Metformin Lowers Serum Cobalamin without Changing Other Markers of Cobalamin Status: A Study on Women with Polycystic Ovary Syndrome
Abstract
:1. Introduction
2. Experimental Section
2.1. Participants and Study Design
2.2. Blood Sample Collection and Storage
2.3. Biochemical Measurements
2.4. Statistically Analysis
3. Results
3.1. Characteristics of the Study Population
3.2. Markers of Cobalamin Status
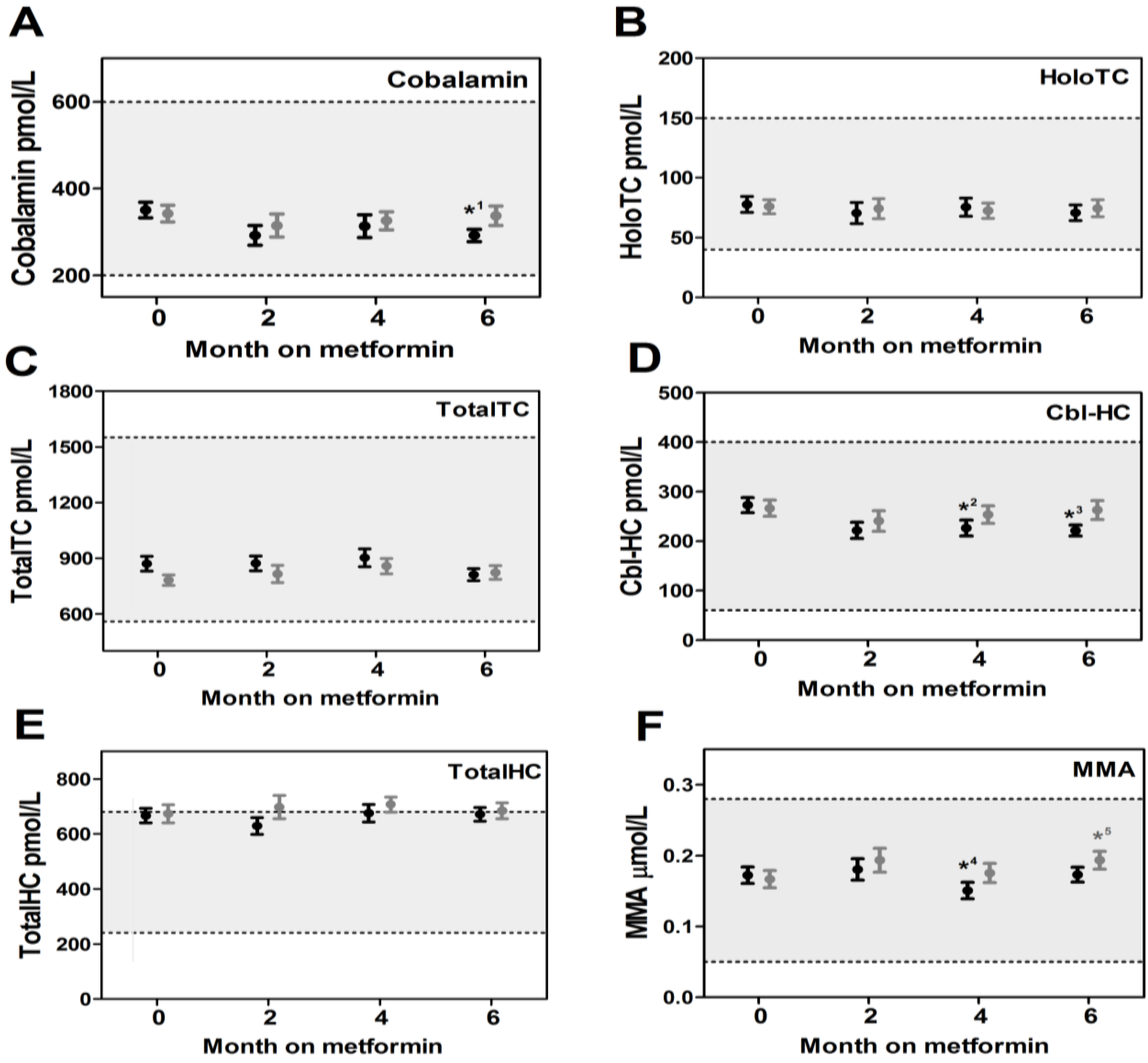
4. Discussion
5. Conclusions
Acknowledgments
Conflict of Interest
References
- Jager, J.; Kooy, A.; Lehert, P.; Wulffelé, M.G.; Kolk, J.; Bets, D.; Verburg, J.; Donker, A.J.; Stehouwer, C.D. Long term treatment with metformin in patients with type 2 diabetes and risk of vitamin B-12 deficiency: Randomized placebo controlled trial. BMJ 2010, 340, c2181. [Google Scholar] [CrossRef]
- Reinstatler, L.; Qi, Y.P.; Williamson, R.S.; Garn, J.V.; Oakley, G.P. Association of biochemical B12 deficiency with metformin therapy and vitamin B12 supplements. Diabetes Care 2012, 35, 327–333. [Google Scholar] [CrossRef]
- DeFronzo, R.A.; Goodman, A.M. Efficacy of metformin in patients with non-insulin-dependent diabetes mellitus. The Multicenter Metformin Study Group. N. Engl. J. Med. 1995, 333, 541–549. [Google Scholar] [CrossRef]
- Tomkin, G.H.; Hadden, D.R.; Weaver, J.A.; Montgomery, D.A. Vitamin-B12 status of patients on long-term metformin therapy. Br. Med. J. 1971, 2, 685–687. [Google Scholar] [CrossRef]
- Wulffele, M.G.; Kooy, A.; Lehert, P.; Bets, D.; Ogterop, J.C.; Burg, B.B.; Donker, A.J.; Stehouwer, C.D. Effects of short-term treatment with metformin on serum concentrations of homocysteine, folate and vitamin B12 in type 2 diabetes mellitus: A randomized, placebo-controlled trial. J. Intern. Med. 2003, 254, 455–463. [Google Scholar] [CrossRef]
- Bauman, W.A.; Shaw, S.; Jayatilleke, E.; Spungen, A.M.; Herbert, V. Increased intake of calcium reverses vitamin B12 malabsorption induced by metformin. Diabetes Care 2000, 23, 1227–1231. [Google Scholar] [CrossRef]
- Mazokopakis, E.E.; Starakis, I.K. Recommendations for diagnosis and management of metformin-induced vitamin B12 (Cbl) deficiency. Diabetes Res. Clin. Pract. 2012, 97, 359–367. [Google Scholar] [CrossRef]
- Lord, J.; Wilkin, T. Metformin in polycystic ovary syndrome. Curr. Opin. Obstet. Gynecol. 2004, 16, 481–486. [Google Scholar] [CrossRef]
- Carlsen, S.M.; Kjotrod, S.; Vanky, E.; Romundstad, P. Homocysteine levels are unaffected by metformin treatment in both nonpregnant and pregnant women with polycystic ovary syndrome. Acta Obstet. Gynecol. Scand. 2007, 86, 145–150. [Google Scholar] [CrossRef]
- Nielsen, M.J.; Rasmussen, M.R.; Andersen, C.B.; Nexo, E.; Moestrup, S.K. Vitamin B12 transport from food to the body’s cells—A sophisticated, multistep pathway. Nat. Rev. Gastroenterol. Hepatol. 2012, 9, 345–354. [Google Scholar] [CrossRef]
- Reynolds, E. Vitamin B12, folic acid, and the nervous system. Lancet Neurol. 2006, 5, 949–960. [Google Scholar] [CrossRef]
- Hvas, A.M.; Nexo, E. Diagnosis and treatment of vitamin B12 deficiency—An update. Haematologica 2006, 91, 1506–1512. [Google Scholar]
- Caspary, W.F.; Zavada, I.; Reimold, W.; Deuticke, U.; Emrich, D.; Willms, B. Alteration of bile acid metabolism and vitamin-B12-absorption in diabetics on biguanides. Diabetologia 1977, 13, 187–193. [Google Scholar] [CrossRef]
- Obeid, R.; Jung, J.; Falk, J.; Herrmann, W.; Geisel, J.; Friesenhahn-Ochs, B.; Lammert, F.; Fassbender, K.; Kostopoulos, P. Serum vitamin B12 not reflecting vitamin B12 status in patients with type 2 diabetes. Biochimie 2013, 95, 1056–1061. [Google Scholar] [CrossRef]
- Greibe, E.; Miller, J.W.; Foutouhi, S.H.; Green, R.; Nexo, E. Metformin increases liver accumulation of vitamin B12—An experimental study in rats. Biochimie 2013, 95, 1061–1065. [Google Scholar]
- Trolle, B.; Flyvbjerg, A.; Kesmodel, U.; Lauszus, F.F. Efficacy of metformin in obese and non-obese women with polycystic ovary syndrome: A randomized, double-blinded, placebo-controlled cross-over trial. Hum. Reprod. 2007, 22, 2967–2973. [Google Scholar] [CrossRef]
- Hustad, S.; Eussen, S.; Midttun, O.; Ulvik, A.; van de Kant, P.M.; Morkrid, L.; Gislefoss, R.; Ueland, P.M. Kinetic modeling of storage effects on biomarkers related to B vitamin status and one-carbon metabolism. Clin. Chem. 2012, 58, 402–410. [Google Scholar] [CrossRef]
- Nexo, E.; Christensen, A.L.; Petersen, T.E.; Fedosov, S.N. Measurement of transcobalamin by ELISA. Clin. Chem. 2000, 46, 1643–1649. [Google Scholar]
- Nexo, E.; Christensen, A.L.; Hvas, A.M.; Petersen, T.E.; Fedosov, S.N. Quantification of holo-transcobalamin, a marker of vitamin B12 deficiency. Clin. Chem. 2002, 48, 561–562. [Google Scholar]
- Morkbak, A.L.; Pedersen, J.F.; Nexo, E. Glycosylation independent measurement of the cobalamin binding protein haptocorrin. Clin. Chem. Acta 2005, 356, 184–190. [Google Scholar] [CrossRef]
- Lakso, H.; Appelblad, P.; Schneede, J. Quantification of Methylmalonic acid in human plasma with hydrophilic interaction liquid chromatography separation and mass spectrometric detection. Clin. Chem. 2008, 54, 2028–2029. [Google Scholar] [CrossRef]
- Nexo, E. Variation with age of reference values for P-cobalamin. Scand. J. Haematol. 1983, 30, 430–432. [Google Scholar] [CrossRef]
- Rasmussen, K.; Moller, J.; Lyngbak, M.; Pedersen, A.M.; Dybkjaer, L. Age- and gender-specific reference intervals for total homocysteine and methylmalonic acid in plasma before and after vitamin supplementation. Clin. Chem. 1996, 42, 630–636. [Google Scholar]
- Leung, S.; Mattman, A.; Snyder, F.; Kassam, R.; Meneilly, G.; Nexo, E. Metformin induced reductions in plasma cobalamin and haptocorrin bound cobalamin levels in elderly diabetic patient. Clin. Biochem. 2010, 43, 759–760. [Google Scholar] [CrossRef]
- Greibe, E.; Andreasen, B.H.; Lildballe, D.L.; Morkbak, A.L.; Hvas, A.M.; Nexo, E. Uptake of cobalamin and markers of cobalamin status: A longitudinal study of healthy pregnant women. Clin. Chem. Lab. Med. 2011, 49, 1877–1882. [Google Scholar]
Supplementary Files
© 2013 by the authors; licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution license (http://creativecommons.org/licenses/by/3.0/).
Share and Cite
Greibe, E.; Trolle, B.; Bor, M.V.; Lauszus, F.F.; Nexo, E. Metformin Lowers Serum Cobalamin without Changing Other Markers of Cobalamin Status: A Study on Women with Polycystic Ovary Syndrome. Nutrients 2013, 5, 2475-2482. https://doi.org/10.3390/nu5072475
Greibe E, Trolle B, Bor MV, Lauszus FF, Nexo E. Metformin Lowers Serum Cobalamin without Changing Other Markers of Cobalamin Status: A Study on Women with Polycystic Ovary Syndrome. Nutrients. 2013; 5(7):2475-2482. https://doi.org/10.3390/nu5072475
Chicago/Turabian StyleGreibe, Eva, Birgitta Trolle, Mustafa V. Bor, Finn F. Lauszus, and Ebba Nexo. 2013. "Metformin Lowers Serum Cobalamin without Changing Other Markers of Cobalamin Status: A Study on Women with Polycystic Ovary Syndrome" Nutrients 5, no. 7: 2475-2482. https://doi.org/10.3390/nu5072475




