Association between Internet Gaming Disorder or Pathological Video-Game Use and Comorbid Psychopathology: A Comprehensive Review
Abstract
1. Introduction
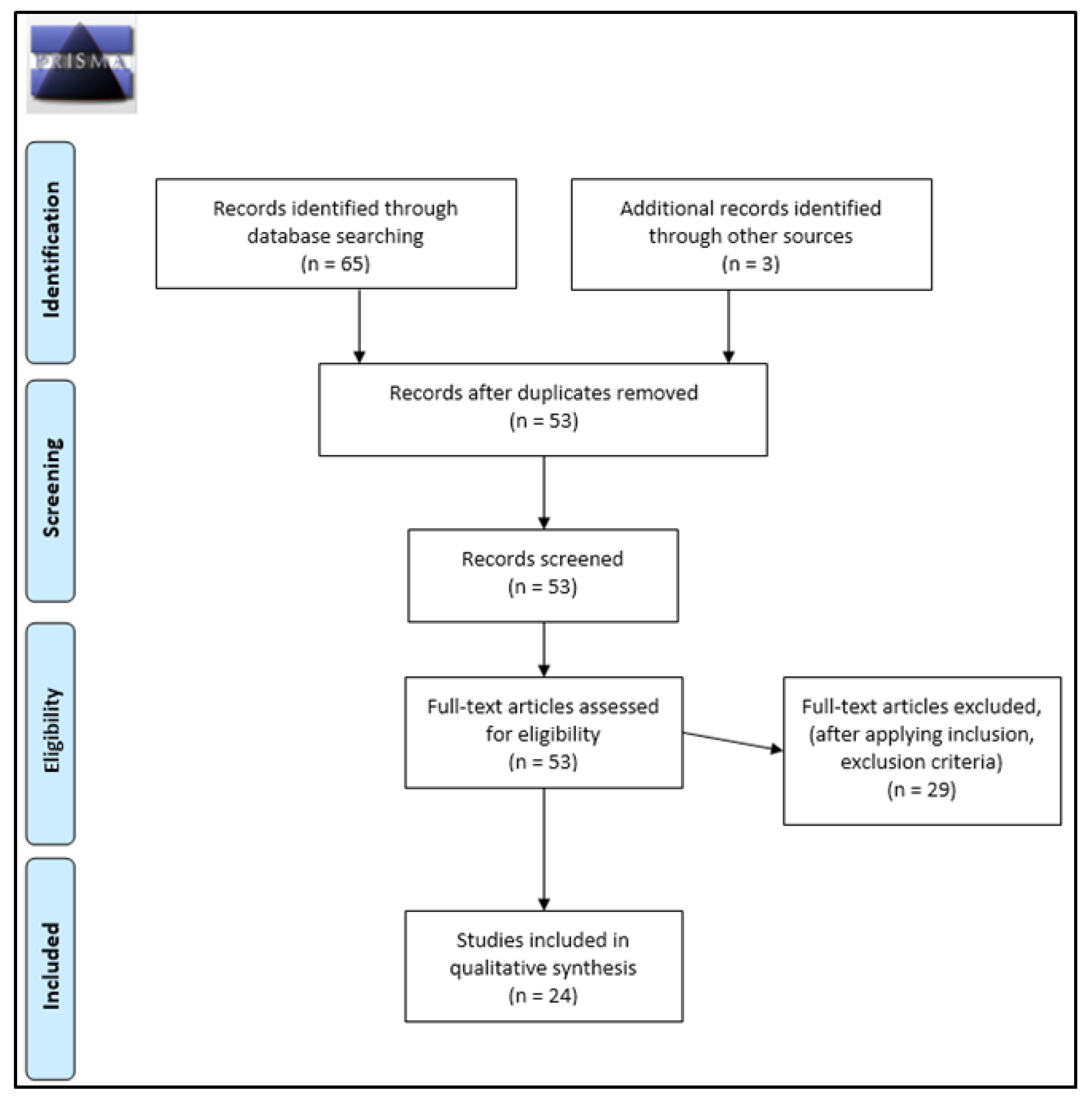
2. Materials and Methods
3. Results
3.1. Design of the Included Studies
3.2. Characteristics of the Used Samples
3.3. Methods of Assessing Internet Gaming Disorder (IGD)
3.4. Methods Assessing Psychopathology
3.5. Effect Size of the Associations of Psychopathology with IGD
3.6. Psychopathology, IGD and Sample Characteristics (Age, Gender)
3.7. IGD and Depression
3.8. IGD and Anxiety
3.9. IGD and Attention Deficit Hyperactivity Disorder (ADHD)
3.10. IGD and Social Phobia and Social Anxiety
3.11. IGD and Obsessive-Compulsive Symptoms
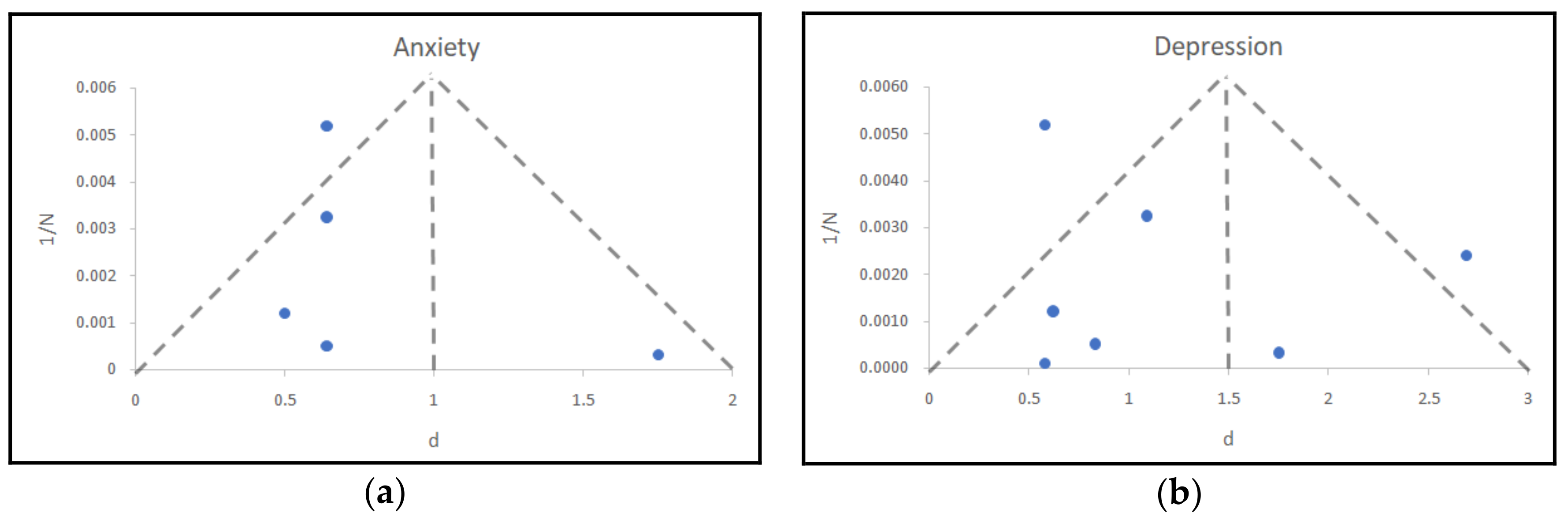
3.12. Publication Bias
4. Discussion
5. Limitations
6. Conclusions
Acknowledgments
Author Contributions
Conflicts of Interest
References
- King, D.L.; Haagsma, M.C.; Delfabbro, P.H.; Gradisar, M.; Griffiths, M.D. Toward a consensus definition of pathological video-gaming: A systematic review of psychometric assessment tools. Clin. Psychol. Rev. 2013, 33, 331–342. [Google Scholar] [CrossRef] [PubMed]
- Sim, T.; Gentile, D.A.; Bricolo, F.; Serpelloni, G.; Gulamoydeen, F. A Conceptual Review of Research on the Pathological Use of Computers, Video Games, and the Internet. Int. J. Ment. Health Addict. 2012, 10, 748–769. [Google Scholar] [CrossRef][Green Version]
- King, D.L.; Delfabbro, P.H. Issues for DSM-5: Video-gaming disorder? Aust. N. Z. J. Psychiatry 2013, 47, 20–22. [Google Scholar] [CrossRef] [PubMed]
- Starcevic, V.; Aboujaoude, E. Internet addiction: Reappraisal of an increasingly inadequate concept. CNS Spectr. 2017, 22, 7–13. [Google Scholar] [CrossRef] [PubMed]
- Thompson, T. Demographic and motivation variables associated with Internet usage activities. Internet Res. 2001, 11, 125–137. [Google Scholar] [CrossRef]
- Weiser, E.B. Gender Differences in Internet Use Patterns and Internet Application Preferences: A Two-Sample Comparison. CyberPsychol. Behav. 2000, 3, 167–178. [Google Scholar] [CrossRef]
- American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders (DSM-5), 5th ed.; American Psychiatric Association: Washington, DC, USA, 2013. [Google Scholar]
- ICD-11 Beta Draft—Mortality and Morbidity Statistics. Available online: https://icd.who.int/dev11/l-m/en (accessed on 17 November 2017).
- Saban, A.; Flisher, A.J. The Association between Psychopathology and Substance Use in Young People: A Review of the Literature. J. Psychoact. Drugs 2010, 42, 37–47. [Google Scholar] [CrossRef] [PubMed]
- Petit, A.; Karila, L.; Chalmin, F.; Lejoyeux, M. Methamphetamine Addiction: A Review of the Literature. J. Addict. Res. Ther. 2012, 1, 2–7. [Google Scholar] [CrossRef]
- Anthony, J.C. Epidemiology of drug dependence and illicit drug use. Curr. Opin. Psychiatry 1991, 4, 435–439. [Google Scholar] [CrossRef]
- Kosten, T.R.; Ziedonis, D.M. Substance abuse and schizophrenia: Editors’ introduction. Schizophr. Bull. 1997, 23, 181–186. [Google Scholar] [CrossRef] [PubMed]
- Lehman, A.F.; Myers, C.P.; Corty, E. Assessment and classification of patients with psychiatric and substance abuse syndromes. Hosp. Community Psychiatry 1989, 40, 1019–1025. [Google Scholar] [CrossRef] [PubMed]
- Carli, V.; Durkee, T.; Wasserman, D.; Hadlaczky, G.; Despalins, R.; Kramarz, E.; Wasserman, C.; Sarchiapone, M.; Hoven, C.W.; Brunner, R.; et al. The association between pathological internet use and comorbid psychopathology: A systematic review. Psychopathology 2013, 46, 1–13. [Google Scholar] [CrossRef] [PubMed]
- Dong, G.; Lu, Q.; Zhou, H.; Zhao, X. Precursor or Sequela: Pathological Disorders in People with Internet Addiction Disorder. PLoS ONE 2011, 6, e14703. [Google Scholar] [CrossRef] [PubMed]
- Floros, G.; Siomos, K.; Stogiannidou, A.; Giouzepas, I.; Garyfallos, G. Comorbidity of psychiatric disorders with Internet addiction in a clinical sample: The effect of personality, defense style and psychopathology. Addict. Behav. 2014, 39, 1839–1845. [Google Scholar] [CrossRef] [PubMed]
- Young, K.S. Cognitive behavior therapy with Internet addicts: Treatment outcomes and implications. Cyberpsychol. Behav. 2007, 10, 671–679. [Google Scholar] [CrossRef] [PubMed]
- Chang, F.-C.; Chiu, C.-H.; Lee, C.-M.; Chen, P.-H.; Miao, N.-F. Predictors of the initiation and persistence of Internet addiction among adolescents in Taiwan. Addict. Behav. 2014, 39, 1434–1440. [Google Scholar] [CrossRef] [PubMed]
- Durkee, T.; Kaess, M.; Carli, V.; Parzer, P.; Wasserman, C.; Floderus, B.; Apter, A.; Balazs, J.; Barzilay, S.; Bobes, J.; et al. Prevalence of pathological internet use among adolescents in Europe: Demographic and social factors. Addiction 2012, 107, 2210–2222. [Google Scholar] [CrossRef] [PubMed]
- Moher, D.; Shamseer, L.; Clarke, M.; Ghersi, D.; Liberati, A.; Petticrew, M.; Shekelle, P.; Stewart, L.A. PRISMA-P Group Preferred reporting items for systematic review and meta-analysis protocols (PRISMA-P) 2015 statement. Syst. Rev. 2015, 4, 1. [Google Scholar] [CrossRef] [PubMed]
- Available online: https://www.crd.york.ac.uk/PROSPERO/ (accessed on 17 November 2017).
- Cohen, J. Statistical Power Analysis for the Behavioral Sciences, 2nd ed.; L. Erlbaum Associates: Hillsdale, NJ, USA, 1988; ISBN 9780805802832. [Google Scholar]
- Chinn, S. A simple method for converting an odds ratio to effect size for use in meta-analysis. Stat. Med. 2000, 19, 3127–3131. [Google Scholar] [CrossRef]
- Baer, S.; Bogusz, E.; Green, D.A. Stuck on screens: Patterns of computer and gaming station use in youth seen in a psychiatric clinic. J. Can. Acad. Child Adolesc. Psychiatry 2011, 20, 86–94. [Google Scholar] [PubMed]
- Cole, S.H.; Hooley, J.M. Clinical and Personality Correlates of MMO Gaming. Soc. Sci. Comput. Rev. 2013, 31, 424–436. [Google Scholar] [CrossRef]
- Jiménez-Murcia, S.; Fernández-Aranda, F.; Granero, R.; Chóliz, M.; La Verde, M.; Aguglia, E.; Signorelli, M.S.; Sá, G.M.; Aymamí, N.; Gómez-Peña, M.; et al. Video game addiction in gambling disorder: Clinical, psychopathological, and personality correlates. Biomed. Res. Int. 2014, 7, 105–110. [Google Scholar] [CrossRef] [PubMed]
- Kim, N.R.; Hwang, S.S.-H.; Choi, J.-S.; Kim, D.-J.; Demetrovics, Z.; Király, O.; Nagygyörgy, K.; Griffiths, M.D.; Hyun, S.Y.; Youn, H.C.; et al. Characteristics and Psychiatric Symptoms of Internet Gaming Disorder among Adults Using Self-Reported DSM-5 Criteria. Psychiatry Investig. 2016, 13, 58. [Google Scholar] [CrossRef] [PubMed]
- King, D.L.; Delfabbro, P.H.; Zwaans, T.; Kaptsis, D. Clinical features and axis I comorbidity of Australian adolescent pathological Internet and video game users. Aust. N. Z. J. Psychiatry 2013, 47, 1058–1067. [Google Scholar] [CrossRef] [PubMed]
- King, D.L.; Delfabbro, P.H. The Cognitive Psychopathology of Internet Gaming Disorder in Adolescence. J. Abnorm. Child Psychol. 2016, 44, 1635–1645. [Google Scholar] [CrossRef] [PubMed]
- Laconi, S.; Pirès, S.; Chabrol, H. Internet gaming disorder, motives, game genres and psychopathology. Comput. Hum. Behav. 2017, 75, 652–659. [Google Scholar] [CrossRef]
- Männikkö, N.; Billieux, J.; Kääriäinen, M. Problematic digital gaming behavior and its relation to the psychological, social and physical health of Finnish adolescents and young adults. J. Behav. Addict. 2015, 4, 281–288. [Google Scholar] [CrossRef] [PubMed]
- Mentzoni, R.A.; Brunborg, G.S.; Molde, H.; Myrseth, H.; Skouverøe, K.J.M.; Hetland, J.; Pallesen, S. Problematic Video Game Use: Estimated Prevalence and Associations with Mental and Physical Health. Cyberpsychol. Behav. Soc. Netw. 2011, 14, 591–596. [Google Scholar] [CrossRef] [PubMed]
- Müller, K.W.; Janikian, M.; Dreier, M.; Wölfling, K.; Beutel, M.E.; Tzavara, C.; Richardson, C.; Tsitsika, A. Regular gaming behavior and internet gaming disorder in European adolescents: Results from a cross-national representative survey of prevalence, predictors, and psychopathological correlates. Eur. Child Adolesc. Psychiatry 2015, 24, 565–574. [Google Scholar] [CrossRef] [PubMed]
- Na, E.; Lee, H.; Choi, I.; Kim, D.-J. Comorbidity of Internet gaming disorder and alcohol use disorder: A focus on clinical characteristics and gaming patterns. Am. J. Addict. 2017, 26, 326–334. [Google Scholar] [CrossRef] [PubMed]
- Starcevic, V.; Berle, D.; Porter, G.; Fenech, P. Problem Video Game Use and Dimensions of Psychopathology. Int. J. Ment. Health Addict. 2011, 9, 248–256. [Google Scholar] [CrossRef]
- Stetina, B.U.; Kothgassner, O.D.; Lehenbauer, M.; Kryspin-Exner, I. Beyond the fascination of online-games: Probing addictive behavior and depression in the world of online-gaming. Comput. Hum. Behav. 2011, 27, 473–479. [Google Scholar] [CrossRef]
- Strittmatter, E.; Kaess, M.; Parzer, P.; Fischer, G.; Carli, V.; Hoven, C.W.; Wasserman, C.; Sarchiapone, M.; Durkee, T.; Apter, A.; et al. Pathological Internet use among adolescents: Comparing gamers and non-gamers. Psychiatry Res. 2015, 228, 128–135. [Google Scholar] [CrossRef] [PubMed]
- Vadlin, S.; Åslund, C.; Hellström, C.; Nilsson, K.W. Associations between problematic gaming and psychiatric symptoms among adolescents in two samples. Addict. Behav. 2016, 61, 8–15. [Google Scholar] [CrossRef] [PubMed]
- Wang, H.R.; Cho, H.; Kim, D.-J. Prevalence and correlates of comorbid depression in a nonclinical online sample with DSM-5 internet gaming disorder. J. Affect. Disord. 2018, 226, 1–5. [Google Scholar] [CrossRef] [PubMed]
- Wartberg, L.; Kriston, L.; Kramer, M.; Schwedler, A.; Lincoln, T.M.; Kammerl, R. Internet gaming disorder in early adolescence: Associations with parental and adolescent mental health. Eur. Psychiatry 2017, 43, 14–18. [Google Scholar] [CrossRef] [PubMed]
- Wei, H.-T.; Chen, M.-H.; Huang, P.-C.; Bai, Y.-M. The association between online gaming, social phobia, and depression: An internet survey. BMC Psychiatry 2012, 12, 92. [Google Scholar] [CrossRef] [PubMed]
- Panagiotidi, M. Problematic Video Game Play and ADHD Traits in an Adult Population. Cyberpsychol. Behav. Soc. Netw. 2017, 20, 292–295. [Google Scholar] [CrossRef] [PubMed]
- Gentile, D.A.; Choo, H.; Liau, A.; Sim, T.; Li, D.; Fung, D.; Khoo, A. Pathological video game use among youths: A two-year longitudinal study. Pediatrics 2011, 127, e319–e329. [Google Scholar] [CrossRef] [PubMed]
- Van Rooij, A.J.; Schoenmakers, T.M.; Vermulst, A.A.; Van Den Eijnden, R.J.J.M.; Van De Mheen, D. Online video game addiction: Identification of addicted adolescent gamers. Addiction 2011, 106, 205–212. [Google Scholar] [CrossRef] [PubMed]
- Hyun, G.J.; Han, D.H.; Lee, Y.S.; Kang, K.D.; Yoo, S.K.; Chung, U.-S.; Renshaw, P.F. Risk factors associated with online game addiction: A hierarchical model. Comput. Hum. Behav. 2015, 48, 706–713. [Google Scholar] [CrossRef]
- Yen, J.-Y.; Liu, T.-L.; Wang, P.-W.; Chen, C.-S.; Yen, C.-F.; Ko, C.-H. Association between Internet gaming disorder and adult attention deficit and hyperactivity disorder and their correlates: Impulsivity and hostility. Addict. Behav. 2017, 64, 308–313. [Google Scholar] [CrossRef] [PubMed]
- Brunborg, G.S.; Mentzoni, R.A.; Frøyland, L.R. Is video gaming, or video game addiction, associated with depression, academic achievement, heavy episodic drinking, or conduct problems? J. Behav. Addict. 2014, 3, 27–32. [Google Scholar] [CrossRef] [PubMed]
- Király, O.; Sleczka, P.; Pontes, H.M.; Urbán, R.; Griffiths, M.D.; Demetrovics, Z. Validation of the Ten-Item Internet Gaming Disorder Test (IGDT-10) and evaluation of the nine DSM-5 Internet Gaming Disorder criteria. Addict. Behav. 2017, 64, 253–260. [Google Scholar] [CrossRef] [PubMed]
- Vadlin, S.; Åslund, C.; Nilsson, K.W. Development and content validity of a screening instrument for gamingaddiction in adolescents: The Gaming Addiction Identification Test (GAIT). Scand. J. Psychol. 2015, 56, 458–466. [Google Scholar] [CrossRef] [PubMed]
- Lemmens, J.S.; Valkenburg, P.M.; Gentile, D.A. The Internet Gaming Disorder Scale. Psychol. Assess. 2015, 27, 567–582. [Google Scholar] [CrossRef] [PubMed]
- Bush, K.; Kivlahan, D.R.; McDonell, M.B.; Fihn, S.D.; Bradley, K.A. The AUDIT alcohol consumption questions (AUDIT-C): An effective brief screening test for problem drinking. Ambulatory Care Quality Improvement Project (ACQUIP). Alcohol Use Disorders Identification Test. Arch. Intern. Med. 1998, 158, 1789–1795. [Google Scholar] [CrossRef] [PubMed]
- Derogatis, L.R.; Lipman, R.S.; Rickels, K.; Uhlenhuth, E.H.; Covi, L. The Hopkins Symptom Checklist (HSCL): A self-report symptom inventory. Behav. Sci. 1974, 19, 1–15. [Google Scholar] [CrossRef] [PubMed]
- Woo, B.S.C.; Chang, W.C.; Fung, D.S.S.; Koh, J.B.K.; Leong, J.S.F.; Kee, C.H.Y.; Seah, C.K.F. Development and validation of a depression scale for Asian adolescents. J. Adolesc. 2004, 27, 677–689. [Google Scholar] [CrossRef] [PubMed]
- Beck, A.T.; Ward, C.H.; Mendelson, M.; Mock, J.; Erbaugh, J. An inventory for measuring depression. Arch. Gen. Psychiatry 1961, 4, 561–571. [Google Scholar] [CrossRef] [PubMed]
- Beck, A.T.; Steer, R.A.; Ball, R.; Ranieri, W.F. Comparison of Beck Depression Inventories-IA and-II in Psychiatric Outpatients. J. Pers. Assess. 1996, 67, 588–597. [Google Scholar] [CrossRef] [PubMed]
- Andresen, E.M.; Malmgren, J.A.; Carter, W.B.; Patrick, D.L. Screening for depression in well older adults: Evaluation of a short form of the CES-D (Center for Epidemiologic Studies Depression Scale). Am. J. Prev. Med. 1994, 10, 77–84. [Google Scholar] [CrossRef]
- Kandel, D.B.; Davies, M. Epidemiology of depressive mood in adolescents: An empirical study. Arch. Gen. Psychiatry 1982, 39, 1205–1212. [Google Scholar] [CrossRef] [PubMed]
- Kühner, C. Fragebogen zur Depressionsdiagnostik nach DSM-IV (FDD-DSMIV); Hogrefe: Göttingen, Germany, 1997. [Google Scholar]
- Svanborg, P.; Ekselius, L. Self-assessment of DSM-IV criteria for major depression in psychiatric out- and inpatients. Nord. J. Psychiatry 2003, 57, 291–296. [Google Scholar] [CrossRef] [PubMed]
- Spitzer, R.L.; Kroenke, K.; Williams, J.B. Validation and utility of a self-report version of PRIME-MD: The PHQ primary care study. Primary Care Evaluation of Mental Disorders. Patient Health Questionnaire. JAMA 1999, 282, 1737–1744. [Google Scholar] [CrossRef] [PubMed]
- Hung, C.-I.; Wang, S.-J.; Liu, C.-Y. Validation of the Depression and Somatic Symptoms Scale by comparison with the Short Form 36 scale among psychiatric outpatients with major depressive disorder. Depress. Anxiety 2009, 26, 583–591. [Google Scholar] [CrossRef] [PubMed]
- Spielberger, C.; Gorsuch, R.L.; Lushene, R.E. Manual for the State/Trait Anxiety Inventory; Consulting Psychologists Press: Palo Alto, CA, USA, 1970. [Google Scholar]
- Birmaher, B.; Khetarpal, S.; Brent, D.; Cully, M.; Balach, L.; Kaufman, J.; Neer, S.M. The Screen for Child Anxiety Related Emotional Disorders (SCARED): Scale construction and psychometric characteristics. J. Am. Acad. Child Adolesc. Psychiatry 1997, 36, 545–553. [Google Scholar] [CrossRef] [PubMed]
- Beck, A.T.; Epstein, N.; Brown, G.; Steer, R.A. An inventory for measuring clinical anxiety: Psychometric properties. J. Consult. Clin. Psychol. 1988, 56, 893–897. [Google Scholar] [CrossRef] [PubMed]
- Spence, S.H. A measure of anxiety symptoms among children. Behav. Res. Ther. 1998, 36, 545–566. [Google Scholar] [CrossRef]
- Spitzer, R.L.; Kroenke, K.; Williams, J.B.W.; Löwe, B. A Brief Measure for Assessing Generalized Anxiety Disorder. Arch. Intern. Med. 2006, 166, 1092. [Google Scholar] [CrossRef] [PubMed]
- Chorpita, B.F.; Yim, L.; Moffitt, C.; Umemoto, L.A.; Francis, S.E. Assessment of symptoms of DSM-IV anxiety and depression in children: A revised child anxiety and depression scale. Behav. Res. Ther. 2000, 38, 835–855. [Google Scholar] [CrossRef]
- Kunttu, K.; Pesonen, T. Student Health Survey 2012: A National Survey among Finnish University Students; Finnish Student Health Service; Ylioppilaiden Terveydenhoitosäätiön Tutkimuksia 47: Helsinki, Finland, 2013. [Google Scholar]
- Zigmond, A.S.; Snaith, R.P. The hospital anxiety and depression scale. Acta Psychiatr. Scand. 1983, 67, 361–370. [Google Scholar] [CrossRef] [PubMed]
- Achenbach, T. Manual for the Youth Self-Report and 1991 Profile; Department of Psychiatry, University of Vermont: Burlington, VT, USA, 1999. [Google Scholar]
- Reynolds, W. Reynolds Adolescent Adjustment Screening InventoryTM (RAASITM): Professional Manual; Psychological Assessment Resources: Lutz, FL, USA, 2001. [Google Scholar]
- Kessler, R.C.; Adler, L.; Ames, M.; Demler, O.; Faraone, S.; Hiripi, E.; Howes, M.J.; Jin, R.; Secnik, K.; Spencer, T.; et al. The World Health Organization Adult ADHD Self-Report Scale (ASRS): A short screening scale for use in the general population. Psychol. Med. 2005, 35, 245–256. [Google Scholar] [CrossRef] [PubMed]
- Goodman, R. The Strengths and Difficulties Questionnaire: A research note. J. Child Psychol. Psychiatry 1997, 38, 581–586. [Google Scholar] [CrossRef] [PubMed]
- DuPaul, G.J. Parent and Teacher Ratings of ADHD Symptoms: Psychometric Properties in a Community-Based Sample. J. Clin. Child Psychol. 1991, 20, 245–253. [Google Scholar] [CrossRef]
- American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders, 4th ed.; American Psychiatric Association Text Revision: Arlington, TA, USA, 2000. [Google Scholar]
- Connor, K.M.; Davidson, J.R.; Churchill, L.E.; Sherwood, A.; Foa, E.; Weisler, R.H. Psychometric properties of the Social Phobia Inventory (SPIN). New self-rating scale. Br. J. Psychiatry 2000, 176, 379–386. [Google Scholar] [CrossRef] [PubMed]
- Mattick, R.P.; Clarke, J.C. Development and validation of measures of social phobia scrutiny fear and social interaction anxiety. Behav. Res. Ther. 1998, 36, 455–470. [Google Scholar] [CrossRef]
- La Greca, A.M.; Stone, W.L. Social Anxiety Scale for Children-Revised: Factor Structure and Concurrent Validity. J. Clin. Child Psychol. 1993, 22, 17–27. [Google Scholar] [CrossRef]
- Derogatis, L.R. SCL-90-R. Administration, Scoring and Procedures Manual; Clinical Psychometric Research Inc.: Baltimore, MD, USA, 1990. [Google Scholar]
- Derogatis, L.R.; Melisaratos, N. The Brief Symptom Inventory: An introductory report. Psychol. Med. 1983, 13, 595–605. [Google Scholar] [CrossRef] [PubMed]
- Laurens, K.; Hodgins, S.; MaughanN, B.; Murray, R.; Rutter, M.; Taylor, E. Community screening for psychotic-like experiences and other putative antecedents of schizophrenia in children aged 9–12 years. Schizophr. Res. 2007, 90, 130–146. [Google Scholar] [CrossRef] [PubMed]
- STARCEVIC, V. Problematic Internet use: A distinct disorder, a manifestation of an underlying psychopathology, or a troublesome behaviour? World Psychiatry 2010, 9, 92–93. [Google Scholar] [CrossRef] [PubMed][Green Version]
- King, D.L.; Delfabbro, P.H.; Griffiths, M.D. Trajectories of Problem Video Gaming Among Adult Regular Gamers: An 18-Month Longitudinal Study. Cyberpsychol. Behav. Soc. Netw. 2013, 16, 72–76. [Google Scholar] [CrossRef] [PubMed]
- Monroe, J. Meta-Analysis for Observational Studies: Statistical Methods for Heterogeneity, Publication Bias and Combining Studies: Statistics; University of California: Los Angeles, CA, USA, 2007. [Google Scholar]
- Sutton, A.J. Methods for Meta-Analysis in Medical Research; J. Wiley: Chichester, UK, 2000; ISBN 9780471490661. [Google Scholar]
- Beutel, M.E.; Hoch, C.; Wölfling, K.; Müller, K.W. Clinical characteristics of computer game and internet addiction in persons seeking treatment in an outpatient clinic for computer game addiction. Z. Psychosom. Med. Psychother. 2011, 57, 77–90. [Google Scholar] [CrossRef] [PubMed]
- Batthyány, D.; Müller, K.W.; Benker, F.; Wölfling, K. Computer game playing: Clinical characteristics of dependence and abuse among adolescents. Wien. Klin. Wochenschr. 2009, 121, 502–509. [Google Scholar] [CrossRef] [PubMed]
- Goby, V.P. Personality and Online/Offline Choices: MBTI Profiles and Favored Communication Modes in a Singapore Study. Cyberpsychol. Behav. 2006, 9, 5–13. [Google Scholar] [CrossRef] [PubMed]
- González-Ibáñez, A.; Mora, M.; Gutiérrez-Maldonado, J.; Ariza, A.; Lourido-Ferreira, M.R. Pathological gambling and age: Differences in personality, psychopathology, and response to treatment variables. Addict. Behav. 2005, 30, 383–388. [Google Scholar] [CrossRef] [PubMed]
- Halpern-Felsher, B.L.; Cauffman, E. Costs and benefits of a decision: Decision-making competence in adolescents and adults. J. Appl. Dev. Psychol. 2001, 22, 257–273. [Google Scholar] [CrossRef]
- Lucas, K.; Sherry, J.L. Sex Differences in Video Game Play. Commun. Res. 2004, 31, 499–523. [Google Scholar] [CrossRef]
- Greenberg, B.S.; Sherry, J.; Lachlan, K.; Lucas, K.; Holmstrom, A. Orientations to Video Games Among Gender and Age Groups. Simul. Gaming 2010, 41, 238–259. [Google Scholar] [CrossRef]
- Young, K. Understanding Online Gaming Addiction and Treatment Issues for Adolescents. Am. J. Fam. Ther. 2009, 37, 355–372. [Google Scholar] [CrossRef]
- Floros, G.; Siomos, K. Patterns of Choices on Video Game Genres and Internet Addiction. Cyberpsychol. Behav. Soc. Netw. 2012, 15, 417–424. [Google Scholar] [CrossRef] [PubMed]
- Elliott, L.; Golub, A.; Ream, G.; Dunlap, E. Video Game Genre as a Predictor of Problem Use. Cyberpsychol. Behav. Soc. Netw. 2012, 15, 155–161. [Google Scholar] [CrossRef] [PubMed]
- King, D.; Delfabbro, P.; Griffiths, M. Video Game Structural Characteristics: A New Psychological Taxonomy. Int. J. Ment. Health Addict. 2010, 8, 90–106. [Google Scholar] [CrossRef]
- Petry, N.M.; Rehbein, F.; Gentile, D.A.; Lemmens, J.S.; Rumpf, H.-J.; Mößle, T.; Bischof, G.; Tao, R.; Fung, D.S.S.; Borges, G.; et al. An international consensus for assessing internet gaming disorder using the new DSM-5 approach. Addiction 2014, 109, 1399–1406. [Google Scholar] [CrossRef] [PubMed]
- Kuss, D.J.; Griffiths, M.D.; Pontes, H.M. Chaos and confusion in DSM-5 diagnosis of Internet Gaming Disorder: Issues, concerns, and recommendations for clarity in the field. J. Behav. Addict. 2017, 6, 103–109. [Google Scholar] [CrossRef] [PubMed]
- Bhandari, A.; Wagner, T. Self-Reported Utilization of Health Care Services: Improving Measurement and Accuracy. Med. Care Res. Rev. 2006, 63, 217–235. [Google Scholar] [CrossRef] [PubMed]
- Kaptsis, D.; King, D.; Delfabbro, P.; Gradisar, M. Withdrawal symptoms in internet gaming disorder: A systematic review. Clin. Psychol. Rev. 2016, 43, 58–66. [Google Scholar] [CrossRef] [PubMed]
| Source | Study Type | N | Population Age a | Sex | Country | IGD Measures | Psychopathology Measures | Psychopathology Outcome | Association | Effect Size | 95% CI of d |
|---|---|---|---|---|---|---|---|---|---|---|---|
| Baer et al., 2011 [24] | cross-sectional | 102 | adolescents 13.7 ± 1.9 | M/F | Canada | Computer/Gaming-station Addiction Scale (CGAS) | Strengths and Difficulties Questionnaire | Emotional problems | full | R2 = 0.29 | – |
| Hyperactivity | full | R2 = 0.18 | – | ||||||||
| Cole & Hooley, 2013 [25] | cross-sectional | 163 | general population 27.3 ± 9.1 | M/F | USA | Generalized Problematic Internet Use Scale (GPIUS) | State-Trait Anxiety Inventory (STAI) | Anxiety state | full | d = 0.26 | −0.05–0.57 |
| Anxiety trait | full | d = 1.07 | 0.74–1.40 | ||||||||
| Social Phobia Scale | Social phobia | full | d = 1.17 | 0.83–1.50 | |||||||
| Jiménez-Murcia et al., 2014 [26] | cross-sectional | 193 | adults with GD 42.4 ± 13.4 | M/F | Spain | Video-game Dependency Test (VDT) | Symptom Checklist 90-revision | Somatization | full | d = 0.57 | 0.16–0.983 |
| Obsessive-Compulsive | full | d = 0.84 | 0.424–1.257 | ||||||||
| Interpersonal Sensitivity | full | d = 0.76 | 0.341–1.169 | ||||||||
| Depression | full | d = 0.58 | 0.17–0.991 | ||||||||
| Anxiety | full | d = 0.64 | 0.216–1.064 | ||||||||
| Hostility | full | d = 0.68 | 0.255–1.106 | ||||||||
| Phobic-Anxiety | full | d = 0.55 | 0.127–0.973 | ||||||||
| Paranoid Ideation | full | d = 0.83 | 0.402–1.259 | ||||||||
| Psychoticism | full | d = 0.56 | 0.137–0.983 | ||||||||
| Kim et al., 2016 [27] | cross-sectional | 3041 | adults 20–49 | M/F | South Korea | IGD diagnostic criteria in DSM-5 | Brief Symptom Inventory (BSI) | Somatization | full | d = 1.59 | 1.481–1.703 |
| Obsessive-Compulsive | full | d = 1.67 | 1.557–1.78 | ||||||||
| Interpersonal Sensitivity | full | d = 1.61 | 1.499–1.721 | ||||||||
| Depression | full | d = 1.75 | 1.642–1.867 | ||||||||
| Anxiety | full | d = 1.75 | 1.642–1.866 | ||||||||
| Hostility | full | d = 1.72 | 1.61–1.834 | ||||||||
| Phobic-Anxiety | full | d = 1.82 | 1.705–1.928 | ||||||||
| Paranoid Ideation | full | d = 1.74 | 1.623–1.847 | ||||||||
| Psychoticism | full | d = 1.76 | 1.646–1.87 | ||||||||
| King et al., 2013 [28] | cross-sectional | 1287 | adolescents 12–18 | M/F | Australia | Pathological Technology Use (PTU) | Revised Children’s Anxiety and Depression Scale | Depression | none | – | |
| Obsessive-Compulsive Disorder (OCD) | none | – | |||||||||
| Anxiety | none | – | |||||||||
| King & Delfabbro, 2016 [29] | cross-sectional | 824 | adolescents 14.1 ± 1.5 | M/F | Australia | IGD Diagnostic criteria in DSM-5 | Depression Anxiety Stress Scales, 21-item version | Depression | full * | d = 0.62 | 0.087–1.155 |
| Anxiety | full * | d = 0.50 | −0.035–1.025 | ||||||||
| Laconi et al., 2017 [30] | cross-sectional | 418 | adults 21.9 ± 3 | M/F | France | Internet Gaming Disorder Test-10 (IGDT-10) | Center for Epidemiologic Studies, Depression Scale-10 | Depression | full | d = 2.687 | 1.969–3.405 |
| Männikkö et al., 2015 [31] | cross-sectional | 293 | general population 18.7 ± 3.4 | M/F | Finland | Gaming Addiction Scale (GAS) | School Health Promotion (SHP) | Depression | full | R2 = 0.17 | - |
| Anxiety | full | R2 = 0.11 | - | ||||||||
| Mentzoni, et al., 2011 [32] | cross-sectional | 816 | general population 15–40 | M/F | Norway | Gaming Addiction Scale for Adolescents (GASA) | Hospital Anxiety and Depression Scale (HADS) | Depression | full | n/a | - |
| Anxiety | full | n/a | - | ||||||||
| Müller et al., 2015 [33] | cross-sectional | 12,938 | adolescents 15.8 ± 0.7 | M/F | Germany | Assessment of Internet and Computer Game Addiction (AICGA) | Youth Self-Report | Anxious-Depression | full | d = 0.34 | 0.183–0.496 |
| Withdrawn-Depression | full | d = 0.35 | 0.347–0.507 | ||||||||
| Na et al., 2017 [34] | cross-sectional | 1819 | adults 20–49 | M/F | South Korea | IGD diagnostic criteria in DSM-5 | Symptom Checklist 90-revision | Depression | full | n/a | - |
| Anxiety | full | n/a | - | ||||||||
| Starcevic et al., 2011 [35] | cross-sectional | 1945 | general population over 14 | M/F | Australia | Video-Game Use Questionnaire (VGUQ) | Symptom Checklist 90 | Somatization | partial> | d = 1.02 | 0.854–1.187 |
| Obsessive-Compulsive | partial | d = 1.365 | 1.196–1.534 | ||||||||
| Interpersonal Sensitivity | partial | d = 1.228 | 1.059–1.396 | ||||||||
| Depression | partial | d = 1.264 | 1.096–1.433 | ||||||||
| Anxiety | partial> | d = 1.149 | 0.981–1.317 | ||||||||
| Hostility | partial> | d = 1.276 | 1.108–1.445 | ||||||||
| Phobic-Anxiety | partial> | d = 1.131 | 0.964–1.299 | ||||||||
| Paranoid Ideation | partial> | d = 1.203 | 1.035–1.371 | ||||||||
| Psychoticism | partial> | d = 1.368 | 1.199–1.537 | ||||||||
| Stetina et al., 2011 [36] | cross-sectional | 468 | general population 11–67 | M/F | Austria | Problematic Internet use scale (ISS-20) | Questionnaire for depression diagnostics (FDD for DSM-IV) | Depression | none | - | - |
| Strittmatter et al., 2015 [37] | cross-sectional | 9758 | adolescents 15.0 ± 1.3 | M/F | Germany | Young Diagnostic Questionnaire (YDQ) | Beck Depression Inventory II | Depression | full | d = 0.58 | 0.449–0.702 |
| Strengths and Difficulties Questionnaire (SDQ) | Hyperactivity | full | d = 0.53 | 0.399–0.652 | |||||||
| Vadlin et al., 2016 [38] | cross-sectional | N1 (1868) N2 (242) | adolescents 12–18 | M/F | Sweden | Gaming Addiction Identification (GAIT) | Depression Self-Rating Scale (DSRS-A) | Depression | full | OR 2.47 (1.44–4.25) | - |
| Spence Children‘s Anxiety Scale (SCAS) | Anxiety | full | OR 2.06 (1.27–3.33) | - | |||||||
| Adult ADHD Self-Report Scale (ASRS-A) | Attention Deficit Hyperactivity Disorder (ADHD) | full | OR 2.43 (1.44–4.11) | - | |||||||
| Psychotic-like experiences (PLEs) | Psychoticism | none | - | - | |||||||
| Wang et al., 2018 [39] | cross-sectional | 7200 | general population 14–39 | M/F | South Korea | IGD diagnostic criteria in DSM-5 | Patient Health Questionnaire9 (PHQ9) | Depression | full | n/a | - |
| Generalized Anxiety Disorder Scale (GAD-7) | Anxiety | n/a | - | - | |||||||
| Wartberg et al., 2017 [40] | cross-sectional | 1095 | adolescents 13.0 ± 0.82 | M/F | Germany | Internet Gaming Disorder Scale (IGDS) | Reynolds Adolescent Adjustment Screening Inventory | Depression and anxiety | full | OR 1.09 (1.02–1.17) | - |
| Hyperactivity | full | OR 1.27 (1.16–1.39) | - | ||||||||
| Wei et al., 2012 [41] | cross-sectional | 722 | general population 21.8 ± 4.9 | M/F | Taiwan | Chen’s Internet Addiction Scale (CIAS) | Depression and Somatic Symptoms Scale (DSSS) | Depression | full | R2 = 0.298 | - |
| Social Phobia Inventory (SPIN) | Social phobia | full | n/a | - | |||||||
| Panagiotidi, 2017 [42] | cross-sectional | 205 | adults 27.4 ± 10 | M/F | United Kingdom | Problem Video-Game Playing Test (PVGT) | ADHD Self-Report Scale (ASRS) | ADHD | full | R2 = 0.22 | - |
| Gentile et al., 2011 [43] | Longitudinal | 3034 | children, adolescents 11.2 ± 2.06 | M/F | Singapore | Pathological Technology Use (PTU) | Asian Adolescent Depression Scale (AADS) | Depression | full | R2 = 0.49 | - |
| Child Anxiety-Related Emotional Disorders (SCARED) | Anxiety | full | R2 = 0.29 | - | |||||||
| Adult ADHD Self-Report Scale (ASRS-A) | ADHD | none | - | - | |||||||
| Social Phobia Inventory (SPIN) | Social phobia | full | R2 = 0.20 | - | |||||||
| Van Rooij et al., 2011 [44] | Longitudinal | T1 (1572) T2 (1476) | children 13–16 | M/F | Deutschland | Compulsive Internet Use Scale (CIUS) | Depressive Mood List | T1: Depression T2: Depression | none full # | n/a | - |
| Revised Social Anxiety Scale for Children | T1: Social anxiety T2: Social anxiety | none none | - | - | |||||||
| Hyun et al., 2015 [45] | case-control | 308 | general population 21.0 ± 5.9 | M/F | South Korea | Young Internet Addiction Scale (YIAS) | Beck Depressive Inventory (BDI) | Depression | full | d = 1.09 | 0.88–1.305 |
| Beck Anxiety Scale (BAI) | Anxiety | full | d = 0.64 | 0.437–0.845 | |||||||
| Dupaul’s ADHD scale (K-ARS) | ADHD | full | d = 1.05 | 0.838–1.262 | |||||||
| Yen et al., 2016 [46] | case-control | 174 | adults 23.29 ± 2.34 23.38 ± 2.40 | M/F | Taiwan | Semi-structured interview with the DSM-5 IGD criteria | ADHD DSM-IV-TR criteria diagnosis for adult and childhood | ADHD | full | OR 13.51 (4.49–40.64) | - |
| Brunborg et al., 2014 [47] | cohort | 1928 | adolescents 13–17 | M/F | Norway | Game Addiction Scale for Adolescents (GASA) | Hopkins Symptom Checklist | Depression | T1: full other time: none | R2 = 0.25 | - - |
| Effect Size | Depression | Anxiety | ADHD/Hyper-Activity | Social Phobia/Anxiety |
|---|---|---|---|---|
| Small a | 2 | 2 | 2 | 0 |
| Moderate b | 3 | 5 | 1 | 0 |
| Large c | 8 | 2 | 4 | 2 |
| None | 2 | 1 | 1 | 1 |
| Total | 15 | 10 | 8 | 3 |
© 2018 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
González-Bueso, V.; Santamaría, J.J.; Fernández, D.; Merino, L.; Montero, E.; Ribas, J. Association between Internet Gaming Disorder or Pathological Video-Game Use and Comorbid Psychopathology: A Comprehensive Review. Int. J. Environ. Res. Public Health 2018, 15, 668. https://doi.org/10.3390/ijerph15040668
González-Bueso V, Santamaría JJ, Fernández D, Merino L, Montero E, Ribas J. Association between Internet Gaming Disorder or Pathological Video-Game Use and Comorbid Psychopathology: A Comprehensive Review. International Journal of Environmental Research and Public Health. 2018; 15(4):668. https://doi.org/10.3390/ijerph15040668
Chicago/Turabian StyleGonzález-Bueso, Vega, Juan José Santamaría, Daniel Fernández, Laura Merino, Elena Montero, and Joan Ribas. 2018. "Association between Internet Gaming Disorder or Pathological Video-Game Use and Comorbid Psychopathology: A Comprehensive Review" International Journal of Environmental Research and Public Health 15, no. 4: 668. https://doi.org/10.3390/ijerph15040668
APA StyleGonzález-Bueso, V., Santamaría, J. J., Fernández, D., Merino, L., Montero, E., & Ribas, J. (2018). Association between Internet Gaming Disorder or Pathological Video-Game Use and Comorbid Psychopathology: A Comprehensive Review. International Journal of Environmental Research and Public Health, 15(4), 668. https://doi.org/10.3390/ijerph15040668





