Evidence for Environmental Noise Effects on Health for the United Kingdom Policy Context: A Systematic Review of the Effects of Environmental Noise on Mental Health, Wellbeing, Quality of Life, Cancer, Dementia, Birth, Reproductive Outcomes, and Cognition
Abstract
1. Introduction
2. Materials and Methods
2.1. Scope of the Review
2.2. Search Strategy
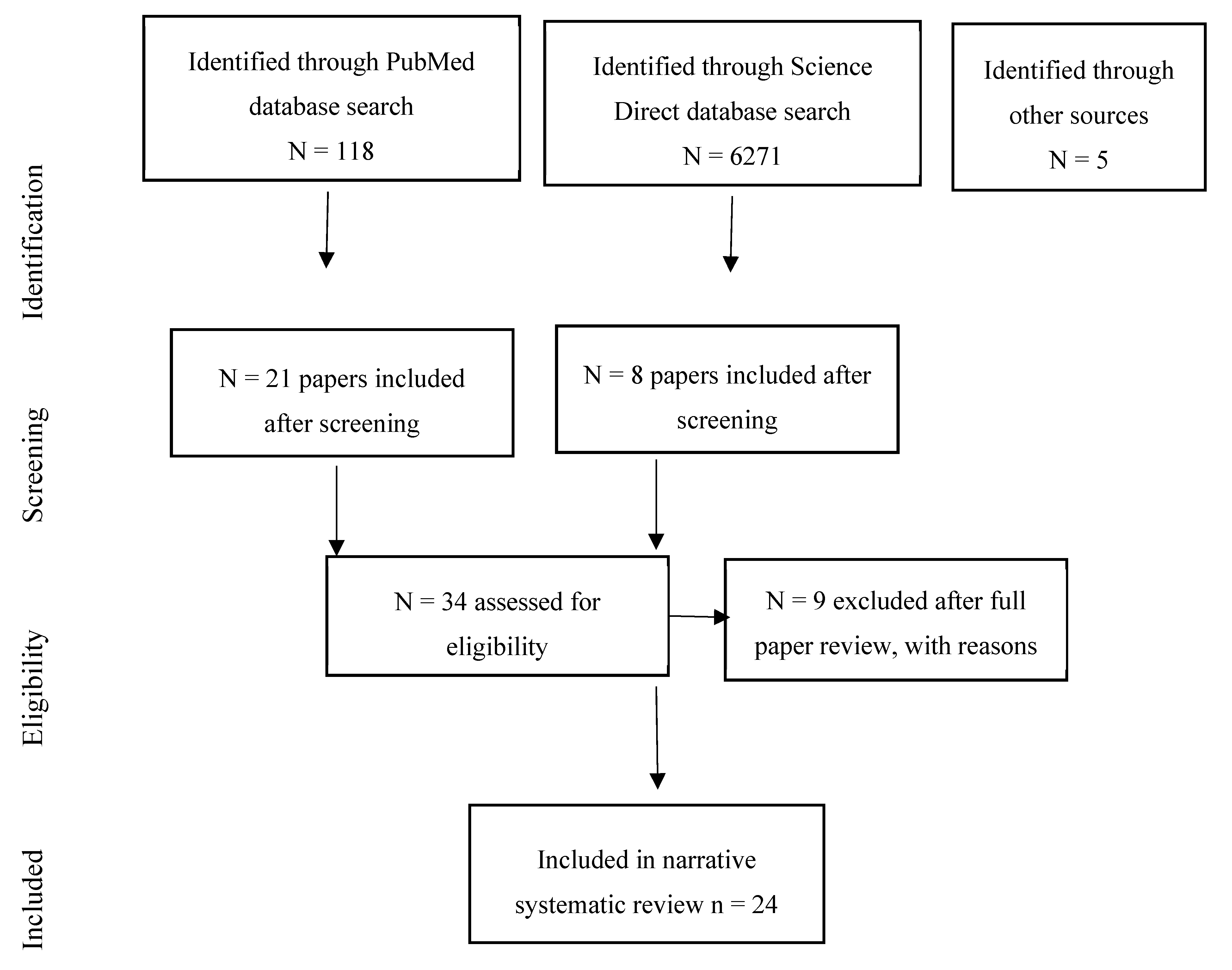
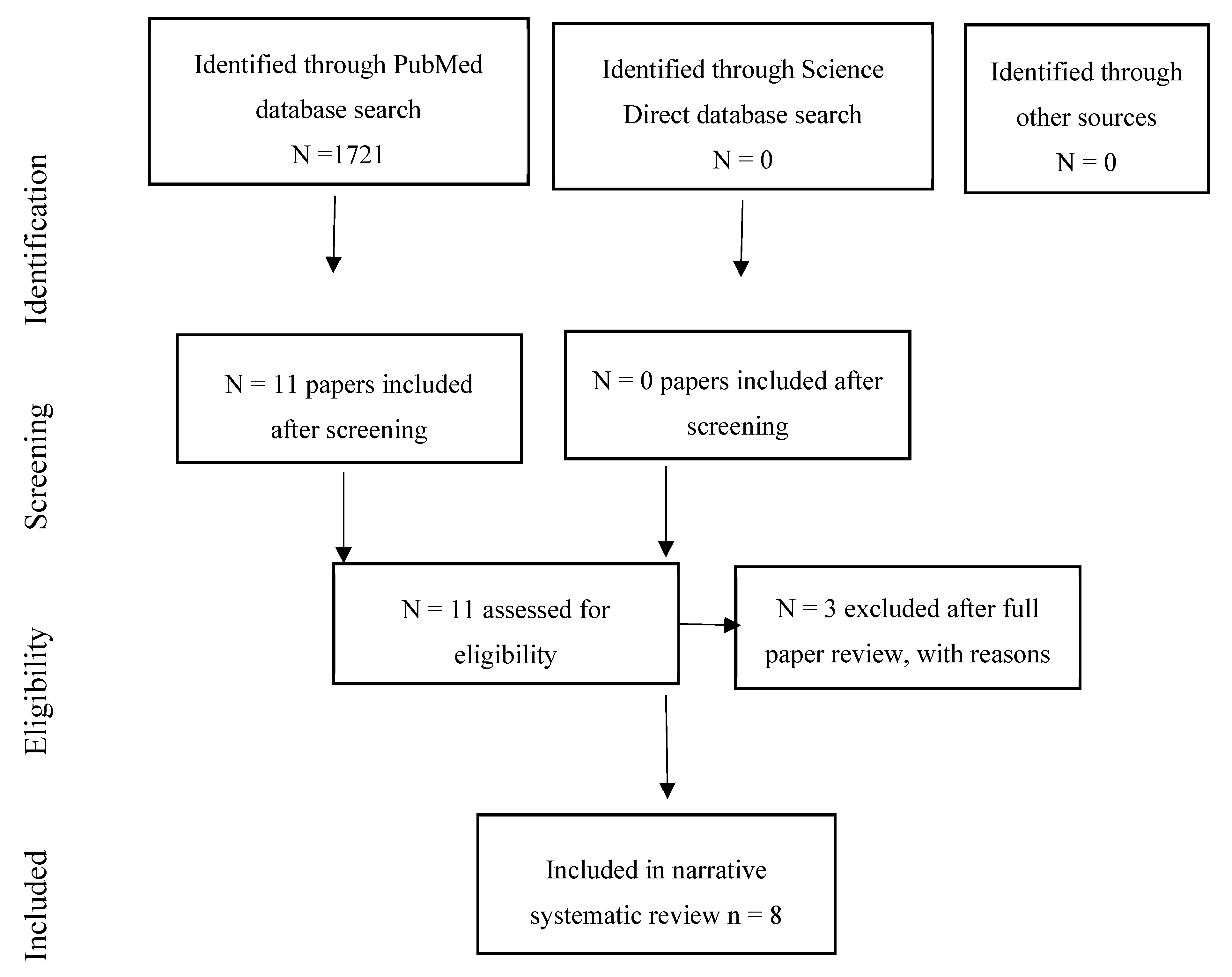
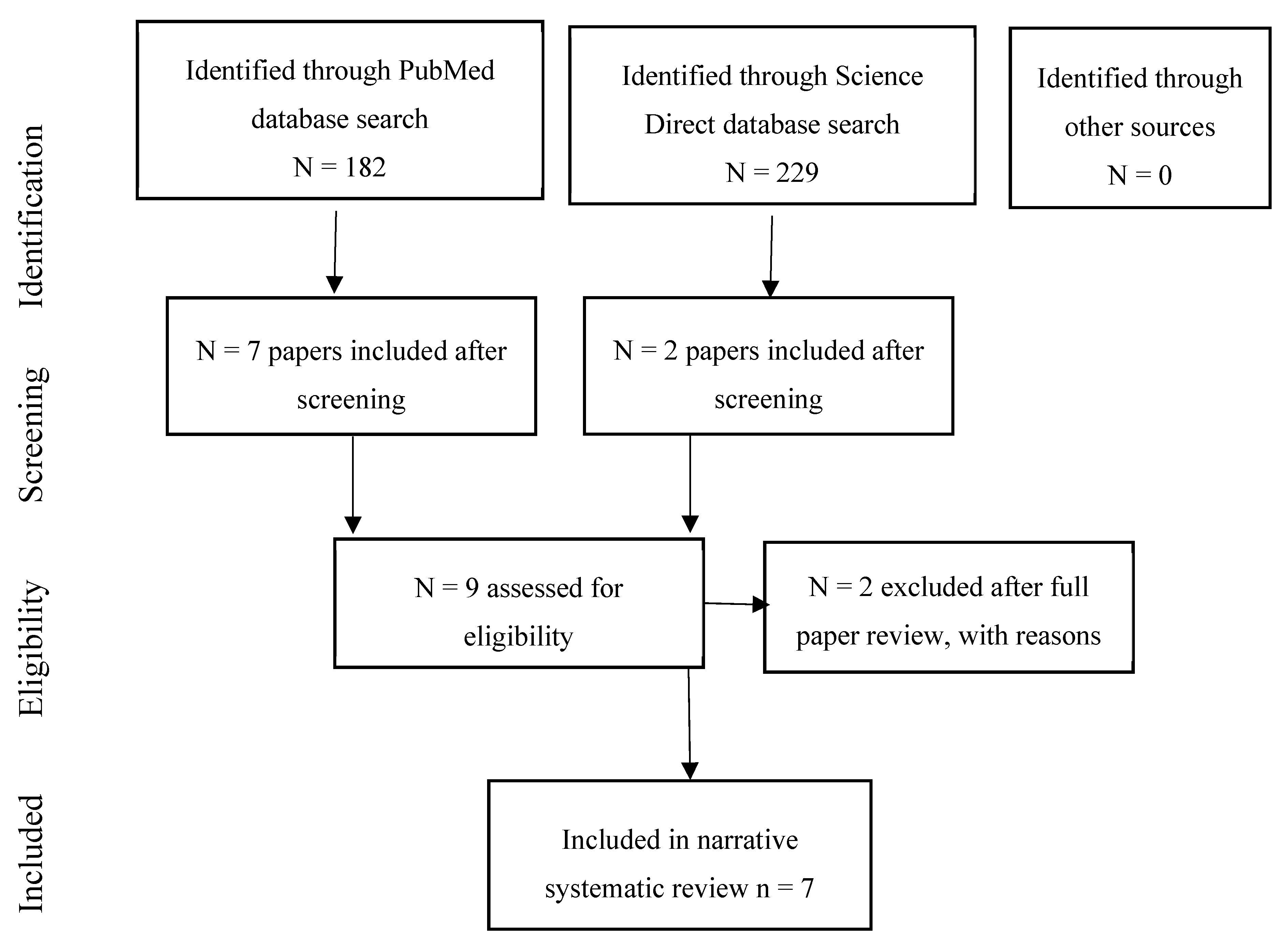
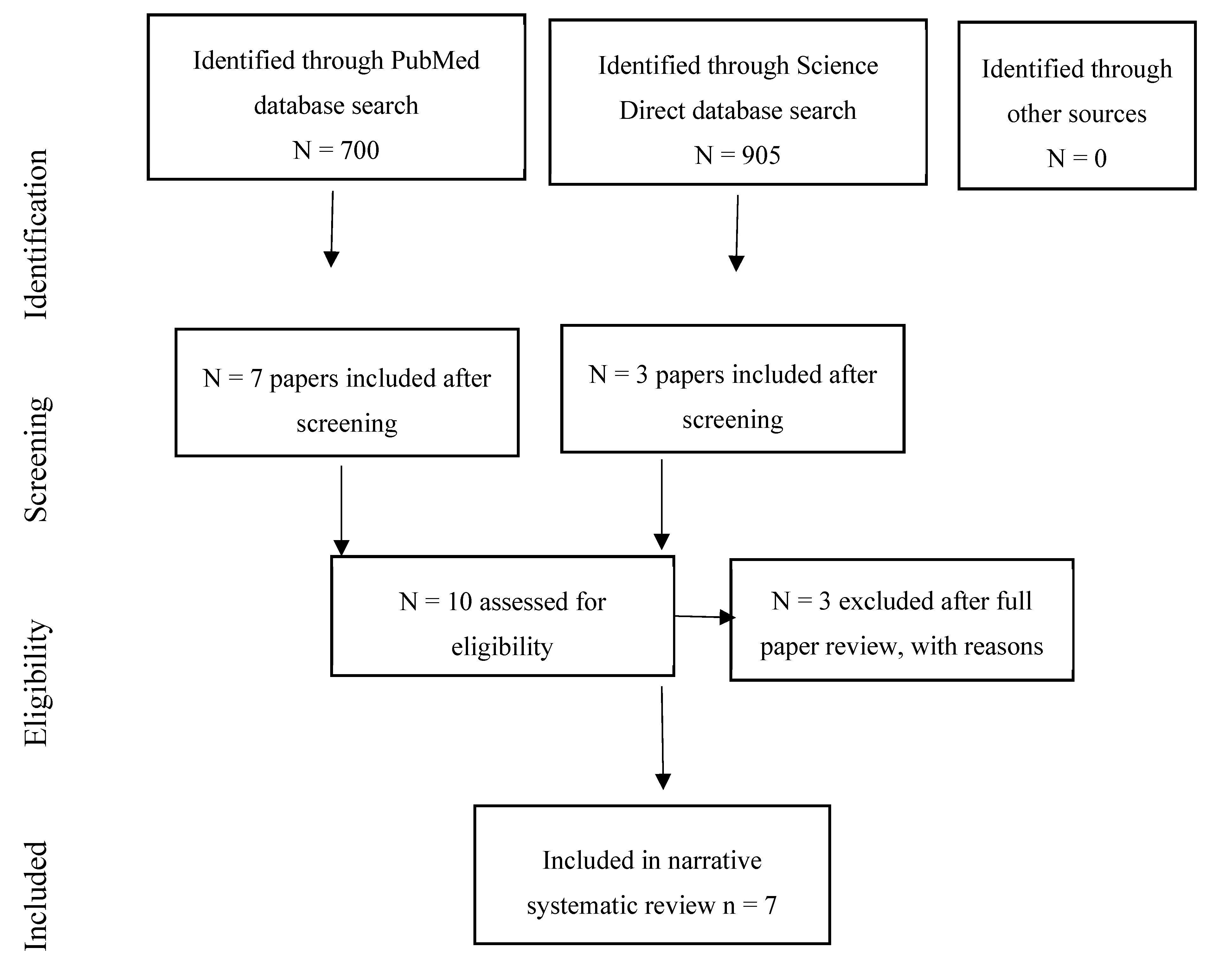
2.3. Data Screening and Review Process
2.4. Data Extraction
- Population: the inclusion criteria were studies of the general population or specific sub-groups of the population in settings (home, public venues, schools).
- Exposure: the inclusion criteria were exposure to high levels of environmental noise from the sources specified above. Included studies either measure or calculate noise exposure levels expressed in decibel values at an appropriate location for the study participants (e.g., home, school). Where calculated levels were available for transportation noise, they reflected the use of roads, railways lines and flight routes. Exclusion criteria included studies using distance to source as a proxy for noise exposure and studies using subjective ratings of noise exposure (including noise annoyance) as a proxy for noise exposure.
- Comparator: the inclusion criteria were that the study has a comparator group with no noise exposure or a lower level of noise exposure.
- Assessment of outcome: the inclusion criteria were that the outcome data came from medical records or interviews or cognitive testing using a known scale or validated assessment method or that the outcome was self-reported from a questionnaire.
- Noise exposure assessment leading to information bias: evaluating whether the paper used established noise metrics in dB; the timeframe of noise measurements, if applicable; and quality of noise modelling, if applicable.
- Bias due to confounding: evaluating whether the study used matching or adjustment in the analysis for potential confounding factors, such as socioeconomic status, which can influence both noise exposure and the health outcome.
- Bias due to selection of participants: whether participants are randomly sampled from a known population and whether the response rate was higher than 60%. Consideration of bias associated with drop out for longitudinal studies.
- Outcome assessment leading to information bias I: whether the assessment of the outcome is objectively measured using a known scale or validated measure.
- Outcome assessment leading to information bias II: whether the assessment is blinded for exposure information in cohort.
2.5. Evaluating the Quality of the Evidence
3. Results
3.1. Mental Health, Wellbeing, and Quality of Life
3.1.1. GRADE Evaluation
3.1.2. Comparison of the Systematic Review Findings of the Review Undertaken for the WHO
3.2. Cancer
GRADE Evaluation
3.3. Dementia and other Neurodegenerative Outcomes
GRADE Evaluation
3.4. Birth and Reproductive Outcomes
3.4.1. GRADE Evaluation
3.4.2. Comparison of the Systematic Review Findings of the Review Undertaken for the WHO
3.5. Cognition
3.5.1. GRADE Evaluation
3.5.2. Comparison of the Systematic Review Findings of the Review Undertaken for the WHO
4. Discussion
4.1. Recommendations for Consideration by the IGCB(N)
4.2. Strengths and Limitations
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
Appendix A
Appendix A.1. Search Terms
- longitudinal study or studies
- prospective study or studies
- retrospective study or studies
- ecological study or studies
- cohort study or studies
- case study or studies
- cross-sectional or cross-sectional study or studies
- noise
- motorcycle or motorcycles and noise
- environment or environmental noise
- residence characteristics or community noise
- traffic noise
- road noise
- motor vehicle noise
- aircraft noise
- airport noise
- railway noise
- industry noise or industrial noise
- build * noise
- vent * noise
- mechanic * and service noise
- air and condition * noise
- neighbor */neighbor * noise
- train noise
- transportation noise
- leisure activities/leisure time and noise
- low frequency noise
- classroom or school noise
- combined noise
- nuisance noise
- air pollution and noise
- household noise
- wind turbine noise/wind farm noise
- dementia
- vascular dementia
- Alzheimer’s disease or Alzheimer disease
- Lewy bodies dementia
- frontotemporal dementia
- cancer
- neoplasm
- carcinoma
- sarcoma
- myeloma
- leukemia
- lymphoma
- birth weight
- pregnancy
- fetus/foetus
- preterm
- gestation
- infertility
- sterile
- malformation
- birth
- labor/labour
- prenatal
- perinatal
- fert * or infert *
- mental health
- emotions or emotional disease/disorder
- psychological diagnosis or symptoms
- mental disorders
- psychiatric disorders
- conduct disorder
- anxiety
- depressive disorder or depression
- health status
- wellbeing or well being or well-being
- personal satisfaction
- quality of life
- behavioural or behavioural issues
- helplessness
- strengths and difficulties questionnaire
- kindl
- hrqol
- whoqol
- General health questionnaire or GHQ
- health surveys
- Short Form-36 or SF-36
- executive function
- working memory
- reasoning
- task flexibility *
- problem solv *
- hyperactive *
- concentr *
- speech intelligibility *
- impair *
- standardised assess* or standardized assess *
- SATS/Sats
- reading
- reading comprehension
- oral comprehension
- memory
- attention
- learn impair *
Appendix A.2. Table A1
| Outcome | Reason for Exclusions |
|---|---|
| Mental Health | |
| 1. Dzhambov, A., Hartig, T., Markevych, I., Tilov, B., & Dimitrova, D. (2018). Urban residential greenspace and mental health in youth: Different approaches to testing multiple pathways yield different conclusions. Environmental Research, 160, 47-59. | Does not report association between noise exposure and mental health |
| 2. Gascon, M., Sanchez-Benavides, G., Dadvand, P., Martinez, D., Gramunt, N., Gotsens, X.,… Nieuwenhuijsen, M. (2018). Long-term exposure to residential green and blue spaces and anxiety and depression in adults: A cross-sectional study. Environmental Research, 162, 231-239. | Does not report association between noise exposure and mental health |
| 3. Xiao, J., Li, X., & Zhang, Z. (2016). DALY-Based Health Risk Assessment of Construction Noise in Beijing, China. International Journal of Environmental Research and Public Health, 13(11), doi:10.3390/ijerph13111045 | Does not directly measure noise |
| 4. Taskaya, S. (2018). Environmental quality and well-being level in Turkey. Environmental Science and Pollution Research International, 25(28), 27935-27944, doi:10.1007/s11356-018-2806-4 | Does not directly measure noise |
| 5. Ma, J., Li, C., Kwan, M. P., & Chai, Y. (2018). A Multilevel Analysis of Perceived Noise Pollution, Geographic Contexts and Mental Health in Beijing. International Journal of Environmental Research and Public Health, 15(7), doi:10.3390/ijerph15071479 | Does not directly measure noise |
| 6. Kamimura, A., Armenta, B., Nourian, M., Assasnik, N., Nourian, K., & Chernenko, A. (2017). Perceived Environmental Pollution and Its Impact on Health in China, Japan, and South Korea. Journal of Preventive Medicine and Public Health. Yebang Uihakhoe Chi, 50(3), 188-194, doi:10.3961/jpmph.17.044 | Does not directly measure noise |
| 7. Hammersen, F., Niemann, H., & Hoebel, J. (2016). Environmental Noise Annoyance and Mental Health in Adults: Findings from the Cross-Sectional German Health Update (GEDA) Study 2012. International Journal of Environmental Research and Public Health, 13(10), doi:10.3390/ijerph13100954 | Does not directly measure noise |
| 8. Dreger, S., Meyer, N., Fromme, H., & Bolte, G. (2015). Environmental noise and incident mental health problems: a prospective cohort study among school children in Germany. Environmental Research, 143, 49-54. | Does not directly measure noise |
| 9. Pun, V. C., Manjourides, J., & Suh, H. H. (2019). Close proximity to roadway and urbanicity associated with mental ill-health in older adults. Science of the Total Environment, 658, 854-860, doi:10.1016/j.scitotenv.2018.12.221 | Does not directly measure noise |
| 10. Skrzypek, M., Kowalska, M., Czech, E. M., Niewiadomska, E., & Zejda, J. E. (2017). Impact of road traffic noise on sleep disturbances and attention disorders amongst school children living in Upper Silesian Industrial Zone, Poland. International Journal of Occupational Medicine and Environmental Health, 30(3), 511-520, doi:10.13075/ijomeh.1896.00823 | Does not directly measure noise |
| Dementia and other neurodegenerative outcomes | |
| 1. Chen, H., Kwong, J. C., Copes, R., Hystad, P., van Donkelaar, A., Tu, K.,… Burnett, R. T. (2017). Exposure to ambient air pollution and the incidence of dementia: A population-based cohort study. Environment International, 108, 271-277. | Does not report association between noise exposure and mental health |
| 2. Chen, H., Kwong, J. C., Copes, R., Tu, K., Villeneuve, P. J., van Donkelaar, A.,… Burnett, R. T. (2017). Living near major roads and the incidence of dementia, Parkinson’s disease, and multiple sclerosis: a population-based cohort study. Lancet, 389(10070), 718-726. | Does not measure noise exposure: measures distance to road |
| Birth and fertility outcomes | |
| 1. Robinson, O., Tamayo, I., de Castro, M., Valentin, A., Giorgis-Allemand, L., Hjertager Krog, N.,… Basagana, X. (2018). The Urban Exposome during Pregnancy and Its Socioeconomic Determinants. Environmental Health Perspectives, 126(7), 077005. | Does not report a relevant health outcome |
| 2. He, S., Smargiassi, A., Low, N., Bilodeau-Bertrand, M., Ayoub, A., & Auger, N. (2019). Residential noise exposure and the longitudinal risk of hospitalization for depression after pregnancy: Postpartum and beyond. Environmental Research, 170, 26-32. | Does not report a relevant health outcome: moved to the mental health review. |
| 3. Nassan, F. L., Chavarro, J. E., Minguez-Alarcon, L., Williams, P. L., Tanrikut, C., Ford, J. B.,… Gaskins, A. J. (2018). Residential distance to major roadways and semen quality, sperm DNA integrity, chromosomal disomy, and serum reproductive hormones among men attending a fertility clinic. International Journal of Hygiene and Environmental Health, 221(5), 830-837. | Does not measure noise exposure: measures distance to road |
| Cancer | |
| 1. Hvidtfeldt, U. A., Sorensen, M., Geels, C., Ketzel, M., Khan, J., Tjonneland, A.,… Raaschou-Nielsen, O. (2019). Long-term residential exposure to PM2.5, PM10, black carbon, NO2, and ozone and mortality in a Danish cohort. Environment International, 123, 265-272. | Does not report a relevant health outcome |
| 2. James, P., Hart, J. E., Banay, R. F., & Laden, F. (2016). Exposure to Greenness and Mortality in a Nationwide Prospective Cohort Study of Women. Environmental Health Perspectives, 124(9), 1344-1352. | Does not report noise exposure |
| 3. Roswall, N., Andersen, Z. J., von Euler-Chelpin, M., Vejborg, I., Lynge, E., Jensen, S. S.,… Sorensen, M. (2018). Residential traffic noise and mammographic breast density in the Diet, Cancer, and Health cohort. Cancer Causes and Control, 29(4-5), 399-404, doi:10.1007/s10552-018-1021-4 | Does not report a relevant health outcome—reports a risk factor for breast cancer not cancer per se. |
| Cognition | |
| 1. Van Aart, C. J. C., Michels, N., Sioen, I., De Decker, A., Bijnens, E. M., Janssen, B. G.,… Nawrot, T. S. (2018). Residential landscape as a predictor of psychosocial stress in the life course from childhood to adolescence. Environment International, 120, 456-463. | Does not report a relevant cognitive outcome. Does report mental health but was already identified in the mental health review. |
| 2. Braat-Eggen, P. E., van Heijst, A., Hornikx, M., & Kohlrausch, A. (2017). Noise disturbance in open-plan study environments: a field study on noise sources, student tasks and room acoustic parameters. Ergonomics, 60(9), 1297-1314. | Experimental study |
| 3. Connolly, D., Dockrell, J., Shield, B., Conetta, R., Mydlarz, C., & Cox, T. (2019). The effects of classroom noise on the reading comprehension of adolescents. Journal of the Acoustical Society of America, 145(1), 372. | Experimental study |
| 4. Forns, J., Dadvand, P., Foraster, M., Alvarez-Pedrerol, M., Rivas, I., López-Vicente, M.,… Sunyer, J. (2016). Traffic-related air pollution, noise at school and behavioural problems in Barcelona schoolchildren: a cross-sectional study. Environmental Health Perspectives, 124(4), 529-535 | Does not report a relevant cognitive outcome. Moved to mental health review. |
| 5. Silva, L. T., Oliveria, I. S., & Silva, J. F. (2016). The impact of urban noise on primary schools. Perceptive evaluation and objective assessment. Applied Acoustics, 106, 2-9. | Does not report a relevant cognitive outcome. Reports attitudes to noise. |
| 6. Onchang, R., & Hawker, D. W. (2018). Community noise exposure and annoyance, activity interference, and academic achievement among university students. Noise Health, 20(94), 69-76. | Does not report on noise exposure and grade point average (reports on the association for noise annoyance) |
References
- Guski, R.; Schreckenberg, D.; Schuemer, R. WHO Environmental Noise Guidelines for the European Region: A systematic review on environmental noise and annoyance. Int. J. Environ. Res. Public Health 2017, 14, 1539. [Google Scholar] [CrossRef] [PubMed]
- Basner, M.; McGuire, S. WHO Environmental Noise Guidelines for the European Region: A Systematic Review on Environmental Noise and Effects on Sleep. Int. J. Environ. Res. Public Health 2018, 15, 519. [Google Scholar] [CrossRef] [PubMed]
- Kempen, E.V.; Casas, M.; Pershagen, G.; Foraster, M. WHO Environmental Noise Guidelines for the European Region: A Systematic Review on Environmental Noise and Cardiovascular and Metabolic Effects: A Summary. Int. J. Environ. Res. Public Health 2018, 15, 379. [Google Scholar] [CrossRef] [PubMed]
- Nieuwenhuijsen, M.J.; Ristovska, G.; Dadvand, P. WHO Environmental Noise Guidelines for the European Region: A systematic review on environmental noise and adverse birth outcomes. Int. J. Environ. Res. Public Health 2017, 14, 1252. [Google Scholar] [CrossRef]
- Clark, C.; Paunović, K. WHO Environmental Noise Guidelines for the European Region: A systematic review on environmental noise and cognition. Int. J. Environ. Res. Public Health 2018, 15, 285. [Google Scholar] [CrossRef]
- Clark, C.; Paunović, K. Systematic review of the evidence on the effects of environmental noise on quality of life, wellbeing and mental health. Int. J. Environ. Res. Public Health 2018, 15, 2400. [Google Scholar] [CrossRef]
- Department for Environment, Food and Rural Affairs. Environmental Noise: Valuing Impacts on: Sleep Disturbance, Annoyance, Hypertension, Productivity and Quiet; Department for Environment, Food and Rural Affairs: London, UK, 2014.
- Interdepartmental Group on Costs and Benefits (Noise) (IGCB(N)). Noise & Health—Valuing the Human Health Impacts of Environmental Noise Exposure; IGCB(N): London, UK, 2010.
- Department for Transport. TAG Unit A3 Environmental Impact Appraisal; Department for Transport: London, UK, 2015.
- HM Treasury. The Green Book. Central Government Guidance on Appraisal and Evaluation; HM Treasury: London, UK, 2018.
- WHO. The World Health Organization Guidelines for Environmental Noise Exposure for the European Region; World Health Organization Europe: Copenhagen, Denmark, 2018. [Google Scholar]
- Sorensen, M.; Ketzel, M.; Overvad, K.; Tjonneland, A.; Raaschou-Nielsen, O. Exposure to road traffic and railway noise and postmenopausal breast cancer: A cohort study. Int. J. Cancer 2014, 134, 2691–2698. [Google Scholar] [CrossRef]
- Roswall, N.; Bidstrup, P.E.; Raaschou-Nielsen, O.; Solvang Jensen, S.; Overvad, K.; Halkjaer, J.; Sorensen, M. Residential road traffic noise exposure and colorectal cancer survival—A Danish cohort study. PLoS ONE 2017, 12, e0187161. [Google Scholar] [CrossRef]
- Carey, I.M.; Anderson, H.R.; Atkinson, R.W.; Beevers, S.D.; Cook, D.G.; Strachan, D.P.; Dajnak, D.; Gulliver, J.; Kelly, F.J. Are noise and air pollution related to the incidence of dementia? A cohort study in London, England. BMJ Open 2018, 8, e022404. [Google Scholar] [CrossRef]
- Andersson, J.; Oudin, A.; Sundstrom, A.; Forsberg, B.; Adolfsson, R.; Nordin, M. Road traffic noise, air pollution, and risk of dementia—Results from the Betula project. Environ. Res. 2018, 166, 334–339. [Google Scholar] [CrossRef]
- Guyatt, G.H.; Oxman, A.D.; Vist, G.; Kunz, R.; Falck-Ytter, Y.; Alonso-Coello, P.; Schünemann, H.J. Rating quality of evidence and strength of recommendations GRADE: An emerging consensus on rating quality of evidence and strength of recommendations. Br. Med. J. 2008, 336, 924–926. [Google Scholar] [CrossRef] [PubMed]
- Cochrane Collaboration. Cochrane Handbook for Systematic Reviews of Interventions; Higgins, J.P.T., Green, S., Eds.; Cochrane Collaboration: Chichester, UK, 2011. [Google Scholar]
- WHO. WHO Handbook for Guideline Development; World Health Organization: Geneva, Switzerland, 2012. [Google Scholar]
- Weyde, K.V.; Krog, N.H.; Oftedal, B.; Magnus, P.; Overland, S.; Stansfeld, S.; Nieuwenhuijsen, M.J.; Vrijheid, M.; de Castro Pascual, M.; Aasvang, G.M. Road traffic noise and children’s inattention. Environ. Health 2017, 16, 127. [Google Scholar] [CrossRef] [PubMed]
- Skrzypek, M.; Kowalska, M.; Czech, E.M.; Niewiadomska, E.; Zejda, J.E. Impact of road traffic noise on sleep disturbances and attention disorders amongst school children living in Upper Silesian Industrial Zone, Poland. Int. J. Occup. Med. Environ. Health 2017, 30, 511–520. [Google Scholar] [CrossRef] [PubMed]
- Ma, J.; Li, C.; Kwan, M.P.; Chai, Y. A Multilevel Analysis of Perceived Noise Pollution, Geographic Contexts and Mental Health in Beijing. Int. J. Environ. Res. Public Health 2018, 15, 1479. [Google Scholar] [CrossRef]
- Feder, K.; Michaud, D.S.; Keith, S.E.; Voicescu, S.A.; Marro, L.; Than, J.; Guay, M.; Denning, A.; Bower, T.J.; Lavigne, E.; et al. An assessment of quality of life using the WHOQOL-BREF among participants living in the vicinity of wind turbines. Environ. Res. 2015, 142, 227–238. [Google Scholar] [CrossRef]
- Seidler, A.; Hegewald, J.; Seidler, A.L.; Schubert, M.; Wagner, M.; Droge, P.; Haufe, E.; Schmitt, J.; Swart, E.; Zeeb, H. Association between aircraft, road and railway traffic noise and depression in a large case-control study based on secondary data. Environ. Res. 2017, 152, 263–271. [Google Scholar] [CrossRef]
- Pun, V.C.; Manjourides, J.; Suh, H.H. Close proximity to roadway and urbanicity associated with mental ill-health in older adults. Sci. Total Environ. 2019, 658, 854–860. [Google Scholar] [CrossRef]
- Xiao, J.; Li, X.; Zhang, Z. DALY-Based Health Risk Assessment of Construction Noise in Beijing, China. Int. J. Environ. Res. Public Health 2016, 13, 1045. [Google Scholar] [CrossRef]
- Dreger, S.; Meyer, N.; Fromme, H.; Bolte, G. Environmental noise and incident mental health problems: A prospective cohort study among school children in Germany. Environ. Res. 2015, 143, 49–54. [Google Scholar] [CrossRef]
- Taskaya, S. Environmental quality and well-being level in Turkey. Environ. Sci. Pollut. Res. Int. 2018, 25, 27935–27944. [Google Scholar] [CrossRef]
- Welch, D.; Dirks, K.N.; Shepherd, D.; McBride, D. Health-related quality of life is impacted by proximity to an airport in noise-sensitive people. Noise Health 2018, 20, 171–177. [Google Scholar] [CrossRef] [PubMed]
- Gascon, M.; Sanchez-Benavides, G.; Dadvand, P.; Martinez, D.; Gramunt, N.; Gotsens, X.; Cirach, M.; Vert, C.; Molinuevo, J.L.; Crous-Bou, M.; et al. Long-term exposure to residential green and blue spaces and anxiety and depression in adults: A cross-sectional study. Environ. Res. 2018, 162, 231–239. [Google Scholar] [CrossRef] [PubMed]
- Dzhambov, A.M.; Markevych, I.; Tilov, B.; Arabadzhiev, Z.; Stoyanov, D.; Gatseva, P.; Dimitrova, D.D. Pathways linking residential noise and air pollution to mental ill-health in young adults. Environ. Res. 2018, 166, 458–465. [Google Scholar] [CrossRef] [PubMed]
- Dzhambov, A.M.; Markevych, I.; Hartig, T.; Tilov, B.; Arabadzhiev, Z.; Stoyanov, D.; Gatseva, P.; Dimitrova, D.D. Multiple pathways link urban green- and bluespace to mental health in young adults. Environ. Res. 2018, 166, 223–233. [Google Scholar] [CrossRef]
- Dzhambov, A.; Hartig, T.; Markevych, I.; Tilov, B.; Dimitrova, D. Urban residential greenspace and mental health in youth: Different approaches to testing multiple pathways yield different conclusions. Environ. Res. 2018, 160, 47–59. [Google Scholar] [CrossRef]
- Dzhambov, A.; Tilov, B.; Markevych, I.; Dimitrova, D. Residential road traffic noise and general mental health in youth: The role of noise annoyance, neighborhood restorative quality, physical activity, and social cohesion as potential mediators. Environ. Int. 2017, 109, 1–9. [Google Scholar] [CrossRef]
- Generaal, E.; Timmermans, E.J.; Dekkers, J.E.C.; Smit, J.H.; Penninx, B. Not urbanization level but socioeconomic, physical and social neighbourhood characteristics are associated with presence and severity of depressive and anxiety disorders. Psychol. Med. 2019, 49, 149–161. [Google Scholar] [CrossRef]
- Kamimura, A.; Armenta, B.; Nourian, M.; Assasnik, N.; Nourian, K.; Chernenko, A. Perceived Environmental Pollution and Its Impact on Health in China, Japan, and South Korea. J. Prev. Med. Public Health 2017, 50, 188–194. [Google Scholar] [CrossRef]
- Zock, J.P.; Verheij, R.; Helbich, M.; Volker, B.; Spreeuwenberg, P.; Strak, M.; Janssen, N.A.H.; Dijst, M.; Groenewegen, P. The impact of social capital, land use, air pollution and noise on individual morbidity in Dutch neighbourhoods. Environ. Int. 2018, 121, 453–460. [Google Scholar] [CrossRef]
- Hammersen, F.; Niemann, H.; Hoebel, J. Environmental Noise Annoyance and Mental Health in Adults: Findings from the Cross-Sectional German Health Update (GEDA) Study 2012. Int. J. Environ. Res. Public Health 2016, 13, 954. [Google Scholar] [CrossRef]
- Lim, J.; Kweon, K.; Kim, H.W.; Cho, S.W.; Park, J.; Sim, C.S. Negative impact of noise and noise sensitivity on mental health in childhood. Noise Health 2018, 20, 199–211. [Google Scholar] [CrossRef]
- Van Aart, C.J.C.; Michels, N.; Sioen, I.; De Decker, A.; Bijnens, E.M.; Janssen, B.G.; De Henauw, S.; Nawrot, T.S. Residential landscape as a predictor of psychosocial stress in the life course from childhood to adolescence. Environ. Int. 2018, 120, 456–463. [Google Scholar] [CrossRef]
- Klompmaker, J.O.; Hoek, G.; Bloemsma, L.D.; Wijga, A.H.; van den Brink, C.; Brunekreef, B.; Lebret, E.; Gehring, U.; Janssen, N.A.H. Associations of combined exposures to surrounding green, air pollution and traffic noise on mental health. Environ. Int. 2019, 129, 525–537. [Google Scholar] [CrossRef]
- Oiamo, T.H.; Luginaah, N.; Baxter, J. Cumulative efects of noise and odour annoyances on environmental and health related quality of life. Soc. Sci. Med. 2015, 146, 191–203. [Google Scholar] [CrossRef]
- Okokon, E.O.; Yli-Tuomi, T.; Turunen, A.W.; Tiittanen, P.; Juutilainen, J.; Lanki, T. Traffic noise, noise annoyance and psychotropic medication use. Environ. Int. 2018, 119, 287–294. [Google Scholar] [CrossRef]
- Leijssen, J.B.; Snijder, M.B.; Timmermans, E.J.; Generaal, E.; Stronks, K.; Kunst, A.E. The association between road traffic noise and depressed mood among different ethnic and socioeconomic groups. The HELIUS study. Int. J. Hyg. Environ. Health 2019, 222, 221–229. [Google Scholar] [CrossRef]
- Zijlema, W.L.; Morley, D.W.; Stolk, R.P.; Rosmalen, J.G. Noise and somatic symptoms: A role for personality traits? Int. J. Hyg. Environ. Health 2015, 218, 543–549. [Google Scholar] [CrossRef]
- Wallas, A.; Eriksson, C.; Gruzieva, O.; Lind, T.; Pyko, A.; Sjostrom, M.; Ogren, M.; Pershagen, G. Road traffic noise and determinants of saliva cortisol levels among adolescents. Int. J. Hyg. Environ. Health 2018, 221, 276–282. [Google Scholar] [CrossRef]
- Lawton, R.N.; Fujiwara, D. Living with aircraft noise: Airport proximity, aviation noise and subjective wellbeing in England. Transp. Res. Part D Transp. Environ. 2016, 42, 104–118. [Google Scholar] [CrossRef]
- Wright, D.M.; Newell, K.; Maguire, A.; O’Reilly, D. Aircraft noise and self-assessed mental health around a regional urban airport: A population based record linkage study. Environ. Health 2018, 17, 74. [Google Scholar] [CrossRef]
- Forns, J.; Dadvand, P.; Foraster, M.; Alvarez-Pedrerol, M.; Rivas, I.; López-Vicente, M.; Suades-Gonzalez, E.; Garcia-Esteban, R.; Esnaola, M.; Cirach, M.; et al. Traffic-related air pollution, noise at school and behavioural problems in Barcelona schoolchildren: A cross-sectional study. Environ. Health Perspect. 2016, 124, 529–535. [Google Scholar] [CrossRef]
- He, S.; Smargiassi, A.; Low, N.; Bilodeau-Bertrand, M.; Ayoub, A.; Auger, N. Residential noise exposure and the longitudinal risk of hospitalization for depression after pregnancy: Postpartum and beyond. Environ. Res. 2019, 170, 26–32. [Google Scholar] [CrossRef] [PubMed]
- Civil Aviation Authority. CAP1506 Survey of Noise Attitudes 2014; Civil Aviation Authority: London, UK, 2017.
- Klatte, M.; Spilski, J.; Mayerl, J.; Möhler, U.; Lachmann, T.; Bergström, K. Effects of aircraft noise on reading and quality of life in primary school children in Germany: Results from the NORAH study. Environ. Behav. 2016, 49, 390–424. [Google Scholar] [CrossRef]
- Zijlema, W.L.; De Kluizenaar, Y.; Van Kamp, I.; Hartman, C.A. Associations between Road Traffic Noise Exposure at Home and School and ADHD in School-Aged Children: The TRAILS Study. In Proceedings of the INTER-NOISE and NOISE-CON Congress and Conference Proceedings, Madrid, Spain, 30 September 2019. [Google Scholar]
- Goodman, R.J. The strengths and difficulties questionnaire. J. Child Psychol. Psych. 1997, 38, 581–586. [Google Scholar] [CrossRef] [PubMed]
- Dzhambov, A.; Lercher, P. Road traffic noise exposure and depression/anxiety: An updated systematic review and meta-analysis. Int. J. Environ. Res. Public Health 2019, 16, 4134. [Google Scholar] [CrossRef]
- Schubert, M.; Hegewald, J.; Freiberg, A.; Starke, K.R.; Augustin, F.; Riedel-Heller, S.G.; Zeeb, H.; Seidler, A. Behavioral and Emotional Disorders and Transportation Noise among Children and Adolescents: A Systematic Review and Meta-Analysis. Int. J. Environ. Res. Public Health 2019, 16, 3336. [Google Scholar] [CrossRef]
- Goodman, A.; Goodman, R. Strengths and difficulties questionnaire as a dimensional measure of child mental health. J. Am. Acad. Child Adolesc. Psychiatry 2009, 48, 400–403. [Google Scholar] [CrossRef]
- Clark, C.; Myron, R.; Stansfeld, S.; Candy, B. A systematic review of the evidence on the effect of the built and physical environment on mental health. J. Public Ment. Health 2007, 6, 14–27. [Google Scholar]
- Roswall, N.; Eriksen, K.T.; Hjortebjerg, D.; Jensen, S.S.; Overvad, K.; Tjonneland, A.; Raaschou-Nielsen, O.; Sorensen, M. Residential Exposure to Road and Railway Noise and Risk of Prostate Cancer: A Prospective Cohort Study. PLoS ONE 2015, 10, e0135407. [Google Scholar] [CrossRef]
- Roswall, N.; Bidstrup, P.E.; Raaschou-Nielsen, O.; Jensen, S.S.; Olsen, A.; Sorensen, M. Residential road traffic noise exposure and survival after breast cancer—A cohort study. Environ. Res. 2016, 151, 814–820. [Google Scholar] [CrossRef]
- Roswall, N.; Raaschou-Nielsen, O.; Ketzel, M.; Overvad, K.; Halkjær, J.; Sørensen, M. Modeled traffic noise at the residence and colorectal cancer incidence: A cohort study. Cancer Causes Control 2017, 28, 745–753. [Google Scholar] [CrossRef]
- Roswall, N.; Andersen, Z.J.; von Euler-Chelpin, M.; Vejborg, I.; Lynge, E.; Jensen, S.S.; Raaschou-Nielsen, O.; Tjonneland, A.; Sorensen, M. Residential traffic noise and mammographic breast density in the Diet, Cancer, and Health cohort. Cancer Causes Control 2018, 29, 399–404. [Google Scholar] [CrossRef]
- Andersen, Z.J.; Jorgensen, J.T.; Elsborg, L.; Lophaven, S.N.; Backalarz, C.; Laursen, J.E.; Pedersen, T.H.; Simonsen, M.K.; Brauner, E.V.; Lynge, E. Long-term exposure to road traffic noise and incidence of breast cancer: A cohort study. Breast Cancer Res. 2018, 20, 119. [Google Scholar] [CrossRef]
- Hegewald, J.; Schubert, M.; Wagner, M.; Droge, P.; Prote, U.; Swart, E.; Mohler, U.; Zeeb, H.; Seidler, A. Breast cancer and exposure to aircraft, road, and railway-noise: A case-control study based on health insurance records. Scand. J. Work. Environ. Health 2017, 43, 509–518. [Google Scholar] [CrossRef]
- Sorensen, M.; Harbo Poulsen, A.; Ketzel, M.; Oksbjerg Dalton, S.; Friis, S.; Raaschou-Nielsen, O. Residential exposure to traffic noise and risk for non-hodgkin lymphoma among adults. Environ. Res. 2015, 142, 61–65. [Google Scholar] [CrossRef]
- Hvidtfeldt, U.A.; Sorensen, M.; Geels, C.; Ketzel, M.; Khan, J.; Tjonneland, A.; Overvad, K.; Brandt, J.; Raaschou-Nielsen, O. Long-term residential exposure to PM2.5, PM10, black carbon, NO2, and ozone and mortality in a Danish cohort. Environ. Int. 2019, 123, 265–272. [Google Scholar] [CrossRef]
- James, P.; Hart, J.E.; Banay, R.F.; Laden, F. Exposure to Greenness and Mortality in a Nationwide Prospective Cohort Study of Women. Environ. Health Perspect. 2016, 124, 1344–1352. [Google Scholar] [CrossRef]
- Tzivian, L.; Dlugaj, M.; Winkler, A.; Hennig, F.; Fuks, K.; Sugiri, D.; Schikowski, T.; Jakobs, H.; Erbel, R.; Jöckel, K.H.; et al. Long-term air pollution and traffic noise exposures and cognitive function:A cross-sectional analysis of the Heinz Nixdorf Recall study. J. Toxicol. Environ. Health Part A 2016, 79, 1057–1069. [Google Scholar] [CrossRef]
- Linares, C.; Culqui, D.; Carmona, R.; Ortiz, C.; Diaz, J. Short-term association between environmental factors and hospital admissions due to dementia in Madrid. Environ. Res. 2017, 152, 214–220. [Google Scholar] [CrossRef]
- Culqui, D.R.; Linares, C.; Ortiz, C.; Carmona, R.; Diaz, J. Association between environmental factors and emergency hospital admissions due to Alzheimer’s disease in Madrid. Sci. Total Environ. 2017, 592, 451–457. [Google Scholar] [CrossRef]
- Chen, H.; Kwong, J.C.; Copes, R.; Tu, K.; Villeneuve, P.J.; van Donkelaar, A.; Hystad, P.; Martin, R.V.; Murray, B.J.; Jessiman, B.; et al. Living near major roads and the incidence of dementia, Parkinson’s disease, and multiple sclerosis: A population-based cohort study. Lancet 2017, 389, 718–726. [Google Scholar] [CrossRef]
- Chen, H.; Kwong, J.C.; Copes, R.; Hystad, P.; van Donkelaar, A.; Tu, K.; Brook, J.R.; Goldberg, M.S.; Martin, R.V.; Murray, B.J.; et al. Exposure to ambient air pollution and the incidence of dementia: A population-based cohort study. Environ. Int. 2017, 108, 271–277. [Google Scholar] [CrossRef]
- Diaz, J.; Martinez-Martin, P.; Rodriguez-Blazquez, C.; Vazquez, B.; Forjaz, M.J.; Ortiz, C.; Carmona, R.; Linares, C. Short-term association between road traffic noise and healthcare demand generated by Parkinson’s disease in Madrid, Spain. Gac. Sanit. 2018, 32, 553–558. [Google Scholar] [CrossRef]
- Carmona, R.; Linares, C.; Recio, A.; Ortiz, C.; Diaz, J. Emergency multiple sclerosis hospital admissions attributable to chemical and acoustic pollution: Madrid (Spain), 2001–2009. Sci. Total Environ. 2018, 612, 111–118. [Google Scholar] [CrossRef]
- Smith, R.B.; Fecht, D.; Gulliver, J.; Beevers, S.D.; Dajnak, D.; Blangiardo, M.; Ghosh, R.E.; Hansell, A.L.; Kelly, F.J.; Anderson, H.R.; et al. Impact of London’s road traffic air and noise pollution on birth weight: Retrospective population based cohort study. BMJ 2017, 359, j5299. [Google Scholar] [CrossRef]
- Wallas, A.; Ekstrom, S.; Bergstrom, A.; Eriksson, C.; Gruzieva, O.; Sjostrom, M.; Pyko, A.; Ogren, M.; Bottai, M.; Pershagen, G. Traffic noise exposure in relation to adverse birth outcomes and body mass between birth and adolescence. Environ. Res. 2019, 169, 362–367. [Google Scholar] [CrossRef]
- Pedersen, M.; Garne, E.; Hansen-Nord, N.; Hjortebjerg, D.; Ketzel, M.; Raaschou-Nielsen, O.; Nybo Andersen, A.M.; Sorensen, M. Exposure to air pollution and noise from road traffic and risk of congenital anomalies in the Danish National Birth Cohort. Environ. Res. 2017, 159, 39–45. [Google Scholar] [CrossRef]
- Hjortebjerg, D.; Nybo Andersen, A.M.; Ketzel, M.; Raaschou-Nielsen, O.; Sorensen, M. Exposure to traffic noise and air pollution and risk for febrile seizure: A cohort study. Scand. J. Work Environ. Health 2018, 44, 539–546. [Google Scholar] [CrossRef]
- Min, K.B.; Min, J.Y. Exposure to environmental noise and risk for male infertility: A population-based cohort study. Environ. Pollut. 2017, 226, 118–124. [Google Scholar] [CrossRef]
- Robinson, O.; Tamayo, I.; de Castro, M.; Valentin, A.; Giorgis-Allemand, L.; Hjertager Krog, N.; Marit Aasvang, G.; Ambros, A.; Ballester, F.; Bird, P.; et al. The Urban Exposome during Pregnancy and Its Socioeconomic Determinants. Environ. Health Perspect. 2018, 126, 077005. [Google Scholar] [CrossRef]
- Nassan, F.L.; Chavarro, J.E.; Minguez-Alarcon, L.; Williams, P.L.; Tanrikut, C.; Ford, J.B.; Dadd, R.; Perry, M.J.; Hauser, R.; Gaskins, A.J. Residential distance to major roadways and semen quality, sperm DNA integrity, chromosomal disomy, and serum reproductive hormones among men attending a fertility clinic. Int. J. Hyg. Environ. Health 2018, 221, 830–837. [Google Scholar] [CrossRef]
- Dzhambov, A.M.; Markevych, I.; Lercher, P. Associations of residential greenness, traffic noise, and air pollution with birth outcomes across Alpine areas. Sci. Total Environ. 2019, 678, 399–408. [Google Scholar] [CrossRef]
- Poulsen, A.H.; Raaschou-Nielsen, O.; Pena, A.; Hahmann, A.N.; Nordsborg, R.B.; Ketzel, M.; Brandt, J.; Sorensen, M. Pregnancy exposure to wind turbine noise and adverse birth outcomes: A nationwide cohort study. Environ. Res. 2018, 167, 770–775. [Google Scholar] [CrossRef]
- Dzhambov, A.; Lercher, P. Road traffic noise exposure and birth outcomes: An updated systematic review and meta-analysis. Int. J. Environ. Res. Public Health 2019, 16, 2522. [Google Scholar] [CrossRef]
- Connolly, D.; Dockrell, J.; Shield, B.; Conetta, R.; Mydlarz, C.; Cox, T. The effects of classroom noise on the reading comprehension of adolescents. J. Acoust. Soc. Am. 2019, 145, 372. [Google Scholar] [CrossRef]
- Braat-Eggen, P.E.; van Heijst, A.; Hornikx, M.; Kohlrausch, A. Noise disturbance in open-plan study environments: A field study on noise sources, student tasks and room acoustic parameters. Ergonomics 2017, 60, 1297–1314. [Google Scholar] [CrossRef]
- Tzivian, L.; Dlugaj, M.; Winkler, A.; Weinmayr, G.; Hennig, F.; Fuks, K.B.; Vossoughi, M.; Schikowski, T.; Weimar, C.; Erbel, R.; et al. Long-Term Air Pollution and Traffic Noise Exposures and Mild Cognitive Impairment in Older Adults: A Cross-Sectional Analysis of the Heinz Nixdorf Recall Study. Environ. Health Perspect. 2016, 124, 1361–1368. [Google Scholar] [CrossRef]
- Papanikolaou, M.; Skenteris, N.; Piperakis, S.M. Effect of external classroom noise on schoolchildren’s reading and mathematics performance: Correlation of noise levels and gender. Int. J. Adolesc. Med. Health 2015, 27, 25–29. [Google Scholar] [CrossRef]
- Tzivian, L.; Jokisch, M.; Winkler, A.; Weimar, C.; Hennig, F.; Sugiri, D.; Soppa, V.J.; Dragano, N.; Erbel, R.; Jockel, K.H.; et al. Associations of long-term exposure to air pollution and road traffic noise with cognitive function-An analysis of effect measure modification. Environ. Int. 2017, 103, 30–38. [Google Scholar] [CrossRef]
- Onchang, R.; Hawker, D.W. Community noise exposure and annoyance, activity interference, and academic achievement among university students. Noise Health 2018, 20, 69–76. [Google Scholar] [CrossRef]
- Silva, L.T.; Oliveria, I.S.; Silva, J.F. The impact of urban noise on primary schools. Perceptive evaluation and objective assessment. Appl. Acoust. 2016, 106, 2–9. [Google Scholar] [CrossRef]
- Spilski, J.; Mayerl, J.; Bergstrom, K.; Mohler, U. Aircraft Noise Exposure and Children’s Cognition: Evidence for a Daytime NAT Criterion. In Proceedings of the INTER-NOISE and NOISE-CON Congress and Conference Proceedings, Hong Kong, China, 7 December 2017. [Google Scholar]
- Spilski, J.; Bergstrom, K.; Mayerl, J.; Mohler, U.; Lachmann, T.; Klatte, M. The Relationship between Aircraft Noise and Reading: Mediator and Moderator Effects. In Proceedings of the 12th ICBEN Congress on Noise as a Public Health Problem, Zurich, Switzerland, 18–22 June 2017. [Google Scholar]
- Foraster, M.; Esnaola, M.; Garcia-Esteban, R.; Lopez-Vicente, M.; Rivas, I.; Sunyer, J. Exposure to Road Traffic Noise and Cognitive Trajectories in School Children. In Proceedings of the INTER-NOISE and NOISE-CON Congress and Conference Proceedings, Madrid, Spain, 30 Septmeber 2019. [Google Scholar]
- Eagan, M.E.; Nicholas, B.; McIntosh, S.; Clark, C.; Evans, G. Assessing Aircraft Noise Conditions Affecting Student Learning—Case Studies; The National Academies Press: Washington, DC, USA, 2017. [Google Scholar]
- Seabi, J.; Cockcroft, K.; Goldschagg, P.; Greyling, M. A prospective follow-up study of the effects of chronic aircraft noise exposure on learners’ reading comprehension in South Africa. J. Expo. Sci. Environ. Epidemiol. 2015, 25, 84–88. [Google Scholar] [CrossRef] [PubMed]
- Clark, C.; Martin, R.; van Kempen, E.; Alfred, T.; Head, J.; Davies, H.W.; Haines, M.M.; Barrio, I.L.; Matheson, M.; Stansfeld, S.A. Exposure-effect relations between aircraft and road traffic noise exposure at school and reading comprehension—The RANCH project. Am. J. Epidemiol. 2006, 163, 27–37. [Google Scholar] [CrossRef] [PubMed]
- Natalwala, A.; Potluri, R.; Uppal, H.; Heun, R. Reasons for hospital admissions in dementia patients in Birmingham, UK, during 2002–2007. Dement. Geriatr. Cogn. Disord. 2008, 26, 499–505. [Google Scholar] [CrossRef] [PubMed]

| WP2: Health Outcome | Temporal Scope of Review |
|---|---|
| Cognition | June 2015 to March 2019 |
| Dementia and other neurodegenerative diseases | January 2014 to March 2019 |
| Mental health, quality of life, and wellbeing | October 2015 to March 2019 |
| Birth and reproductive outcomes | January 2017 to March 2019 |
| Cancer | January 2014 to March 2019 |
| Reference | Bias due Exposure Assessment | Bias due to Confounding | Bias due to Selection of Participants | Bias due to Health Outcome Assessment | Bias due to Not Blinded Outcome Assessment | Total Risk of Bias |
|---|---|---|---|---|---|---|
| Weyde, Envt Health, 2017 | Low | Low | High | Unclear | Low | High |
| Feder et al., Environ Res, 2015 | Low | Low | Low | Low | Low | Low |
| Seidler et al., Environ Res, 2017 | Unclear | Low | Low | Low | Low | Unclear |
| Welch et al., Noise Health, 2018 | Low | Unclear | Low | Low | Low | Unclear |
| Klatte et al., Environ & Behavior, 2016 | Low | Low | Low | Low | Low | Low |
| Dzhambov et al., Environ Res, 2018a | Low | Low | Unclear | Low | Low | Unclear |
| Generaal et al., Psychol Med, 2019 | Low | Low | High | Low | Low | Unclear |
| Dzhambov et al., Environ Res, 2018b | Low | Low | Unclear | Low | Low | Unclear |
| Dzhambov et al., Environ Int., 2017 | Low | Low | Unclear | Low | Low | Unclear |
| Zock et al., Environ Int., 2018 | Low | Low | Low | Low | Low | Low |
| Lim et al., Noise Health, 2018 | Low | Low | High | Low | Low | Unclear |
| Forns et al., Enviro Health Perspectives, 2016 | Low | Low | Low | Low | Low | Low |
| He et al., Environ Res., 2019 | Low | Low | Unclear | Low | Low | Unclear |
| Civil Aviation Authority, 2017 | Low | High | Low | Low | Low | Unclear |
| Van Aart et al., Environ Int., 2018 | Low | Low | High | Low | Low | Unclear |
| Klompmaker et al., Environ Int., 2019 | Low | Low | Unclear | Low | Low | Unclear |
| Okokon et al., Environ Int., 2018 | Low | Low | Unclear | Low | Low | Unclear |
| Oiamo et al., Soc Sci Med., 2015 | Low | High | Unclear | Low | Low | Unclear |
| Leijssen et al., IJERPH, 2019 | Low | Low | Low | Low | Low | Low |
| Zijlema et al., Int. J Hygiene E Health., 2015 | Low | Low | Unclear | Low | Low | Unclear |
| Wallas et al., Int. J Hygiene E Health., 2018 | Low | Unclear | High | Low | Low | Unclear |
| Lawton et al., Transport Res Part D., 2016 | Low | Low | Low | Low | Low | Low |
| Wright et al., Environ Health., 2018 | Low | Low | Low | Low | Low | Low |
| Zijlema et al., Internoise., 2019 | Low | Low | Unclear | Low | Low | Unclear |
| Reference | Bias due Exposure Assessment | Bias due to Confounding | Bias due to Selection of Participants | Bias due to Health Outcome Assessment | Bias due to Not Blinded Outcome Assessment | Total Risk of Bias |
|---|---|---|---|---|---|---|
| Andersen et al., Lynge Breast Cancer Res., 2018 | Low | Low | Low | Low | Low | Low |
| Hegewald et al., Scandinavian J Work Envt Health, 2017 | Low | Low | Low | Low | Low | Low |
| Roswall et al., Environ Research, 2016 | Low | Low | Low | Low | Low | Low |
| Roswall, et al., Cancer, Causes & Control, 2017 | Low | Low | Low | Low | Low | Low |
| Roswall et al., PloS One, 2015 | Low | Low | Low | Low | Low | Low |
| Roswall et al., PloS One, 2017 | Low | Low | Low | Low | Low | Low |
| Sorensen et al., I J of Cancer, 2014 | Low | Low | Low | Low | Low | Low |
| Sorensen et al., Environmental Research, 2015 | Low | Low | Low | Low | Low | Low |
| Reference | Bias due Exposure Assessment | Bias due to Confounding | Bias due to Selection of Participants | Bias due to Health Outcome Assessment | Bias due to Not Blinded Outcome Assessment | Total Risk of Bias |
|---|---|---|---|---|---|---|
| Andersson et al., Environmental Research, 2018 | Low | Low | Unclear | Low | Low | Unclear |
| Carey et al., BMJ Open, 2018 | Low | Low | Low | Low | Low | Low |
| Culqui et al., Science of Total Environment, 2017 | Low | High | Low | Low | Low | Unclear |
| Linares et al., Environ Res., 2017 | Low | High | Low | Low | Low | Unclear |
| Tzivian et al., Environmental Health Perspectives, 2016 | Low | Low | Unclear | Low | Low | Unclear |
| Diaz et al., Gac Sanit, 2018 | Low | High | Low | Low | Low | Unclear |
| Carmona et al., Science of Total Environment, 2017 | Low | High | Low | Low | Low | Unclear |
| Reference | Bias due Exposure Assessment | Bias due to Confounding | Bias due to Selection of Participants | Bias due to Health Outcome Assessment | Bias due to Not Blinded Outcome Assessment | Total Risk of Bias |
|---|---|---|---|---|---|---|
| Hjortebjerg et al., Scand J Work Environ Health, 2018 | Low | Low | Low | Low | Low | Low |
| Min & Min, Environ Pollut., 2017 | Low | Low | Low | Low | Low | Low |
| Pedersen et al., Environ Res., 2017 | Low | Low | Low | Low | Low | Low |
| Smith et al., BMJ, 2017 | Low | Low | Low | Low | Low | Low |
| Wallas et al., Environ Res., 2019 | Low | Low | Low | Low | Low | Low |
| Poulsen et al., Environ Res., 2018 | Low | Low | Low | Low | Low | Low |
| Dzhamov et al., Sci Tot Envt., 2019 | Low | Low | Low | Low | Low | Low |
| Reference | Bias due Exposure Assessment | Bias due to Confounding | Bias due to Selection of Participants | Bias due to Health Outcome Assessment | Bias due to Not Blinded Outcome Assessment | Total Risk of Bias |
|---|---|---|---|---|---|---|
| Papanikolaou et al., Int J Adolesc Med Health, 2015 | Unclear | High | Unclear | Low | Low | High |
| Seabi et al., J Expo Sci Environ Epidemiol., 2015 | Low | Low | High | Low | Low | Unclear |
| Tzivian et al., Environ Health Perspectives, 2016 | Low | Low | Low | Low | Low | Low |
| Tzivian et al., J Toxicol Environ Health A, 2017 | Low | Low | Low | Low | Low | Low |
| Klatte et al., Environ & Behavior, 2016 | Low | Low | Low | Low | Low | Low |
| Spilski et al., ICBEN, 2017 | Low | Low | Low | Low | Low | Low |
| Spilski et al., Internoise, 2017 | Low | Low | Low | Low | Low | Low |
| Eagen et al., Transport Research Board, 2017 | Low | High | High | High | Unclear | High |
| Foraster et al., Internoise, 2017 | Low | Low | Unclear | Low | Low | Unclear |
| Mental Health, Wellbeing and Quality of Life | Environmental Noise Exposure | |||
|---|---|---|---|---|
| Domain | Aircraft Noise: Quality of Evidence and Assessment of Effect | Road Traffic Noise: Quality of Evidence and Assessment of Effect | Railway Noise: Quality of Evidence and Assessment of Effect | Wind Turbine Noise: Quality of Evidence and Assessment of Effect |
| Self-reported quality of life or health | Very low quality—no effect (4) | n.a. | n.a. | Very low quality—no effect (1) |
| Self-reported depression, anxiety, and psychological symptoms | n.a. | Very low quality—no effect (7) | Very low quality—no effect (1) | n.a. |
| Interview measures of depressive and anxiety disorders | Low quality—harmful effect (2) | Low quality—harmful effect (4) | Low quality—harmful effect (3) | n.a. |
| Wellbeing | Very low quality—harmful effect (3) | n.a. | n.a. | n.a. |
| Emotional and conduct symptoms in children | n.a. | Low quality—harmful effect (3) | n.a. | n.a. |
| Hyperactivity | n.a. | Low quality—harmful effect (3) | n.a. | n.a. |
| Cortisol in children | n.a. | Very low quality—harmful effect (1) | n.a. | n.a. |
| Medication intake for the treatment of anxiety and depression | n.a. | Very low quality—harmful effect (2) | Very low quality—harmful effect (1) | n.a. |
| ADHD in children | n.a. | Very low quality—no effect (1) | n.a. | n.a. |
| Cancer | Environmental Noise Exposure | |||
|---|---|---|---|---|
| Domain | Aircraft Noise: Quality of Evidence and Assessment of Effect | Road Traffic Noise: Quality of Evidence and Assessment of Effect | Railway Noise: Quality of Evidence and Assessment of Effect | Wind Turbine Noise: Quality of Evidence and Assessment of Effect |
| Cancer mortality | n.a. | High quality—no effect (2) | n.a. | n.a. |
| Incidence of breast cancer | Low quality—harmful effect (1) | Low quality—harmful effect (3) | Low quality—harmful effect (2) | n.a. |
| Incidence of colorectal cancer | n.a. | Low quality—harmful effect (1) | Low quality—no effect (1) | n.a. |
| Incidence of prostate cancer | n.a. | Low quality—no effect (1) | Low quality—no effect (1) | n.a. |
| Incidence of non-Hodgkin lymphoma | n.a. | Low quality—harmful effect (1) | n.a. | n.a. |
| Dementia and Other Neurodegenerative Outcomes | Environmental Noise Exposure |
|---|---|
| Domain | Road Traffic Noise: Quality of Evidence and Assessment of Effect |
| Incidence of vascular dementia | Low quality—no effect (2) |
| Dementia related emergency admissions | Very low quality—harmful effect (2) |
| Cognitive assessment of dementia symptoms | Very low quality—harmful effect (1) |
| Multiple sclerosis related emergency admissions | Very low quality—harmful effect (1) |
| Parkinson’s Disease emergency admissions | Very low quality—harmful effect (1) |
| Parkinson’s Disease healthcare | Very low quality—harmful effect (1) |
| n.a. no studies available to evaluate (n) number of papers evaluated |
| Birth and Reproductive Outcomes | Environmental Noise Exposure | |||
|---|---|---|---|---|
| Domain | Aircraft Noise Quality of Evidence and Assessment of Effect | Road Traffic Noise Quality of Evidence and Assessment of Effect | Railway Noise Quality of Evidence and Assessment of Effect | Wind Turbine Noise Quality of Evidence and Assessment of Effect |
| Low birth weight | n.a. | High quality—no effect (3) | Very low quality—no effect (1) | Moderate quality—no effect (1) |
| Pre-term birth | n.a. | Moderate quality—no effect (1) | n.a. | Moderate quality—no effect (1) |
| Small for gestational age | n.a. | Moderate quality—no effect (2) | Very low quality—no effect (1) | Moderate quality—no effect (1) |
| Congenital abnormalities | n.a. | Low quality—no effect (1) | n.a. | n.a. |
| Febrile seizures | n.a. | Low quality—harmful effect (1) | n.a. | n.a. |
| Male fertility | n.a. | Low quality—harmful effect (1) | n.a. | n.a. |
| Cognition | Environmental Noise Exposure | |||
|---|---|---|---|---|
| Domain | Aircraft Noise: Quality of Evidence and Assessment of Effect | Road Traffic Noise: Quality of Evidence and Assessment of Effect | Railway Noise: Quality of Evidence and Assessment of Effect | Wind Turbine Noise: Quality of Evidence and Assessment of Effect |
| Reading comprehension | Very low quality—harmful effect (4) | Very low quality—harmful effect (1) | n.a. | n.a. |
| Mathematics | n.a. | Very low quality—harmful effect (1) | n.a. | n.a. |
| Working memory | n.a. | Low quality—harmful effect (1) | n.a. | n.a. |
| Attention | n.a. | Low quality—harmful effect (1) | n.a. | n.a. |
| Student distraction | Very low quality—harmful effect (1) | n.a. | n.a. | n.a. |
| Assessment of adult cognition | n.a. | Very low quality—harmful effect (2) | n.a. | n.a. |
| Outcome | WHO Clark & Paunovic 2018 | Current Review |
|---|---|---|
| Aircraft noise | ||
| Self-reported quality of life or health | Very low quality—no effect | Very low quality—no effect (A similar assessment of very low quality evidence for no effect of wind turbine noise on self-reported quality of life or health was also found in the current review. This was not found in the WHO review.) |
| Medication intake for treatment of anxiety and depression | Very low quality—harmful effect | n.a. |
| Self-reported depression, anxiety and psychological symptoms | n.a. | n.a. |
| Interview measures of depressive and anxiety disorders | Very low quality—harmful effect | Low quality—harmful effect |
| Emotional and conduct disorders in children | Low quality—no effect | n.a. |
| Hyperactivity | Low quality—harmful effect | n.a. |
| Wellbeing | Not evaluated in the review | Very low quality—harmful effect |
| Road noise | ||
| Self-reported quality of life or health | Low quality—no effect | n.a. |
| Medication intake for treatment of anxiety and depression | Very low quality—no effect | Very low quality—harmful effect |
| Self-reported depression, anxiety and psychological symptoms | Very low quality—no effect | Very low quality—no effect |
| Interview measures of depressive and anxiety disorders | Very low quality—no effect | Low quality—harmful effect |
| Emotional and conduct disorders in children | Moderate quality—harmful effect | Low quality—harmful effect |
| Hyperactivity in children | Moderate quality—harmful effect | Low quality—harmful effect |
| Cortisol in children | n.a. | Very low quality—harmful effect |
| Wellbeing | Not included in this review | n.a. |
| ADHD in children | Not included in this review | Very low quality—no effect |
| Railway noise | ||
| Self-reported quality of life or health | Low—harmful effect | n.a. |
| Medication intake for treatment of anxiety and depression | n.a. | Very low quality—harmful effect |
| Self-reported depression, anxiety and psychological symptoms | n.a. | Very low quality—no effect |
| Interview measures of depressive and anxiety disorders | n.a. | Low quality—harmful effect |
| Emotional and conduct disorders in children | Moderate quality—harmful effect | n.a. |
| Hyperactivity | Moderate quality—no effect | n.a. |
| Wellbeing | n.a. | n.a. |
| Outcome | WHO Clark and Paunovic 2018 | Current Review |
|---|---|---|
| Aircraft noise | ||
| Low birth weight | Very low quality—no effect | n.a. |
| Pre-term birth | Very low quality—no effect | n.a. |
| Small for gestational age | n.a. | n.a. |
| Cognitive abnormalities | Very low quality—no effect | n.a. |
| Febrile seizures | n.a. | n.a. |
| Male infertility | n.a. | n.a. |
| Road noise | ||
| Low birth weight | Low quality—no effect | High quality—no effect |
| Pre-term birth | Low birth weight | Moderate quality—no effect |
| Small for gestational age | Low birth weight | Moderate quality—no effect |
| Cognitive abnormalities | n.a. | Low quality—no effect |
| Febrile seizures | n.a. | Low quality—harmful effect |
| Male infertility | n.a. | Low quality—harmful effect |
| Railway noise | ||
| Low birth weight | n.a. | Very low quality—no effect |
| Pre-term birth | n.a. | n.a. |
| Small for gestational age | n.a. | Very low quality—no effect |
| Cognitive abnormalities | n.a. | n.a. |
| Febrile seizures | n.a. | n.a. |
| Male infertility | n.a. | n.a. |
| Outcome | WHO Clark and Paunovic 2018 | Current Review |
|---|---|---|
| Aircraft noise | ||
| Reading comprehension | Moderate quality—harmful effect | Very low quality—harmful effect |
| Mathematics | n.a. | n.a. |
| Working memory | Very low quality—no effect | n.a. |
| Attention | Low quality—no effect | n.a. |
| Student distraction | n.a. | Very low quality—harmful effect |
| Assessment of adult cognition | n.a. | n.a. |
| Standardized assessment tests | Moderate quality—harmful effect | n.a. |
| Long-term and short-term memory | Moderate quality—harmful effect | n.a. |
| Road noise | ||
| Reading comprehension | Very low quality—no effect | Very low quality—harmful effect |
| Mathematics | n.a. | Very low quality—harmful effect |
| Working memory | Low quality—no effect | Low quality—harmful effect |
| Attention | Very low quality- no effect | Low quality—harmful effect |
| Student distraction | n.a. | n.a. |
| Assessment of adult cognition | n.a. | Very low quality—harmful effect |
| Standardized assessment tests | Very low quality- harmful effect | n.a. |
| Long-term and short-term memory | Very low quality- harmful effect | n.a. |
| Railway noise | ||
| Reading comprehension | n.a. | n.a. |
| Mathematics | n.a. | n.a. |
| Working memory | n.a. | n.a. |
| Attention | Very low quality—no effect | n.a. |
| Student distraction | n.a. | n.a. |
| Assessment of adult cognition | n.a. | n.a. |
| Standardized assessment tests | Moderate quality—harmful effect | n.a. |
| Long-term and short-term memory | Very low quality—harmful effect | n.a. |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Clark, C.; Crumpler, C.; Notley, H. Evidence for Environmental Noise Effects on Health for the United Kingdom Policy Context: A Systematic Review of the Effects of Environmental Noise on Mental Health, Wellbeing, Quality of Life, Cancer, Dementia, Birth, Reproductive Outcomes, and Cognition. Int. J. Environ. Res. Public Health 2020, 17, 393. https://doi.org/10.3390/ijerph17020393
Clark C, Crumpler C, Notley H. Evidence for Environmental Noise Effects on Health for the United Kingdom Policy Context: A Systematic Review of the Effects of Environmental Noise on Mental Health, Wellbeing, Quality of Life, Cancer, Dementia, Birth, Reproductive Outcomes, and Cognition. International Journal of Environmental Research and Public Health. 2020; 17(2):393. https://doi.org/10.3390/ijerph17020393
Chicago/Turabian StyleClark, Charlotte, Clare Crumpler, and Hilary Notley. 2020. "Evidence for Environmental Noise Effects on Health for the United Kingdom Policy Context: A Systematic Review of the Effects of Environmental Noise on Mental Health, Wellbeing, Quality of Life, Cancer, Dementia, Birth, Reproductive Outcomes, and Cognition" International Journal of Environmental Research and Public Health 17, no. 2: 393. https://doi.org/10.3390/ijerph17020393
APA StyleClark, C., Crumpler, C., & Notley, H. (2020). Evidence for Environmental Noise Effects on Health for the United Kingdom Policy Context: A Systematic Review of the Effects of Environmental Noise on Mental Health, Wellbeing, Quality of Life, Cancer, Dementia, Birth, Reproductive Outcomes, and Cognition. International Journal of Environmental Research and Public Health, 17(2), 393. https://doi.org/10.3390/ijerph17020393




