Association between Cervical Spondylosis and Migraine: A Nationwide Retrospective Cohort Study
Abstract
1. Introduction
2. Methods
2.1. Data Source
2.2. Sampled Participants
2.3. Outcome and Comorbidities
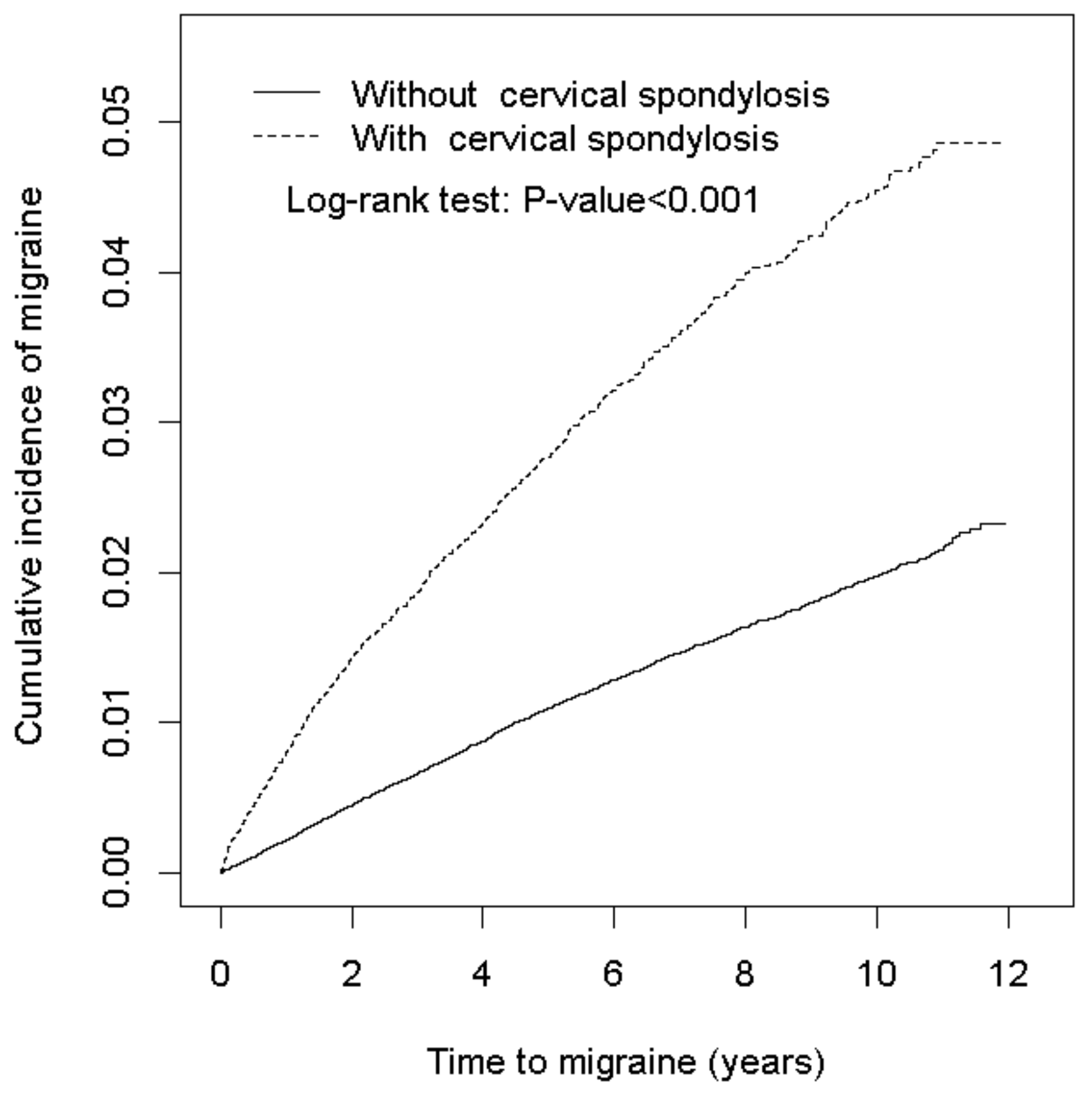
2.4. Statistical Analysis
3. Results
4. Discussion
5. Conclusions
Acknowledgments
Author Contributions
Conflicts of Interest
Abbreviations
| CS | cervical spondylosis |
| HR | hazard ratio |
| CI | confidence interval |
| NHIRD | National Health Insurance Research Database |
| LHID2000 | Longitudinal Health Insurance Database 2000 |
| ICD-9-CM | International Classification of Diseases, Ninth Revision, Clinical Modification |
References
- Vos, T.; Abajobir, A.A.; Abbafati, C.; Abate, K.H.; Abbas, K.M.; Abd-Allah, F.; Abdulkader, R.S.; Abdulle, A.M.; Abebo, T.A.; Abera, S.F.; et al. Global, regional, and national incidence, prevalence, and years lived with disability for 328 diseases and injuries for 195 countries, 1990–2016: A systematic analysis for the Global Burden of Disease Study 2016. Lancet 2017, 390, 1211–1259. [Google Scholar] [CrossRef]
- Steiner, T.J.; Stovner, L.J.; Vos, T.; Jensen, R.; Katsarava, Z. Migraine is first cause of disability in under 50s: Will health politicians now take notice? J. Headache Pain 2018, 19, 17. [Google Scholar] [CrossRef] [PubMed]
- Bloudek, L.M.; Stokes, M.; Buse, D.C.; Wilcox, T.K.; Lipton, R.B.; Goadsby, P.J.; Varon, S.F.; Blumenfeld, A.M.; Katsarava, Z.; Pascual, J.; et al. Cost of healthcare for patients with migraine in five European countries: Results from the International Burden of Migraine Study (IBMS). J. Headache Pain 2012, 13, 361–378. [Google Scholar] [CrossRef] [PubMed]
- Costa, C.; Tozzi, A.; Rainero, I.; Cupini, L.M.; Calabresi, P.; Ayata, C.; Sarchielli, P. Cortical spreading depression as a target for anti-migraine agents. J. Headache Pain 2013, 14, 62. [Google Scholar] [CrossRef] [PubMed]
- Akerman, S.; Holland, P.R.; Goadsby, P.J. Diencephalic and brainstem mechanisms in migraine. Nat. Rev. Neurosci. 2011, 12, 570–584. [Google Scholar] [CrossRef] [PubMed]
- Olesen, J.; Burstein, R.; Ashina, M.; Tfelt-Hansen, P. Origin of pain in migraine: Evidence for peripheral sensitisation. Lancet Neurol. 2009, 8, 679–690. [Google Scholar] [CrossRef]
- Gasparini, C.F.; Smith, R.A.; Griffiths, L.R. Genetic and biochemical changes of the serotonergic system in migraine pathobiology. J. Headache Pain 2017, 18, 20. [Google Scholar] [CrossRef] [PubMed]
- Tajti, J.; Vecsei, L. The mechanism of peripheral and central sensitization in migraine. A literature review. Neuropsychopharmacol. Hung. 2009, 11, 15–21. [Google Scholar] [PubMed]
- Martin, P.R. Behavioral Management of Migraine Headache Triggers: Learning to Cope with Triggers. Curr. Pain Headache Rep. 2010, 14, 221–227. [Google Scholar] [PubMed]
- Levy, D.; Strassman, A.M.; Burstein, R. A Critical View on the Role of Migraine Triggers in the Genesis of Migraine Pain. Headache 2009, 49, 953–957. [Google Scholar] [CrossRef] [PubMed]
- Biondi, D.M. Cervicogenic headache: A review of diagnostic and treatment strategies. J. Am. Osteopath. Assoc. 2005, 105, 16S–22S. [Google Scholar] [PubMed]
- Kaniecki, R.G. Migraine and tension-type headache—An assessment of challenges in diagnosis. Neurology 2002, 58, S15–S20. [Google Scholar] [PubMed]
- Escher, C.M.; Paracka, L.; Dressler, D.; Kollewe, K. Botulinum toxin in the management of chronic migraine: Clinical evidence and experience. Ther. Adv. Neurol. Disord. 2017, 10, 127–135. [Google Scholar] [CrossRef] [PubMed]
- Szok, D.; Csati, A.; Vecsei, L.; Tajti, J. Treatment of Chronic Migraine with OnabotulinumtoxinA: Mode of Action, Efficacy and Safety. Toxins 2015, 7, 2659–2673. [Google Scholar] [CrossRef] [PubMed]
- Robbins, M.S.; Kuruvilla, D.; Blumenfeld, A.; Charleston, L.; Sorrell, M.; Robertson, C.E.; Grosberg, B.M.; Bender, S.D.; Napchan, U.; Ashkenazi, A. Trigger point injections for headache disorders: Expert consensus methodology and narrative review. Headache 2014, 54, 1441–1459. [Google Scholar] [CrossRef] [PubMed]
- Fernandez-de-las-Penas, C.; Cuadrado, M.L. Therapeutic options for cervicogenic headache. Expert Rev. Neurother. 2014, 14, 39–49. [Google Scholar] [PubMed]
- Martinovic, Z.; Buder, N.; Velickovic, R.; Milovanovic, M. Comorbidity of migraine and somatic diseases. Med. Pregl. 2005, 58, 342–346. [Google Scholar] [PubMed]
- Database NHIR. Taiwan. 2016. Available online: http://nhird.nhri.org.tw/en/index.html (accessed on 28 June 2016).
- Hu, W.S.; Lin, C.L. CHA2DS2-VASc score for ischaemic stroke risk stratification in patients with chronic obstructive pulmonary disease with and without atrial fibrillation: A nationwide cohort study. EP Eur. 2017. [Google Scholar] [CrossRef] [PubMed]
- Lee, C.W.; Lin, C.L.; Lin, P.Y.; Thielke, S.; Su, K.P.; Kao, C.H. Antidepressants and risk of dementia in migraine patients: A population-based case-control study. Prog. Neuropsychopharmacol. Biol. Psychiatry 2017, 77, 83–89. [Google Scholar] [PubMed]
- Wang, S.J.; Fuh, J.L.; Huang, S.Y.; Yang, S.S.; Wu, Z.A.; Hsu, C.H.; Wang, C.H.; Yu, H.Y.; Wang, P.J.; Taiwan MAP Study Group. Diagnosis and development of screening items for migraine in neurological practice in Taiwan. J. Formos. Med. Assoc. 2008, 107, 485–494. [Google Scholar] [PubMed]
- Blau, J.N.; MacGregor, E.A. Migraine and the neck. Headache 1994, 34, 88–90. [Google Scholar] [CrossRef] [PubMed]
- Haldeman, S.; Dagenais, S. Cervicogenic headaches: A critical review. Spine J. 2001, 1, 31–46. [Google Scholar] [CrossRef]
- Schrot, R.J.; Mathew, J.S.; Li, Y.; Beckett, L.; Bae, H.W.; Kim, K.D. Headache relief after anterior cervical discectomy: Post hoc analysis of a randomized investigational device exemption trial. J. Neurosurg. Spine 2014, 21, 217–222. [Google Scholar] [CrossRef] [PubMed]
- Riina, J.; Anderson, P.A.; Holly, L.T.; Flint, K.; Davis, K.E.; Riew, K.D. The Effect of an Anterior Cervical Operation for Cervical Radiculopathy or Myelopathy on Associated Headaches. J. Bone Joint Surg. Am. 2009, 91A, 1919–1923. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Marcus, D.A.; Scharff, L.; Mercer, S.; Turk, D.C. Musculoskeletal abnormalities in chronic headache: A controlled comparison of headache diagnostic groups. Headache 1999, 39, 21–27. [Google Scholar] [CrossRef] [PubMed]
- Vetvik, K.G.; MacGregor, E.A. Sex differences in the epidemiology, clinical features, and CrossMark pathophysiology of migraine. Lancet Neurol. 2017, 16, 76–87. [Google Scholar] [CrossRef]
- Wang, C.; Tian, F.; Zhou, Y.; He, W.; Cai, Z. The incidence of cervical spondylosis decreases with aging in the elderly, and increases with aging in the young and adult population: A hospital-based clinical analysis. Clin. Interv. Aging 2016, 11, 47–53. [Google Scholar] [PubMed]
- Woolf, C.J. Central sensitization: Implications for the diagnosis and treatment of pain. Pain 2011, 152, S2–S15. [Google Scholar] [CrossRef] [PubMed]
- Takano, M.; Kawabata, S.; Komaki, Y.; Shibata, S.; Hikishima, K.; Toyama, Y.; Okano, H.; Nakamura, M. Inflammatory cascades mediate synapse elimination in spinal cord compression. J. Neuroinflamm. 2014, 11, 40. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Beattie, M.S.; Manley, G.T. Tight squeeze, slow burn: Inflammation and the aetiology of cervical myelopathy. Brain 2011, 134, 1259–1261. [Google Scholar] [CrossRef] [PubMed]
- Murphy, R.K.J.; Sun, P.; Xu, J.Q.; Wang, Y.; Sullivan, S.; Gamble, P.; Wagner, J.; Wright, N.N.; Dorward, I.G.; Riew, D.; et al. Magnetic Resonance Imaging Biomarker of Axon Loss Reflects Cervical Spondylotic Myelopathy Severity. Spine 2016, 41, 751–756. [Google Scholar] [CrossRef] [PubMed]
- Allison, D.J.; Ditor, D.S. Immune dysfunction and chronic inflammation following spinal cord injury. Spinal Cord 2015, 53, 14–18. [Google Scholar] [CrossRef] [PubMed]
- Steilen, D.; Hauser, R.; Woldin, B.; Sawyer, S. Chronic neck pain: Making the connection between capsular ligament laxity and cervical instability. Open Orthop. J. 2014, 8, 326–345. [Google Scholar] [PubMed]
- Menezes, A.H. Craniovertebral junction database analysis: Incidence, classification, presentation, and treatment algorithms. Childs Nerv. Syst. 2008, 24, 1101–1108. [Google Scholar] [CrossRef] [PubMed]
- Mitchell, J. Vertebral Artery Blood flow Velocity Changes Associated with Cervical Spine rotation: A Meta-Analysis of the Evidence with implications for Professional Practice. J. Man. Manip. Ther. 2009, 17, 46–57. [Google Scholar] [CrossRef] [PubMed]
- Watson, D.H.; Drummond, P.D. Head pain referral during examination of the neck in migraine and tension-type headache. Headache 2012, 52, 1226–1235. [Google Scholar] [CrossRef] [PubMed]
- Fernandez-de-Las-Penas, C.; Cuadrado, M.L.; Pareja, J.A. Myofascial trigger points, neck mobility and forward head posture in unilateral migraine. Cephalalgia 2006, 26, 1061–1070. [Google Scholar] [CrossRef] [PubMed]
- Fernandez-de-Las-Penas, C. Myofascial Head Pain. Curr. Pain Headache Rep. 2015, 19, 28. [Google Scholar] [CrossRef] [PubMed]
- Noseda, R.; Constandil, L.; Bourgeais, L.; Chalus, M.; Villanueva, L. Changes of meningeal excitability mediated by corticotrigeminal networks: A link for the endogenous modulation of migraine pain. J. Neurosci. 2010, 30, 14420–14429. [Google Scholar] [CrossRef] [PubMed]
- Sauro, K.M.; Becker, W.J. The stress and migraine interaction. Headache 2009, 49, 1378–1386. [Google Scholar] [CrossRef] [PubMed]
- Revanappa, K.K.; Moorthy, R.K.; Alexander, M.; Rajshekhar, V. Recovery of sympathetic skin response after central corpectomy in patients with moderate and severe cervical spondylotic myelopathy. Br. J. Neurosurg. 2017, 31, 199–204. [Google Scholar] [CrossRef] [PubMed]
- Li, J.; Gu, T.; Yang, H.; Liang, L.; Jiang, D.J.; Wang, Z.C.; Yuan, W.; Wang, X.W. Sympathetic nerve innervation in cervical posterior longitudinal ligament as a potential causative factor in cervical spondylosis with sympathetic symptoms and preliminary evidence. Med. Hypotheses 2014, 82, 631–635. [Google Scholar] [CrossRef] [PubMed]
- Gu, Q.G.; Jiang, D.J.; Wang, X.W.; Chen, D.Y.; Yuan, W. Chronic compression of the posterior longitudinal ligament of the cervical spine is associated with abnormal discharge of middle cervical ganglion. Int. J. Clin. Exp. Med. 2014, 7, 4316–4321. [Google Scholar] [PubMed]
- Peng, K.P.; Wang, S.J. Migraine diagnosis: Screening items, instruments, and scales. Acta Anaesthesiol. Taiwan 2012, 50, 69–73. [Google Scholar] [CrossRef] [PubMed]
| Variable | Cervical Spondylosis | ||
|---|---|---|---|
| No | Yes | Standard Mean Difference | |
| (N =111,720) | (N =27,930) | ||
| Sex | 0.99 | ||
| Women | 63,592(56.9) | 15,898(56.9) | |
| Men | 48,128(43.1) | 12,032(43.1) | |
| Age stratified | 0.99 | ||
| ≤49 | 40,452(36.2) | 10,113(36.2) | |
| 50–64 | 41,880(37.5) | 10,470(37.5) | |
| 65+ | 29,388(26.3) | 7347(26.3) | |
| Age, mean ± SD a | 55.1(14.0) | 55.6(13.6) | <0.001 |
| Comorbidity | |||
| Hypertension | 36,886(33.0) | 11,658(41.7) | <0.001 |
| Hyperlipidemia | 22,730(20.4) | 8887(31.8) | <0.001 |
| Depression | 4498(4.03) | 2252(8.06) | <0.001 |
| Coronary artery disease | 17,160(15.4) | 6941(24.9) | <0.001 |
| Anxiety | 10,300(9.22) | 5607(20.1) | <0.001 |
| Sleep disorder | 20,851(18.7) | 9450(33.8) | <0.001 |
| Irritable bowel syndrome | 4969(4.45) | 2487(8.90) | <0.001 |
| Diabetes | 10,876(9.74) | 3182(11.4) | <0.001 |
| Fibromyalgia | 4599(4.12) | 2984(10.7) | <0.001 |
| Variable | Event | PY | Rate # | Crude HR (95% CI) | Adjusted HR & (95% CI) |
|---|---|---|---|---|---|
| Cervical spondylosis | |||||
| No | 1414 | 677,913 | 2.09 | 1.00 | 1.00 |
| Yes | 883 | 171,179 | 5.16 | 2.48(2.28, 2.69) *** | 2.03(1.86, 2.22) *** |
| Age group, year | |||||
| 20−49 | 997 | 330,050 | 3.02 | 1.46(1.31, 1.64) *** | 1.81(1.58, 2.06) *** |
| 50−64 | 874 | 317,220 | 2.76 | 1.32(1.18, 1.48) *** | 1.40(1.24, 1.58) *** |
| ≥65 | 426 | 201,822 | 2.11 | 1.00 | 1.00 |
| Sex | |||||
| Female | 1719 | 494,959 | 3.47 | 2.14(1.95, 2.35) *** | 1.92(1.74, 2.11) *** |
| Male | 578 | 354,133 | 1.63 | 1.00 | 1.00 |
| Comorbidity | |||||
| Hypertension | |||||
| No | 1465 | 570,275 | 2.57 | 1.00 | 1.00 |
| Yes | 832 | 278,816 | 2.98 | 1.15(1.06, 1.25) ** | 1.06(0.95, 1.18) |
| Hyperlipidemia | |||||
| No | 1698 | 668,229 | 2.54 | 1.00 | 1.00 |
| Yes | 599 | 180,862 | 3.31 | 1.29(1.17, 1.41) *** | 1.01(0.91, 1.12) |
| Depression | |||||
| No | 2090 | 813,829 | 2.57 | 1.00 | 1.00 |
| Yes | 207 | 35,263 | 5.87 | 2.24(1.94, 2.58) *** | 1.13(0.97, 1.32) |
| Coronary artery disease | |||||
| No | 1800 | 711,569 | 2.53 | 1.00 | 1.00 |
| Yes | 497 | 137,523 | 3.61 | 1.42(1.28, 1.56) *** | 1.20(1.07, 1.35) ** |
| Anxiety | |||||
| No | 1785 | 764,303 | 2.34 | 1.00 | 1.00 |
| Yes | 512 | 84,789 | 6.04 | 2.53(2.30, 2.80) *** | 1.48(1.32, 1.66) *** |
| Sleep disorder | |||||
| No | 1444 | 690,750 | 2.09 | 1.00 | 1.00 |
| Yes | 853 | 158,342 | 5.39 | 2.52(2.31, 2.74) *** | 1.81(1.64, 1.99) *** |
| Irritable bowel syndrome | |||||
| No | 2105 | 809,522 | 2.60 | 1.00 | 1.00 |
| Yes | 192 | 39,569 | 4.85 | 1.83(1.57, 2.12) *** | 1.24(1.06,1.44) ** |
| Diabetes | |||||
| No | 2112 | 775,714 | 2.72 | 1.00 | 1.00 |
| Yes | 185 | 73,378 | 2.52 | 0.91(0.78, 1.05) | - |
| Fibromyalgia | |||||
| No | 2127 | 808,699 | 2.63 | 1.00 | 1.00 |
| Yes | 170 | 4093 | 4.21 | 1.57(1.34, 1.83) *** | 1.08(0.92, 1.27) |
| Variable | Cervical spondylosis | |||||||
|---|---|---|---|---|---|---|---|---|
| No | Yes | Crude HR (95% CI) | Adjusted HR & (95% CI) | |||||
| Event | PY | Rate # | Event | PY | Rate # | |||
| Sex | ||||||||
| Women | 1082 | 395,676 | 2.73 | 637 | 99,282 | 6.42 | 2.35(2.13, 2.59) *** | 1.93(1.74, 2.14) *** |
| Men | 332 | 282,237 | 1.18 | 246 | 71,896 | 3.42 | 2.91(2.47, 3.44) *** | 2.32(1.95, 2.76) *** |
| Stratify age | ||||||||
| ≤49 | 620 | 264,087 | 2.35 | 377 | 65,963 | 5.72 | 2.44(2.14, 2.77) *** | 1.94(1.70, 2.23) *** |
| 50–64 | 532 | 253,619 | 2.10 | 342 | 63,600 | 5.38 | 2.56(2.24, 2.94) *** | 2.05(1.78, 2.36) *** |
| 65+ | 377 | 160,207 | 1.64 | 164 | 41,615 | 3.94 | 2.42(1.99, 2.94) *** | 2.08(1.70, 2.55) *** |
| Comorbidity ‡ | ||||||||
| No | 520 | 342,246 | 1.52 | 180 | 49,454 | 3.64 | 2.40(2.02, 2.84) *** | 2.36(1.99, 2.80) *** |
| Yes | 894 | 335,667 | 2.66 | 703 | 121,725 | 5.78 | 2.19(1.98, 2.41) *** | 2.10(1.91, 2.32) *** |
| Variable | N | Events | PYs | Rate # | Crude HR (95% CI) | Adjusted HR & 95% CI) |
|---|---|---|---|---|---|---|
| Without cervical spondylosis | 111,720 | 1414 | 677,913 | 2.09 | 1.00 | 1.00 |
| Type of Cervical spondylosis | ||||||
| Cervical spondylosis without myelopathy | 24,287 | 771 | 150,298 | 5.13 | 2.47(2.26, 2.69 ) *** | 2.01(1.83, 2.20) *** |
| Cervical spondylosis with myelopathy | 3643 | 112 | 20,880 | 5.36 | 2.55(2.10, 3.09) *** | 2.19(1.80, 2.66) *** |
© 2018 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Lin, W.-S.; Huang, T.-F.; Chuang, T.-Y.; Lin, C.-L.; Kao, C.-H. Association between Cervical Spondylosis and Migraine: A Nationwide Retrospective Cohort Study. Int. J. Environ. Res. Public Health 2018, 15, 587. https://doi.org/10.3390/ijerph15040587
Lin W-S, Huang T-F, Chuang T-Y, Lin C-L, Kao C-H. Association between Cervical Spondylosis and Migraine: A Nationwide Retrospective Cohort Study. International Journal of Environmental Research and Public Health. 2018; 15(4):587. https://doi.org/10.3390/ijerph15040587
Chicago/Turabian StyleLin, Wang-Sheng, Tung-Fu Huang, Tien-Yow Chuang, Cheng-Li Lin, and Chia-Hung Kao. 2018. "Association between Cervical Spondylosis and Migraine: A Nationwide Retrospective Cohort Study" International Journal of Environmental Research and Public Health 15, no. 4: 587. https://doi.org/10.3390/ijerph15040587
APA StyleLin, W.-S., Huang, T.-F., Chuang, T.-Y., Lin, C.-L., & Kao, C.-H. (2018). Association between Cervical Spondylosis and Migraine: A Nationwide Retrospective Cohort Study. International Journal of Environmental Research and Public Health, 15(4), 587. https://doi.org/10.3390/ijerph15040587





