Patient Assessment and Chronic Pain Self-Management in Ethnomedicine: Seasonal and Ecosystemic Embodiment in Ayurvedic Patient-Centered Care
Abstract
1. Introduction
Environment and Chronic Pain Management in Biomedicine
2. Methods
2.1. Participants and Procedures
2.2. Ethical Considerations
2.3. Case Study Approach Employing Inductive Qualitative Content Analysis
2.4. Validity and Reliability
3. Findings
3.1. Seasonal and Daily Cycles with Subjective Pain Perception
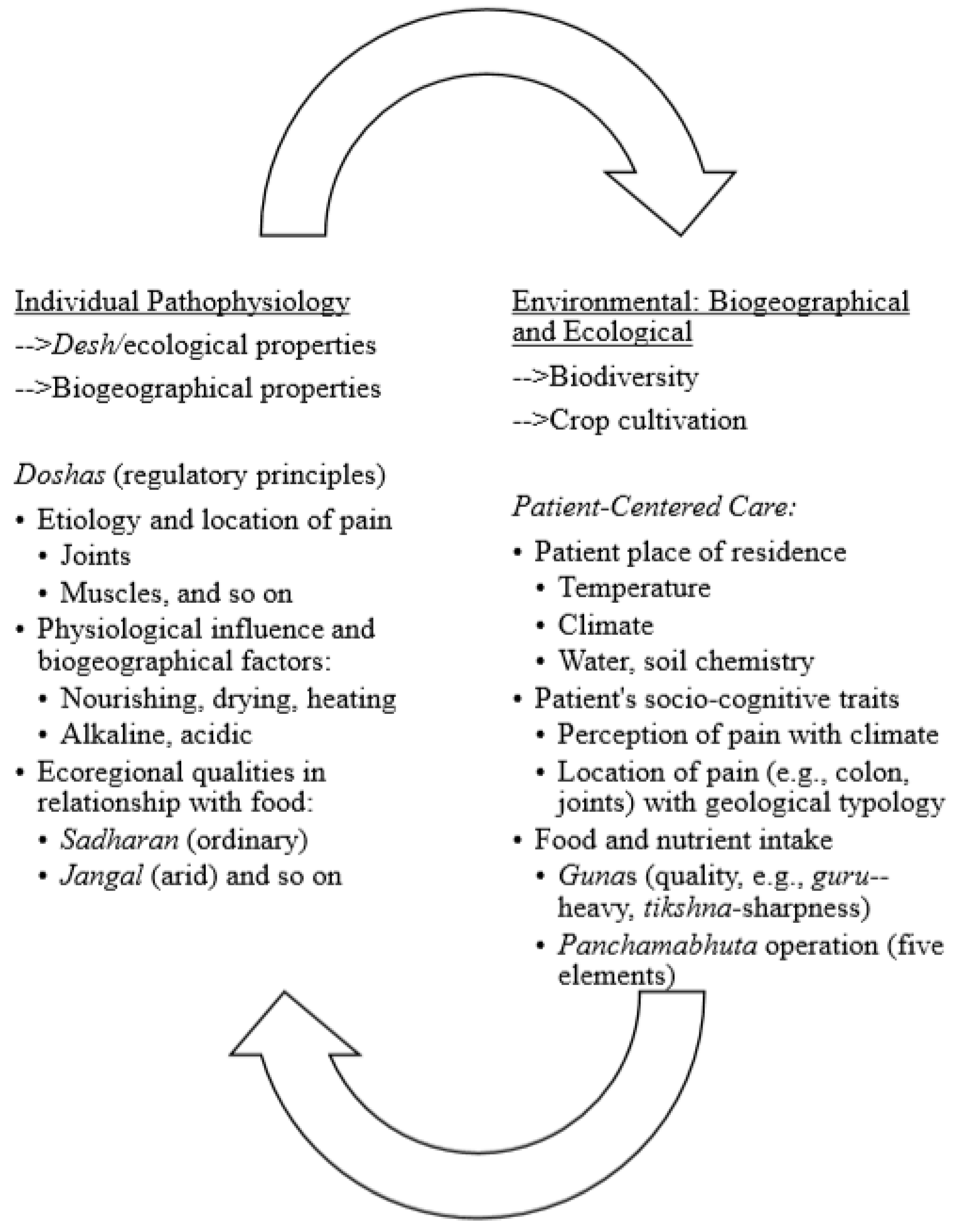
3.2. Biogeographical and Ecological Regions with Subjective Pain Perception
4. Discussion
4.1. Limitations
4.2. Pragmatic Recommendations
5. Conclusions
Funding
Conflicts of Interest
Appendix A
Interview Protocol Domains (Partial List)
- Communication of mind-body-spirit practices for chronic pain
- Ayurvedic protocol for increasing patient knowledge of their own body and managing pain with particular attention to patient dinacharya/ritucharya/dosha/phanchabhuta/guna/veerya/vipaka?
- The manas/atma element in Ayurvedic practices. Role of the patient and kal in treatment.
- Ayurveda’s description of the self (atman)-principle and its role in diagnosis and treatment in chronic pain. Mechanisms of operation of effective processes, identifying expected outcomes keeping in mind patient role and provider communication.
- Understanding the mind (manas) in experience (pragya) in addressing pain related conditions. Understanding the principle guiding the use of herbs (jadi/buti) with mind (manas) in chronic pain management.
- CAM practice protocol: Communicating the connection between diet (ahar) and mind (manas) with respect to chronic pain management in the Ayurvedic protocol. Understanding the positioning of the location (desha)/environment in diagnosis and treatment relationship.
- Focusing attention (man) and regulating emotions in mind-body practices: Understanding the role and principle of operation of ahar and vanaspati (herbs) in this cycle/relationship in the Ayurvedic protocol.
References
- Goldberg, D.S.; McGee, S.J. Pain as a global public health priority. BMC Public Health 2011, 11, 770. [Google Scholar] [CrossRef] [PubMed]
- Heyward, J.; Jones, C.M.; Compton, W.M.; Lin, D.H.; Losby, J.L.; Murimi, I.B.; Baldwin, G.T.; Ballreich, J.M.; Thomas, D.A.; Bicket, M.C.; et al. Coverage of Nonpharmacologic Treatments for Low Back Pain Among US Public and Private Insurers. JAMA Netw. Open 2018, 1, e183044. [Google Scholar] [CrossRef] [PubMed]
- Jensen, M.P.; Turner, J.A.; Romano, J.M.; Karoly, P. Coping with chronic pain: A critical review of the literature. Pain 1991, 47, 249–283. [Google Scholar] [CrossRef]
- Osterweis, M.; Kleinman, A.; Mechanic, D. (Eds.) Pain and Disability: Clinical, Behavioral, and Public Policy Perspectives; Institute of Medicine; Committee on Pain, Disability, and Chronic Illness Behavior; National Academies Press: Washington, DC, USA, 1987. [Google Scholar]
- Lee, C.; Crawford, C.; Swann, S. Active Self-Care Therapies for Pain (PACT) Working Group Multimodal, Integrative Therapies for the Self-Management of Chronic Pain Symptoms. Pain Med. 2014, 15, S76–S85. [Google Scholar] [CrossRef]
- McCormack, B.; McCance, T. Developing a conceptual framework for person centered nursing. J. Adv. Nurs. 2006, 56, 472–479. [Google Scholar] [CrossRef]
- Agarwal, V. Re-conceptualizing pain through patient-centered care in the complementary and alternative medicine therapeutic relationship. J. Adv. Nurs. 2018, 74, 2406–2415. [Google Scholar] [CrossRef]
- Little, P.; Everitt, H.; Williamson, I.; Warner, G.; Moore, M.; Gould, C.; Ferrier, K.; Payne, S. Observational study of effect of patient centeredness and positive approach on outcomes of general practice consultations. BMJ 2001, 323, 908–911. [Google Scholar] [CrossRef] [PubMed]
- Elder, C.; Ritenbaugh, C.; Aickin, M.; Hammerschlag, R.; Dworkin, S.; Mist, S.; Harris, R.E. Reductions in Pain Medication Use Associated with Traditional Chinese Medicine for Chronic Pain. Perm. J. 2012, 16, 18–23. [Google Scholar]
- Kanodia, A.K.; Legedza, A.T.R.; Davis, R.B.; Eisenberg, D.M.; Phillips, R.S. Perceived Benefit of Complementary and Alternative Medicine (CAM) for Back Pain: A National Survey. J. Am. Board Fam. Med. 2010, 23, 354–362. [Google Scholar] [CrossRef]
- Yuan, Q.-L.; Guo, T.-M.; Liu, L.; Sun, F.; Zhang, Y.-G. Traditional Chinese Medicine for Neck Pain and Low Back Pain: A Systematic Review and Meta-Analysis. PLoS ONE 2015, 10, e0117146. [Google Scholar] [CrossRef]
- Sharma, K.; Sahoo, J.; Sahu, D.; Chattopadhyay, A.; Kumar, S.; Mishra, S.S. Therapeutic evaluation of “Ayush Tulsi Jiwan Plus” oil for chronic musculoskeletal pain relief. AYU 2015, 36, 387–396. [Google Scholar] [CrossRef]
- Singh, H.; Bhushan, S.; Arora, S.; Buttar, H.S.; Arora, S.; Singh, B. Alternative treatment strategies for neuropathic pain: Role of Indian medicinal plants and compounds of plant origin—A review. Biomed. Pharmacother. 2017, 92, 634–650. [Google Scholar] [CrossRef]
- Singh, S.K.; Rajoria, K. Ayurvedic approach for management of ankylosing spondylitis: A case report. J. Ayurveda Integr. Med. 2016, 7, 53–56. [Google Scholar] [CrossRef][Green Version]
- Tekur, P.; Nagarathna, R.; Nagendra, H.R.; Haldavnekar, R.V. Effect of yogic colon cleansing (Laghu Sankhaprakshalana Kriya) on pain, spinal flexibility, disability and state anxiety in chronic low back pain. Int. J. Yoga 2014, 7, 111–119. [Google Scholar] [CrossRef]
- Kumar, S.; Dobos, G.J.; Rampp, T. The Significance of Ayurvedic Medicinal Plants. J. Evid.-Based Integr. Med. 2016, 22, 494–501. [Google Scholar] [CrossRef]
- Parsons, S.; Harding, G.; Breen, A.; Foster, N.; Pincus, T.; Vogel, S.; Underwood, M. Will shared decision making between patients with chronic musculoskeletal pain and physiotherapists, osteopaths and chiropractors improve patient care? Fam. Pract. 2011, 29, 203–212. [Google Scholar] [CrossRef]
- Astin, J.A. Why Patients Use Alternative Medicine. JAMA 1998, 279, 1548–1553. [Google Scholar] [CrossRef]
- Fleming, S.; Rabago, D.P.; Mundt, M.P.; Fleming, M.F. CAM therapies among primary care patients using opioid therapy for chronic pain. BMC Complement. Altern. Med. 2007, 7, 15. [Google Scholar] [CrossRef]
- Ndao-Brumblay, S.K.; Green, C.R. Predictors of Complementary and Alternative Medicine Use in Chronic Pain Patients. Pain Med. 2010, 11, 16–24. [Google Scholar] [CrossRef]
- Eisenberg, D.M.; Kessler, R.C.; Van Rompay, M.I.; Kaptchuk, T.J.; Wilkey, S.A.; Appel, S.; Davis, R.B. Perceptions about complementary therapies relative to conventional therapies among adults who use both: results from a national survey. Ann. Intern. Med. 2001, 135, 344–351. [Google Scholar] [CrossRef]
- Sherman, K.; Cherkin, D.C.; Connelly, M.T.; Erro, J.H.; Savetsky, J.B.; Davis, R.B.; Eisenberg, D.M. Complementary and alternative medical therapies for chronic low back pain: What treatments are patients willing to try? BMC Complement. Altern. Med. 2004, 4, 9. [Google Scholar] [CrossRef]
- Kessler, C.; Ostermann, T.; Meier, L.; Stapelfeldt, E.; Schütte, S.; Duda, J.; Michalsen, A. Additive Complex Ayurvedic Treatment in Patients with Fibromyalgia Syndrome Compared to Conventional Standard Care Alone: A Nonrandomized Controlled Clinical Pilot Study (KAFA Trial). Evid.-Based Complement. Altern. Med. 2013, 2013, 751403. [Google Scholar] [CrossRef] [PubMed]
- Naraindas, H. Of spineless babies and folic acid: Evidence and efficacy in biomedicine and ayurvedic medicine. Soc. Sci. Med. 2006, 62, 2658–2669. [Google Scholar] [CrossRef] [PubMed]
- Agarwal, V. Breaking Boundaries: Complementary and Alternative Medicine Provider Framing of Preventive Care. Qual. Health Res. 2017, 27, 2019–2029. [Google Scholar] [CrossRef] [PubMed]
- Mahesh, S.; Wele, A.; Patgiri, B.J.; Pórszász, R. Review of Pain: An Ayurvedic Approach. Int. Res. J. Pharm. 2019, 10. [Google Scholar] [CrossRef]
- Saper, R. Integrative Medicine and Health Disparities. Glob. Adv. Health Med. 2016, 5, 5–8. [Google Scholar] [CrossRef]
- Tan, G.; Craine, M.H.; Bair, M.J.; Garcia, M.K.; Giordano, J.; Jensen, M.P.; McDonald, S.M.; Patterson, D.; Sherman, R.A.; Williams, W.; et al. Efficacy of selected complementary and alternative medicine interventions for chronic pain. J. Rehabil. Res. Dev. 2007, 44, 195–222. [Google Scholar] [CrossRef]
- Chauhan, A.; Semwal, D.K.; Mishra, S.S.P.; Semwal, R.B. Ayurvedic research an methodology: Present status and future strategies. Ayush 2015, 36, 364–369. [Google Scholar] [CrossRef]
- Singh, R.H. Exploring issues in the development of Ayurvedic research methodology. J. Ayurveda Integr. Med. 2010, 1, 91–95. [Google Scholar] [CrossRef]
- Narahari, S.R.; Aggithaya, M.G.; Thamban, C.; Muralidharan, K.; Kanjarpane, A.B. How knowledgeable are investigators studying therapies of traditional medicines? Selendang Ayu Oil Spill Lessons Learn. 2014, 35, 243–251. [Google Scholar] [CrossRef]
- Ma, S.-X. Neurobiology of Acupuncture: Toward CAM. Evid.-Based Complement. Altern. Med. 2004, 1, 41–47. [Google Scholar] [CrossRef]
- Okada, K.; Kawakita, K. Analgesic Action of Acupuncture and Moxibustion: A Review of Unique Approaches in Japan. Evid.-Based Complement. Altern. Med. 2007, 6, 11–17. [Google Scholar] [CrossRef]
- Anyinam, C. Ecology and ethnomedicine: Exploring links between current environmental crisis and indigenous medical practices. Soc. Sci. Med. 1995, 40, 321–329. [Google Scholar] [CrossRef]
- Larme, A.C. Environment, vulnerability, and gender in Andean ethnomedicine. Soc. Sci. Med. 1998, 47, 1005–1015. [Google Scholar] [CrossRef]
- McOliver, C.A.; Camper, A.K.; Doyle, J.; Eggers, M.J.; E Ford, T.; Lila, M.A.; Berner, J.; Campbell, L.; Donatuto, J. Community-Based Research as a Mechanism to Reduce Environmental Health Disparities in American Indian and Alaska Native Communities. Int. J. Environ. Res. Public Health 2015, 12, 4076–4100. [Google Scholar] [CrossRef]
- Street, R.; Smith, M.; Moshabela, M.; Shezi, B.; Webster, C.; Falkenberg, T. Traditional health practitioners and sustainable development: A case study in South Africa. Public Health 2018, 165, 1–5. [Google Scholar] [CrossRef]
- Chorgade, M.S. Drug Discovery and Development; John Wiley: Hoboken, NJ, USA, 2007; Volume 2. [Google Scholar]
- Isaac, G.; Finn, S.; Joe, J.R.; Hoover, E.; Gone, J.; Lefthand-Begay, C.; Hill, S. Native American Perspectives on Health and Traditional Ecological Knowledge. Environ. Health Perspect. 2018, 126, 125002. [Google Scholar] [CrossRef]
- Rasmussen, S.J. Female sexuality, social reproduction, and the politics of medical intervention in Niger: Kel Ewey Tuareg perspectives. Cult. Med. Psychiatry 1994, 18, 433–462. [Google Scholar] [CrossRef]
- Patwardhan, B. Strengthening the Ayurveda ecosystem. J. Ayurveda Integr. Med. 2016, 7, 73–75. [Google Scholar] [CrossRef]
- Melzack, R.; Wall, P.D. Pain Mechanisms: A New Theory. Science 1965, 150, 971–978. [Google Scholar] [CrossRef]
- Bushnell, M.; Case, L.; Ceko, M.; Cotton, V.; Gracely, J.; Low, L.A.; Pitcher, M.; Villemure, C. Effect of environment on the long-term consequences of chronic pain. Pain 2015, 156, S42–S49. [Google Scholar] [CrossRef]
- Craig, A.D. A new view of pain as a homeostatic emotion. Trends Neurosci. 2003, 26, 303–307. [Google Scholar] [CrossRef]
- Ulrich, R. View through a window may influence recovery from surgery. Science 1984, 224, 420–421. [Google Scholar] [CrossRef]
- Tse, M.Y.M.; Ng, J.K.F.; Chung, J.; Wong, T.K.S. The effect of visual stimuli on pain threshold and tolerance. J. Clin. Nurs. 2002, 11, 462–469. [Google Scholar] [CrossRef]
- Perlman, D.M.; Salomons, T.; Davidson, R.J.; Lutz, A. Differential effects on pain intensity and unpleasantness of two meditation practices. Emotion 2010, 10, 65–71. [Google Scholar] [CrossRef]
- Zeidan, F.; Martucci, K.; Kraft, R.A.; Gordon, N.S.; McHaffie, J.G.; Coghill, R.C. Brain mechanisms supporting the modulation of pain by mindfulness meditation. J. Neurosci. 2011, 31, 5540–5548. [Google Scholar] [CrossRef]
- Bruehl, S.; Liu, X.; Burns, J.W.; Chont, M.; Jamison, R.N. Associations between daily chronic pain intensity, daily anger expression, and trait anger expressiveness: An ecological momentary assessment study. Pain 2012, 153, 2352–2358. [Google Scholar] [CrossRef]
- Skelly, A.C.; Chou, R.; Dettori, J.R.; Turner, J.A.; Friedly, J.L.; Rundell, S.D.; Fu, R.; Brodt, E.D.; Ngoc Wasson, B.S.; Cassandra, M.P.H.; et al. Noninvasive nonpharmacological treatment for chronic pain: A systematic review. In Comparative Effectiveness Review No. 209; Agency for Healthcare Research and Quality: Rockville, MD, USA, 2018. [Google Scholar]
- Center for Substance Abuse Treatment. Chronic pain management. In Managing Chronic Pain in Adults with or in Recovery from Substance Use Disorders; Substance Abuse and Mental Health Services Administration: Rockville, MD, USA, 2012; Volume 3. [Google Scholar]
- Hassed, C. Mind-body therapies—Use in chronic pain management. Aust. Fam. Physician 2013, 42, 112–117. [Google Scholar]
- Creswell, J.W. Research Design: Qualitative, Quantitative, and Mixed Methods Approaches; Sage: Thousand Oaks, CA, USA, 2013. [Google Scholar]
- Agarwal, V. The semi-structured interviewing method in a qualitative study examining complementary and alternative medicine providers’ knowledge discourse. Sage Res. Methods Cases Med. Health 2020. [Google Scholar]
- Yin, R.K. Case Study Research and Applications: Design and Methods; Sage: Thousand Oaks, CA, USA, 2018. [Google Scholar]
- Elo, S.; Kyngäs, H. The qualitative content analysis process. J. Adv. Nurs. 2008, 62, 107–115. [Google Scholar] [CrossRef]
- Strauss, A.L.; Corbin, J.M. Grounded Theory in Practice; Sage: Thousand Oaks, CA, USA, 1997. [Google Scholar]
- Jenkins, D.G.; Ricklefs, R.E. Biogeography and ecology: two views of one world. Philos. Trans. R. Soc. B Biol. Sci. 2011, 366, 2331–2335. [Google Scholar] [CrossRef]
- Golley, F.B. A History of the Ecosystem Concept in Ecology: More than the Sum of the Parts; Yale University Press: New Haven, CT, USA, 1996. [Google Scholar]
- Whittaker, R. Island Biogeography: Ecology, Evolution, and Conservation; Oxford University Press: New York, NY, USA, 1988. [Google Scholar]
- Moreau, A.; Carol, L.; Dedianne, M.C.; Dupraz, C.; Perdrix, C.; Lainé, X.; Souweine, G. What perceptions do patients have of decision making (DM)? Toward an integrative patient-centered care model. A qualitative study using focus-group interviews. Patient Educ. Couns. 2012, 87, 206–211. [Google Scholar] [CrossRef]
- Patton, M.Q. Qualitative Evaluation and Research Methods, 2nd ed.; Sage: Newbury Park, CA, USA, 1990. [Google Scholar]
- Agarwal, V. An Ecology of Wholeness: Medical Humanism, Chronic Illness, and the Body in Pain; Lexington Books: New York, NY, USA, pre-publication.

| Pseudonym | Age (Years) | Education | Specialty | Profession * | Employment (Years) *** | City † |
|---|---|---|---|---|---|---|
| A | 32 | MD Ayurveda ‡ (BAMS) | Dravyaguna | Ayurvedic Physician & Practitioner | 9 | Pune |
| B | 45 | MA, Ayurveda; MA, Sanskrit | Ayurvedic physician | 20 | Pune | |
| C | 44 | BAMS & MD, Ayurved | Kayachikitsa | Ayurvedic physician | 18 | Pune |
| D | 51 | BAMS Ayurveda MS in Ayurvedic Dietetics | Medicine & Surgery | Ayurveda physician/ practitioner | 27 | Mumbai |
| E | 33 | BAMS Ayurveda | Medicine & Surgery | Ayurveda physician/ practitioner | 10 | Mumbai |
| F | 26 | BAMS Ayurveda | Medicine & Surgery | Ayurveda physician/ practitioner | 2 | Delhi |
| G | 34 | MD, Ayurveda | Charak Samhita | Ayurveda physician and academician | 17 | Pune |
| H | 46 | BAMS Ayurveda | Medicine & Surgery | Ayurved Acharya ** (Physician) | 20 | Pune |
| I | 46 | BAMS Ayurveda, MA, Yoga | Medicine & Surgery, Yoga | Ayurved Consultant, Physician, Yoga teacher | 22 | Pune |
| J | 69 | MD, PhD, Ayurveda | Medicine & Surgery | Professor & Government of India | 35 | Delhi |
| Phase I | Location | Phase II (Supporting Phase I) | Location | Goal | Outcome |
|---|---|---|---|---|---|
| Preliminary research examining current literature | USA | Review of author’s own previous findings and data | USA | Identifying conceptual domains, challenges, gaps | Semi-structured interview Protocol development (conceptual domains) |
| Vipassana meditation | Dhamma Giri, Igatpuri, Nashik, Maharashtra, India | Observation of cultural artifacts, symbolism, practices as they constitute healing, body-self integration, reflexivity, and whole-person conceptualization | Igatpuri, Shani Shingnapur, Nashik, Pune, New Delhi, India. | Experiential integration of body awareness, healing, reflection/reflexivity and whole-person conceptualization | Protocol construction, refining of conceptual domains and probes |
| Participant recruitment | Pune, Maharashtra, India and New Delhi, India | Advanced course in Ayurvedic Diet and Nutrition Tour of Ayurveda pharmacological laboratories, national and regional teaching institutions | Pune, Maharashtra, India | Understand Ayurvedic diagnostic and prognostic principles in chronic pain through deeper learning supported by semi-structured in-depth interviews with Ayurvedic physician participants | Recruitment of Ayurvedic physicians, scheduling interviews, administering informed consent, data transcription |
| Validity and Reliability/Rigor | USA and India | Data analysis and presentation | USA | Organization of data, member validation, iterative interpretation | Preliminary themes, saturation, fixing themes |
| Discussion and Synthesis of results | USA | Conclusion and recommendations | USA | Situating findings and contribution with prior studies, significance, and recommendations | conceptual framework, significance, future directions |
© 2020 by the author. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Agarwal, V. Patient Assessment and Chronic Pain Self-Management in Ethnomedicine: Seasonal and Ecosystemic Embodiment in Ayurvedic Patient-Centered Care. Int. J. Environ. Res. Public Health 2020, 17, 2842. https://doi.org/10.3390/ijerph17082842
Agarwal V. Patient Assessment and Chronic Pain Self-Management in Ethnomedicine: Seasonal and Ecosystemic Embodiment in Ayurvedic Patient-Centered Care. International Journal of Environmental Research and Public Health. 2020; 17(8):2842. https://doi.org/10.3390/ijerph17082842
Chicago/Turabian StyleAgarwal, Vinita. 2020. "Patient Assessment and Chronic Pain Self-Management in Ethnomedicine: Seasonal and Ecosystemic Embodiment in Ayurvedic Patient-Centered Care" International Journal of Environmental Research and Public Health 17, no. 8: 2842. https://doi.org/10.3390/ijerph17082842
APA StyleAgarwal, V. (2020). Patient Assessment and Chronic Pain Self-Management in Ethnomedicine: Seasonal and Ecosystemic Embodiment in Ayurvedic Patient-Centered Care. International Journal of Environmental Research and Public Health, 17(8), 2842. https://doi.org/10.3390/ijerph17082842




