1. Introduction
On March 11, 2020, the World Health Organization announced officially the coronavirus pandemic which was first detected in Wuhan, China in December of 2019 [
1]. By March 16, 2020, the new coronavirus labeled COVID-19 had spread globally across 151 territories affecting 167,511 persons and killing more than 6500 [
2]. Ten days later, the U.S. emerged as the epicenter of COVID-19, surpassing China’s case count [
3,
4]. As of April 13, 2020, the U.S. reported 582,468 cases of COVID-19 and 23,622 deaths [
5], representing approximately 30% and 20% of the world’s COVID-19 morbidity and mortality. In the U.S., the state of Colorado, which is the focus of this study, reported the third highest number of COVID-19 cases (
n = 7691) in the West, following the states of California and Washington, respectively [
6,
7]. Approximately 329 deaths were documented, since the first case of COVID-19 was reported on February 20 in Colorado [
6,
8].
Recent reports indicate, like in many other states [
9], that COVID-19 incidence and deaths are disproportionately affecting communities of color in Colorado [
10,
11]. As of April 13, 2020, approximately 36.7% of cases and 26.7% of deaths were persons of Hispanic, non-Hispanic Black, and non-Hispanic Native Hawaiian or Pacific Islander origins, of which Hispanics shared the greatest burden of COVID-19 incidence and deaths [
11]. Although the Colorado Department of Public Health and Environment (CDPHE) has yet to release socioeconomic information about COVID-19 cases, it is likely that these racial and ethnic disparities also correspond to inequalities in the social determinants of health, “the conditions in places where people live, learn, work, and play” [
12]. As governmental and nongovernmental organizations report, communities of color and lower income persons face greater vulnerability to COVID-19 due to social, health and environmental disparities, such as lack of access to healthy foods, quality housing, health insurance and healthcare, and greater exposure to ambient air pollution [
9,
13]. Relatedly, such communities are also disproportionately affected by preexisting chronic conditions such as diabetes, cancer, and asthma [
14], which may increase risk for severe COVID-19 health outcomes [
15,
16,
17]. In Massachusetts, for example, researchers estimated that areas with higher levels of poverty, overcrowding, and populations of color were significantly associated with excess deaths during the first 15 weeks of 2020 [
18]. Similarly, in New York, hospitalizations and deaths are distributed unevenly across racial and socioeconomic lines [
19]. In Colorado, the Executive Director of CDPHE states, ‘We know that social and health care inequities affect outcomes, and that becomes even more apparent in times of disaster’ (as quoted in [
10]).
Within this context, the aim of this rapid study was to examine the initial spatial patterns of COVID-19 in Colorado and explore preliminary associations with social determinants of health and chronic conditions. Using geographic information systems (GIS) and bivariate correlation analyses, this study investigated COVID-19 incidence and deaths from March 14, 2020 to April 8, 2020 at the county-level and the wider social, economic, and health context of emergence. Understanding the geographic patterns of COVID-19 in Colorado and the social determinants context may assist public health investigators with socially relevant insights, particularly as new information emerges about COVID-19 disparities among Colorado’s population.
2. Data
Publicly available COVID-19 data were downloaded daily from the Colorado COVID-19 online summaries, including geospatial information from CDPHE [
6,
20] and their Open Data Portal [
21]. COVID incidence data include laboratory-confirmed and probable cases, and persons who tested positive for COVID-19 while visiting were assigned to the county where they were identified [
22]. Social determinants of health data were retrieved from the social vulnerability index (SVI) dataset (2014–2018) from Centers for Disease Control and Prevention (CDC) (see [
23] for variables’ details). These SVI data intended for the assessment of population vulnerability to disasters [
24], include proxy variables for socioeconomic status, household composition, and minority status. To date, SVI data have been employed to examine wildfires [
25], physical inactivity [
26], and mental health and housing affordability [
27]. Among SVI variables, a few indicators may be more relevant to vulnerability and exposure such as poverty and overcrowding, both of which have been correlated with influenza [
28,
29], and recently, COVID-19 [
18], although at the census-tract and zipcode levels. Chronic conditions, such as asthma and diabetes hospitalizations (age-adjusted, per 100,000), heart disease mortality (age-adjusted, per 100,000), cancer mortality (age-adjusted, per 100,000), and obesity prevalence (adults, %), as well as influenza hospitalizations (age-adjusted, per 100,000) and mental health-related outcomes (suicide deaths and drug-related deaths, both per 100,000) were obtained from CDPHE [
21], CDC [
30], and County Health Rankings [
31]. Health data represent the time period, 2013–2017, except for cancer (2012–2016) and obesity (2017). All datasets represent county-level estimates.
3. Methods
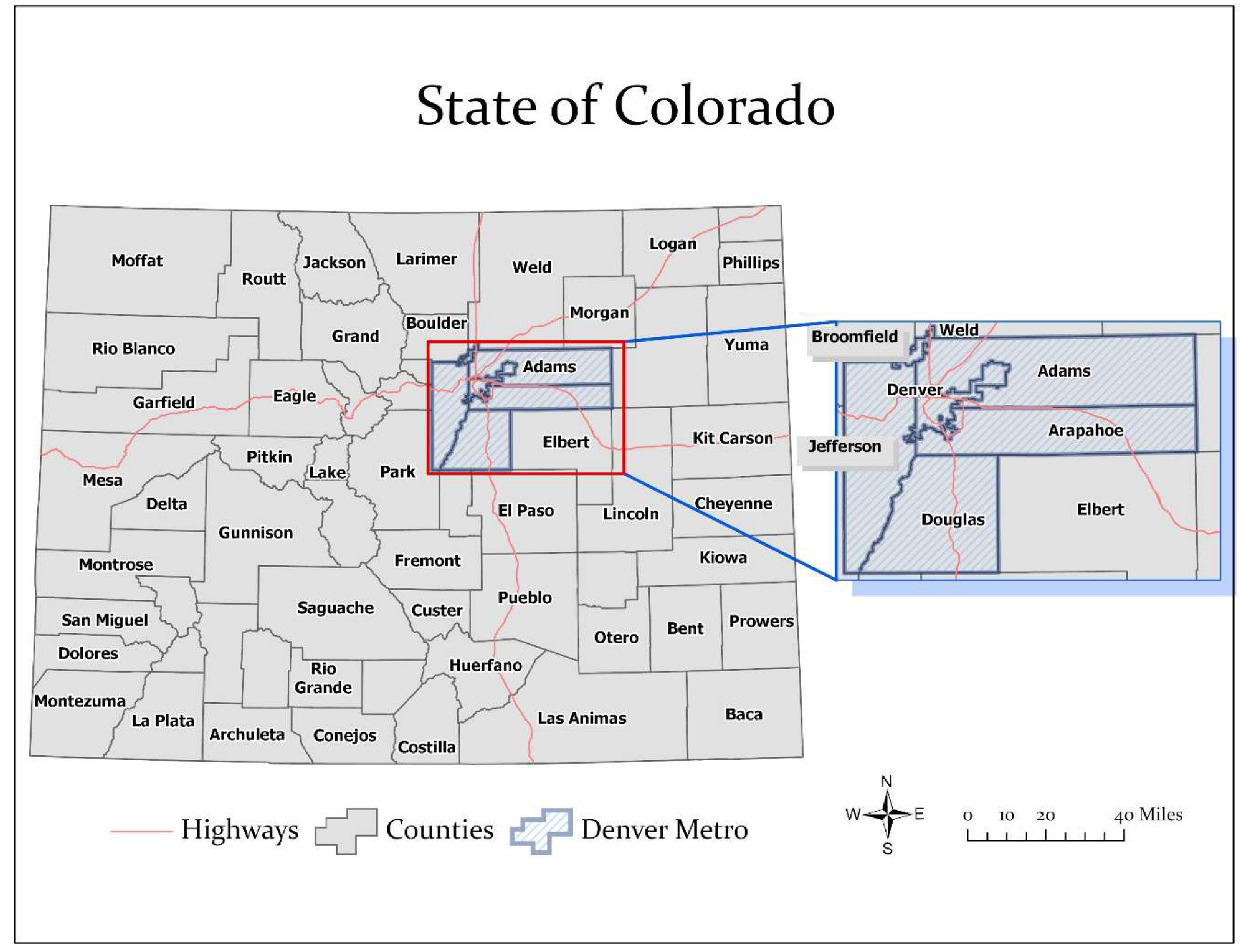
The state of Colorado has a population of 5,695,430 distributed across 64 counties, including those in the Denver metropolitan region (see
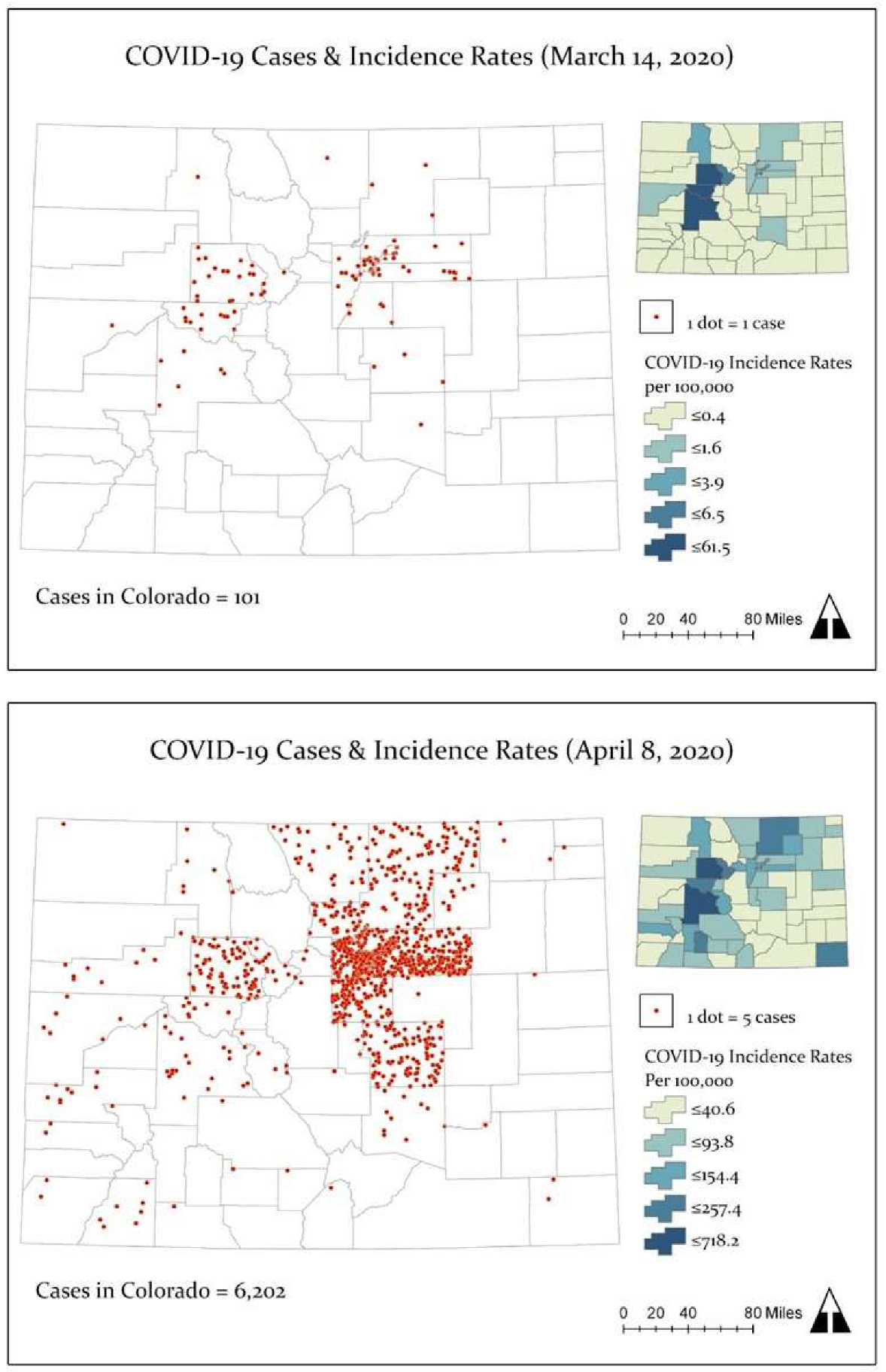
Figure 1). Dot density and choropleth maps of COVID-19 cases for March 14, 2020 and April 8, 2020 were generated in ArcGIS Pro (Esri Inc., Redlands, CA, USA) [
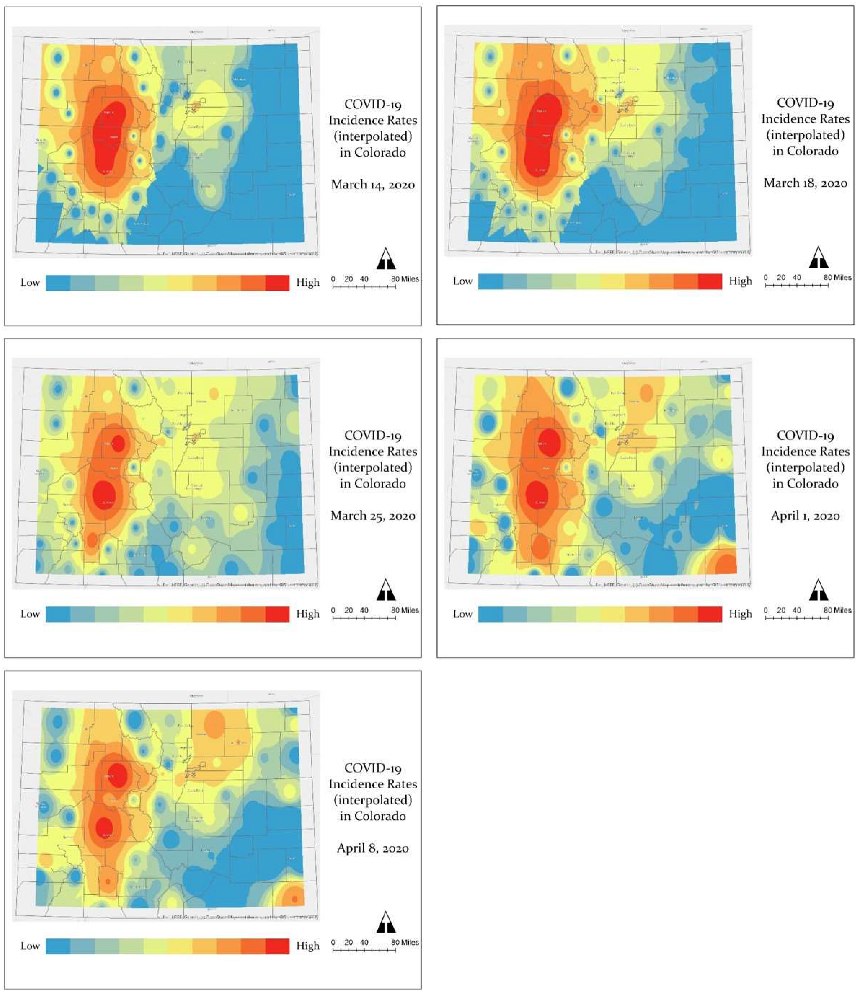
32]. An inverse distance weighted (IDW) algorithm was also used to interpolate and create a 3D continuous surface for mapping the sequential progression of COVID-19 rates across counties at five time points (March 14, March 18, March 25, April 1, and April 8). The fundamental assumption of IDW is that the interpolated surface is the result of locational dependency at the sampling points, whose influence decreases as the distance increases from its sampled location [
33]. The IDW maps represent crude hotspots of COVID-19 incidence displayed from high (red) to low (blue) rates. To estimate the change in disease incidence, rate ratios comparing county-level COVID-19 incidence rate differences between March 14 and April 8 were calculated by dividing the current rate by the older rate. The ratio represents how many times higher the current rate is compared to the older rate. COVID-19-related mortality was assessed by calculating two estimates: percent of deaths in a county relative to the total number of deaths in Colorado and case fatality rate. The latter measurement was estimated by dividing county-level cases by county-level deaths and multiplying by 100.
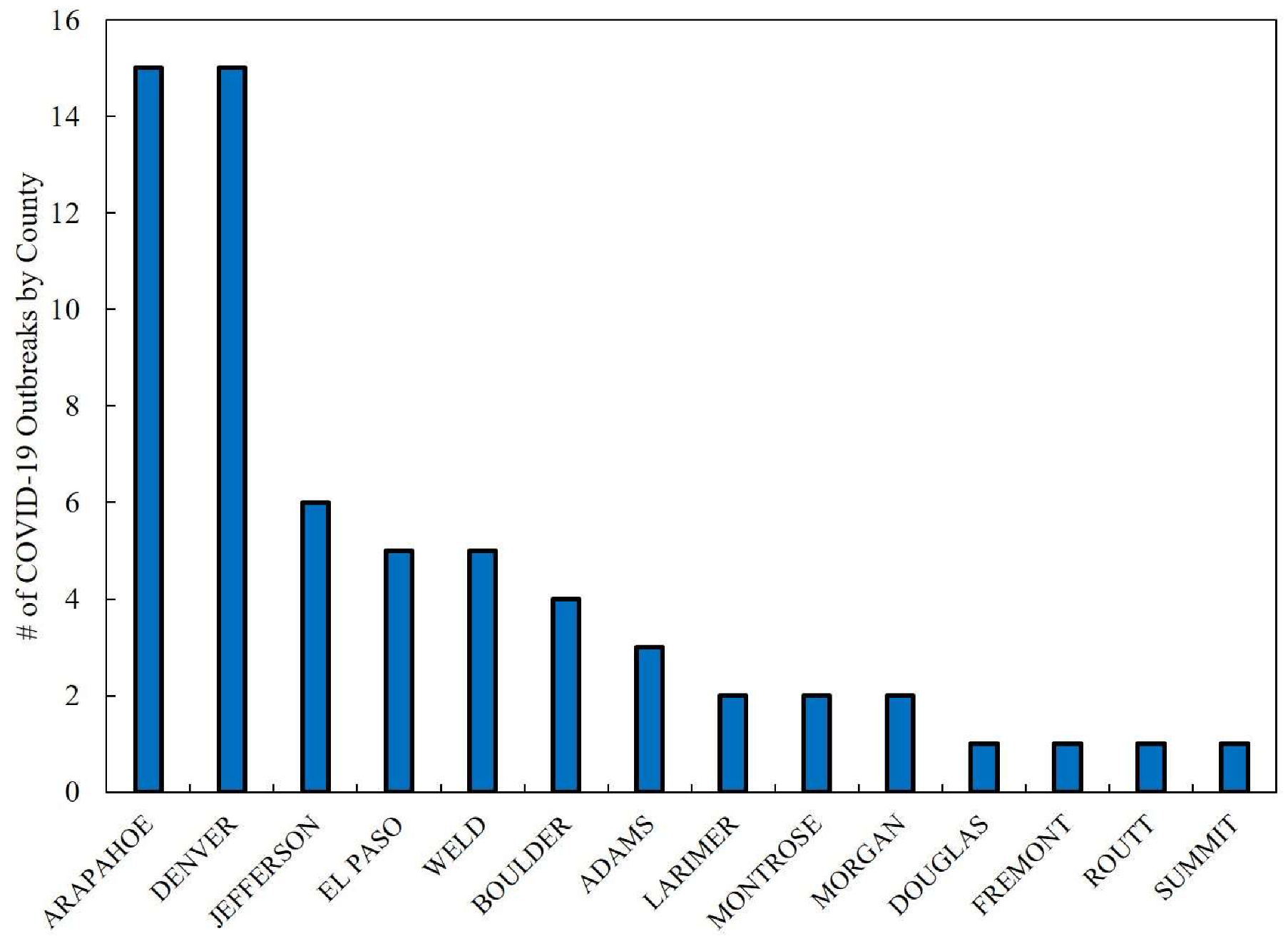
COVID-19 outbreak data [
34], which CDPHE began releasing on April 15, 2020 consisting of cases and deaths, associated with facilities by county, mainly for senior living, but also including meat-packing plants and jails, were also evaluated from March 11 to April 8.
To contextualize COVID-19 emergence, county-level profiles were generated to compare descriptively the wider social and health (i.e., chronic conditions, mainly) determinants context in Colorado. Rate ratios were calculated for each of the health outcome variables and social determinants of health indicators by dividing the county-level value by the state average. Similar profiles and rate ratios were utilized to contextualize mental health and housing disparities at the census tract-level in Colorado [
27]. Potential associations between COVID-19 incidence and death rates with social and health determinants were estimated using Pearson’s correlation in IBM-SPSS (IBM Corp., Armonk, NY, USA) [
35].
Lastly, using rate ratios described earlier, the spatial overlap of counties with several chronic conditions above the state average were compared with counties with higher rates of COVID-19 incidence.
5. Conclusions
In summary, this rapid analysis examined the geographic patterns of COVID-19 emergence during an initial period of spatial progression across counties in Colorado. From March 14 to April 8, 2020, COVID-19 incidence intensified around the first areas of detection, i.e., mountain communities and ski towns west of Denver (e.g., Eagle and Gunnison) and north and south of Denver’s metropolitan area (e.g., Weld and El Paso), and evolved into new hot spots of risk north and south of Eagle County, and in eastern Colorado. Overall the greatest increase in COVID-19 incidence rates was observed in Weld County, which reported the highest incidence rate along the Urban Front Range, even higher than counties within Denver’s metropolitan area. Weld County also had the second highest percentage of deaths in Colorado, and the greatest number of cases and deaths associated with outbreaks at many senior living facilities and a meat packing plant, in particular, where 245 persons were infected of which 6 died [
43].
A preliminary analysis of COVID-19 incidence and deaths reveals that percentage of deaths are higher along the Urban Front Range, while the rate of death (i.e., case fatality) is potentially higher in some rural counties with smaller populations. Some social and health determinant factors associated (not causal) with patterns of higher COVID-19-related death rates were population density and asthma hospitalization, suggestive of urban areas, and poverty and unemployment, suggestive of rural areas.
Although in general chronic conditions were not correlated with COVID-19 incidence, except asthma, an assessment of spatial overlap of multiple chronic conditions with COVID-19 suggests that areas of higher rates of several chronic conditions (e.g., diabetes and cancer) may potentially coincide (i.e., at the county-level) with areas of higher rates of COVID-19. In Colorado, the number of people diagnosed with multiple chronic conditions has been rising. In 2015, the prevalence of multiple chronic conditions (MCCs) among Colorado’s adult population, particularly older individuals—a growing demographic—was 35.2% [
44], an estimate significantly higher than the U.S. average (25.7%). As chronic conditions accrue, they decrease the quality of life and increase risk for mortality [
45]. For public health, this may suggest a higher number of individuals vulnerable to COVID-19 in certain counties, and draws attention to a larger syndemic health problem where synergies between COVID-19 intersect with MCCs, as well as inequality of social determinants of health.
As lockdown restrictions began to ease in Colorado in early May [
46], as well as across the U.S., the state reported 16,635 confirmed and probable cases of COVID-19, 842 deaths, and 163 outbreaks at facilities, many senior living-related, across 56 counties [
6]. Colorado at this time ranked second among states in the U.S. West in the number of cases and deaths [
7]. As the number of COVID-19 cases continue to rise, racial and ethnic disparities in COVID-19 incidence increase as well. Approximately, 45.3% of cases are Hispanics and Blacks (as of May 3), even though these communities only make up 25.6% of Colorado’s population [
6].
Although testing in Colorado has increased (as of May 3, 81,352 persons have been tested), the capacity to adequately address the pandemic in the state remains limited by supply (according to the Governor) [
47]. Colorado’s COVID-19 response is also challenged by the ability of communities to decrease exposure to COVID-19 by social distancing, an important preventive measure for respiratory diseases. According to the Colorado Health Institute [
48], which developed an index in Colorado based on overcrowding, population density, and workplace data (e.g., essential workers), the practice of social distancing is challenging for lower income persons and communities of color, including immigrants, because of crowded housing and work that requires they be present and work in close proximity to others. The Colorado Health Institute index suggests that social distancing is not only a problem for urban areas in the Denver metro, such as the suburbs of Adams County. It is also a challenge for rural communities within counties such as Weld, where there is a higher proportion of persons working in low-wage essential jobs [
48] with greater exposures to COVID-19, and the least capacities to cope with health effects (e.g., with health insurance) and the economic fallout.
This study has several limitations given the nature of a rapid study (i.e., short time frame) and the rapidly evolving context of the pandemic, which includes changes to the counts of new cases and deaths as new information updates previous daily summaries posted online. The most recent assessment of case counts in Colorado shows a difference of 26 cases between the estimate used in this study for April 8 and May 3, for example [
6]. That is approximately a 1% difference in cases. Additionally, testing is limited in Colorado, and information by county is not yet available publicly to gain a better understanding of how widespread COVID-19 was geographically. Furthermore, the study did not have access to geographic-level race/ethnicity or socioeconomic information about COVID-19 incidence. Therefore, evaluating the impact of social determinants on communities of color through correlations at the population-level is only a preliminary view. Lastly, the urban/rural differences (e.g., higher death rates and unemployment in rural areas) found in this study warrant further examination since we only analyzed county-level estimates. Conducting a finer analysis with more locally spatial information including socioeconomic and race/ethnicity data, for example, may reveal that within counties death rates are much higher in urban areas with high unemployment, poverty and other social disparities, as a recent study has shown in Massachusetts [
18]. Nevertheless, our study provides potential insights for future investigators to consider when additional COVID-19 data becomes available, including census tract-level estimates and demographic information to better understand geographic patterns and social and health risk factors.