An Exploration of Complementary Feeding Practices, Information Needs and Sources
Abstract
:1. Introduction
2. Materials and Methods
2.1. Study Design and Sample Size
2.2. Inclusion and Exclusion Criteria
2.3. Recruitment
2.4. Procedure
2.5. Materials
2.5.1. Questionnaire
2.5.2. Interview
2.6. Data Analysis
3. Results
3.1. Participant Characteristics
3.2. Current Feeding Practices in North Lanarkshire
3.2.1. Age Introduced to Solids
3.2.2. Types of Food and Drinks Given
3.2.3. Feeding Methods
3.2.4. Vitamin Supplements
3.3. Concerns of Parents in North Lanarkshire
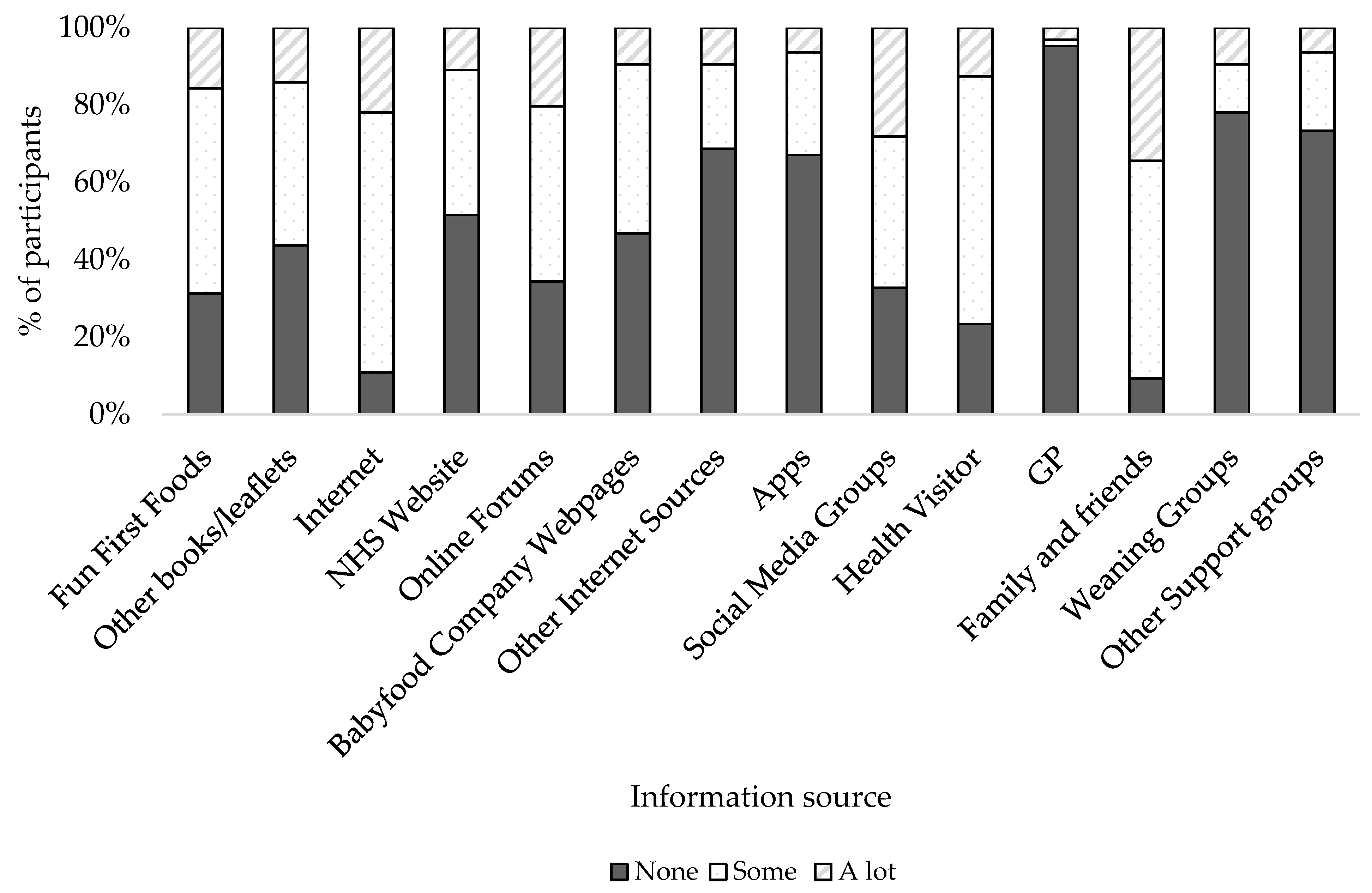
3.4. Information Sources and Needs of Parents in North Lanarkshire
Information Needs
3.5. Qualitative Data
3.5.1. Weaning Practices
Expectation vs. Reality
“at first I was really excited, and I couldn’t wait to start and sort of couldn’t wait to start him on food, he’s going love it, it’s going to be great then obviously it was really, quite a bit disheartening because he wasn’t that interested”.(P08)
“I was really excited, I love it, I love watching them try new things and see how they react. But then when you have to introduce more lumps I get apprehensive, like will he choke and all those sorts of things”.(P24)
“I wanted to wean him early… I know the guidelines is six months” (P07), or “just felt like [the infant] was ready”.
“I followed them, she was fine with her milk, she was satisfied with her milk, I didn’t feel any reason to go before the recommendations”.(P20)
“he was guzzling milk, he was up to 32oz a day”.(P25)
“she was constantly grabbing food off of everybody else, so it was like you may as well have, you may as well start having some food.”(P04)
Mothers Concerns with Child’s Eating
“until I kind of got more confident and then I started the baby-led weaning”.(P42)
“I was debating whether I was going to let her do it herself, baby-led weaning, and backed out of it because I was petrified of her choking”.(P18)
“You don’t really get information on what if they do have a severe allergy. So I’ve tried to keep the allergy foods to a minimum”,(P18)
“I introduced the same foods for a number of days to make sure there was no allergies there, especially things like strawberries and things that people are prone to have allergies”.(P07)
“Portion size and things like that I was not really too sure what to give”.(P20)
3.5.2. Information Sources and Needs
National Health Service (NHS)—The Official Advice
“I did find the NHS book quite helpful just knowing what to give, what not to give”.(P06)
“The NHS website is very up to date, but I just think there’s a wee bit of, maybe the people who are out in the community do need to catch up with the current information a wee bit because it doesn’t seem to marry up.”(P17)
“often I don’t feel like I want to phone the health visitor up just to ask about something random”.(P06)
Practical Advice
“not that there was any class that I really saw that was available to be honest, because I maybe would have considered it if there was”.(P03)
“Online videos would be really, really good. I think a lot of the time videos are good, rather than recipes.”(P16)
Need for More Information
“it’s a really big Facebook page, it’s got 2500 members and it’s all local mums that’s on it.”(P07)
“It’s easier to access as well, its quicker to access information online than it is to contact a health professional about it and wait until they get back to you”.(P17)
“it was more inspiration around meals, what they should be getting, initial foods that you should introduce them to, to begin with and they how to kind of build that in”.(P26)
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Acknowledgments
Conflicts of Interest
References
- Scientific Advisory Committee on Nutrition. Feeding in the First Year of Life; Public Health England: London, UK, 2018.
- Fewtrell, M.; Bronsky, J.; Campoy, C.; Domellof, M.; Embleton, N.; Fidler Mis, N.; Hojsak, I.; Hulst, J.M.; Indrio, F.; Lapillonne, A.; et al. Complementary Feeding: A Position Paper by the European Society for Paediatric Gastroenterology, Hepatology, and Nutrition (ESPGHAN) Committee on Nutrition. J. Pediatr. Gastroenterol. Nutr. 2017, 64, 119–132. [Google Scholar] [CrossRef] [PubMed]
- Muraro, A.; Halken, S.; Arshad, S.H.; Beyer, K.; Dubois, A.E.; Du Toit, G.; Eigenmann, P.A.; Grimshaw, K.E.; Hoest, A.; Lack, G.; et al. EAACI food allergy and anaphylaxis guidelines. Primary prevention of food allergy. Allergy 2014, 69, 590–601. [Google Scholar] [CrossRef] [PubMed]
- Agostoni, C.; Decsi, T.; Fewtrell, M.; Goulet, O.; Kolacek, S.; Koletzko, B.; Michaelsen, K.F.; Moreno, L.; Puntis, J.; Rigo, J.; et al. Complementary feeding: A commentary by the ESPGHAN Committee on Nutrition. J. Pediatr. Gastroenterol. Nutr. 2008, 46, 99–110. [Google Scholar] [CrossRef] [PubMed]
- Garcia, A.L.; Raza, S.; Parrett, A.; Wright, C.M. Nutritional content of infant commercial weaning foods in the UK. Arch. Dis. Child. 2013, 98, 793–797. [Google Scholar] [CrossRef] [PubMed]
- McAndrew, F.; Thompson, J.; Fellows, L.; Large, A.; Speed, M.; Renfrew, M. Infant Feeding Survey 2010; Health and Scocial Care Inforamtion Centre: Leeds, UK, 2012. [Google Scholar]
- The Scottish Government. Scottish Maternal and Infant Nutrition Survey 2017; The Scottish Government: Edinburgh, UK, 2018.
- Loudon, K.; Buchanan, S.; Ruthven, I. The everyday life information seeking behaviours of first-time mothers. J. Doc. 2016, 72, 24–46. [Google Scholar] [CrossRef]
- The Scottish Government. Having a Baby in Scotland 2013: Women’s Experiences of Maternity Care; The Scottish Government: Edinburgh, UK, 2014.
- Harrison, M.; Brodribb, W.; Hepworth, J. A qualitative systematic review of maternal infant feeding practices in transitioning from milk feeds to family foods. Matern. Child Nutr. 2017, 13, e12360. [Google Scholar] [CrossRef] [PubMed]
- Tully, L.; Wright, C.M.; McCormick, D.; Garcia, A.L. Assessing the Potential for Integrating Routine Data Collection on Complementary Feeding to Child Health Visits: A Mixed-Methods Study. Int. J. Environ. Res. Public Health 2019, 16, 1722. [Google Scholar] [CrossRef]
- Bryman, A. Social Research Methods, 3rd ed.; Oxford University Press: Oxford, UK, 2008. [Google Scholar]
- The Scottish Government. SIMD ranks and domain ranks. In The Scottish Indicator of Multiple Deprivation; The Scottish Government: Edinburgh, UK, 2016. [Google Scholar]
- Doub, A.E.; Moding, K.J.; Stifter, C.A. Infant and maternal predictors of early life feeding decisions. The timing of solid food introduction. Appetite 2015, 92, 261–268. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Taylor, C.M.; Wernimont, S.M.; Northstone, K.; Emmett, P.M. Picky/fussy eating in children: Review of definitions, assessment, prevalence and dietary intakes. Appetite 2015, 95, 349–359. [Google Scholar] [CrossRef] [Green Version]
- Nicklaus, S. Children’s acceptance of new foods at weaning. Role of practices of weaning and of food sensory properties. Appetite 2011, 57, 812–815. [Google Scholar] [CrossRef]
- Caton, S.J.; Blundell, P.; Ahern, S.M.; Nekitsing, C.; Olsen, A.; Moller, P.; Hausner, H.; Remy, E.; Nicklaus, S.; Chabanet, C.; et al. Learning to eat vegetables in early life: The role of timing, age and individual eating traits. PLoS ONE 2014, 9, e97609. [Google Scholar] [CrossRef] [PubMed]
- Brown, A.; Jones, S.W.; Rowan, H. Baby-Led Weaning: The Evidence to Date. Curr. Nutr. Rep. 2017, 6, 148–156. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Brown, A.; Lee, M. An exploration of experiences of mothers following a baby-led weaning style: Developmental readiness for complementary foods. Matern. Child Nutr. 2013, 9, 233–243. [Google Scholar] [CrossRef] [PubMed]
- Brown, A.; Lee, M. A descriptive study investigating the use and nature of baby-led weaning in a UK sample of mothers. Matern. Child Nutr. 2011, 7, 34–47. [Google Scholar] [CrossRef] [PubMed]
- Cameron, S.L.; Heath, A.L.; Taylor, R.W. Healthcare professionals’ and mothers’ knowledge of, attitudes to and experiences with, Baby-Led Weaning: A content analysis study. BMJ Open 2012, 2, e001542. [Google Scholar] [CrossRef] [PubMed]
- Michie, S.; Yardley, L.; West, R.; Patrick, K.; Greaves, F. Developing and Evaluating Digital Interventions to Promote Behavior Change in Health and Health Care: Recommendations Resulting From an International Workshop. J. Med. Internet Res. 2017, 19, e232. [Google Scholar] [CrossRef] [PubMed]
- Russell, S. Netmums: Online support for parents. Community Pract. J. Community Pract. Health Visit. Assoc. 2006, 79, 44–45. [Google Scholar]
- Bentley, J.P.; Bond, D.; de Vroome, M.; Yip, E.; Nassar, N. Factors Associated with Recurrent Infant Feeding Practices in Subsequent Births. J. Hum. Lact. Off. J. Int. Lact. Consult. Assoc. 2016, 32, 721–729. [Google Scholar] [CrossRef] [PubMed]
| Parents | n (%) |
|---|---|
| SIMD | |
| Quintile 1 | 16 (25) |
| Quintile 2 | 17 (27) |
| Quintile 3 | 12 (19) |
| Quintile 4 | 11 (17) |
| Quintile 5 | 8 (13) |
| First-time parent (% yes) | 40 (63) |
| Mother | |
| Education level * | |
| Low | 4 (6) |
| Medium | 16 (25) |
| High | 42 (66) |
| Father | |
| Education level ** | |
| Low | 9 (14) |
| Medium | 21 (33) |
| High | 24 (38) |
| Times/Week | Meat/Fish/Eggs | Commercial Baby Food | Green Leafy Vegetables | Sour Fruit | Other Fruit | Sweet Snacks |
|---|---|---|---|---|---|---|
| 0 | 24 (38%) | 18 (28%) | 10 (15%) | 26 (41%) | 7 (11%) | 41 (64%) |
| 1 | 4 (6%) | 4 (6%) | 3 (5%) | 6 (9%) | 2 (3%) | 3 (5%) |
| 2–4 | 14 (22%) | 14 (22%) | 20 (31%) | 20 (31%) | 19 (30%) | 13 (20%) |
| 5–6 | 7 (11%) | 7 (11%) | 8 (13%) | 3 (5%) | 12 (19%) | 4 (6%) |
| 7+ | 15 (23%) | 21 (33%) | 23 (36%) | 9 (14%) | 24 (37%) | 3 (5%) |
| Breast Milk | Formula Milk | Cow’s Milk | Diluting Juice | Water | Other | |
| 0 | 55 (86%) | 9 (14%) | 60 (94%) | 53 (83%) | 13 (20%) | 63 (98%) |
| 1–2 | 2 (3%) | 7 (11%) | 3 (5%) | 8 (13%) | 25 (39%) | 1 (2%) |
| 3–4 | 0 (0%) | 29 (45%) | 1 (1%) | 1 (1%) | 21 (33%) | 0 (0%) |
| 5+ | 7 (11%) | 19 (30%) | 0 (0%) | 2 (3%) | 5 (8%) | 0 (0%) |
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Garcia, A.L.; Looby, S.; McLean-Guthrie, K.; Parrett, A. An Exploration of Complementary Feeding Practices, Information Needs and Sources. Int. J. Environ. Res. Public Health 2019, 16, 4311. https://doi.org/10.3390/ijerph16224311
Garcia AL, Looby S, McLean-Guthrie K, Parrett A. An Exploration of Complementary Feeding Practices, Information Needs and Sources. International Journal of Environmental Research and Public Health. 2019; 16(22):4311. https://doi.org/10.3390/ijerph16224311
Chicago/Turabian StyleGarcia, Ada L., Sarah Looby, Kimberley McLean-Guthrie, and Alison Parrett. 2019. "An Exploration of Complementary Feeding Practices, Information Needs and Sources" International Journal of Environmental Research and Public Health 16, no. 22: 4311. https://doi.org/10.3390/ijerph16224311
APA StyleGarcia, A. L., Looby, S., McLean-Guthrie, K., & Parrett, A. (2019). An Exploration of Complementary Feeding Practices, Information Needs and Sources. International Journal of Environmental Research and Public Health, 16(22), 4311. https://doi.org/10.3390/ijerph16224311






