Cost-Effectiveness of a New Nordic Diet as a Strategy for Health Promotion
Abstract
:1. Introduction
- -
- Gastronomic potential and Nordic identity—dishes based on high-quality organic food products with a Nordic origin and cultural heritage. Tastes from arctic seafood, and colour and flavor variation from plant foods, such as berries, cabbages, roots, legumes, potatoes and herbs should contribute to creating a Nordic identity.
- -
- Health—relatively low meat intake and high intake of legumes, vegetables, fruit, whole grains, seafood, potatoes, nuts, herbs, etc., compared with the average diet in many Western countries, including Denmark. This dietary composition should contribute to the prevention of health disorders such as weight gain, type 2 diabetes, cardiovascular diseases and cancer, but should also help maintaining and improving general physical, mental and social well-being via.
- -
- Sustainability—use of locally grown foods to minimize transport of food stuffs, use of organic products (which are perceived by many as more sustainable than non-organic products due to more “natural” production methods involving organic soil management, abandonment of pesticides and artificial fertilizers, higher animal welfare, etc.) and foods sourced from the wild countryside, shift from meat to plant products and focus on minimizing food waste (by developing a few hundred recipes incorporating reuse) should contribute to reducing environmental impacts associated with food production.
2. Data and Methods
2.1. Data
2.2. Models
- -
- Unchanged total energy intake (coefficient represents energy content in commodity )
- -
- maximum limits to intake of some foods or nutrients (coefficient characterizes commodity with respect to constraint ) , and
- -
- minimum limits to intake of some other foods or nutrients (coefficient characterizes commodity with respect to constraint )
3. Results
| Consumed Quantities (1000 tonnes) | Expenditure, mill. € | |||
|---|---|---|---|---|
| ADD | NND | ADD | NND | |
| Grain-based foods | 1005 | 1317 | 1789 | 1857 |
| Meat | 293 | 179 | 2722 | 1670 |
| Seafood | 65 | 81 | 603 | 745 |
| Dairy and fats | 960 | 771 | 1898 | 1646 |
| Fruits and vegetables | 847 | 1432 | 2321 | 5185 |
| Other foods | 357 | 305 | 1614 | 1718 |
| Foods total | 10,948 | 12,821 | ||
| Beverages | 1204 | 1304 | 2644 | 2898 |
| Total | 13,591 | 15,719 | ||
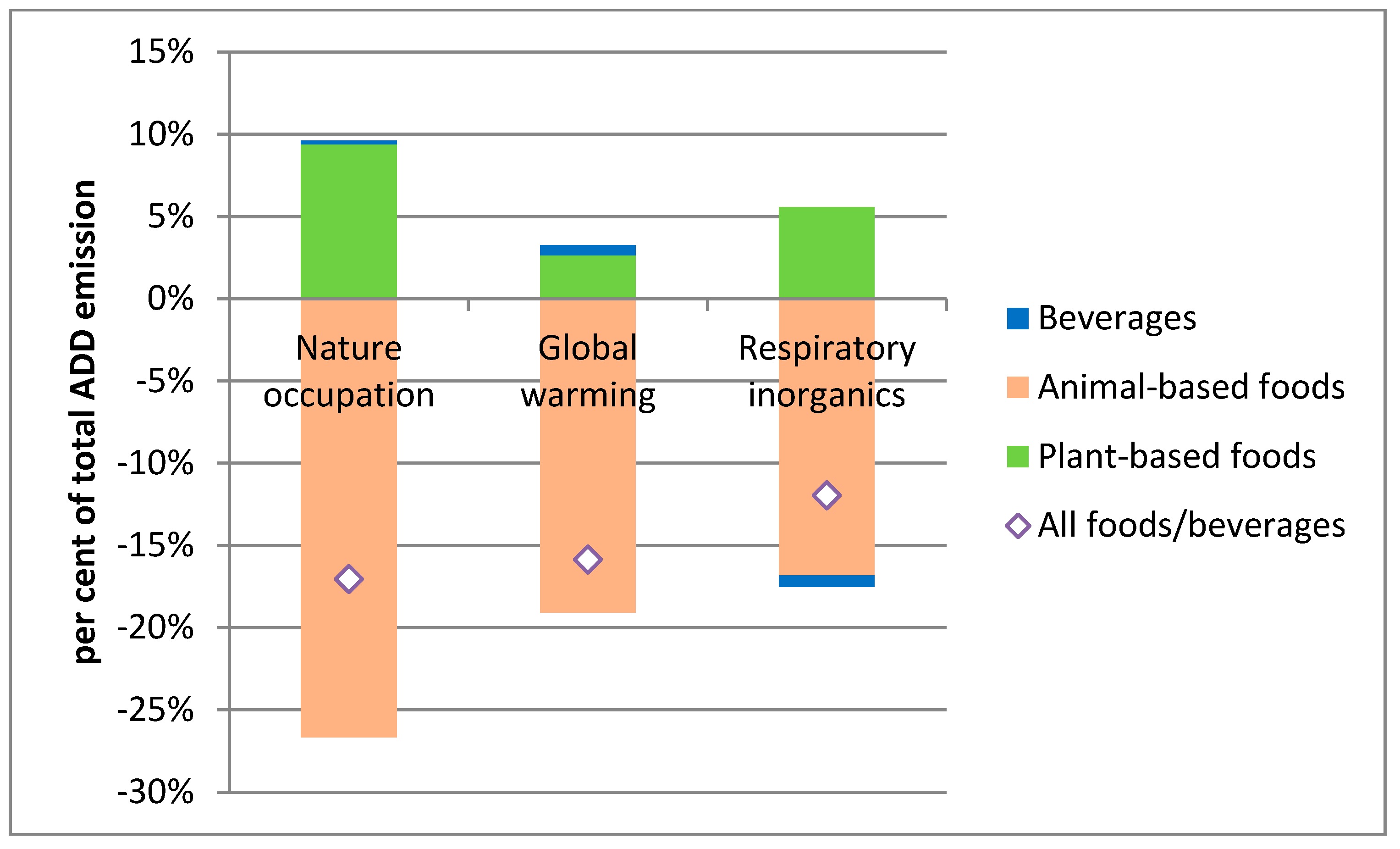
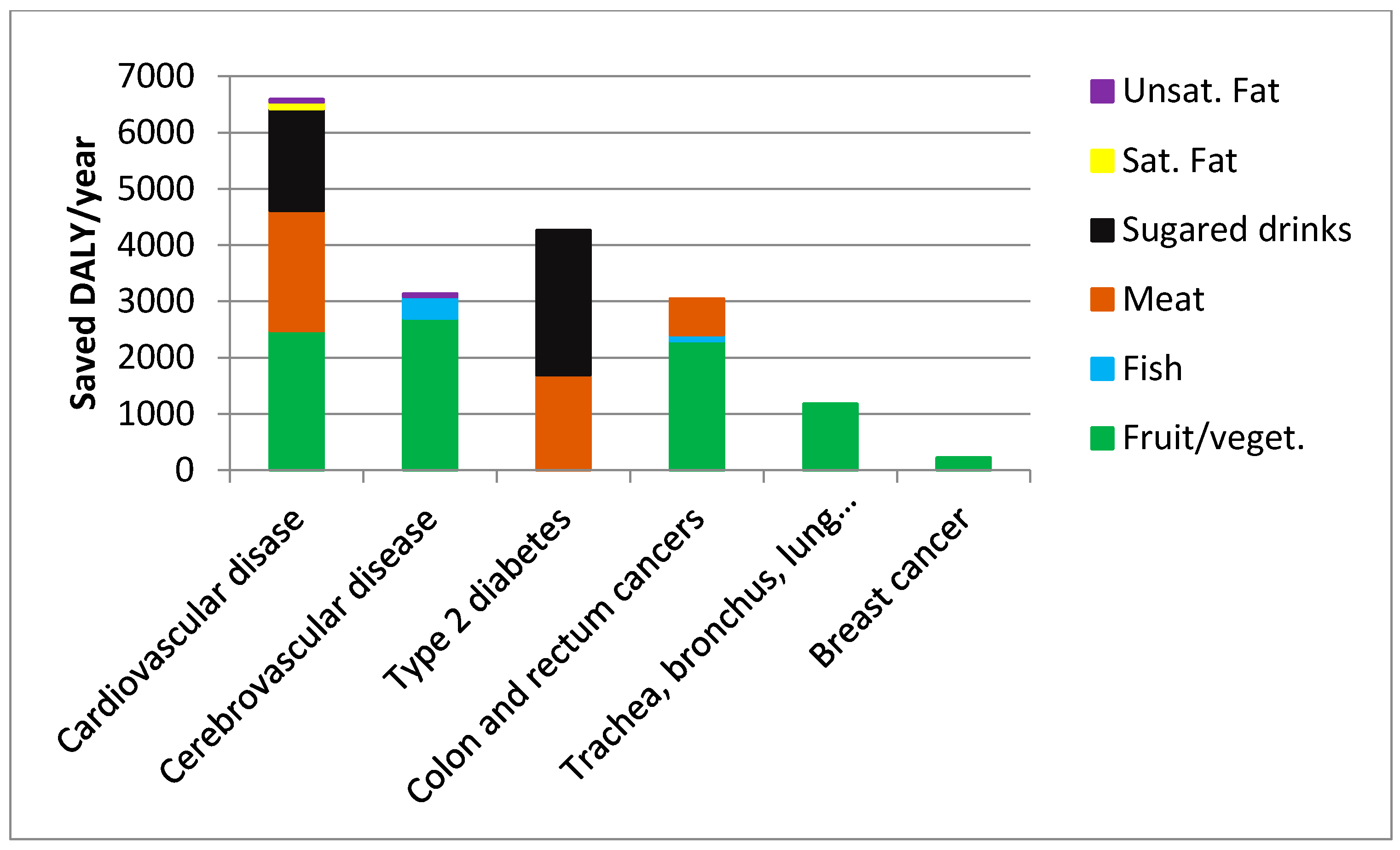
| ADD | NND | Environmental Benefit | Net Cost/DALY | Food and Beverage Expenditure | Disease Reduction (DALY) | |
|---|---|---|---|---|---|---|
| €/adult_Equivalent/year | €/Adult Equivalent | €1.000 | per cent Difference | per cent Reduction | ||
| I | 2323 | 2699 | 110–179 | 89–121 | 16.2 | 10.1 |
| II | 2383 | 2794 | 110–179 | 69–89 | 17.2 | 15.0 |
| III | 2482 | 2860 | 110–179 | 62–84 | 15.2 | 14.1 |
| IV | 2715 | 3143 | 110–179 | 70–90 | 15.7 | 14.4 |
| V | 2813 | 3240 | 110–179 | 78–99 | 15.2 | 13.4 |
| All income classes | 2667 | 3084 | 110–179 | 73–94 | 15.7 | 13.8 |
4. Discussion
5. Conclusions
Supplementary Materials
| Dietary Component | Average Content in the NND (g/day) | Average Content in the Danish Population’s Diet 2010 (g/day) |
|---|---|---|
| Ingredients, g/10 MJ | ||
| Fruit | >300 (250–350) | 240 |
| Vegetables | >400 (350–450) | 181 |
| Including | ||
| - berries | (50–100) | 5 |
| - cabbages | >29 (25–35) | 9 |
| - root vegetables | >150 | 38 |
| - legumes | >30 | 7 |
| Fresh herbs | As much as possible (≥1) | |
| Potatoes | >140 (140–160) | 106 |
| Plants and mushrooms from the wild countryside | 5 (3–7) | <1 |
| Whole grains | >75 | 36 |
| Nuts | >30 | 1 |
| Fish and shellfish | >43 (40–50) | 22 |
| Seaweed | 5 (3–7) | <1 |
| Free-range livestock | 85–100 (90–110) | 143 |
| Including | ||
| - game | >4 (2–6) | <1 |
| Macronutrients etc. | ||
| Protein (E%) | 18 (15–23) | 15 |
| Total carbohydrate (incl. fibres), E% | 52 (48–56) | 50 |
| Added sugar (E%) | <10 | |
| Total fat (E%) | 30 (25–35) | 35 |
| Saturated fat (E%) | <10 | 15 |
| Nordic produce (%) | ≥95 | |
| Organic (%) | ≥75 |
| Unit | COI/COD Approach, Based on Adjusted US GDP/Capita | COI/COD Approach, Based on Unadjusted US GDP/Capita | |
|---|---|---|---|
| Human toxicity, carcinogens | €/kg C2H3Cl-eq | 0.2823 | 0.2854 |
| Human toxicity, non-carcinogens | €/kg C2H3Cl-eq | 0.2826 | 0.2854 |
| Respiratory inorganics | €/kg PM2.5-eq | 70.4198 | 45.4682 |
| Ozone layer depletion | €/kg CFC-11-eq | 106.0406 | 70.2595 |
| Ecotoxicity, aquatic | €/kg TEG-eq w | 0.0000 | 0.0000 |
| Ecotoxicity, terrestrial | €/kg TEG-eq w | 0.0012 | 0.0006 |
| Nature occupation | €/m2 agr.land | 0.1293 | 0.0690 |
| Global warming | €/kg CO2-eq | 0.0865 | 0.0459 |
| Acidification | €/m2 UES | 0.0081 | 0.0043 |
| Eutrophication, aquatic | €/kg NO3-eq | 0.1056 | 0.0564 |
| Eutrophication, terrestrial | €/m2 UES | 0.0130 | 0.0070 |
| Respiratory organics | €/pers × ppm × h | 0.2662 | 0.1705 |
| Photochemical ozone vegetation | €/m2 × ppm × hours | 0.0004 | 0.0003 |
| Cardio-Vascular Disease | Stroke | Diabetes | Stomach Cancer | Lung Cancer | Breast Cancer | |
|---|---|---|---|---|---|---|
| Fruits and vegetables exposure, 200 g/day | 1 | 1 | 1 | 1 | 1 | 1 |
| 300 g/day | 0.97 | 0.95 | 1 | 0.77 | 0.89 | 0.95 |
| 400 g/day | 0.93 | 0.89 | 1 | 0.77 | 0.89 | 0.95 |
| 500 g/day | 0.88 | 0.82 | 1 | 0.77 | 0.89 | 0.95 |
| 600 g/day | 0.83 | 0.74 | 1 | 0.77 | 0.89 | 0.95 |
| Fish, exposure, 10 g/day | 1 | 0.93 | 1 | 0.87 | 1 | 1 |
| 20 g/day | 1 | 0.78 | 1 | 0.89 | 1 | 1 |
| 50 g/day | 1 | 0.73 | 1 | 0.83 | 1 | 1 |
| 150 g/day | 1 | 0.48 | 1 | 0.84 | 1 | 1 |
| Red meat exposure +100 g/day | 1.00 | 1 | 1.18 | 1.08 | 1 | 1 |
| Processed meat exposure +50 g/day | 1.42 | 1 | 1.3 | 1.01 | 1 | 1 |
| Sugared drinks exposure, 10 g/day | 1 | 1 | 1 | 1 | 1 | 1 |
| 25 g/day | 1 | 1 | 1.06 | 1 | 1 | 1 |
| 160 g/day | 1.04 | 1 | 1.5 | 1 | 1 | 1 |
| 250 g/day | 1.23 | 1 | 1.85 | 1 | 1 | 1 |
| Whole grain exposure +10 g/day | 0.90 | 1 | 0.79 | 1 | 1 | 1 |
| Total fat exposure, +5 E% | 1.00 | 1 | 1 | 1 | 1 | 1 |
| Saturated fat exposure, +5 E% | 1.05 | 1 | 1 | 1 | 1 | 1 |
| Monounsaturated fat exposure, +5 E% | 0.96 | 0.91 | 1 | 1 | 1 | 1 |
| Polyunsaturated fat exposure +5 E% | 0.92 | 0.91 | 1 | 1 | 1 | 1 |
Acknowledgments
Author Contributions
Conflicts of Interest
List of Abbreviations
| OPUS | Acronym for the project “Optimal well-being, development and health for Danish children through a healthy New Nordic Diet” |
| NND | New Nordic Diet |
| ADD | New Nordic Diet |
References
- Lim, S.S.; Vos, T.; Flaxman, A.D.; Danaei, G.; Shibuya, K.; Adair-Rohani, A.; AlMazroa, M.A.; Amann, M.; Anderson, H.R.; Andrews, K.G.; et al. A comparative risk assessment of burden of disease and injury attributable to 67 risk factors and risk factor clusters in 21 regions, 1990–2010: A systematic analysis for the Global Burden of Disease Study 2010. Lancet 2012, 380, 2224–2260. [Google Scholar] [CrossRef]
- Trichopoulou, A.; Costacou, T.; Bamia, C.; Trichopoulos, D. Adherence to a Mediterranean diet and survival in a Greek population. N. Engl. J. Med. 2003, 348, 2599–2608. [Google Scholar] [CrossRef] [PubMed]
- Bocuse d’Or. The Bocuse d’Or Winners’ Academy 2012. Available online: http://www.bocusedor-europe.com/the-winners-of-the-2-aa2-bocuse-d-or-europe (accessed on 9 January 2013).
- Mithril, C.; Dragsted, L.O.; Meyer, C.; Tetens, I.; Biltoft-Jensen, A.; Astrup, A. Dietary composition and nutrient content of the New Nordic Diet. Publ. Health Nutr. 2012. [Google Scholar] [CrossRef] [PubMed]
- Drewnowski, A.; Darmon, N. The economics of obesity: Dietary energy density and energy cost. Am. J. Clin. Nutr. 2005, 82, 2655–2735. [Google Scholar]
- Drewnowski, A.; Darmon, N. Food choices and diet costs: An economic analysis. J. Nutr. 2005, 135, 900–904. [Google Scholar] [PubMed]
- Darmon, N.; Drewnowski, A. Does social class predict diet quality? Am. J. Clin. Nutr. 2008, 87, 1107–1117. [Google Scholar] [PubMed]
- Schröder, H.; Marrugat, J.; Covas, M.I. High monetary costs of dietary patterns associated with lower body mass index: A population-based study. Int. J. Obes. 2006, 30, 1574–1579. [Google Scholar] [CrossRef] [PubMed]
- Rydén, P.J.; Hagfors, L. Diet cost, diet quality and socio-economic position: How are they related and what contributes to differences in diet costs? Publ. Health Nutr. 2011. [Google Scholar] [CrossRef] [PubMed]
- Drewnowski, A.; Eichelsdoerfer, P. The Mediterranean diet: Does it have to cost more? Publ. Health Nutr. 2009, 12, 1621–1628. [Google Scholar] [CrossRef] [PubMed]
- Statistics Denmark, Statistikbanken. Available online: http://www.statistikbanken.dk (accessed on 10 May 2014).
- EcoInvent. 2014. Available online: http://www.ecoinvent.org/database/ (accessed on 7 February 2014).
- LCA Food Database. 2004. Available online: http://www.lcafood.dk (accessed on 7 February 2014).
- Saxe, H. The New Nordic Diet is an effective tool in environmental protection: It reduces the associated socio-economic cost of diets. Am. J. Clin. Nutr. 2014, 99, 1117–1125. [Google Scholar] [CrossRef] [PubMed]
- Eshet, T.; Ayalon, O.; Shecther, M. Valuation of externalities of selected waste management alternatives: A comparative review and analysis. Resour. Conserv. Recycl. 2006, 46, 335–364. [Google Scholar] [CrossRef]
- Dubgaard, A.; Laugesen, F.M.; Ståhl, E.L.; Bang, J.R.; Schou, E.; Jacobsen, B.H.; Ørum, J.E.; Jensen, J.D. Analyse af Omkostningseffektiviteten ved Drivhusgasreducerende Tiltag i Relation til Landbruget (Analysis of Cost Effectiveness of Greenhouse Gas Reducing Interventions in Agriculture); IFRO Report No. 221; University of Copenhagen: Copenhagen, Denmark, 2013. [Google Scholar]
- Weidema, B.P.; Wesnæs, M.; Hermansen, J.; Kristensen, T.; Halberg, N. Environmental Improvement Potentials of Meat and Dairy Products. JRC Scientific and Technical Report. EUR 23491 EN. 2008. Available online: ftp://ftp.jrc.es/pub/library/Impro_Meet.pdf (accessed on 12 April 2012).
- Weidema, B.P. Using the budget constraint to monetarise impact assessment results. Ecol. Econ. 2009, 68. [Google Scholar] [CrossRef]
- Morgenstern, H.; Bursic, E.S. A method for using epidemiologic data to estimate the potential impact of an intervention on the health status of a target population. J. Comm. Health 1982, 7, 292–309. [Google Scholar] [CrossRef]
- He, F.J.; Nowson, C.A.; MacGregor, G.A. Fruit and vegetable consumption and stroke: Meta-analysis of cohort studies. Lancet 2006, 367, 320–326. [Google Scholar] [CrossRef]
- He, F.J.; Nowson, C.A.; Lucas, M.; MacGregor, G.A. Increased consumption of fruit and vegetables is related to a reduced risk of coronary heart disease: Meta-analysis of cohort studies. J. Hum. Hypertens. 2007, 21, 717–728. [Google Scholar] [CrossRef] [PubMed]
- Joshipura, K.J.; Ascherio, A.; Manson, J.E.; Stampfer, M.J.; Rimm, E.B.; Speizer, F.E.; Hennekens, C.H.; Spiegelman, D.; Willett, W.C. Fruit and vegetable intake in relation to risk of ischemic stroke. JAMA 1999, 282, 1233–1239. [Google Scholar] [CrossRef] [PubMed]
- Gillman, M.W.; Cupples, L.A.; Gagnon, D.; Posner, B.M.; Ellison, R.C.; Castelli, W.P.; Wolf, P.A. Protective effect of fruits and vegetables on development of stroke in men. JAMA 1995, 273, 1113–1117. [Google Scholar] [CrossRef] [PubMed]
- World Cancer Research Fund/American Institute for Cancer Research (WCRF/AICR). Food, Nutrition, Physical Activity, and the Prevention of Cancer: A Global Perspective; AICR: Washington, DC, USA, 2007. [Google Scholar]
- Brennan, P.; Hsu, C.C.; Moullan, N.; Szeszenia-Dabrowska, N.; Lissowska, J.; Zaridze, D.; Rudnai, P.; Fabianova, E.; Mates, D.; Bencko, V.; et al. Effect of cruciferous vegetables on lung cancer in patients stratified by genetic status: A mendelian randomization approach. Lancet 2005, 366, 1558–1560. [Google Scholar] [CrossRef]
- Smith-Warner, S.A.; Spiegelman, D.; Yaun, S.S.; Adami, H.-O.; Beeson, W.L.; van den Brandt, P.A.; Folsom, R.A.; Fraser, G.E.; Freudenheim, J.L.; Goldbohm, R.A.; et al. Intake of fruits and vegetables and risk of breast cancer—A pooled analysis of cohort studies. JAMA 2001, 285, 769–776. [Google Scholar] [CrossRef] [PubMed]
- Van Gils, C.H.; Peeters, P.H.M.; Bueno-de-Mesquita, H.B.; Boshuizen, H.C.; Lahmann, P.H.; Clavel-Chapelon, F.; Thiébaut, A.; Kesse, E.; Sieri, S.; Palli, D.; et al. Consumption of vegetables and fruits and risk of breast cancer. JAMA 2005, 293, 183–193. [Google Scholar] [CrossRef] [PubMed]
- Mozaffarian, D.; Kumanyika, S.K.; Lemaitre, R.N.; Olson, J.L.; Burke, G.L.; Siscovick, D.S. Cereal, fruit, and vegetable fiber intake and the risk of cardiovascular disease in elderly individuals. JAMA 2003, 289, 1659–1666. [Google Scholar] [CrossRef] [PubMed]
- Pereira, M.A.; O’Reilly, E.; Augustsson, K.; Fraser, G.E.; Goldbourt, U.; Heitmann, B.L.; Hallmans, G.; Knekt, P.; Liu, S.; Pietinen, P.; et al. Dietary fiber and risk of coronary heart disease—A pooled analysis of cohort studies. Arch. Intern. Med. 2004, 164, 370–376. [Google Scholar] [CrossRef] [PubMed]
- Rimm, E.B.; Ascherio, A.; Giovannucci, E.; Spiegelman, D.; Stampfer, M.J.; Willett, W.C. Vegetable, fruit, and cereal fiber intake and risk of coronary heart disease among men. JAMA 1996, 275, 447–451. [Google Scholar] [CrossRef] [PubMed]
- Wolk, A.; Manson, J.E.; Stampfer, M.J.; Colditz, G.A.; Hu, F.B.; Speizer, F.E.; Hennekens, C.H.; Willett, W.C. Long-term intake of dietary fiber and decreased risk of coronary heart disease among women. JAMA 1999, 281, 1998–2004. [Google Scholar] [CrossRef] [PubMed]
- Liu, S.; Buring, J.E.; Sesso, H.D.; Rimm, E.B.; Willett, W.C.; Manson, J.E. A prospective study of dietary fiber intake and risk of cardiovascular disease among women. J. Am. Coll. Cardiol. 2002, 39, 49–56. [Google Scholar] [CrossRef]
- Casiglia, E.; Tikhonoff, V.; Caffi, S.; Boschetti, G.; Grasselli, C.; Saugo, M.; Giordano, N.; Rapisarda, V.; Spinella, P.; Palatini, P. High dietary fiber intake prevents stroke at a population level. Clin. Nutr. 2013, 32, 811–818. [Google Scholar] [CrossRef] [PubMed]
- Bingham, S.A.; Day, N.E.; Luben, R.; Ferrari, P.; Slimani, N.; Norat, T.; Clavel-Chapelon, F.; Kesse, E.; Nieters, A.; Boeing, H.; et al. Dietary fibre in food and protection against colorectal cancer in the European Prospective Investigation into Cancer and Nutrition (EPIC): An observational study. Lancet 2003, 361, 1496–1501. [Google Scholar] [CrossRef]
- Park, Y.; Hunter, D.J.; Spiegelman, D.; Bergkvist, L.; Berrino, F.; van den Brandt, P.A.; Buring, J.E.; Colditz, G.A.; Freudenheim, J.L.; Fuchs, C.S.; et al. Dietary fiber intake and risk of colorectal cancer—A pooled analysis of prospective cohort studies. JAMA 2005, 294, 2849–2857. [Google Scholar] [CrossRef] [PubMed]
- Hu, F.B.; Stampfer, M.J.; Manson, J.E.; Rimm, E.; Colditz, G.A.; Rosner, B.A.; Hennekens, C.H.; Willett, W.C. Dietary fat intake and the risk of coronary heart disease in women. N. Engl. J. Med. 1997, 337, 1491–1499. [Google Scholar] [CrossRef] [PubMed]
- Mozaffarian, D.; Micha, R.; Wallace, S. Effects on coronary heart disease of increasing polyunsaturated fat in place of saturated fat: A systematic review and meta-analysis of randomized controlled trials. PLoS Med. 2010, 7, 1–10. [Google Scholar] [CrossRef] [PubMed]
- Jakobsen, M.U.; O’Reilly, E.J.; Heitmann, B.L.; Pereira, M.A.; Bälter, K.; Fraser, G.E.; Goldbourt, U.; Hallmans, G.; Knekt, P.; Liu, S.; et al. Major types of dietary fat and risk of coronary heart disease: A pooled analysis of 11 cohort studies. Am. J. Clin. Nutr. 2009, 89, 1–8. [Google Scholar] [CrossRef] [PubMed]
- Willett, W.C.; Stampfer, M.J.; Manson, J.E.; Colditz, G.A.; Speizer, F.E.; Rosner, B.A.; Hennekens, C.H. Intake of trans fatty acids and risk of coronary heart disease among women. Lancet 1993, 341, 581–585. [Google Scholar] [CrossRef]
- Oomen, C.M.; Ocké, M.C.; Feskens, E.J.M.; van Erp-Baart, M.-A.J.; Kok, F.J.; Kromhout, D. Association between trans fatty acid intake and 10-year risk of coronary heart disease in the Zutphen Elderly Study: A prospective population-based study. Lancet 2001, 357, 746–751. [Google Scholar] [CrossRef]
- Atkinson, C.; Whitley, E.; Ness, A.; Baker, I. Associations between types of dietary fat and fish intake and risk of stroke in the Caerphilly Prospective Study (CaPS). Public Health 2011, 125, 345–348. [Google Scholar] [CrossRef] [PubMed]
- He, K.; Rimm, E.B.; Marchant, A.; Rosner, B.A.; Stampfer, M.J.; Willett, W.C.; Ascherio, A. Fish consumption and risk of stroke in men. JAMA 2002, 288, 3130–3136. [Google Scholar] [CrossRef] [PubMed]
- Iso, H.; Rexrode, K.M.; Stampfer, M.J.; Manson, J.E.; Colditz, G.A.; Speizer, F.E.; Hennekens, C.H.; Willett, W.C. Intake of fish and omega-3 fatty acid and risk of stroke in women. JAMA 2001, 285, 304–312. [Google Scholar] [CrossRef] [PubMed]
- Chao, A.; Thun, M.J.; Connell, C.J.; McCullough, M.L.; Jacobs, E.J.; Flanders, W.D.; Rodriguez, C.; Sinha, R.; Calle, E.E. Meat consumption and risk of colorectal cancer. JAMA 2005, 293, 172–182. [Google Scholar] [CrossRef] [PubMed]
- Wolk, A.; Larsson, S.C.; Johansson, J.-E.; Ekman, P. Long-term fatty fish consumption and renal cell carcinoma incidence in women. JAMA 2006, 296, 1371–1376. [Google Scholar] [CrossRef] [PubMed]
- Micha, R.; Wallace, S.K.; Mozaffarian, D. Red and processed meat consumption and risk of incident coronary heart disease, stroke, and diabetes: A systematic review and meta-analysis. Circulation 2010, 121, 2271–2283. [Google Scholar] [CrossRef] [PubMed]
- Pan, A.; Sun, Q.; Bernstein, A.M.; Schulze, M.B.; Manson, J.A.E.; Willett, W.C.; Hu, F.B. Red meat consumption and risk of type 2 diabetes: 3 Cohorts of US adults and an updated meta-analysis. Am. J. Clin. Nutr. 2011, 94, 1088–1096. [Google Scholar] [CrossRef] [PubMed]
- Dalmeijer, G.W.; Struijk, E.A.; van der Schouw, Y.T.; Soedamah-Muthu, S.S.; Verschuren, W.M.M.; Boer, J.M.A.; Geleijnse, J.M.; Beulens, J.W.J. Dairy intake and coronary heart disease or stroke—A population-based cohort study. Int. J. Cardiol. 2013, 167, 925–929. [Google Scholar] [CrossRef] [PubMed]
- Cho, E.; Smith-Warner, S.A.; Spiegelman, D.; Beeson, W.L.; van den Brandt, P.A.; Colditz, G.A.; Folsom, A.R.; Fraser, G.E.; Freudenheim, J.L.; Giovannucci, E.; et al. Dairy foods, calcium, and colorectal cancer: A pooled analysis of 10 cohort studies. J. Natl. Cancer Inst. 2004, 96, 1015–1022. [Google Scholar] [CrossRef] [PubMed]
- Mellen, P.B.; Walsh, T.F.; Herrington, D.M. Whole grain intake and cardiovascular disease: A meta-analysis. Nutr. Metab. Cardiovasc. Dis. 2008, 18, 283–290. [Google Scholar] [CrossRef] [PubMed]
- De Munter, J.S.L.; Hu, F.B.; Spiegelman, D.; Franz, M.; van Dam, R.M. Whole grain, bran, and germ intake and risk of type 2 diabetes: A prospective cohort study and systematic review. PLoS Med. 2007, 4, 1385–1395. [Google Scholar] [CrossRef] [PubMed]
- Fung, T.T.; Malik, V.; Rexrode, K.M.; Manson, J.E.; Willett, W.C.; Hu, F.B. Sweetened beverage consumption and risk of coronary heart disease in women. Am. J. Clin. Nutr. 2009, 89, 1037–1042. [Google Scholar] [CrossRef] [PubMed]
- Hu, F.B.; Malik, V.S. Sugar-sweetened beverages and risk of obesity and type 2 diabetes: Epidemiologic evidence. Physol. Behav. 2010, 100, 47–54. [Google Scholar] [CrossRef] [PubMed]
- Pedersen, A.N.; Fagt, S.; Groth, M.V.; Christensen, T.; Biltoft-Jensen, A.; Matthiesen, J.; Andersen, N.L.; Kørup, K.; Hartkopp, H.; Ygil, K.H.; et al. Danskernes Kostvaner 2003–2008—Hovedresultater (Danes’ Dietary Habits 2003–2008—Main Results); Report; Danish Technical University, National Food Institute: Søborg, Denmark, 2010. [Google Scholar]
- WHO. Global Burden of Disease (GBD) Summary Tables. 2004. Available online: http://www.who.int/entity/healthinfo/global_burden_disease/DALY14_2004.xls?ua=1 (accessed on 29 June 2015).
- Brouwer, W.B.F.; Niessen, L.W.; Postma, M.J.; Rutten, F.F.H. Need for differential discounting of costs and health effects in cost effectiveness analyses. BMJ 2005, 331, 446–448. [Google Scholar] [CrossRef] [PubMed]
- Folkesundhedsrapporten Danmark 2007 (Report on Public Health in Denmark in 2007); Danish Institute of Public Health: Copenhagen, Denmark, 2007.
- Drewnowski, A.; Monsivais, P.; Maillot, M. Low-energy-density diets are associated with higher diet quality and higher diet costs in French Adjults. J. Am. Diet. Assoc. 2007, 107, 1028–1032. [Google Scholar] [CrossRef] [PubMed]
- Jensen, J.D.; Poulsen, S.K. The new Nordic Diet—Consumer expenditures and economic incentives estimated from a controlled intervention. BMC Public Health 2013, 13, 1114. [Google Scholar] [CrossRef] [PubMed]
- Van Baal, P.H.M.; van den Berg, M.; Hoogenveen, R.T.; Vijgen, S.M.C.; Engelfriet, P.M. Cost-effectiveness of a low-calorie diet and Orlistat for obese persons: Modeling long-term health gains through prevention of obesity-related chronic diseases. Value Health 2008, 11, 1033–1040. [Google Scholar] [CrossRef] [PubMed]
- Moodie, M.; Haby, M.; Wake, M.; Gold, L.; Carter, R. Cost-effectiveness of a family-based GP-mediated intervention targeting overweight and moderately obese children. Econ. Hum. Biol. 2008, 6, 363–376. [Google Scholar] [CrossRef] [PubMed]
- Raynor, H.A.; Kolanowski, C.K.; Esterlis, I.; Epstein, L.H. A cost-analysis of adopting a healthful diet in a family-based obesity treatment program. J. Am. Diet. Assoc. 2002, 102, 645–656. [Google Scholar] [CrossRef]
- Kristiansen, I.S.; Eggen, A.E.; Thelle, D.S. Cost effectiveness of incremental programmes for lowering serum cholesterol concentration: Is individual intervention worthwhile? Brit. Med. J. 1991, 302, 1119–1122. [Google Scholar] [CrossRef] [PubMed]
- Dalziel, K.; Segal, L. Time to give nutrition interventions a higher profile: Cost-effectiveness of 10 nutrition interventions. Health Prom. Int. 2007, 22, 271–282. [Google Scholar] [CrossRef] [PubMed]
- Barton, P.; Andronis, L.; Briggs, A.; McPherson, K.; Capewell, S. Effectiveness and cost effectiveness of cardiovascular disease prevention in whole populations: Modelling study. Brit. Med. J. 2011, 343, d4044. [Google Scholar] [CrossRef] [PubMed]
- WHO. Threshold Values for Intervention Cost-Effectiveness by Region. Available online: http://www.who.int/choice/costs/CER_levels/en/ (accessed on 27 February 2015).
- Michelsen, A.; Holm, L.; Jensen, K.O. Consumer acceptance of the New Nordic Diet. An exploratory study. Appetite 2013, 70, 14–21. [Google Scholar] [CrossRef] [PubMed]
© 2015 by the authors; licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Jensen, J.D.; Saxe, H.; Denver, S. Cost-Effectiveness of a New Nordic Diet as a Strategy for Health Promotion. Int. J. Environ. Res. Public Health 2015, 12, 7370-7391. https://doi.org/10.3390/ijerph120707370
Jensen JD, Saxe H, Denver S. Cost-Effectiveness of a New Nordic Diet as a Strategy for Health Promotion. International Journal of Environmental Research and Public Health. 2015; 12(7):7370-7391. https://doi.org/10.3390/ijerph120707370
Chicago/Turabian StyleJensen, Jørgen Dejgård, Henrik Saxe, and Sigrid Denver. 2015. "Cost-Effectiveness of a New Nordic Diet as a Strategy for Health Promotion" International Journal of Environmental Research and Public Health 12, no. 7: 7370-7391. https://doi.org/10.3390/ijerph120707370
APA StyleJensen, J. D., Saxe, H., & Denver, S. (2015). Cost-Effectiveness of a New Nordic Diet as a Strategy for Health Promotion. International Journal of Environmental Research and Public Health, 12(7), 7370-7391. https://doi.org/10.3390/ijerph120707370





