The Healthy Primary School of the Future: A Contextual Action-Oriented Research Approach
Abstract
:1. Background
2. Methods
2.1. The Healthy Primary School of the Future
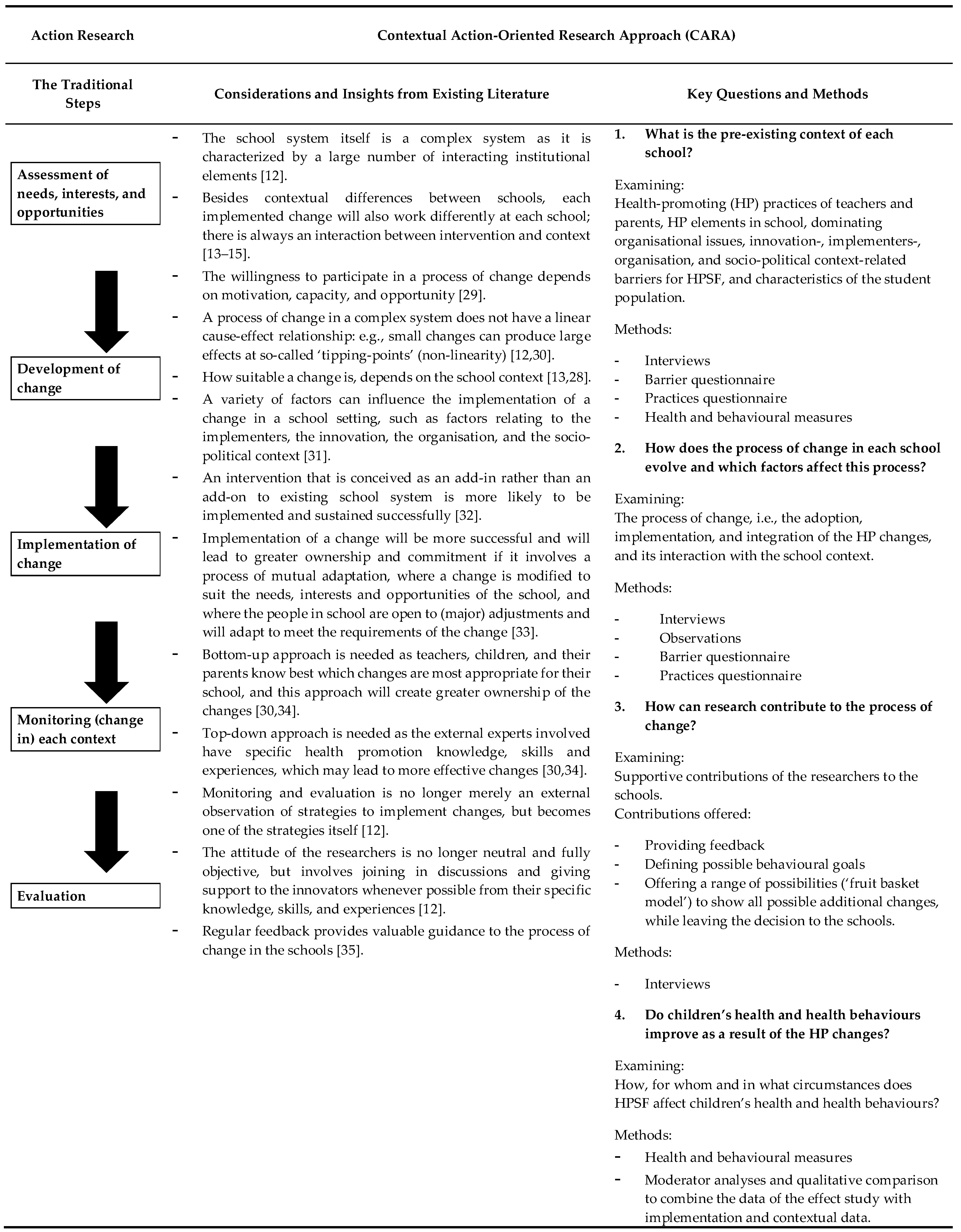
2.2. Contextual Action-Oriented Research Approach (CARA)
2.2.1. What Is the Pre-Existing Context of Each School?
2.2.2. How Does the Process of Change in Each School Evolve and Which Factors Affect This Process?
2.2.3. How Can Research Contribute to the Process of Change?
2.2.4. Do Children’s Health and Health Behaviours Improve as a Result of the HP Changes?
3. Discussion
4. Conclusions
Supplementary Materials
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Arcaya, M.C.; Arcaya, A.L.; Subramanian, S. Inequalities in health: Definitions, concepts, and theories. Glob. Health Action 2015, 8, 27106. [Google Scholar] [CrossRef] [PubMed]
- Marmot, M.; Allen, J.; Bell, R.; Bloomer, E.; Goldblatt, P. WHO European review of social determinants of health and the health divide. Lancet 2012, 380, 1011–1029. [Google Scholar] [CrossRef]
- Ogden, C.L.; Carroll, M.D.; Flegal, K.M. Epidemiologic trends in overweight and obesity. Endocrinol. Metab. Clin. 2003, 32, 741–760. [Google Scholar] [CrossRef]
- Suhrcke, M.; de Paz Nieves, C. The Impact of Health and Health Behaviours on Educational Outcomes in High-Income Countries: A Review of the Evidence; World Health Organization, Regional Office for Europe: Copenhagen, Denmark, 2011. [Google Scholar]
- Verrotti, A.; Penta, L.; Zenzeri, L.; Agostinelli, S.; De Feo, P. Childhood obesity: Prevention and strategies of intervention. A systematic review of school-based interventions in primary schools. J. Endocrinol. Investig. 2014, 37, 1155–1164. [Google Scholar] [CrossRef] [PubMed]
- Lohrmann, D.K. A complementary ecological model of the coordinated school health program. Public Health Rep. 2008, 123, 695–703. [Google Scholar] [CrossRef] [PubMed]
- Gubbels, J.S.; Van Kann, D.H.; de Vries, N.K.; Thijs, C.; Kremers, S.P. The next step in health behavior research: The need for ecological moderation analyses-an application to diet and physical activity at childcare. Int. J. Behav. Nutr. Phys. Act. 2014, 11, 52. [Google Scholar] [CrossRef] [PubMed]
- Leurs, M.T.; Schaalma, H.P.; Jansen, M.W.; Mur-Veeman, I.M.; Leger, L.H.S.; De Vries, N. Development of a collaborative model to improve school health promotion in the Netherlands. Health Promot. Int. 2005, 20, 296–305. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Lytle, L.A.; Seifert, S.; Greenstein, J.; McGovern, P. How do children’s eating patterns and food choices change over time? Results from a cohort study. Am. J. Health Promot. 2000, 14, 222–228. [Google Scholar] [CrossRef] [PubMed]
- Bonell, C.; Humphrey, N.; Fletcher, A.; Moore, L.; Anderson, R.; Campbell, R. Why schools should promote students’ health and wellbeing. BMJ 2014, 348, g3078. [Google Scholar] [CrossRef] [PubMed]
- Brown, T.; Summerbell, C. Systematic review of school-based interventions that focus on changing dietary intake and physical activity levels to prevent childhood obesity: An update to the obesity guidance produced by the National Institute for Health and Clinical Excellence. Obes. Rev. 2009, 10, 110–141. [Google Scholar] [CrossRef] [PubMed]
- Patton, M.Q. Developmental Evaluation: Applying Complexity Concepts to Enhance Innovation and Use; Guilford Press: New York, NY, USA, 2011. [Google Scholar]
- Moore, G.F.; Audrey, S.; Barker, M.; Bond, L.; Bonell, C.; Hardeman, W.; Moore, L.; O’Cathain, A.; Tinati, T.; Wight, D.; et al. Process evaluation of complex interventions: Medical Research Council guidance. BMJ 2015, 350, h1258. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Pawson, R.; Tilley, N. Realistic Evaluation; Sage: London, UK, 1997. [Google Scholar]
- Darlington, E.J.; Simar, C.; Jourdan, D. Implementation of a health promotion programme: A ten-year retrospective study. Health Education 2017, 117, 252–279. [Google Scholar] [CrossRef]
- Jansen, M.; Kuppens, E. Op Zoek Naar de Limburg-Factor [Finding the Limburg Factor]; GGD Zuid Limburg: Geleen, The Netherlands, 2015. [Google Scholar]
- Steenbakkers, M.; Vermeer, A.J.M.; Janssen-Goffin, M.J.H.; Hajema, K.J. Een Nieuwe Kijk op Gezondheid in Zuid-Limburg. Regionaal Rapport Volksgezondheid Toekomstverkenning 2014. [A New Look at Health in Southern Limburg. Public Health Status and Forecasts 2014]; GGD Zuid-Limburg [Regional Public Health Services Southern Limburg]: Geleen, The Netherlands, 2014. [Google Scholar]
- Willeboordse, M.; Jansen, M.; van den Heijkant, S.; Simons, A.; Winkens, B.; de Groot, R.; Bartelink, N.; Kremers, S.P.; van Assema, P.; Savelberg, H.H.; et al. The Healthy Primary School of the Future: Study protocol of a quasi-experimental study. BMC Public Health 2016, 16, 639. [Google Scholar] [CrossRef] [PubMed]
- Vermeer, A.J.M.B.N.; Hesdahl, M.H.; Janssen-Goffin, M.J.H.; Linssen, E.C.A.J.; Rutten, N.; Hajema, K.J. Lokale Rapporten Volksgezondheid Toekomst Verkenning: Een Nieuwe kijk op Gezondheid in Heerlen, Kerkrade, Landgraaf en Brunssum; [Local Reports on Public Health Development: A New Perspective on Health in Heerlen, Kerkrade, Landgraaf and Brunssum]; GGD Zuid Limburg: Geleen, The Netherlands, 2014. [Google Scholar]
- Jungbluth, P. De Opbrengst van Basisscholen in Zuid-Limburg in 2009 en 2010. [The Proceeds of Primary Schools in South Limburg in 2009 and 2010]; Maastricht University: Maastricht, The Netherlands, 2011. [Google Scholar]
- Schils, T. Leerlingen in Het Voortgezet Onderwijs: Wie Zitten Daar? Hoe Zitten ze in Hun vel? Hoe Slim zijn ze? [Pupils in Secondary Education: Who Are They? What is Their Sense of Self-Worth? How Smart Are They?]; Kaans Reports K04201102-K04201104; Kaans/Maastricht University School of Business and Economics: Maastricht, The Netherlands, 2011. [Google Scholar]
- Lee, A. Health-promoting schools. Appl. Health Econ. Health Policy 2009, 7, 11–17. [Google Scholar] [CrossRef] [PubMed]
- Boot, N.M.; van Assema, P.; Hesdahl, B.; Leurs, M.; de Vries, N.K. Gezondheidsbevordering en voortgezet onderwijs: Verstandshuwelijk of echte liefde? [Health promotion and secondary education: Marriage of convenience or true love?]. Tijdschrift voor Gezondheidswetenschappen 2010, 88, 127–135. [Google Scholar] [CrossRef]
- Mertler, C.A. Action Research: Improving Schools and Empowering Educators; Sage Publications: Thousand Oaks, CA, USA, 2016. [Google Scholar]
- Boot, N.; van Assema, P.; Hesdahl, B.; de Vries, N. Professional assistance in implementing school health policies. Health Educ. 2010, 110, 294–308. [Google Scholar] [CrossRef]
- Rutter, H.; Savona, N.; Glonti, K.; Bibby, J.; Cummins, S.; Finegood, D.T.; Greaves, F.; Harper, L.; Hawe, P.; Moore, L.; et al. The need for a complex systems model of evidence for public health. Lancet 2017. [Google Scholar] [CrossRef]
- Hawe, P.; Shiell, A.; Riley, T. Complex interventions: How “out of control” can a randomised controlled trial be? BMJ 2004, 328, 1561. [Google Scholar] [CrossRef] [PubMed]
- Poland, B.; Krupa, G.; McCall, D. Settings for health promotion: An analytic framework to guide intervention design and implementation. Health Promot. Pract. 2009, 10, 505–516. [Google Scholar] [CrossRef] [PubMed]
- Michie, S.; van Stralen, M.M.; West, R. The behaviour change wheel: A new method for characterising and designing behaviour change interventions. Implement. Sci. 2011, 6, 42. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Van Kann, D.H.; Jansen, M.; de Vries, S.; de Vries, N.; Kremers, S. Active Living: Development and quasi-experimental evaluation of a school-centered physical activity intervention for primary school children. BMC Public Health 2015, 15, 1315. [Google Scholar] [CrossRef] [PubMed]
- Fleuren, M.A.; Paulussen, T.G.; Van Dommelen, P.; Van Buuren, S. Towards a measurement instrument for determinants of innovations. Int. J. Qual. Health Care 2014, 26, 501–510. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Nielsen, G.; Mygind, E.; Bølling, M.; Otte, C.R.; Schneller, M.B.; Schipperijn, J.; Ejbye-Ernst, N.; Bentsen, P. A quasi-experimental cross-disciplinary evaluation of the impacts of education outside the classroom on pupils’ physical activity, well-being and learning: The TEACHOUT study protocol. BMC Public Health 2016, 16, 1117. [Google Scholar] [CrossRef] [PubMed]
- Reiser, B.J.; Spillane, J.P.; Steinmuler, F.; Sorsa, D.; Carney, K.; Kyza, E. (Eds.) Investigating the mutual adaptation process in teachers’ design of technology-infused curricula. In Proceedings of the Fourth International Conference of the Learning Sciences, Ann Arbor, MI, USA, 14–17 June 2000; Erlbaum: Mahwah, NJ, USA, 2000. [Google Scholar]
- Laverack, G.; Labonte, R. A planning framework for community empowerment goals within health promotion. Health Policy Plan. 2000, 15, 255–262. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Waterman, H.; Tillen, D.; Dickson, R.; De Koning, K. Action Research: A Systematic Review and Guidance for Assessment; Health Technology Assessment: Winchester, UK, 2000; Volume 5. [Google Scholar]
- Green, L.; Kreuter, M. The Precede–Proceed model. In Health Promotion Planning: An Educational Approach, 3rd ed.; Mayfield Publishing Company: Mountain View, CA, USA, 1999; pp. 32–43. [Google Scholar]
- Konijnendijk, A.A.; Boere-Boonekamp, M.M.; Fleuren, M.A.; Haasnoot, M.E.; Need, A. What factors increase Dutch child health care professionals’ adherence to a national guideline on preventing child abuse and neglect? Child Abus. Neglect. 2016, 53, 118–127. [Google Scholar] [CrossRef] [PubMed]
- Verberne, L.M.; Kars, M.C.; Schepers, S.A.; Schouten-van Meeteren, A.Y.; Grootenhuis, M.A.; van Delden, J.J. Barriers and facilitators to the implementation of a paediatric palliative care team. BMC Palliat. Care 2018, 17, 23. [Google Scholar] [CrossRef] [PubMed]
- Gevers, D.W. Parental Influences on Child Snacking: Advancing Research; Maastricht University: Maastricht, The Netherlands, 2016. [Google Scholar]
- O’Connor, T.M.; Cerin, E.; Hughes, S.O.; Robles, J.; Thompson, D.I.; Mendoza, J.A.; Baranowski, T.; Lee, R.E. Psychometrics of the preschooler physical activity parenting practices instrument among a Latino sample. Int. J. Behav. Nutr. Phys. Act. 2014, 11, 3. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Gevers, D.W.; Kremers, S.P.; de Vries, N.K.; van Assema, P. Patterns of food parenting practices and children’s intake of energy-dense snack foods. Nutrients 2015, 7, 4093–4106. [Google Scholar] [CrossRef] [PubMed]
- Gubbels, J.S.; Sleddens, E.F.; Raaijmakers, L.C.; Gies, J.M.; Kremers, S.P. The Child-care Food and Activity Practices Questionnaire (CFAPQ): Development and first validation steps. Public Health Nutr. 2016, 19, 1964–1975. [Google Scholar] [CrossRef] [PubMed]
- Kremers, S.P.; de Bruijn, G.-J.; Droomers, M.; van Lenthe, F.; Brug, J. Moderators of environmental intervention effects on diet and activity in youth. Am. J. Prev. Med. 2007, 32, 163–172. [Google Scholar] [CrossRef] [PubMed]
- Green, J.; Tones, K. For debate. Towards a secure evidence base for health promotion. J. Public Health 1999, 21, 133–139. [Google Scholar] [CrossRef] [Green Version]
| Physical Activity | Healthy Nutrition |
|---|---|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
© 2018 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Bartelink, N.H.M.; Van Assema, P.; Jansen, M.W.J.; Savelberg, H.H.C.M.; Willeboordse, M.; Kremers, S.P.J. The Healthy Primary School of the Future: A Contextual Action-Oriented Research Approach. Int. J. Environ. Res. Public Health 2018, 15, 2243. https://doi.org/10.3390/ijerph15102243
Bartelink NHM, Van Assema P, Jansen MWJ, Savelberg HHCM, Willeboordse M, Kremers SPJ. The Healthy Primary School of the Future: A Contextual Action-Oriented Research Approach. International Journal of Environmental Research and Public Health. 2018; 15(10):2243. https://doi.org/10.3390/ijerph15102243
Chicago/Turabian StyleBartelink, Nina H. M., Patricia Van Assema, Maria W. J. Jansen, Hans H. C. M. Savelberg, Maartje Willeboordse, and Stef P. J. Kremers. 2018. "The Healthy Primary School of the Future: A Contextual Action-Oriented Research Approach" International Journal of Environmental Research and Public Health 15, no. 10: 2243. https://doi.org/10.3390/ijerph15102243
APA StyleBartelink, N. H. M., Van Assema, P., Jansen, M. W. J., Savelberg, H. H. C. M., Willeboordse, M., & Kremers, S. P. J. (2018). The Healthy Primary School of the Future: A Contextual Action-Oriented Research Approach. International Journal of Environmental Research and Public Health, 15(10), 2243. https://doi.org/10.3390/ijerph15102243






