Coronavirus-Related Health Literacy: A Cross-Sectional Study in Adults during the COVID-19 Infodemic in Germany
Abstract
1. Introduction
2. Methods
2.1. Study Design and Target Group
2.2. Measures
2.2.1. Sociodemographic Indicators
2.2.2. Feeling Informed or Confused about the Coronavirus
2.2.3. Health Literacy
- Mean score of ≤2.5: “inadequate health literacy”
- Mean score of >2.5–<3: “problematic health literacy”
- Mean score of ≥3: “sufficient health literacy”
2.3. Data Analyses
2.4. Ethical Considerations
3. Results
3.1. Sample Characteristics
3.2. Psychometric Properties
3.2.1. Reliability
3.2.2. Validity
3.3. Health Literacy
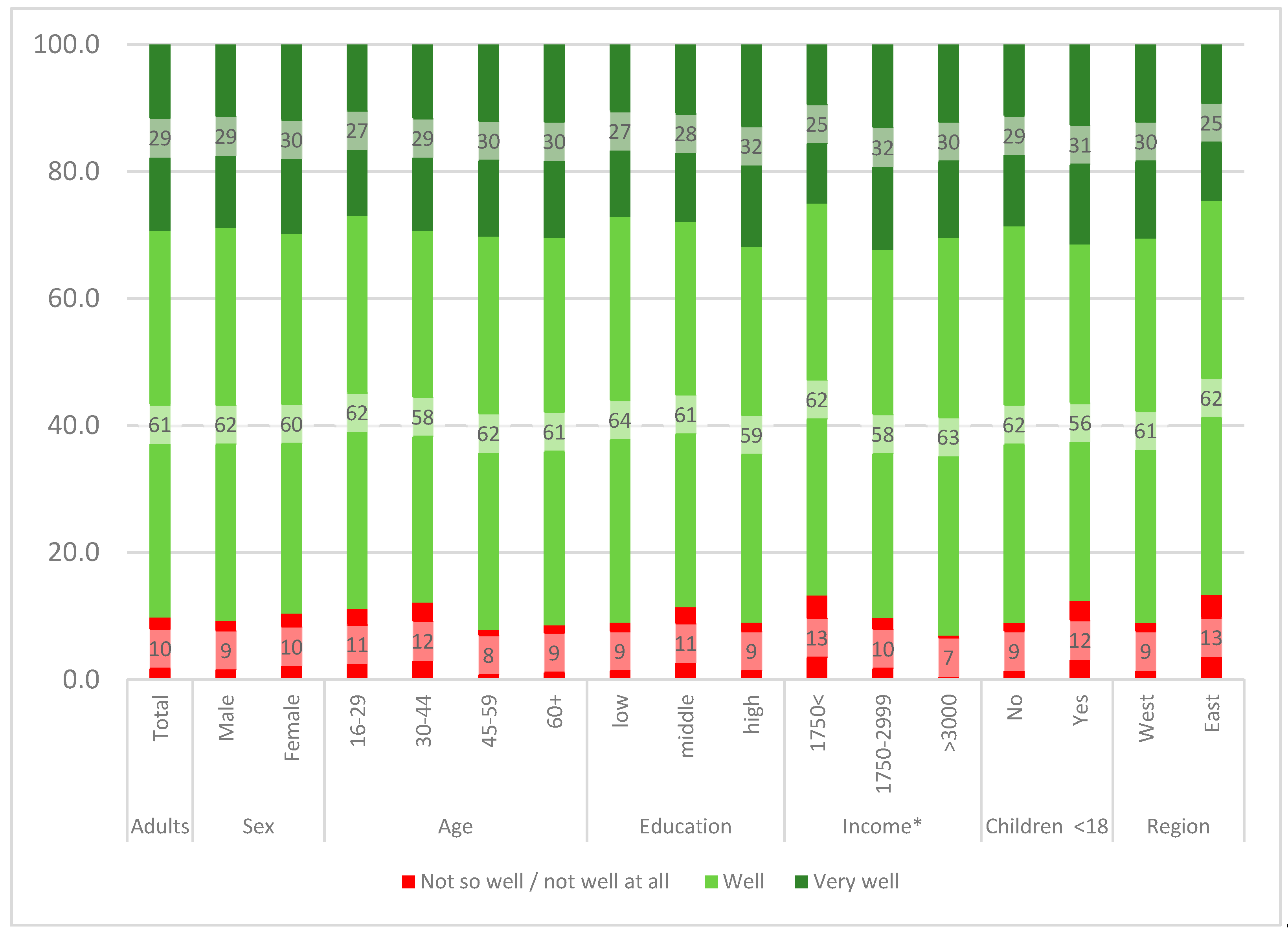
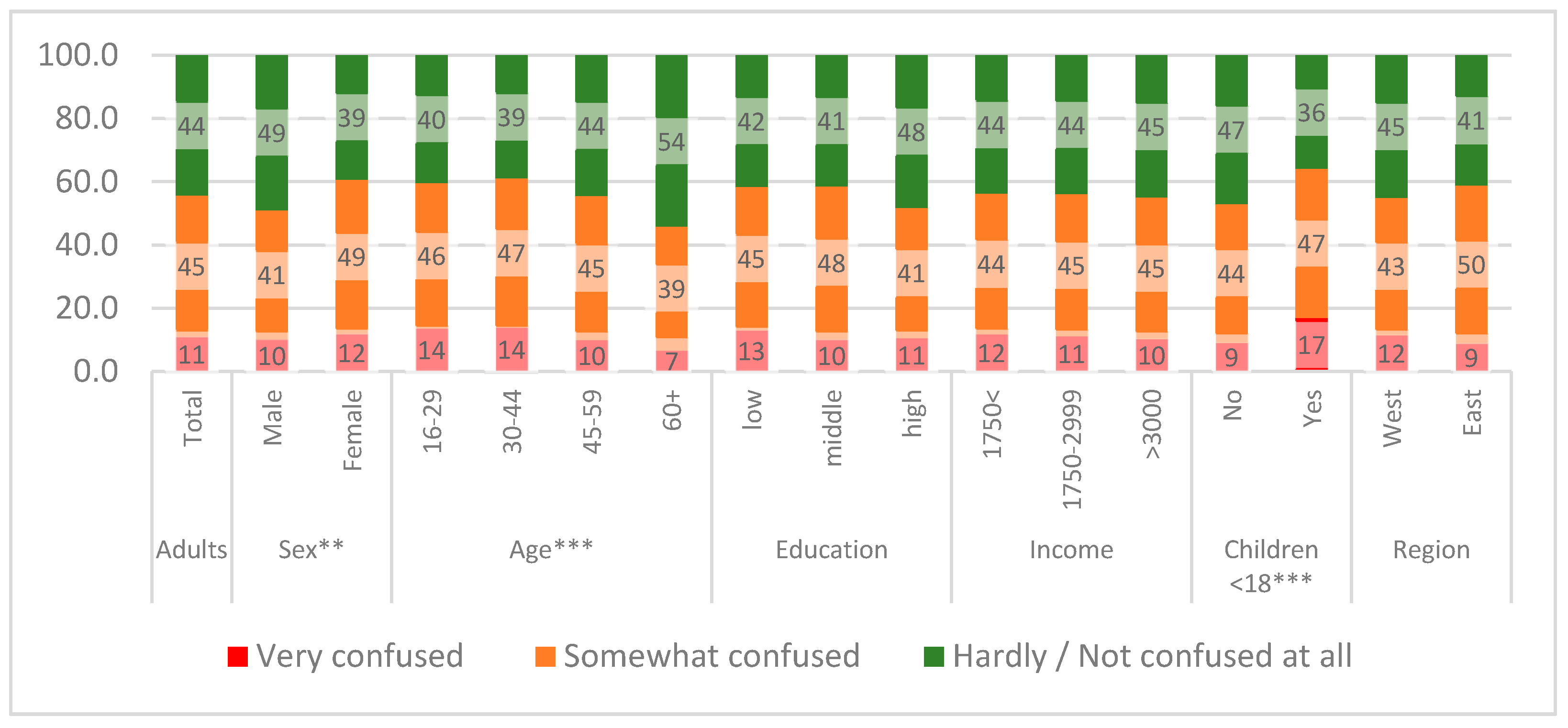
3.4. Feeling Informed or Confused about the Coronavirus during the Infodemic
4. Discussion
4.1. Coronavirus-Related Health Literacy
4.2. Information Tasks and Challenges
4.3. Infodemic and Associated Influences on Information Uptake and Use
4.3.1. Being Informed about Coronavirus
4.3.2. Being Confused about Coronavirus
4.3.3. Health Literacy and Infodemic
4.4. Feasibility of the Questionnaire
5. Limitations
6. Conclusions
Supplementary Materials
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- European Centre for Disease Prevention and Control. ECDC Communicable Disease Threats Report (CDTR). Available online: https://www.ecdc.europa.eu/sites/default/files/documents/Communicable-disease-threats-report-21-mar-2020-PUBLIC.pdf (accessed on 22 March 2020).
- Casadevall, A.; Pirofski, L.-A. The convalescent sera option for containing COVID-19. J. Clin. Investig. 2020, 130, 1545–1548. [Google Scholar] [CrossRef]
- Liu, Y.; Yan, L.-M.; Wan, L.; Xiang, T.-X.; Le, A.; Liu, J.-M.; Peiris, M.; Poon, L.L.M.; Zhang, W. Viral dynamics in mild and severe cases of COVID-19. Lancet Infect. Dis. 2020, 20, 656–657. [Google Scholar] [CrossRef]
- Hua, J.; Shaw, R. Corona Virus (COVID-19) “Infodemic” and Emerging Issues through a Data Lens: The Case of China. Int. J. Environ. Res. Public Health 2020, 17, 2309. [Google Scholar] [CrossRef]
- Zarocostas, J. How to fight an infodemic. Lancet 2020, 395, 676. [Google Scholar] [CrossRef]
- World Health Organization. Novel Coronavirus (2019-nCoV)—Situation Report 13. Available online: https://www.who.int/docs/default-source/coronaviruse/situation-reports/20200202-sitrep-13-ncov-v3.pdf (accessed on 16 May 2020).
- Rothkopf, D.J. When the Buzz Bites Back. Available online: http://www.udel.edu/globalagenda/2004/student/readings/infodemic.html (accessed on 27 May 2020).
- Nielsen, R.K.; Fletcher, R.; Newman, N.; Brennen, J.S.; Howard, P.N. Navigating the ‘Infodemic’: How People in Six Countries Access and Rate News and Information about Coronavirus. 2020. Available online: https://reutersinstitute.politics.ox.ac.uk/sites/default/files/2020-04/Navigating%20the%20Coronavirus%20Infodemic%20FINAL.pdf (accessed on 27 May 2020).
- Ashrafi-Rizi, H.; Kazempour, Z. Information Diet in Covid-19 Crisis; a Commentary. Arch. Acad. Emerg. Med. 2020, 8, e30. [Google Scholar]
- Ashrafi-Rizi, H.; Kazempour, Z. Information Typology in Coronavirus (COVID-19) Crisis; a Commentary. Arch. Acad. Emerg. Med. 2020, 8, e19. [Google Scholar]
- Brennen, J.S.; Simon, F.M.; Howard, P.N.; Nielsen, R.K. Types, Sources, and Claims of Covid-19 Misinformation. 2020. Available online: https://reutersinstitute.politics.ox.ac.uk/sites/default/files/2020-04/Brennen-COVID19MisinformationFINAL(3).pdf (accessed on 29 May 2020).
- Baines, D.; Elliott, R.J.R. Defining Misinformation, Disinformation and Malinformation: An Urgent Need for Clarity during the COVID-19 Infodemic; Discussion Papers 20; Department of Economics, University of Birmingham: Birmingham, UK, 2020. [Google Scholar]
- Luengo-Oroz, M.; Hoffmann Pham, K.; Bullock, J.; Kirkpatrick, R.; Luccioni, A.; Rubel, S.; Wachholz, C.; Chakchouk, M.; Biggs, P.; Nguyen, T.; et al. Artificial intelligence cooperation to support the global response to COVID-19. Nat. Mach. Intell. 2020, 577, 706. [Google Scholar] [CrossRef]
- World Health Organization. Infodemic management: A key component of the COVID-19 global response. Weekly Epidemiological Record 2020, 95, 145–148. Available online: https://apps.who.int/iris/handle/10665/331775 (accessed on 24 May 2020).
- World Health Organization. Coronavirus Disease 2019 (COVID-19)—Situation Report 86. Available online: https://www.who.int/docs/default-source/coronaviruse/situation-reports/20200415-sitrep-86-covid-19.pdf?sfvrsn=c615ea20_6 (accessed on 16 May 2020).
- van den Broucke, S. Why health promotion matters to the COVID-19 pandemic, and vice versa. Health Promot. Int. 2020, 35, 181–186. [Google Scholar] [CrossRef] [PubMed]
- Information Literacy Group. CILIP Definition of Information Literacy 2018. 2018. Available online: https://infolit.org.uk/ILdefinitionCILIP2018.pdf (accessed on 22 May 2020).
- Sentell, T.; Vamos, S.; Okan, O. Interdisciplinary Perspectives on Health Literacy Research Around the World: More Important Than Ever in a Time of COVID-19. Int. J. Environ. Res. Public Health 2020, 17, 3010. [Google Scholar] [CrossRef] [PubMed]
- Paakkari, L.; Okan, O. COVID-19: Health literacy is an underestimated problem. Lancet Public Health 2020, 5, e249–e250. [Google Scholar] [CrossRef]
- Okan, O.; Sørensen, K.; Messer, M. COVID-19: A guide to good practice on keeping people well informed. Conversation 2020, 19, 2020. [Google Scholar]
- Sørensen, K. Covid-19: Digital Health Literacy Is a Key to Saving Time, Costs and Lives. Available online: https://www.ictandhealth.com/news/covid-19-digital-health-literacy-is-a-key-to-saving-time-costs-and-lives/ (accessed on 11 April 2020).
- Abel, T.; McQueen, D. Critical health literacy and the COVID-19 crisis. Health Promot. Int. 2020, daaa040. [Google Scholar] [CrossRef] [PubMed]
- Sørensen, K.; van den Broucke, S.; Fullam, J.; Doyle, G.; Pelikan, J.M.; Slonska, Z.; Brand, H. Health literacy and public health: A systematic review and integration of definitions and models. BMC Public Health 2012, 12, 80. [Google Scholar] [CrossRef] [PubMed]
- Parker, R.; Ratzan, S.C. Health literacy: A second decade of distinction for Americans. J. Health Commun. 2010, 15 (Suppl. 2), 20–33. [Google Scholar] [CrossRef] [PubMed]
- Brach, C.; Keller, D.; Hernandez, L.M.; Baur, C.; Parker, R.; Dreyer, B.; Schyve, P.; Lemerise, A.J.; Schillinger, D. Ten Attributes of Health Literate Health Care Organizations; Institute of Medicine, Ed.; National Academy of Sciences: Washington, DC, USA, 2012. [Google Scholar]
- Pelikan, J.M. Health-literate healthcare organisations. In International Handbook of Health Literacy: Research, Practice and Policy across the Lifespan; Okan, O., Bauer, U., Levin-Zamir, D., Pinheiro, P., Sørensen, K., Eds.; Policy Press: Bristol, UK, 2019; pp. 539–553. ISBN 978-1-4473-4452-0. [Google Scholar]
- Berkman, N.D.; Sheridan, S.L.; Donahue, K.E.; Halpern, D.J.; Crotty, K. Low health literacy and health outcomes: An updated systematic review. Ann. Intern. Med. 2011, 155, 97–107. [Google Scholar] [CrossRef] [PubMed]
- Sørensen, K.; Pelikan, J.M.; Röthlin, F.; Ganahl, K.; Slonska, Z.; Doyle, G.; Fullam, J.; Kondilis, B.; Agrafiotis, D.; Uiters, E.; et al. Health literacy in Europe: Comparative results of the European Health Literacy Survey (HLS-EU). Eur. J. Public Health 2015, 25, 1053–1058. [Google Scholar] [CrossRef]
- Eichler, K.; Wieser, S.; Brügger, U. The costs of limited health literacy: A systematic review. Int. J. Public Health 2009, 54, 313–324. [Google Scholar] [CrossRef]
- Vernon, J.; Trujillo, A.; Rosenbaum, S.; DeBuono, B. Low Health Literacy: Implications for National Health Policy; National Bureau of Economic Research: Storrs, CT, USA, 2007. [Google Scholar]
- Palumbo, R. Examining the impacts of health literacy on healthcare costs. An evidence synthesis. Health Serv. Manag. Res. 2017, 30, 197–212. [Google Scholar] [CrossRef]
- Levin-Zamir, D.; Baron-Epel, O.B.; Cohen, V.; Elhayany, A. The association of health literacy with health behavior, socioeconomic indicators, and self-assessed health from a national adult survey in Israel. J. Health Commun. 2016, 21, 61–68. [Google Scholar] [CrossRef]
- Stormacq, C.; van den Broucke, S.; Wosinski, J. Does health literacy mediate the relationship between socioeconomic status and health disparities? Integrative review. Health Promot. Int. 2019, 34, e1–e17. [Google Scholar] [CrossRef] [PubMed]
- Kutner, M.; Greenberg, E.; Jin, Y.; Paulsen, C. The Health Literacy of America’s Adults: Results from the 2003 National Assessment of Adult Literacy (NCES 2006-483); U.S. Department of Education, National Center for Education Statistics: Washington, DC, USA, 2006.
- Nielsen-Bohlman, L.; Panzer, A.M.; Kindig, D.A. Health Literacy: A Prescription to End Confusion; Institute of Medicine; National Academies Press: Washington, DC, USA, 2004; ISBN 978-0-309-28332-8. [Google Scholar]
- Duong, T.V.; Aringazina, A.; Baisunova, G.; Pham, T.V.; Pham, K.M.; Truong, T.Q.; Nguyen, K.T.; Oo, W.M.; Mohamad, E.; Su, T.T.; et al. Measuring health literacy in Asia: Validation of the HLS-EU-Q47 survey tool in six Asian countries. J. Epidemiol. 2017, 27, 80–86. [Google Scholar] [CrossRef] [PubMed]
- Schaeffer, D.; Berens, E.-M.; Vogt, D. Health Literacy in the German Population. Dtsch. Arztebl. Int. 2017, 114, 53–60. [Google Scholar] [CrossRef] [PubMed]
- Nguyen, H.T.; Do, B.N.; Pham, K.M.; Kim, G.B.; Dam, H.T.B.; Nguyen, T.T.; Nguyen, T.T.P.; Nguyen, Y.H.; Sørensen, K.; Pleasant, A.; et al. Fear of COVID-19 Scale-Associations of Its Scores with Health Literacy and Health-Related Behaviors among Medical Students. Int. J. Environ. Res. Public Health 2020, 17, 4164. [Google Scholar] [CrossRef]
- Nguyen, H.C.; Nguyen, M.H.; Do, B.N.; Tran, C.Q.; Nguyen, T.T.P.; Pham, K.M.; Pham, L.V.; Tran, K.V.; Duong, T.T.; Tran, T.V.; et al. People with Suspected COVID-19 Symptoms Were More Likely Depressed and Had Lower Health-Related Quality of Life: The Potential Benefit of Health Literacy. J. Clin. Med. 2020, 9, 965. [Google Scholar] [CrossRef]
- Dadaczynski, K.; Okan, O.; Rathmann, K. COVID-19 Health Literacy Survey: University Students (COVID-HL-Survey). Questionnaire and Scale Documentation; Public Health Centre Fulda at Fulda University of Applied Sciences; Interdisciplinary Centre for Health Literacy Research at Bielefeld University: Fulda and Bielefeld, Germany, 2020. [Google Scholar]
- Dadaczynski, K.; Okan, O.; Rathmann, K. Research on COVID-19 and Health Literacy: COVID-HL Consoritum. Available online: http://covid-hl.eu/ (accessed on 30 March 2020).
- Sørensen, K.; van den Broucke, S.; Pelikan, J.M.; Fullam, J.; Doyle, G.; Slonska, Z.; Kondilis, B.; Stoffels, V.; Osborne, R.H.; Brand, H. Measuring health literacy in populations: Illuminating the design and development process of the European Health Literacy Survey Questionnaire (HLS-EU-Q). BMC Public Health 2013, 13, 948. [Google Scholar] [CrossRef]
- Pelikan, J.M.; Ganahl, K. Measuring health literacy in general populations: Primary findings from the HLS-EU Consortium’s health literacy assessment effort. In Health Literacy: New Directions in Research, Theory and Practice; Logan, R.A., Siegel, E.R., Eds.; IOS Press Incorporated: Amsterdam, The Netherlands, 2017; pp. 34–59. ISBN 9781614997894. [Google Scholar]
- Röthlin, F.; Pelikan, J.; Ganahl, K. Die Gesundheitskompetenz von 15-jährigen Jugendlichen in Österreich. Abschlussbericht der österreichischen Gesundheitskompetenz Jugendstudie im Auftrag des Hauptverbands der österreichischen Sozialversicherungsträger (HVSV); Ludwig Boltzmann Gesellschaft GmbH: Vienna, Austria, 2013. [Google Scholar]
- Jordan, S.; Hoebel, J. Gesundheitskompetenz von Erwachsenen in Deutschland: Ergebnisse der Studie “Gesundheit in Deutschland aktuell” (GEDA). Bundesgesundheitsblatt Gesundheitsforschung Gesundheitsschutz 2015, 58, 942–950. [Google Scholar] [CrossRef]
- Okan, O.; de Sombre, S.; Hurrelmann, K.; Berens, E.-M.; Bauer, U.; Schaeffer, D. COVID-19 based health literacy in the German population [In German: Covid-19-Gesundheitskompetenz der Bevölkerung]. Monit. Versorg. 2020, 13, 40–45. [Google Scholar] [CrossRef]
- Federal Statistical Office of Germany. Mikrozensus 2018: Population and Occupation [In German: Bevölkerung und Erwerbstätigkeit. Haushalte und Familien. Ergebnisse des Mikrozensus 2018]; Statistisches Bundesamt: Wiesbaden, Germany, 2019. [Google Scholar]
- Arbuckle, J.L. IBM SPSS AMOS 22 Users’ Guide; IBM Corp.: Chicago, IL, USA, 2013. [Google Scholar]
- Weiber, R.; Mühlhaus, D. Strukturgleichungsmodellierung; Springer: Berlin/Heidelberg, Germany, 2014; ISBN 978-3-642-35011-5. [Google Scholar]
- Tabachnick, B.G.; Fidell, L.S. Using Multivariate Statistics, 7th ed.; Pearson/Allyn and Bacon: Boston, MA, USA, 2019; ISBN 9780134790541. [Google Scholar]
- IBM Corp. IBM SPSS Statistics for Windows, Version 22.0; IBM Corp.: Armonk, NY, USA, 2013. [Google Scholar]
- Cronbach, L.J.; Shavelson, R.J. My Current Thoughts on Coefficient Alpha and Successor Procedures. Educ. Psychol. Meas. 2004, 64, 391–418. [Google Scholar] [CrossRef]
- Hooper, D.; Coughlan, J.; Mullen, M.R. Structural Equation Modelling: Guidelines for Determining Model Fit. Electron. J. Bus. Res. Methods 2008, 6, 53–60. [Google Scholar]
- Pelikan, J.M.; Ganahl, K.; Roethlin, F. Health literacy as a determinant, mediator and/or moderator of health: Empirical models using the European Health Literacy Survey dataset. Glob. Health Promot. 2018, 1757975918788300. [Google Scholar] [CrossRef] [PubMed]
- ZDF. ZDF-Politbarometer. Available online: https://www.zdf.de/nachrichten/politik/politbarometer-corona-massnahmen-100.html (accessed on 5 June 2020).
- Möthe, A. Eine Woche Kontaktsperre: Wie Die Bevölkerung Die Corona-Maßnahmen Beurteilt. Available online: https://www.handelsblatt.com/politik/deutschland/datenanalyse-eine-woche-kontaktsperre-wie-die-bevoelkerung-die-corona-massnahmen-beurteilt/25697634.html?ticket=ST-779603-Qb9JhdDbBxxeunpPOOCt-ap6 (accessed on 5 June 2020).
- CIVEY. Live-Lagebericht Public Sector Vorschau. Available online: https://app.civey.com/dashboards/live-lagebericht-public-sector-vorschau-1855 (accessed on 5 June 2020).
- Altmann, D.M.; Douek, D.C.; Boyton, R.J. What policy makers need to know about COVID-19 protective immunity. Lancet 2020, 395, 1527–1529. [Google Scholar] [CrossRef]
- Hernández-García, I.; Giménez-Júlvez, T. Assessment of Health Information About COVID-19 Prevention on the Internet: Infodemiological Study. JMIR Public Health Surveill. 2020, 6, e18717. [Google Scholar] [CrossRef] [PubMed]
- Cuan-Baltazar, J.Y.; Muñoz-Perez, M.J.; Robledo-Vega, C.; Pérez-Zepeda, M.F.; Soto-Vega, E. Misinformation of COVID-19 on the Internet: Infodemiology Study. JMIR Public Health Surveill. 2020, 6, e18444. [Google Scholar] [CrossRef]
- Eurostat. Internet Access of Households, 2013 and 2018. 2019. Available online: https://ec.europa.eu/eurostat/statistics-explained/index.php?title=Digital_economy_and_society_statistics_-_households_and_individuals (accessed on 4 June 2020).
- BITKOM. Internet Use and Access Based on EUROSTAT. Available online: https://www.bitkom.org/Presse/Presseinformation/Hamburger-und-Pfaelzer-surfen-besonders-haeufig-im-Web.html (accessed on 4 June 2020).
- Robert Koch Institute. Coronavirus Disease 2019 (COVID-19): Daily Situation Report of the Robert Koch Institute: 4.3.2020. Available online: https://www.rki.de/DE/Content/InfAZ/N/Neuartiges_Coronavirus/Situationsberichte/2020-03-04-en.pdf?__blob=publicationFile (accessed on 4 June 2020).
- Wirtschafts- und Sozialwissenschaftliches Institut. Wer leistet unbezahlte Arbeit? Available online: https://www.wsi.de/de/faust-detail.htm?sync_id=7793 (accessed on 4 June 2020).
- Work Stress and Health in a Globalized Economy. The Model of Effort-Reward Imbalance; Siegrist, J., Wahrendorf, M., Eds.; Springer International Publishing: Cham, Switzerland, 2016; ISBN 9783319329376. [Google Scholar]
- Bidmon, S.; Terlutter, R. Gender Differences in Searching for Health Information on the Internet and the Virtual Patient-Physician Relationship in Germany: Exploratory Results on How Men and Women Differ and Why. J. Med. Internet Res. 2015, 17, e156. [Google Scholar] [CrossRef]
- Eysenbach, G.; Powell, J.; Kuss, O.; Sa, E.-R. Empirical studies assessing the quality of health information for consumers on the world wide web: A systematic review. JAMA 2002, 287, 2691–2700. [Google Scholar] [CrossRef]
- Vaezi, A.; Javanmard, S.H. Infodemic and Risk Communication in the Era of CoV-19. Adv. Biomed. Res. 2020, 9, 10. [Google Scholar] [CrossRef]
- Cinelli, M.; Quattrociocchi, W.; Galeazzi, A.; Valensise, C.M.; Brugnoli, E.; Schmidt, A.L.; Zola, P.; Zollo, F.; Scala, A. The COVID-19 Social Media Infodemic. arXiv 2020, arXiv:2003.05004. [Google Scholar]
- Merchant, R.M.; Lurie, N. Social Media and Emergency Preparedness in Response to Novel Coronavirus. JAMA 2020, 323, 2011–2012. [Google Scholar] [CrossRef]
- Medford, R.J.; Saleh, S.N.; Sumarsono, A.; Perl, T.M.; Lehmann, C.U. An “Infodemic”: Leveraging High-Volume Twitter Data to Understand Public Sentiment for the COVID-19 Outbreak. Open Forum Infect. Dis. 2020, 7, ofaa258. [Google Scholar] [CrossRef]
- Kyriakidou, M.; Morani, M.; Soo, N.; Cushion, S. Government and Media Misinformation about COVID-19 Is Confusing the Public. LSE COVID-19 Blog 2020, Blog Entry. Available online: https://blogs.lse.ac.uk/covid19/2020/05/07/government-and-media-misinformation-about-covid-19-is-confusing-the-public/ (accessed on 7 May 2020).
- Eysenbach, G. Infodemiology and infoveillance tracking online health information and cyberbehavior for public health. Am. J. Prev. Med. 2011, 40, S154–S158. [Google Scholar] [CrossRef] [PubMed]
- Finbråten, H.S.; Wilde-Larsson, B.; Nordström, G.; Pettersen, K.S.; Trollvik, A.; Guttersrud, Ø. Establishing the HLS-Q12 short version of the European Health Literacy Survey Questionnaire: Latent trait analyses applying Rasch modelling and confirmatory factor analysis. BMC Health Serv. Res. 2018, 18, 506. [Google Scholar] [CrossRef] [PubMed]
- Nakayama, K.; Osaka, W.; Togari, T.; Ishikawa, H.; Yonekura, Y.; Sekido, A.; Matsumoto, M. Comprehensive health literacy in Japan is lower than in Europe: A validated Japanese-language assessment of health literacy. BMC Public Health 2015, 15, 505. [Google Scholar] [CrossRef] [PubMed]
- Pleasant, A. Advancing Health Literacy Measurement: A Pathway to Better Health and Health System Performance. J. Health Commun. 2014, 19, 1481–1496. [Google Scholar] [CrossRef] [PubMed]
| Tools | # of Items | Score | Answers Dichotomized * | Scores Transformed † | Cut-Off Values (Relative) | Cut-Off Values (Absolute) |
|---|---|---|---|---|---|---|
| HLS-EU-Q47 [28,42] | 47 | Mean | No | Yes | a ≤ 50% (½) 50% < b < 66% (~⅔) 66.6% ≤ c < 84% (~⅚) 84 ≤ d | 0 < a ≤ 25 25 < b < 33 33 ≤ c < 42 42 ≤ d |
| HLS-EU-Q16 [44] | 16 | Sum | Yes | No | a ≤ 50% 50% < b < 81.3% 81.3% ≤ c | 0 < a < 9 9 ≤ b < 13 13 ≤ c |
| HLS-COVID-Q22 [46] | 22 | Mean | No | No | ≤ 50% 50% < b < 66% 66% ≤ c | a ≤ 2.5 2.5 < b < 3 3 ≤ c |
| Model | χ2/df | NFI | IFI | TLI | CFI | RMSEA [95% CI] | SRMR |
|---|---|---|---|---|---|---|---|
| Model 1 | 7.664 | 0.872 | 0.887 | 0.871 | 0.887 | 0.080 [0.077–0.084] | 0.048 |
| Model 2 | 5.996 | 0.902 | 0.917 | 0.904 | 0.916 | 0.069 [0.066–0.073] | 0.043 |
| Questionnaire and Subscales | Subscale “Access” | Subscale “Understand” | Subscale “Appraise” | Subscale “Apply” |
|---|---|---|---|---|
| HLS-COVID-Q22 | 0.880 ** | 0.897 ** | 0.876 ** | 0.874 ** |
| Subscale “access” | 1 | 0.742 ** | 0.690 ** | 0.647 ** |
| Subscale “understand” | - | 1 | 0.675 ** | 0.736 ** |
| Subscale “appraise” | - | - | 1 | 0.729 ** |
| Study Population | Health Literacy Levels [%] | Health Literacy Scores | |||
|---|---|---|---|---|---|
| “Inadequate” | “Problematic” | “Sufficient” | Mean (SD) | p | |
| Total (n = 1037) | 15.2 | 34.9 | 49.9 | 2.99 (0.49) | |
| Sex | |||||
| Female (n = 505; 48.7%) | 15.2 | 34.5 | 50.3 | 2.99 (0.49) | ref. |
| Male (n = 532; 51.3%) | 15.2 | 35.2 | 49.6 | 2.99 (0.49) | 0.904 |
| Age | |||||
| 16–29 (n = 226; 21.8%) | 14.8 | 39.0 | 46.2 | 2.96 (0.48) | 0.326 |
| 30–44 (n = 267; 25.7%) | 15.9 | 31.4 | 52.7 | 2.99 (0.50) | ref. |
| 45–59 (n = 319; 30.8%) | 15.2 | 32.6 | 52.2 | 3.02 (0.50) | 0.877 |
| 60+ (n = 225; 21.7%) | 14.8 | 38.0 | 47.2 | 2.98 (0.48) | 0.614 |
| Education | |||||
| Low (n = 264; 25.5%) | 18.0 | 35.8 | 46.1 | 2.94 (0.52) | 0.597 |
| Medium (n = 347; 33.5%) | 15.3 | 35.6 | 49.2 | 2.98 (0.49) | ref. |
| High (n = 425; 41%) | 13.4 | 33.7 | 52.9 | 3.03 (0.48) | 0.161 |
| Household income | |||||
| Below 1750 € (n = 327; 31.5%) | 18.1 | 34.4 | 47.6 | 2.96 (0.52) | 0.496 |
| 1750–2999 € (n = 327; 31.5%) | 13.9 | 34.8 | 51.3 | 3.00 (0.48) | ref. |
| 3000 € + (n = 383; 37%) | 13.9 | 35.4 | 50.8 | 3.01 (0.48) | 0.409 |
| Do you have children younger than 18? | |||||
| Yes (n = 257; 24.8%) | 18.6 | 30.4 | 51.0 | 2.96 (0.54) | ref. |
| No (n = 780; 75.2%) | 14.1 | 36.3 | 49.6 | 3.00 (0.48) | 0.633 |
| Region | |||||
| Former Western Germany (n = 832; 80.3%) | 15.6 | 33.6 | 50.8 | 2.99 (0.49) | ref. |
| Former East Germany (n = 205; 19.7%) | 13.7 | 39.9 | 46.4 | 2.97 (0.49) | 0.322 |
| How well are you informed about the coronavirus? | |||||
| Very well (n = 304; 29.3%) | 4.7 | 28.3 | 67.0 | 3.23 (0.50) | <0.001 |
| Well (n = 631; 60.9%) | 13.6 | 39.7 | 46.7 | 2.95 (0.41) | ref. |
| Not so well/not well at all (n = 102; 9.8%) | 56.4 | 24.5 | 19.1 | 2.51 (0.51) | <0.001 |
| Do you feel confused about COVID-19 information? | |||||
| Very confused (n = 115; 11.1%) | 40.2 | 28.2 | 31.6 | 2.72 (0.57) | <0.01 |
| Somewhat confused (n = 463; 44.6%) | 17.0 | 42.4 | 40.6 | 2.90 (0.43) | ref. |
| Barely confused/not confused at all (n = 459; 44.3%) | 7.1 | 28.9 | 64.0 | 3.15 (0.47) | <0.001 |
| # | How Easy or Difficult is It for You to… | Related HLS-EU-Q Item a | Very Difficult | Difficult | Easy | Very Easy | Mean (SD) |
|---|---|---|---|---|---|---|---|
| 1 | Find information about the coronavirus on the internet? | 1; 2 | 1.2 | 6.4 | 49.7 | 42.7 | 3.34 (0.65) |
| 2 | Find information on the internet about protective behaviors that can help to prevent infection with the coronavirus? | 13; 33 | 1.1 | 9.9 | 52.4 | 36.6 | 3.25 (0.67) |
| 3 | Find information in newspapers, magazines and on TV about behaviors that can help to prevent infection with the coronavirus? | 13; 33 | 2.3 | 16.3 | 54.5 | 26.8 | 3.06 (0.72) |
| 4 | Find information on how to recognize if I have likely become infected with the coronavirus? | 8; 18 | 6.2 | 27.6 | 46.7 | 19.6 | 2.80 (0.82) |
| 5 | Find information on how to find professional help in case of coronavirus infection? | 2; 4 | 6.0 | 27.7 | 46.1 | 20.2 | 2.81 (0.83) |
| 6 | Find information on how I much I am at risk for being infected with the coronavirus? | 2; 4 | 4.1 | 28.9 | 46.4 | 20.6 | 2.84 (0.79) |
| 7 | Understand your doctor’s, pharmacist’s or nurse’s instructions on protective measures against coronavirus infection? | 4; 8 | 1.0 | 9.7 | 57.7 | 31.5 | 3.20 (0.65) |
| 8 | Understand recommendations of authorities regarding protective measures against coronavirus infection? | 10; 23 | 2.6 | 13.0 | 53.7 | 30.7 | 3.13 (0.73) |
| 9 | Understand advice from family members or friends regarding protective measures against coronavirus infection? | 14; 37 | 2.2 | 12.5 | 58.3 | 27.0 | 3.10 (0.69) |
| 10 | Understand information in the media on how to protect myself against coronavirus infection? | 15; 39 | 1.3 | 11.2 | 58.3 | 29.2 | 3.15 (0.66) |
| 11 | Understand risks of the coronavirus that I find on the internet? | 9; 21 | 1.8 | 17.1 | 55.2 | 25.9 | 3.05 (0.71) |
| 12 | Understand risks of the coronavirus that I find in newspapers, magazines or on TV? | 3; 5 | 2.3 | 17.8 | 56.0 | 23.9 | 3.01 (0.71) |
| 13 | Judge if information on the coronavirus and the coronavirus epidemic in the media is reliable? | 11; 28 | 11.3 | 36.5 | 39.0 | 13.1 | 2.54 (0.86) |
| 14 | Judge which behaviors are associated with a higher risk of coronavirus infection? | 16; 43 | 3.6 | 18.4 | 53.6 | 24.4 | 2.99 (0.76) |
| 15 | Judge what protective measures you can apply to prevent a coronavirus infection? | 5; 11 | 2.6 | 15.5 | 54.4 | 27.4 | 3.07 (0.73) |
| 16 | Judge how much I am at risk for a coronavirus infection? | 11; 43 | 3.8 | 27.4 | 45.8 | 23.0 | 2.88 (0.80) |
| 17 | Judge if I have been infected with coronavirus? | 11; 43 | 11.3 | 40.5 | 34.8 | 13.4 | 2.50 (0.86) |
| 18 | Decide how you can protect yourself from coronavirus infection based on information in the media? | 12; 31 | 3.6 | 17.3 | 57.5 | 21.6 | 2.97 (0.73) |
| 19 | Follow instructions from your doctor or pharmacist regarding how to handle the coronavirus situation? | 7; 16 | 2.1 | 12.0 | 58.1 | 27.8 | 3.11 (0.69) |
| 20 | Use information the doctor gives you to decide how to handle an infection with the coronavirus? | 6; 13 | 2.3 | 17.0 | 59.4 | 21.3 | 3.00 (0.69) |
| 21 | Use media information to decide how to handle an infection with the coronavirus? | 6; 13 | 4.2 | 27.9 | 50.3 | 17.6 | 2.81 (0.77) |
| 22 | to behave in a way to avoid infecting others? | 12; 31 | 2.5 | 11.9 | 52.1 | 33.5 | 3.17 (0.73) |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Okan, O.; Bollweg, T.M.; Berens, E.-M.; Hurrelmann, K.; Bauer, U.; Schaeffer, D. Coronavirus-Related Health Literacy: A Cross-Sectional Study in Adults during the COVID-19 Infodemic in Germany. Int. J. Environ. Res. Public Health 2020, 17, 5503. https://doi.org/10.3390/ijerph17155503
Okan O, Bollweg TM, Berens E-M, Hurrelmann K, Bauer U, Schaeffer D. Coronavirus-Related Health Literacy: A Cross-Sectional Study in Adults during the COVID-19 Infodemic in Germany. International Journal of Environmental Research and Public Health. 2020; 17(15):5503. https://doi.org/10.3390/ijerph17155503
Chicago/Turabian StyleOkan, Orkan, Torsten Michael Bollweg, Eva-Maria Berens, Klaus Hurrelmann, Ullrich Bauer, and Doris Schaeffer. 2020. "Coronavirus-Related Health Literacy: A Cross-Sectional Study in Adults during the COVID-19 Infodemic in Germany" International Journal of Environmental Research and Public Health 17, no. 15: 5503. https://doi.org/10.3390/ijerph17155503
APA StyleOkan, O., Bollweg, T. M., Berens, E.-M., Hurrelmann, K., Bauer, U., & Schaeffer, D. (2020). Coronavirus-Related Health Literacy: A Cross-Sectional Study in Adults during the COVID-19 Infodemic in Germany. International Journal of Environmental Research and Public Health, 17(15), 5503. https://doi.org/10.3390/ijerph17155503






