Visits to Pediatric Clinics by Adult Patients: A Nationwide Survey in Taiwan
Abstract
1. Introduction
2. Materials and Methods
2.1. Data Collection
2.2. Study Population
2.3. Statistical Analysis
3. Results
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Chuang, C.M.; Chan, I.C.; Lee, Y.S.; Tsao, P.C.; Yang, C.F.; Soong, W.J.; Chen, T.J.; Jeng, M.J. Role of Pediatricians in the Ambulatory Care of Children in Taiwan, 1999–2011. Pediatr. Neonatol. 2014. [Google Scholar] [CrossRef] [PubMed]
- Somerville, J.; Report of the British Cardiac Society Working Party. Grown-up congenital heart (GUCH) disease: Current needs and provision of service for adolescents and adults with congenital heart disease in the UK. Heart 2002, 88. [Google Scholar] [CrossRef]
- Geerlings, R.P.; Aldenkamp, A.P.; de With, P.H.; Zinger, S.; Gottmer-Welschen, L.M.; de Louw, A.J. Transition to adult medical care for adolescents with epilepsy. Epilepsy Behav. 2015, 44, 127–135. [Google Scholar] [CrossRef] [PubMed]
- Pinhas-Hamiel, O.; Zeitler, P. The global spread of type 2 diabetes mellitus in children and adolescents. J. Pediatr. 2005, 146, 693–700. [Google Scholar] [CrossRef] [PubMed]
- Dabelea, D.; Mayer-Davis, E.J.; Saydah, S.; Imperatore, G.; Linder, B.; Divers, J.; Bell, R.; Badaru, A.; Talton, J.W.; Crume, T.; et al. Prevalence of type 1 and type 2 diabetes among children and adolescents from 2001 to 2009. JAMA 2014, 311, 1778–1786. [Google Scholar] [CrossRef] [PubMed]
- Fegran, L.; Hall, E.O.; Uhrenfeldt, L.; Aagaard, H.; Ludvigsen, M.S. Adolescents’ and young adults’ transition experiences when transferring from paediatric to adult care: A qualitative metasynthesis. Int. J. Nurs. Stud. 2014, 51, 123–135. [Google Scholar] [CrossRef] [PubMed]
- Lee, Y.A. Diabetes care for emerging adults: Transition from pediatric to adult diabetes care systems. Ann. Pediatr. Endocrinol. Metab. 2013, 18, 106–110. [Google Scholar] [CrossRef] [PubMed]
- Lotstein, D.S.; Seid, M.; Klingensmith, G.; Case, D.; Lawrence, J.M.; Pihoker, C.; Dabelea, D.; Mayer-Davis, E.J.; Gilliam, L.K.; Corathers, S.; et al. Transition from pediatric to adult care for youth diagnosed with type 1 diabetes in adolescence. Pediatrics 2013, 131, e1062–e1070. [Google Scholar] [CrossRef] [PubMed]
- Chen, Y.H. Trends in Low Fertility and Policy Responses in Taiwan. Jpn. J. Popul. 2012, 10, 78–88. [Google Scholar]
- Yang, L.Y.; Lynn, A.M.; Chen, T.J. Ambulatory Care Visits to Pediatricians in Taiwan: A Nationwide Analysis. Int. J. Environ. Res. Public Health 2015, 12, 14043–14054. [Google Scholar] [CrossRef] [PubMed]
- Shao, C.C.; Chang, C.P.; Chou, L.F.; Chen, T.J.; Hwang, S.J. The ecology of medical care in Taiwan. J. Chin. Med. Assoc. 2011, 74, 408–412. [Google Scholar] [CrossRef] [PubMed]
- Data Subset of NHIRD. Available online: https://nhird.nhri.org.tw/en/Data_Subsets.html (accessed on 18 July 2018).
- Free Online Searchable 2009 ICD-9-CM. National Center for Health Statistics (NCHS). Available online: http://icd9cm.chrisendres.com/ (accessed on 18 July 2018).
- Clinical Classifications Software (CCS) for ICD-9-CM. HCUP CCS. Healthcare Cost and Utilization Project (HCUP). Agency for Healthcare Research and Quality: Rockville, MD. Available online: http://www.hcup-us.ahrq.gov/toolssoftware/ccs/ccs.jsp (accessed on 18 July 2018).
- Chiu, N.C.; Ho, C.H.; Shen, S.H.; Tsuei, Y.C.; Lee, K.L.; Huang, C.Y.; Li, H.Y.; Chen, T.J. Impact of hysterosalpingography after operative treatment for ectopic pregnancy in Taiwan: A 16-year Nationwide Population-Based Analysis. Medicine 2017, 96, e7263. [Google Scholar] [CrossRef] [PubMed]
- Wang, P.H.; Sheu, B.C.; Yeh, J.Y. The Sunset Industry: Obstetrics and gynecology concerns about the shortage of obstetricians and gynecologists. Am. J. Obstet. Gynecol. 2009, 201, e12. [Google Scholar] [CrossRef] [PubMed]
- Lee, R.; Mason, A.; Members of the NTA Network. Is low fertility really a problem? Population aging, dependency, and consumption. Science 2014, 10, 229–234. [Google Scholar] [CrossRef] [PubMed]
- Lynn, A.M.; Lai, L.J.; Lin, M.H.; Chen, T.J.; Hwang, S.J.; Wang, P.H. Pattern of Ambulatory Care Visits to Obstetrician-Gynecologists in Taiwan: A Nationwide Analysis. Int. J. Environ. Res. Public Health 2015, 12, 6832–6841. [Google Scholar] [CrossRef] [PubMed]
- Viner, R. Transition from paediatric to adult care. Bridging the gaps or passing the buck? Arch. Dis. Child. 1999, 81, 271–275. [Google Scholar] [CrossRef] [PubMed]
- Crowley, R.; Wolfe, I.; Lock, K.; McKee, M. Improving the transition between paediatric and adult healthcare: A systematic review. Arch. Dis. Child. 2011, 96, 548–553. [Google Scholar] [CrossRef] [PubMed]
- Wysocki, T.; Hough, B.S.; Ward, K.M.; Green, L.B. Diabetes mellitus in the transition to adulthood: Adjustment, self-care, and health status. J. Dev. Behav. Pediatr. 1992, 13, 194–201. [Google Scholar] [CrossRef] [PubMed]
- Watson, A.R. Non-compliance and transfer from paediatric to adult transplant unit. Pediatr. Nephrol. 2000, 14, 469–472. [Google Scholar] [CrossRef] [PubMed]
- Oeffinger, K.C.; Mertens, A.C.; Hudson, M.M.; Gurney, J.G.; Casillas, J.; Chen, H.; Whitton, J.; Yeazel, M.; Yasui, Y.; Robison, L.L. Health care of young adult survivors of childhood cancer: A report from the Childhood Cancer Survivor Study. Ann. Fam. Med. 2004, 2, 61–70. [Google Scholar] [CrossRef] [PubMed]
- Yeung, E.; Kay, J.; Roosevelt, G.E.; Brandon, M.; Yetman, A.T. Lapse of care as a predictor for morbidity in adults with congenital heart disease. Int. J. Cardiol. 2008, 125, 62–65. [Google Scholar] [CrossRef] [PubMed]
- Webb, N.; Harden, P.; Lewis, C.; Tizzard, S.; Walsh, G.; Wray, J.; Watson, A. Building consensus on transition of transplant patients from paediatric to adult healthcare. Arch. Dis. Child. 2010, 95, 606–611. [Google Scholar] [CrossRef] [PubMed]
- Somerville, J. Management of adults with congenital heart disease: An increasing problem. Annu. Rev. Med. 1997, 48, 283–293. [Google Scholar] [CrossRef] [PubMed]
- Kaemmerer, H.; Bauer, U.; de Haan, F.; Flesch, J.; Gohlke-Bärwolf, C.; Hagl, S.; Hess, J.; Hofbeck, M.; Kallfelz, H.C.; Lange, P.E.; et al. Recommendations for improving the quality of the interdisciplinary medical care of grown-ups with congenital heart disease (GUCH). Int. J. Cardiol. 2011, 150, 59–64. [Google Scholar] [CrossRef] [PubMed]
- Patterson, C.C.; Dahlquist, G.G.; Gyurus, E.; Green, A.; Soltesz, G.; EURODIAB Study Group. Incidence trends for childhood type 1 diabetes in Europe during 1989–2003 and predicted new cases 2005–20: A multicentre prospective registration study. Lancet 2009, 373, 2027–2033. [Google Scholar] [CrossRef]
- Chang, C.P.; Chou, C.L.; Chou, Y.C.; Shao, C.C.; Su, H.I.; Chen, T.J.; Chou, L.F.; Yu, H.C. The ecology of gynecological care for women. Int. J. Environ. Res. Public Health 2014, 11, 7669–7677. [Google Scholar] [CrossRef] [PubMed]
- Hajjar, I.; Kotchen, J.M.; Kotchen, T.A. Hypertension: Trends in prevalence, incidence, and control. Annu. Rev. Public Health 2006, 27, 465–490. [Google Scholar] [CrossRef] [PubMed]
- Wu, M.H.; Yu, J.Y.; Huang, C.H. Theoretical system dynamics modeling for Taiwan pediatric workforce in an era of national health insurance and low birth rates. Pediatr. Neonatol. 2013, 54, 389–396. [Google Scholar] [CrossRef] [PubMed]
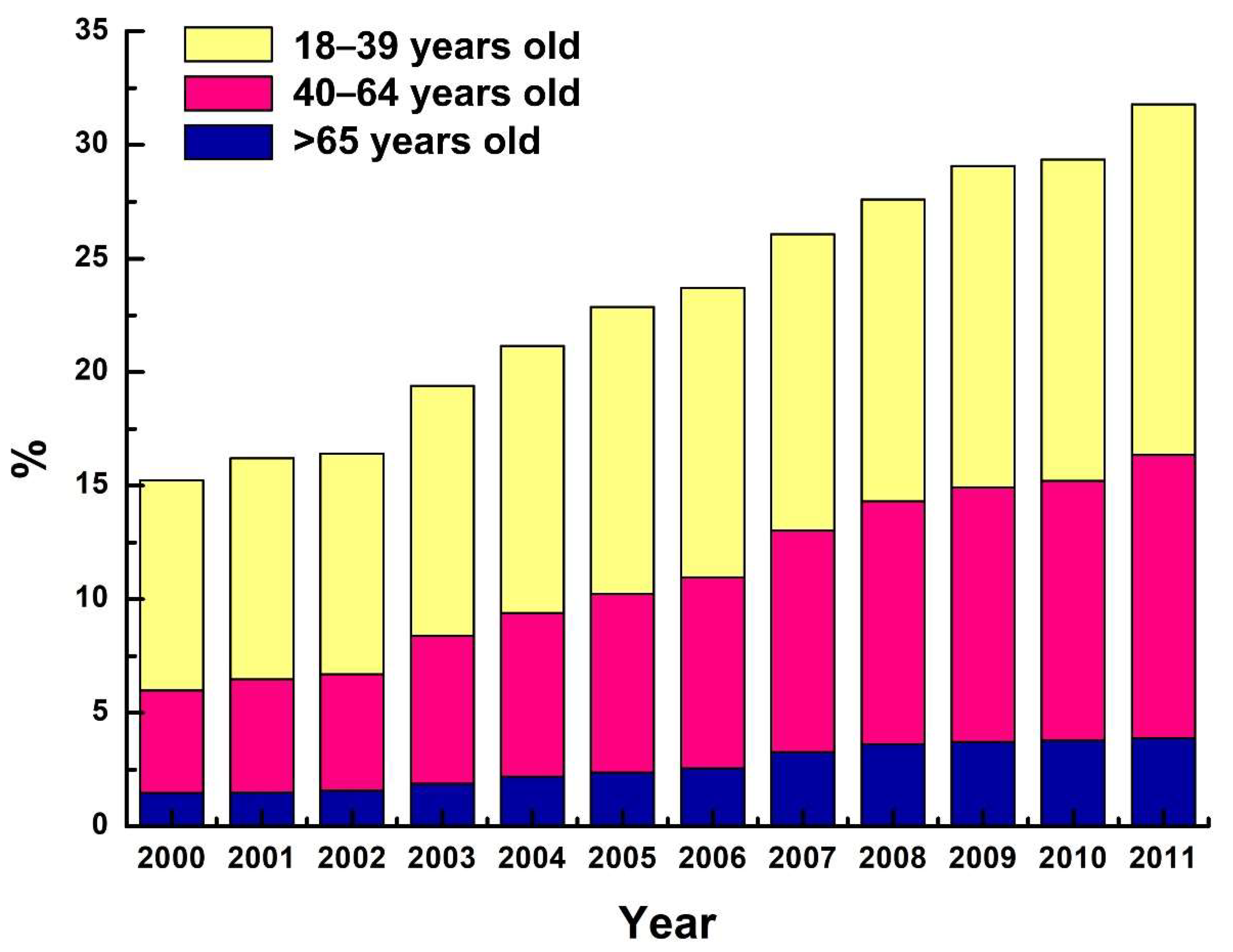
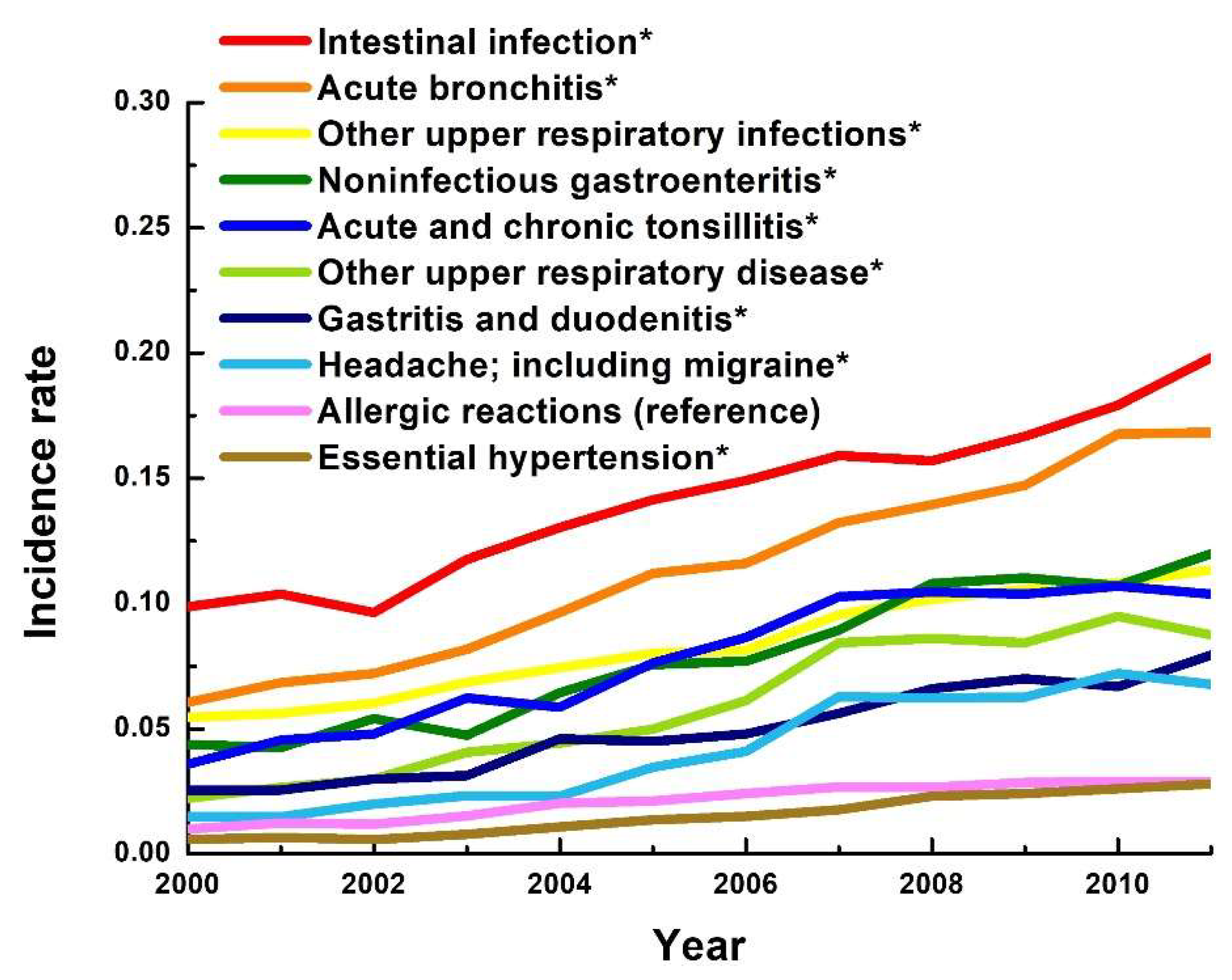
| Age Group, Years | Visit Year | |||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Hospital Level | 2000 | 2001 | 2002 | 2003 | 2004 | 2005 | 2006 | 2007 | 2008 | 2009 | 2010 | 2011 |
| 0–17 | ||||||||||||
| Academic medical center | 4296 | 4092 | 4131 | 2928 | 3021 | 2832 | 2456 | 2517 | 2387 | 2331 | 2449 | 2250 |
| Metropolitan hospital | 4983 | 5065 | 5607 | 4440 | 4532 | 3924 | 3433 | 3418 | 3508 | 3628 | 3448 | 3653 |
| Local community hospital | 3298 | 3186 | 3278 | 2703 | 2870 | 2508 | 2205 | 2250 | 2167 | 2214 | 2252 | 2293 |
| Physician clinic | 26,090 | 24,596 | 25,113 | 25,269 | 27,443 | 29,231 | 26,895 | 30,432 | 29,477 | 30,315 | 31,200 | 32,168 |
| 18–39 | ||||||||||||
| Academic medical center | 94 | 98 | 105 | 104 | 115 | 122 | 117 | 137 | 136 | 139 | 167 | 198 |
| Metropolitan hospital | 37 | 39 | 70 | 63 | 118 | 115 | 91 | 102 | 84 | 113 | 113 | 100 |
| Local community hospital | 40 | 51 | 57 | 56 | 89 | 98 | 95 | 86 | 101 | 96 | 81 | 138 |
| Physician clinic | 4039 | 4100 | 4202 | 4605 | 5314 | 5961 | 5530 | 6482 | 6576 | 7327 | 7512 | 8687 |
| 40–64 | ||||||||||||
| Academic medical center | 18 | 20 | 18 | 15 | 26 | 14 | 23 | 17 | 12 | 15 | 24 | 25 |
| Metropolitan hospital | 8 | 12 | 17 | 19 | 22 | 17 | 13 | 16 | 24 | 23 | 15 | 26 |
| Local community hospital | 17 | 21 | 17 | 30 | 29 | 23 | 25 | 25 | 30 | 29 | 27 | 37 |
| Physician clinic | 2022 | 2146 | 2285 | 2793 | 3389 | 3870 | 3795 | 5041 | 5477 | 6014 | 6306 | 7285 |
| >65 | ||||||||||||
| Academic medical center | 6 | 4 | 8 | 6 | 6 | 1 | 4 | 6 | 2 | 7 | 5 | 3 |
| Metropolitan hospital | 2 | 2 | 3 | 7 | 4 | 3 | 4 | 6 | 2 | 3 | 7 | 2 |
| Local community hospital | 10 | 11 | 9 | 8 | 12 | 7 | 9 | 11 | 11 | 22 | 15 | 21 |
| Physician clinic | 650 | 640 | 699 | 801 | 1028 | 1174 | 1157 | 1689 | 1861 | 1985 | 2076 | 2273 |
| Total | 45,610 | 44,083 | 45,619 | 43,847 | 48,018 | 49,900 | 45,852 | 52,235 | 51,855 | 54,261 | 55,697 | 59,159 |
| Rank | Academic Medical Center | Metropolitan Hospital | Local Community Hospital | Physician Clinic |
|---|---|---|---|---|
| 1 | Epilepsy | URD | URI | URI |
| 2 | URD | URI | URD | Acute bronchitis |
| 3 | CVCA | Acute bronchitis | Acute bronchitis | Tonsillitis |
| 4 | Anemia | Tonsillitis | Asthma | Gastroenteritis |
| 5 | URI | Pneumonia | Allergic reactions | Influenza |
| 6 | Asthma | Epilepsy | Pneumonia | Intestinal infection |
| 7 | SLE | Asthma | Tonsillitis | Gastritis and duodenitis |
| 8 | Endocrine | Allergic reactions | Gastroenteritis | Allergic reactions |
| 9 | Acute bronchitis | Gastroenteritis | Hypertension | URD |
| 10 | Pneumonia | Anemia | CVD | Hypertension |
| Top 10 Order | Academic Medical Center | Metropolitan Hospital | Local Community Hospital | Physician Clinic |
|---|---|---|---|---|
| 1 | Epilepsy | Jaundice | URI | URI |
| 2 | CVCA | URI | Jaundice | Acute bronchitis |
| 3 | URD | URD | Acute bronchitis | Tonsillitis |
| 4 | Anemia | Acute bronchitis | Tonsillitis | Gastroenteritis |
| 5 | Jaundice | Allergic reactions | URD | URD |
| 6 | SLE | Asthma | Admission | Gastritis and duodenitis |
| 7 | Asthma | Epilepsy | Allergic reactions | Allergic reactions |
| 8 | URI | Immunizations | GID | Intestinal infection |
| 9 | Congenital anomalies | Perinatal conditions | Gastroenteritis | Headache |
| 10 | DM | Pneumonia | Hypertension | Hypertension |
| Top 10 Order | Academic Medical Center | Metropolitan Hospital | Local Community Hospital | Physician Clinic |
|---|---|---|---|---|
| 1 | Epilepsy | Jaundice | URI | URI |
| 2 | CVCA | URI | Jaundice | Acute bronchitis |
| 3 | Jaundice | Allergic reactions | Acute bronchitis | Tonsillitis |
| 4 | Anemia | URD | Immunizations | URD |
| 5 | DM | Immunizations | Tonsillitis | Gastroenteritis |
| 6 | Congenital anomalies | Acute bronchitis | URD | Gastritis and duodenitis |
| 7 | SLE | Pneumonia | Allergic reactions | LRD |
| 8 | URI | Admission | Admission | Hypertension |
| 9 | Asthma | Tonsillitis | Pneumonia | Allergic reactions |
| 10 | URD | FUO | GID | Headache |
© 2018 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Lee, K.-L.; Lynn, A.-M.; Chen, T.-J.; Yang, L.-Y.; Chiang, S.-C. Visits to Pediatric Clinics by Adult Patients: A Nationwide Survey in Taiwan. Int. J. Environ. Res. Public Health 2018, 15, 1538. https://doi.org/10.3390/ijerph15071538
Lee K-L, Lynn A-M, Chen T-J, Yang L-Y, Chiang S-C. Visits to Pediatric Clinics by Adult Patients: A Nationwide Survey in Taiwan. International Journal of Environmental Research and Public Health. 2018; 15(7):1538. https://doi.org/10.3390/ijerph15071538
Chicago/Turabian StyleLee, Kang-Lung, An-Min Lynn, Tzeng-Ji Chen, Ling-Yu Yang, and Shu-Chiung Chiang. 2018. "Visits to Pediatric Clinics by Adult Patients: A Nationwide Survey in Taiwan" International Journal of Environmental Research and Public Health 15, no. 7: 1538. https://doi.org/10.3390/ijerph15071538
APA StyleLee, K.-L., Lynn, A.-M., Chen, T.-J., Yang, L.-Y., & Chiang, S.-C. (2018). Visits to Pediatric Clinics by Adult Patients: A Nationwide Survey in Taiwan. International Journal of Environmental Research and Public Health, 15(7), 1538. https://doi.org/10.3390/ijerph15071538






