Diabetes Prevention in the New York City Sikh Asian Indian Community: A Pilot Study
Abstract
:1. Introduction
2. Methods
2.1. Framework
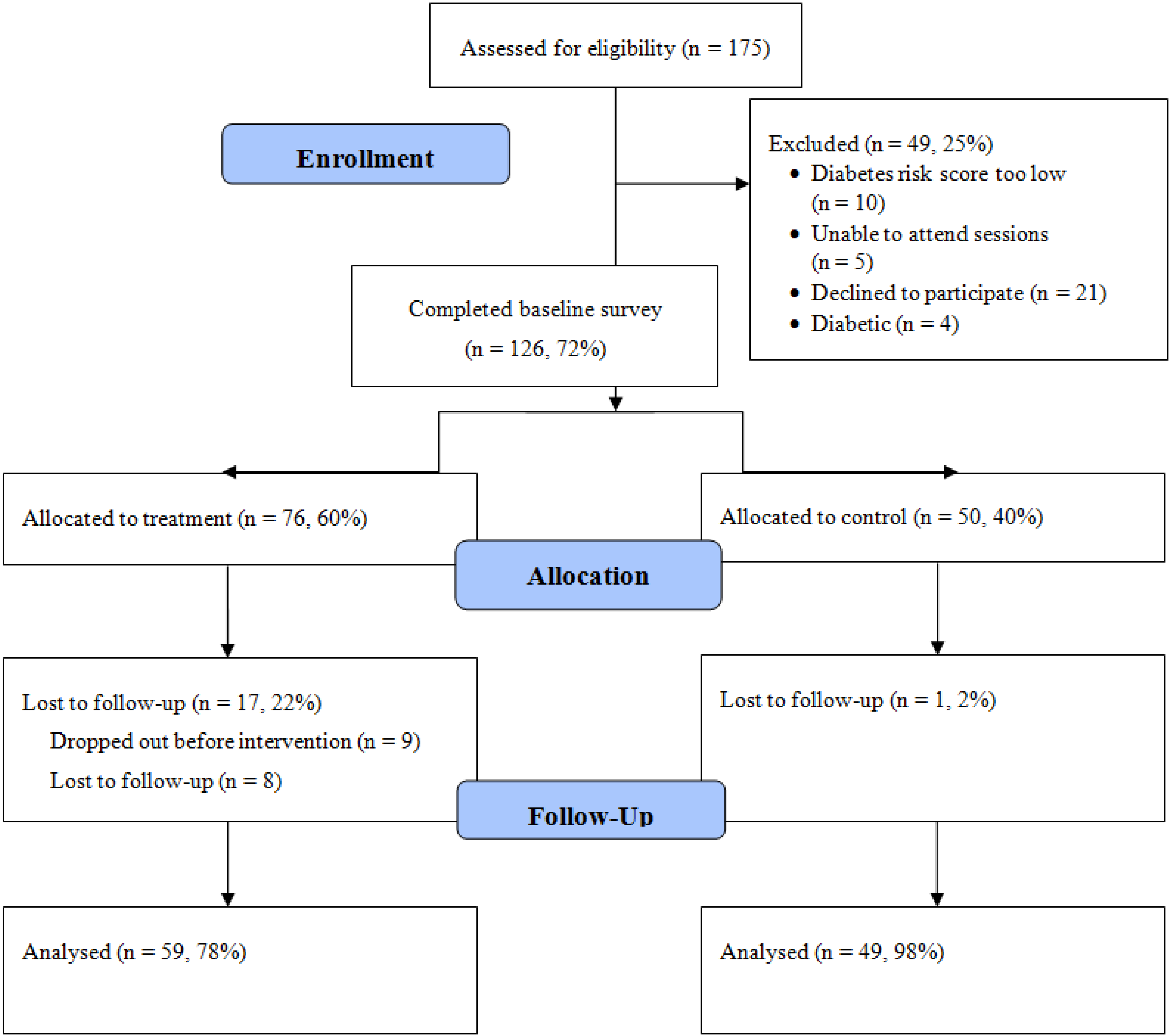
2.2. Recruitment and Study Design
| Stage of Research Process | Engagement of Community Partners/Representatives |
|---|---|
| Project Initiation | Academic agency conducted a health needs assessment survey in collaboration with South Asian community organizations in 2007 which highlighted high burden of diabetes in this population. |
| Prior to grant submission, academic agency worked with largest Sikh social service agency in New York City to develop a diabetes prevention protocol. | |
| Grant submission was developed collaboratively and awarded. | |
| Memorandums of Understanding were developed jointly by academic and community partner outlining roles and responsibilities on the project. Grant funds are distributed across both community and academic partners. | |
| CBO selected key community partners (community leaders, religious leaders, health providers, media) to participate in coalition; Academic agency identified health professionals with expertise on topic areas relevant to the intervention. | |
| Study Design | CHWs hired by the CBO were based at CBO site to build capacity within the organization and ensure acceptance by the community. |
| Coalition tailored existing curricula and developed evaluation tools for use in the Sikh community, with particular importance placed upon cultural relevancy of concepts and examples, and linguistic concordance. | |
| Screening tool adapted to include Asian BMI categories based on input from community health providers. | |
| Community partner input into study design facilitated adapting the DPP for the Sikh community (e.g., reduction of the total number of sessions, translation of study materials). | |
| Due to concerns regarding the close-knit nature of the community within neighborhoods and negative community perceptions regarding randomization at the individual level, partners recommended that the treatment and control groups should be allocated by neighborhood. | |
| Study Implementations | CHWs recruited participants at partner gurdwara sites as well as other community locations; collaborative meetings were held with key gurdwara leaders to ensure support and ownership for the project. |
| Intervention was delivered by trained CHWs who were members of the communityData was collected by trained CHWs who were members of the community. | |
| Analysis & Interpretation | Outcomes, challenges, and lessons learned were assessed and reviewed by the coalition in a continuous process through weekly calls and monthly meetings to adapt and refine the intervention and ensure continued cultural and linguistic relevancy. |
| CBO partners and community representatives consulted to interpret data findings. | |
| Dissemination of Findings | Held community forums and presented project findings in “lay language”. |
| Dissemination of study findings to ethnic media. | |
| CHW Supervisor served as co-presenter at multiple public health conferences; CBO staff serve as co-authors on project publications. | |
| Sustainability | Ongoing efforts to sustain funding for diabetes- and health promotion-related education and services so that project activities can continue beyond existing grant. |
| New health priority areas identified by CBO based on formative research conducted for this project; funding sought and secured by CBO. |
2.3. Intervention
| Project RICE Curriculum Session Title & Content | Corresponding DPP/PTP Session | Tailored Cultural Components |
|---|---|---|
| Diabetes prevention: Diabetes information; Prevention of diabetes; Myths and Facts about diabetes; Goal-setting. | Welcome to the Lifestyle Balance Program Diabetes Overview: Part 1 | Concept of prevention tied to Sikh core values, e.g., discussion of the concept of “Saint-Soldier” in Sikhism, which promotes discipline in spiritual practice as well as in social responsibilities |
| Discussion of diabetes prevalence and increased risk of diabetes in Asians | ||
| Discussion of diabetes among Sikh Asian Indians | ||
| Explanation of BMI and at-risk BMI in Asian communities | ||
| Dispelling common cultural misconceptions regarding diabetes (e.g., getting diabetes is a natural part of aging)Incorporation of culturally appropriate images and language | ||
| Nutrition: Nutrition and Food; Eating a balanced diet; The Plate Method; Overcoming barriers to eating out/social situations; Reading a Nutrition Label; Goal-setting for healthy eating. | Be a Fat Detective Three Ways to Eat Less Fat Healthy Eating Take Charge of What’s Around You Problem Solving Four Keys to Healthy Eating Out Make Social Cues Work For You Portion Size | Photos of typical Punjabi/North Indian foods |
| Healthy elements in traditional Indian cooking (e.g., whole grain options for rotis, incorporating fruits and vegetables) | ||
| Identifying and limiting deep-fried snacks high in salt and sweets high in fat and sugar; substituting sweets with fruits | ||
| Healthy vegetarian options | ||
| Healthy versions of popular Indian recipes | ||
| Following the Plate Method with traditional Punjabi foods | ||
| Managing expectations for eating langar at gurdwara | ||
| Reading food labels | ||
| Working with women participants to improve nutrition in the entire household | ||
| Incorporation of culturally appropriate images and language | ||
| Physical activity: Caloric intake and energy balance; Benefits and types of exercise; Injury prevention; Incorporating routines; Overcoming barriers; Practice activity and goal-setting. | Getting Started Being Active Move Those Muscles Take Charge of What’s Around You Tip the Calorie Balance Problem Solving Jump Start Your Activity Plan Make Social Cues Work for You | Discussion of physical activity as essential to physical and mental fitness (e.g., encouragement to practice similar discipline in physical activity as in prayer) |
| Home-based exercise/activities | ||
| Practice Activity | ||
| Incorporation of culturally appropriate images and language | ||
| Diabetes complications and other cardiovascular diseases: Diabetes complications; Heart disease and stroke; Staying motivated and goal-setting. | Diabetes Overview: Part 2 Problem Solving Ways to Stay Motivated | Discussion of diabetes complications, heart disease, stroke |
| Discussion of prevention and inter-connectedness of chronic diseases | ||
| Discussion of cholesterol and fats in diet, blood pressure and salt in diet | ||
| Review of popular Punjabi foods high in salt and fat and limiting these foods | ||
| Incorporation of culturally appropriate images/language | ||
| Stress and family support: Effects of stress on health; Stress and anger management; Strategies to manage depression; Family support and goal-setting. | Talk Back to Negative Thoughts The Slippery Slope of Lifestyle Change You Can Manage Stress Problem Solving Ways to Stay Motivated Get Your Family and Friends Involved | Discussion of Naam Simran, a meditation practice in Sikhism |
| Progressive muscle relaxation for stress relief | ||
| Strategies to manage depression; discussion around stigma associated with mental health (e.g., depression) | ||
| Incorporation of culturally appropriate images and language | ||
| Access to healthcare: Communicating with the doctor; Preparing for a doctor’s visit; Accessing health services. | Partner with Your Health Care Provider Ways to Stay Motivated | Preparing for a doctor’s visit |
| Communicating with the doctor | ||
| Patient bill of rights and language access laws | ||
| Review of NYC Health and Hospitals Corporation Options Program and the Affordable Care Act | ||
| Health access resources and providers who speak Punjabi | ||
| Incorporation of culturally appropriate images and language |
2.4. Data Collection and Measures
2.4.1. Quantitative Data Collection
2.4.2. Qualitative Data Collection
2.5. Data Analysis
2.5.1. Quantitative Data Analysis
2.5.2. Qualitative Data Analysis
3. Results and Discussion
3.1. Quantitative Results
3.1.1. Feasibility
3.1.2. Efficacy
| Characteristics | Treatment Group | Control Group | p-value |
|---|---|---|---|
| Demographics | |||
| Age (years), mean (SD) | 46.3 (11.6) | 47.8 (9.5) | 0.40 |
| Female | 73 (96.1) | 29 (58.0) | <0.01 |
| Born outside the U.S. | 76 (100.0) | 50 (100.0) | 1.00 |
| Years lived in U.S., mean (SD) | 10.5 (6.9) | 14.9 (6.8) | <0.01 |
| Married | 71 (93.4) | 47 (97.9) | 0.26 |
| Education | <0.01 | ||
| <High school | 12 (16.2) | 4 (8.2) | |
| High school/some college | 43 (58.1) | 42 (85.7) | |
| College graduate | 19 (25.7) | 3 (6.1) | |
| Speaks English not well or not at all | 28 (37.8) | 26 (52.0) | 0.12 |
| Health insurance | 0.03 | ||
| Uninsured | 9 (13.0) | 14 (31.1) | |
| Public/hospital card | 50 (72.5) | 29 (64.4) | |
| Private | 10 (14.5) | 2 (4.0) | |
| Fair or poor self-reported health | 13 (17.6) | 24 (50.0) | <0.01 |
| Clinical variables | |||
| Weight (lbs), mean (SD) | 162.4 (26.6) | 174.9 (23.0) | <0.01 |
| BMI (kg/m2), mean (SD) | 28.2 (4.0) | 28.6 (3.0) | 0.57 |
| Overweight (23–27.49) | 30 (39.5) | 16 (32.0) | |
| Obese (≥27.50) | 41 (53.9) | 32 (64.0) | |
| Glucose (mg/dL), mean (SD) | 112.3 (34.0) | 110.7 (21.6) | 0.78 |
| Cholesterol (mg/dL), mean (SD) | 152.1 (37.9) | 138.9 (33.9) | 0.07 |
| Systolic BP (mmHg), mean (SD) | 129.8 (15.9) | 128.7 (16.7) | 0.73 |
| Diastolic BP (mmHg), mean (SD) | 83.9 (9.0) | 85.6 (10.8) | 0.35 |
| Hypertensive | 22 (30.6) | 17 (34.0) | |
| Pre-hypertensive | 37 (51.4) | 23 (46.0) |
| Outcome Measures | Treatment (T) Group n = 54 | Control (C) Group n = 48 | |||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|
| n | Mean BL | Mean 3 M | Mean 6 M | p-value (BL–6 M) | n | Mean BL | Mean 3 M | Mean 6 M | p-value (BL–6 M) | T vs. C p-value | |
| Clinical variables | |||||||||||
| Weight, lbs | 54 | 160.2 (27.7) | 157.5 (26.6) | 155.4 (25.4) | <0.01 | 48 | 174.8 (23.2) | 169.1 (22.8) | 173.7 (19.3) | 0.53 | 0.10 |
| BMI, kg/m2 | 54 | 27.8 (4.2) | 27.4 (4.1) | 27.0 (4.0) | <0.01 | 48 | 28.6 (3.0) | 27.7 (3.0) | 28.5 (2.7) | 0.69 | 0.08 |
| Waist circumference, inches | 49 | 36.7 (5.9) | 35.2 (4.6) | 34.6 (4.2) | <0.01 | 42 | 36.7 (3.4) | 35.8 (3.5) | 35.4 (2.8) | <0.01 | 0.39 |
| Glucose | 50 | 114.5 (36.8) | 96.7 (17.6) | 88.9 (16.5) | <0.01 | 40 | 111.3 (22.0) | 102.2 (19.3) | 113.0 (12.0) | 0.56 | <0.01 |
| Cholesterol | 46 | 144.7 (35.7) | 182.7 (43.3) | 168.7 (30.5) | <0.01 | 40 | 138.5 (34.4) | 111.7 (20.3) | 137.3 (30.8) | 0.85 | <0.01 |
| Systolic BP | 51 | 131.6 (16.6) | 118.6 (12.4) | 118.2 (10.6) | <0.01 | 47 | 128.0 (16.2) | 118.4 (16.1) | 112.1 (12.1) | <0.01 | 0.47 |
| Diastolic BP | 51 | 83.1 (8.6) | 78.4 (8.3) | 78.0 (7.4) | <0.01 | 47 | 86.0 (10.5) | 79.8 (8.8) | 79.9 (5.6) | <0.01 | 0.61 |
| Controlled BP, n (%) | 51 | 36 (70.6) | 45 (88.2) | 49 (96.1) | <0.01 | 47 | 33 (70.2) | 42 (89.4) | 45 (95.7) | <0.01 | n/a |
| Physical activity | |||||||||||
| Any physical activity, n (%) | 53 | 2 (3.8) | 44 (83.0) | 47 (88.7) | <0.01 | 38 | 15 (39.5) | 27 (71.1) | 19 (50.0) | 0.36 | n/a |
| Social interaction (1–4, 4 = highest) | 53 | 1.4 (0.6) | 2.4 (0.8) | 3.6 (0.5) | <0.01 | 46 | 1.7 (0.7) | 1.6 (0.6) | 1.9 (0.6) | 0.04 | <0.01 |
| Food behaviors | |||||||||||
| Portion control (1–4, 4 = highest) | 49 | 1.8 (0.8) | 2.5 (0.8) | 3.6 (0.7) | <0.01 | 46 | 2.9 (0.9) | 2.1 (0.8) | 2.7 (0.6) | 0.09 | <0.01 |
| Eats brown rice often/almost always, n (%) | 40 | 2 (5.0) | 7 (17.5) | 10 (25.0) | <0.01 | 26 | 0 (0.0) | 0 (0.0) | 0 (0.0) | 1.0 | n/a |
| Diabetes knowledge | |||||||||||
| ADA diabetes knowledge Scale (0–8, 8 = highest) | 51 | 3.6 (2.3) | 5.5 (1.5) | 6.5 (0.6) | <0.01 | 44 | 3.5 (2.1) | 5.3 (1.5) | 4.9 (1.3) | <0.01 | <0.01 |
| Michigan diabetes knowledge scale (0–7, 7 = highest) | 50 | 1.1 (1.0) | 3.1 (1.5) | 3.2 (1.0) | <0.01 | 45 | 2.1 (1.2) | 3.4 (1.8) | 3.1 (1.0) | <0.01 | <0.01 |
3.1.3. Acceptability
| Program Evaluation | Intervention Group (n = 59) n (%) |
|---|---|
| Would you say you use the social service agency as a resource | |
| A lot | 54 (91.5) |
| Some | 5 (8.5) |
| How often does the following treat you with respect and dignity (great deal of the time) | |
| CHW | 58 (100.0) |
| Primary care doctor | 49 (86.0) |
| Health professionals besides doctors | 36 (62.1) |
| I am able to tell the CHW things that I cannot tell my doctor | |
| Strongly agree | 43 (72.9) |
| Agree | 15 (25.4) |
| Disagree | 1 (1.7) |
| The CHW helped me to change my behaviors | |
| Strongly agree | 54 (91.5) |
| Agree | 5 (8.5) |
| I see a doctor more often because of the CHW | |
| Strongly agree | 31 (52.5) |
| Agree | 28 (47.5) |
| I feel more confident asking my doctor questions because of the CHW | |
| Strongly agree | 32 (54.2) |
| Agree | 27 (45.8) |
| Overall, how satisfied are you with the CHW? (out of 10) | |
| 8–Very satisfied | 1 (1.7) |
| 9 | 6 (10.3) |
| 10–Totally satisfied | 51 (88.0) |
3.2. Qualitative Results
3.2.1. Feasibility
3.2.2. Efficacy
3.2.3. Acceptability
4. Discussion
| Challenges | Reason | Modifications Made to Full Intervention |
|---|---|---|
| Difficulty recruiting male participants | Sikh males are concentrated in small business and service sector position with long work hours | Working with gurdwara leadership to recruit more men into the project |
| Accommodating male participant schedules through additional sessions at convenient times | ||
| Word-of-mouth referrals—ask screening and intervention participants to refer their friends and family members | ||
| Lack of awareness regarding prevention | Misperception regarding the need for diabetes prevention in the absence of a diabetes diagnosis; general lack of community-level emphasis on prevention | Stronger partnerships and outreach to gurdwara leadership and staff to promote awareness for prevention |
| Better messaging of the social and financial implications of having the disease vs. attending a free program | ||
| Hold more community education events on diabetes and diabetes prevention in the Sikh American community | ||
| Goal-setting for participants | Participants were reluctant to engage in goal-setting or not familiar with the process | CHWs will receive additional training on motivational interviewing and goal-setting that is culturally tailored |
| Retention | Participants were unable to sustain participation due to family obligations and/or work schedules | Accommodating participants’ schedules by offering additional sessions at convenient times |
| Building in more incentives/prizes for retention | ||
| Marketing of Project RICE at routinely held health fairs to increase awareness of the program |
5. Conclusions and Implications
Acknowledgments
Author Contributions
Conflicts of Interest
References
- Guariguata, L.; Linnenkamp, U.; Beagley, J.; Whiting, D.R.; Cho, N.H. Global estimates of the prevalence of hyperglycaemia in pregnancy for 2013 for the IDF Diabetes Atlas. Diabetes Res. Clin. Pract. 2014, 103, 176–185. [Google Scholar] [CrossRef]
- Barnes, P.M.; Adams, P.F.; Powell-Griner, E. Health characteristics of the Asian adult population: United States, 2004–2006. Adv. Data 2008, 394, 1–22. [Google Scholar]
- Gupta, L.S.; Wu, C.C.; Young, S.; Perlman, S.E. Prevalence of diabetes in New York City, 2002–2008: Comparing foreign-born South Asians and other Asians with U.S.-born whites, blacks, and hispanics. Diabetes Care 2011, 34, 1791–1793. [Google Scholar] [CrossRef]
- Islam, N.S.; Wyatt, L.C.; Kapadia, S.B.; Rey, M.J.; Trinh-Shevrin, C.; Kwon, S.C. Diabetes and associated risk factors among Asian American subgroups in New York City. Diabetes Care 2013, 36. [Google Scholar] [CrossRef]
- Kanaya, A.M.; Wassel, C.L.; Mathur, D.; Stewart, A.; Herrington, D.; Budoff, M.J.; Randpura, V.; Liu, K. Prevalence and correlates of diabetes in South Asian Indians in the United States: Findings from the metabolic syndrome and atherosclerosis in South. asians living in america study and the multi-ethnic study of atherosclerosis. Metab. Syndr. Relat. Disord. 2010, 8, 157–164. [Google Scholar] [CrossRef]
- Wang, E.J.; Wong, E.C.; Dixit, A.A.; Fortmann, S.P.; Linde, R.B.; Palaniappan, L.P. Type 2 diabetes: Identifying high risk Asian American subgroups in a clinical population. Diabetes Res. Clin. Pract. 2011, 93, 248–254. [Google Scholar] [CrossRef]
- Venkataraman, R.; Nanda, N.C.; Baweja, G.; Parikh, N.; Bhatia, V. Prevalence of diabetes mellitus and related conditions in Asian Indians living in the United States. Amer. J. Cardiol. 2004, 94, 977–980. [Google Scholar] [CrossRef]
- Rajpathak, S.N.; Gupta, L.S.; Waddell, E.N.; Upadhyay, U.D.; Wildman, R.P.; Kaplan, R.; Wassertheil-Smoller, S.; Wylie-Rosett, J. Elevated risk of type 2 diabetes and metabolic syndrome among Asians and south Asians: Results from the 2004 New York City HANES. Ethn. Dis. 2010, 20, 225–230. [Google Scholar]
- Diabetes Prevention Program Research. The Diabetes Prevention Program. (DPP): Description of lifestyle intervention. Diabetes Care 2002, 25, 2165–2171. [CrossRef]
- Knowler, W.C.; Barrett-Connor, E.; Fowler, S.E.; Hamman, R.F.; Lachin, J.M.; Walker, E.A.; Nathan, D.M. Reduction in the incidence of type 2 diabetes with lifestyle intervention or metformin. N. Engl. J. Med. 2002, 346, 393–403. [Google Scholar] [CrossRef]
- Boltri, J.M.; Davis-Smith, M.; Okosun, I.S.; Seale, J.P.; Foster, B. Translation of the national institutes of health diabetes prevention program in African American churches. J. Natl. Med. Assoc. 2011, 103, 194–202. [Google Scholar]
- Ackermann, R.T.; Finch, E.A.; Brizendine, E.; Zhou, H.; Marrero, D.G. Translating the diabetes prevention program into the community: The DEPLOY Pilot Study. Amer. J. Prev. Med. 2008, 35, 357–363. [Google Scholar] [CrossRef]
- Amundson, H.A.; Butcher, M.K.; Gohdes, D.; Hall, T.O.; Harwell, T.S.; Helgerson, S.D.; Vanderwood, K.K. Translating the Diabetes Prevention Program into practice in the general community: Findings from the Montana Cardiovascular Disease and Diabetes Prevention Program. Diabetes Educ. 2009, 35, 209–210, 213–214, 216–220. [Google Scholar] [CrossRef]
- Hamman, R.F.; Wing, R.R.; Edelstein, S.L.; Lachin, J.M.; Bray, G.A.; Delahanty, L.; Hoskin, M.; Kriska, A.M.; Mayer-Davis, E.J.; Pi-Sunyer, X.; et al. Effect of weight loss with lifestyle intervention on risk of diabetes. Diabetes Care 2006, 29, 2102–2107. [Google Scholar] [CrossRef]
- Jaber, L.A.; Pinelli, N.R.; Brown, M.B.; Funnell, M.M.; Anderson, R.; Hammand, A.; Herman, W.H. Feasibility of group lifestyle intervention for diabetes prevention in Arab Americans. Diabetes Res. Clin. Pract. 2011, 91, 307–315. [Google Scholar] [CrossRef]
- Katula, J.A.; Vitolins, M.Z.; Morgan, T.M.; Lawlor, M.S.; Blackwell, C.S.; Isom, S.P.; Pedley, C.F.; Goff, D.C., Jr. The Healthy Living Partnerships to Prevent Diabetes study: 2-year outcomes of a randomized controlled trial. Amer. J. Prev. Med. 2013, 44, S324–S332. [Google Scholar] [CrossRef]
- Katula, J.A.; Vitolins, M.Z.; Rosenberger, E.L.; Blackwell, C.S.; Morgan, T.M.; Lawlor, M.S.; Goff, D.C., Jr. One-year results of a community-based translation of the Diabetes Prevention Program: Healthy-living Partnerships to Prevent Diabetes (HELP PD) Project. Diabetes Care 2011, 34, 1451–1457. [Google Scholar] [CrossRef]
- Kramer, M.K.; McWilliams, J.R.; Chen, H.Y.; Siminerio, L.M. A community-based diabetes prevention program: Evaluation of the group lifestyle balance program delivered by diabetes educators. Diabetes Educ. 2011, 37, 659–668. [Google Scholar] [CrossRef]
- Matvienko, O.A.; Hoehns, J.D. A lifestyle intervention study in patients with diabetes or impaired glucose tolerance: Translation of a research intervention into practice. J. Am. Board Fam. Med. 2009, 22, 535–543. [Google Scholar] [CrossRef]
- Mau, M.K.; Keawe’aimoku Kaholokula, J.; West, M.R.; Leake, A.; Efird, J.T.; Rose, C.; Palakiko, D.M.; Yoshimura, S.; Kekauoha, P.B.; Gomes, H. Translating diabetes prevention into native Hawaiian and Pacific Islander communities: The PILI’Ohana pilot project. Prog. Community Health Partnersh 2010, 4, 7–16. [Google Scholar] [CrossRef]
- Ockene, I.S.; Tellez, T.L.; Rosal, M.C.; Reed, G.W.; Mordes, J.; Merriam, P.A.; Olendzki, B.C.; Handelman, G.; Nicolosi, R.; Ma, Y. Outcomes of a Latino community-based intervention for the prevention of diabetes: The Lawrence Latino Diabetes Prevention Project. Amer. J. Public Health 2012, 102, 336–342. [Google Scholar] [CrossRef]
- Seidel, M.C.; Powell, R.O.; Zgibor, J.C.; Siminerio, L.M.; Piatt, G.A. Translating the Diabetes Prevention Program. into an urban medically underserved community: A nonrandomized prospective intervention study. Diabetes Care 2008, 31, 684–689. [Google Scholar] [CrossRef]
- Vincent, D.; McEwen, M.M.; Hepworth, J.T.; Stump, C.S. The effects of a community-based, culturally tailored diabetes prevention intervention for high-risk adults of Mexican descent. Diabetes Educ. 2014, 40, 202–213. [Google Scholar] [CrossRef]
- Jackson, L. Translating the Diabetes Prevention Program into practice: A review of community interventions. Diabetes Educ. 2009, 35, 309–320. [Google Scholar] [CrossRef]
- Gutierrez, J.; Devia, C.; Weiss, L.; Chantarat, T.; Ruddock, C.; Linnell, J.; Golub, M.; Godfrey, L.; Rosen, R.; Calman, N. Health, community, and spirituality: Evaluation of a multicultural faith-based diabetes prevention program. Diabetes Educ. 2014, 40, 214–222. [Google Scholar]
- Vadheim, L.M.; Brewer, K.A.; Kassner, D.R.; Vanderwood, K.K.; Hall, T.O.; Butcher, M.K.; Helgerson, S.D.; Harwell, T.S. Effectiveness of a lifestyle intervention program among persons at high risk for cardiovascular disease and diabetes in a rural community. J. Rural Health 2010, 26, 266–272. [Google Scholar] [CrossRef]
- Coppell, K.J.; Tipene-Leach, D.C.; Pahau, H.L.; Williams, S.M.; Abel, S.; Iles, M.; Hindmarsh, J.H.; Mann, J.I. Two-year results from a community-wide diabetes prevention intervention in a high risk indigenous community: The Ngati and healthy project. Diabetes Res. Clin. Pract. 2009, 85, 220–227. [Google Scholar] [CrossRef]
- Islam, N.S.; Zanowiak, J.M.; Wyatt, L.C.; Chun, K.; Lee, L.; Kwon, S.C.; Trinh-Shevrin, C. A randomized-controlled, pilot intervention on diabetes prevention and healthy lifestyles in the New York City Korean community. J. Community Health 2013, 38, 1030–1041. [Google Scholar] [CrossRef]
- Davis-Smith, Y.M.; Boltri, J.M.; Seale, J.P.; Shellenberger, S.; Blalock, T.; Tobin, B. Implementing a diabetes prevention program in a rural African-American church. J. Natl. Med. Assoc. 2007, 99, 440–446. [Google Scholar]
- Merriam, P.A.; Tellez, T.L.; Rosal, M.C.; Olendzki, B.C.; Ma, Y.; Pagoto, S.L.; Ockene, I.S. Methodology of a diabetes prevention translational research project utilizing a community-academic partnership for implementation in an underserved Latino community. BMC Med. Res. Methodol. 2009, 9. [Google Scholar] [CrossRef]
- Vincent, D.; McEwen, M.M.; Hepworth, J.T.; Stump, C.S. Challenges and success of recruiting and retention for a culturally tailored diabetes prevention program for adults of Mexican descent. Diabetes Educ. 2013, 39, 222–230. [Google Scholar] [CrossRef]
- Williams, L.B.; Sattin, R.W.; Dias, J.; Garvin, J.T.; Marion, L.; Joshua, T.; Kriska, A.; Kramer, M.K.; Echouffo-Tcheugui, J.B.; Freeman, A.; et al. Design of a cluster-randomized controlled trial of a diabetes prevention program within African-American churches: The fit body and soul study. Contemp. Clin. Trials 2013, 34, 336–347. [Google Scholar] [CrossRef]
- Parikh, P.; Simon, E.P.; Fei, K.; Looker, H.; Goytia, C.; Horowitz, C.R. Results of a pilot diabetes prevention intervention in east Harlem, New York City: Project HEED. Amer. J. Public Health 2010, 100, S232–S239. [Google Scholar] [CrossRef]
- Ramachandran, A.; Snehalatha, C. Diabetes prevention programs. Med. Clin. North Am. 2011, 95, 353–372. [Google Scholar] [CrossRef]
- Wallia, S.; Bhopal, R.S.; Douglas, A.; Bhopal, R.; Sharma, A.; Hutchison, A.; Murray, G.; Gill, J.; Sattar, N.; Lawton, J.; et al. Culturally adapting the prevention of diabetes and obesity in south Asians (PODOSA) trial. Health Promot. Int. 2013, in press. [Google Scholar]
- Tang, T.S.; Sohal, P.S.; Garg, A.K. Evaluating a diabetes self-management support peer leader training programme for the English- and Punjabi-speaking South.-Asian community in Vancouver. Diabet. Med. 2013, 30, 746–752. [Google Scholar] [CrossRef]
- U.S. Census Bureau. American Community Survey 1-year Estimates 2012. Available online: http://factfinder2.census.gov/ (accessed on 21 March 2014).
- South Asian Americans Leading Together and the Asian American Federation. A demographic snapshot of south Asians in the United States. Available online: http://saalt.org/wp-content/uploads/2012/09/Demographic-Snapshot-Asian-American-Foundation-2012.pdf (accessed on 21 March 2014).
- Mann, G.S.; Numrich, P.; Williams, R. Buddhists, Hindus and Sikhs in America: A Short History; Oxford University Press: New York, NY, USA, 2007. [Google Scholar]
- Venugopal, A. Sikhs Lobby the Census. Available online: http://www.wnyc.org/story/86445-sikhs-lobby-the-census/ (accessed on 16 May 2014).
- The Sikh Coalition. Making Our Voices Heard: A Civil Rights Agenda for New York City’s Sikhs. Available online: http://www.sikhcoalition.org/documents/pdf/RaisingOurVoicesReport.pdf (accessed on 12 May 2014).
- Ivey, S.L.; Patel, S.; Kalra, P.; Greenlund, K.; Srinivasan, S.; Grewal, D. Cardiovascular health among Asian Indians (CHAI): A community research project. J. Interprof. Care 2004, 18, 391–402. [Google Scholar] [CrossRef]
- Bhatnagar, D.; Anand, I.S.; Durrington, P.N.; Patel, D.J.; Wander, G.S.; Mackness, M.I.; Creed, F.; Tomenson, B.; Chandrashekhar, Y.; Winterbotham, M. Coronary risk factors in people from the Indian subcontinent living in west London and their siblings in India. Lancet 1995, 345, 405–409. [Google Scholar] [CrossRef]
- Hussain, S.M.; Oldenburg, B.; Wang, Y.; Zoungas, S.; Tonkin, A.M. Assessment of cardiovascular disease risk in south Asian populations. Int. J. Vasc. Med. 2013, 2013. [Google Scholar] [CrossRef]
- American Diabetes Association. Are You at Risk? Available online: http://www.diabetes.org/are-you-at-risk (accessed on 12 May 2014).
- Bang, H.; Edwards, A.M.; Bomback, A.S.; Ballantyne, C.M.; Brillon, D.; Callahan, M.A.; Teutsch, S.M.; Mushlin, A.I.; Kern, L.M. Development and validation of a patient self-assessment score for diabetes risk. Ann. Intern. Med. 2009, 151, 775–783. [Google Scholar] [CrossRef]
- WHO Expert Consultation. Appropriate body-mass index for Asian populations and its implications for policy and intervention strategies. Lancet 2004, 363, 157–163. [Google Scholar] [CrossRef]
- National Diabetes Education Program. Small Steps, Big Rewards. Your Gam Plan to Prevent Type 2 Diabetes: Information for Patients. Available online: http://www.ndep.nih.gov/publications/PublicationDetail.aspx?PubId=71 (accessed on 12 May 2014).
- Zheng, W.; McLerran, D.F.; Rolland, B.; Zhang, X.; Inoue, M.; Matsuo, K.; He, J.; Gupta, P.C.; Ramadas, K.; Tsugane, S.; et al. Association between body-mass index and risk of death in more than 1 million Asians. N. Engl. J. Med. 2011, 364, 719–729. [Google Scholar]
- Glynn, R.J.; Brookhart, M.A.; Stedman, M.; Avorn, J.; Solomon, D.H. Design of cluster-randomized trials of quality improvement interventions aimed at medical care providers. Med. Care 2007, 45, S38–S43. [Google Scholar]
- The Newest New Yorkers. Available online: http://s3.documentcloud.org/documents/929300/the-newest-new-yorkers-2013-edition.pdf (accessed on 21 March 2014).
- U.S. Census Bureau. American Community Survey 5-year Estimates: Selected Characteristics of the Native and Foreign-born Populations, 2008–2012. Available online: http://factfinder2.census.gov/ (accessed on 12 May 2014).
- National Heart Lung and Blood Institute. Healthy Heart, Healthy Family: A Community Health Worker’s Manual for the Filipino Community. Available online: http://www.nhlbi.nih.gov/health/prof/heart/other/chdfilipino/intro.htm (accessed on 12 May 2014).
- National Diabetes Education Program. Power to Prevent: A Family Lifestyle Approach to Diabetes Prevention. Available online: http://ndep.nih.gov/media/power-to-prevent-508.pdf (accessed on 21 March 2014).
- Islam, N.S.; Wyatt, L.C.; Patel, S.D.; Shapiro, E.; Tandon, S.D.; Mukherji, B.R.; Tanner, M.; Rey, M.J.; Trinh-Shevrin, C. Evaluation of a community health worker pilot intervention to improve diabetes management in Bangladeshi immigrants with type 2 diabetes in New York city. Diabetes Educ. 2013, 39, 478–493. [Google Scholar] [CrossRef]
- Ruiz, Y.; Matos, S.; Kapadia, S.; Islam, N.; Cusack, A.; Kwong, S.; Trinh-Shevrin, C. Lessons learned from a community-academic initiative: The development of a core competency-based training for community-academic initiative community health workers. Amer. J. Public Health 2012, 102, 2372–2379. [Google Scholar] [CrossRef]
- Ursua, R.A.; Aguilar, D.E.; Wyatt, L.C.; Katigbak, C.; Islam, N.S.; Tandon, D.S.; Nur, P.R.M.Q.; van Devanter, N.; Rey, M.; Trinh-Shevrin, C. A community health worker intervention to improve management of hypertension among Filipino Americans in New York and New Jersey: A pilot study. Ethn. Dis. 2014, 24, 67–76. [Google Scholar]
- U.S. Census Bureau. Design and Methodology: American Community Survey. Available online: http://www.census.gov/history/pdf/ACSHistory.pdf (accessed on 12 May 2014).
- Centers for Disease Control and Prevention. Behavioral Risk Factor Surveillance System: Questionnaires. Available online: http://www.cdc.gov/brfss/questionnaires.htm (accessed on 12 May 2014).
- Bandura, A. Self-efficacy Beliefs of Adolescents; Information Age Publishing: New York, NY, USA, 2006. [Google Scholar]
- Fitzgerald, J.T.; Funnell, M.M.; Hess, G.E.; Barr, P.A.; Anderson, R.M.; Hiss, R.G.; Davis, W.K. The reliability and validity of a brief diabetes knowledge test. Diabetes Care 1998, 21, 706–710. [Google Scholar] [CrossRef]
- Nothwehr, F.; Dennis, L.; Wu, H. Measurement of behavioral objectives for weight management. Health Educ. Behav. 2007, 34, 793–809. [Google Scholar] [CrossRef]
- Yeary, K.H.; Cornell, C.E.; Turner, J.; Moore, P.; Bursac, Z.; Prewitt, E.; West, D.S. Feasibility of an evidence-based weight loss intervention for a faith-based, rural, African American population. Prev. Chronic. Dis. 2011, 8. Available online: http://www.cdc.gov/pcd/issues/2011/nov/10_0194.htm (accessed on 16 May 2014).
- Dodani, S.; Fields, J.Z. Implementation of the fit body and soul, a church-based life style program for diabetes prevention in high-risk African Americans: A feasibility study. Diabetes Educ. 2010, 36, 465–472. [Google Scholar] [CrossRef]
- Boltri, J.M.; Davis-Smith, Y.M.; Seale, J.P.; Shellenberger, S.; Okosun, I.S.; Cornelius, M.E. Diabetes prevention in a faith-based setting: Results of translational research. J. Public Health Manag. Pract. 2008, 14, 29–32. [Google Scholar] [CrossRef]
- Olansky, L.; Kennedy, L. Finger-stick glucose monitoring: Issues of accuracy and specificity. Diabetes Care 2010, 33, 948–949. [Google Scholar] [CrossRef]
- Arvey, S.R.; Fernandez, M.E. Identifying the core elements of effective community health worker programs: A research agenda. Amer J. Public Health 2012, 102, 1633–1637. [Google Scholar] [CrossRef]
© 2014 by the authors; licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution license (http://creativecommons.org/licenses/by/3.0/).
Share and Cite
Islam, N.S.; Zanowiak, J.M.; Wyatt, L.C.; Kavathe, R.; Singh, H.; Kwon, S.C.; Trinh-Shevrin, C. Diabetes Prevention in the New York City Sikh Asian Indian Community: A Pilot Study. Int. J. Environ. Res. Public Health 2014, 11, 5462-5486. https://doi.org/10.3390/ijerph110505462
Islam NS, Zanowiak JM, Wyatt LC, Kavathe R, Singh H, Kwon SC, Trinh-Shevrin C. Diabetes Prevention in the New York City Sikh Asian Indian Community: A Pilot Study. International Journal of Environmental Research and Public Health. 2014; 11(5):5462-5486. https://doi.org/10.3390/ijerph110505462
Chicago/Turabian StyleIslam, Nadia S., Jennifer M. Zanowiak, Laura C. Wyatt, Rucha Kavathe, Hardayal Singh, Simona C. Kwon, and Chau Trinh-Shevrin. 2014. "Diabetes Prevention in the New York City Sikh Asian Indian Community: A Pilot Study" International Journal of Environmental Research and Public Health 11, no. 5: 5462-5486. https://doi.org/10.3390/ijerph110505462




