Maternal Depressive Symptoms and Child Behavior among Mexican Women and Their Children
Abstract
:1. Introduction
2. Materials and Methods
2.1. Data Collection
2.2. Sample
2.3. Measures
2.3.1. Child Behavior Problems
2.3.2. Maternal Depressive Symptoms
2.3.3. Household-Level Measures
2.4. Statistical Analysis
2.5. Ethical Review
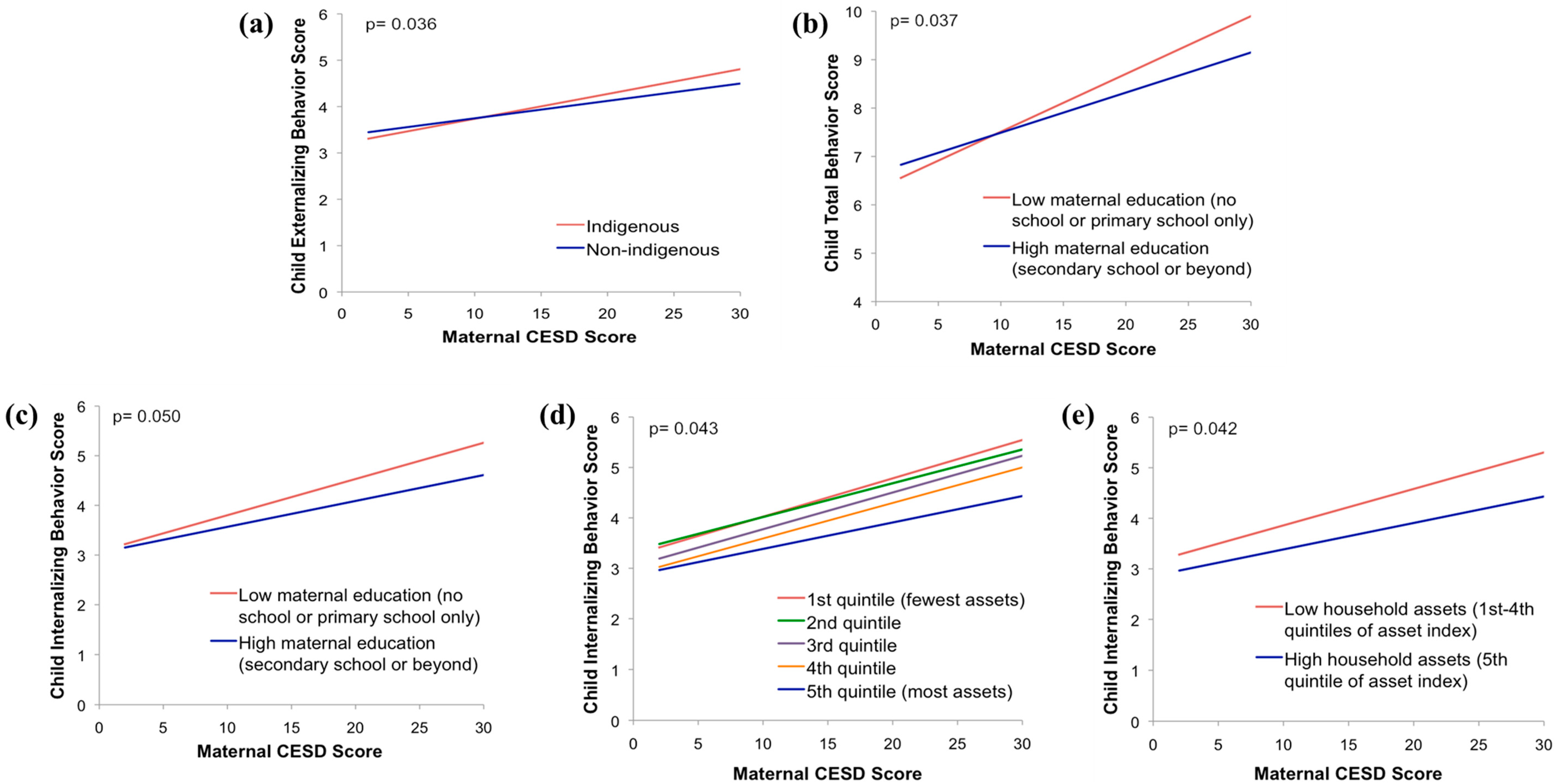
3. Results
4. Discussion
5. Conclusions
Supplementary Materials
Acknowledgments
Author Contributions
Conflicts of Interest
References
- Moussavi, S.; Chatterji, S.; Verdes, E.; Tandon, A.; Patel, V.; Ustun, B. Depression, chronic diseases, and decrements in health: Results from the World Health Surveys. Lancet 2007, 370, 851–858. [Google Scholar] [CrossRef]
- Shidhaye, P.; Giri, P. Maternal depression: A hidden burden in developing countries. Ann. Med. Health Sci. Res. 2014, 4, 463–465. [Google Scholar] [CrossRef] [PubMed]
- Lund, C.; Breen, A.; Flisher, A.J.; Kakuma, R.; Corrigall, J.; Joska, J.A.; Swartz, L.; Patel, V. Poverty and common mental disorders in low and middle income countries: A systematic review. Soc. Sci. Med. 2010, 71, 517–528. [Google Scholar] [CrossRef] [PubMed]
- Fleischer, N.E.; Fernald, L.C.H.; Hubbard, A.E. Depressive Symptoms in Low-Income Women in Rural Mexico. Epidemiology 2007, 18, 678–685. [Google Scholar] [CrossRef] [PubMed]
- Burke, H.M.; Fernald, L.C.; Gertler, P.J.; Adler, N.E. Depressive symptoms are associated with blunted cortisol stress responses in very low-income women. Psychosom. Med. 2005, 67, 211–216. [Google Scholar] [CrossRef] [PubMed]
- Wachs, T.D.; Black, M.M.; Engle, P.L. Maternal Depression: A Global Threat to Children’s Health, Development, and Behavior and to Human Rights. Child Dev. Perspect. 2009, 3, 51–59. [Google Scholar] [CrossRef]
- Walker, S.P.; Wachs, T.D.; Grantham-McGregor, S.; Black, M.M.; Nelson, C.A.; Huffman, S.L.; Baker-Henningham, H.; Chang, S.M.; Hamadani, J.D.; Lozoff, B.; et al. Inequality in early childhood: Risk and protective factors for early child development. Lancet 2011, 378, 1325–1338. [Google Scholar] [CrossRef]
- Black, M.M.; Baqui, A.H.; Zaman, K.; McNary, S.W.; Le, K.; Arifeen, S.E.; Hamadani, J.D.; Parveen, M.; Yunus, M.; Black, R.E. Depressive symptoms among rural Bangladeshi mothers: Implications for infant development. J. Child Psychol. Psychiatry 2007, 48, 764–772. [Google Scholar] [CrossRef] [PubMed]
- Galler, J.R.; Harrison, R.H.; Ramsey, F.; Forde, V.; Butler, S.C. Maternal depressive symptoms affect infant cognitive development in Barbados. J. Child Psychol. Psychiatry Allied Discip. 2000, 41, 747–757. [Google Scholar] [CrossRef]
- Parsons, C.E.; Young, K.S.; Rochat, T.J.; Kringelbach, M.L.; Stein, A. Postnatal depression and its effects on child development: A review of evidence from low- and middle-income countries. Br. Med. Bull. 2012, 101, 57–79. [Google Scholar] [CrossRef] [PubMed]
- Patel, V.; Rahman, A.; Jacob, K.S.; Hughes, M. Effect of maternal mental health on infant growth in low income countries: New evidence from South Asia. Br. Med. J. 2004, 328, 820–823. [Google Scholar] [CrossRef] [PubMed]
- Surkan, P.J.; Kennedy, C.E.; Hurley, K.M.; Black, M.M. Maternal depression and early childhood growth in developing countries: Systematic review and meta-analysis. Bull. World Health Org. 2011, 89, 607–615. [Google Scholar] [CrossRef] [PubMed]
- Rahman, A.; Harrington, R.; Bunn, J. Can maternal depression increase infant risk of illness and growth impairment in developing countries? Child Care Health Dev. 2002, 28, 51–56. [Google Scholar] [CrossRef] [PubMed]
- Rahman, A.; Iqbal, Z.; Bunn, J.; Lovel, H.; Harrington, R. Impact of maternal depression on infant nutritional status and illness: A cohort study. Arch. Gen. Psychiatry 2004, 61, 946–952. [Google Scholar] [CrossRef] [PubMed]
- Stewart, R.C.; Bunn, J.; Vokhiwa, M.; Umar, E.; Kauye, F.; Fitzgerald, M. Common mental disorder and associated factors amongst women with young infants in rural Malawi. Soc. Psychiatry Psychiatr. Epidemiol. 2010, 45, 551–559. [Google Scholar] [CrossRef] [PubMed]
- Guo, N.; Bindt, C.; Te Bonle, M.; Appiah-Poku, J.; Hinz, R.; Barthel, D.; Koffi, M.; Posdzich, S.; Deymann, S.; Barkmann, C.; et al. Association of antepartum and postpartum depression in Ghanaian and Ivorian women with febrile illness in their offspring: A prospective birth cohort study. Am. J. Epidemiol. 2013, 178, 1394–1402. [Google Scholar] [CrossRef] [PubMed]
- Goodman, S.H. Genesis and epigenisis of psychopathology in children with depressed mothers: Toward an integrative biopsychosocial perspective. In Neurodevelopmental Mechanisms in the Genesis and Epigenesis of Psychopathology: Future Research Directions; Cicchetti, D., Walker, E., Eds.; Cambridge University Press: New York, NY, USA, 2003; pp. 428–460. [Google Scholar]
- Goodman, S.H.; Rouse, M.H.; Connell, A.M.; Broth, M.R.; Hall, C.M.; Heyward, D. Maternal Depression and Child Psychopathology: A Meta-Analytic Review. Clin. Child Fam. Psychol. Rev. 2011, 14, 1–27. [Google Scholar] [CrossRef] [PubMed]
- National Resarch Council and Institute of Medicine. Depression in Parents, Parenting, and Children: Opportunities to Improve Identification, Treatment, and Prevention; The National Academies Press: Washington, DC, USA, 2009; pp. 1–470. [Google Scholar]
- Gelaye, B.; Rondon, M.B.; Araya, R.; Williams, M.A. Epidemiology of maternal depression, risk factors, and child outcomes in low-income and middle-income countries. Lancet Psychiatry 2016, 3, 973–982. [Google Scholar] [CrossRef]
- Agnafors, S.; Sydsjo, G.; Dekeyser, L.; Svedin, C.G. Symptoms of depression postpartum and 12 years later-associations to child mental health at 12 years of age. Matern. Child Health J. 2013, 17, 405–414. [Google Scholar] [CrossRef] [PubMed]
- Conners-Burrow, N.A.; McKelvey, L.; Perry, D.; Whiteside-Mansell, L.; Kraleti, S.; Mesman, G.; Holmes, K.; Kyzer, A. Low-Level Symptoms of Depression in Mothers of Young Children are Associated with Behavior Problems in Middle Childhood. Matern. Child Health J. 2016, 20, 516–524. [Google Scholar] [CrossRef] [PubMed]
- Giallo, R.; Woolhouse, H.; Gartland, D.; Hiscock, H.; Brown, S. The emotional-behavioural functioning of children exposed to maternal depressive symptoms across pregnancy and early childhood: A prospective Australian pregnancy cohort study. Eur. Child Adolesc. Psychiatry 2015, 24, 1233–1244. [Google Scholar] [CrossRef] [PubMed]
- Cooper, P.J.; Tomlinson, M.; Swartz, L.; Woolgar, M.; Murray, L.; Molteno, C. Post-partum depression and the mother-infant relationship in a South African peri-urban settlement. Br. J. Psychiatry 1999, 175, 554–558. [Google Scholar] [CrossRef] [PubMed]
- Richter, L.M.; Griesel, R.D.; Barbarin, O. Behavioral Problems among Preschool Children in South Africa: A Six-Year Longitudinal Perspective from Birth to Age Five. In International Perspectives on Child and Adolescent Mental Health; Nirbhay, J.P.L., Singh, N., Ashvind, N.S., Eds.; Elsevier: Amsterdam, The Netherlands, 2000; pp. 159–182. [Google Scholar]
- Hadley, C.; Tegegn, A.; Tessema, F.; Asefa, M.; Galea, S. Parental symptoms of common mental disorders and children’s social, motor, and language development in sub-Saharan Africa. Ann. Hum. Biol. 2008, 35, 259–275. [Google Scholar] [CrossRef] [PubMed]
- Falceto, O.G.; Giugliani, E.R.J.; Fernandes, C.L.C. Influence of parental mental health on early termination of breast-feeding: A case-control study. J. Am. Board Fam. Pract. 2004, 17, 173–183. [Google Scholar] [CrossRef] [PubMed]
- Galler, J.R.; Harrison, R.H.; Ramsey, F.; Chawla, S.; Taylor, J. Postpartum feeding attitudes, maternal depression, and breastfeeding in Barbados. Infant Behav. Dev. 2006, 29, 189–203. [Google Scholar] [CrossRef] [PubMed]
- Patel, V.; Rodrigues, M.; DeSouza, N. Gender, poverty, and postnatal depression: A study of mothers in Goa, India. Am. J. Psychiatry 2002, 159, 43–47. [Google Scholar] [CrossRef] [PubMed]
- Engle, P.L. Maternal mental health: Program and policy implications. Am. J. Clin. Nutr. 2009, 89, 963S–966S. [Google Scholar] [CrossRef] [PubMed]
- Huang, L.N.; Freed, R.; Huang, L.N.; Freed, R. The Spiraling Effects of Maternal Depression on Mothers, Children, Families and Communities; Annie, E., Ed.; Issue Brief #2; Casey Foundation: Baltimore, MD, USA, 2006. [Google Scholar]
- Cummings, E.M.; Davies, P.T. Maternal depression and child development. J. Child Psychol. Psychiatry 1994, 35, 73–112. [Google Scholar] [CrossRef] [PubMed]
- Bettes, B.A. Maternal Depression and Motherese—Temporal and Intonational Features. Child Dev. 1988, 59, 1089–1096. [Google Scholar] [CrossRef] [PubMed]
- Livingood, A.B.; Daen, P.; Smith, B.D. The depressed mother as a source of stimulation for her infant. J. Clin. Psychol. 1983, 39, 369–375. [Google Scholar] [CrossRef]
- Field, T.; Healy, B.; Goldstein, S.; Guthertz, M. Behavior-State Matching and Synchrony in Mother Infant Interactions of Nondepressed Versus Depressed Dyads. Dev. Psychol. 1990, 26, 7–14. [Google Scholar] [CrossRef]
- Cooper, P.J.; Tomlinson, M.; Swartz, L.; Landman, M.; Molteno, C.; Stein, A.; McPherson, K.; Murray, L. Improving quality of mother-infant relationship and infant attachment in socioeconomically deprived community in South Africa: Randomised controlled trial. BMJ 2009, 338, b974. [Google Scholar] [CrossRef] [PubMed]
- Ozer, E.J.; Fernald, L.C.; Manley, J.; Gertler, P.J. Effects of a conditional cash transfer program on children’s behavior problems. Pediatrics 2009, 123, e630–e637. [Google Scholar] [CrossRef] [PubMed]
- Ozer, E.J.; Fernald, L.C.H.; Weber, A.; Flynn, E.P.; VanderWeele, T.J. Does alleviating poverty affect mothers’ depressive symptoms? A quasi-experimental investigation of Mexico’s Oportunidades programme. Int. J. Epidemiol. 2011, 40, 1565–1576. [Google Scholar] [CrossRef] [PubMed]
- Fernald, L.C.H.; Gertler, P.J.; Neufeld, L.M. Ten-year impact of Oportunidades—Mexico’s conditional cash transfer program—On child growth, cognition, language and behavior. Lancet 2009, 374, 1997–2005. [Google Scholar] [CrossRef]
- Zill, N. Behavior Problems Index Based on Parent Report; Child Trends: Washington, DC, USA, 1990. [Google Scholar]
- Pachter, L.M.; Auinger, P.; Palmer, R.; Weitzman, M. Do parenting and the home environment, maternal depression, neighborhood, and chronic poverty affect child behavioral problems differently in different racial-ethnic groups? Pediatrics 2006, 117, 1329–1338. [Google Scholar] [CrossRef] [PubMed]
- Lumeng, J.C.; Gannon, K.; Cabral, H.J.; Frank, D.A.; Zuckerman, B. Association between clinically meaningful behavior problems and overweight in children. Pediatrics 2003, 112, 1138–1145. [Google Scholar] [CrossRef] [PubMed]
- Kahn, R.S.; Wilson, K.; Wise, P.H. Intergenerational health disparities: Socioeconomic status, women’s health conditions, and child behavior problems. Public Health Rep. 2005, 120, 399–408. [Google Scholar] [CrossRef] [PubMed]
- Radloff, L.S. The CES-D Scale: A Self-Report Depression Scale for Research in the General Population. Appl. Psychol. Meas. 1977, 1, 385–401. [Google Scholar] [CrossRef]
- Masten, W.G.; Caldwell-Colbert, A.T.; Alcala, S.J.; Mijares, B.E. Reliability and validity of the Center for Epidemiological Studies Depression Scale/Confiabilidad y validez de la Escala de Depresion del Centro de Estudios Epidemiologicos. Hisp. J. Behav. Sci. 1986, 8, 77–84. [Google Scholar] [CrossRef]
- Salgado de Snyder, V.N.; Maldonado, M. Características psicométricas de la Escala de Depresión del Centro de Estudios Epidemiológicos en mujeres mexicanas adultas de áreas rurales [Psychometric characteristics of the Center for Epidemiologic Studies Depression Scale in adult Mexican women from rural areas]. Salud Publica Mex. 1994, 36, 200–209. [Google Scholar] [PubMed]
- Golding, J.M.; Aneshensel, C.S. Factor structure of the Center for Epidemiologic Studies Depression Scale among Mexican Americans and non-Hispanic Whites. Psychol. Assess. 1989, 1, 163–168. [Google Scholar] [CrossRef]
- Garcia, M.; Marks, G. Depressive Symptomatology among Mexican-American Adults—An Examination with the Ces-D Scale. Psychiatry Res. 1989, 27, 137–148. [Google Scholar] [CrossRef]
- Falkingham, J.; Namazie, C. Measuring Health and Poverty: A Review of Approaches to Identifying the Poor; DFID Health Systems Resource Centre: London, UK, 2002. [Google Scholar]
- Aiken, L.S.; West, S.G.; Reno, R.R. Multiple Regression: Testing and Interpreting Interactions; Sage: Newcastle upon Tyne, UK, 1991. [Google Scholar]
- Statacorp. Stata Statistical Software: Release 14; Statacorp LP: College Station, TX, USA, 2015. [Google Scholar]
- Hall, G.; Patrinos, H.A. Indigenous Peoples, Poverty, and Human Development in Latin America; Palgrave Macmillan: New York, NY, USA, 2006; 308p. [Google Scholar]
- Lovejoy, M.C.; Graczyk, P.A.; O’Hare, E.; Neuman, G. Maternal depression and parenting behavior: A meta-analytic review. Clin. Psychol. Rev. 2000, 20, 561–592. [Google Scholar] [CrossRef]
- Woolhouse, H.; Gartland, D.; Mensah, F.; Giallo, R.; Brown, S. Maternal depression from pregnancy to 4 years postpartum and emotional/behavioural difficulties in children: Results from a prospective pregnancy cohort study. Arch. Womens Ment. Health 2016, 19, 141–151. [Google Scholar] [CrossRef] [PubMed]
- Beil, H.; Beeber, L.S.; Schwartz, T.A.; Lewis, G. Cost-effectiveness of alternative treatments for depression in low-income women. J. Ment. Health Policy Econ. 2013, 16, 55–65. [Google Scholar] [PubMed]
- Ho, R.C.; Mak, K.K.; Chua, A.N.; Ho, C.S.; Mak, A. The effect of severity of depressive disorder on economic burden in a university hospital in Singapore. Expert Rev. Pharmacoecon. Outcomes Res. 2013, 13, 549–559. [Google Scholar] [CrossRef] [PubMed]
- Gracey, M.; King, M. Indigenous health part 1: Determinants and disease patterns. Lancet 2009, 374, 65–75. [Google Scholar] [CrossRef]
- King, M.; Smith, A.; Gracey, M. Indigenous health part 2: The underlying causes of the health gap. Lancet 2009, 374, 76–85. [Google Scholar] [CrossRef]
- Conners-Burrow, N.A.; Bokony, P.; Whiteside-Mansell, L.; Jarrett, D.; Kraleti, S.; McKelvey, L.; Kyzer, A. Low-level depressive symptoms reduce maternal support for child cognitive development. J. Pediatr. Health Care 2014, 28, 404–412. [Google Scholar] [CrossRef] [PubMed]
- Stubbs, B.; Vancampfort, D.; Veronese, N.; Thompson, T.; Fornaro, M.; Schofield, P.; Solmi, M.; Mugisha, J.; Carvalho, A.F.; Koyanagi, A. Depression and pain: Primary data and meta-analysis among 237,952 people across 47 low- and middle-income countries. Psychol. Med. 2017, 47, 2906–2917. [Google Scholar] [CrossRef] [PubMed]
- Aihara, Y.; Shrestha, S.; Sharma, J. Household water insecurity, depression and quality of life among postnatal women living in urban Nepal. J. Water Health 2016, 14, 317–324. [Google Scholar] [CrossRef] [PubMed]
- Atkinson, L.; Paglia, A.; Coolbear, J.; Niccols, A.; Parker, K.C.; Guger, S. Attachment security: A meta-analysis of maternal mental health correlates. Clin. Psychol. Rev. 2000, 20, 1019–1040. [Google Scholar] [CrossRef]
- Tomlinson, M.; Cooper, P.; Murray, L. The mother-infant relationship and infant attachment in a South African peri-urban settlement. Child Dev. 2005, 76, 1044–1054. [Google Scholar] [CrossRef] [PubMed]
- Kim, S.; Thibodeau, R.; Jorgensen, R.S. Shame, guilt, and depressive symptoms: A meta-analytic review. Psychol. Bull. 2011, 137, 68–96. [Google Scholar] [CrossRef] [PubMed]
- Dunford, E.; Granger, C. Maternal Guilt and Shame: Relationship to Postnatal Depression and Attitudes towards Help-Seeking. J. Child Fam. Stud. 2017, 26, 1692–1701. [Google Scholar] [CrossRef]
- Mills, R.S.; Hastings, P.D.; Serbin, L.A.; Stack, D.M.; Abela, J.R.; Arbeau, K.A.; Lall, D.I. Depressogenic thinking and shame proneness in the development of internalizing problems. Child Psychiatry Hum. Dev. 2015, 46, 194–208. [Google Scholar] [CrossRef] [PubMed]
- DeJong, H.; Fox, E.; Stein, A. Rumination and postnatal depression: A systematic review and a cognitive model. Behav. Res. Ther. 2016, 82 (Suppl. C), 38–49. [Google Scholar] [CrossRef] [PubMed]
- Psychogiou, L.; Moberly, N.J.; Parry, E.; Russell, A.E.; Nath, S.; Kallitsoglou, A.; Psychogiou, L. Does fathers’ and mothers’ rumination predict emotional symptoms in their children? Br. J. Clin. Psychol. 2017, 56, 431–442. [Google Scholar] [CrossRef] [PubMed]
- Apter-Levy, Y.; Feldman, M.; Vakart, A.; Ebstein, R.P.; Feldman, R. Impact of maternal depression across the first 6 years of life on the child’s mental health, social engagement, and empathy: The moderating role of oxytocin. Am. J. Psychiatry 2013, 170, 1161–1168. [Google Scholar] [CrossRef] [PubMed]
- Goodman, S.H.; Gotlib, I.H. Risk for psychopathology in the children of depressed mothers: A developmental model for understanding mechanisms of transmission. Psychol. Rev. 1999, 106, 458–490. [Google Scholar] [CrossRef] [PubMed]
- LeMoult, J.; Chen, M.C.; Foland-Ross, L.C.; Burley, H.W.; Gotlib, I.H. Concordance of mother-daughter diurnal cortisol production: Understanding the intergenerational transmission of risk for depression. Biol. Psychol. 2015, 108, 98–104. [Google Scholar] [CrossRef] [PubMed]
- Gotlib, I.H.; LeMoult, J.; Colich, N.L.; Foland-Ross, L.C.; Hallmayer, J.; Joormann, J.; Lin, J.; Wolkowitz, O.M. Telomere length and cortisol reactivity in children of depressed mothers. Mol. Psychiatry 2015, 20, 615–620. [Google Scholar] [CrossRef] [PubMed]
- Liu, Y.; Ho, R.C.-M.; Mak, A. InterleUKin (IL)-6, tumour necrosis factor alpha (TNF-α) and soluble interleUKin-2 receptors (sIL-2R) are elevated in patients with major depressive disorder: A meta-analysis and meta-regression. J. Affect. Disord. 2012, 139, 230–239. [Google Scholar] [CrossRef] [PubMed]
- Karlsson, L.; Nousiainen, N.; Scheinin, N.M.; Maksimow, M.; Salmi, M.; Lehto, S.M.; Tolvanen, M.; Lukkarinen, H.; Karlsson, H. Cytokine profile and maternal depression and anxiety symptoms in mid-pregnancy—The FinnBrain Birth Cohort Study. Arch. Womens Ment. Health 2017, 20, 39–48. [Google Scholar] [CrossRef] [PubMed]
- Lund, C.; De Silva, M.; Plagerson, S.; Cooper, S.; Chisholm, D.; Das, J.; Knapp, M.; Patel, V. Global Mental Health 1 Poverty and mental disorders: Breaking the cycle in low-income and middle-income countries. Lancet 2011, 378, 1502–1514. [Google Scholar] [CrossRef]
- Patel, V.; Araya, R.; Chatterjee, S.; Chisholm, D.; Cohen, A.; De Silva, M.; Hosman, C.; McGuire, H.; Rojas, G.; van Ommeren, M. Treatment and prevention of mental disorders in low-income and middle-income countries. Lancet 2007, 370, 991–1005. [Google Scholar] [CrossRef]
- Vally, Z.; Maggott, C. Evaluating the Outcome of Cultural Adaptations of Cognitive-Behavioural Therapy for Adult Depression: A Meta-Analysis of Treatment Studies in Developing Countries. Int. J. Adv. Couns. 2015, 37, 293–304. [Google Scholar] [CrossRef]
- Barrera, A.Z.; Wickham, R.E.; Munoz, R.F. Online prevention of postpartum depression for Spanish- and English-speaking pregnant women: A pilot randomized controlled trial. Internet Interv. 2015, 2, 257–265. [Google Scholar] [CrossRef] [PubMed]
- Zhang, M.W.; Tsang, T.; Cheow, E.; Ho, C.S.; Yeong, N.B.; Ho, R.C. Enabling psychiatrists to be mobile phone app developers: Insights into app development methodologies. JMIR mHealth uHealth 2014, 2. [Google Scholar] [CrossRef] [PubMed]
- Rahman, A.; Fisher, J.; Bower, P.; Luchters, S.; Tran, T.; Yasamy, M.T.; Saxena, S.; Waheed, W. Interventions for common perinatal mental disorders in women in low- and middle-income countries: A systematic review and meta-analysis. Bull. World Health Org. 2013, 91, 593–601I. [Google Scholar] [CrossRef] [PubMed]
- Lara, M.A. Erinatal Depression in Mexican Women: Prevalence, Risk Factors, and Prevention of Postpartum Depression. In Perinatal Depression among Spanish-Speaking and Latin American Women: A Global Perspective on Detection and Treatment; Lara-Cinisomo, S., Wisner, K.L., Eds.; Springer: New York, NY, USA, 2014; pp. 97–110. [Google Scholar]
| Variable | Mean (SD) or % | |
|---|---|---|
| Maternal characteristics | ||
| Age (years) | 31.08 (7.65) | |
| Relationship Status | ||
| Married or in a relationship | 93.31% | |
| Single, separated, widowed, or divorced | 6.69% | |
| Education (highest level attended) | ||
| No school or kindergarten only | 14.57% | |
| Some primary school | 68.14% | |
| Some secondary school | 14.66% | |
| Some post-secondary school | 2.63% | |
| CES-D score a (0–60 point scale) | 16.17 (9.44) | |
| Child characteristics | ||
| Gender | ||
| Female | 49.32% | |
| Male | 50.68% | |
| Age (months) | 48.73 (13.54) | |
| 24–36 months | 23.39% | |
| 37–48 months | 26.68% | |
| 49–60 months | 25.35% | |
| 61–72 months | 24.59% | |
| Behavior problems index | ||
| Total score (0–19 point scale) | 8.22 (4.20) | |
| Internalizing score (0–10 point scale) | 4.20 (2.49) | |
| Externalizing score (0–9 point scale) | 4.02 (2.34) | |
| Household characteristics | ||
| State of Mexico | ||
| Guerrero | 15.04% | |
| Hidalgo | 13.87% | |
| Michoacán | 9.46% | |
| Puebla | 16.50% | |
| Querétaro | 4.21% | |
| San Luis Potosí | 14.25% | |
| Veracruz | 26.68% | |
| Indigenous ethnicity (based on language spoken) | 40.21% | |
| Household size (number of people) | 6.09 (2.28) | |
| Rooms in house (excluding kitchen, bathroom, passageways) | 1.81 (0.99) | |
| Crowding (number of people per room in house) | 4.13 (2.24) | |
| Household features | ||
| Land has running water | 55.40% | |
| House has electricity | 89.64% | |
| House has dirt floor | 47.50% | |
| Owns draft animals (horses, mules, burros) | 25.01% | |
| Owns grazing animals (pigs, goats, sheep) | 37.66% | |
| Owns small animals (hens, chickens, turkeys) | 57.50% | |
| Household assets | ||
| TV | 65.56% | |
| Radio | 59.48% | |
| Gas stove | 37.75% | |
| Refrigerator | 27.49% | |
| Washing machine | 9.30% | |
| Other home appliances | 54.80% | |
| Car | 12.40% | |
| Boiler | 3.65% | |
| Child Behavior Outcome | β (95% CI) | Significant Covariates at p < 0.05, Variable (Direction of Effect) | ||
|---|---|---|---|---|
| Total child behavior score | ||||
| Total CES-D score | 0.114 *** (0.101, 0.127) | Child age (+), female (−), maternal age (−), asset index quintiles 3, 4, 5 (−) | ||
| CES-D subscale scores | ||||
| Somatic | 0.298 *** (0.252, 0.344) | Child age (+), female (−), maternal age (−), asset index quintiles 4, 5 (−) | ||
| Negative affect | 0.242 *** (0.206, 0.279) | Child age (+), female (−), maternal age (−), asset index quintiles 3, 4, 5 (−) | ||
| Positive affect | 0.129 *** (0.087, 0.171) | Child age (+), female (−), maternal age (−), asset index quintiles 4, 5 (−) | ||
| Interpersonal | 0.370 *** (0.313, 0.427) | Child age (+), female (−), maternal age (−), asset index quintile 5 (−) | ||
| Internalizing child behavior score | ||||
| Total CES-D score | 0.069 *** (0.061, 0.076) | Child age (+), maternal age (−), asset index quintiles 3, 4, 5 (−) | ||
| CES-D subscale | ||||
| Somatic | 0.176 *** (0.149, 0.202) | Child age (+), maternal advanced school (−), asset index quintiles 4, 5 (−) | ||
| Negative affect | 0.159 *** (0.138, 0.180) | Maternal age (−), maternal advanced school (−), asset index quintiles 3, 4, 5 (−) | ||
| Positive affect | 0.072 *** (0.047, 0.096) | Maternal secondary school (−), asset index quintiles 4, 5 (−) | ||
| Interpersonal | 0.228 *** (0.194, 0.262) | Asset index quintiles 4, 5 (−) | ||
| Externalizing child behavior score | ||||
| Total CES-D score | 0.045 *** (0.038, 0.052) | Child age (+), female (−), maternal age (−) | ||
| CES-D subscale scores | ||||
| Somatic | 0.122 *** (0.097, 0.147) | Child age (+), female (−), maternal age (−) | ||
| Negative affect | 0.084 *** (0.063, 0.104) | Child age (+), female (−), maternal age (−) | ||
| Positive affect | 0.057 *** (0.035, 0.080) | Child age (+), female (−), maternal age (−) | ||
| Interpersonal | 0.142 *** (0.110, 0.175) | Child age (+), female (−), maternal age (−) | ||
© 2017 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Flynn, E.P.; Chung, E.O.; Ozer, E.J.; Fernald, L.C.H. Maternal Depressive Symptoms and Child Behavior among Mexican Women and Their Children. Int. J. Environ. Res. Public Health 2017, 14, 1566. https://doi.org/10.3390/ijerph14121566
Flynn EP, Chung EO, Ozer EJ, Fernald LCH. Maternal Depressive Symptoms and Child Behavior among Mexican Women and Their Children. International Journal of Environmental Research and Public Health. 2017; 14(12):1566. https://doi.org/10.3390/ijerph14121566
Chicago/Turabian StyleFlynn, Emily P., Esther O. Chung, Emily J. Ozer, and Lia C. H. Fernald. 2017. "Maternal Depressive Symptoms and Child Behavior among Mexican Women and Their Children" International Journal of Environmental Research and Public Health 14, no. 12: 1566. https://doi.org/10.3390/ijerph14121566
APA StyleFlynn, E. P., Chung, E. O., Ozer, E. J., & Fernald, L. C. H. (2017). Maternal Depressive Symptoms and Child Behavior among Mexican Women and Their Children. International Journal of Environmental Research and Public Health, 14(12), 1566. https://doi.org/10.3390/ijerph14121566






