Does Hydrotherapy Impact Behaviours Related to Mental Health and Well-Being for Children with Autism Spectrum Disorder? A Randomised Crossover-Controlled Pilot Trial
Abstract
1. Introduction
2. Materials and Methods
2.1. Participants
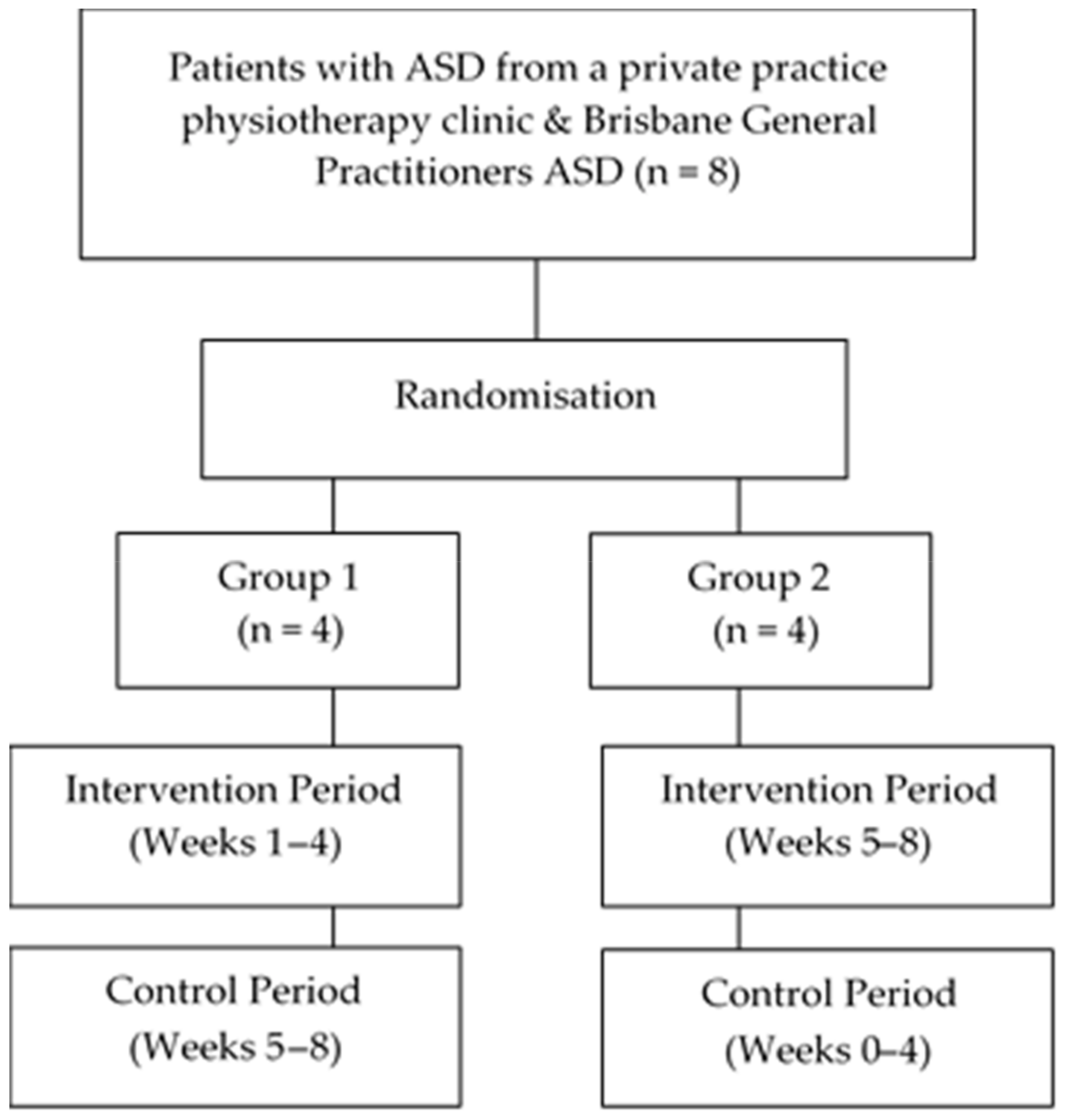
2.2. Study Design
2.3. Hydrotherapy Intervention
2.4. Outcome Measures
2.5. Statistical Analysis
3. Results
3.1. Participant Flow
3.2. Treatment Characteristics
3.3. Adverse Events
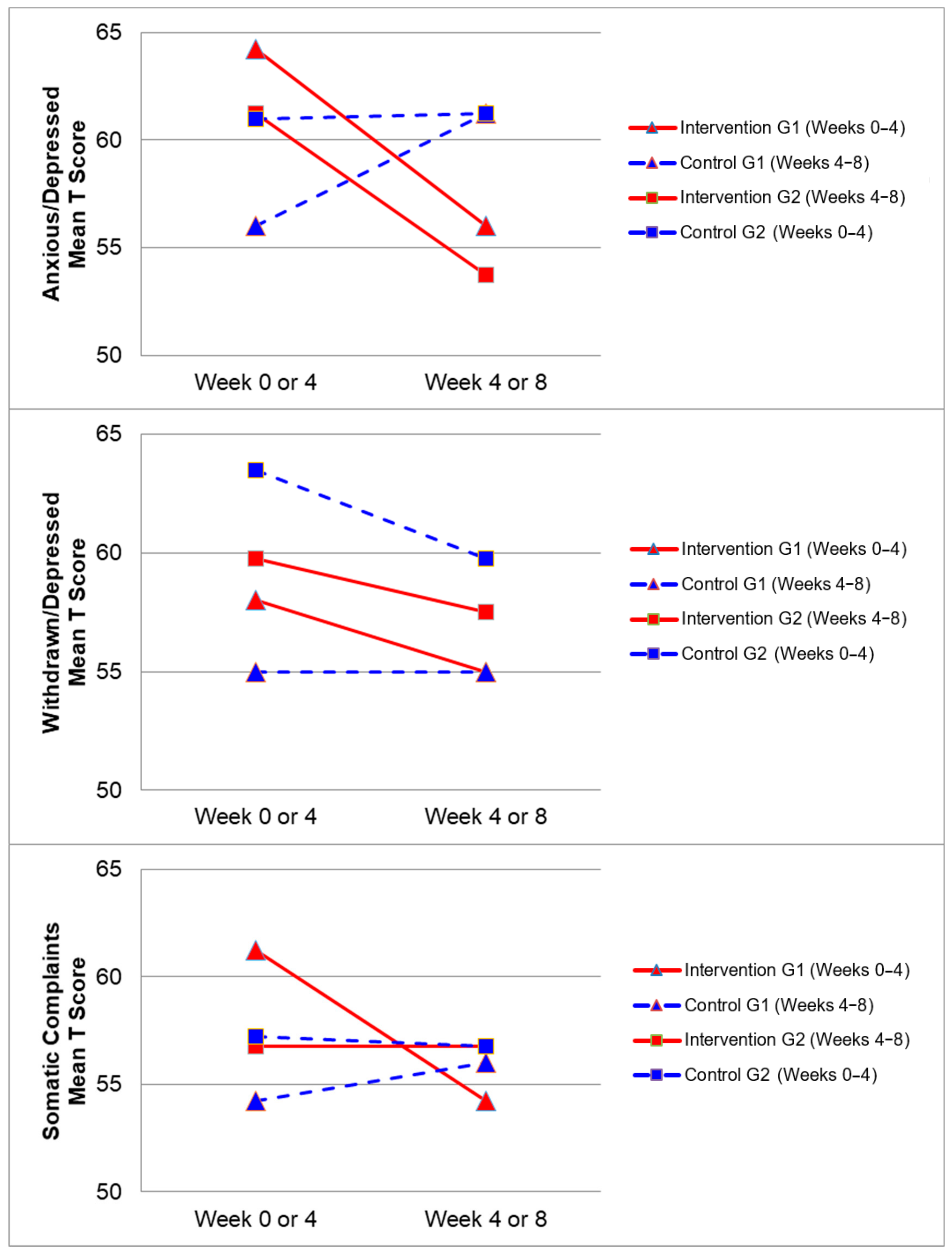
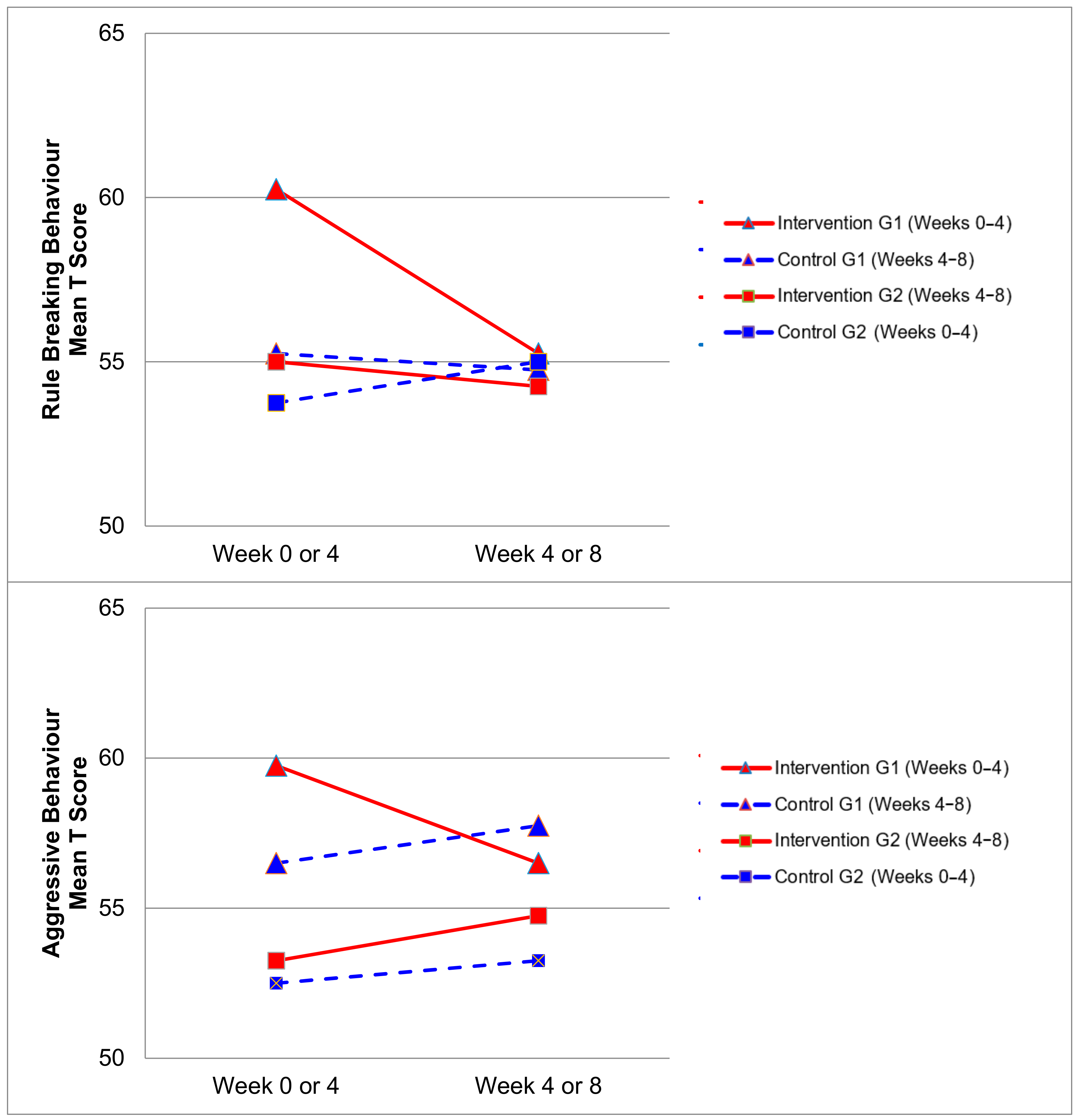
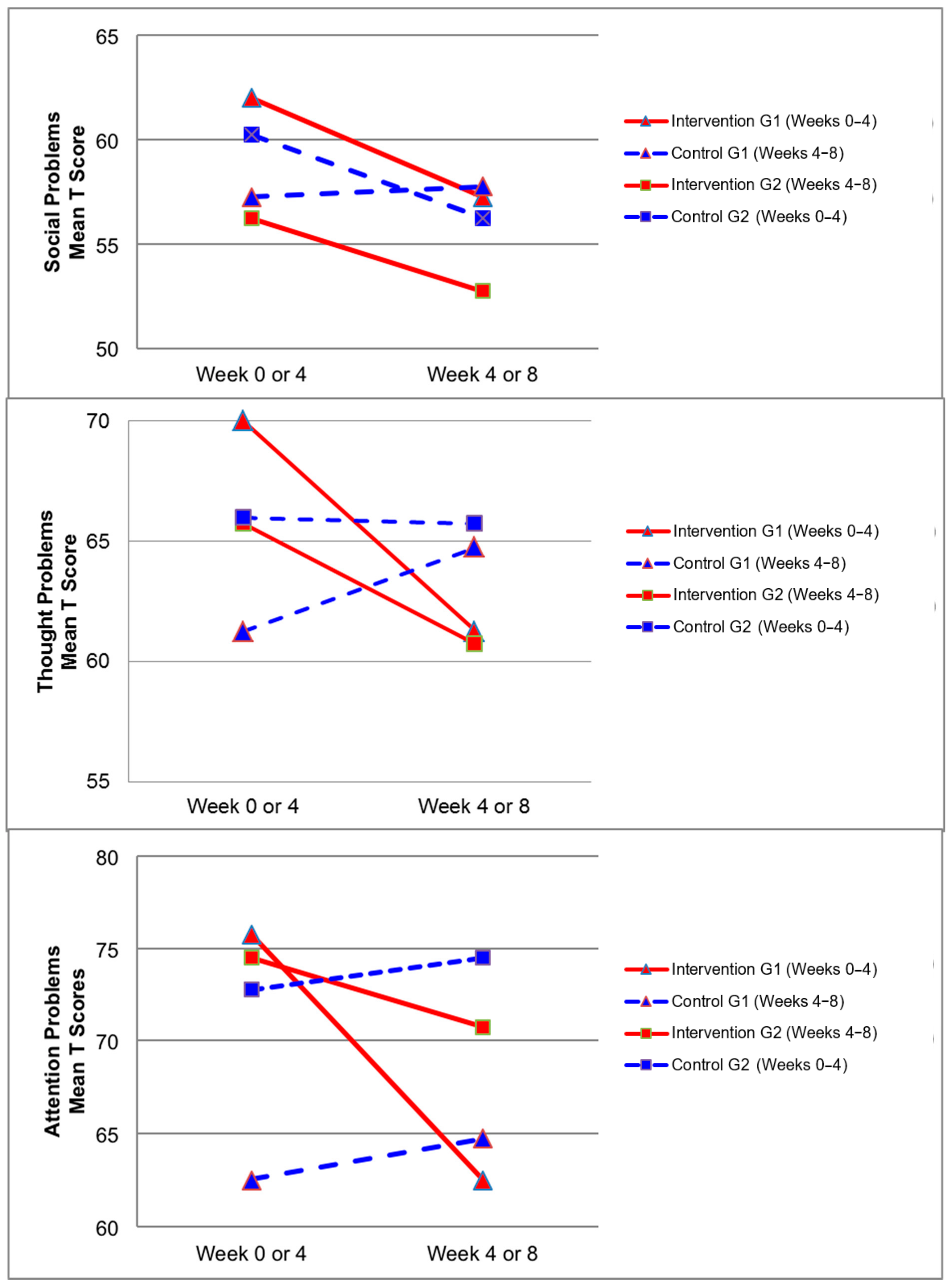
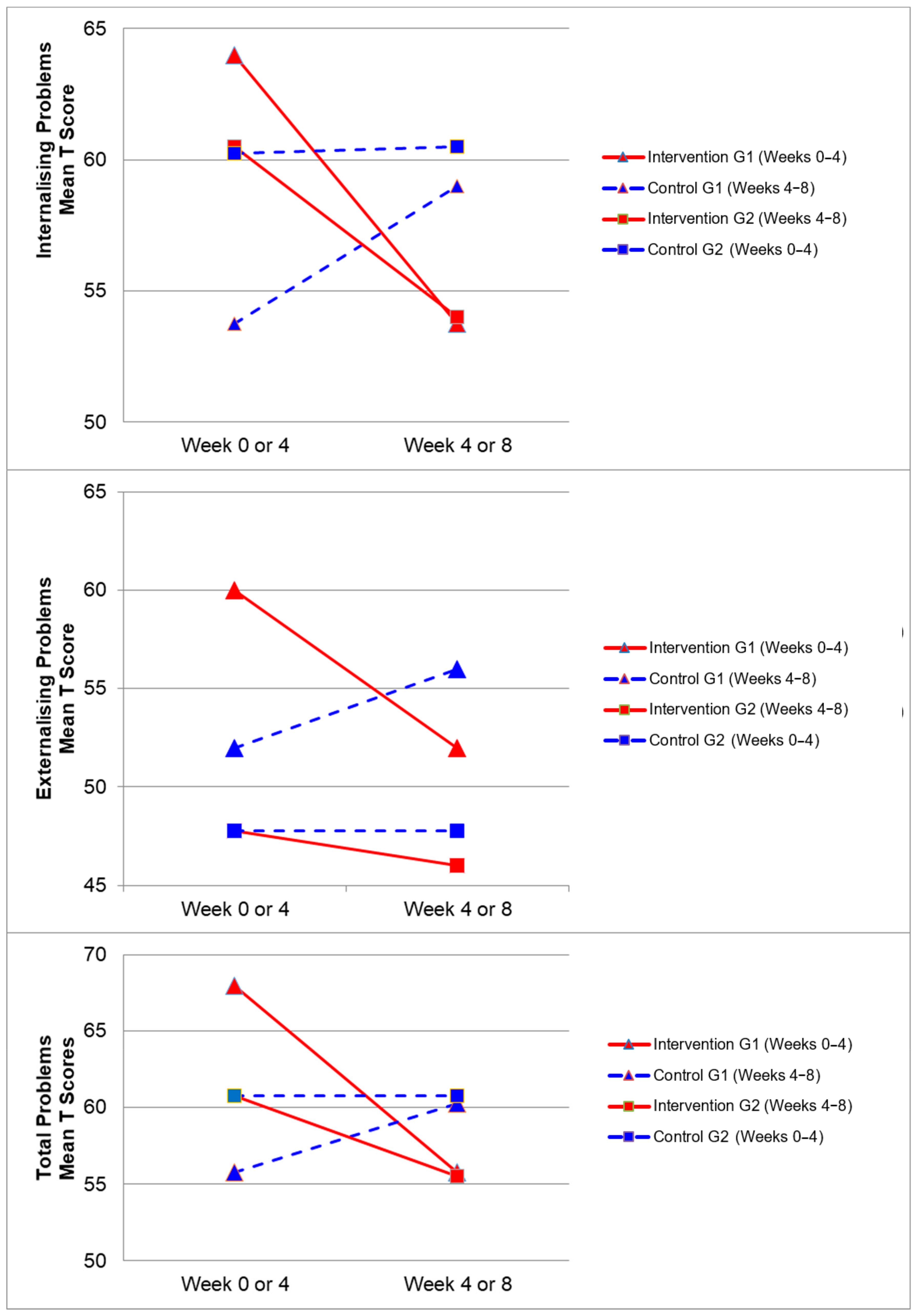
3.4. CBCL Scores
4. Discussion
4.1. Strengths
4.2. Limitations and Future Research
5. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Association, A.P. Diagnostic and Statistical Manual of Mental Disorders (DSM-5®); American Psychiatric Pub: Washington, DC, USA, 2013. [Google Scholar]
- Provost, B.; Lopez, B.R.; Heimerl, S. A comparison of motor delays in young children: Autism spectrum disorder, developmental delay, and developmental concerns. J. Autism Dev. Disord. 2007, 37, 321–328. [Google Scholar] [CrossRef]
- Bandini, L.G.; Gleason, J.; Curtin, C.; Lividini, K.; Anderson, S.E.; Cermak, S.A.; Maslin, M.; Must, A. Comparison of physical activity between children with autism spectrum disorders and typically developing children. Autism 2013, 17, 44–54. [Google Scholar] [CrossRef] [PubMed]
- Torrance, B.; McGuire, K.A.; Lewanczuk, R.; McGavock, J. Overweight, physical activity and high blood pressure in children: A review of the literature. Vasc. Health Risk Manag. 2007, 3, 139. [Google Scholar] [PubMed]
- Biddle, S.J.; Asare, M. Physical activity and mental health in children and adolescents: A review of reviews. Br. J. Sports Med. 2011, 45, 886–895. [Google Scholar] [CrossRef] [PubMed]
- Diener, E. Subjective well-being: The science of happiness and a proposal for a national index. Am. Psychol. 2000, 55, 34. [Google Scholar] [CrossRef]
- Ryff, C.D. Happiness is everything, or is it? Explorations on the meaning of psychological well-being. J. Personal. Soc. Psychol. 1989, 57, 1069. [Google Scholar] [CrossRef]
- Ahn, S.; Fedewa, A.L. A meta-analysis of the relationship between children’s physical activity and mental health. J. Pediatric. Psychol. 2011, 36, 385–397. [Google Scholar] [CrossRef]
- Penedo, F.J.; Dahn, J.R. Exercise and well-being: A review of mental and physical health benefits associated with physical activity. Curr. Opin. Psychiatry 2005, 18, 189–193. [Google Scholar] [CrossRef]
- Bremer, E.; Crozier, M.; Lloyd, M. A systematic review of the behavioural outcomes following exercise interventions for children and youth with autism spectrum disorder. Autism 2016, 20, 899–915. [Google Scholar] [CrossRef]
- Lang, R.; Koegel, L.K.; Ashbaugh, K.; Regester, A.; Ence, W.; Smith, W. Physical exercise and individuals with autism spectrum disorders: A systematic review. Res. Autism Spectr. Disord. 2010, 4, 565–576. [Google Scholar] [CrossRef]
- Wrotniak, B.H.; Epstein, L.H.; Dorn, J.M.; Jones, K.E.; Kondilis, V.A. The relationship between motor proficiency and physical activity in children. Pediatrics 2006, 118, e1758–e1765. [Google Scholar] [CrossRef] [PubMed]
- Dumas, H.; Francesconi, S. Aquatic therapy in pediatrics. Phys. Occup. Ther. Pediatrics 2001, 20, 63–78. [Google Scholar]
- Sam, S.K.L. Effects of exercise-based interventions for children with Autism Spectrum Disorder (ASD): A systematic review and meta-analysis. Res. Autism Spectr. Disord. 2015, 6, 46–57. [Google Scholar]
- Mortimer, R.; Privopoulos, M.; Kumar, S. The effectiveness of hydrotherapy in the treatment of social and behavioral aspects of children with autism spectrum disorders: A systematic review. J. Multidiscip. Healthc. 2014, 7, 93. [Google Scholar] [PubMed]
- Christie, B. Doctors revise declaration of Helsinki. BMJ Br. Med. J. 2000, 321, 913. [Google Scholar] [CrossRef]
- The National Health and Medical Research Council. The Australian Research Council; the Australian Vice-Chancellors’ Committee. National Statement on Ethical Conduct in Human Research 2007 (Updated May 2015) Commonwealth of Australia. Available online: https://www.nhmrc.gov.au/about-us/publications/national-statement-ethical-conduct-human-research-2007-updated-2018 (accessed on 13 January 2020).
- Carere, A.; Warburton, M.; Orr, R.M. Does hydrotherapy improve a patient’s sense of mental wellbeing to a greater extent than physiotherapy prescribed home exercise programs alone. J. Aquat. Phys. Ther. 2017, 25, 2–11. [Google Scholar]
- Achenbach, T.M. Child Behavior Checklist for Ages 6–18; University of Vermont: Burlington, VT, USA, 2001. [Google Scholar]
- Achenbach, T.M.; Rescorla, L.A. Manual for the ASEBA Preschool Forms and Profiles; University of Vermont: Burlington, VT, USA, 2000. [Google Scholar]
- Mazefsky, C.A.; Anderson, R.; Conner, C.M.; Minshew, N. Child behavior checklist scores for school-aged children with autism: Preliminary evidence of patterns suggesting the need for referral. J. Psychopathol. Behav. Assess. 2011, 33, 31–37. [Google Scholar] [CrossRef]
- Deighton, J.; Croudace, T.; Fonagy, P.; Brown, J.; Patalay, P.; Wolpert, M. Measuring mental health and wellbeing outcomes for children and adolescents to inform practice and policy: A review of child self-report measures. Child. Adolesc. Psychiatry Ment. Health 2014, 8, 14. [Google Scholar] [CrossRef]
- Sawyer, M.G.; Arney, F.M.; Baghurst, P.A.; Clark, J.J.; Graetz, B.W.; Kosky, R.J.; Nurcombe, B.; Patton, G.C.; Prior, M.R.; Raphael, B. The Mental Health of Young People in Australia; Blackwell Science: Hoboken, NJ, USA, 2000. [Google Scholar]
- Sawyer, M.G.; Arney, F.M.; Baghurst, P.A.; Clark, J.J.; Graetz, B.W.; Kosky, R.J.; Nurcombe, B.; Patton, G.C.; Prior, M.R.; Raphael, B. The mental health of young people in Australia: Key findings from the child and adolescent component of the national survey of mental health and well-being. Aust. N. Z. J. Psychiatry 2001, 35, 806–814. [Google Scholar] [CrossRef]
- Jelsma, D.; Geuze, R.H.; Mombarg, R.; Smits-Engelsman, B.C. The impact of Wii Fit intervention on dynamic balance control in children with probable Developmental Coordination Disorder and balance problems. Hum. Mov. Sci. 2014, 33, 404–418. [Google Scholar] [CrossRef]
- Kreutzer, J.S.; DeLuca, J.; Caplan, B. Encyclopedia of Clinical Neuropsychology; Springer: Berlin/Heidelberg, Germany, 2011. [Google Scholar]
- Shafii, S.L.R.N.; Shafii, M.M.D. Clinical Guide to Depression in Children and Adolescents; APA: Washington, DC, USA, 1992. [Google Scholar]
- Cohen, J. Statistical Power Analysis for the Behavioural Sciences, 2nd ed.; Academic Press: Cambridge, MA, USA, 1988. [Google Scholar]
- Bölte, S.; Dickhut, H.; Poustka, F. Patterns of parent-reported problems indicative in autism. Psychopathology 1999, 32, 93–97. [Google Scholar] [CrossRef] [PubMed]
- Duarte, C.S.; Bordin, I.A.; De Oliveira, A.; Bird, H. The CBCL and the identification of children with autism and related conditions in Brazil: Pilot findings. J. Autism Dev. Disord. 2003, 33, 703–707. [Google Scholar] [CrossRef] [PubMed]
- Noterdaeme, M.; Minow, F.; Amorosa, H. Applicability of the Child Behavior Checklist in developmentally delayed children. Zeitschrift für Kinder und Jugendpsychiatrie und Psychotherapie 1999, 27, 183–188. [Google Scholar] [CrossRef]
- Galper, D.I.; Trivedi, M.H.; Barlow, C.E.; Dunn, A.L.; Kampert, J.B. Inverse association between physical inactivity and mental health in men and women. Med. Sci. Sports Exerc. 2006, 38, 173–178. [Google Scholar] [CrossRef] [PubMed]
- Oriel, K.N.; Kanupka, J.W.; DeLong, K.S.; Noel, K. The impact of aquatic exercise on sleep behaviors in children with autism spectrum disorder: A pilot study. Focus Autism Other Dev. Disabil. 2016, 31, 254–261. [Google Scholar] [CrossRef]
- Pan, C.-Y. Effects of water exercise swimming program on aquatic skills and social behaviors in children with autism spectrum disorders. Autism 2010, 14, 9–28. [Google Scholar] [CrossRef] [PubMed]
- Chu, C.-H.; Pan, C.-Y. The effect of peer-and sibling-assisted aquatic program on interaction behaviors and aquatic skills of children with autism spectrum disorders and their peers/siblings. Res. Autism Spectr. Disord. 2012, 6, 1211–1223. [Google Scholar] [CrossRef]
- Ennis, E. The effects of a physical therapy-directed aquatic program on children with autism spectrum disorders. J. Aquat. Phys. Ther. 2011, 19, 4–10. [Google Scholar]
- Yanardag, M.; Akmanoglu, N.; Yilmaz, I. The effectiveness of video prompting on teaching aquatic play skills for children with autism. Disabil. Rehabil. 2013, 35, 47–56. [Google Scholar] [CrossRef]
- Yilmaz, I.; Yanardağ, M.; Birkan, B.; Bumin, G. Effects of swimming training on physical fitness and water orientation in autism. Pediatrics. Int. 2004, 46, 624–626. [Google Scholar] [CrossRef]
| Participants | Mean Age (Years) | Gender | Receives Special Education | Academic or Other Problems at School | Neuro -Developmental Diagnoses | Adjunct Therapy |
|---|---|---|---|---|---|---|
| 1–6 | 9.21 | M | Yes (n = 6) | Yes (n = 5) No (n = 1) | ASD (n = 6) ADHD (n = 1 | ST (n = 4) OT (n = 4) PT (n = 2) PSY (n = 1) TD (n = 1) |
| 7–8 | 7.26 | F | Yes (n = 1) No (n = 1) | Yes (n = 1) No (n = 1) | ASD (n = 2) | ST (n = 1) OT (n = 1) |
| Skill | Activity |
|---|---|
| Cardiovascular Fitness | • Free swim * Swimming through large plastic hoop * Horizontal rope climbing with 10 m nautical rope Somersaulting in waterJumping into water from pool edge Prolonged independent submersion * Diving to place/retrieve objects from pool bottom: rubber animals, play coins, rings * Races: front crawl, back crawl * |
| Swimming Skills | • Free swim * Races: front crawl, back crawl * Swimming through large plastic hoop * Diving to place/retrieve objects from pool bottom: rubber animals, play coins, rings * |
| Relaxation and Sensory Input | • Weaving/seaweeding Dragging through water with plastic kickboard on stomach and side Floating on back Prolonged independent submersion * Dragging forward/backward and spinning in inflatable ring |
| Cognitive tasks | • Shape matching with Shape-O Counting play diving coins |
| Balance | • Walking along narrow beam in water Walking along submerged 10 m nautical tight rope Egg and spoon balance up/down entry ramp * |
| Eye–Hand Coordination | • Throwing/catching soft soccer ball Diving to place/retrieve objects from pool bottom: rubber animals, play coins, rings * Play foam sword fighting Retrieving floating rings with foam sword or wooden spoon Ring toss Hitting and keeping rubber ball above water in group Egg and spoon balance up/down entry ramp * Tossing small plastic balls into floating hoop |
| Participant | Intervention 1 | Intervention 2 | Intervention 3 | Intervention 4 |
|---|---|---|---|---|
| 1 | 4 | 3 | 3 | N/A |
| 2 | 4 | 4 | 4 | 4 |
| 3 | 1 | 1 | 4 | 4 |
| 4 | 3 | 4 | 3 | 4 |
| 5 | 3 | 4 | N/A | N/A |
| 6 | 4 | 4 | N/A | 4 |
| 7 | 3 | 3 | 3 | 3 |
| 8 | 4 | 1 | 2 | 2 |
| Domains and Syndromes | Groups 1 and 2 Combined Mean (SD) | Group 1 Mean (SD) | Group 2 Mean (SD) |
|---|---|---|---|
| Internalising Problems Domain | |||
| Anxious/Depressed Syndrome | 83.00 (18.38) | 90.75 (9.84) | 75.25 (23.06) |
| Withdrawn/Depressed Syndrome | 75.63 (17.04) | 73.00 (20.45) | 78.25 (15.52) |
| Somatic Complaints Syndrome | 75.38 (20.90) | 81.75 (21.63) | 69.00 (21.02) |
| Domain Summary | 79.63 (24.32) | 87.5 (15.26) | 71.75 (31.33) |
| Externalising Problems Domain | |||
| Rule Breaking Behaviour Syndrome | 71.75 (19.20) | 81.50 (15.61) | 62.00 (19.04) |
| Aggressive Behaviour Syndrome | 68.13 (16.53) | 76.75 (17.56) | 59.50 (11.44) |
| Domain Summary | 62.63 (28.36) | 79.00 (14.51) | 46.25 (30.84) |
| Other Problems Domain | |||
| Social Problems Syndrome | 83.75 (10.33) | 86.00 (10.42) | 81.5 (11.27) |
| Thought Problems Syndrome | 92.00 (11.71) | 94.25 (5.85) | 89.75 (16.50) |
| Attention Problems Syndrome | 98.38 (0.92) | 98.50 (1.00) | 98.25 (0.96) |
| Total Problems | 88.375 (11.48) | 94.00 (8.72) | 82.75 (12.12) |
| Domains and Syndromes | Intervention Period | Control Period | ||||||
|---|---|---|---|---|---|---|---|---|
| Pre-Intervention n = 8 | Post-Intervention n = 8 | Change Score | Pre- to Post-Intervention Difference | Pre-Control n = 8 | Post-Control n = 8 | Change Score | Pre- to Post-Control Difference | |
| Mean (SD) | Mean (SD) | % | p-value | Mean (SD) | Mean (SD) | % | p-value | |
| Internalising Problems Domain | ||||||||
| Anxious/Depressed Syndrome | 62.75 (9.44) | 54.88 (5.17) | 7.87 | 0.02 * ††† 1 | 58.50 (9.72) | 61.25 (9.51) | −2.75 | 0.31 |
| Withdrawn/Depressed Syndrome | 58.88 (7.20) | 56.25 (7.05) | 2.63 | 0.34 | 59.25 (11.96) | 57.38 (7.07) | 1.88 | 0.50 |
| Somatic Complaints Syndrome | 59.00 (8.60) | 55.50 (7.03) | 3.50 | 0.18 | 55.75 (7.40) | 56.38 (7.35) | −0.63 | 0.56 |
| Domain Summary | 62.25 (7.74) | 53.88 (8.06) | 8.38 | 0.03 * ††† 2 | 57.00 (11.76) | 59.75 (7.81) | −2.75 | 0.29 |
| Externalising Problems Domain | ||||||||
| Rule Breaking Behaviour Syndrome | 57.63 (7.62) | 54.75 (7.32) | 2.88 | 0.07 | 54.50 (6.65) | 54.88 (6.42) | −0.38 | 0.84 |
| Aggressive Behaviour Syndrome | 56.50 (8.19) | 55.63 (10.24) | 0.875 | 0.59 | 54.50 (8.59) | 55.50(9.35) | −1.00 | 0.51 |
| Domain Summary | 53.88 (12.33) | 49.00 (14.21) | 4.88 | 0.06 | 49.88 (11.36) | 51.88 (11.99) | −2.00 | 0.37 |
| Other Problems Domain | ||||||||
| Social Problems Syndrome | 59.13 (5.77) | 55.00 (5.45) | 4.13 | 0.08 | 58.75 (6.11) | 57.00 (3.78) | 1.75 | 0.36 |
| Thought Problems Syndrome | 67.88 (7.00) | 61.00 (9.62) | 6.88 | 0.03 * ††† 3 | 63.63 (10.01) | 65.25 (7.74) | −1.63 | 0.59 |
| Attention Problems Syndrome | 75.13 (9.88) | 66.63 (12.60) | 8.50 | 0.01 * †† 4 | 67.63 (10.91) | 69.63 (13.46) | −2.00 | 0.53 |
| Total Problems | 64.38 (6.09) | 55.63 (10.22) | 8.75 | 0.02 * ††† 5 | 58.25 (10.00) | 60.50 (7.21) | −2.25 | 0.32 |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Mills, W.; Kondakis, N.; Orr, R.; Warburton, M.; Milne, N. Does Hydrotherapy Impact Behaviours Related to Mental Health and Well-Being for Children with Autism Spectrum Disorder? A Randomised Crossover-Controlled Pilot Trial. Int. J. Environ. Res. Public Health 2020, 17, 558. https://doi.org/10.3390/ijerph17020558
Mills W, Kondakis N, Orr R, Warburton M, Milne N. Does Hydrotherapy Impact Behaviours Related to Mental Health and Well-Being for Children with Autism Spectrum Disorder? A Randomised Crossover-Controlled Pilot Trial. International Journal of Environmental Research and Public Health. 2020; 17(2):558. https://doi.org/10.3390/ijerph17020558
Chicago/Turabian StyleMills, Whitney, Nicholas Kondakis, Robin Orr, Michael Warburton, and Nikki Milne. 2020. "Does Hydrotherapy Impact Behaviours Related to Mental Health and Well-Being for Children with Autism Spectrum Disorder? A Randomised Crossover-Controlled Pilot Trial" International Journal of Environmental Research and Public Health 17, no. 2: 558. https://doi.org/10.3390/ijerph17020558
APA StyleMills, W., Kondakis, N., Orr, R., Warburton, M., & Milne, N. (2020). Does Hydrotherapy Impact Behaviours Related to Mental Health and Well-Being for Children with Autism Spectrum Disorder? A Randomised Crossover-Controlled Pilot Trial. International Journal of Environmental Research and Public Health, 17(2), 558. https://doi.org/10.3390/ijerph17020558






