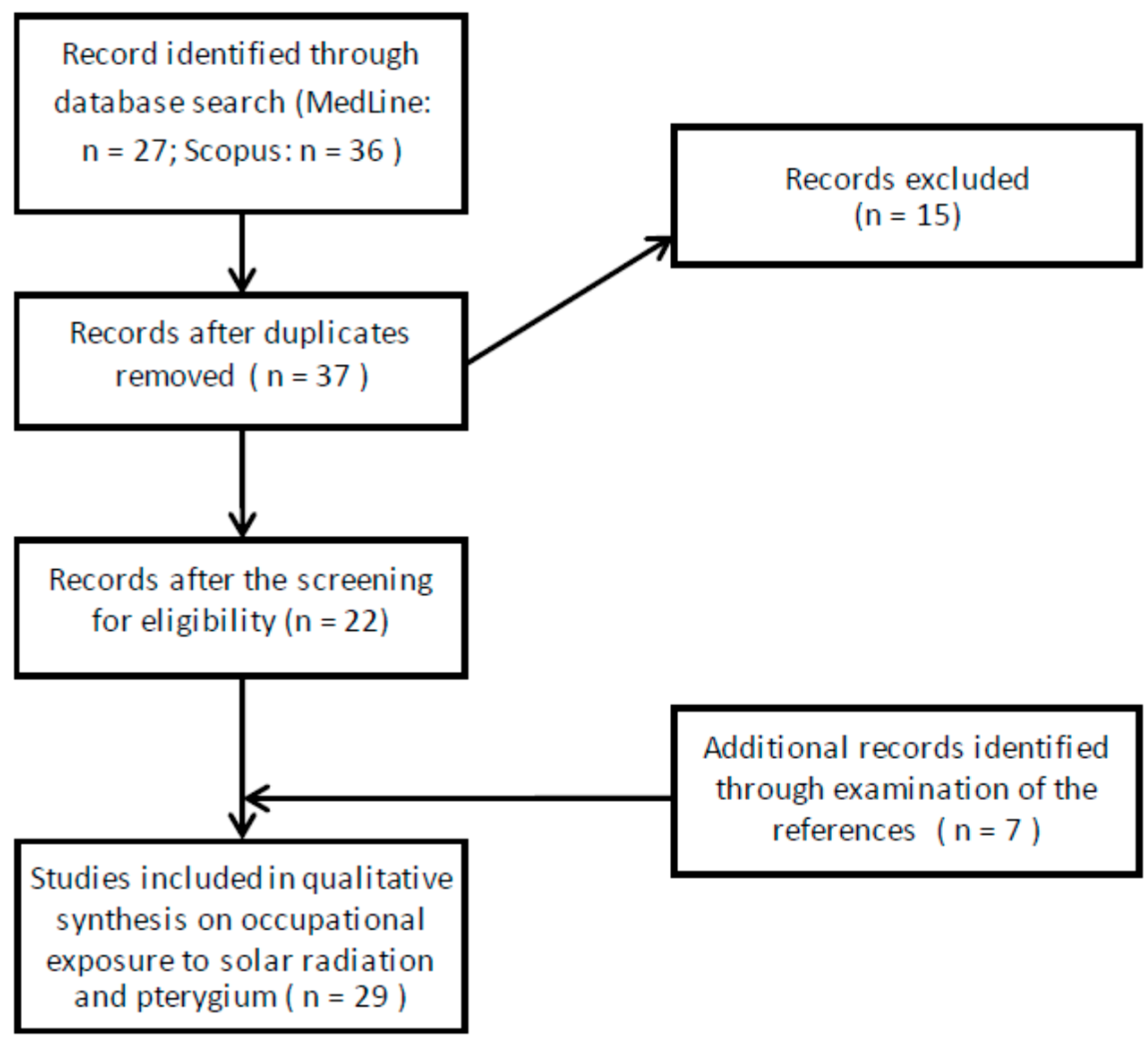
3.1. Areas at Moderate UV Risk
Six studies on occupational exposure to solar radiation and pterygium have been found in areas at moderate risk considering the mean annual UV index in last ten years: 1 from Europe (Spain) [
17], 2 from China [
18,
19] and 3 from South Korea [
20,
21,
22] (
Table 2).
Viso et al. (2011) [
17] evaluated pterygium prevalence in North-West Spain in 619 subjects >40 years, of which 37.0% were males. Pterygium prevalence was 5.9%, increasing significantly with age (
p < 0.005), and was higher in females (6.5% vs. 4.8% in males). Pterygium was significantly associated with outdoor activity, with an OR of 2.28 (95% CI: 1.04–4.98). Another factor positively associated with the disease was fluorescein staining (OR = 2.64; 95% CI: 1.08–6.46).
In China (Beijing area) the longitudinal study of Zhao et al. (2013) [
18] found a 10-Years pterygium incidence in 2628 subjects (mean age 40 years at the baseline, pterygium prevalence = 2.5% of 2695 subjects) of 4.9%. Farmers were more frequently represented in pterygium group and the OR at the univariate analysis was 3.67 (95% CI: 2.5–5.4) versus non farmers, but the association was not significant at multivariate analysis (
p = 0.47), where only the rural region of habitation (
p < 0.001) and a lower fasting blood glucose concentration (
p = 0.009) were significant. In the rural area of North China Li et al. [
19] investigated 8445 subjects, aged >18 years: the overall pterygium prevalence was 2.5% (1.2% bilateral) (95% confidence interval (CI): 1.0–1.4%). According to multivariable analysis, pterygium presence was significantly associated with outdoor work (OR: 1.8; 95% CI: 1.2–2.6), but also with age >70 years (OR: 29.0; 95% CI: 13.6–61.6) and male sex (OR: 1.9; 95% CI: 1.4–2.6), while no association was found for smoke and alcohol use history.
Three large national South-Korean studies have been included in the review [
20,
21,
22]. Lim et al. [
20] collected data from a large sample of 13,204 individuals (age 40 years or older), 821 diagnosed with pterygium and 12,383 controls. The frequency of outdoor workers was higher in cases than in controls (38.2% vs. 21.9%,
p < 0.001), but in a multivariate analysis only the reporting of >5 h per day outdoor was significantly associated (OR: 1.47; 95% CI: 1.11–1.94). Other risk factors identified were age (OR: 1.05; 95% CI: 1.05–1.06) and male gender (OR: 1.28; 95% CI: 1.01–1.61) and lower level of education (OR: 3.98; 95% CI: 2.24–7.06), while urban residency was negatively associated (OR: 0.56; 95% CI: 0.45–0.70). In another South Korean population based study, Nam et al. [
21] investigated 16,234 adults with an overall pterygium prevalence of 7.1%. Outdoor workers were more represented in the pterygium group compared to controls, both in males (2.6% vs. 1%,
p < 0.001) and in females (2.9% vs. 0.7%,
p < 0.001). Also the reporting of ≥5 h per day of sun exposure was positively associated: 2.6% vs. 0.9% in males (
p < 0.001) and 3% vs. 0.7% in females (
p < 0.001). This study was primarily aimed to investigate the association between pterygium and obesity, finding a significant association in obese women: OR = 1.35 (95% CI: 1.02–1.77). Finally, in the 2 years prospective study of Lee et al. [
22] on 9839 adults aged 19–74 years, pterygium incidence was of 6%. Pterygium frequency was almost 3 times higher in OW than in indoor workers (OR: 3.1; 95% CI: 1.9–4.8 at a multiple logistic regression analysis). Low educational status and longer working hours were also significantly associated.
3.2. Areas at High UV Risk
Four studies on occupational exposure to solar radiation and pterygium have been found in areas at high risk considering the mean annual UV index in last ten years (
Table 3): 2 from Iran [
23,
24], 1 from Japan [
25] and 1 from U.S. [
26].
Rezvan et al. [
23] reported on 5190 people from the urban population of Shahroud (Iran), who underwent an ophthalmological examination: pterygium prevalence was 9.4% (95% CI: 8.6–10.3), 2.9% (95% CI: 2.4–3.3) bilateral. A significant difference in pterygium prevalence was found between OWs and indoor workers (14.7% vs. 8.4%); furthermore, the prevalence of pterygium in OWs spending half time outdoor and half time indoor was 9.3%, compared to 14.7% in full time OW: the difference is significant (
p < 0.001), supporting an exposure-effect relation. Pterygium was found to be significantly associated also with male sex (11.4% in males vs. 8.0%), and with age only in females. The other risk factor observed was a low educational level: pterygium prevalence was higher in illiterates than in subjects with a college education (16.5% vs. 5.4%,
p < 0.001). In the other Iranian study Malekifar et al. [
24] investigated 210 pterygium or pinguecula cases and an equal number of controls from the dry and high altitude province of Ilam. Outdoor occupation (
p < 0.001) and also welding experience (
p < 0.001) were significantly associated with pterygium at the univariate analysis, while in multivariate analysis only family history of pterygium, cigarette smoking, history of baking, age and severe blepharitis were significantly associated (
p < 0.001,
p < 0.001,
p = 0.002,
p = 0.023 and
p = 0.002, respectively) and, among OWs, only farmers showed a significant OR of 3.84 (95% CI: 1.01–14.67,
p = 0.049) for having pterygium.
Tano et al. [
25] provided an ocular examination to 2312 subjects in Northern Japan, mean age 64.3 years: pterygium prevalence was 4.4%. OW were more represented in the pterygium group than in controls (29.7% vs. 22.3%), with a slightly higher prevalence of 5.7% (OR = 1.47; 95% CI: 0.9–2.3, not significant) and in particular in those with a bilateral disease (36.1% vs. 22.5%, OR = 1.95; 95% CI: 0.98–3.9, not significant). Only age was found to be significantly associated with pterygium in a multivariate analysis.
In the 2009 study of West et al. [
26] a population-based sample of 4774 Hispanic subjects aged >40 years and living in Arizona (US) was collected. The participants were examined by an ophthalmologist and the pterygium prevalence was 24% in men, compared with 11% in women. OWs were more likely to be male, with low economic income and low educational level: both these three factors were significantly associated with the presence of pterygium. Male sex was associated with an OR = 2.67 (95% CI: 2.2–3.2). A low educational level was positively associated with an OR = 2.8 (95% CI: 2.2–3.6) for less than 6 years spent at school in total and also for a period of 6–11 years (OR = 1.8; 95% CI: 1.4–2.2) versus those with a scholarity higher than 11 years in total. Also the mean annual economic income was significant different between pterygium group and controls, adjusted for age and sex (
p < 0.001). Other factors associated were the history of diabetes (
p = 0.03), smoke (
p = 0.02) and of bilateral cataract surgery (
p = 0.004), while hypertension, alcohol use and any cataract presence were found to be not associated.
3.3. Areas at Very High UV Risk
Seven studies on occupational exposure to solar radiation and pterygium have been found in areas at very high risk considering the mean annual UV index in last ten years (
Table 4): 1 study from the Norfolk Islands in Australia [
27], 5 studies from Asia, of which 2 from South China [
28,
29], 1 from South Japan [
30], 1 from North India [
31] and 1 from Taiwan [
32], and 1 study from the Hawaii islands in U.S. [
33].
The Australian study by Sherwin et al. (2008) [
27] was aimed to investigate the association between conjunctival ultraviolet autofluorescence (UVAF), a biomarker of ocular UVR exposure, and pterygium. 641 residents aged ≥15 years of the Norfolk Island in the South Pacific completed a sun exposure questionnaire and underwent autorefraction and ocular examination. The overall pterygium prevalence was 10.9%, higher in males (15% vs. 7.7% in females,
p = 0.003). Spending more than three-quarters of the day outside was significantly associated with pterygium presence at a multivariate analysis with an OR of 2.22 (95% CI: 1.20–4.09,
p = 0.011). Males who spent more than the 75% of the day in outdoor activities were more likely to be OW. Other positively associated factors with pterygium were UVAF per 10 mmq (OR 1.16; 95% CI: 1.16–1.28) and a tanning skin phenotype (OR 2.17; 95% CI: 1.20–3.92).
Zhong et al. [
28] investigated a large Bai nationality group in south-west China with 2133 subjects >50 years: pterygium was associated with outdoor work with an OR of 1.51 (95% CI: 1.10–1.92). Other factors associated were increasing age (significant OR ranging from 1.47 to 1.79 according to the age group, female sex (OR: 1.42; 95% CI: 1.08–1.88), low education level (OR: 1.26; 95% CI: 1.03–1.56), while BMI, hypertension, diabetes, smoking and alcohol use history were not associated. The same Bai group was investigated after 5 years by Li et al. (2015) [
29] to determine the 5-year pterygium incidence, that was of 6.8% (95% CI: 5.2–8.4), significantly higher in women than in men (8.8% vs. 3.8%;
p = 0.003). Outdoor occupation was the only significant associated variable at multivariate analysis: OR = 2.52 (95% CI: 1.27–4.95).
A Japanese study [
30] was conducted in the population aged >40 years on Kumejima Island: 3762 subjects were examined and pterygium prevalence was 30.8% (13.1% bilateral). History of outdoor work was found to be significantly associated with a higher pterygium risk in a logistic regression analysis: OR = 1.82 (95% CI: 1.33 to 2.50). The frequency of OWs was 77.8% in the pterygium group vs. 59.0% in controls (
p < 0.001). Considering the main occupations, farmers were the 31.8% of the pterygium group vs. the 22.4% of the controls (
p < 0.001), and fishermen were 4.2% vs. 2.4% (
p = 0.003). Other positive associations with pterygium were found for older age (OR = 1.02; 95% CI: 1.01–1.03), male sex (OR = 1.33; 95% CI: 1.03–1.63), hyperopic refraction (OR = 1.08; 95% CI: 1.03–1.13), while a negative association was found with the values of the intraocular pressure (OR = 0.96; 95% CI: 0.94–0.98).
In a nine months prospective study conducted in Northern India [
31] on 200 patients treated for pterygium, Authors observed that the frequency of the disease increased with the numbers of hours usually worked outdoor (6–8 h on average), not further quantifying this suggested association.
The Taiwanese study of Chen et al. [
32] conducted in the rural area of the Chiayi County (South Taiwan) considered 2197 subjects aged >40 years: pterygium prevalence was 25.2%, increasing with age (30.1% in subjects 60–60 years,
p < 0.0001). OWs were found to be at a higher risk for having pterygium, with an OR of 1.47 (95% CI: 1.17–1.86). Other risk factors were male sex (OR = 1.31; 95% CI: 1.08–1.60), smoking history (OR = 1.36; 95% CI: 1.02–1.83) and living in a seaside area (OR = 1.65; 95% CI: 1.35–2.03).
Finally, a U.S. study [
33] was conducted in the Oahu Island, Hawaii, in a group of 169 subjects aged 18–80 years: 52.1% were non-surfers, 24.3% occasional surfers, 8.9% recreational surfers and 14.8% professional surfers, based on their lifetime surfing hours. The overall pterygium prevalence was 11.9% (5.3% bilateral). Also the history of outdoor occupation, other than professional surfing, was significantly associated with pterygium (
p = 0.04), as well as lifetime surfing hours (
p < 0.0001). Other associated factors were Hawaiian residence (
p = 0.009) and Hawaiian/Pacific Islander ethnicity (
p = 0.002).
3.4. Areas at Extremely High UV Risk
Twelve studies were conducted in world areas at extremely high risk according to the mean annual UVI: three in Africa (Ghana [
34], Nigeria [
35] and Ethiopia [
36]), two in Central/South America (Barbados [
37] and Brazil [
38]) and seven in Asia (four from South India [
39,
40,
41,
42], one from Thailand [
43] and two from Singapore [
44,
45]) (
Table 5).
In Africa, Essuman et al. [
34] performed a prospective study of 60 consecutive patients from Ghana, aged 17–75 years, treated for primary pterygium with a surgical excision and then followed after the operation for 30 months. 58% of the patients were females. The overall frequency of pterygium recurrence was 37%. No significant association was found between pterygium recurrence and outdoor occupation. The study by Achigbu and Ezepue [
35] investigated a group of 615 commercial motorcyclists, mean age 38.1 years, in South-Eastern Nigeria. The prevalence of pterygium was 19.3%. Considering the severity of the disease, the majority of these OW had an early stage lesion (52%), while the 46% of the sample had a medium stage and the remaining 2% had the most severe lesions. Pterygium was significantly associated with the length of employment as commercial riders (
p = 0.009). Furthermore, the authors reported a lack of protective effect of regular use of sunglasses during work (
p = 0.188). Anbesse et al. [
36] studied pterygium prevalence in 390 subjects, mean age 38.7 years, living in Northwest Ethiopia, finding that the 38.7% of the participants were affected by the disease. OWs resulted at a significantly higher risk for pterygium (OR = 3.8; 95% CI: 2.18–6.46), and the regular use of sunglasses and hat was a protective factor (OR = 0.40; 95% CI: 0.2–0.78). Other associated factors were age classes (OR = 2.20; 95% CI: 1.22–3.39 for the age class 41–60 years, OR = 7.97; 95% CI: 2.74–23.17 for the age class 61–86 years), male sex (OR = 2.20; 95% CI: 1.28–3.82), use of traditional eye medications (OR = 2.55; 95% CI: 1.04–5.9) and inheritance for pterygium (OR = 6.68; 95% CI: 2.53–17.6).
Considering Central/South American studies, Nemesure et al. [
37] conducted a longitudinal study in the Barbados Islands, evaluating the nine-year incidence of pterygium in a sample of 1888 participants, aged 40–84 years at the baseline. After a 9-year follow up the development of pterygium was observed in the 11.6% of the subjects, for an average of 1.3% incidence per year, with no significant association with increasing age. OW were found at a higher risk for pterygium occurrence at a multivariate analysis (OR = 1.51: 95% CI: 1.05–2.16). Darker skin pigmentation and glasses/contact lenses use were reported to be significant protective factors (OR = 0.67; 95% CI: 0.46–0.97 and OR = 0.58; 95% CI: 0.42–0.81, respectively). Another South American study was conducted by Coutts et al. in Amazonia region of Brazil in 2011 [
38]. The study included 225 subjects aged >20 years living in three different places: Manaus city (
n = 89), on the riverside (
n = 116) and inside the rainforest (
n = 20). Pterygium prevalence was 52%, lower in Manaus city, higher close to the river (62.5%) and much higher inside the rainforest (75%). Overall, the 46% of the subjects had a bilateral lesion. Among the rainforest inhabitants, the percentage of OW reached the 70%, and the 67% of people living on the riverside, while OWs were only the 31% of the Manaus participants. In this group, subjects who worked outdoor showed an increase in the severity of pterygium: OWs represented the 57% of the subjects with grade 2 pteygium in this group, while they were the 93.3% of patients with a grade 3 lesion (
p = 0.0001) and the 100% of the subjects with the most severe lesions (grade 4,
p = 0.0004).
Among the seven Asian studies, four were from South India [
38,
39,
40,
41]: in these studies outdoor workers were found to be at risk for pterygium development with a significant OR = 1.8 (95% CI: 1.5–2.2,
p < 0.001) in the large population study conducted by Marmamula et al. [
40] in 10,293 subjects, while in the study by Asokan et al. [
38] considering the general population of an urban and a rural district (7774 subjects) the type of work was not associated with pterygium: only rural residence and higher lifetime UV exposure were significantly associated with the presence of pterygium (
p < 0.0001). In these two studies also other pterygium risk factors were considered: Asokan et al. found a pterygium prevalence of 9.5%, higher in subjects reporting a non-use of glasses (OR: 1.41; 95% CI: 1.12–1.79), while smoking, use of alcohol, diabetes and hypertension were not associated. Marmamula et al. found that the prevalence of pterygium (mean 11.7%) increased with age and for those who lived in rural areas (OR = 1.8, 95% CI: 10.9–12.6), while higher education level had a protective effect (OR = 0.6; 95% CI: 0.5–0.7;
p < 0.001). The prospective study of Salagar et al. (2013) [
41] on South-Indian patients treated for pterygium showed that the 80% of 100 patients followed for 1 year were OWs, with a higher frequency of complicated pterygia (X
2 = 7.7,
p < 0.001). Another Indian study was conducted in 331 salt workers with a mean age of 41.9 years by Cherian et al. [
39]: these OWs were exposed to sunlight with high reflections and the pterygium prevalence was 13%, higher in males.
A study conducted in Thailand (Artornsombudh et al. [
42]) was aimed to investigate the prevalence of conjunctival neoplasia in patients diagnosed for pterygium: 482 subjects, mean age 56.5 years, were studied and the prevalence of conjunctival epithelial neoplasia was approximately 1.8%. Among the patients, the 53.7% were farmers, 18.7% laborers, 4.6% merchants, 1% truck drivers and 22% pure indoor workers.
In Singapore the prevalence of pterygium in an urban Malay population of 3280 subjects aged 40–79 years (Cajucom et al. [
43]) was 12.3% (4.9% bilateral). The severity of pterygium was graded on 3 levels, and the history of outdoor occupation was associated only with severe pterygium (Grade 3) at multivariate analysis (OR = 2.2; 95% CI: 1.1–4.5,
p = 0.03). Pterygium of any grade was independently associated with increasing age (OR = 1.3; 95% CI: 1.1–1.4), male sex (OR = 1.9; 95% CI: 1.5–2.6) and high systolic blood pressure (OR = 1.6; 95% CI: 1.2–2.1). The other study performed in Singapore by Ang et al. (2012) [
44] considered three different ethnic groups Malays, Indians and Chinese persons >40 years of age for a total of 8906 participants who underwent an ocular examination. The overall pterygium prevalence was 10.1%, while severe pterygium was diagnosed in 1.6% of the subjects. The prevalence was higher in Malays (15.5%) than in Chinese (7.0%;
p < 0.001) or Indians (7.0%;
p < 0.001). Only severe pterygium was associated with outdoor occupation (OR = 2.1; 95% CI: 1.1–4.0;
p = 0.02), and the ethnic group did not affected this association. Other pterygium associated factors in a multivariate analysis were increasing age (
p < 0.001), male sex (
p < 0.001) and low education level (
p < 0.001).