Integrating Public Health into Climate Change Policy and Planning: State of Practice Update
Abstract
1. Introduction
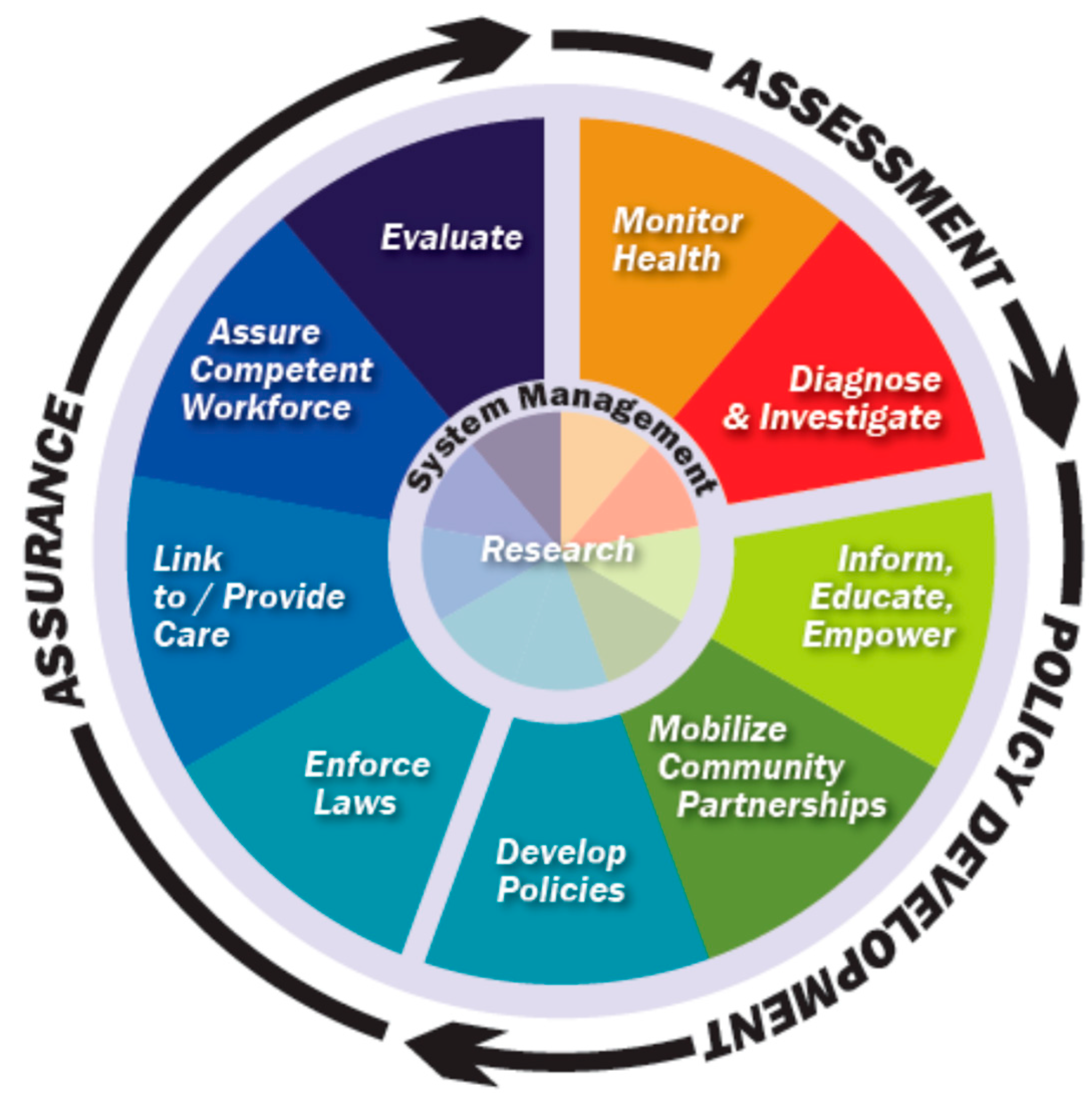
Approach
2. Results
2.1. Assessment
2.1.1. Monitor Health
Exposure to Climate Hazards
Vulnerability
Disease Surveillance
2.1.2. Investigate and Diagnose
2.2. Policy Development
2.2.1. Inform, Educate, Empower
2.2.2. Mobilize Partnerships
Coordinate across Government Levels
Collaborate across Public Health and Non-Health Sectors
Non-Government Partnerships
2.2.3. Develop Policies
Mitigation
Adaptation
2.3. Assurance
2.3.1. Enforce Laws and Regulations
2.3.2. Link to and Provide Care
2.3.3. Assure Competent Workforce
2.3.4. Evaluate
2.4. Research
3. Discussion
4. Conclusions
Author Contributions
Funding
Conflicts of Interest
References
- Ebi, K.L.; Ogden, N.H.; Semenza, J.C.; Woodward, A. Detecting and Attributing Health Burdens to Climate Change. Environ. Health Perspect. 2017, 125, 085004. [Google Scholar] [CrossRef]
- Watts, N.; Amann, M.; Ayeb-Karlsson, S.; Belesova, K.; Bouley, T.; Boykoff, M.; Byass, P.; Cai, W.; Campbell-Lendrum, D.; Chambers, J.; et al. The Lancet Countdown on health and climate change: From 25 years of inaction to a global transformation for public health. Lancet 2018, 391, 581–630. [Google Scholar] [CrossRef]
- Bulletin of the American Meteorological Society (BAMS). Explaining Extreme Events of 2017 from a Climate Perspective. 2018. Available online: https://www.ametsoc.org/ams/index.cfm/publications/bulletin-of-the-american-meteorological-society-bams/explaining-extreme-events-from-a-climate-perspective/ (accessed on 13 June 2019).
- Watts, J. World is Finally Waking up to Climate Change, Says ‘Hothouse Earth’ Author. The Guardian. 19 August 2018. Available online: https://www.theguardian.com/environment/2018/aug/17/world-waking-up-to-reality-climate-change-hothouse-earth-author (accessed on 13 June 2019).
- Intergovernmental Panel on Climate Change (IPCC). Summary for Policymakers. In Global Warming of 1.5 °C; An IPCC Special Report on the impacts of global warming of 1.5 °C above pre-industrial levels and related global greenhouse gas emission pathways, in the context of strengthening the global response to the threat of climate change, sustainable development, and efforts to eradicate poverty; Masson-Delmotte, V., Zhai, P., Pörtner, H.-O., Roberts, D., Skea, J., Shukla, P.R., Pirani, A., Moufouma-Okia, Péan, C., Pidcock, R., et al., Eds.; World Meteorological Organization: Geneva, Switzerland, 2018; p. 32. Available online: https://www.ipcc.ch/sr15/chapter/summary-for-policy-makers/ (accessed on 12 March 2019).
- Berry, P.; Enright, P.M.; Shumake-Guillemot, J.; Villalobos-Prats, E.; Campbell-Lendrum, D. Assessing Health Vulnerabilities and Adaptation to Climate Change: A Review of International Progress. Int. J. Environ. Res. Public Health 2018, 15, 2626. [Google Scholar] [CrossRef]
- Barata, M.; Ligeti, E.; De Simone, G.; Dickinson, T.; Jack, D.; Penney, J.; Rahman, M.; Zimmerman, R. Climate change and human health in cities. In Climate Change and Cities: First Assessment Report of the Urban Climate Change Research Network; Rosenzweig, C., Solecki, W.D., Hammer, S.A., Mehrotra, S., Eds.; Cambridge University Press: Cambridge, UK, 2011; Available online: http://uccrn.org/files/2014/02/ARC3-Chapter-7.pdf (accessed on 10 February 2017).
- Woodward, A.J.; Samet, J.M. Climate Change, Hurricanes, and Health. Am. J. Public Health 2018, 108, 33–35. [Google Scholar] [CrossRef]
- Georgeson, L.; Maslin, M.; Poessinouw, M.; Howard, S. Adaptation responses to climate change differ between global megacities. Nat. Clim. Chang. 2016, 6, 584–588. [Google Scholar] [CrossRef]
- Aylett, A. Institutionalizing the urban governance of climate change adaptation: Results of an international survey. Urban Clim. 2015, 14, 4–16. [Google Scholar] [CrossRef]
- Araos, M.; Austin, S.E.; Berrang-Ford, L.; Ford, J.D. Public Health Adaptation to Climate Change in Large Cities: A Global Baseline. Int. J. Health Serv. 2016, 46, 53–78. [Google Scholar] [CrossRef]
- World Health Organization. Climate Change and Health: Key Facts. Available online: http://www.who.int/mediacentre/factsheets/fs266/en/ (accessed on 8 January 2019).
- Watts, N.; Adger, W.N.; Ayeb-Karlsson, S.; Bai, Y.; Byass, P.; Campbell-Lendrum, D.; Colburn, T.; Cox, P.M.; Depledge, M.; Depoux, A.; et al. The Lancet Countdown: Tracking progress on health and climate change. Lancet 2017, 389, 1151–1164. [Google Scholar] [CrossRef]
- Austin, S.E.; Biesbroek, R.; Berrang-Ford, L.; Ford, J.D.; Parker, S.; Fleury, M.D. Public Health Adaptation to Climate Change in OECD Countries. Int. J. Environ. Res. Public Health 2016, 13, 889. [Google Scholar] [CrossRef]
- Workman, A.; Blashki, G.; Bowen, K.J.; Karoly, D.J.; Wiseman, J. The Political Economy of Health Co-Benefits: Embedding Health in the Climate Change Agenda. Int. J. Environ. Res. Public Health 2018, 15, 674. [Google Scholar] [CrossRef]
- Frumkin, H.; Hess, J.; Luber, G.; Malilay, J.; McGeehin, M. Climate change: The public health response. Am. J. Public Health 2008, 98, 435–445. [Google Scholar] [CrossRef]
- Institute of Medicine. The Future of Public Health; The National Academies Press: Washington, DC, USA, 1988. [Google Scholar] [CrossRef]
- Centers for Disease Control and Prevention (CDC). United States Public Health 101. Available online: https://www.cdc.gov/stltpublichealth/publichealthservices/pdf/usph101.pdf (accessed on 12 March 2019).
- Novick, L.F.; Morrow, C.B. A Framework for Public Health Administration and Practice. In Public Health Administration: Principles for Population-Based Management; Novick, L.F., Morrow, C.B., Mays, G.P., Eds.; Jones and Bartlett Publishers: Sudbury, MA, USA, 2008. [Google Scholar]
- Centers for Disease Control and Prevention. CDC’s Climate and Health Program. Available online: https://www.cdc.gov/nceh/information/climate_and_health.htm (accessed on 12 March 2019).
- Marinucci, G.D.; Luber, G.; Uejio, C.K.; Saha, S.; Hess, J.J. Building Resilience against Climate Effects—A Novel Framework to Facilitate Climate Readiness in Public Health Agencies. Int. J. Environ. Res. Public Health 2014, 11, 6433–6458. [Google Scholar] [CrossRef]
- Sheehan, M.C.; Fox, M.A.; Kaye, C.H.; Resnick, B. Integrating health into local climate response: Lessons from the US CDC Climate-Ready States and Cities Initiative. Environ. Health Perspect. 2017, 125, 094501. [Google Scholar] [CrossRef]
- Wheeler, N.; Watts, N. Climate Change: From Science to Practice. Curr. Environ. Health Rep. 2018, 5, 170–178. [Google Scholar] [CrossRef]
- Centers for Disease Control and Prevention (CDC). The 10 Essential Public Health Services Figure. Available online: https://www.cdc.gov/stltpublichealth/publichealthservices/essentialhealthservices.html (accessed on 3 October 2018).
- World Meteorological Organization. Global Framework for Climate Services. 2018. Available online: http://www.wmo.int/gfcs/ (accessed on 8 January 2019).
- Jancloes, M.; Anderson, V.; Gosselin, P.; Mee, C.; Chong, N.J. WWOSC 2014: Research needs for better health resilience to weather hazards. Int. J. Environ. Res. Public Health 2015, 12, 2895–2900. [Google Scholar] [CrossRef]
- Georgeson, L.; Maslin, M.; Poessinouw, M. Global disparity in the supply of commercial weather and climate information services. Sci. Adv. 2017, 3, e1602632. [Google Scholar] [CrossRef]
- Climate Data Factory. Ready to Use Future Climate Information. Available online: https://theclimatedatafactory.com/ (accessed on 12 March 2019).
- Kickbusch, I. Global Health Governance Challenges 2016—Are We Ready? Int. J. Health Policy Manag. 2016, 5, 349–353. [Google Scholar] [CrossRef]
- English, P.B.; Richardson, M.J. Components of Population Vulnerability and Their Relationship With Climate-Sensitive Health Threats. Curr. Environ. Health Rep. 2016, 3, 91–98. [Google Scholar] [CrossRef]
- Mayhew, S.; Hanefeld, J. Planning adaptive health systems: The climate challenge. Lancet Glob. Health 2014, 2, e625–e626. [Google Scholar] [CrossRef]
- Manangan, A.P.; Uejio, C.K.; Saha, S.; Schramm, P.J.; Marinucci, G.D.; Brown, C.L.; Hess, J.J.; Luber, G. Assessing Health Vulnerability to Climate Change: A Guide for Health Departments; Climate and Health Technical Report Series Climate and Health Program; Centers for Disease Control and Prevention, US CDC. Available online: https://www.cdc.gov/climateandhealth/pubs/assessinghealthvulnerabilitytoclimatechange.pdf (accessed on 12 March 2019).
- United States Global Change Research Program (US GCRP). Health. 2016. Available online: https://health2016.globalchange.gov/ (accessed on 8 January 2019).
- Wolf, M.; Comerford, C. 2014—San Francisco Climate & Health Profile, San Francisco Department of Public Health Climate and Health Program. Available online: https://sfclimatehealth.org/wp-content/uploads/2018/12/SFDPH_ClimateHealthProfile_FinalDraft.pdf (accessed on 13 June 2019).
- University of Notre Dame. Global Adaptation Initiative (GAIN). Available online: https://gain.nd.edu/ (accessed on 19 March 2019).
- Preston, B.L.; Yuen, E.J.; Westaway, R.M. Putting vulnerability to climate change on the map: A review of approaches, benefits, and risks. Sustain. Sci. 2011, 6, 177–202. [Google Scholar] [CrossRef]
- Bao, J.; Li, X.; Yu, C. The construction and validation of the heat vulnerability index, a review. Int. J. Environ. Res. Public Health 2015, 12, 7220–7234. [Google Scholar] [CrossRef] [PubMed]
- Bakkensen, L.A.; Fox-Lent, C.; Read, L.K.; Linkov, I. Validating Resilience and Vulnerability Indices in the Context of Natural Disasters. Risk Anal. 2018, 37, 982–1004. [Google Scholar] [CrossRef] [PubMed]
- Centers for Disease Control and Prevention (CDC). National Environmental Public Health Tracking Program Data Explorer. Available online: https://ephtracking.cdc.gov/DataExplorer/#/ (accessed on 13 June 2019).
- Moulton, A.D.; Schramm, P.J. Climate Change and Public Health Surveillance: Toward a Comprehensive Strategy. J. Public Health Manag. Pract. 2017, 23, 618. [Google Scholar] [CrossRef] [PubMed]
- Houghton, A.; English, P. An approach to developing local climate change environmental public health indicators, vulnerability assessments, and projections of future impacts. J. Environ. Public Health 2014, 132057. [Google Scholar] [CrossRef] [PubMed]
- Wilder-Smith, A.; Tissera, H.; AbuBakar, S.; Kittayapong, P.; Logan, J.; Neumayr, A.; Rocklöv, J.; Byass, P.; Louis, V.R.; Tozan, Y.; et al. Novel tools for the surveillance and control of dengue: Findings by the Dengue Tools research consortium. Glob. Health Action 2018, 11, 1. [Google Scholar] [CrossRef]
- Tsai, S.; Hamby, T.; Chu, A.; Gleason, J.A.; Goodrow, G.M.; Gu, H.; Lifshitz, E.; Fagliano, J.A. Development and Application of Syndromic Surveillance for Severe Weather Events Following Hurricane Sandy. Disaster Med. Public Health Prep. 2016, 10, 463–471. [Google Scholar] [CrossRef]
- Ebi, K.L.; Berry, P.; Hayes, K.; Boyer, C.; Sellers, S.; Enright, P.M.; Hess, J.J. Stress Testing the Capacity of Health Systems to Manage Climate Change-Related Shocks and Stresses. Int. J. Environ. Res. Public Health 2018, 15, 2370. [Google Scholar] [CrossRef]
- Erwin, P.C.; Brownson, R.C. Macro trends and the future of public health practice. Annu. Rev. Public Health 2017, 38, 393–412. [Google Scholar] [CrossRef]
- Morano, L.H.; Watkins, S. Evaluation of diagnostic codes in morbidity and mortality data sources for heat-related illness surveillance. Public Health Rep. 2017, 132, 326–335. [Google Scholar] [CrossRef]
- Reis, S.; Morris, G.; Fleming, L.E.; Beck, S.; Taylor, T.; White, M.; Depledge, M.H.; Steinle, S.; Sabel, C.E.; Cowie, H.; et al. Integrating health and environmental impact analysis. Public Health 2015, 129, 1383–1389. [Google Scholar] [CrossRef]
- Hess, J.J.; Eidson, M.; Tlumak, J.E.; Raab, K.K.; Luber, G. An Evidence-Based Public Health Approach to Climate Change Adaptation. Environ. Health Perspect. 2014, 122, 1177–1186. [Google Scholar] [CrossRef] [PubMed]
- Gallina, V.; Torresan, S.; Critto, A.; Sperotto, A.; Glade, T.; Marcomini, A. A review of multi-risk methodologies for natural hazards: Consequences and challenges for a climate change impact assessment. J. Environ. Manag. 2016, 168, 123–132. [Google Scholar] [CrossRef] [PubMed]
- Sperotto, A.; Molina, J.L.; Torresan, S.; Critto, A.; Marcomini, A. Reviewing bayesian networks potentials for climate change impacts assessment and management: A multi-risk perspective. J. Environ. Manag. 2017, 202, 320–331. [Google Scholar] [CrossRef] [PubMed]
- Landis, W.G.; Durda, J.L.; Brooks, M.L.; Chapman, P.M.; Menzie, C.A.; Stahl, R.G., Jr.; Stauber, J.L. Ecological risk assessment in the context of global climate change. Environ. Toxicol. Chem. 2013, 32, 79–92. [Google Scholar] [CrossRef] [PubMed]
- Hess, J.J.; McDowell, J.Z.; Luber, G. Integrating climate change adaptation into public health practice: Using adaptive management to increase adaptive capacity and build resilience. Environ. Health Perspect. 2012, 120, 171–179. [Google Scholar] [CrossRef] [PubMed]
- Whicker, J.J.; Janecky, D.R.; Doerr, T.B. Adaptive management: A paradigm for remediation of public facilities following a terrorist attack. Risk Anal. 2008, 28, 1445–1456. [Google Scholar] [CrossRef] [PubMed]
- European Commission and European Environment Agency. Climate-ADAPT. Available online: https://climate-adapt.eea.europa.eu/ (accessed on 19 March 2019).
- WHO. Health Impact Assessment. 2019. Available online: https://www.who.int/hia/tools/process/en/ (accessed on 8 January 2019).
- Brown, H.L.; Proust, K.; Spickett, J.; Capon, A. The potential role of health impact assessment in tackling the complexity of climate change adaptation for health. Health Promot. J. Austr. 2011, 22, S48–S53. [Google Scholar] [CrossRef] [PubMed]
- American Public Health Association (APHA). Health in All Policies: A Guide for State and Local Governments. 2013. Available online: https://www.apha.org/topics-and-issues/health-in-all-policies (accessed on 19 March 2019).
- Brown, H.; Spickett, J.; Katscherian, D. A health impact assessment framework for assessing vulnerability and adaptation planning for climate change. Int. J. Environ. Res. Public Health 2014, 11, 12896–12914. [Google Scholar] [CrossRef]
- Akerlof, K.; DeBono, R.; Berry, P.; Leiserowitz, A.; Roser-Renouf, C.; Clarke, K.L.; Rogaeva, A.; Nisbet, M.C.; Weathers, M.R.; Maibach, E.W. Public perceptions of climate change as a human health risk: Surveys of the United States, Canada and Malta. Int. J. Environ. Res. Public Health 2010, 7, 2559–2606. [Google Scholar] [CrossRef]
- Maibach, E.W.; Kreslake, J.M.; Roser-Renouf, C.; Rosenthal, S.; Feinberg, G.; Leiserowitz, A.A. Do Americans understand that global warming is harmful to human health? Evidence from a national survey. Ann. Glob. Health 2015, 81, 396–409. [Google Scholar] [CrossRef]
- Hathaway, J.; Maibach, E.W. Health Implications of Climate Change: A Review of the Literature About the Perception of the Public and Health Professionals. Curr. Environ. Health Rep. 2018, 5, 197–204. [Google Scholar] [CrossRef] [PubMed]
- Ziegler, C.; Morelli, V.; Fawibe, O. Climate Change and Underserved Communities. Prim. Care 2017, 44, 171–184. [Google Scholar] [CrossRef] [PubMed]
- Kreslake, J.M.; Price, K.M.; Sarfaty, M. Developing effective communication materials on the health effects of climate change for vulnerable groups: A mixed methods study. BMC Public Health 2016, 16, 946. [Google Scholar] [CrossRef] [PubMed]
- Depoux, A.; Hémono, M.; Puig-Malet, S.; Pédron, R.; Flahault, A. Communicating climate change and health in the media. Public Health Rev. 2017, 38, 7. [Google Scholar] [CrossRef] [PubMed]
- Amelung, D.; Fischer, H.; Kruse, L.; Sauerborn, R. Defogging Climate Change Communication: How Cognitive Research Can Promote Effective Climate Communication. Front. Psychol. 2016, 7, 1340. [Google Scholar] [CrossRef]
- Chadwick, A.E. Climate change, health, and communication: A primer. Health Commun. 2016, 31, 782–785. [Google Scholar] [CrossRef]
- Dervin, K.; Rudolph, L. Workshop Executive Summary: Climate Change and Health Communications; Center for Climate Change and Health: Oakland, CA, USA, 2015; Available online: http://usclimateandhealthalliance.org/wp-content/uploads/2016/06/ClimateChangeHealthCommunication2016.pdf (accessed on 19 March 2019).
- Zia, A.; Todd, A.M. Evaluating the effects of ideology on public understanding of climate change science: How to improve communication across ideological divides? Public Underst. Sci. 2010, 19, 743–761. [Google Scholar] [CrossRef]
- Leas, E.C.; Althouse, B.M.; Dredze, M.; Obradovich, N.; Fowler, J.H.; Noar, S.M.; Allem, J.-P.; Ayers, J.W. Big data sensors of organic advocacy: The case of Leonardo DiCaprio and climate change. PLoS ONE 2016, 11, e0159885. [Google Scholar] [CrossRef]
- Bulkeley, H. Cities and the Governing of Climate Change. Annu. Rev. Environ. Resour. 2010, 35, 229–253. [Google Scholar] [CrossRef]
- Austin, S.E.; Ford, J.D.; Berrang-Ford, L.; Araos, M.; Parker, S.; Fleury, M.D. Public health adaptation to climate change in Canadian jurisdictions. Int. J. Environ. Res. Public Health 2015, 12, 623–651. [Google Scholar] [CrossRef]
- Bowen, K.J.; Ebi, K.; Friel, S.; McMichael, A.J. A multi-layered governance framework for incorporating social science insights into adapting to the health impacts of climate change. Glob. Health Action 2013, 10, 21820. [Google Scholar] [CrossRef] [PubMed]
- United States Global Change Research Program. National Climate Assessment. Available online: https://nca2014.globalchange.gov/ (accessed on 19 March 2019).
- Lane, K.; Charles-Guzman, K.; Wheeler, K.; Abid, Z.; Graber, N.; Matte, T. Health effects of coastal storms and flooding in urban areas: A review and vulnerability assessment. J. Environ. Public Health 2013, 2013, 913064. [Google Scholar] [CrossRef] [PubMed]
- Bowen, K.J.; Ebi, K.L. Health risks of climate change in the World Health Organization South-East Asia Region. WHO South East Asia J. Public Health 2017, 6, 3–8. [Google Scholar] [CrossRef] [PubMed]
- Patz, J.A.; Grabow, M.L.; Limaye, V.S. When It Rains, It Pours: Future Climate Extremes and Health. Ann. Glob. Health 2014, 80, 332–344. [Google Scholar] [CrossRef] [PubMed]
- McCarney, P.; Blanco, H.; Carmin, J.; Colley, M. Cities and climate change. In Climate Change and Cities: First Assessment Report of the Urban Climate Change Research Network; Rosenzweig, C., Solecki, W.D., Hammer, S.A., Mehrotra, S., Eds.; Cambridge University Press: Cambridge, UK, 2011; pp. 249–269. Available online: http://uccrn.org/files/2014/02/ARC3-Chapter-9.pdf (accessed on 8 January 2019).
- Conlon, K.C.; Kintziger, K.W.; Jagger, M.; Stefanova, L.; Uejio, C.K.; Konrad, C. Working with Climate Projections to Estimate Disease Burden. Int. J. Environ. Res. Public Health 2016, 13, 804. [Google Scholar] [CrossRef] [PubMed]
- Machalaba, C.; Romanelli, C.; Stoett, P.; Baum, S.E.; Bouley, T.A.; Daszak, P.; Karesh, W.B. Climate Change and Health: Transcending Silos to Find Solutions. Ann. Glob. Health 2015, 81, 445–458. [Google Scholar] [CrossRef] [PubMed]
- U.S. Climate Resilience Toolkit. Iñupiat Work to Preserve Food and Traditions on Alaska’s North Slope. Available online: https://toolkit.climate.gov/case-studies/i%C3%B1upiat-work-preserve-food-and-traditions-alaskas-north-slope (accessed on 19 March 2019).
- U.S. Climate Resilience Toolkit. Students Promote Flood Resilience and Reduce Insurance Costs. Available online: https://toolkit.climate.gov/case-studies/students-promote-flood-resilience-and-reduce-insurance-costs (accessed on 19 March 2019).
- Gao, J.; Kovats, S.; Vardoulakis, S.; Wilkinson, P.; Woodward, A.; Li, J.; Gu, S.; Liu, X.; Wu, H.; Wang, J.; et al. Public health co-benefits of greenhouse gas emissions reduction: A systematic review. Sci. Total Environ. 2018, 627, 388–402. [Google Scholar] [CrossRef]
- Markandya, A.; Sampedro, J.; Smith, S.J.; Van Dingenen, R.; Pizarro-Irizar, C.; Arto, I.; González-Eguino, M. Health co-benefits from air pollution and mitigation costs of the Paris Agreement: A modelling study. Lancet Planet. Health 2018, 2, e126–133. [Google Scholar] [CrossRef]
- De Nazelle, A.; Nieuwenhuijsen, M.J.; Antó, J.M.; Brauer, M.; Briggs, D.; Braun-Fahrlander, C.; Cavill, N.; Cooper, A.R.; Desqueyroux, H.; Fruin, S.; et al. Improving health through policies that promote active travel: A review of evidence to support integrated health impact assessment. Environ. Int. 2011, 37, 766–777. [Google Scholar] [CrossRef]
- Sabel, C.E.; Hiscock, R.; Asikainen, A.; Bi, J.; Depledge, M.; van den Elshout, S.; Friedrich, R.; Huang, G.; Hurley, F.; Jantunen, M.; et al. Public health impacts of city policies to reduce climate change: Findings from the URGENCHE EU-China project. Environ. Health 2016, 15, S25. [Google Scholar] [CrossRef]
- Quam, V.G.M.; Rocklöv, J.; Quam, M.B.M.; Lucas, R.A.I. Assessing Greenhouse Gas Emissions and Health Co-Benefits: A Structured Review of Lifestyle-Related Climate Change Mitigation Strategies. Int. J. Environ. Res. Public Health 2017, 14, 468. [Google Scholar] [CrossRef] [PubMed]
- Monforti-Ferrario, F.; Kona, A.; Peduzzi, E.; Pernigotti, D.; Pisoni, E. The impact on air quality of energy saving measures in the major cities signatories of the Covenant of Mayors initiative. Environ. Int. 2018, 118, 222–234. [Google Scholar] [CrossRef] [PubMed]
- Kwan, S.C.; Hashim, J. A review on co-benefits of mass public transportation in climate change mitigation. Sustain. Cities Soc. 2016, 22, 11–18. [Google Scholar] [CrossRef]
- Oliveira, J.A.; Doll, C.N.; Siri, J.; Dreyfus, M.; Farzaneh, H.; Capon, A. Urban governance and the systems approaches to health-environment co-benefits in cities. Cad. Saude Publica 2015, 31, S25–S38. [Google Scholar] [CrossRef] [PubMed]
- Yip, C.S.C.; Crane, G.; Karnon, J. Systematic review of reducing population meat consumption to reduce greenhouse gas emissions and obtain health benefits: Effectiveness and models assessments. Int. J. Public Health 2013, 58, 683–693. [Google Scholar] [CrossRef]
- Remais, J.V.; Hess, J.J.; Ebi, K.L.; Markandya, A.; Balbus, J.M.; Wilkinson, P.; Haines, A.; Chalabi, Z. Estimating the health effects of greenhouse gas mitigation strategies: Addressing parametric, model, and valuation challenges. Environ. Health Perspect. 2014, 122, 447–455. [Google Scholar] [CrossRef] [PubMed]
- Ürge-Vorsatz, D.; Herrero, S.T.; Dubash, N.K.; Lecocq, F. Measuring the Co-Benefits of Climate Change Mitigation. Annu. Rev. Environ. Resour. 2014, 39, 549–582. [Google Scholar] [CrossRef]
- Hayes, K.; Poland, B. Addressing Mental Health in a Changing Climate: Incorporating Mental Health Indicators into Climate Change and Health Vulnerability and Adaptation Assessments. Int. J. Environ. Res. Public Health 2018, 15, 1806. [Google Scholar] [CrossRef]
- Banwell, N.; Rutherford, S.; Mackey, B.; Chu, C. Towards Improved Linkage of Disaster Risk Reduction and Climate Change Adaptation in Health: A Review. Int. J. Environ. Res. Public Health 2018, 15, 793. [Google Scholar] [CrossRef]
- Runkle, J.; Svendsen, E.R.; Hamann, M.; Kwok, R.K.; Pearce, J. Population Health Adaptation Approaches to the Increasing Severity and Frequency of Weather-Related Disasters Resulting From our Changing Climate: A Literature Review and Application to Charleston, South Carolina. Curr. Environ. Health Rep. 2018, 5, 439–452. [Google Scholar] [CrossRef]
- Luber, G.; Knowlton, K.; Balbus, J.; Frumkin, H.; Hayden, M.; Hess, J.; McGeehin, M.; Sheats, N.; Backer, L.; Beard, C.B.; et al. Chapter 9: Human Health. In Climate Change Impacts in the United States: The Third National Climate Assessment; Melillo, J.M., Richmond, T.C., Yohe, G.W., Eds.; U.S. Global Change Research Program: Washington, DC, USA, 2014; pp. 220–256. [Google Scholar]
- Hess, J.; Ebi, K.L. Iterative management of heat early warning systems in a changing climate. Ann. N. Y. Acad. Sci. 2016, 1382, 21–30. [Google Scholar] [CrossRef] [PubMed]
- Semenza, J.C. Prototype early warning systems for vector-borne diseases in Europe. Int. J. Environ. Res. Public Health 2015, 12, 6333–6351. [Google Scholar] [CrossRef] [PubMed]
- Confalonieri, U.E.; Menezes, J.A.; Margonari de Souza, C. Climate change and adaptation of the health sector: The case of infectious diseases. Virulence 2015, 6, 554–557. [Google Scholar] [CrossRef] [PubMed]
- Toloo, G.; FitzGerald, G.; Aitken, P.; Verrall, K.; Tong, S. Evaluating the effectiveness of heat warning systems: Systematic review of epidemiological evidence. Int. J. Public Health 2013, 58, 667–681. [Google Scholar] [CrossRef] [PubMed]
- Lowe, D.; Ebi, K.L.; Forsberg, B. Heatwave Early Warning Systems and Adaptation Advice to Reduce Human Health Consequences of Heatwaves. Int. J. Environ. Res. Public Health 2011, 8, 4623–4648. [Google Scholar] [CrossRef] [PubMed]
- Xu, Z.; FitzGerald, G.; Guo, Y.; Jalaludin, B.; Tong, S. Impact of heatwave on mortality under different heatwave definitions: A systematic review and meta-analysis. Environ. Int. 2016, 89–90, 193–203. [Google Scholar] [CrossRef] [PubMed]
- Li, M.; Gu, S.; Bi, P.; Yang, J.; Liu, Q. Heat waves and morbidity: Current knowledge and further direction-a comprehensive literature review. Int. J. Environ. Res. Public Health 2015, 12, 5256–5283. [Google Scholar] [CrossRef] [PubMed]
- Ballester, J.; Lowe, R.; Diggle, P.J.; Rodó, X. Seasonal forecasting and health impact models: Challenges and opportunities. Ann. N. Y. Acad. Sci. 2016, 1382, 8–20. [Google Scholar] [CrossRef]
- Wu, X.; Lu, Y.; Zhou, S.; Chen, L.; Xu, B. Impact of climate change on human infectious diseases: Empirical evidence and human adaptation. Environ. Int. 2016, 86, 14–23. [Google Scholar] [CrossRef]
- Brown, L.; Murray, V. Examining the relationship between infectious diseases and flooding in Europe: A systematic literature review and summary of possible public health interventions. Disaster Health 2013, 1, 117–127. [Google Scholar] [CrossRef]
- Chowdhury, F.R.; Nur, Z.; Hassan, N.; von Seidlein, L.; Dunachie, S. Pandemics, pathogenicity and changing molecular epidemiology of cholera in the era of global warming. Ann. Clin. Microbiol. Antimicrob. 2017, 16, 10. [Google Scholar] [CrossRef] [PubMed]
- Yang, G.J.; Utzinger, J.; Lv, S.; Qian, Y.J.; Li, S.Z.; Wang, Q.; Bergquist, R.; Vounatsou, P.; Li, W.; Yang, K.; et al. The Regional Network for Asian Schistosomiasis and Other Helminth Zoonoses (RNAS(+)) target diseases in face of climate change. Adv. Parasitol. 2010, 73, 101–135. [Google Scholar] [CrossRef] [PubMed]
- Akter, R.; Hu, W.; Naish, S.; Banu, S.; Tong, S. Joint effects of climate variability and socioecological factors on dengue transmission: Epidemiological evidence. Trop. Med. Int. Health 2017, 22, 656–669. [Google Scholar] [CrossRef] [PubMed]
- Mabaso, M.L.; Ndlovu, N.C. Critical review of research literature on climate-driven malaria epidemics in sub-Saharan Africa. Public Health 2012, 126, 909–919. [Google Scholar] [CrossRef] [PubMed]
- Rataj, E.; Kunzweiler, K.; Garthus-Niegel, S. Extreme weather events in developing countries and related injuries and mental health disorders-a systematic review. BMC Public Health 2016, 16, 1020. [Google Scholar] [CrossRef] [PubMed]
- Phua, K.L. Redesigning healthcare systems to meet the health challenges associated with climate change in the twenty-first century. J. Emerg. Manag. 2015, 13, 255–263. [Google Scholar] [CrossRef] [PubMed]
- Balbus, J.; Berry, P.; Brettle, M.; Jagnarine-Azan, S.; Soares, A.; Ugarte, C.; Varangu, L.; Prats, E.V. Enhancing the sustainability and climate resiliency of health care facilities: A comparison of initiatives and toolkits. Rev. Panam. de Salud Pública 2016, 40, 174–180. [Google Scholar]
- Curtis, S.; Fair, A.; Wistow, J.; Val, D.V.; Oven, K. Impact of extreme weather events and climate change for health and social care systems. Environ. Health 2017, 16, 128. [Google Scholar] [CrossRef]
- Urban Land Institute. Developing Urban Resilience: Spaulding Rehabilitation Hospital. 2018. Available online: https://developingresilience.uli.org/case/spaulding-rehabilitation-hospital/ (accessed on 29 March 2019).
- Eckelman, M.J.; Sherman, J. Environmental Impacts of the U.S. Health Care System and Effects on Public Health. PLoS ONE 2016, 11, e0157014. [Google Scholar] [CrossRef]
- Health Care Without Harm (HCWH). HCWH Europe Launches New Project to Measure GHG Emissions from European Hospitals. Available online: https://noharm-uscanada.org/articles/news/europe/hcwh-europe-launches-new-project-measure-ghg-emissions-european-hospitals (accessed on 11 March 2019).
- Hayes, K.; Berry, P.; Ebi, K.L. Factors Influencing the Mental Health Consequences of Climate Change in Canada. Int. J. Environ. Res. Public Health 2019, 16, 1583. [Google Scholar] [CrossRef]
- Obradovich, N.; Migliorini, R.; Paulus, M.P.; Rahwan, I. Empirical evidence of mental health risks posed by climate change. Proc. Natl. Acad. Sci. USA 2018, 115, 10953–10958. [Google Scholar] [CrossRef] [PubMed]
- Global Consortium on Climate and Health Education. Courses and Resources. Available online: https://www.mailman.columbia.edu/research/global-consortium-climate-and-health-education/courses-resources (accessed on 11 March 2019).
- Maxwell, J.; Blashki, G. Teaching about Climate Change in medical education: An opportunity. J. Public Health Res. 2016, 5, 14–20. [Google Scholar] [CrossRef] [PubMed]
- Friedrich, M. Medical Community Gathers Steam to Tackle Climate’s Health Effects. JAMA 2017, 317, 1511–1513. [Google Scholar] [CrossRef] [PubMed]
- Teherani, A.; Nishimura, H.; Apatira, L.; Newman, T.; Ryan, S. Identification of core objectives for teaching sustainable healthcare education. Med. Educ. Online 2017, 22, 1386042. [Google Scholar] [CrossRef] [PubMed]
- Gould, S.; Rudolph, L. Challenges and Opportunities for Advancing Work on Climate Change and Public Health. Int. J. Environ. Res. Public Health 2015, 12, 15649–15672. [Google Scholar] [CrossRef]
- Bouzid, M.; Hooper, L.; Hunter, P.R. The Effectiveness of Public Health Interventions to Reduce the Health Impact of Climate Change: A Systematic Review of Systematic Reviews. PLoS ONE 2013, 8, e62041. [Google Scholar] [CrossRef] [PubMed]
- Ebi, K.L.; Otmani del Barrio, M. Lessons Learned on Health Adaptation to Climate Variability and Change: Experiences Across Low-and Middle-Income Countries. Environ. Health Perspect. 2017, 125, 065001. [Google Scholar] [CrossRef]
- Panic, M.; Ford, J.D. A review of national-level adaptation planning with regards to the risks posed by climate change on infectious diseases in 14 OECD nations. Int. J. Environ. Res. Public Health 2013, 10, 7083–7109. [Google Scholar] [CrossRef]
- Hutton, G.; Menne, B. Economic evidence on the health impacts of climate change in Europe. Environ. Health Insights 2014, 8, 43–52. [Google Scholar] [CrossRef]
- Schmitt, L.H.; Graham, H.M.; White, P.C. Economic evaluations of the health impacts of weather-related extreme events: A scoping review. Int. J. Environ. Res. Public Health 2016, 13, 1105. [Google Scholar] [CrossRef]
- World Health Organization (WHO). Protecting Health from Climate Change: Global Research Priorities. 2009. Available online: http://www.who.int/globalchange/publications/9789241598187/en/ (accessed on 11 March 2019).
- Hosking, J.; Campbell-Lendrum, D. How Well Does Climate Change and Human Health Research Match the Demands of Policymakers? A Scoping Review. Environ. Health Perspect. 2012, 120, 1076–1082. [Google Scholar] [CrossRef] [PubMed]
- Verner, G.; Schütte, S.; Knop, J.; Sankoh, O.; Sauerborn, R. Health in climate change research from 1990 to 2014: Positive trend, but still underperforming. Glob. Health Action 2016, 9, 30723. [Google Scholar] [CrossRef] [PubMed]
- Hess, J.J.; Lm, S.; Knowlton, K.; Saha, S.; Dutta, P.; Ganguly, P.; Tiwari, A.; Jaiswal, A.; Sheffield, P.; Sarkar, J.; et al. Building Resilience to Climate Change: Pilot Evaluation of the Impact of India’s First Heat Action Plan on All-Cause Mortality. J. Environ. Public Health 2018, 2018, 7973519. [Google Scholar] [CrossRef] [PubMed]
| Core Function | Essential Service | Iterative Climate-Health Risk Assessment Framework a | Some Key Available Tools for Health and Climate |
|---|---|---|---|
| Assessment |
|
|
|
| Policy Development |
|
|
|
| Assurance |
|
|
|
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Fox, M.; Zuidema, C.; Bauman, B.; Burke, T.; Sheehan, M. Integrating Public Health into Climate Change Policy and Planning: State of Practice Update. Int. J. Environ. Res. Public Health 2019, 16, 3232. https://doi.org/10.3390/ijerph16183232
Fox M, Zuidema C, Bauman B, Burke T, Sheehan M. Integrating Public Health into Climate Change Policy and Planning: State of Practice Update. International Journal of Environmental Research and Public Health. 2019; 16(18):3232. https://doi.org/10.3390/ijerph16183232
Chicago/Turabian StyleFox, Mary, Christopher Zuidema, Bridget Bauman, Thomas Burke, and Mary Sheehan. 2019. "Integrating Public Health into Climate Change Policy and Planning: State of Practice Update" International Journal of Environmental Research and Public Health 16, no. 18: 3232. https://doi.org/10.3390/ijerph16183232
APA StyleFox, M., Zuidema, C., Bauman, B., Burke, T., & Sheehan, M. (2019). Integrating Public Health into Climate Change Policy and Planning: State of Practice Update. International Journal of Environmental Research and Public Health, 16(18), 3232. https://doi.org/10.3390/ijerph16183232






