Risk Factors and Behaviours of Schoolchildren with Myopia in Taiwan
Abstract
1. Introduction
2. Methods
2.1. Study Design and Patient Population
2.2. Ethics, Governance, and Consent
2.3. Outcome Measures
2.4. Risk Factors
2.5. Vision Care Knowledge
- Long-acting mydriatic agent is harmful to eyes.
- Long-acting mydriatic agent is proven to be effective in controlling myopia.
- Vision deteriorates faster for people with myopic squinting and seeing without appropriate corrective lenses.
- It is better not to wear eyeglasses, even when you have myopia, since eyeglasses may very likely make your vision worse.
- Pupil dilating effect will disappear once you stop using mydriatic agents.
- Corrective lens power should be less than your real power since the full correction lenses may accelerate myopia progression.
- Usage of electronic devices will accelerate myopia progression.
- Eye health and vision can be improved by adequate outdoor activities and exercise.
- “30/10 Rule” refers to every 30 min spent in near work activity requires a 10-min rest.
- High myopia is nothing to worry about. It is not associated with retinal problems, glaucoma, cataracts, or any other eye diseases.
2.6. Sampling
2.7. Multivariate Regression Analysis
3. Results
3.1. Patient Demographics
3.2. Multivariate Analyses and Sensitivity Tests
4. Discussion
Limitations
5. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Pruett, R.C. Complications associated with posterior staphyloma. Curr. Opin. Ophthalmol. 1998, 9, 16–22. [Google Scholar] [CrossRef] [PubMed]
- Saw, S.M.; Gazzard, G.; Shih-Yen, E.C.; Chua, W.H. Myopia and associated pathological complications. Ophthalmic Physiol. Opt. 2005, 25, 381–391. [Google Scholar] [CrossRef] [PubMed]
- Saw, S.M. How blinding is pathological myopia? Br. J. Ophthalmol. 2006, 90, 525–526. [Google Scholar] [CrossRef] [PubMed]
- Hsu, W.M.; Cheng, C.Y.; Liu, J.H.; Tsai, S.Y.; Chou, P. Prevalence and causes of visual impairment in an elderly Chinese population in Taiwan: The Shihpai Eye Study. Ophthalmology 2004, 111, 62–69. [Google Scholar] [CrossRef] [PubMed]
- Iwase, A.; Araie, M.; Tomidokoro, A.; Yamamoto, T.; Shimizu, H.; Kitazawa, Y. Tajimi Study Group. Prevalence and causes of low vision and blindness in a Japanese adult population: The Tajimi Study. Ophthalmology 2006, 113, 1354–1362. [Google Scholar] [CrossRef]
- Xu, L.; Wang, Y.; Li, Y.; Wang, Y.; Cui, T.; Li, J.; Jonas, J.B. Causes of blindness and visual impairment in urban and rural areas in Beijing: The Beijing Eye Study. Ophthalmology 2006, 113, 1134. [Google Scholar] [CrossRef]
- Buch, H.; Vinding, T.; La Cour, M.; Appleyard, M.; Jensen, G.B.; Nielsen, N.V. Prevalence and causes of visual impairment and blindness among 9980 Scandinavian adults: The Copenhagen City Eye Study. Ophthalmology 2004, 111, 53–61. [Google Scholar] [CrossRef]
- Klaver, C.C.; Wolfs, R.C.; Vingerling, J.R.; Hofman, A.; de Jong, P.T. Age-specific prevalence and causes of blindness and visual impairment in an older population: The Rotterdam Study. Arch. Ophthalmol. 1998, 116, 653–658. [Google Scholar] [CrossRef]
- Cotter, S.A.; Varma, R.; Ying-Lai, M.; Azen, S.P.; Klein, R. Los Angeles Latino Eye Study Group. Causes of low vision and blindness in adult Latinos: The Los Angeles Latino Eye Study. Ophthalmology 2006, 113, 1574–1582. [Google Scholar] [CrossRef]
- Gifford, P.; Gifford, K.L. The future of myopia control contact lenses. Optom. Vis. Sci. 2016, 93, 336–343. [Google Scholar] [CrossRef]
- Wu, P.C.; Chang, L.C.; Niu, Y.Z.; Chen, M.L.; Liao, L.L.; Chen, C.T. Myopia prevention in Taiwan. Ann. Eye Sci. 2018, 3, 12. [Google Scholar] [CrossRef]
- Linn, G.; Ying, Y.; Chang, K. The determinants of obstetricians’ willingness to undertake delivery by vaginal birth after cesarean section in Taiwan. Ther. Clin. Risk Manag. 2019, 15, 991–1002. [Google Scholar] [CrossRef] [PubMed]
- Chen, Y.T.; Ying, Y.H.; Chang, K.; Hsieh, Y.H. Study of Patients’ Willingness to Pay for a Cure of Chronic Obstructive Pulmonary Disease in Taiwan. Int. J. Environ. Res. Public Health 2016, 13, 273. [Google Scholar] [CrossRef] [PubMed]
- Lang, H.C.; Chang, K.; Ying, Y.H. Quality of Life, Treatments, and Patient Willingness to Pay for a Complete Remission for Cervical Cancer in Taiwan. Health Econ. 2012, 21, 1217–1233. [Google Scholar] [CrossRef] [PubMed]
- Lan, W.; Zhao, F.; Lin, L.; Li, Z.; Zeng, J.; Yang, Z.; Morgan, I.G. Refractive Errors in 3–6 Year-Old Chinese Children: A Very Low Prevalence of Myopia? PLoS ONE 2013, 8, e78003. [Google Scholar] [CrossRef]
- Armstrong, R.A. Statistical guidelines for the analysis of data obtained from one or both eyes. Ophthalmic Physiol. Opt. 2013, 33, 7–14. [Google Scholar] [CrossRef]
- Mutti, D.O.; Mitchell, G.L.; Moeschberger, M.L.; Jones, L.A.; Zadnik, K. Parental myopia, near work, school achievement, and children’s refractive error. Investig. Ophthalmol. Vis. Sci. 2002, 43, 3633–3640. [Google Scholar]
- Mutti, D.O.; Semina, E.; Marazita, M.; Cooper, M.; Murray, J.C.; Zadnik, K. Genetic loci for pathological myopia are not associated with juvenile myopia. Am. J. Med. Gene 2002, 112, 355–360. [Google Scholar] [CrossRef]
- Lee, Y.Y.; Lo, C.T.; Sheu, S.J.; Lin, J.L. What factors are associated with myopia in young adults? A survey study in Taiwan military conscripts. Investig. Ophthalmol. Vis. Sci. 2013, 54, 1026–1033. [Google Scholar] [CrossRef]
- Grosvenor, T. A review and a suggested classification system for myopia on the basis of age-related prevalence and age of onset. Am. J. Optom. Physiol. Opt. 1987, 64, 545–554. [Google Scholar] [CrossRef]
- Mutti, D.O.; Zadnik, K. The utility of three predictors of childhood myopia: A Bayesian analysis. Vision Res. 1995, 35, 1345–1352. [Google Scholar] [PubMed]
- Congdon, N.G.; Friedman, D.S.; Lietman, T. Important causes of visual impairment in the world today. JAMA 2003, 290, 2057–2060. [Google Scholar] [CrossRef] [PubMed]
- Shih, Y.F.; Chen, C.H.; Chou, A.C.; Ho, T.C.; Lin, L.L.K.; Hung, P.T. Effects of different concentrations of atropine on controlling myopia in myopic children. J. Ocul. Pharmacol. Ther. 1999, 15, 85–90. [Google Scholar] [CrossRef] [PubMed]
- Clarke, K.A. The Phantom Menace: Omitted Variable Bias in Econometric Research. Confl. Manag. Peace Sci. 2005, 22, 341–352. [Google Scholar] [CrossRef]
- Wooldridge, J.M. Omitted Variable Bias: The Simple Case. Available online: http://hedibert.org/wp-content/uploads/2016/09/Bias-omittedvariable.pdf (accessed on 13 March 2020).
- Ying, Y.H.; Linn, G.; Chang, K. Vaginal Birth after Cesarean Section in Taiwan: A Population-Based Study. J. Clin. Med. 2019, 8, 1203. [Google Scholar] [CrossRef]
- Quek, T.P.; Chua, C.G.; Chong, C.S.; Chong, J.H.; Hey, H.W.; Lee, J.; Lim, Y.F.; Saw, S.M. Prevalence of refractive errors in teenage high school students in Singapore. Ophthalmic Physiol. Opt. 2004, 24, 47–55. [Google Scholar] [CrossRef]
- Curtin, B.J.; Karlin, D.B. Axial length measurements and fundus changes of the myopic eye. Am. J. Ophthalmol. 1971, 71, 42–53. [Google Scholar] [CrossRef]
- Mutti, D.O.; Jones, L.A.; Moeschberger, M.L.; Zadnik, K. AC/A ratio, age, and refractive error in children. Investig. Ophthalmol. Vis. Sci. 2000, 41, 2469–2478. [Google Scholar] [CrossRef]
- Rose, K.A.; Morgan, I.G.; Ip, J.; Kifley, A.; Huynh, S.; Smith, W.; Mitchell, P. Outdoor activity reduces the prevalence of myopia in children. Ophthalmology 2008, 115, 1279–1285. [Google Scholar] [CrossRef]
- Huang, H.M.; Chang, D.S.; Wu, P.C. The Association between Near Work Activities and Myopia in Children-A Systematic Review and Meta-Analysis. PLoS ONE 2015, 10, e0140419. [Google Scholar] [CrossRef]
- Dixit, R.; Jindal, M.; Gupta, P.; Dubey, A. Excessive Usage of Illuminated Screen a Risk Factor for Myopia in Adolescent Population. Int. J. Curr. Med Appl. Sci. 2016, 10, 173–176. [Google Scholar]
- China Grain Products Research & Development Institute. 2016 Annual Report on Value Added and Promotion of Foold Supplement Industry. Available online: https://www.functionalfood.org.tw/pld/survey2015.pdf (accessed on 2 March 2020).
- Rosner, M.; Belkin, M. Intelligence, Education, and Myopia in Males. Arch. Ophthalmol. 1987, 105, 1508–1511. [Google Scholar] [CrossRef] [PubMed]
- Saw, S.M.; Wu, H.M.; Seet, B.; Wong, T.Y.; Yap, E.; Chia, K.S.; Stone, R.A.; Lee, L. Academic achievement, close up work parameters, and myopia in Singapore military conscripts. Br. J. Ophthalmol. 2001, 85, 855–860. [Google Scholar] [CrossRef] [PubMed]
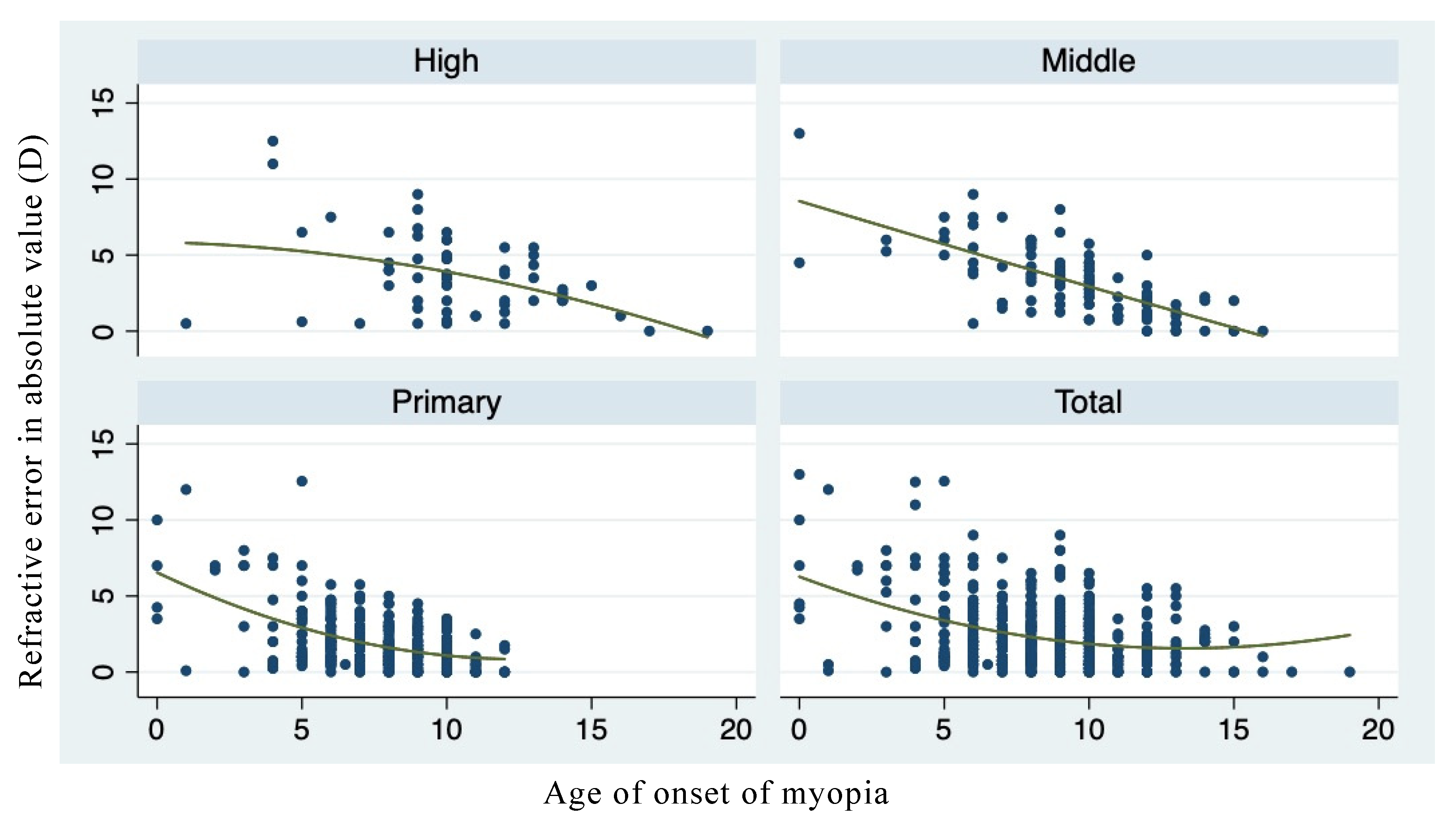
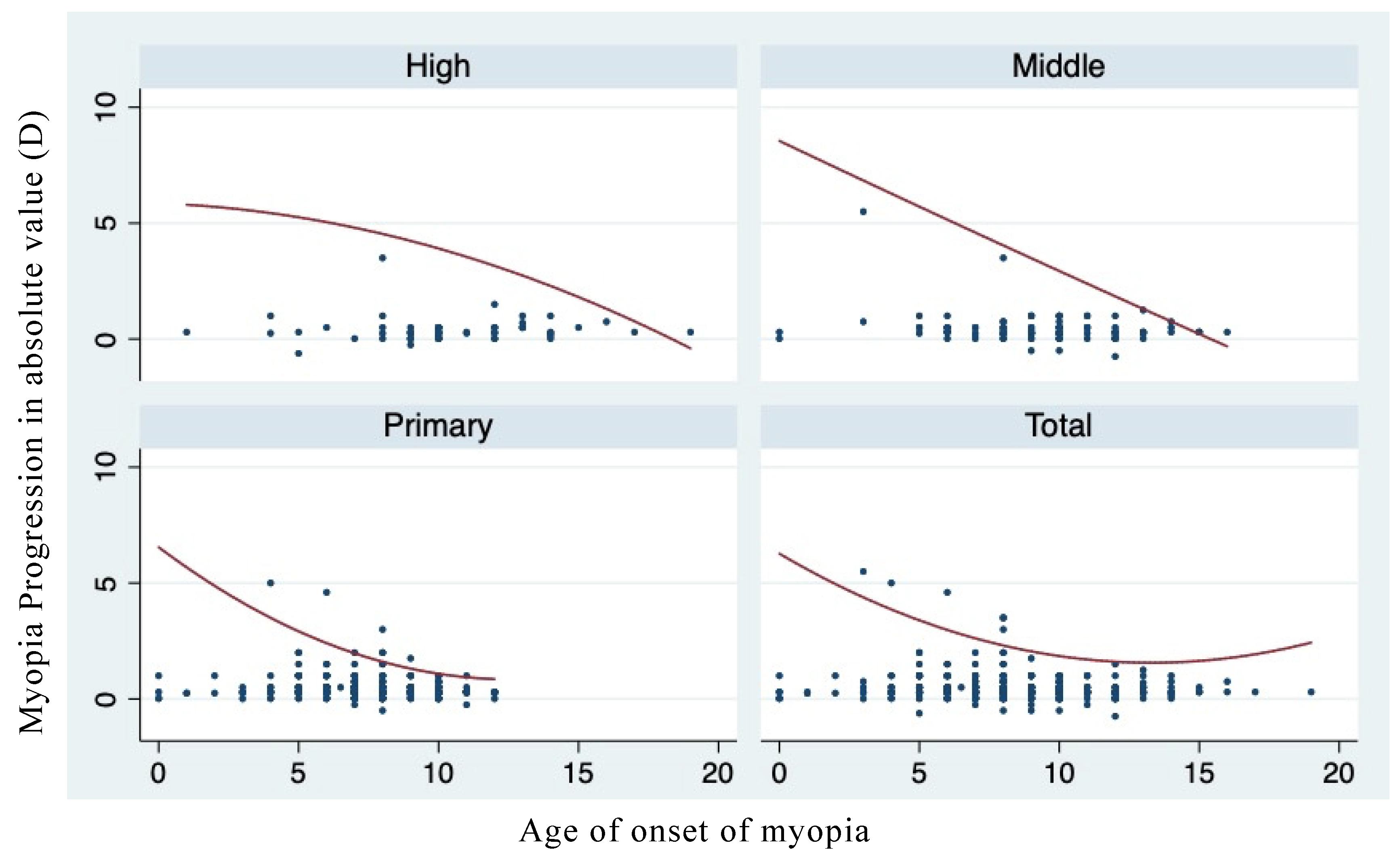
| Total | Primary | Middle | High School | |
|---|---|---|---|---|
| Number | 522 | 344 | 115 | 63 |
| Age (years) | 11.31 (3.08) | 9.58 (1.91) | 13.55 (1.21) | 16.60 (1.32) |
| Boy (%) | 49.81 | 53.20 | 45.22 | 39.68 |
| BMI † | 18.63 (4.02) | 17.57 (3.48) | 20.08 (4.01) | 21.89 (4.31) |
| Family Income (USD, monthly) | 3132.32 (1382.7) | 3180.3 (1394.15) | 3084.93 (1339.60) | 2885.20 (1394.26) |
| Frequency of seeing an opthalmologist (months) | 4.17 (1.80) | 3.92 (1.80) | 4.62 (1.65) | 4.76 (1.87) |
| Private School (%) | 22.56 | 19.82 | 23.00 | 36.51 |
| Cram School (%) | 62.45 | 64.50 | 66.37 | 44.44 |
| Activity Hours | ||||
| Cram School (hours per day) | 1.98 (1.97) | 2.17 (2.06) | 1.81 (1.83) | 1.11 (1.49) |
| Electronic Devises (hours per day) | 1.94 (1.43) | 1.54 (1.26) | 2.30 (1.36) | 3.43 (1.27) |
| TV (hours per day) | 1.77 (1.16) | 1.83 (1.10) | 1.63 (1.15) | 1.71 (1.41) |
| Study (hours per day) | 3.08 (1.10) | 2.93 (0.97) | 3.26 (1.21) | 3.50 (1.24) |
| Sleep (hours per day) | 7.66 (1.12) | 7.90 (1.11) | 7.29 (0.95) | 7.00 (0.96) |
| Outdoor activities (hours per week) | 3.68 (3.42) | 3.80 (3.19) | 3.65 (4.15) | 3.16 (3.19) |
| Refractive error (D) ‡ | 2.42 (2.13) | 1.95 (1.83) | 3.20 (2.23) | 3.62 (2.54) |
| Myopia Progression (D) (in past year) | 0.50 (0.63) | 0.53 (0.61) | 0.47 (0.74) | 0.42 (0.56) |
| Knowledge | 76.52 (10.22) | 77.18 (9.96) | 75.00 (10.51) | 75.67 (10.92) |
| Onset Age | 8.24 (2.71) | 7.46 (0.18) | 9.46 (2.95) | 10.36 (3.20) |
| Other Eye Disorders | ||||
| Amblyopia | 9.41% | 9.55% | 8.03% | 11.11% |
| Strabismus | 5.69% | 6.27% | 5.36% | 3.17% |
| Total | Primary | Middle | High School | |
|---|---|---|---|---|
| Number | 522 | 344 | 115 | 63 |
| Supplements (%) | ||||
| Vitamin | 15.32 | 14.82 | 19.13 | 11.11 |
| Fish oil | 9.34 | 10.50 | 7.82 | 6.35 |
| Lutein | 13.98 | 13.08 | 14.78 | 17.46 |
| Mydriatic (%) | 97.31 | 97.09 | 97.39 | 98.41 |
| Atropine (0.125%) | 28.8 | 31.39 | 21.73 | 23.80 |
| Corrective methods (%) | 57.28 | 49.72 | 72.17 | 71.42 |
| Spectacles | 56.32 | 48.54 | 71.30 | 71.42 |
| Contact lenses | 3.25 | 2.48 | 5.21 | 4.76 |
| Orthokeratology | 0.57 | 0.00 | 1.73 | 1.58 |
| Total | Primary | Middle | High School | |
|---|---|---|---|---|
| Reading | 3.71 (1.18) | 3.74 (1.21) | 3.65 (1.10) | 3.63 (1.15) |
| TV | 3.57 (1.35) | 3.67 (1.32) | 3.27 (1.49) | 3.61 (1.26) |
| Outdoor activities | 3.80 (1.20) | 3.86 (1.17) | 3.61 (1.27) | 3.78 (1.14) |
| Sleep | 3.45 (1.31) | 3.36 (1.31) | 3.48 (1.37) | 3.85 (1.10) |
| Genetics | 3.45 (1.26) | 3.54 (1.26) | 3.44 (1.22) | 3.00 (1.20) |
| Space | 2.89 (1.22) | 2.93 (1.23) | 2.94 (1.20) | 2.56 (1.16) |
| Injury | 2.24 (1.31) | 2.25 (1.30) | 2.14 (1.31) | 2.38 (1.34) |
| (1) | (2) | (3) | |
|---|---|---|---|
| All Children | Primary School | Secondary School | |
| Length (years) | 0.13 *** | 0.15 *** | 0.10 *** |
| (8.12) | (9.38) | (4.07) | |
| Boy | 0.01 | 0.08 ** | 0.05 |
| (1.20) | (1.77) | (0.56) | |
| Growth in Height (cm) | 0.01 | 0.02 * | 0.01 |
| (1.35) | (1.87) | (0.35) | |
| BMI | 0.02 * | 0.03 ** | 0.02 |
| (1.63) | (2.00) | (0.69) | |
| Weight (kg) | −0.01 | −0.01 * | −0.00 |
| (−1.40) | (−1.74) | (−0.49) | |
| Space | −0.03 ** | −0.04 ** | 0.01 |
| (−1.84) | (−2.05) | (0.37) | |
| Income | 0.00 | −0.10 | 0.14 * |
| (0.04) | (−1.44) | (1.73) | |
| Mydriatic | 0.06 * | 0.10 ** | 0.08 |
| (1.83) | (1.84) | (0.79) | |
| Eye Care Knowledge | −0.004 ** | −0.003 ** | −0.01 |
| (−1.89) | (−1.76) | (−1.09) | |
| Genetic | 0.08 * | 0.05 * | 0.003 |
| (1.72) | (1.68) | (0.04) | |
| Private School | −0.11 ** | −0.11 ** | −0.11 |
| (−2.06) | (−1.90) | (−1.05) | |
| School Performance | −0.02 * | −0.03 *** | 0.013 |
| (−1.80) | (−2.74) | (0.57) | |
| Food Supplement | |||
| Vitamin | −0.01 | 0.14 * | −0.23 ** |
| (−0.07) | (1.87) | (−2.15) | |
| Fish oil | −0.02 | −0.08 | −0.04 |
| (−0.21) | (−0.69) | (−0.18) | |
| Activity Hours | |||
| Cram School | 0.02 * | 0.02 | 0.01 |
| (1.63) | (1.11) | (0.18) | |
| Electronics | −0.01 | −0.04 | −0.003 |
| (−0.65) | (−1.37) | (−0.11) | |
| TV | −0.01 | −0.01 | −0.02 |
| (−0.59) | (−0.36) | (−0.57) | |
| Study | 0.003 | −0.05 * | 0.05 |
| (0.14) | (−1.88) | (1.20) | |
| Sleep | −0.007 | 0.001 | −0.04 |
| (−0.31) | (0.05) | (−0.94) | |
| Ourdoor Exercise | −0.01 * | −0.003 | −0.01 |
| (−1.60) | (−0.60) | (−1.09) | |
| Middle School | 0.243 *** | ||
| (3.32) | |||
| High School | 0.0934 | ||
| (0.72) | |||
| N | 522 | 272 | 250 |
| R2 | 0.35 | 0.43 | 0.27 |
| (1) | (2) | (3) | |
|---|---|---|---|
| All Children | Primary School | Secondary School | |
| Length (years) | 0.02 * | 0.02 ** | 0.01 |
| (1.76) | (1.81) | (0.74) | |
| Boy | 0.03 | 0.04 * | 0.05 |
| (1.22) | (1.75) | (0.67) | |
| Growth in Height | 0.01 ** | 0.03 *** | −0.002 |
| (cm) | (1.92) | (3.71) | (−0.16) |
| BMI | 0.02 ** | 0.02 ** | 0.003 |
| (2.28) | (2.00) | (0.17) | |
| Weight (kg) | −0.01 *** | −0.01 ** | −0.004 |
| (−3.37) | (−2.30) | (−0.91) | |
| Space | −0.002 | 0.01 | −0.01 |
| (−0.22) | (0.60) | (−0.49) | |
| Income ‡ | 0.03 | 0.03 | −0.001 |
| (0.76) | (0.94) | (−0.02) | |
| Mydratic Use | −0.03 | −0.03 | −0.03 |
| (−1.00) | (−0.66) | (−0.47) | |
| Private School | −0.03 | −0.04 | 0.01 |
| (−0.85) | (−1.14) | (0.11) | |
| Eye Care | −0.001 | −0.0001 | −0.001 |
| Knowledge | (−0.32) | (−0.07) | (−0.58) |
| Genetics | 0.03 * | 0.06 ** | −0.01 |
| (1.66) | (1.99) | (−0.22) | |
| School Performance | −0.01 | −0.01 | 0.003 |
| (−0.87) | (−1.26) | (0.17) | |
| Food Supplements | |||
| Vitamin | −0.01 | −0.03 | 0.05 |
| (−0.12) | (−0.70) | (0.40) | |
| Fish oil | 0.01 | 0.04 | −0.02 |
| (0.28) | (0.73) | (−0.28) | |
| Activity Hours | |||
| Cram School | 0.01 * | 0.01 | 0.02 |
| (1.62) | (1.47) | (1.37) | |
| Electronics | 0.04 ** | 0.01 | 0.05 * |
| (2.26) | (0.45) | (1.80) | |
| TV | −0.01 | 0.02 | −0.02 |
| (−0.42) | (1.10) | (−0.88) | |
| Study | 0.01 | −0.02 | 0.01 |
| (0.34) | (−0.88) | (0.34) | |
| Sleep | −0.00 | 0.01 | −0.02 |
| (−0.01) | (0.39) | (−0.73) | |
| Outdoore Exercise | −0.0002 | −0.01 * | −0.01 |
| (−0.04) | (−1.65) | (−0.98) | |
| Middle School | 0.002 | ||
| (0.05) | |||
| High School | −0.04 | ||
| (−0.45) | |||
| N | 522 | 272 | 250 |
| R2 | 0.08 | 0.15 | 0.08 |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Cheng, H.-C.; Chang, K.; Shen, E.; Luo, K.-S.; Ying, Y.-H. Risk Factors and Behaviours of Schoolchildren with Myopia in Taiwan. Int. J. Environ. Res. Public Health 2020, 17, 1967. https://doi.org/10.3390/ijerph17061967
Cheng H-C, Chang K, Shen E, Luo K-S, Ying Y-H. Risk Factors and Behaviours of Schoolchildren with Myopia in Taiwan. International Journal of Environmental Research and Public Health. 2020; 17(6):1967. https://doi.org/10.3390/ijerph17061967
Chicago/Turabian StyleCheng, Han-Chih, Koyin Chang, Elizabeth Shen, Kai-Shin Luo, and Yung-Hsiang Ying. 2020. "Risk Factors and Behaviours of Schoolchildren with Myopia in Taiwan" International Journal of Environmental Research and Public Health 17, no. 6: 1967. https://doi.org/10.3390/ijerph17061967
APA StyleCheng, H.-C., Chang, K., Shen, E., Luo, K.-S., & Ying, Y.-H. (2020). Risk Factors and Behaviours of Schoolchildren with Myopia in Taiwan. International Journal of Environmental Research and Public Health, 17(6), 1967. https://doi.org/10.3390/ijerph17061967





