Rotating Night Shift Work, Exposure to Light at Night, and Glomerular Filtration Rate: Baseline Results from a Chinese Occupational Cohort
Abstract
1. Introduction
2. Materials and Methods
2.1. Study Design and Population
2.2. Assessment of GFR
2.3. Assessment of Shift Work
2.4. Assessment of Bedroom Light Environment
2.5. Assessment of Covariates
2.6. Statistical Analysis
3. Results
3.1. General Characteristics of the Participants
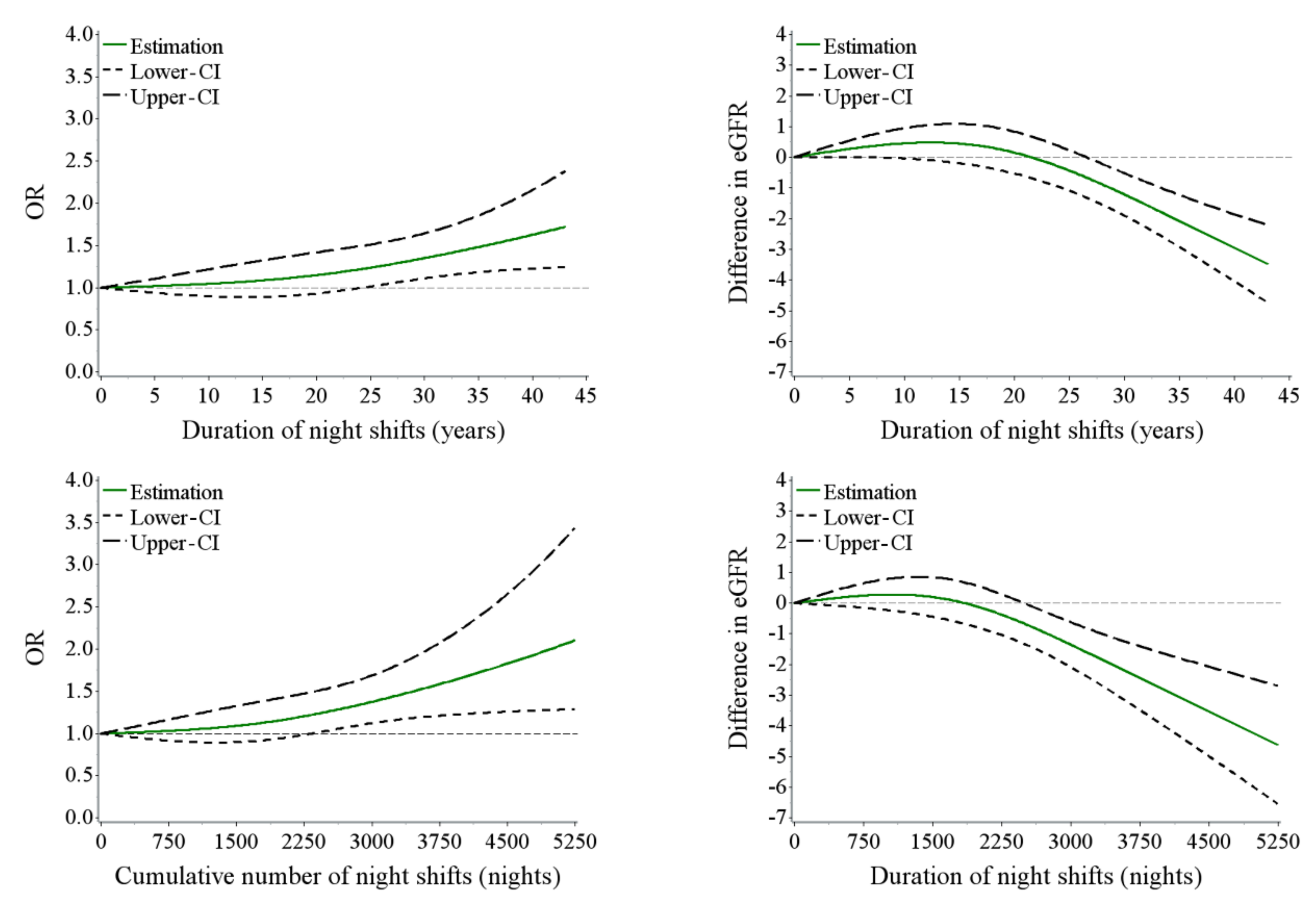
3.2. Night Shift Work, LAN and eGFR
3.3. Sensitivity Analyses
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- James, S.M.; Honn, K.A.; Gaddameedhi, S.; Van Dongen, H.P.A. Shift Work: Disrupted Circadian Rhythms and Sleep-Implications for Health and Well-Being. Curr. Sleep Med. Rep. 2017, 3, 104–112. [Google Scholar] [CrossRef] [PubMed]
- De Bacquer, D.; Van Risseghem, M.; Clays, E.; Kittel, F.; De Backer, G.; Braeckman, L. Rotating shift work and the metabolic syndrome: A prospective study. Int. J. Epidemiol. 2009, 38, 848–854. [Google Scholar] [CrossRef] [PubMed]
- Falchi, F.; Cinzano, P.; Duriscoe, D.; Kyba, C.C.M.; Elvidge, C.D.; Baugh, K.; Portnov, B.A.; Rybnikova, N.A.; Furgoni, R. The new world atlas of artificial night sky brightness. Sci. Adv. 2016, 2, e1600377. [Google Scholar] [CrossRef] [PubMed]
- Elvidge, C.D.; Keith, D.M.; Tuttle, B.T.; Baugh, K.E. Spectral identification of lighting type and character. Sensors 2010, 10, 3961–3988. [Google Scholar] [CrossRef]
- Yang, C.; Wang, H.; Zhao, X.; Matsushita, K.; Coresh, J.; Zhang, L.; Zhao, M.H. CKD in China: Evolving Spectrum and Public Health Implications. Am. J. Kidney Dis. 2020, 76, 258–264. [Google Scholar] [CrossRef]
- Wang, F.; He, K.; Wang, J.; Zhao, M.H.; Li, Y.; Zhang, L.; Saran, R.; Bragg-Gresham, J.L. Prevalence and Risk Factors for CKD: A Comparison Between the Adult Populations in China and the United States. Kidney Int. Rep. 2018, 3, 1135–1143. [Google Scholar] [CrossRef]
- Firsov, D.; Bonny, O. Circadian rhythms and the kidney. Nat. Rev. Nephrol. 2018, 14, 626–635. [Google Scholar] [CrossRef]
- Callaway, E.; Ledford, H. Medicine Nobel awarded for work on circadian clocks. Nature 2017, 550, 18. [Google Scholar] [CrossRef]
- Hulsegge, G.; Loef, B.; van Kerkhof, L.W.; Roenneberg, T.; van der Beek, A.J.; Proper, K.I. Shift work, sleep disturbances and social jetlag in healthcare workers. J. Sleep Res. 2019, 28, e12802. [Google Scholar] [CrossRef]
- Ricardo, A.C.; Knutson, K.; Chen, J.; Appel, L.J.; Bazzano, L.; Carmona-Powell, E.; Cohan, J.; Kurella Tamura, M.; Steigerwalt, S.; Thornton, J.D.; et al. The Association of Sleep Duration and Quality with CKD Progression. J. Am. Soc. Nephrol. 2017, 28, 3708–3715. [Google Scholar] [CrossRef]
- Thomas, C.; Power, C. Shift work and risk factors for cardiovascular disease: A study at age 45 years in the 1958 British birth cohort. Eur. J. Epidemiol. 2010, 25, 305–314. [Google Scholar] [CrossRef] [PubMed]
- DiBona, G.F. Nervous kidney. Interaction between renal sympathetic nerves and the renin-angiotensin system in the control of renal function. Hypertension 2000, 36, 1083–1088. [Google Scholar] [CrossRef] [PubMed]
- Uhm, J.Y.; Kim, H.R.; Kang, G.H.; Choi, Y.G.; Park, T.H.; Kim, S.Y.; Chang, S.S.; Choo, W.O. The association between shift work and chronic kidney disease in manual labor workers using data from the Korea National Health and Nutrition Examination Survey (KNHANES 2011–2014). Ann. Occup. Environ. Med. 2018, 30, 69. [Google Scholar] [CrossRef] [PubMed]
- Kang, E.K.; Kang, G.H.; Uhm, J.Y.; Choi, Y.G.; Kim, S.Y.; Chang, S.S.; Kim, H.R. Association between shift work and microalbuminuria: Data from KNHANES (2012–2014). Ann. Occup. Environ. Med. 2017, 29, 37. [Google Scholar] [CrossRef]
- Charles, L.E.; Gu, J.K.; Fekedulegn, D.; Andrew, M.E.; Violanti, J.M.; Burchfiel, C.M. Association between shiftwork and glomerular filtration rate in police officers. J. Occup. Environ. Med. 2013, 55, 1323–1328. [Google Scholar] [CrossRef] [PubMed]
- Boogaard, P.J.; Caubo, M.E. Increased albumin excretion in industrial workers due to shift work rather than to prolonged exposure to low concentrations of chlorinated hydrocarbons. Occup. Environ. Med. 1994, 51, 638–641. [Google Scholar] [CrossRef]
- Zhang, S.; Wang, Y.; Wang, Z.; Wang, H.; Xue, C.; Li, Q.; Guan, W.; Yuan, J. Rotating night shift work and non-alcoholic fatty liver disease among steelworkers in China: A cross-sectional survey. Occup. Environ. Med. 2020, 77, 333–339. [Google Scholar] [CrossRef]
- Levey, A.S.; Stevens, L.A.; Schmid, C.H.; Zhang, Y.L.; Castro, A.F., 3rd; Feldman, H.I.; Kusek, J.W.; Eggers, P.; Van Lente, F.; Greene, T.; et al. A new equation to estimate glomerular filtration rate. Ann. Intern. Med. 2009, 150, 604–612. [Google Scholar] [CrossRef]
- Webster, A.C.; Nagler, E.V.; Morton, R.L.; Masson, P. Chronic Kidney Disease. Lancet 2017, 389, 1238–1252. [Google Scholar] [CrossRef]
- Wang, F.; Zhang, L.; Zhang, Y.; Zhang, B.; He, Y.; Xie, S.; Li, M.; Miao, X.; Chan, E.Y.; Tang, J.L.; et al. Meta-analysis on night shift work and risk of metabolic syndrome. Obes. Rev. 2014, 15, 709–720. [Google Scholar] [CrossRef]
- McFadden, E.; Jones, M.E.; Schoemaker, M.J.; Ashworth, A.; Swerdlow, A.J. The relationship between obesity and exposure to light at night: Cross-sectional analyses of over 100,000 women in the Breakthrough Generations Study. Am. J. Epidemiol. 2014, 180, 245–250. [Google Scholar] [CrossRef] [PubMed]
- Davis, S.; Mirick, D.K.; Stevens, R.G. Night shift work, light at night, and risk of breast cancer. J. Natl. Cancer Inst. 2001, 93, 1557–1562. [Google Scholar] [CrossRef] [PubMed]
- Tingley, D.; Teppei, H.; Mit, Y.; Keele, L.; Imai, K. Mediation: R Package for Causal Mediation Analysis. J. Statal. Softw. 2014, 59, 1–38. [Google Scholar]
- Carrero, J.J.; Hecking, M.; Chesnaye, N.C.; Jager, K.J. Sex and gender disparities in the epidemiology and outcomes of chronic kidney disease. Nat. Rev. Nephrol. 2018, 14, 151–164. [Google Scholar] [CrossRef]
- Kim, S.J.; Kim, J.W.; Cho, Y.S.; Chung, K.J.; Yoon, H.; Kim, K.H. Influence of Circadian Disruption Associated With Artificial Light at Night on Micturition Patterns in Shift Workers. Int. Neurourol. J. 2019, 23, 258–264. [Google Scholar] [CrossRef]
- Manohar, S.; Thongprayoon, C.; Cheungpasitporn, W.; Mao, M.A.; Herrmann, S.M. Associations of rotational shift work and night shift status with hypertension: A systematic review and meta-analysis. J. Hypertens. 2017, 35, 1929–1937. [Google Scholar] [CrossRef]
- Fu, S.; Sun, Y.; Luo, L.; Ye, P. Relationship of arterial compliance and blood pressure with microalbuminuria and mildly decreased glomerular filtration rate: A Chinese community-based analysis. PLoS ONE 2014, 9, e101013. [Google Scholar] [CrossRef]
- Qiu, Y.; Zhao, Q.; Gu, Y.; Wang, N.; Yu, Y.; Wang, R.; Zhang, Y.; Zhu, M.; Liu, X.; Jiang, Y.; et al. Association of Metabolic Syndrome and Its Components with Decreased Estimated Glomerular Filtration Rate in Adults. Ann. Nutr. Metab. 2019, 75, 168–178. [Google Scholar] [CrossRef]
- Hashimoto, J.; Ito, S. Central pulse pressure and aortic stiffness determine renal hemodynamics: Pathophysiological implication for microalbuminuria in hypertension. Hypertension 2011, 58, 839–846. [Google Scholar] [CrossRef]
- Cottone, S.; Mulè, G.; Guarneri, M.; Palermo, A.; Lorito, M.C.; Riccobene, R.; Arsena, R.; Vaccaro, F.; Vadalà, A.; Nardi, E.; et al. Endothelin-1 and F2-isoprostane relate to and predict renal dysfunction in hypertensive patients. Nephrol. Dial. Transplant. 2009, 24, 497–503. [Google Scholar] [CrossRef]
- Schibler, U.; Ripperger, J.; Brown, S.A. Peripheral circadian oscillators in mammals: Time and food. J. Biol. Rhythms 2003, 18, 250–260. [Google Scholar] [CrossRef] [PubMed]
- Wehrens, S.M.T.; Christou, S.; Isherwood, C.; Middleton, B.; Gibbs, M.A.; Archer, S.N.; Skene, D.J.; Johnston, J.D. Meal Timing Regulates the Human Circadian System. Curr. Biol. 2017, 27, 1768–1775. [Google Scholar] [CrossRef] [PubMed]
- Koch, B.C.; Nagtegaal, J.E.; Kerkhof, G.A.; ter Wee, P.M. Circadian sleep-wake rhythm disturbances in end-stage renal disease. Nat. Rev. Nephrol. 2009, 5, 407–416. [Google Scholar] [CrossRef]
- McMullan, C.J.; Curhan, G.C.; Forman, J.P. Association of short sleep duration and rapid decline in renal function. Kidney Int. 2016, 89, 1324–1330. [Google Scholar] [CrossRef] [PubMed]
- Yamamoto, R.; Shinzawa, M.; Isaka, Y.; Yamakoshi, E.; Imai, E.; Ohashi, Y.; Hishida, A. Sleep Quality and Sleep Duration with CKD are Associated with Progression to ESKD. Clin. J. Am. Soc. Nephrol. 2018, 13, 1825–1832. [Google Scholar] [CrossRef]
- Kecklund, G.; Axelsson, J. Health consequences of shift work and insufficient sleep. BMJ 2016, 355, i5210. [Google Scholar] [CrossRef]
- Roskoden, F.C.; Kruger, J.; Vogt, L.J.; Gartner, S.; Hannich, H.J.; Steveling, A.; Lerch, M.M.; Aghdassi, A.A. Physical Activity, Energy Expenditure, Nutritional Habits, Quality of Sleep and Stress Levels in Shift-Working Health Care Personnel. PLoS ONE 2017, 12, e0169983. [Google Scholar] [CrossRef]
- Oberleithner, H. Aldosterone makes human endothelium stiff and vulnerable. Kidney Int. 2005, 67, 1680–1682. [Google Scholar] [CrossRef]
- Ishigaki, S.; Ohashi, N.; Isobe, S.; Tsuji, N.; Iwakura, T.; Ono, M.; Sakao, Y.; Tsuji, T.; Kato, A.; Miyajima, H.; et al. Impaired endogenous nighttime melatonin secretion relates to intrarenal renin-angiotensin system activation and renal damage in patients with chronic kidney disease. Clin. Exp. Nephrol. 2016, 20, 878–884. [Google Scholar] [CrossRef]
| Variables | Overall | Non-Decreased eGFR | Decreased eGFR | |
|---|---|---|---|---|
| (n = 6869) | (n = 5860) | (n = 1009) | p Value | |
| Age (year), mean ± SD | 44.2 ± 8.0 | 43.6 ± 8.1 | 47.9 ± 6.3 | <0.001 |
| Sex, n (%) | ||||
| Male | 6283 (91.5) | 5370 (91.6) | 913 (90.5) | 0.226 |
| Female | 586 (8.5) | 490 (8.4) | 96 (9.5) | |
| Ethnicity, n (%) | 0.494 | |||
| Han | 6727 (97.9) | 5736 (97.9) | 991 (98.2) | |
| Others | 142 (2.1) | 124 (2.1) | 18 (1.8) | |
| BMI (kg/m2), mean ± SD | 25.2 ± 3.4 | 25.1 ± 3.4 | 25.7 ± 3.3 | <0.001 |
| Smoking status, n (%) | 0.196 | |||
| Never | 2817 (41.0) | 2409 (41.1) | 408 (40.4) | |
| Ever | 549 (8.0) | 454 (7.6) | 95 (9.4) | |
| Current | 3503 (51.0) | 2997 (51.1) | 506 (50.2) | |
| Alcohol consumption, n (%) | 0.233 | |||
| Never | 3936 (57.3) | 3353 (57.2) | 583 (57.8) | |
| Ever | 393 (5.7) | 325 (5.6) | 68 (6.7) | |
| Current | 2540 (37.0) | 2182 (37.2) | 358 (35.5) | |
| Education level, n (%) | <0.001 | |||
| Primary or illiterate | 86 (1.3) | 71 (1.2) | 15 (1.5) | |
| Middle or high school | 5326 (77.5) | 4483 (76.5) | 843 (83.6) | |
| University or college | 1457 (21.2) | 1306 (22.3) | 151 (15.0) | |
| Physical activity, n (%) | 0.270 | |||
| Low | 80 (1.2) | 70 (1.2) | 10 (1.0) | |
| Moderate | 522 (7.6) | 457 (7.8) | 65 (6.4) | |
| High | 6267 (91.2) | 5333 (91.0) | 934 (92.6) | |
| Duration of night shift work (years), n (%) | <0.001 | |||
| Day work | 1029 (15.0) | 896 (15.3) | 133 (13.2) | |
| Q1 (1–12) | 1471 (21.4) | 1317 (22.5) | 154 (15.3) | |
| Q2 (13–20) | 1495 (21.8) | 1328 (22.7) | 167 (16.6) | |
| Q3 (21–28) | 1314 (19.1) | 1102 (18.8) | 212 (21.0) | |
| Q4 (29–43) | 1560 (22.7) | 1217 (20.8) | 343 (34.0) | |
| Brightness of bedroom ambient LAN, n (%) | 0.856 | |||
| Darkest level | 3782 (55.1) | 3222 (55.0) | 560 (55.5) | |
| Middle level | 2276 (33.1) | 1949 (33.2) | 327 (32.4) | |
| Lightest level | 811 (11.8) | 689 (11.8) | 122 (12.1) | |
| Living duration of current residence, n (%) | 0.899 | |||
| <5 years | 2191 (31.9) | 1862 (31.8) | 329 (32.6) | |
| 6–10 years | 1642 (23.9) | 1400 (23.9) | 242 (24.0) | |
| 11–20 years | 1682 (24.5) | 1444 (24.6) | 238 (23.4) | |
| >20 years | 1354 (19.7) | 1154 (19.7) | 200 (19.8) | |
| Number of times light on (times/night), n (%) | 0.645 | |||
| 0 | 4194 (61.1) | 3584 (61.2) | 610 (60.5) | |
| 1 | 2172 (31.6) | 1854 (31.6) | 318 (31.5) | |
| ≥2 | 503 (7.3) | 422 (7.2) | 81 (8.0) | |
| Sleep duration (h), mean ± SD | 6.8 ± 1.2 | 6.8 ± 1.2 | 6.8 ± 1.2 | 0.005 |
| Insomnia, n (%) | 0.990 | |||
| No | 4560 (66.4) | 3890 (66.4) | 670 (66.4) | |
| Yes | 2309 (33.6) | 1970 (33.6) | 339 (33.6) | |
| Diabetes, n (%) | 0.150 | |||
| No | 6147 (89.5) | 5257 (89.7) | 890 (88.2) | |
| Yes | 722 (10.5) | 603 (10.3) | 119 (11.8) | |
| Fasting blood glucose (mmol/L), median (IQR) | 5.8 (5.4 to 6.3) | 5.8 (5.4 to 6.3) | 5.9 (5.5 to 6.4) | <0.001 |
| Hypertension, n (%) | <0.001 | |||
| No | 5109 (74.4) | 4447 (75.9) | 662 (65.6) | |
| Yes | 1760 (25.6) | 1413 (24.1) | 347 (34.4) | |
| Systolic blood pressure (mmHg), mean ± SD | 129.0 ± 16.0 | 128.5 ± 15.8 | 131.8 ± 17.2 | <0.001 |
| Diastolic blood pressure (mmHg), mean ± SD | 82.5 ± 10.4 | 82.2 ± 10.2 | 84.7 ± 11.0 | <0.001 |
| Hyperuricemia, n (%) | <0.001 | |||
| No | 4586 (66.8) | 4070 (60.5) | 516 (51.1) | |
| Yes | 2283 (33.2) | 1790 (30.6) | 493 (48.9) | |
| Serum uric acid (μmol/L), mean ± SD | 385.8 ± 94.2 | 385.3 ± 94.7 | 389.2 ± 91.1 | 0.244 |
| a Proteinuria (mg/dl), n (%) | <0.001 | |||
| A1 (<30) | 6745 (98.2) | 5772 (98.5) | 973 (96.4) | |
| A2-A3 (≥30) | 124 (1.8) | 88 (1.5) | 36 (3.6) |
| Exposure Metrics | Decreased eGFR | OR (95% CI) | |||
|---|---|---|---|---|---|
| No, n (%) | Yes, n (%) | Model 1 | Model 2 | Model 3 | |
| Duration of night shift (years) | |||||
| Day work | 896 (15.3) | 133 (13.2) | 1.00 | 1.00 | 1.00 |
| Q1 (1–12) | 1317 (22.5) | 154 (15.3) | 0.79 (0.61 to 1.01) | 1.10 (0.85 to 1.42) | 1.03 (0.79 to 1.34) |
| Q2 (13–20) | 1328 (22.7) | 167 (16.6) | 0.84 (0.66 to 1.08) | 1.12 (0.87 to 1.44) | 1.01 (0.78 to 1.31) |
| Q3 (21–28) | 1102 (18.8) | 212 (21.0) | 1.29 (1.02 to 1.63) | 1.32 (1.04 to 1.68) | 1.28 (1.01 to 1.64) |
| Q4 (29–43) | 1217 (20.8) | 343 (34.0) | 1.89 (1.52 to 2.36) | 1.40 (1.12 to 1.75) | 1.37 (1.09 to 1.73) |
| p for trend | <0.001 | <0.001 | 0.001 | ||
| Brightness of bedroom ambient LAN | |||||
| Darkest level | 3222 (55.0) | 560 (55.5) | 1.00 | 1.00 | 1.00 |
| Middle level | 1949 (33.3) | 327 (32.4) | 0.96 (0.83 to 1.12) | 0.91 (0.78 to 1.06) | 0.90 (0.77 to 1.05) |
| Lightest level | 689 (11.8) | 122 (12.1) | 0.99 (0.80 to 1.23) | 0.97 (0.78 to 1.21) | 0.94 (0.75 to 1.18) |
| Groups | Duration of Night Shifts (Years) | |||||
|---|---|---|---|---|---|---|
| Day Work | Q1 (1–12) | Q2 (13–20) | Q3 (21–28) | Q4 (29–43) | p for Interaction | |
| Sex | 0.128 | |||||
| Male, OR (95% CI) | 1.00 | 0.99 (0.74 to 1.31) | 1.02 (0.78 to 1.35) | 1.36 (1.04 to 1.76) | 1.40 (1.12 to 1.79) | |
| Female, OR (95% CI) | 1.00 | 0.88 (0.40 to 1.95) | 0.65 (0.29 to 1.47) | 0.65 (0.29 to 1.47) | 0.79 (0.34 to 1.87) | |
| BMI | 0.725 | |||||
| <25, OR (95% CI) | 1.00 | 1.13 (0.77 to 1.67) | 1.23 (0.84 to 1.80) | 1.48 (1.02 to 2.13) | 1.57 (1.11 to 2.20) | |
| ≥25, OR (95% CI) | 1.00 | 0.92 (0.64 to 1.32) | 0.84 (0.59 to 1.19) | 1.11 (0.79 to 1.55) | 1.18 (0.85 to 1.63) | |
| Brightness of bedroom ambient LAN | 0.905 | |||||
| Darkest level, OR (95% CI) | 1.00 | 1.03 (0.71 to 1.49) | 1.05 (0.74 to 1.51) | 1.37 (0.97 to 1.94) | 1.45 (1.04 to 2.03) | |
| Middle or Lightest level, OR (95% CI) | 1.00 | 1.06 (0.73 to 1.54) | 1.00 (0.68 to 1.47) | 1.23 (0.86 to 1.76) | 1.32 (0.95 to 1.83) | |
| Diabetes | 0.724 | |||||
| No, OR (95% CI) | 1.00 | 0.98 (0.7 to 1.30) | 0.99 (0.76 to 1.30) | 1.26 (0.97 to 1.63) | 1.29 (1.01 to 1.66) | |
| Yes, OR (95% CI) | 1.00 | 1.56 (0.66 to 3.69) | 1.11 (0.44 to 2.82) | 1.49 (0.64 to 3.47) | 1.88 (0.91 to 3.90) | |
| Hypertension | 0.683 | |||||
| No, OR (95% CI) | 1.00 | 1.01 (0.74 to 1.38) | 0.95 (0.69 to 1.29) | 1.20 (0.89 to 1.62) | 1.38 (1.03 to 1.84) | |
| Yes, OR (95% CI) | 1.00 | 1.06 (0.65 to 1.72) | 1.21 (0.76 to 1.94) | 1.50 (0.96 to 2.32) | 1.37 (0.91 to 2.06) | |
| Hyperuricemia | 0.077 | |||||
| No, OR (95% CI) | 1.00 | 0.98 (0.68 to 1.42) | 1.28 (0.90 to 1.82) | 1.37 (0.98 to 1.91) | 1.56 (1.15 to 2.12) | |
| Yes, OR (95% CI) | 1.00 | 1.02 (0.69 to 1.49) | 0.78 (0.53 to 1.15) | 1.16 (0.80 to 1.70) | 1.13 (0.78 to 1.64) | |
| Insomnia | 0.833 | |||||
| No, OR (95% CI) | 1.00 | 0.99 (0.72 to 1.36) | 0.96 (0.70 to 1.32) | 1.21 (0.89 to 1.63) | 1.38 (1.04 to 1.84) | |
| Yes, OR (95% CI) | 1.00 | 1.11 (0.70 to 178) | 1.10 (0.70 to 1.75) | 1.41 (0.91 to 2.20) | 1.42 (0.93 to 2.15) | |
| Short sleep duration | 0.896 | |||||
| No, OR (95% CI) | 1.00 | 1.16 (0.77 to 1.74) | 1.15 (0.77 to 1.71) | 1.50 (1.03 to 2.19) | 1.49 (1.05 to 2.12) | |
| Yes, OR (95% CI) | 1.00 | 0.98 (0.69 to 1.38) | 0.92 (0.65 to 1.30) | 1.13 (0.81 to 1.59) | 1.31 (0.95 to 1.81) | |
| Mediators | Effect Size (95% CI) | p-Value |
|---|---|---|
| Systolic blood pressure (mmHg) | ||
| ACME | −0.021 (−0.060 to 0.006) | 0.160 |
| ADE | −1.188 (−1.916 to −0.458) | <0.001 |
| Total effect | −1.210 (−1.924 to −0.483) | <0.001 |
| Proportion of mediation | 0.018 (−0.006 to 0.073) | 0.160 |
| Diastolic blood pressure (mmHg) | ||
| ACME | −0.077 (−0.134 to −0.030) | <0.001 |
| ADE | −1.133 (−1.851 to −0.409) | <0.001 |
| Total effect | −1.210 (−1.925 to −0.483) | <0.001 |
| Proportion of mediation | 0.064 (0.024 to 0.167) | <0.001 |
| Fasting blood glucose (mmol/L) | ||
| ACME | 0.037 (−0.021 to 0.093) | 0.200 |
| ADE | −1.231 (−1.919 to −0.504) | <0.001 |
| Total effect | −1.194 (−1.885 to −0.463) | <0.001 |
| Proportion of mediation | −0.031 (−0.113 to 0.018) | <0.001 |
| Serum uric acid (μmol/L) | ||
| ACME | −0.002 (−0.019 to 0.010) | 0.730 |
| ADE | −1.286 (−2.068 to −0.545) | 0.004 |
| Total effect | −1.288 (−2.070 to −0.548) | 0.004 |
| Proportion of mediation | 0.002 (−0.009 to 0.015) | 0.730 |
| Sleep duration (hours) | ||
| ACME | 0.031 (−0.049 to 0.112) | 0.480 |
| ADE | −1.243 (−1.893 to −0.503) | <0.001 |
| Total effect | −1.213 (−1.867 to −0.485) | <0.001 |
| Proportion of mediation | −0.025 (−0.125 to 0.045) | <0.001 |
| AIS score | ||
| ACME | −0.014 (−0.047 to 0.005) | 0.210 |
| ADE | −1.200 (−1.882 to −0.466) | <0.001 |
| Total effect | −1.214 (−1.896 to −0.489) | <0.001 |
| Proportion of mediation | 0.012 (−0.006 to 0.053) | 0.210 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Zhang, S.; Wang, Y.; Zhu, Y.; Li, X.; Song, Y.; Yuan, J. Rotating Night Shift Work, Exposure to Light at Night, and Glomerular Filtration Rate: Baseline Results from a Chinese Occupational Cohort. Int. J. Environ. Res. Public Health 2020, 17, 9035. https://doi.org/10.3390/ijerph17239035
Zhang S, Wang Y, Zhu Y, Li X, Song Y, Yuan J. Rotating Night Shift Work, Exposure to Light at Night, and Glomerular Filtration Rate: Baseline Results from a Chinese Occupational Cohort. International Journal of Environmental Research and Public Health. 2020; 17(23):9035. https://doi.org/10.3390/ijerph17239035
Chicago/Turabian StyleZhang, Shengkui, Yongbin Wang, Ying Zhu, Xiaoming Li, Yang Song, and Juxiang Yuan. 2020. "Rotating Night Shift Work, Exposure to Light at Night, and Glomerular Filtration Rate: Baseline Results from a Chinese Occupational Cohort" International Journal of Environmental Research and Public Health 17, no. 23: 9035. https://doi.org/10.3390/ijerph17239035
APA StyleZhang, S., Wang, Y., Zhu, Y., Li, X., Song, Y., & Yuan, J. (2020). Rotating Night Shift Work, Exposure to Light at Night, and Glomerular Filtration Rate: Baseline Results from a Chinese Occupational Cohort. International Journal of Environmental Research and Public Health, 17(23), 9035. https://doi.org/10.3390/ijerph17239035






