Predictors of Prevention Failure in College Students Participating in Two Indicated Depression Prevention Programs
Abstract
:1. Introduction
2. Method
2.1. Participants
2.2. Procedures
2.3. Prevention Conditions
2.4. Measures
2.5. Data Completeness and Data Analysis
3. Results
3.1. Risk for Depression Persistence
3.2. Risk Factor Variables
| Variables | 1 | 2 | 3 | 4 | 5 | 6 | 7 | 8 | 9 | 10 | 11 | 12 | 13 |
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| 1. Male sex | 1 | ||||||||||||
| 2. Age | −0.216 | 1 | |||||||||||
| 3. Single marital status | −0.029 | 0.177 | 1 | ||||||||||
| 4. High social class | 0.234 | 0.040 | −0.036 | 1 | |||||||||
| 5. Academic year | −0.369 | 0.213 | 0.357 | −0.189 | 1 | ||||||||
| 6. Rural residence | −0.156 | 0.266 | 0.044 | −0.023 | 0.200 | 1 | |||||||
| 7. Sport practice | 0.145 | −0.098 | −0.234 | −0.102 | −0.029 | −0.181 | 1 | ||||||
| 8. Anxiety symptoms | 0.112 | 0.259 | 0.271 | −0.009 | 0.224 | 0.144 | 0.173 | 1 | |||||
| 9. Depressive symptoms | 0.141 | 0.076 | 0.073 | −0.123 | 0.149 | 0.117 | 0.166 | 0.571 | 1 | ||||
| 10. Irrational beliefs | −0.146 | −0.354 | 0.129 | −0.055 | 0.136 | −0.035 | −0.023 | 0.119 | 0.241 | 1 | |||
| 11. Assertiveness | 0.036 | 0.244 | −0.146 | 0.132 | −0.165 | 0.093 | −0.068 | −0.354 | −0.216 | −0.280 | 1 | ||
| 12. Pleasant activities | −0.325 | 0.082 | −0.069 | −0.145 | −0.046 | 0.179 | −0.017 | −0.131 | −0.232 | −0.181 | 0.175 | 1 | |
| 13. Life change units | 0.162 | 0.291 | 0.041 | 0.048 | −0.121 | −0.025 | −0.029 | 0.072 | 0.001 | −0.067 | 0.240 | 0.055 | 1 |
| Mean (% occurrence for 1, 3, 4, 5, 6, 7) | 18.0 | 23.3 | 93.2 | 7.5 | 55.6 | 41.4 | 27.8 | 15.0 | 25.3 | 69.6 | −14.1 | 17.5 | 382.9 |
| Standard deviation | NA | 4.5 | NA | NA | NA | NA | NA | 8.5 | 7.9 | 8.6 | 20.4 | 10.8 | 207.1 |
| Correlation with outcome | 0.032 | 0.272 | 0.012 | 0.256 | 0.163 | 0.011 | 0.093 | 0.261 | 0.154 | −0.022 | −0.359 | −0.238 | 0.105 |
3.3. Classification Tree Analysis
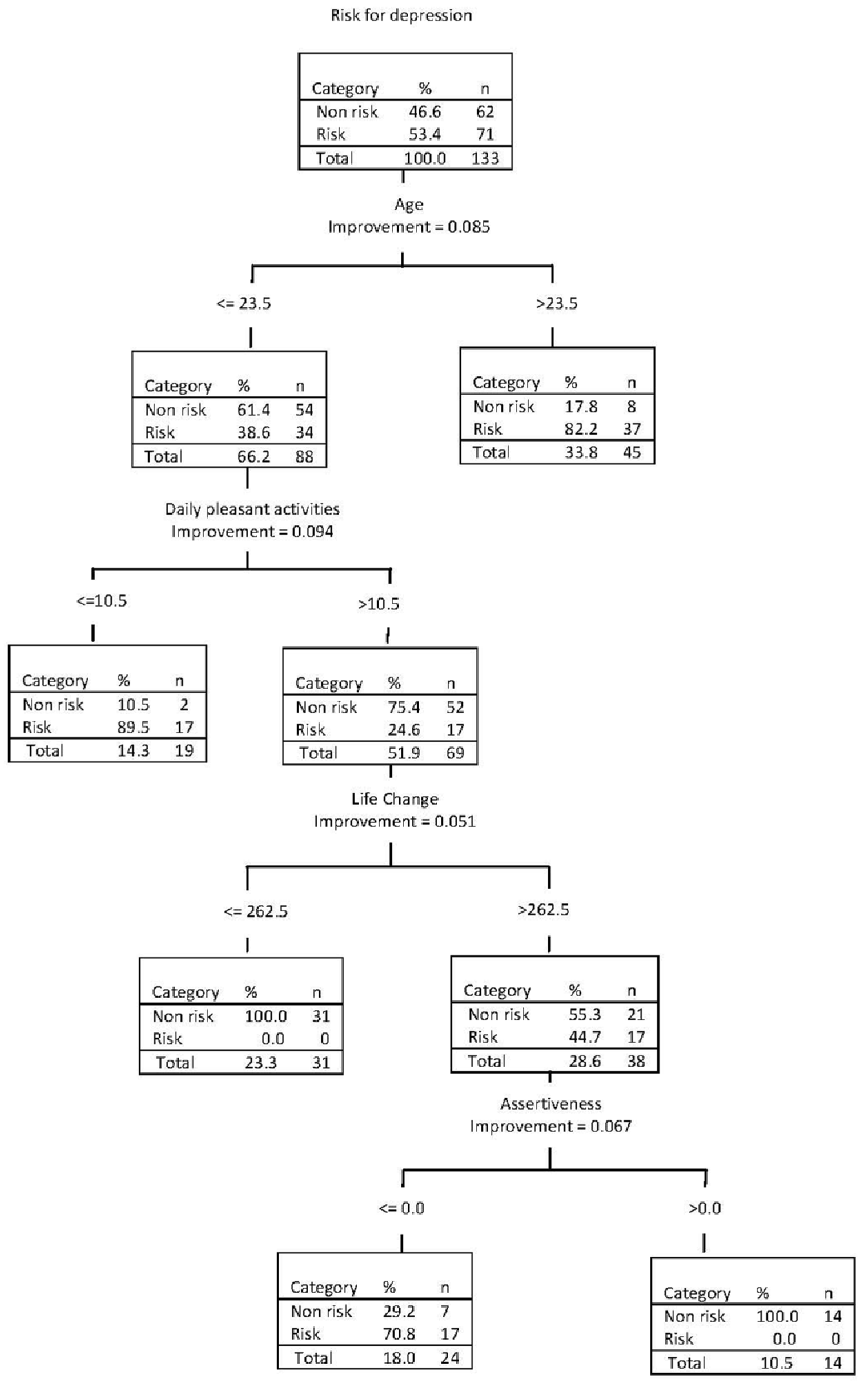
4. Discussion
5. Conclusions
Acknowledgments
Author Contributions
Conflicts of Interest
References
- Pillay, A.L.; Edwards, S.D.; Gambu, S.Q.; Dhlomo, R.M. Depression among university students in South Africa. Psychol. Rep. 2002, 91, 725–728. [Google Scholar] [CrossRef]
- Tomoda, A.; Mori, K.; Kimura, M.; Takahashi, T.; Kitamura, T. One-year prevalence and incidence of depression among first-year university students in Japan: A preliminary study. Psychiat. Clin. Neurosciences 2000, 54, 583–588. [Google Scholar] [CrossRef]
- Vázquez, F.L.; Blanco, V. Prevalence of DSM-IV major depression among Spanish university students. J. Amer. Coll. Health 2008, 57, 165–171. [Google Scholar] [CrossRef]
- Adams, T.B.; Wharton, C.M.; Quilter, L.; Hirsch, T. The association between mental health and acute infectious illness among a national sample of 18- to 24-year-old college students. J. Amer. Coll. Health 2008, 56, 657–663. [Google Scholar] [CrossRef]
- Kessler, R.C.; Walters, E.E.; Forthofer, M.S. The social consequences of psychiatric disorders, III: Probability of marital stability. Amer. J. Psychiat. 1998, 155, 1092–1096. [Google Scholar]
- Suicide Prevention Resource Center. Promoting Mental Health and Preventing Suicide in College and University Settings; Education Development Center, Inc.: Newton, MA, USA, 2004. [Google Scholar]
- Hysenbegasi, A.; Hass, S.L.; Rowland, C.R. The impact of depression on the academic productivity of university students. J. Ment. Health. Policy Econ. 2005, 8, 145–151. [Google Scholar]
- Miech, R.A.; Caspi, A.; Moffitt, T.E.; Wright, B.R.E.; Silva, P.A. Low socioeconomic status and mental disorders: A longitudinal study of selection and causation during young adulthood. Amer. J. Sociol. 1999, 104, 1096–1131. [Google Scholar]
- Cuijpers, P.; Smit, F.; Willemse, G. Predicting the onset of major depression in subjects with subthreshold depression in primary care: A prospective study. Acta Psychiat. Scand. 2005, 111, 133–138. [Google Scholar] [CrossRef]
- Cuijpers, P.; de Graaf, R.; van Dorsselaer, S. Minor depression: Risk profiles, functional disability, health care use and risk of developing major depression. J. Affect. Disorders 2004, 79, 71–79. [Google Scholar] [CrossRef]
- Vázquez, F.L.; Blanco, V. Symptoms of depression and related factors among Spanish university students. Psychol. Rep. 2006, 99, 583–590. [Google Scholar]
- Fergusson, D.M.; Horwood, L.J.; Ridder, E.M.; Beautrais, A.L. Subthreshold depression in adolescence and mental health outcomes in adulthood. Arch. Gen. Psychiat. 2005, 62, 66–72. [Google Scholar] [CrossRef]
- Gotlib, I.H.; Lewinsohn, P.M.; Seeley, J.R. Symptoms versus a diagnosis of depression: Differences in psychosocial functioning. J. Consult. Clin. Psychol. 1995, 63, 90–100. [Google Scholar] [CrossRef]
- Fava, G.A. Subclinical symptoms in mood disorders: Pathophysiological and therapeutic implications. Psychol. Med. 1999, 29, 47–61. [Google Scholar] [CrossRef]
- Mrazek, P.; Haggerty, R.J. Reducing Risks for Mental Disorders. Frontiers for Preventive Intervention Research; National Academy Press: Washington, DC, USA, 1994. [Google Scholar]
- Sutton, J.M. Prevention of depression in youth: A qualitative review and future suggestions. Clin. Psychol. Rev. 2007, 27, 552–571. [Google Scholar] [CrossRef]
- Muñoz, R.F.; Cuijpers, P.; Smit, F.; Barrera, A.Z.; Leykin, Y. Prevention of major depression. Annu. Rev. Clin. Psychol. 2010, 6, 181–212. [Google Scholar] [CrossRef]
- Horowitz, J.L.; Garber, J. The prevention of depressive symptoms in children and adolescents: A meta-analytic review. J. Consult. Clin. Psychol. 2006, 74, 401–415. [Google Scholar] [CrossRef]
- Seligman, M.E.P.; Schulman, P.; DeRubeis, R.J.; Hollon, S.D. The prevention of depression and anxiety. Prev. Treat. 1999, 2. [Google Scholar] [CrossRef]
- Seligman, M.E.P.; Schulman, P.; Tryon, A.M. Group prevention of depression and anxiety symptoms. Behav. Res. Ther. 2007, 45, 1111–1126. [Google Scholar] [CrossRef]
- Vázquez, F.L.; Torres, A.; Blanco, V.; Díaz, O.; Otero, P.; Hermida, E. Comparison of relaxation training with a cognitive-behavioural intervention for indicated prevention of depression in university students: A randomized controlled trial. J. Psychiat. Res. 2012, 46, 1456–1463. [Google Scholar]
- Curry, J.; Rohde, P.; Simons, A.; Silva, S.; Vitiello, B.; Kratochvil, C.; Reinecke, M.; Feeny, N.; Wells, K.; Pathak, S.; et al. Predictors and moderators of acute outcome in the Treatment for Adolescents With Depression Study (TADS). J. Am. Acad. Child. Adolesc. Psychiat. 2006, 45. [Google Scholar] [CrossRef]
- Spek, V.; Nyklíček, I.; Cuijpers, P.; Pop, V. Predictors of outcome of group and internet-based cognitive behaviour therapy. J. Affect. Disord. 2008, 105. [Google Scholar] [CrossRef]
- Bouteyre, E.; Maurel, M.; Bernaud, J.L. Daily hassles and depressive symptoms among first year psychology students in France: The role of coping and social support. Stress Health 2007, 23, 93–99. [Google Scholar] [CrossRef]
- Eisenberg, D.; Gollust, S.E.; Golberstein, E.; Hefner, J.L. Prevalence and correlates of depression, anxiety, and suicidality among university students. Amer. J. Orthopsychiat. 2007, 77, 534–542. [Google Scholar] [CrossRef]
- Crowell, B.A.; George, L.K.; Blazer, D.; Landerman, R. Psychosocial risk factors and urban/rural differences in the prevalence of major depression. Brit. J. Psychiat. 1986, 149, 307–314. [Google Scholar] [CrossRef]
- McLennan, J. University blues: Depression among tertiary students during an academic year. Brit. J. Guid. Couns. 1992, 20, 186–192. [Google Scholar] [CrossRef]
- Elliot, C.A.; Kennedy, C.; Morgan, G.; Anderson, S.K.; Morris, D. Undergraduate physical activity and depressive symptoms: A national study. Am. J. Health Behav. 2012, 36, 230–241. [Google Scholar] [CrossRef]
- Lewinsohn, P.M. The Behavioural Study and Treatment of Depression. In Progress in Behaviour Modification; Hersen, M., Eisler, R.M., Miller, P.M., Eds.; Academic Press: New York, NY, USA, 1975; Volume 1, pp. 19–65. [Google Scholar]
- Lewinsohn, P.M.; Hoberman, H.; Teri, L.; Hautzinger, M. An integrative theory of depression. In Theoretical Issues in Behavior Therapy; Bootzin, R.R., Ed.; Academic Press: New York, NY, USA, 1985; pp. 291–315. [Google Scholar]
- Bitsika, V.; Sharpley, C.F. Comorbidity of anxiety-depression among Australian university students: Implications for student counsellors. Brit. J. Guid. Couns. 2012, 40, 385–394. [Google Scholar] [CrossRef]
- Lemon, S.C.; Roy, J.; Clark, M.A.; Friedmann, P.D.; Rakowski, W. Classification and regression tree analysis in public health: Methodological review and comparison with logistic regression. Ann. Behav. Med. 2003, 26, 172–181. [Google Scholar]
- Haukoos, J.S.; Witt, M.D.; Zeumer, C.M.; Lee, T.J.; Halamka, J.D.; Lewis, R.J. Emergency department triage of patients infected with HIV. Acad. Emerg. Med. 2002, 9, 880–888. [Google Scholar] [CrossRef]
- Schoevers, R.A.; Smit, F.; Deeg, D.J.; Cuijpers, P.; Dekker, J.; van Tilburg, W.; Beekman, A.T.F. Prevention of late-life depression in primary care: Do we know where to begin? Amer. J. Psychiat. 2006, 163, 1611–1621. [Google Scholar] [CrossRef]
- Seeley, J.R.; Stice, E.; Rohde, P. Screening for depression prevention: Identifying adolescent girls at high risk for future depression. J. Abnormal Psychol. 2009, 118, 161–170. [Google Scholar] [CrossRef]
- Radloff, L.S. A CES-D scale: A self-report depression scale for research in the general population. Appl. Psychol. Meas. 1977, 1, 385–401. [Google Scholar] [CrossRef]
- Worth, A.P.; Cronin, M.T.D. The use of discriminant analysis, logistic regression and classification tree analysis in the development of classification models for human health effects. J. Mol. Struct. 2003, 622, 97–111. [Google Scholar] [CrossRef]
- Hosmer, D.W.; Lemeshow, S. Applied Logistic Regression, 2nd ed.; Wiley: New York, NY, USA, 2000. [Google Scholar]
- Berman, M.I.; Hegel, M.T. Predicting depression outcome in mental health treatment: A recursive partitioning analysis. Psychother. Res. 2014. [Google Scholar] [CrossRef]
- Siddique, J.; Chung, J.Y.; Brown, C.H.; Miranda, J. Comparative Effectiveness of Medication versus Cognitive Behavioral Therapy in a Randomized Controlled Trial of Low-income Young Minority Women with Depression. J. Consult. Clin. Psychol. 2012, 80, 995–1006. [Google Scholar] [CrossRef]
- Blanco, V.; Rohde, P.; Vázquez, F.L.; Torres, A. Identification of caregivers at greatest risk of major depression in two prevention studies. Psycother. Res. 2013. [Google Scholar] [CrossRef]
- Rohde, P.; Stice, E.; Gau, J.M. Effects of three depression prevention interventions on risk for depressive disorder onset in the context of depression risk factors. Prev. Sci. 2012, 13. [Google Scholar] [CrossRef]
- Muñoz, R.F.; Ying, Y.W. The Prevention of Depression: Research and Practice; Johns Hopkins University Press: Baltimore, MD, USA, 1993. [Google Scholar]
- Lewinsohn, P.M.; Muñoz, R.; Youngren, M.A.; Zeiss, A. Control Your Depression; Fireside Books: New York, NY, USA, 1992. [Google Scholar]
- Lewinsohn, P.M.; Hoberman, H.M.; Rosenbaum, M. A prospective study of risk factors for unipolar depression. J. Abnormal Psychol. 1988, 97, 251–264. [Google Scholar] [CrossRef]
- Van Dam, E.A.; Hosman, C.M.H.; Hoogduin, C.A.L.; Schaap, C.P.D.R. The coping with depression course: Short-term outcomes and mediating effects of a randomized controlled trial in the treatment of subclinical depression. Behav. Ther. 2003, 34, 381–396. [Google Scholar] [CrossRef]
- Stice, E.; Burton, E.; Bearman, S.K.; Rohde, P. Randomized trial of a brief depression prevention program: An elusive search for a psychosocial placebo control condition. Behav. Res. Ther. 2007, 45, 863–876. [Google Scholar] [CrossRef]
- Westerhof, G.J.; Bohlmeijer, E.T.; van Beljouw, I.M.J.; Pot, A.M. Improvement in personal meaning mediates the effects of a life review intervention on depressive symptoms in a randomized controlled trial. Gerontologist 2010, 50, 541–549. [Google Scholar] [CrossRef]
- Folkman, S.; Chesney, M.; Collette, L.; Boccellari, A.; Cooke, M. Postbereavement depressive mood and its prebereavement predictors in HIV+ and HIV− gay men. J. Pers. Soc. Psychol. 1996, 70, 336–348. [Google Scholar] [CrossRef]
- Ginsburg, G.S.; Baker, E.V.; Mullany, B.C.; Barlow, A.; Goklish, N.; Hastings, R; Thurm, A.E.; Speakman, K.; Reid, R.; Walkup, J. Depressive symptoms among reservation-based pregnant American Indian adolescents. MCHJ 2008, 12, S110–S118. [Google Scholar]
- Orr, S.T.; Blazer, D.G.; James, S.A.; Reiter, J.P. Depressive symptoms and indicators of maternal health status during pregnancy. J. Womens Health 2007, 16, 535–542. [Google Scholar] [CrossRef]
- Van Voorhees, B.W.; Paunesku, D.; Gollan, J.; Kuwabara, S.; Reinecke, M.; Basu, A. Predicting future risk of depressive episode in adolescents: The Chicago Adolescent Depression Risk Assessment (CADRA). Ann. Fam. Med. 2008, 6, 503–511. [Google Scholar] [CrossRef]
- Muñoz, R.F.; Ying, Y.W.; Armas, R.; Chan, F.; Gurza, R. The San Francisco Depression Prevention Research Project: A Randomized Trial with Medical Outpatients. In Depression Prevention: Research Directions; Muñoz, R.F., Ed.; Hemisphere Press: Washington, DC, USA, 1987; pp. 199–215. [Google Scholar]
- Muñoz, R.F.; Le, H.N.; Ippen, C.G.; Díaz, M.A.; Urizar, G.G.; Soto, J.; Mendelson, T.; Delucchi, K.; Lieberman, A.F. Prevention of postpartum depression in low-income women: Development of the Mamás y bebés/mothers and babies course. Cogn. Behav. Pract. 2007, 14. [Google Scholar] [CrossRef]
- Bernstein, D.A.; Borkovec, T.D. Progressive Relaxation Training: A Manual for the Helping Profession; Research Press: Champaign, IL, USA, 1973. [Google Scholar]
- Davis, M.; McKay, M.; Eshelman, E.R. The Relaxation and Stress Reduction Workbook; New Harbinger: Richmond, CA, USA, 1980. [Google Scholar]
- Jorm, A.F.; Morgan, A.J.; Hetrick, S.E. Relaxation for depression. Cochrane Database Syst. Rev. 2008. [Google Scholar] [CrossRef]
- First, M.B.; Spitzer, R.L.; Gibbon, M.; Williams, J.B.W. Structured Clinical Interview for DSM-IV Axis I Disorders—Clinician Version (SCID-CV); American Psychiatric Press: Washington, DC, USA, 1997. [Google Scholar]
- Himmelfarb, S.; Murrell, S.A. Reliability and validity of five mental health scales in older persons. J. Gerontol. 1983, 38, 333–339. [Google Scholar] [CrossRef]
- Beck, A.T.; Epstein, N.; Brown, G.; Steer, R. An inventory for measuring clinical anxiety: Psychometric properties. J. Consult. Clin. Psychol. 1988, 56, 893–897. [Google Scholar] [CrossRef]
- Malouff, J.M.; Schutte, N.S. Development and validation of a measure of irrational belief. J. Consult. Clin. Psychol. 1986, 54, 860–862. [Google Scholar] [CrossRef]
- Jones, R.A. A factored measure of Ellis’ irrational belief system with personality and maladjustment correlates. Diss. Abstr. Int. 1969, 29, 4379–4380. [Google Scholar]
- Crowne, D.P.; Marlowe, D. The Approval Motive: Studies in Evaluative Dependence; Wiley: New York, NY, USA, 1964. [Google Scholar]
- Rathus, S.A. A 30-item schedule for assessing assertive behavior. Behav. Ther. 1973, 4, 398–406. [Google Scholar] [CrossRef]
- Muñoz, R.F.; Miranda, J. Group Therapy Manual for Cognitive-behavioral Treatment of Depression; RAND: California, CA, USA, 2000. [Google Scholar]
- Holmes, T.H.; Rahe, R.H. The social readjustment rating scale. J. Psychosom. Res. 1967, 11, 213–218. [Google Scholar] [CrossRef]
- Miller, M.A.; Rahe, R.H. Life changes scaling for the 1990s. J. Psychosom. Res. 1997, 43, 279–292. [Google Scholar] [CrossRef]
- Guillemin, F.; Bombardier, C.; Beaton, D. Cross-cultural adaptation of health related quality of life measures: Literature review and proposed guidelines. J. Clin. Epidemiol. 1993, 43, 1417–1432. [Google Scholar] [CrossRef]
- Brislin, R.W.; Lonner, W.J.; Thorndike, E.M. Cross-cultural Research Methods; Wiley: New York, NY, USA, 1973. [Google Scholar]
- Steinberg, D.; Colla, P. CART—Classification and Regression Trees; Salford Systems: San Diego, CA, USA, 1997. [Google Scholar]
- Bandura, A. Principles of Behavior Modification; Holt, Rinehart & Winston: New York, NY, USA, 1969. [Google Scholar]
- Baykan, Z.; Naçar, M.; Çetinkaya, F. Depression, anxiety, and stress among last-year students at Erciyes University Medical School. Acad. Psychiat. 2012, 36, 64–65. [Google Scholar]
- Cuijpers, P.; van Straten, A.; Warmerdam, L. Behavioral activation treatments of depression: A meta-analysis. Clin. Psychol. Rev. 2007, 27, 318–326. [Google Scholar] [CrossRef]
- Morgan, A.J.; Jorm, A.F. Self-help interventions for depressive disorders and depressive symptoms: A systematic review. Ann. Gen. Psychiatry 2008, 7. [Google Scholar] [CrossRef]
- Lewinsohn, P.M.; Graf, M. Pleasant activities and depression. J. Consult. Clin. Psychol. 1973, 41, 261–268. [Google Scholar] [CrossRef]
- Harmon, T.M.; Nelson, R.O.; Hayes, S.C. Self-monitoring of mood versus activity by depressed clients. J. Consult. Clin. Psychol. 1980, 48, 30–38. [Google Scholar] [CrossRef]
- Haase, C.M.; Heckhausen, J.; Silbereisen, R.K. The interplay of occupational motivation and well-being during the transition from university to work. Dev. Psychol. 2012, 48, 1739–1751. [Google Scholar] [CrossRef]
- Peng, L.; Zhang, J.; Li, M.; Li, P.; Zhang, Y.; Zuo, X.; Miao, Y.; Xu, Y. Negative life events and mental health of Chinese medical students: The effect of resilience, personality and social support. Psychiat. Res. 2012, 196, 138–141. [Google Scholar] [CrossRef]
- Gau, J.M.; Stice, E.; Rohde, P.; Seeley, J.R. Negative life events and substance use moderate cognitive-behavioral adolescent depression prevention intervention. Cogn. Behav. Ther. 2012, 41, 241–250. [Google Scholar] [CrossRef]
- Ross, S.E.; Neibling, B.C.; Heckert, T.M. Sources of stress among college students. Coll. Stud. J. 1999, 33, 312–317. [Google Scholar]
- Langone, M. Assertiveness and Lewinsohn’s theory of depression: An empirical test. Behav. Ther. 1979, 2, 21. [Google Scholar]
- Nezu, A.M.; Nezu, C.M.; Nezu, V.A. Depression, general distress, and causal attributions among university students. J. Abnormal Psychol. 1986, 95, 184–186. [Google Scholar] [CrossRef]
- Lazarus, R.; Folkman, S. Stress, Appraisal and Coping; Springer: New York, NY, USA, 1984. [Google Scholar]
- Tomaka, J.; Palacios, R.; Schneider, K.T.; Colotla, M.; Concha, J.B.; Harrald, M.M. Assertiveness predicts threat and challenge reactions to potential stress among women. J. Pers. Soc. Psychol. 1999, 76, 1008–1021. [Google Scholar] [CrossRef]
- Pryor, J.H.; Hurtado, S.; DeAngelo, L.; Palucki Blake, L.; Tran, S. The American Freshman: National Norms Fall 2010; Higher Education Research Institute, UCLA: Los Angeles, CA, USA, 2010. [Google Scholar]
© 2014 by the authors; licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution license (http://creativecommons.org/licenses/by/3.0/).
Share and Cite
Blanco, V.; Rohde, P.; Vázquez, F.L.; Otero, P. Predictors of Prevention Failure in College Students Participating in Two Indicated Depression Prevention Programs. Int. J. Environ. Res. Public Health 2014, 11, 3803-3821. https://doi.org/10.3390/ijerph110403803
Blanco V, Rohde P, Vázquez FL, Otero P. Predictors of Prevention Failure in College Students Participating in Two Indicated Depression Prevention Programs. International Journal of Environmental Research and Public Health. 2014; 11(4):3803-3821. https://doi.org/10.3390/ijerph110403803
Chicago/Turabian StyleBlanco, Vanessa, Paul Rohde, Fernando L. Vázquez, and Patricia Otero. 2014. "Predictors of Prevention Failure in College Students Participating in Two Indicated Depression Prevention Programs" International Journal of Environmental Research and Public Health 11, no. 4: 3803-3821. https://doi.org/10.3390/ijerph110403803
APA StyleBlanco, V., Rohde, P., Vázquez, F. L., & Otero, P. (2014). Predictors of Prevention Failure in College Students Participating in Two Indicated Depression Prevention Programs. International Journal of Environmental Research and Public Health, 11(4), 3803-3821. https://doi.org/10.3390/ijerph110403803





