Monogenic Diabetes: A Diagnostic Algorithm for Clinicians
Abstract
:1. Introduction
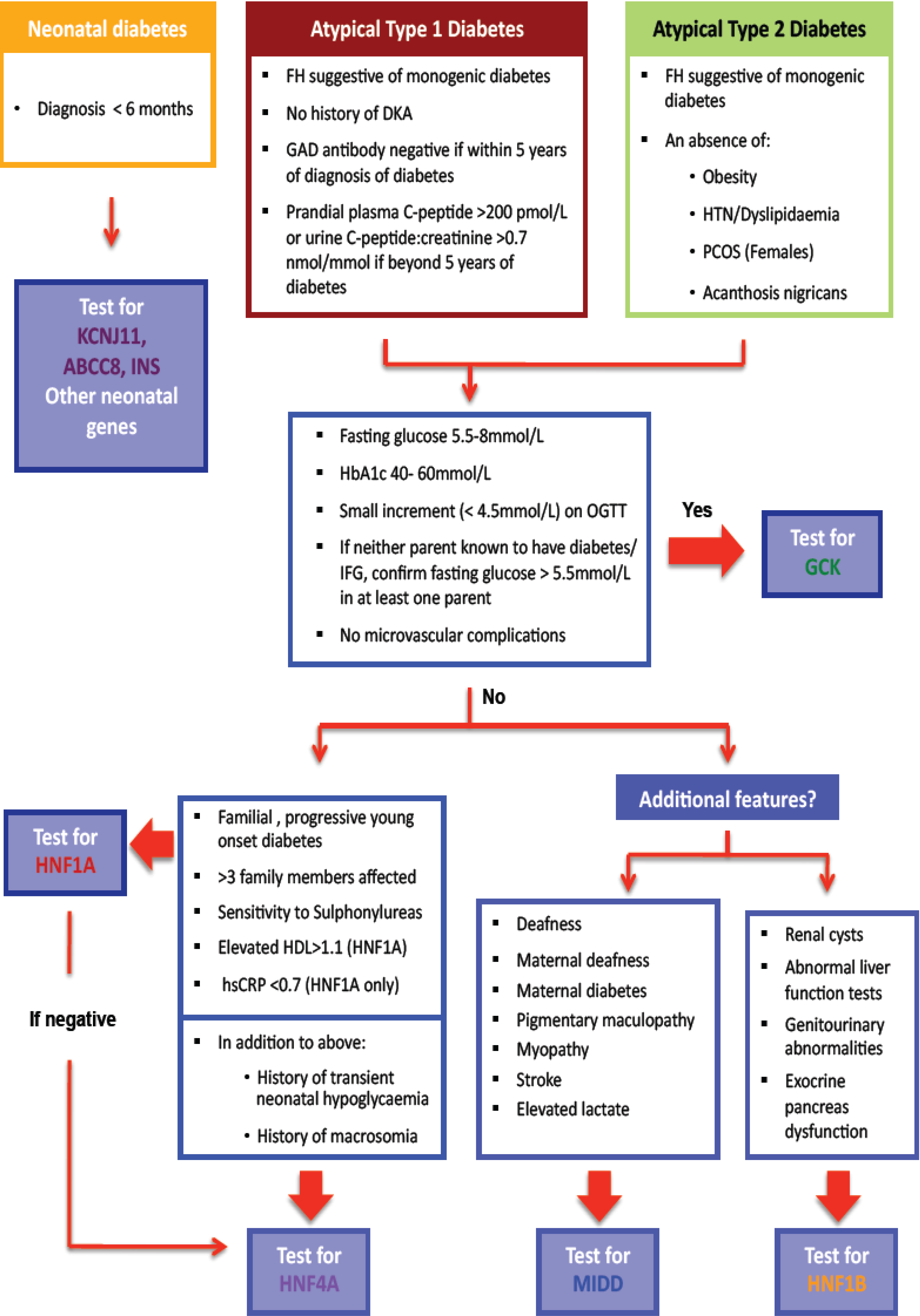
2. Overview of Monogenic Beta Cell Diabetes Associated with Recognizable Phenotypes (Table 1)
2.1. Monogenic Diabetes that Present in Infancy
| Features associated with diabetes | Type 1 diabetes | Young onset Type 2 diabetes | Monogenic diabetes | |||||
|---|---|---|---|---|---|---|---|---|
| GCK ∗ | HNF1A # | HNF4A # | HNF1B # | Neonatal diabetes | MIDD ≠ | |||
| DKA | Yes | No | No | No ∞ | No ∞ | No | Yes | Yes/No |
| Parent affected | 2%–4% | Yes | Yes ≈ | Yes | Yes | Yes | variable | Mother |
| Age of onset | 6 months to adulthood | Adolescence and young adulthood | Birth | Teens to young adulthood | Teens to young adulthood | Teens to young adulthood | <6 months | Young adulthood |
| Obesity | Population frequency | Increased frequency | Population frequency | Population frequency | Population frequency | Population frequency | Population frequency | Rare |
| Glycaemic pattern | Acute General hyperglycaemia | Progressive hyperglycemia | Stable, mild fasting glycaemia | Post-prandial hyperglycaemia initially, progressing to general hyperglycemia | Post-prandial hyperglycaemia initially, progressing to general hyperglycemia | Post-prandial hyperglycaemia initially Progressing to general hyperglycemia | Acute General hyperglycaemia | Variable dysglycaemic pattern either acute or slowly progressive |
| β cell antibodies ± | Yes | No | No | No | No | No | No | No |
| C-peptide ¥ | Very low/Absent (>5 years) | Raised/Normal | Normal | Low but Detectable | Low but Detectable | Low but Detectable | Absent but detectable once treated with SU | Low but detectable |
| hsCRP | Normal | High/High normal | Normal | Very low | Normal | Normal | Normal | Normal |
| Additional clinical features | Other autoimmune disease (Thyroid, coeliac etc.) | Dyslipidaemia, PCOS, Hypertension, Acanthosis Nigricans | Absence of microvascular and macrovascular complications | Low renal threshold for glucose in early stages of diabetes | Macrosomia and transient neonatal hypoglycaemia | High renal involvement e.g., cysts etc. | Transient in 50% of cases, although may relapse | Deafness, short stature, macular dystrophy |
2.2. Monogenic Diabetes Detected in Adolescence or Adulthood
2.2.1. Glucokinase Monogenic Diabetes
2.2.2. Hepatocyte Nuclear Factor (HNF) Monogenic Diabetes
2.2.3. Maternally Inherited Diabetes and Deafness
2.3. Monogenic Diabetes due to Rare Etiologies
3. Diagnosing Monogenic Diabetes Is Cost Effective
3.1. Neonatal Diabetes
3.2. GCK, HNF1A and HNF4A
4. Design of an Algorithm for the Diagnosis of Suspected Monogenic Diabetes
4.1. The Importance of Atypical Features
4.2. Selecting the Most Likely Gene(s) for Testing
4.3. The Use of Additional Biochemical Tests May Aid in Diagnosis (See Table 1)
4.3.1. C-Peptide
4.3.2. Islet Cell Autoantibodies
4.3.3. Highly Sensitive CRP
4.3.4. High-Density Lipoprotein (HDL)
5. Cascade Genetic Testing of Family Members
6. Conclusions
Acknowledgments
Conflicts of Interest
References
- Murphy, R.; Ellard, S.; Hattersley, A. Clinical implications of a molecular genetic classification of monogenic β-cell diabetes. Nat. Clin. Pract. Endoc. 2008, 4, 200–213. [Google Scholar] [CrossRef]
- Shields, B.M.; Hicks, S.; Shepherd, M.H.; Colclough, K.; Hattersley, A.T.; Ellard, S. Maturity-onset diabetes of the young (MODY): How many cases are we missing? Diabetologia 2010, 53, 2504–2508. [Google Scholar] [CrossRef]
- Hattersley, A.T.; Bruining, J.; Shield, J.; Njolstad, P.; Donaghue, K.C. The diagnosis and management of monogenic diabetes in children and adolescents. Pediatr. Diabetes 2009, 10, 33–42. [Google Scholar]
- American Diabetes Association. Diagnosis and classification of diabetes mellitus. Diabetes Care 2012, 35, S64–S71. [CrossRef]
- Ellard, S.; Bellanne-Chantelot, C.; Hattersley, A.T. Best practice guidelines for the molecular genetic diagnosis of maturity-onset diabetes of the young. Diabetologia 2008, 51, 546–553. [Google Scholar] [CrossRef]
- Vaxillaire, M.; Bonnefond, A.; Froguel, P. The lessons of early-onset monogenic diabetes for the understanding of diabetes pathogenesis. Clin. Pract. Endocrinol. Metab. 2012, 26, 171–187. [Google Scholar]
- Temple, I.K.; Gardner, R.J.; Mackay, D.J.G.; Barber, J.C.K.; Robinson, D.O.; Shield, J.P.H. Transient neonatal diabetes: Widening the understanding of the etiopathogenesis of diabetes. Diabetes 2000, 49, 1359–1366. [Google Scholar] [CrossRef]
- Slingerland, A.S.; Shields, B.M.; Flanagan, S.E.; Bruining, G.J.; Noordam, K.; Gach, A.; Mlynarski, W.; Malecki, M.T.; Hattersley, A.T.; Ellard, S. Referral rates for diagnostic testing support an incidence of permanent neonatal diabetes in three European countries of at least 1 in 260,000 live births. Diabetologia 2009, 52, 1683–1685. [Google Scholar] [CrossRef] [Green Version]
- Gloyn, A.L.; Pearson, E.R.; Antcliff, J.F.; Proks, P.; Bruining, G.J.; Slingerland, A.S.; Howard, N.; Srinivasan, S.; Silva, J.M.C.L.; Molnes, J.; et al. Activating mutations in the gene encoding the ATP-sensitive potassium-channel subunit Kir6.2 and permanent neonatal diabetes. N. Engl. J. Med. 2004, 350, 1838–1849. [Google Scholar] [CrossRef]
- Babenko, A.P.; Polak, M.; Cave, H.; Busiah, K.; Czernichow, P.; Scharfmann, R.; Bryan, J.; Aguilar-Bryan, L.; Vaxillaire, M.; Frogue, P. Activating mutations in the ABCC8 gene in neonatal diabetes mellitus. N. Engl. J. Med. 2006, 355, 456–466. [Google Scholar] [CrossRef]
- Flanagan, S.E.; Patch, A.M.; Mackay, D.J.G.; Edghill, E.L.; Gloyn, A.L.; Robinson, D.; Shield, J.P.H.; Temple, I.K.; Ellard, S.; Hattersley, A.T. Mutations in ATP-sensitive K+ channel genes cause transient neonatal diabetes and permanent diabetes in childhood or adulthood. Diabetes 2007, 56, 1930–1937. [Google Scholar] [CrossRef]
- Pearson, E.R.; Flechtner, I.; Njølstad, P.R.; Malecki, M.T.; Flanagan, S.E.; Larkin, B.; Ashcroft, F.M.; Klimes, I.; Codner, E.; Iotova, V.; et al. Switching from insulin to oral sulfonylureas in patients with diabetes due to Kir6.2 mutations. N. Engl. J. Med. 2006, 355, 467–477. [Google Scholar] [CrossRef]
- Hattersley, A.T.; Ashcroſt, F.M. Activating mutations in Kir6.2 and neonatal diabetes: New clinical syndromes, new scientific insights, and new therapy. Diabetes 2005, 54, 2503–2513. [Google Scholar] [CrossRef]
- Slingerland, A.S.; Hurkx, W.; Noordamet, K.; Flanagan, S.E.; Jukema, J.W.; Meiners, L.C.; Bruining, G.J.; Hattersley, A.T.; Hadders-Algra, M. Sulphonylurea therapy improves cognition in a patient with theV59M KCNJ11 mutation. Diabetic Med. 2008, 25, 277–281. [Google Scholar] [CrossRef]
- Slingerland, A.S.; Nuboer, R.; Hadders-Algra, M.; Hattersley, A.T.; Bruining, G.J. Improved motor development and good long-term glycaemic control with sulfonylurea treatment in apatient with the syndrome of intermediate developmental delay, early-onset generalised epilepsy and neonatal diabetes associated with the V59M mutation in the KCNJ11 gene. Diabetologia 2006, 49, 2559–2563. [Google Scholar] [CrossRef]
- Boesgaard, T.R.; Pruhova, S.; Andersson, E.A.; Cinek, O.; Obermannova, B.; Lauenborg, J.; Damm, P.; Bergholdt, R.; Pociot, F.; Pisinger, C.; et al. Further evidence that mutations in INS can be a rare cause of Maturity-Onset Diabetes of the Young (MODY). BMC Med. Genet. 2010. [Google Scholar] [CrossRef] [Green Version]
- Molven, A.; Ringdal, M.; Nordbø, A.M.; Ræder, H.; Støy, J.; Lipkind, G.M.; Steiner, D.F.; Philipson, L.H.; Bergmann, I.; Aarskog, D.; et al. Mutations in the insulin gene can cause MODY and autoantibody-negative type 1 diabetes. Diabetes 2008, 57, 1131–1135. [Google Scholar] [CrossRef]
- Ashcroft, F.M.; Rorsman, P. Diabetes mellitus and the β cell: The last ten years. Cell 2012, 148, 1160–1171. [Google Scholar] [CrossRef]
- Matschinsky, F.M.; Randle, P.J. Evolution of the glucokinase glucose sensor paradigm for pancreatic beta cells. Diabetologia 1993, 36, 1215–1217. [Google Scholar] [CrossRef]
- Stride, A.; Vaxillaire, M.; Tuomi, T.; Barbetti, F.; Njølstad, P.R.; Hansen, T.; Costa, A.; Conget, I.; Pedersen, O.; Søvik, O.; et al. The genetic abnormality in the beta cell determines the response to an oral glucose load. Diabetologia 2002, 45, 427–435. [Google Scholar] [CrossRef]
- Velho, G.; Blanche, H.; Vaxillaire, M.; Bellanne-Chantelot, C.; Pardini, V.C.; Timsit, J.; Passa, Ph.; Deschamp, I.; Robert, J.-J.; Weber, I.T.; et al. Identification of 14 new glucokinase mutations and description of the clinical profile of 42 MODY-2 families. Diabetologia 1997, 40, 217–224. [Google Scholar] [CrossRef]
- Steele, A.M.; Wensley, K.J.; Ellard, E.; Murphy, R.; Shepherd, M.; Colclough, K.; Shields, B.M.; Hattersley, A.T. Use of HbA1c in the identification of patients with hyperglycaemia caused by a glucokinase mutation: Observational case control studies. PLoS One 2013, 8, e65326. [Google Scholar] [CrossRef]
- Njølstad, P.R.; Søvik, O.; Cuesta-Munoz, A.; Bjørkhaug, L.; Massa, O.; Barbetti, F.; Undlien, D.E.; Shiota, C.; Magnuson, M.A.; Molven, A.; et al. Neonatal diabetes mellitus due to complete glucokinase deficiency. N. Engl. J. Med. 2001, 344, 1588–1592. [Google Scholar] [CrossRef]
- Njølstad, P.R.; Sagen, J.V.; Bjørkhaug, L.; Odili, S.; Shehadeh, N.; Bakry, D.; Sarici, S.M.; Alpay, F.; Molnes, J.; Molven, A.; et al. Matschinsky. Permanent neonatal diabetes caused by glucokinase deficiency: Inborn error of the glucose-insulin signaling pathway. Diabetes 2003, 52, 2854–2860. [Google Scholar] [CrossRef]
- Murphy, R.; Tura, A.; Clark, P.M.; Holst, J.J.; Mari, A.; Hattersley, A.T. Glucokinase, the pancreatic glucose sensor, is not the gut glucose sensor. Diabetologia 2009, 52, 154–159. [Google Scholar] [CrossRef]
- Martin, D.; Bellanne-Chantelot, C.; Deschamps, I.; Froguel, P.; Robert, J.J.; Velho, G. Long-term follow-up of oral glucose tolerance test-derived glucose tolerance and insulin secretion and insulin sensitivity indexes in subjects with glucokinase mutations (MODY2). Diabetes Care 2008, 31, 1321–1323. [Google Scholar] [CrossRef]
- Colomand, C.; Corcoy, R. Maturity onset diabetes of the young and pregnancy. Best Pract. Res. Clin. Endocrinol.Metab. 2010, 24, 605–615. [Google Scholar] [CrossRef]
- Ellard, S.; Beards, F.; Allen, L.I.S.; Shepherd, M.; Ballantyne, E.; Harvey, R.; Hattersley, A.T. A high prevalence of glucokinase mutations in gestational diabetic subjects selected by clinical criteria. Diabetologia 2000, 43, 250–253. [Google Scholar]
- Spyer, G.; Hattersley, A.T.; Sykes, J.E.; Sturley, R.H.; MacLeod, K.M. Influence of maternal and fetal glucokinase mutations in gestational diabetes. Am. J. Obstet. Gynecol. 2001, 185, 240–241. [Google Scholar] [CrossRef]
- Chakera, A.J.; Carleton, V.L.; Ellard, S.; Wong, J.; Yue, D.K.; Pinner, J.; Hattersley, A.T.; Ross, G.P. Antenatal diagnosis of fetal genotype determines if maternal hyperglycaemia due to a glucokinase mutation requires treatment. Diabetes Care 2012, 35, 1832–1834. [Google Scholar] [CrossRef]
- Maestro, M.A.; Cardalda, C.; Boj, S.F.; Luco, R.F.; Servitja, J.M.; Ferrer, J. Distinct roles of HNF1beta, HNF1alpha, and HNF4alpha in regulating pancreas development, beta-cell function and growth. Endocr. Dev. 2007, 12, 33–45. [Google Scholar]
- Fajans, S.S.; Bell, G.I.; Polonsky, K.S. Molecular mechanisms and clinical pathophysiology of maturity-onset diabetes of the young. N. Eng. J. Med. 2001, 345, 971–980. [Google Scholar] [CrossRef]
- Stride, A.; Ellard, S.; Clark, P.; Shakespeare, L.; Salzmann, M.; Shepherd, M.; Hattersley, A.T. β-cell dysfunction, insulin sensitivity, and glycosuria precede diabetes in hepatocyte nuclear factor-1α mutation carriers. Diabetes Care 2005, 28, 1751–1756. [Google Scholar]
- Kapoor, R.R.; Locke, J.; Colclough, K.; Wales, J.; Conn, J.J.; Hattersley, A.T.; Ellard, S.; Hussain, K. Persistent hyperinsulinemic hypoglycaemia and maturity-onset diabetes of the young due to heterozygous HNF4A mutations. Diabetes 2008, 57, 1659–1663. [Google Scholar] [CrossRef]
- Isomaa, B.; Henricsson, M.; Lehto, M.; Forsblom, C.; Karanko, S.; Sarelin, L.; Häggblom, M.; Groop, L. Chronic diabetic complications in patients with MODY3 diabetes. Diabetologia 1998, 41, 467–473. [Google Scholar] [CrossRef]
- Edghill, E.L.; Bingham, C.; Ellard, S.; Hattersley, A.T. Mutations in hepatocyte nuclear factor-1β and their related phenotypes. J. Med. Genet. 2006, 43, 84–90. [Google Scholar]
- Shepherd, M.; Shields, B.; Ellard, S.; Rubio-Cabezas, O.; Hattersley, A.T. A genetic diagnosis of HNF1A diabetes alters treatment and improves glycaemic control in the majority of insulin-treated patients. Diabet. Med. 2009, 26, 437–441. [Google Scholar] [CrossRef]
- Shepherd, M.; Pearson, E.R.; Houghton, J.; Salt, G.; Ellard, S.; Hattersley, A.T. No deterioration in glycemic control in HNF-1alpha maturity-onset diabetes of the young following transfer from long-term insulin to sulphonylureas. Diabetes Care. 2003, 26, 3191–3192. [Google Scholar] [CrossRef]
- Murphy, R.; Turnbull, D.M.; Walker, M.; Hattersley, A.T. Clinical features, diagnosis and management of maternally inherited diabetes and deafness (MIDD) associated with the 3243A>G mitochondrial point mutation. Diabet. Med. 2008, 25, 383–399. [Google Scholar]
- Maassen, J.A.; Janssen, G.M.C.; 'tHart, L.M. Molecular mechanisms of mitochondrial diabetes (MIDD). Ann. Med. 2005, 37, 213–221. [Google Scholar] [CrossRef]
- Guillausseau, P.-J.; Massin, P.; Dubois-LaForgue, D.; Timsit, J.; Virally, M.; Gin, H.; Bertin, E.; Blickle, J.-F.; Bouhanick, B.; Cahen, J.; et al. Maternally inherited diabetes and deafness: A multicenter study. Ann. Intern. Med. 2001, 134, 721–728. [Google Scholar] [CrossRef]
- Dykens, J.A.; Jamieson, J.; Marroquin, L.; Nadanaciva, S.; Billis, P.A.; Will, Y. Biguanide-induced mitochondrial dysfunction yields increased lactate production and cytotoxicity of aerobically-poised HepG2 cells and human heptaocytes in vitro. Toxicol. Appl. Pharmacol. 2008, 233, 203–210. [Google Scholar] [CrossRef]
- Suzuki, S.; Hinokio, Y.; Ohtomo, M.; Hirai, M.; Hirai, A.; Chiba, M.; Kasuga, S.; Satoh, Y.; Akai, H.; Toyota, T. The effects of coenzyme Q10 treatment on maternally inherited diabetes mellitus and deafness, and mitochondrial DNA 3243 (A to G) mutation. Diabetologia 1998, 41, 584–588. [Google Scholar] [CrossRef]
- Bowman, P.; Flanagan, S.E.; Edghill, E.L.; Damhuis, A.; Shepherd, M.H.; Paisey, R.; Hattersley, A.T.; Ellard, S. Heterozygous ABCC8 mutations are a cause of MODY. Diabetologia 2012, 55, 123–127. [Google Scholar] [CrossRef]
- Greeley, S.A.W.; John, P.R.; Winn, A.N.; Ornelas, J.; Lipton, R.B.; Philipson, L.H.; Bell, G.I.; Huang, E.S. The cost-effectiveness of personalized genetic medicine: The case of genetic testing in neonatal diabetes. Diabetes Care 2011, 34, 622–627. [Google Scholar] [CrossRef]
- Naylor, R.N.; John, P.R.; Winn, A.N.; Philipson, L.H.; Greeley, S.A.W.; Bell, G.I.; Huang, E.S. The Cost-Effectiveness of MODY Genetic Testing. Diabetes 2012, 61, A36. [Google Scholar] [CrossRef]
- Verge, C.F.; Howard, N.J.; Rowley, M.J.; Mackay, I.R.; Zimmet, P.Z.; Egan, M.; Hulinska, H.; Hulinsky, I.; Silvestrini, R.A.; Kamath, S.; et al. Anti-glutamate decarboxylase and other antibodies at the onset of childhood IDDM: A population-based study. Diabetologia 1994, 37, 1113–1120. [Google Scholar] [CrossRef]
- Schober, E.; Rami, B.; Grabert, M.; Thon, A.; Kapellen, T.; Reinehr, T.; Holl, R.W. Phenotypical aspects of maturity-onset diabetes of the young (MODY diabetes) in comparison with Type 2 diabetes mellitus (T2DM) in children and adolescents: Experience from a large multicentre database. Diabet. Med. 2009, 26, 466–473. [Google Scholar] [CrossRef]
- Shields, B.M.; McDonald, T.J.; Ellard, S.; Campbell, M.J.; Hyde, C.; Hattersley, A.T. The development and validation of a clinical prediction model to determine the probability of MODY in patients with young-onset diabetes. Diabetologia 2012, 55, 1265–1272. [Google Scholar] [CrossRef]
- Wang, L.; Lovejoy, N.F.; Faustman, D.L. Persistence of prolonged C-peptide production in type 1 diabetes as measured with an ultrasensitive C-peptide assay. Diabetes Care 2012, 35, 465–470. [Google Scholar] [CrossRef]
- Besser, R.E.; Shields, B.M.; Hammersley, S.E.; Colclough, K.; McDonald, T.J.; Gray, Z.; Heywood, J.J.; Barrett, T.G.; Hattersley, A.T. Home urine C-peptide creatinine ratio (UCPCR) testing can identify type 2 and MODY in pediatric diabetes. Pediatr. Diabetes 2013, 14, 181–188. [Google Scholar]
- Wenzlau, J.M.; Juhl, K.; Yu, L.; Moua, O.; Sarkar, S.A.; Gottlieb, P.; Rewers, M.; Eisenbarth, G.S.; Jansen, J.; Davidson, H.W.; et al. The cation efflux transporter ZnT8 (Slc30A8) is a major autoantigen in human type 1 diabetes. Proc. Natl. Acad. Sci. USA 2008, 104, 17040–17045. [Google Scholar]
- McDonald, T.J.; Colclough, K.; Brown, R.; Shields, B.; Shepherd, M.; Bingley, P.; Williams, A.; Hattersley, A.T.; Ellard, S. Islet autoantibodies can discriminate maturity‐onset diabetes of the young (MODY) from Type 1 diabetes. Diabet. Med. 2011, 28, 1028–1033. [Google Scholar] [CrossRef]
- Owen, K.R.; Thanabalasingham, G.; James, T.J.; Karpe, F.; Farmer, A.J.; McCarthy, M.I.; Gloyn, A.L. Assessment of high-sensitivity C-reactive protein levels as diagnostic discriminator of maturity-onset diabetes of the young due to HNF1A mutations. Diabetes Care 2010, 33, 1919–1924. [Google Scholar] [CrossRef]
- McDonald, T.J.; Shields, B.M.; Lawry, J.; Owen, K.R.; Gloyn, A.L.; Ellard, S.; Hattersley, A.T. High-sensitivity CRP discriminates HNF1A-MODY from other subtypes of diabetes. Diabetes Care 2011, 34, 1860–1862. [Google Scholar] [CrossRef]
- McDonald, T.J.; McEneny, J.; Pearson, E.R.; Thanabalasingham, G.; Szopa, M.; Shields, B.; Ellard, S.; Owen, K.R.; Malecki, M.T.; Hattersley, A.T.; et al. Lipoprotein composition in HNF1A-MODY: Differentiating between HNF1A-MODY and type 2 diabetes. Clin. Chim. Acta 2012, 413, 927–932. [Google Scholar] [CrossRef]
© 2013 by the authors; licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution license (http://creativecommons.org/licenses/by/3.0/).
Share and Cite
Carroll, R.W.; Murphy, R. Monogenic Diabetes: A Diagnostic Algorithm for Clinicians. Genes 2013, 4, 522-535. https://doi.org/10.3390/genes4040522
Carroll RW, Murphy R. Monogenic Diabetes: A Diagnostic Algorithm for Clinicians. Genes. 2013; 4(4):522-535. https://doi.org/10.3390/genes4040522
Chicago/Turabian StyleCarroll, Richard W., and Rinki Murphy. 2013. "Monogenic Diabetes: A Diagnostic Algorithm for Clinicians" Genes 4, no. 4: 522-535. https://doi.org/10.3390/genes4040522




