Application of Monoclonal Antibody G250 Recognizing Carbonic Anhydrase IX in Renal Cell Carcinoma
Abstract
:1. Introduction
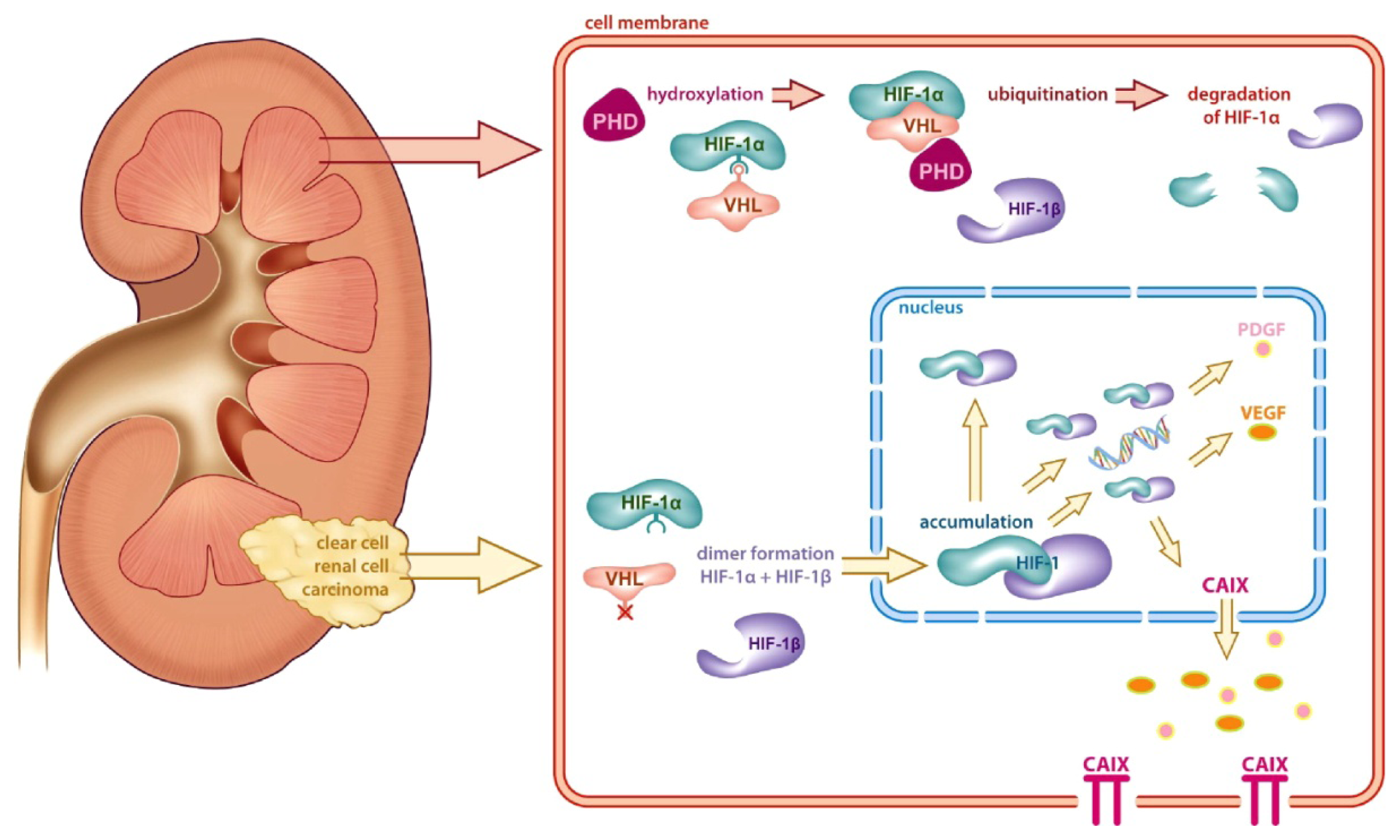
2. Cloning of G250 Antigen and Relation to ccRCC
3. Clinical Studies with mAbG250
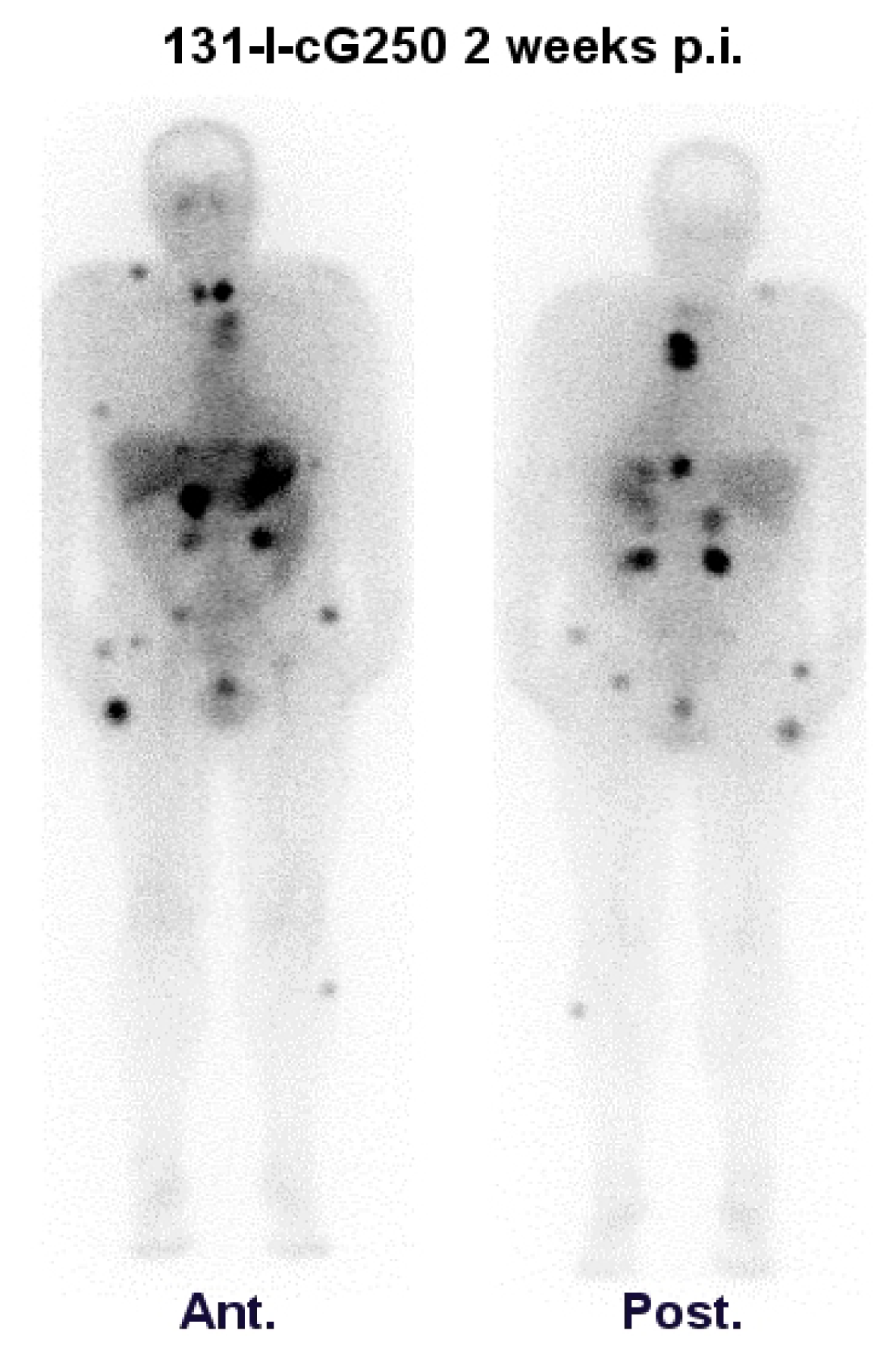
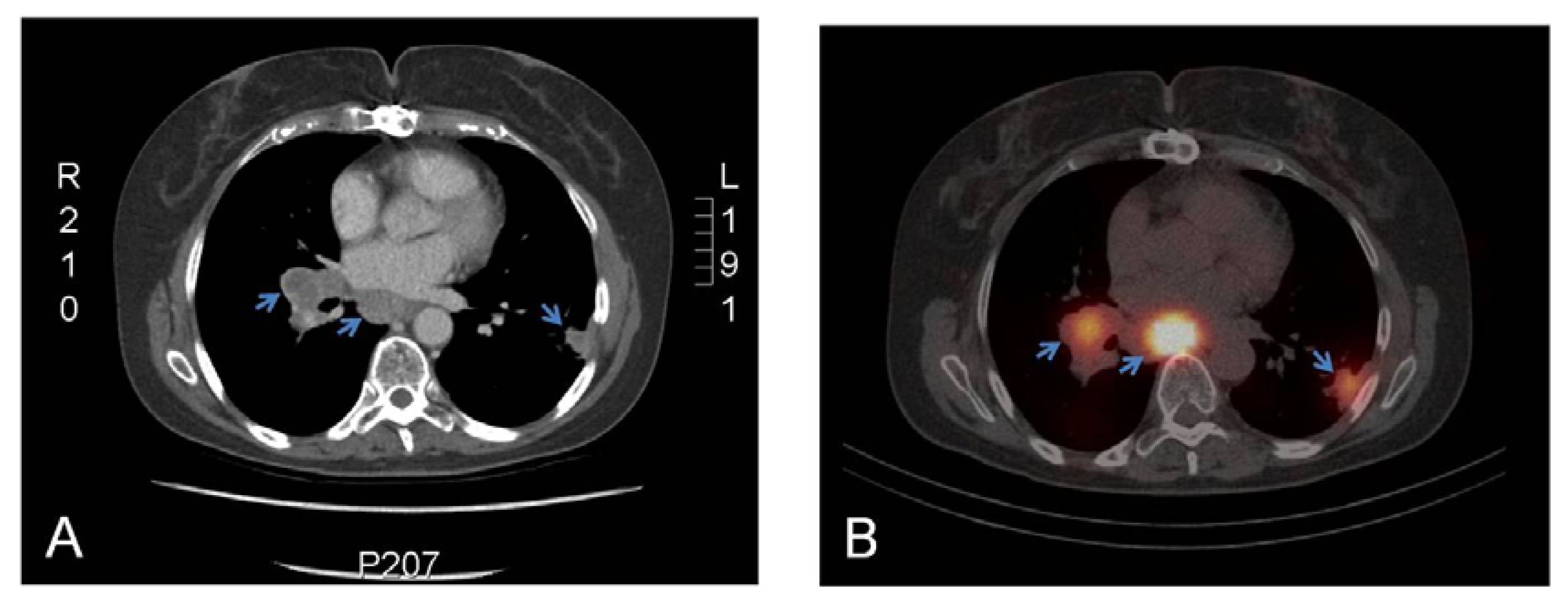
3.1. Imaging Studies
3.2. Therapy Studies
3.3. Therapeutic Studies with Unmodified cG250
4. Future Prospects
5. Conclusion
Conflict of Interest
References
- Jemal, A.; Siegel, R.; Ward, E.; Hao, Y.; Xu, J.; Thun, M.J. Cancer statistics, 2009. CA Cancer J. Clin 2009, 59, 225–249. [Google Scholar]
- Patard, J.J.; Pignot, G.; Escudier, B.; Eisen, T.; Bex, A.; Sternberg, C.; Rini, B.; Roigas, J.; Choueiri, T.; Bukowski, R.; et al. Icud-eau international consultation on kidney cancer 2010: Treatment of metastatic disease. Eur. Urol 2011, 60, 684–690. [Google Scholar]
- Motzer, R.J.; Rini, B.I.; Bukowski, R.M.; Curti, B.D.; George, D.J.; Hudes, G.R.; Redman, B.G.; Margolin, K.A.; Merchan, J.R.; Wilding, G.; et al. Sunitinib in patients with metastatic renal cell carcinoma. JAMA 2006, 295, 2516–2524. [Google Scholar]
- Escudier, B.; Eisen, T.; Stadler, W.M.; Szczylik, C.; Oudard, S.; Siebels, M.; Negrier, S.; Chevreau, C.; Solska, E.; Desai, A.A.; et al. Sorafenib in advanced clear-cell renal-cell carcinoma. N. Engl. J. Med 2007, 356, 125–134. [Google Scholar]
- Rixe, O.; Bukowski, R.M.; Michaelson, M.D.; Wilding, G.; Hudes, G.R.; Bolte, O.; Motzer, R.J.; Bycott, P.; Liau, K.F.; Freddo, J.; et al. Axitinib treatment in patients with cytokine-refractory metastatic renal-cell cancer: A phase II study. Lancet Oncol 2007, 8, 975–984. [Google Scholar]
- Sternberg, C.N.; Davis, I.D.; Mardiak, J.; Szczylik, C.; Lee, E.; Wagstaff, J.; Barrios, C.H.; Salman, P.; Gladkov, O.A.; Kavina, A.; et al. Pazopanib in locally advanced or metastatic renal cell carcinoma: Results of a randomized phase III trial. J. Clin. Oncol 2010, 28, 1061–1068. [Google Scholar]
- Escudier, B.; Bellmunt, J.; Negrier, S.; Bajetta, E.; Melichar, B.; Bracarda, S.; Ravaud, A.; Golding, S.; Jethwa, S.; Sneller, V. Phase III trial of bevacizumab plus interferon alfa-2a in patients with metastatic renal cell carcinoma (avoren): Final analysis of overall survival. J. Clin. Oncol 2010, 28, 2144–2150. [Google Scholar]
- Coppin, C.; Kollmannsberger, C.; Le, L.; Porzsolt, F.; Wilt, T.J. Targeted therapy for advanced renal cell cancer (rcc): A cochrane systematic review of published randomised trials. BJU Int 2011, 108, 1556–1563. [Google Scholar]
- Oosterwijk, E.; Ruiter, D.J.; Hoedemaeker, P.J.; Pauwels, E.K.; Jonas, U.; Zwartendijk, J.; Warnaar, S.O. Monoclonal antibody g250 recognizes a determinant present in renal-cell carcinoma and absent from normal kidney. Int. J. Cancer 1986, 38, 489–494. [Google Scholar]
- Uemura, H.; Nakagawa, Y.; Yoshida, K.; Saga, S.; Yoshikawa, K.; Hirao, Y.; Oosterwijk, E. Mn/ca ix/g250 as a potential target for immunotherapy of renal cell carcinomas. Br. J. Cancer 1999, 81, 741–746. [Google Scholar]
- Bismar, T.A.; Bianco, F.J.; Zhang, H.; Li, X.; Sarkar, F.H.; Sakr, W.A.; Grignon, D.J.; Che, M. Quantification of g250 mrna expression in renal epithelial neoplasms by real-time reverse transcription-pcr of dissected tissue from paraffin sections. Pathology 2003, 35, 513–517. [Google Scholar]
- Pastorek, J.; Pastorekova, S.; Callebaut, I.; Mornon, J.P.; Zelnik, V.; Opavsky, R.; Zat’ovicova, M.; Liao, S.; Portetelle, D.; Stanbridge, E.J.; et al. Cloning and characterization of mn, a human tumor-associated protein with a domain homologous to carbonic anhydrase and a putative helix-loop-helix DNA binding segment. Oncogene 1994, 9, 2877–2888. [Google Scholar]
- Grabmaier, K.; Vissers, J.L.; de Weijert, M.C.; Oosterwijk-Wakka, J.C.; van Bokhoven, A.; Brakenhoff, R.H.; Noessner, E.; Mulders, P.A.; Merkx, G.; Figdor, C.G.; et al. Molecular cloning and immunogenicity of renal cell carcinoma-associated antigen g250. Int. J. Cancer 2000, 85, 865–870. [Google Scholar]
- Grabmaier, K.; A de Weijert, M.C.; Verhaegh, G.W.; Schalken, J.A.; Oosterwijk, E. Strict regulation of caix(g250/mn) by hif-1alpha in clear cell renal cell carcinoma. Oncogene 2004, 23, 5624–5631. [Google Scholar]
- Gnarra, J.R.; Tory, K.; Weng, Y.; Schmidt, L.; Wei, M.H.; Li, H.; Latif, F.; Liu, S.; Chen, F.; Duh, F.M.; et al. Mutations of the vhl tumour suppressor gene in renal carcinoma. Nat. Genet 1994, 7, 85–90. [Google Scholar]
- Jaakkola, P.; Mole, D.R.; Tian, Y.M.; Wilson, M.I.; Gielbert, J.; Gaskell, S.J.; von Kriegsheim, A.; Hebestreit, H.F.; Mukherji, M.; Schofield, C.J.; et al. Targeting of hif-alpha to the von hippel-lindau ubiquitylation complex by o2-regulated prolyl hydroxylation. Science 2001, 292, 468–472. [Google Scholar]
- Schofield, C.J.; Ratcliffe, P.J. Signalling hypoxia by hif hydroxylases. Biochem. Biophys. Res. Commun 2005, 338, 617–626. [Google Scholar]
- Ivanov, S.; Liao, S.Y.; Ivanova, A.; Danilkovitch-Miagkova, A.; Tarasova, N.; Weirich, G.; Merrill, M.J.; Proescholdt, M.A.; Oldfield, E.H.; Lee, J.; et al. Expression of hypoxia-inducible cell-surface transmembrane carbonic anhydrases in human cancer. Am. J. Pathol 2001, 158, 905–919. [Google Scholar]
- Potter, C.; Harris, A.L. Hypoxia inducible carbonic anhydrase ix, marker of tumour hypoxia, survival pathway and therapy target. Cell Cycle 2004, 3, 164–167. [Google Scholar]
- Stillebroer, A.B.; Mulders, P.F.; Boerman, O.C.; Oyen, W.J.; Oosterwijk, E. Carbonic anhydrase ix in renal cell carcinoma: Implications for prognosis, diagnosis, and therapy. Eur. Urol. 2010, 58, 75–83. [Google Scholar]
- Poeppel, T.D.; Krause, B.J.; Heusner, T.A.; Boy, C.; Bockisch, A.; Antoch, G. Pet/ct for the staging and follow-up of patients with malignancies. Eur. J. Radiol 2009, 70, 382–392. [Google Scholar]
- Patard, J.J. Incidental renal tumours. Curr. Opin. Urol 2009, 19, 454–458. [Google Scholar]
- Van Dijk, J.; Zegveld, S.T.; Fleuren, G.J.; Warnaar, S.O. Localization of monoclonal antibody g250 and bispecific monoclonal antibody cd3/g250 in human renal-cell carcinoma xenografts: Relative effects of size and affinity. Int. J. Cancer 1991, 48, 738–743. [Google Scholar]
- Kranenborg, M.H.; Boerman, O.C.; de Weijert, M.C.; Oosterwijk-Wakka, J.C.; Corstens, F.H.; Oosterwijk, E. The effect of antibody protein dose of anti-renal cell carcinoma monoclonal antibodies in nude mice with renal cell carcinoma xenografts. Cancer 1997, 80, 2390–2397. [Google Scholar]
- Steffens, M.G.; Kranenborg, M.H.; Boerman, O.C.; Zegwaart-Hagemeier, N.E.; Debruyne, F.M.; Corstens, F.H.; Oosterwijk, E. Tumor retention of 186re-mag3, 111in-dtpa and 125i labeled monoclonal antibody g250 in nude mice with renal cell carcinoma xenografts. Cancer Biother. Radiopharm 1998, 13, 133–139. [Google Scholar]
- Steffens, M.G.; Oosterwijk, E.; Kranenborg, M.H.; Manders, J.M.; Debruyne, F.M.; Corstens, F.H.; Boerman, O.C. In vivo and in vitro characterizations of three 99mtc-labeled monoclonal antibody g250 preparations. J. Nucl. Med 1999, 40, 829–836. [Google Scholar]
- Van Dijk, J.; Oosterwijk, E.; van Kroonenburgh, M.J.; Jonas, U.; Fleuren, G.J.; Pauwels, E.K.; Warnaar, S.O. Perfusion of tumor-bearing kidneys as a model for scintigraphic screening of monoclonal antibodies. J. Nucl. Med 1988, 29, 1078–1082. [Google Scholar]
- Oosterwijk, E.; Bander, N.H.; Divgi, C.R.; Welt, S.; Wakka, J.C.; Finn, R.D.; Carswell, E.A.; Larson, S.M.; Warnaar, S.O.; Fleuren, G.J.; et al. Antibody localization in human renal cell carcinoma: A phase i study of monoclonal antibody g250. J. Clin. Oncol 1993, 11, 738–750. [Google Scholar]
- Divgi, C.R.; Bander, N.H.; Scott, A.M.; O’Donoghue, J.A.; Sgouros, G.; Welt, S.; Finn, R.D.; Morrissey, F.; Capitelli, P.; Williams, J.M.; et al. Phase i/ii radioimmunotherapy trial with iodine-131-labeled monoclonal antibody g250 in metastatic renal cell carcinoma. Clin. Cancer Res 1998, 4, 2729–2739. [Google Scholar]
- Steffens, M.G.; Boerman, O.C.; Oosterwijk-Wakka, J.C.; Oosterhof, G.O.; Witjes, J.A.; Koenders, E.B.; Oyen, W.J.; Buijs, W.C.; Debruyne, F.M.; Corstens, F.H.; et al. Targeting of renal cell carcinoma with iodine-131-labeled chimeric monoclonal antibody g250. J. Clin. Oncol 1997, 15, 1529–1537. [Google Scholar]
- Steffens, M.G.; Boerman, O.C.; Oyen, W.J.; Kniest, P.H.; Witjes, J.A.; Oosterhof, G.O.; van Leenders, G.J.; Debruyne, F.M.; Corstens, F.H.; Oosterwijk, E. Intratumoral distribution of two consecutive injections of chimeric antibody g250 in primary renal cell carcinoma: Implications for fractionated dose radioimmunotherapy. Cancer Res 1999, 59, 1615–1619. [Google Scholar]
- Brouwers, A.H.; Dorr, U.; Lang, O.; Boerman, O.C.; Oyen, W.J.; Steffens, M.G.; Oosterwijk, E.; Mergenthaler, H.G.; Bihl, H.; Corstens, F.H. 131I-cg250 monoclonal antibody immunoscintigraphy vs. [18F]fdg-pet imaging in patients with metastatic renal cell carcinoma: A comparative study. Nucl. Med. Commun 2002, 23, 229–236. [Google Scholar]
- Brouwers, A.H.; Buijs, W.C.; Oosterwijk, E.; Boerman, O.C.; Mala, C.; de Mulder, P.H.; Corstens, F.H.; Mulders, P.F.; Oyen, W.J. Targeting of metastatic renal cell carcinoma with the chimeric monoclonal antibody g250 labeled with 131I or 111In: An intrapatient comparison. Clin. Cancer Res 2003, 9, 3953S–3960S. [Google Scholar]
- Divgi, C.R.; Pandit-Taskar, N.; Jungbluth, A.A.; Reuter, V.E.; Gonen, M.; Ruan, S.; Pierre, C.; Nagel, A.; Pryma, D.A.; Humm, J.; et al. Preoperative characterisation of clear-cell renal carcinoma using iodine-124-labelled antibody chimeric g250 (124I-cg250) and pet in patients with renal masses: A phase i trial. Lancet Oncol 2007, 8, 304–310. [Google Scholar]
- Divgi, C.R.; Uzzo, R.G.; Gatsonis, C.; Bartz, R.; Treutner, S.; Yu, J.Q.; Chen, D.; Carrasquillo, J.A.; Larson, S.; Bevan, P.; et al. Positron emission tomography/computed tomography identification of clear cell renal cell carcinoma: Results from the redect trial. J. Clin. Oncol 2013, 31, 187–194. [Google Scholar]
- Muselaers, C.H.; Boerman, O.C.; Oosterwijk, E.; Langenhuijsen, J.F.; Oyen, W.J.; Mulders, P.F. Indium-111-labeled girentuximab immunospect as a diagnostic tool in clear cell renal cell carcinoma. Eur. Urol. 2013. [Google Scholar] [CrossRef]
- Steffens, M.G.; Oosterwijk, E.; Zegwaart-Hagemeier, N.E.; van’t Hof, M.A.; Debruyne, F.M.; Corstens, F.H.; Boerman, O.C. Immunohistochemical analysis of intratumoral heterogeneity of [131I]cg250 antibody uptake in primary renal cell carcinomas. Br. J. Cancer 1998, 78, 1208–1213. [Google Scholar]
- Durrbach, A.; Angevin, E.; Poncet, P.; Rouleau, M.; Chavanel, G.; Chapel, A.; Thierry, D.; Gorter, A.; Hirsch, R.; Charpentier, B.; et al. Antibody-mediated endocytosis of g250 tumor-associated antigen allows targeted gene transfer to human renal cell carcinoma in vitro. Cancer Gene Ther 1999, 6, 564–571. [Google Scholar]
- Genega, E.M.; Ghebremichael, M.; Najarian, R.; Fu, Y.N.; Wang, Y.H.; Argani, P.; Grisanzio, C.; Signoretti, S. Carbonic anhydrase ix expression in renal neoplasms correlation with tumor type and grade. Am. J. Clin. Pathol 2010, 134, 873–879. [Google Scholar]
- Van Schaijk, F.G.; Broekema, M.; Oosterwijk, E.; van Eerd, J.E.; McBride, B.J.; Goldenberg, D.M.; Corstens, F.H.; Boerman, O.C. Residualizing iodine markedly improved tumor targeting using bispecific antibody-based pretargeting. J. Nucl. Med 2005, 46, 1016–1022. [Google Scholar]
- Brouwers, A.H.; van Eerd, J.E.; Frielink, C.; Oosterwijk, E.; Oyen, W.J.; Corstens, F.H.; Boerman, O.C. Optimization of radioimmunotherapy of renal cell carcinoma: Labeling of monoclonal antibody cg250 with 131I, 90Y, 177Lu, or 186Re. J. Nucl. Med 2004, 45, 327–337. [Google Scholar]
- Steffens, M.G.; Boerman, O.C.; de Mulder, P.H.; Oyen, W.J.; Buijs, W.C.; Witjes, J.A.; van den Broek, W.J.; Oosterwijk-Wakka, J.C.; Debruyne, F.M.; Corstens, F.H.; et al. Phase I radioimmunotherapy of metastatic renal cell carcinoma with 131I-labeled chimeric monoclonal antibody g250. Clin. Cancer Res 1999, 5, 3268S–3274S. [Google Scholar]
- Divgi, C.R.; O’Donoghue, J.A.; Welt, S.; O’Neel, J.; Finn, R.; Motzer, R.J.; Jungbluth, A.; Hoffman, E.; Ritter, G.; Larson, S.M.; et al. Phase I clinical trial with fractionated radioimmunotherapy using 131I-labeled chimeric g250 in metastatic renal cancer. J. Nuclear Med 2004, 45, 1412–1421. [Google Scholar]
- Brouwers, A.H.; Mulders, P.F.; de Mulder, P.H.; van den Broek, W.J.; Buijs, W.C.; Mala, C.; Joosten, F.B.; Oosterwijk, E.; Boerman, O.C.; Corstens, F.H.; et al. Lack of efficacy of two consecutive treatments of radioimmunotherapy with 131I-cg250 in patients with metastasized clear cell renal cell carcinoma. J. Clin. Oncol 2005, 23, 6540–6548. [Google Scholar]
- Stillebroer, A.B.; Boerman, O.C.; Desar, I.M.; Boers-Sonderen, M.J.; van Herpen, C.M.; Langenhuijsen, J.F.; Smith-Jones, P.M.; Oosterwijk, E.; Oyen, W.J.; Mulders, P.F. Phase 1 radioimmunotherapy study with lutetium 177-labeled anti-carbonic anhydrase IX monoclonal antibody girentuximab in patients with advanced renal cell carcinoma. Eur. Urol. 2012. [Google Scholar] [CrossRef]
- Davis, I.D.; Wiseman, G.A.; Lee, F.T.; Gansen, D.N.; Hopkins, W.; Papenfuss, A.T.; Liu, Z.; Moynihan, T.J.; Croghan, G.A.; Adjei, A.A.; et al. A phase i multiple dose, dose escalation study of cg250 monoclonal antibody in patients with advanced renal cell carcinoma. Cancer Immun 2007, 7, 13. [Google Scholar]
- Bleumer, I.; Knuth, A.; Oosterwijk, E.; Hofmann, R.; Varga, Z.; Lamers, C.; Kruit, W.; Melchior, S.; Mala, C.; Ullrich, S.; et al. A phase ii trial of chimeric monoclonal antibody g250 for advanced renal cell carcinoma patients. Br. J. Cancer 2004, 90, 985–990. [Google Scholar]
- WILEX Ariser, adjuvant rencarex® immunotherapy phase iii trial to study efficacy in non-metastatic rcc. Available online: http://www.wilex.de/portfolio-english/rencarex/phase-iii-ariser/ (accessed on 28 April 2013).
- Davis, I.D.; Liu, Z.; Saunders, W.; Lee, F.T.; Spirkoska, V.; Hopkins, W.; Smyth, F.E.; Chong, G.; Papenfuss, A.T.; Chappell, B.; et al. A pilot study of monoclonal antibody cg250 and low dose subcutaneous il-2 in patients with advanced renal cell carcinoma. Cancer Immun 2007, 7, 14. [Google Scholar]
- Bleumer, I.; Oosterwijk, E.; Oosterwijk-Wakka, J.C.; Voller, M.C.; Melchior, S.; Warnaar, S.O.; Mala, C.; Beck, J.; Mulders, P.F. A clinical trial with chimeric monoclonal antibody wx-g250 and low dose interleukin-2 pulsing scheme for advanced renal cell carcinoma. J. Urol 2006, 175, 57–62. [Google Scholar]
- Siebels, M.; Rohrmann, K.; Oberneder, R.; Stahler, M.; Haseke, N.; Beck, J.; Hofmann, R.; Kindler, M.; Kloepfer, P.; Stief, C. A clinical phase I/II trial with the monoclonal antibody cg250 (rencarex(r)) and interferon-alpha-2a in metastatic renal cell carcinoma patients. World J. Urol 2011, 29, 121–126. [Google Scholar]
- Brouwers, A.H.; Buijs, W.C.; Mulders, P.F.; de Mulder, P.H.; van den Broek, W.J.; Mala, C.; Oosterwijk, E.; Boerman, O.C.; Corstens, F.H.; Oyen, W.J. Radioimmunotherapy with [131I]cg250 in patients with metastasized renal cell cancer: Dosimetric analysis and immunologic response. Clin. Cancer Res 2005, 11, 7178S–7186S. [Google Scholar]
- Sharkey, R.M.; Behr, T.M.; Mattes, M.J.; Stein, R.; Griffiths, G.L.; Shih, L.B.; Hansen, H.J.; Blumenthal, R.D.; Dunn, R.M.; Juweid, M.E.; et al. Advantage of residualizing radiolabels for an internalizing antibody against the b-cell lymphoma antigen, cd22. Cancer Immunol. Immunother 1997, 44, 179–188. [Google Scholar]
- Stillebroer, A.B.; Zegers, C.M.; Boerman, O.C.; Oosterwijk, E.; Mulders, P.F.; O’Donoghue, J.A.; Visser, E.P.; Oyen, W.J. Dosimetric analysis of 177Lu-cg250 radioimmunotherapy in renal cell carcinoma patients: Correlation with myelotoxicity and pretherapeutic absorbed dose predictions based on 111In-cg250 imaging. J. Nucl. Med 2012, 53, 82–89. [Google Scholar]
- Surfus, J.E.; Hank, J.A.; Oosterwijk, E.; Welt, S.; Lindstrom, M.J.; Albertini, M.R.; Schiller, J.H.; Sondel, P.M. Anti-renal-cell carcinoma chimeric antibody g250 facilitates antibody-dependent cellular cytotoxicity with in vitro and in vivo interleukin-2-activated effectors. J. Immunother. Emphasis Tumor Immunol 1996, 19, 184–191. [Google Scholar]
- Liu, Z.; Smyth, F.E.; Renner, C.; Lee, F.T.; Oosterwijk, E.; Scott, A.M. Anti-renal cell carcinoma chimeric antibody g250: Cytokine enhancement of in vitro antibody-dependent cellular cytotoxicity. Cancer Immunol. Immunother 2002, 51, 171–177. [Google Scholar]
- Brouwers, A.H.; Frielink, C.; Oosterwijk, E.; Oyen, W.J.; Corstens, F.H.; Boerman, O.C. Interferons can upregulate the expression of the tumor associated antigen g250-mn/ca IX, a potential target for (radio)immunotherapy of renal cell carcinoma. Cancer Biother. Radiopharm 2003, 18, 539–547. [Google Scholar]
- Bui, M.H.; Seligson, D.; Han, K.R.; Pantuck, A.J.; Dorey, F.J.; Huang, Y.; Horvath, S.; Leibovich, B.C.; Chopra, S.; Liao, S.Y.; et al. Carbonic anhydrase IX is an independent predictor of survival in advanced renal clear cell carcinoma: Implications for prognosis and therapy. Clin. Cancer Res 2003, 9, 802–811. [Google Scholar]
- Bui, M.H.; Visapaa, H.; Seligson, D.; Kim, H.; Han, K.R.; Huang, Y.; Horvath, S.; Stanbridge, E.J.; Palotie, A.; Figlin, R.A.; et al. Prognostic value of carbonic anhydrase IX and ki67 as predictors of survival for renal clear cell carcinoma. J. Urol 2004, 171, 2461–2466. [Google Scholar]
- Atkins, M.; Regan, M.; McDermott, D.; Mier, J.; Stanbridge, E.; Youmans, A.; Febbo, P.; Upton, M.; Lechpammer, M.; Signoretti, S. Carbonic anhydrase ix expression predicts outcome of interleukin 2 therapy for renal cancer. Clin. Cancer Res 2005, 11, 3714–3721. [Google Scholar]
- Dudek, A.Z.; Yee, R.T.; Manivel, J.C.; Isaksson, R.; Yee, H.O. Carbonic anhydrase ix expression is associated with improved outcome of high-dose interleukin-2 therapy for metastatic renal cell carcinoma. Anticancer Res 2010, 30, 987–992. [Google Scholar]
- Smith, I.; Procter, M.; Gelber, R.D.; Guillaume, S.; Feyereislova, A.; Dowsett, M.; Goldhirsch, A.; Untch, M.; Mariani, G.; Baselga, J.; et al. 2-year follow-up of trastuzumab after adjuvant chemotherapy in her2-positive breast cancer: A randomised controlled trial. Lancet 2007, 369, 29–36. [Google Scholar]
- Lamers, C.H.; Sleijfer, S.; Vulto, A.G.; Kruit, W.H.; Kliffen, M.; Debets, R.; Gratama, J.W.; Stoter, G.; Oosterwijk, E. Treatment of metastatic renal cell carcinoma with autologous t-lymphocytes genetically retargeted against carbonic anhydrase IX: First clinical experience. J. Clin. Oncol 2006, 24, e20–e22. [Google Scholar]
- Lamers, C.H.; Sleijfer, S.; van Steenbergen, S.; van Elzakker, P.; van Krimpen, B.; Groot, C.; Vulto, A.; den Bakker, M.; Oosterwijk, E.; Debets, R.; et al. Treatment of metastatic renal cell carcinoma with caix car-engineered t cells: Clinical evaluation and management of on-target toxicity. Mol. Ther 2013, 21, 904–912. [Google Scholar]
- Oosterwijk-Wakka, J.C.; Kats-Ugurlu, G.; Leenders, W.P.; Kiemeney, L.A.; Old, L.J.; Mulders, P.F.; Oosterwijk, E. Effect of tyrosine kinase inhibitor treatment of renal cell carcinoma on the accumulation of carbonic anhydrase IX-specific chimeric monoclonal antibody cg250. BJU Int 2011, 107, 118–125. [Google Scholar]
- Muselaers, S.; Boerman, O.; Stillebroer, A.; Desar, I.; Sonderen, M.; van Herpen, C.; Oosterwijk, E.; Leenders, W.; Mulders, P.; Oyen, W. Sorafenib decreases indium-111-girentuximab tumor uptake in clear cell renal cell carcinoma patients. J. Nuc. Med 2012, 53, 27. [Google Scholar]
- Murri-Plesko, M.T.; Hulikova, A.; Oosterwijk, E.; Scott, A.M.; Zortea, A.; Harris, A.L.; Ritter, G.; Old, L.; Bauer, S.; Swietach, P.; et al. Antibody inhibiting enzymatic activity of tumour-associated carbonic anhydrase isoform IX. Eur. J. Pharmacol 2011, 657, 173–183. [Google Scholar]
| Ref. | Year | Agent | Number of patients | Patients | Outcome # | Remarks |
|---|---|---|---|---|---|---|
| Oosterwijk et al. [28] | 1993 | 131I-mG250 | 15 | Primary RCC | 12/12 pts | Phase I, dose escalation |
| Steffens et al. [30] | 1997 | 131I-cG250 | 16 | Primary RCC | 13/13 pts | Phase I, dose escalation |
| Steffens et al. [31] | 1999 | 131I-cG250 & 111In-cG250 | 10 | Primary RCC | 10/10 pts | Dual label study |
| Brouwers et al. [32] | 2002 | 131I-cG250 vs. 18F-FDG | 20 | M + RCC | 131I-cG250: 34/112 lesions 18F-FDG: 77/112 lesions | Comparative intrapatient study |
| Brouwers et al. [33] | 2003 | 131I-cG250 & 111In-cG250 | 5 | M + RCC | 111In-cG250: 47 lesions 131I-cG250: 30 lesions | Comparative intrapatient study |
| Divgi et al. [34] | 2007 | 124I-cG250 | 26 | Primary RCC | 15/16 ccRCC imaged | Prospective cG250-immunoPET |
| Divgi et al. [35] | 2013 | 124I-cG250 | 226 | Primary RCC | 124/143 ccRCC imaged (sens. & spec. 86%) | Phase III, REDECT trial |
| Muselaers et al. [36] | 2013 | 111In-cG250 | 29 | Primary RCC | 15/16 ccRCC imaged | 111In-cG250 immunoSPECT |
| Ref. | Year | Agent | Number of patients | Patients | Response | Duration Response | Remarks |
|---|---|---|---|---|---|---|---|
| Divgi et al. [29] | 1998 | 131I-mG250 | 33 | M + RCC | 17 SD; 16 PD | 2–3 mo | Phase I/II |
| Steffens et al. [42] | 1999 | 131I-cG250 | 12 | M + RCC | 1 PR; 1 SD; 10 PD | 9+; 3–6 mo | Phase I Activity dose |
| Divgi et al. [43] | 2004 | 131I-cG250 | 15 | M + RCC | 7 SD; 8 PD | 2–11 mo | Phase I fractionated dose |
| Brouwers et al. [44] | 2005 | 131I-cG250 Two doses | 27 | M + RCC | 5 SD; 22 PD | 3–12 mo | Phase I two high doses |
| Stillebroer et al. [45] | 2012 | 177Lu-cG250 Multiple doses | 23 | M + RCC | 1 PR; 17 SD | 9+; 3+ mo | Phase I dose escalation |
| Davis et al. [46] | 2007 | cG250 | 12 | M + RCC | 1 CR; 8 SD; 3 PD | 6–66 wk | Phase I |
| Bleumer et al. [47] | 2004 | cG250 | 36 | M + RCC | 1 CR; 1 PR; 8 SD; 26 PD | 1–20+ wk | Phase II |
| ARISER [48] | cG250 | 864 | High risk, after nephrectomy | No benefit * | Phase III | ||
| Davis et al. [49] | 2007 | cG250 + IL-2 | 9 | M + RCC | 2 SD; 7 PD | 6, 12 wk | Phase I |
| Bleumer et al. [50] | 2006 | cG250 + IL-2 | 35 | M + RCC | 1 PR; 7 SD; 27 PD | 95+; 24+ wk | Phase II |
| Siebels et al. [51] | 2011 | cG250 + IFN-2α | 31 | M + RCC | 1 CR; 9 SD | 17+; 24+ wk | Phase II |
© 2013 by the authors; licensee MDPI, Basel, Switzerland This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution license ( http://creativecommons.org/licenses/by/3.0/).
Share and Cite
Oosterwijk-Wakka, J.C.; Boerman, O.C.; Mulders, P.F.A.; Oosterwijk, E. Application of Monoclonal Antibody G250 Recognizing Carbonic Anhydrase IX in Renal Cell Carcinoma. Int. J. Mol. Sci. 2013, 14, 11402-11423. https://doi.org/10.3390/ijms140611402
Oosterwijk-Wakka JC, Boerman OC, Mulders PFA, Oosterwijk E. Application of Monoclonal Antibody G250 Recognizing Carbonic Anhydrase IX in Renal Cell Carcinoma. International Journal of Molecular Sciences. 2013; 14(6):11402-11423. https://doi.org/10.3390/ijms140611402
Chicago/Turabian StyleOosterwijk-Wakka, Jeannette C., Otto C. Boerman, Peter F. A. Mulders, and Egbert Oosterwijk. 2013. "Application of Monoclonal Antibody G250 Recognizing Carbonic Anhydrase IX in Renal Cell Carcinoma" International Journal of Molecular Sciences 14, no. 6: 11402-11423. https://doi.org/10.3390/ijms140611402




