Evaluation of the Mitragynine Content, Levels of Toxic Metals and the Presence of Microbes in Kratom Products Purchased in the Western Suburbs of Chicago
Abstract
1. Introduction
2. Materials and Methods
2.1. Source of Products
2.2. Microbiological Testing
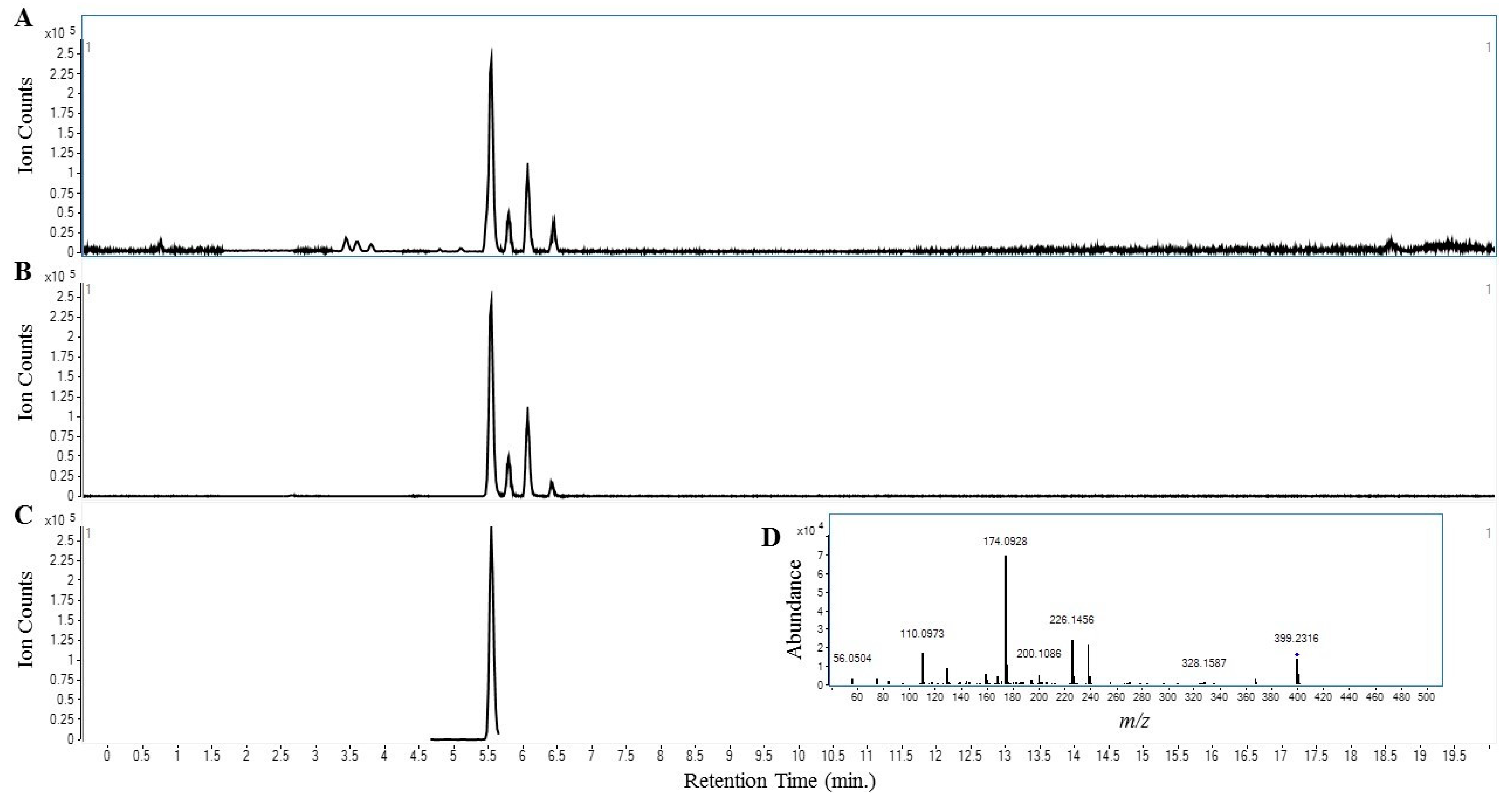
2.3. Mitragynine Analysis
2.4. Metal Analyses
3. Results
4. Discussion
5. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Adkins, J.E.; Boyer, E.W.; McCurdy, C.R. Mitragyna speciosa, a psychoactive tree from Southeast Asia with opioid activity. Curr. Top. Med. Chem. 2011, 11, 1165–1175. [Google Scholar] [CrossRef] [PubMed]
- Brown, P.N.; Lund, J.A.; Murch, S.J. A botanical, phytochemical and ethnomedicinal review of the genus Mitragyna korth: Implications for products sold as kratom. J. Ethnopharmacol. 2017, 202, 302–325. [Google Scholar] [CrossRef] [PubMed]
- Jansen, K.L.; Prast, C.J. Ethnopharmacology of kratom and the Mitragyna alkaloids. J. Ethnopharmacol. 1988, 23, 115–119. [Google Scholar] [CrossRef]
- Cinosi, E.; Martinotti, G.; Simonato, P.; Singh, D.; Demetrovics, Z.; Roman-Urrestarazu, A.; Bersani, F.S.; Vicknasingam, B.; Piazzon, G.; Li, J.H.; et al. Following “the Roots” of Kratom (Mitragyna speciosa): The Evolution of an Enhancer from a Traditional Use to Increase Work and Productivity in Southeast Asia to a Recreational Psychoactive Drug in Western Countries. Biomed. Res. Int. 2015, 2015, 968786. [Google Scholar] [CrossRef] [PubMed]
- Singh, D.; Narayanan, S.; Vicknasingam, B. Traditional and non-traditional uses of Mitragynine (Kratom): A survey of the literature. Brain Res. Bull. 2016, 126, 41–46. [Google Scholar] [CrossRef]
- Vicknasingam, B.; Narayanan, S.; Beng, G.T.; Mansor, S.M. The informal use of kratom (Mitragyna speciosa) for opioid withdrawal in the northern states of peninsular Malaysia and implications for drug substitution therapy. Int. J. Drug Policy 2010, 21, 283–288. [Google Scholar] [CrossRef]
- Kruegel, A.C.; Grundmann, O. The medicinal chemistry and neuropharmacology of kratom: A preliminary discussion of a promising medicinal plant and analysis of its potential for abuse. Neuropharmacology 2018, 134, 108–120. [Google Scholar] [CrossRef]
- Kruegel, A.C.; Gassaway, M.M.; Kapoor, A.; Varadi, A.; Majumdar, S.; Filizola, M.; Javitch, J.A.; Sames, D. Synthetic and Receptor Signaling Explorations of the Mitragyna Alkaloids: Mitragynine as an Atypical Molecular Framework for Opioid Receptor Modulators. J. Am. Chem. Soc. 2016, 138, 6754–6764. [Google Scholar] [CrossRef]
- Varadi, A.; Marrone, G.F.; Palmer, T.C.; Narayan, A.; Szabo, M.R.; Le, R.V.; Grinnell, S.G.; Subrath, J.J.; Warner, E.; Kalra, S.; et al. Mitragynine/Corynantheidine Pseudoindoxyls As Opioid Analgesics with Mu Agonism and Delta Antagonism, Which Do Not Recruit beta-Arrestin-2. J. Med. Chem. 2016, 59, 8381–8397. [Google Scholar] [CrossRef]
- Obeng, S.; Kamble, S.H.; Reeves, M.E.; Restrepo, L.F.; Patel, A.; Behnke, M.; Chear, N.J.; Ramanathan, S.; Sharma, A.; Leon, F.; et al. Investigation of the Adrenergic and Opioid Binding Affinities, Metabolic Stability, Plasma Protein Binding Properties, and Functional Effects of Selected Indole-Based Kratom Alkaloids. J. Med. Chem. 2020, 63, 433–439. [Google Scholar] [CrossRef]
- Suhaimi, F.W.; Yusoff, N.H.; Hassan, R.; Mansor, S.M.; Navaratnam, V.; Muller, C.P.; Hassan, Z. Neurobiology of Kratom and its main alkaloid mitragynine. Brain Res. Bull. 2016, 126, 29–40. [Google Scholar] [CrossRef] [PubMed]
- Prozialeck, W.C.; Jivan, J.K.; Andurkar, S.V. Pharmacology of kratom: An emerging botanical agent with stimulant, analgesic and opioid-like effects. J. Am. Osteopath. Assoc. 2012, 112, 792–799. [Google Scholar] [CrossRef] [PubMed]
- Grundmann, O. Patterns of Kratom use and health impact in the US-Results from an online survey. Drug Alcohol Depend. 2017, 176, 63–70. [Google Scholar] [CrossRef] [PubMed]
- Schimmel, J.; Amioka, E.; Rockhill, K.; Haynes, C.M.; Black, J.C.; Dart, R.C.; Iwanicki, J.L. Prevalence and description of kratom (Mitragyna speciosa) use in the United States: A cross-sectional study. Addiction 2020. [Google Scholar] [CrossRef] [PubMed]
- Garcia-Romeu, A.; Cox, D.J.; Smith, K.E.; Dunn, K.E.; Griffiths, R.R. Kratom (Mitragyna speciosa): User demographics, use patterns, and implications for the opioid epidemic. Drug Alcohol Depend. 2020, 208, 107849. [Google Scholar] [CrossRef] [PubMed]
- Smith, K.E.; Lawson, T. Prevalence and motivations for kratom use in a sample of substance users enrolled in a residential treatment program. Drug Alcohol Depend. 2017, 180, 340–348. [Google Scholar] [CrossRef]
- Swogger, M.T.; Hart, E.; Erowid, F.; Erowid, E.; Trabold, N.; Yee, K.; Parkhurst, K.A.; Priddy, B.M.; Walsh, Z. Experiences of Kratom Users: A Qualitative Analysis. J. Psychoact. Drugs 2015, 47, 360–367. [Google Scholar] [CrossRef]
- Swogger, M.T.; Walsh, Z. Kratom use and mental health: A systematic review. Drug Alcohol Depend. 2018, 183, 134–140. [Google Scholar] [CrossRef]
- Prozialeck, W.C.; Avery, B.A.; Boyer, E.W.; Grundmann, O.; Henningfield, J.E.; Kruegel, A.C.; McMahon, L.R.; McCurdy, C.R.; Swogger, M.T.; Veltri, C.A.; et al. Kratom policy: The challenge of balancing therapeutic potential with public safety. Int. J. Drug Policy 2019, 70, 70–77. [Google Scholar] [CrossRef] [PubMed]
- Prozialeck, W.C. Update on the Pharmacology and Legal Status of Kratom. J. Am. Osteopath. Assoc. 2016, 116, 802–809. [Google Scholar] [CrossRef]
- Anwar, M.; Law, R.; Schier, J. Notes from the Field: Kratom (Mitragyna speciosa) Exposures Reported to Poison Centers—United States, 2010–2015. MMWR Morb. Mortal. Wkly. Rep. 2016, 65, 748–749. [Google Scholar] [CrossRef] [PubMed]
- Warner, M.L.; Kaufman, N.C.; Grundmann, O. The pharmacology and toxicology of kratom: From traditional herb to drug of abuse. Int. J. Legal Med. 2016, 130, 127–138. [Google Scholar] [CrossRef] [PubMed]
- Olsen, E.O.; O’Donnell, J.; Mattson, C.L.; Schier, J.G.; Wilson, N. Notes from the Field: Unintentional Drug Overdose Deaths with Kratom Detected—27 States, July 2016–December 2017. MMWR Morb. Mortal. Wkly. Rep. 2019, 68, 326–327. [Google Scholar] [CrossRef] [PubMed]
- DEA. Schedules of Controlled Substances: Temporary Placement of Mitragynine and 7-Hydroxymitragynine Into Schedule I. Notes: Document number: 2016-20803. Available online: https://www.federalregister.gov/documents/2016/08/31/2016-20803/schedules-of-controlled-substances-temporary-placement-of-mitragynine-and-7-hydroxymitragynine-into (accessed on 31 August 2016).
- Griffin, O.H., III; Daniels, J.A.; Gardner, E.A. Do You Get What You Paid For? An Examination of Products Advertised as Kratom. J. Psychoactive. Drugs 2016, 48, 330–335. [Google Scholar] [CrossRef] [PubMed]
- Griffin, O.H.; Webb, M.E. The Scheduling of Kratom and Selective Use of Data. J. Psychoactive. Drugs 2018, 50, 114–120. [Google Scholar] [CrossRef] [PubMed]
- Kuehn, B. Kratom-Related Deaths. JAMA 2019, 321, 1966. [Google Scholar] [CrossRef]
- Corkery, J.M.; Streete, P.; Claridge, H.; Goodair, C.; Papanti, D.; Orsolini, L.; Schifano, F.; Sikka, K.; Korber, S.; Hendricks, A. Characteristics of deaths associated with kratom use. J. Psychopharmacol. 2019, 33, 1102–1123. [Google Scholar] [CrossRef]
- Scott, T.M.; Yeakel, J.K.; Logan, B.K. Identification of mitragynine and O-desmethyltramadol in Kratom and legal high products sold online. Drug Test. Anal. 2014, 6, 959–963. [Google Scholar] [CrossRef]
- CDC. Multistate Outbreak of Salmonella Infections Linked to Kratom (Final Update). Available online: https://www.cdc.gov/Salmonella/kratom-02-18/index.html (accessed on 18 June 2020).
- Dixon, R.B.; Waggoner, D.; Davis, M.; Rembold, K.; Dasgupta, A. Contamination of Some Kratom Products with Salmonella. Ann. Clin. Lab. Sci. 2019, 49, 675–677. [Google Scholar]
- Rauch, H.E.; Haendiges, J.; Balkey, M.; Hoffmann, M. Five Closed Salmonella enterica Genome Sequences from a 2017–2018 Multistrain, Multistate Kratom Outbreak. Microbiol. Resour. Announc. 2020, 9. [Google Scholar] [CrossRef]
- FDA. Statement by FDA Commisioner Scott Gottlieb, M.D., on Risk of Heavy Metals, including Nickel and Lead, Found in Some Kratom Products. Available online: https://www.fda.gov/NewsEvents/Newsroom/PressAnnouncements/ucm626738.htm (accessed on 18 June 2020).
- FDA. Laboratory Analysis of Kratom Products for Heavy Metals. Available online: https://www.fda.gov/news-events/public-health-focus/laboratory-analysis-kratom-products-heavy-metals (accessed on 18 June 2020).
- FDA. BAM Chapter 5: Salmonella. Available online: https://www.fda.gov/food/laboratory-methods-food/bam-chapter-5-salmonella (accessed on 17 June 2020).
- Braley, C.; Hondrogiannis, E.M. Differentiation of Commercially Available Kratom by Purported Country of Origin using Inductively Coupled Plasma-Mass Spectrometry. J. Forensic. Sci. 2020, 65, 428–437. [Google Scholar] [CrossRef] [PubMed]
- Fowble, K.L.; Musah, R.A. A validated method for the quantification of mitragynine in sixteen commercially available Kratom (Mitragyna speciosa) products. Forensic. Sci. Int. 2019, 299, 195–202. [Google Scholar] [CrossRef]
- Raffa, R.B.; Pergolizzi, J.V.; Taylor, R.; Ossipov, M.H.; Group, N.R. Nature’s first “atypical opioids”: Kratom and mitragynines. J. Clin. Pharm. Ther. 2018, 43, 437–441. [Google Scholar] [CrossRef] [PubMed]
- Lydecker, A.G.; Sharma, A.; McCurdy, C.R.; Avery, B.A.; Babu, K.M.; Boyer, E.W. Suspected Adulteration of Commercial Kratom Products with 7-Hydroxymitragynine. J. Med. Toxicol. 2016, 12, 341–349. [Google Scholar] [CrossRef] [PubMed]
- Wong, D.; Nielsen, T.B.; Bonomo, R.A.; Pantapalangkoor, P.; Luna, B.; Spellberg, B. Clinical and Pathophysiological Overview of Acinetobacter Infections: A Century of Challenges. Clin. Microbiol. Rev. 2017, 30, 409–447. [Google Scholar] [CrossRef] [PubMed]
- FDA. Q3D(R1) Elemental Impurities Guidance for Industry. Available online: https://www.fda.gov/media/135956/download (accessed on 18 June 2020).
- ATSDR. Toxicologic Profile for Lead. Available online: https://semspub.epa.gov/work/05/930045.pdf (accessed on 18 June 2020).
- Ramanathan, S.; McCurdy, C.R. Kratom (Mitragyna speciosa): Worldwide issues. Curr. Opin. Psychiatry 2020, 33, 312–318. [Google Scholar] [CrossRef]
- Rusmana, Y.; Einhorn, B. U.S. Hunger For Opioid Alternative Drives Boom in Borneo Jungle. Available online: https://www.bloomberg.com/news/features/2018-06-05/u-s-hunger-for-opioid-alternative-drives-boom-in-borneo-jungle (accessed on 18 June 2020).
- Galey, M.L.; van der Ent, A.; Iqbal, M.C.M.; Rajakaruna, N. Ultramafic geoecology of South and Southeast Asia. Bot. Stud. 2017, 58, 18. [Google Scholar] [CrossRef]
- Albalak, R.; Noonan, G.; Buchanan, S.; Flanders, W.D.; Gotway-Crawford, C.; Kim, D.; Jones, R.L.; Sulaiman, R.; Blumenthal, W.; Tan, R.; et al. Blood lead levels and risk factors for lead poisoning among children in Jakarta, Indonesia. Sci. Total. Environ. 2003, 301, 75–85. [Google Scholar] [CrossRef]
- Budianta, W. Lead Contamination In Soil Of Yogyakarta City, Indonesia. J. Appl. Geol. 2015, 4. [Google Scholar] [CrossRef]
- AKA. American Kratom Association Announces Good Manufacturing Practice (GMP) Standars for Vendors. Available online: https://www.prnewswire.com/news-releases/american-kratom-association-announces-good-manufacturing-practice-gmp-standards-for-vendors-300753751.html (accessed on 5 December 2018).
- AKA. AKA GMP Qualified Vendors. Available online: https://www.kratomplants.com/how-to-earn-the-aka-gmp-qualified-kratom-vendor-status/ (accessed on 18 June 2020).
| Sample # | Product | Vendor |
|---|---|---|
| 1 1A | Expert Botanicals Maeng Da Capsules | Westmont, IL, USA |
| 2 2A | mK Botanicals Maeng Da Capsules | Westmont, IL, USA |
| 3 3A | OPMS Maeng Da Capsules | Lisle, IL, USA |
| 4 4A | CBD Kratom Thai Maeng Da Capsules | Elmhurst, IL, USA |
| 5 5A | CBD Kratom Mixed Malay Capsules | Elmhurst, IL, USA |
| 6 6A | CBD Kratom Indo Red Bantuagle Capsules | Elmhurst, IL, USA |
| 7 7A | OPMS Gold Kratom Extract Capsules | Aurora, IL, USA |
| 8 8A | NJOY Kratom Red Malay Powder | Lisle, IL, USA |
| CFU/g Product | |||
|---|---|---|---|
| Product # | Sheep Blood Agar a | MacConkey Agar b, c | |
| 37 °C | 37 °C | 42 °C | |
| 1 | >1 × 108 | 6.7 × 104 | 2.6 × 104 |
| 1A | 3.4 × 105 | 6.5 × 104 | 3 × 104 |
| 2 | 3.3 × 105 | 0 | 0 |
| 2A | 2.5 × 105 | 1 | 2 |
| 3 | 0 | 0 | 0 |
| 3A | 0 | 0 | 0 |
| 4 | >1 × 108 | 4.1 × 105 | 1.6 × 106 |
| 4A | 6.4 × 105 | 3.2 × 105 | 3.6 × 105 |
| 5 | >1 × 108 | 8.7 × 104 | 0 |
| 5A | 2.9 × 105 | 1.7 × 104 | 2.0 × 104 |
| 6 | >1 × 108 | 4.2 × 105 | 0 |
| 6A | 8.0 × 105 | 8.7 × 104 | 5.5 × 104 |
| 7 | 0 | 0 | 0 |
| 7A | 0 | 0 | 0 |
| 8 | 4.2 × 105 | 4.3 × 104 | 8 × 102 |
| 8A | 2.1 × 105 | 2.0 × 104 | 2.0 × 104 |
| Target | Amount (µg/mL) | MF | Exact Mass | M + H | Retention Time | CID | Transition |
|---|---|---|---|---|---|---|---|
| Kratom Alkaloids | |||||||
| Mitragynine | - | C23H30N2O4 | 398.2206 | 399.2279 | 5.55 | 30 | 399.23 --> 174.09 |
| 7-Hydroxymitragynine | - | C23H30N2O5 | 414.2155 | 415.2228 | 2.58 | 30 | 415.22 --> 190.09 |
| Opioids | |||||||
| Buprenorphine | 100 | C29H41NO4 | 467.3036 | 468.3109 | 3.83 | 45 | 468.3 --> 396.2 |
| Codeine | 100 | C18H21NO3 | 299.1521 | 300.1594 | 1.37 | 56 | 300.2 --> 165.0 |
| Fentanyl | 10 | C22H28N2O | 336.2202 | 337.2275 | 3.74 | 44 | 337.5 --> 188.0 |
| Hydrocodone | 100 | C18H21NO3 | 299.1521 | 300.1594 | 2.11 | 32 | 300.2 --> 199.2 |
| Hydromorphone | 100 | C17H19NO3 | 285.1365 | 286.1438 | 0.80 | 36 | 286.2 --> 185.1 |
| Meperidine | 100 | C15H21NO2 | 247.1572 | 248.1645 | 3.01 | 37 | 248.2 --> 220.0 |
| (±)-Methadone | 100 | C21H27NO | 309.2093 | 310.2166 | 4.31 | 43 | 310.2 --> 105.0 |
| Morphine | 100 | C17H19NO3 | 285.1365 | 286.1438 | 0.63 | 44 | 286.2 --> 165.2 |
| Naloxone | 100 | C19H21NO4 | 327.1471 | 328.1544 | 1.27 | 35 | 328.3 --> 212.1 |
| Naltrexone | 100 | C20H23NO4 | 341.1627 | 342.1700 | 1.87 | 40 | 342.3 --> 212.2 |
| Oxycodone | 100 | C18H21NO4 | 315.1471 | 316.1544 | 1.91 | 20 | 316.2 --> 298.1 |
| Oxymorphone | 100 | C17H19NO4 | 301.1314 | 302.1387 | 0.69 | 24 | 302.1 --> 284.2 |
| cis-Tramadol HCl | 100 | C16H25NO2 | 263.1885 | 264.1958 | 2.71 | 31 | 262.2 --> 58.1 |
| Benzodiazepines | |||||||
| Alprazolam | 250 | C17H13ClN4 | 308.0829 | 309.0902 | 6.83 | 25 | 309.1 --> 281.1 |
| 40 | 309.1 --> 205.1 | ||||||
| Clonazepam | 250 | C15H10ClN3O3 | 315.0411 | 316.0484 | 6.94 | 25 | 316.1 --> 270.1 |
| 40 | 316.1 --> 214.1 | ||||||
| Diazepam | 250 | C16H13ClN2O | 284.0716 | 285.0789 | 8.28 | 25 | 285.1 --> 154.0 |
| 30 | 285.1 --> 193.1 | ||||||
| Flunitrazepam | 250 | C16H12FN3O3 | 313.0863 | 314.0936 | 7.49 | 25 | 314.1 --> 268.1 |
| 35 | 314.1 --> 239.2 | ||||||
| Lorazepam | 250 | C15H10Cl2N2O2 | 320.0119 | 321.0192 | 6.88 | 20 | 321.0 --> 275.1 |
| 33 | 321.0 --> 229.1 | ||||||
| Nitrazepam | 250 | C15H11N3O3 | 281.0800 | 282.0873 | 6.33 | 25 | 282.1 --> 236.2 |
| 35 | 282.1 --> 180.1 | ||||||
| Oxazepam | 250 | C15H11ClN2O2 | 286.0509 | 287.0582 | 6.54 | 20 | 287.0 --> 241.2 |
| 35 | 287.0 --> 104.0 | ||||||
| Temazepam | 250 | C16H13ClN2O2 | 300.0666 | 301.0739 | 7.64 | 20 | 301.0 --> 255.1 |
| 40 | 301.0 --> 177.1 |
| Product # | Mitragynine (mg/g) | Opioid Screen | Benzodiazepine Screen |
|---|---|---|---|
| 1 | 3.99 | ND | ND |
| 1A | 3.35 | ND | ND |
| 2 | 11.33 | ND | ND |
| 2A | 8.03 | ND | ND |
| 3 | 10.13 | ND | ND |
| 3A | 9.99 | ND | ND |
| 4 | 4.55 | ND | ND |
| 4A | 9.25 | ND | ND |
| 5 | 8.16 | ND | ND |
| 5A | 10.05 | ND | ND |
| 6 | 7.54 | ND | ND |
| 6A | 8.00 | ND | ND |
| 7 | 59.76 | ND | ND |
| 7A | 60.36 | ND | ND |
| 8 | 9.34 | ND | ND |
| 8A | 10.12 | ND | ND |
| Product # | Metal Concentration (μg/g Raw Kratom Product) | ||||||
|---|---|---|---|---|---|---|---|
| As | Cd | Cr | Fe | Hg | Ni | Pb | |
| 1 | 0.24 | 0.029 | 3.9 | 348 | 0.018 | 2.4 | 0.32 |
| 1A | 0.24 | 0.043 | 2.6 | 420 | 0.012 | 2.8 | 0.40 |
| 2 | 0.09 | 0.028 | 1.6 | 187 | 0.009 | 1.0 | 0.16 |
| 2A | 0.22 | 0.024 | 2.2 | 460 | 0.013 | 3.0 | 0.53 |
| 3 | 0.20 | 0.028 | 3.5 | 371 | 0.013 | 2.6 | 0.34 |
| 3A | 0.36 | 0.025 | 5.7 | 710 | 0.014 | 4.3 | 0.45 |
| 4 | 0.12 | 0.028 | 0.21 | 259 | 0.017 | 1.4 | 1.6 |
| 4A | 0.18 | 0.063 | 4.3 | 430 | 0.012 | 7.4 | 0.34 |
| 5 | 0.27 | 0.032 | 2.6 | 850 | 0.010 | 2.6 | 0.41 |
| 5A | 0.29 | 0.050 | 4.8 | 640 | 0.025 | 3.8 | 0.025 |
| 6 | 0.25 | 0.040 | 1.5 | 542 | 0.016 | 3.4 | 0.25 |
| 6A | 0.19 | 0.027 | 2.5 | 510 | 0.017 | 3.4 | 0.39 |
| 7 | ND | ND | ND | ND | ND | ND | ND |
| 7A | ND | ND | ND | 1.6 | ND | ND | ND |
| 8 | 0.11 | 0.028 | 0.39 | 270 | 0.014 | 0.73 | 0.45 |
| 8A | 0.12 | 0.020 | 0.86 | 350 | 0.012 | 1.6 | 0.58 |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Prozialeck, W.C.; Edwards, J.R.; Lamar, P.C.; Plotkin, B.J.; Sigar, I.M.; Grundmann, O.; Veltri, C.A. Evaluation of the Mitragynine Content, Levels of Toxic Metals and the Presence of Microbes in Kratom Products Purchased in the Western Suburbs of Chicago. Int. J. Environ. Res. Public Health 2020, 17, 5512. https://doi.org/10.3390/ijerph17155512
Prozialeck WC, Edwards JR, Lamar PC, Plotkin BJ, Sigar IM, Grundmann O, Veltri CA. Evaluation of the Mitragynine Content, Levels of Toxic Metals and the Presence of Microbes in Kratom Products Purchased in the Western Suburbs of Chicago. International Journal of Environmental Research and Public Health. 2020; 17(15):5512. https://doi.org/10.3390/ijerph17155512
Chicago/Turabian StyleProzialeck, Walter C., Joshua R. Edwards, Peter C. Lamar, Balbina J. Plotkin, Ira M. Sigar, Oliver Grundmann, and Charles A. Veltri. 2020. "Evaluation of the Mitragynine Content, Levels of Toxic Metals and the Presence of Microbes in Kratom Products Purchased in the Western Suburbs of Chicago" International Journal of Environmental Research and Public Health 17, no. 15: 5512. https://doi.org/10.3390/ijerph17155512
APA StyleProzialeck, W. C., Edwards, J. R., Lamar, P. C., Plotkin, B. J., Sigar, I. M., Grundmann, O., & Veltri, C. A. (2020). Evaluation of the Mitragynine Content, Levels of Toxic Metals and the Presence of Microbes in Kratom Products Purchased in the Western Suburbs of Chicago. International Journal of Environmental Research and Public Health, 17(15), 5512. https://doi.org/10.3390/ijerph17155512








