) p-value | RMSEA | CFI | TLI | WRMR | Cronbach’s α |
|---|---|---|---|---|---|---|---|---|
| A Dealing with health-related information | Two-factor | 153.80 (42) p < 0.0001 | 0.068 | 0.947 | 0.931 | 1.134 | 0.772 | |
| f1 behavioral | 7 | |||||||
| f2 cognitive | 4 | |||||||
| B Communication and interaction skills | Single-factor f3 behavioral/communicative | 4 | 2.79 (2) p = 0.247 | 0.026 | 0.997 | 0.992 | 0.333 | 0.589 |
| C Attitudes toward one’s own health and health information | Single-factor f4 affective/conative | 5 | 15.69 (5) p = 0.008 | 0.061 | 0.964 | 0.928 | 0.626 | 0.539 |
| Overall model Scales A+B+C | Single-factor | 20 | 868.86 (170) p < 0.0001 | 0.084 | 0.821 | 0.800 | 1.783 | 0.824 |
| Overall model Scales A+B+C | Four-factor f1, f2, f3, f4 | 20 | 522.83 (163) p < 0.0001 | 0.062 | 0.908 | 0.893 | 1.336 | 0.824 |
| Scale | HLAT-8 | NVS | Self-Efficacy | Subjective Heath Status |
|---|---|---|---|---|
| n | (565) | (555) | (573) | (576) |
| Cronbach’s α coefficient/KR-20 | 0.673 | 0.756 a | 0.856 | n.a. |
| A Dealing with health-related information | 0.528 *** | 0.144 *** | 0.464 *** | −0.253 *** |
| B Communication and interaction skills | 0.484 *** | 0.028 (n.s.) | 0.383 *** | −0.209 *** |
| C Attitudes toward one’s own health and health information | 0.459 *** | 0.077 (n.s.) | 0.383 *** | −0.207 *** |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Domanska, O.M.; Bollweg, T.M.; Loer, A.-K.; Holmberg, C.; Schenk, L.; Jordan, S. Development and Psychometric Properties of a Questionnaire Assessing Self-Reported Generic Health Literacy in Adolescence. Int. J. Environ. Res. Public Health 2020, 17, 2860. https://doi.org/10.3390/ijerph17082860
Domanska OM, Bollweg TM, Loer A-K, Holmberg C, Schenk L, Jordan S. Development and Psychometric Properties of a Questionnaire Assessing Self-Reported Generic Health Literacy in Adolescence. International Journal of Environmental Research and Public Health. 2020; 17(8):2860. https://doi.org/10.3390/ijerph17082860
Chicago/Turabian StyleDomanska, Olga Maria, Torsten Michael Bollweg, Anne-Kathrin Loer, Christine Holmberg, Liane Schenk, and Susanne Jordan. 2020. "Development and Psychometric Properties of a Questionnaire Assessing Self-Reported Generic Health Literacy in Adolescence" International Journal of Environmental Research and Public Health 17, no. 8: 2860. https://doi.org/10.3390/ijerph17082860
APA StyleDomanska, O. M., Bollweg, T. M., Loer, A.-K., Holmberg, C., Schenk, L., & Jordan, S. (2020). Development and Psychometric Properties of a Questionnaire Assessing Self-Reported Generic Health Literacy in Adolescence. International Journal of Environmental Research and Public Health, 17(8), 2860. https://doi.org/10.3390/ijerph17082860





