Radiation Dose in the Thyroid and the Thyroid Cancer Risk Attributable to CT Scans for Pediatric Patients in One General Hospital of China
Abstract
:1. Introduction
2. Materials and Methods
2.1. Collection of CT Scans
2.2. Dose Estimation
2.3. Cancer Risk Estimation for the Chinese Population


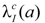 is the baseline incidence rates of sex- and age-specific thyroid cancer in mainland China. In Equations (3) and (4), ERR per Gy are shown for males and females, respectively.
is the baseline incidence rates of sex- and age-specific thyroid cancer in mainland China. In Equations (3) and (4), ERR per Gy are shown for males and females, respectively.3. Results
3.1. Collected Information
| Protocols | Frequency | Percentage (%) |
|---|---|---|
| Paranasal sinus | 136 | 10.4 |
| Head | 696 | 53.3 |
| Chest | 139 | 10.6 |
| Abdomen/pelvis | 242 | 18.5 |
| Spine | 40 | 3.1 |
| limb/others | 54 | 4.1 |
| Total | 1,307 | 100 |
| Age (years) at Scan | CT Protocol | |||||
|---|---|---|---|---|---|---|
| Paranasal Sinus CT | Head CT | Chest CT | ||||
| Boys | Girls | Boys | Girls | Boys | Girls | |
| 0 | - | - | 5 | 6 | 1 | 1 |
| 1–<5 | 4 | - | 83 | 50 | 6 | 5 |
| 5–<10 | 35 | 18 | 193 | 82 | 12 | 6 |
| 10–15 | 50 | 29 | 193 | 65 | 51 | 31 |
| Overall | 89 | 47 | 470 | 203 | 70 | 43 |
3.2. Radiation Dose
| Parameters | Paranasal Sinus CT | Head CT | Chest CT | ||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|
| Exposed age (years) | 1–<5 | 5–<10 | 10–15 | 0 | 1–<5 | 5–<10 | 10–15 | 0 | 1–<5 | 5–<10 | 10–15 |
| Kilovoltage (kV) | 120 | 120 | 120 | 118 a | 120 | 120 | 120 | 120 | 120 | 120 | 120 |
| Tube current (mA) | 255 | 237 | 254 | 161 | 178 | 164 | 163 | 313 | 300 | 375 | 330 |
| Rotation time (s) | 0.5 | 0.5 | 0.5 | 1.5 | 1.5 | 1.5 | 1.5 | 0.5 | 0.5 | 0.5 | 0.5 |
| pitch | 0.688 | 0.688 | 0.688 | 1 | 1 | 1 | 1 | 0.688 | 0.688 | 0.938 | 0.938 |
| CTDIvol (m Gy) | 32.4 | 34.7 | 35.1 | 29.9 | 33.8 | 33.6 | 34.1 | 10.4 | 11.8 | 14.1 | 11.6 |
| DLP (m Gy·cm) | 369.3 | 337.5 | 399.0 | 327.7 | 374.1 | 394.2 | 413.2 | 243.0 | 254.2 | 358.0 | 353.8 |
| Scan mode | Spiral | Axial | Spiral | ||||||||
| Detector collimation (mm) | 16 × 1.5 | 16 × 1.5 | 16 × 1.5 | ||||||||
| Scan thickness (mm) | 5 | 6 | 5 | ||||||||
| Scan-field-of-view | From frontal sinus to upper alveolar bone | Covered cranium | From thoracic inlet to the costophrenic angle | ||||||||
| CT protocol | Age (years) at Scan | |||
|---|---|---|---|---|
| 0 | 1–<5 | 5–<10 | 10–15 | |
| Paranasal sinus CT | - | 0.92 | 0.65 | 0.61 |
| Head CT | 2.45 | 1.82 | 1.38 | 1.10 |
| Chest CT | 5.76 | 4.34 | 3.50 | 2.63 |
3.3. Cancer Risk
| Gender | Age at Exposure | |||
|---|---|---|---|---|
| 0 | 5 | 10 | 15 | |
| Boys | 136 | 91 | 60 | 39 |
| Girls | 964 | 639 | 422 | 275 |
| Age at Exposure | Paranasal Sinus CT | Head CT | Chest CT |
|---|---|---|---|
| Mean (Min-Max) | Mean (Min-Max) | Mean (Min-Max) | |
| Girls | |||
| 0 | - | 23.6 (-) | 55.5 (-) |
| 1–<5 | - | 14.5 (12.6–48.5) | 40.3 (30.1–65.4) |
| 5–<10 | 3.6 (3.0–4.2) | 8.0 (6.3–32.5) | 26.4 (16.0–44.7) |
| 10–15 | 2.2 (1.7–2.6) | 3.5 (2.8–4.6) | 8.8 (7.0–27.5) |
| Overall | 2.7 (1.7–4.2) | 8.7 (2.8–48.5) | 14.1 (7.0–65.4) |
| Boys | |||
| 0 | - | 3.4 (-) | 7.8 (-) |
| 1–<5 | 1.0 (0.9–1.1) | 2.0 (1.8–3.6) | 5.8 (4.3–8.5) |
| 5–<10 | 0.5 (0.4–0.6) | 1.1 (0.9–3.2) | 2.9 (2.3–5.4) |
| 10–15 | 0.3 (0.2–0.4) | 0.5 (0.4–1.3) | 1.5 (1.0–7.9) |
| Overall | 0.4 (0.2–1.1) | 1.1 (0.4–3.6) | 2.2 (1.0–8.5) |
4. Discussion
5. Conclusions
Acknowledgments
Author Contributions
Conflicts of Interest
References
- Kilfoy, B.A.; Zheng, T.; Holford, T.R.; Han, X.; Ward, M.H.; Sjodin, A.; Zhang, Y.; Bai, Y.; Zhu, C.; Guo, G.L.; et al. International patterns and trends in thyroid cancer incidence, 1973–2002. Cancer Causes Control 2009, 20, 525–531. [Google Scholar] [CrossRef]
- Davies, L.; Welch, H.G. Increasing incidence of thyroid cancer in the United States, 1973–2002. J. Am. Med. Assoc. 2006, 295, 2164–2167. [Google Scholar] [CrossRef]
- Liu, S.Q.; Zhang, S.Q.; Chen, W.Q.; Chen, L.L.; Zhang, S.W.; Zhang, X.D.; Zheng, R.S. Trend of ineidence and mortality on thyroid cancer in China during 2003–2007. Chin. J. Epidemoil. 2012, 33, 1044–1048. [Google Scholar]
- Qian, B.; He, M.; Dong, S.; Wang, J.; Chen, K. Incidence and mortality of thyroid cancers in Tianjin from 1981 to 2001. Chin. J. Endocinol. Metab. 2005, 21, 432–434. [Google Scholar]
- Wang, N.; Zhu, W.-X.; Xing, X.-M.; Yang, L.; Li, P.-P.; You, W.-C. Time trends of cancer incidence in urban beijing, 1998–2007. Chin. J. Cancer Res. 2011, 23, 15–20. [Google Scholar] [CrossRef]
- Zhu, C.; Zheng, T.; Kilfoy, B.A.; Han, X.; Ma, S.; Ba, Y.; Bai, Y.; Wang, R.; Zhu, Y.; Zhang, Y.; et al. A birth cohort analysis of the incidence of papillary thyroid cancer in the United States, 1973–2004. Thyroid 2009, 19, 1061–1066. [Google Scholar] [CrossRef]
- Schonfeld, S.J.; Lee, C.; Berrington de Gonzalez, A. Medical exposure to radiation and thyroid cancer. Clin. Oncol. (R. Coll. Radiol.) 2011, 23, 244–250. [Google Scholar] [CrossRef]
- International Commission on Radiological Protection. The 2007 Recommendations of the International Commission on Radiological Protection. ICRP publication 103. Ann. ICRP 2007, 37, 1–332.
- Mettler, F.A., Jr.; Huda, W.; Yoshizumi, T.T.; Mahesh, M. Effective doses in radiology and diagnostic nuclear medicine: A catalog. Radiology 2008, 248, 254–263. [Google Scholar] [CrossRef]
- Brenner, D.J.; Hall, E.J. Computed tomography—An increasing source of radiation exposure. N. Engl. J. Med. 2007, 357, 2277–2284. [Google Scholar] [CrossRef]
- United Nations Scientific Committee on the Effects of Atomic Radiation. Sources and Effects of Ionizing Radiation. UNSCEAR 2008 Report to the General Assembly with Annexes; United Nations: New York, NY, USA, 2010.
- Dawson, P.; Punwani, S. The thyroid dose burden in medical imaging: A re-examination. Eur. J. Radiol. 2009, 69, 74–79. [Google Scholar] [CrossRef]
- Al-Senan, R.; Mueller, D.L.; Hatab, M.R. Estimating thyroid dose in pediatric CT exams from surface dose measurement. Phys. Med. Biol. 2012, 57, 4211–4221. [Google Scholar] [CrossRef]
- Huda, W.; Spampinato, M.V.; Tipnis, S.V.; Magill, D. Computation of thyroid doses and carcinogenic radiation risks to patients undergoing neck CT examinations. Radiat. Prot. Dosimetry 2013, 156, 436–444. [Google Scholar] [CrossRef]
- Pearce, M.S.; Salotti, J.A.; Little, M.P.; McHugh, K.; Lee, C.; Kim, K.P.; Howe, N.L.; Ronckers, C.M.; Rajaraman, P.; Craft, A.W.; et al. Radiation exposure from CT scans in childhood and subsequent risk of leukaemia and brain tumours: A retrospective cohort study. Lancet 2012, 380, 499–505. [Google Scholar] [CrossRef]
- Mathews, J.D.; Forsythe, A.V.; Brady, Z.; Butler, M.W.; Goergen, S.K.; Byrnes, G.B.; Giles, G.G.; Wallace, A.B.; Anderson, P.R.; Guiver, T.A.; et al. Cancer risk in 680,000 people exposed to computed tomography scans in childhood or adolescence: Data linkage study of 11 million Australians. Br. Med. J. 2013, 346. [Google Scholar] [CrossRef]
- Fan, Y.-H.; Yue, B.-R.; Liu, L.-T. Present situation and analysis of medical radioactive equipment. (in Chinese). Chin. Med. Equip. 2005, 2, 51–53. [Google Scholar]
- Zhang, W.-J.; Cao, J.-S.; Yuan, L.; Sun, Q.-F.; Su, X. The situation and analysis of radiology equipment in China. (in Chinese). Chin. J. Radiol. Med. Protect. 2012, 32, 87–89. [Google Scholar]
- Su, Y.; Chen, J.; Xiao, G.; Sun, Q.-F.; Niu, H.; Fu, Y. Investigation of CT scan frequency in children based on RIS in a hospital. (in Chinese). Chin. J. Radiol. Med. Protect. 2014, 34, 41–44. [Google Scholar]
- Feng, S.-T.; Law, M.-W.; Huang, B.; Ng, S.; Li, Z.-P.; Meng, Q.-F.; Khong, P.-L. Radiation dose and cancer risk from pediatric CT examinations on 64-slice CT: A phantom study. Eur. J. Radiol. 2010, 76, e19–e23. [Google Scholar]
- Vano, E.; Ten, J.I.; Fernandez, J.M.; Prieto, C.; Ordiales, J.M.; Martinez, D. Quality control and patient dosimetry in digital radiology. On line system: new features and transportability. Radiat. Prot. Dosimetry 2008, 129, 144–146. [Google Scholar] [CrossRef]
- Tsalafoutas, I.A.; Metallidis, S.I. A method for calculating the dose length product from CT DICOM images. Br. J. Radiol. 2011, 84, 236–243. [Google Scholar]
- dicom.offis.de-home. Available online: http://dicom.offis.de/ (accessed on 1 November 2013 ).
- Shrimpton, P.C.; Hillier, M.C.; Lewis, M.A.; Dunn, M. National survey of doses from CT in the UK: 2003. Br. J. Radiol. 2006, 79, 968–980. [Google Scholar] [CrossRef]
- Khursheed, A.; Hillier, M.C.; Shrimpton, P.C.; Wall, B.F. Influence of patient age on normalized effective doses calculated for CT examinations. Br. J. Radiol. 2002, 75, 819–830. [Google Scholar]
- Committee to Assess Health Risks from Exposure to Low Levels of Ionizing Radiation; Board on Radiation Effects Research (BRER); Division on Earth and Life Studies (DELS); National Research Council. Health Risks from Exposure to Low Levels of Ionizing Radiation: BEIR VII-Phase 2; National Academies Press: Washington, DC, USA, 2006.
- National Cancer Center. Disease Prevention and Control Bureau. Chinese Cancer Registry Annual Reptort; Ministry of Health: Beijing, China, 2008.
- Department of Population and Employment Statistics of the National Bureau of Statistics of China. China Population & Emloyment Statistics Yearbook. China Statistics Press: Beijing, China, 2010. [Google Scholar]
- Li, X.; Niu, H.; Su, Q.; Ma, W. Estimation of baseline lifetime risk of developed cancer related to radiation exposure in China. (in Chinese). Chin. J. Radiol. Med. Protect. 2011, 31, 695–697. [Google Scholar]
- Verdun, F.R.; Gutierrez, D.; Vader, J.P.; Aroua, A.; Alamo-Maestre, L.T.; Bochud, F.; Gudinchet, F. CT radiation dose in children: A survey to establish age-based diagnostic reference levels in Switzerland. Eur. Radiol. 2008, 18, 1980–1986. [Google Scholar] [CrossRef]
- Journy, N.; Ancelet, S.; Rehel, J.-L.; Mezzarobba, M.; Aubert, B.; Laurier, D.; Bernier, M.-O. Predicted cancer risks induced by computed tomography examinations during childhood, by a quantitative risk assessment approach. Radiat. Environ. Biophys. 2013, 53, 39–54. [Google Scholar]
- Tzedakis, A.; Damilakis, J.; Perisinakis, K.; Stratakis, J.; Gourtsoyiannis, N. The effect of z overscanning on patient effective dose from multidetector helical computed tomography examinations. Med. Phys. 2005, 32, 1621–1629. [Google Scholar] [CrossRef]
- Managing Patient Dose in Computed Tomography. Available online: http://www.icrp.org/publication.asp?id=ICRP%20Publication%2087 (accessed on 4 March 2014).
- Shah, N.B.; Platt, S.L. ALARA: Is there a cause for alarm? Reducing radiation risks from computed tomography scanning in children. Current Opin. Pediatr. 2008, 20, 243–247. [Google Scholar] [CrossRef]
- Ron, E.; Lubin, J.H.; Shore, R.E.; Mabuchi, K.; Modan, B.; Pottern, L.M.; Schneider, A.B.; Tucher, M.A.; Boice, J.D. Thyroid cancer after exposure to external radiation: A pooled analysis of seven studies. Radiat. Res. 1995, 141, 259–277. [Google Scholar] [CrossRef]
- Report of the NCI-CDC Working Group to Revise the 1985 NIH Radioepidemiological Tables. Available online: http://dceg.cancer.gov/files/NIH_No_03-5387.pdf (accessed on 4 March 2014).
- 1990 Recommendations of the International Commission on Radiological Protection. Available online: http://www.icrp.org/publication.asp?id=ICRP%20Publication%2060 (accessed on 4 March 2014).
© 2014 by the authors; licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution license (http://creativecommons.org/licenses/by/3.0/).
Share and Cite
Su, Y.-P.; Niu, H.-W.; Chen, J.-B.; Fu, Y.-H.; Xiao, G.-B.; Sun, Q.-F. Radiation Dose in the Thyroid and the Thyroid Cancer Risk Attributable to CT Scans for Pediatric Patients in One General Hospital of China. Int. J. Environ. Res. Public Health 2014, 11, 2793-2803. https://doi.org/10.3390/ijerph110302793
Su Y-P, Niu H-W, Chen J-B, Fu Y-H, Xiao G-B, Sun Q-F. Radiation Dose in the Thyroid and the Thyroid Cancer Risk Attributable to CT Scans for Pediatric Patients in One General Hospital of China. International Journal of Environmental Research and Public Health. 2014; 11(3):2793-2803. https://doi.org/10.3390/ijerph110302793
Chicago/Turabian StyleSu, Yin-Ping, Hao-Wei Niu, Jun-Bo Chen, Ying-Hua Fu, Guo-Bing Xiao, and Quan-Fu Sun. 2014. "Radiation Dose in the Thyroid and the Thyroid Cancer Risk Attributable to CT Scans for Pediatric Patients in One General Hospital of China" International Journal of Environmental Research and Public Health 11, no. 3: 2793-2803. https://doi.org/10.3390/ijerph110302793
APA StyleSu, Y.-P., Niu, H.-W., Chen, J.-B., Fu, Y.-H., Xiao, G.-B., & Sun, Q.-F. (2014). Radiation Dose in the Thyroid and the Thyroid Cancer Risk Attributable to CT Scans for Pediatric Patients in One General Hospital of China. International Journal of Environmental Research and Public Health, 11(3), 2793-2803. https://doi.org/10.3390/ijerph110302793




