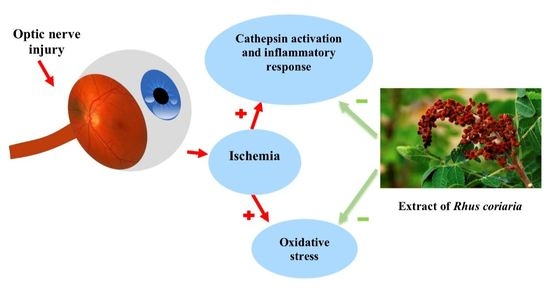
Neuroprotective and Anti-Inflammatory Effects of Rhus coriaria Extract in a Mouse Model of Ischemic Optic Neuropathy
Abstract
:1. Introduction
2. Experimental Section
2.1. Collection and Authentication of the Herb
2.2. Preparation of R. coriaria Extract
2.3. Antioxidant Capacity Assays
2.3.1. ABTS (2,2′-Azino-Bis(3-Ethylbenzothiazoline-6-Sulphonic Acid) Radical Scavenging Assay
2.3.2. DPPH (2-Diphenyl-1-Picrylhydrazyl) Scavenging Assay
2.3.3. B-Carotene Bleaching Assay
2.4. Characterization of the Extract
2.4.1. Estimation of Total Phenolic Content
2.4.2. Total Flavonoids Assay
2.4.3. Gas Chromatography-Mass Spectrometry (GC-MS) Screening
2.5. In Vivo Study of the Mouse Ischemic Optic Neuropathy Model
2.5.1. Animal Studies
2.5.2. Animal Treatment
2.5.3. Optic Nerve Crush Injury
2.5.4. Fluorescence Molecular Tomography (FMT) Imaging
2.6. Statistical Analysis
3. Results
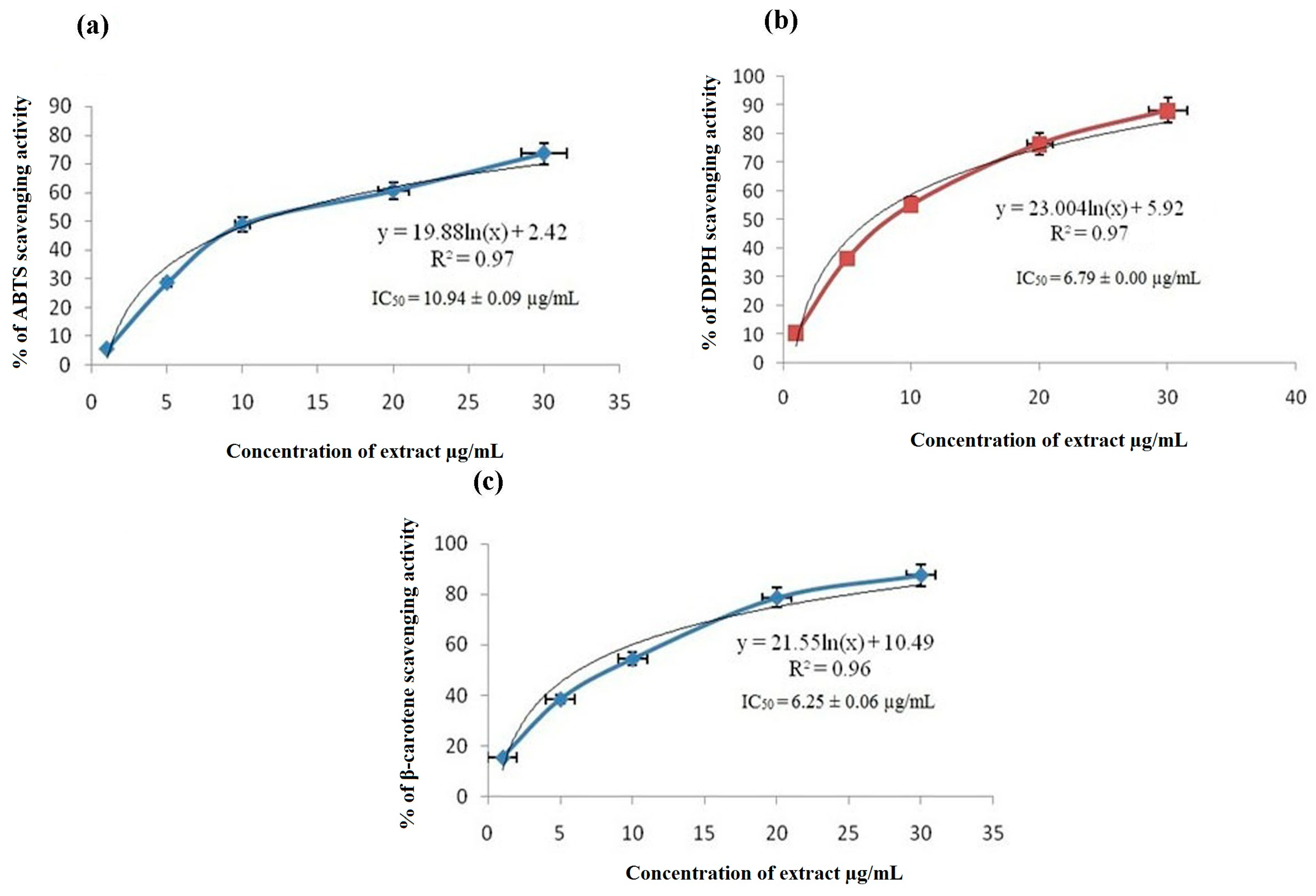
3.1. ABTS Radical Scavenging Assay
3.2. DPPH Scavenging Assay
3.3. β-Carotene Bleaching Assay
3.4. Assays for Total Phenolics and Total Flavonoids Content
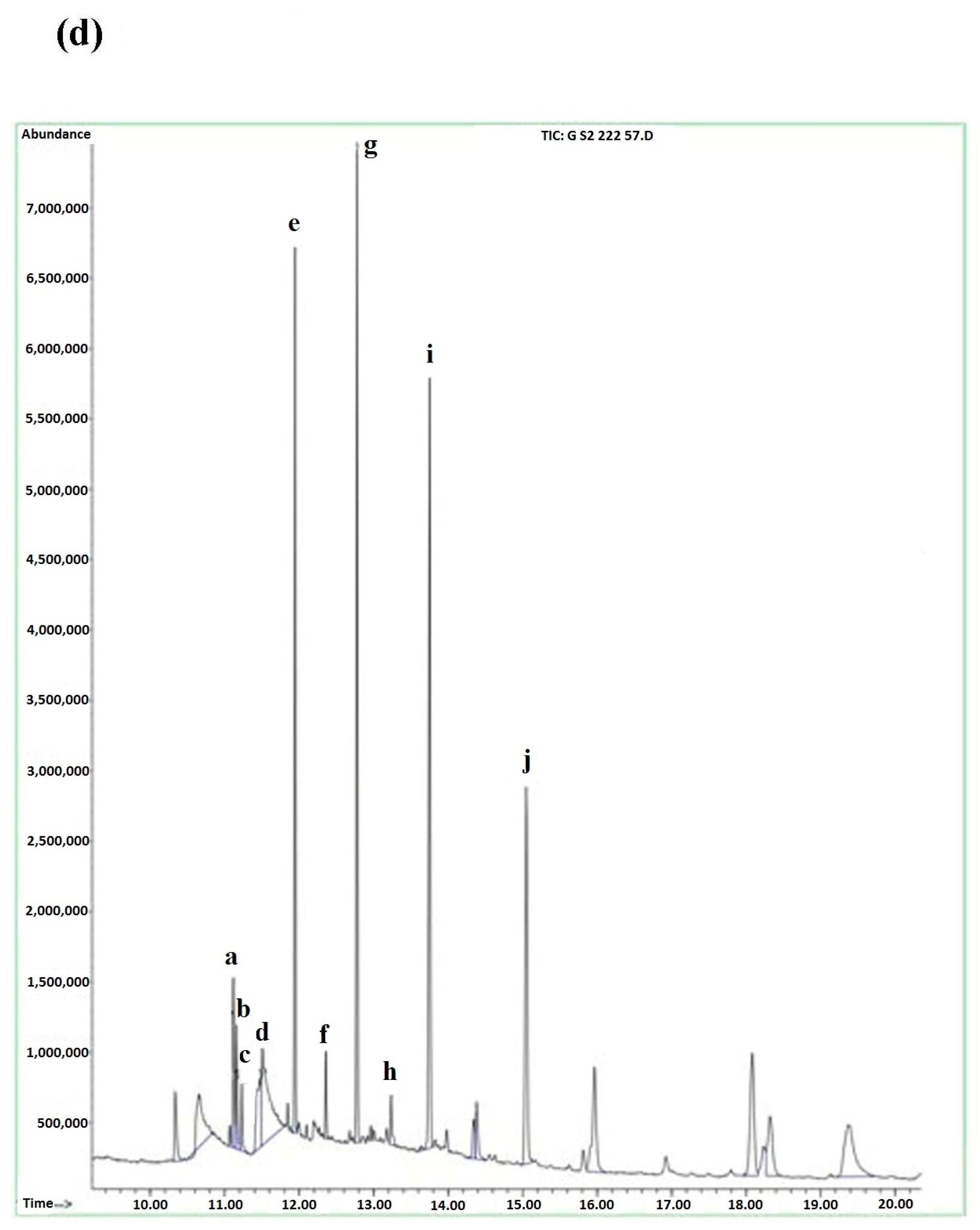
3.5. GC-MS
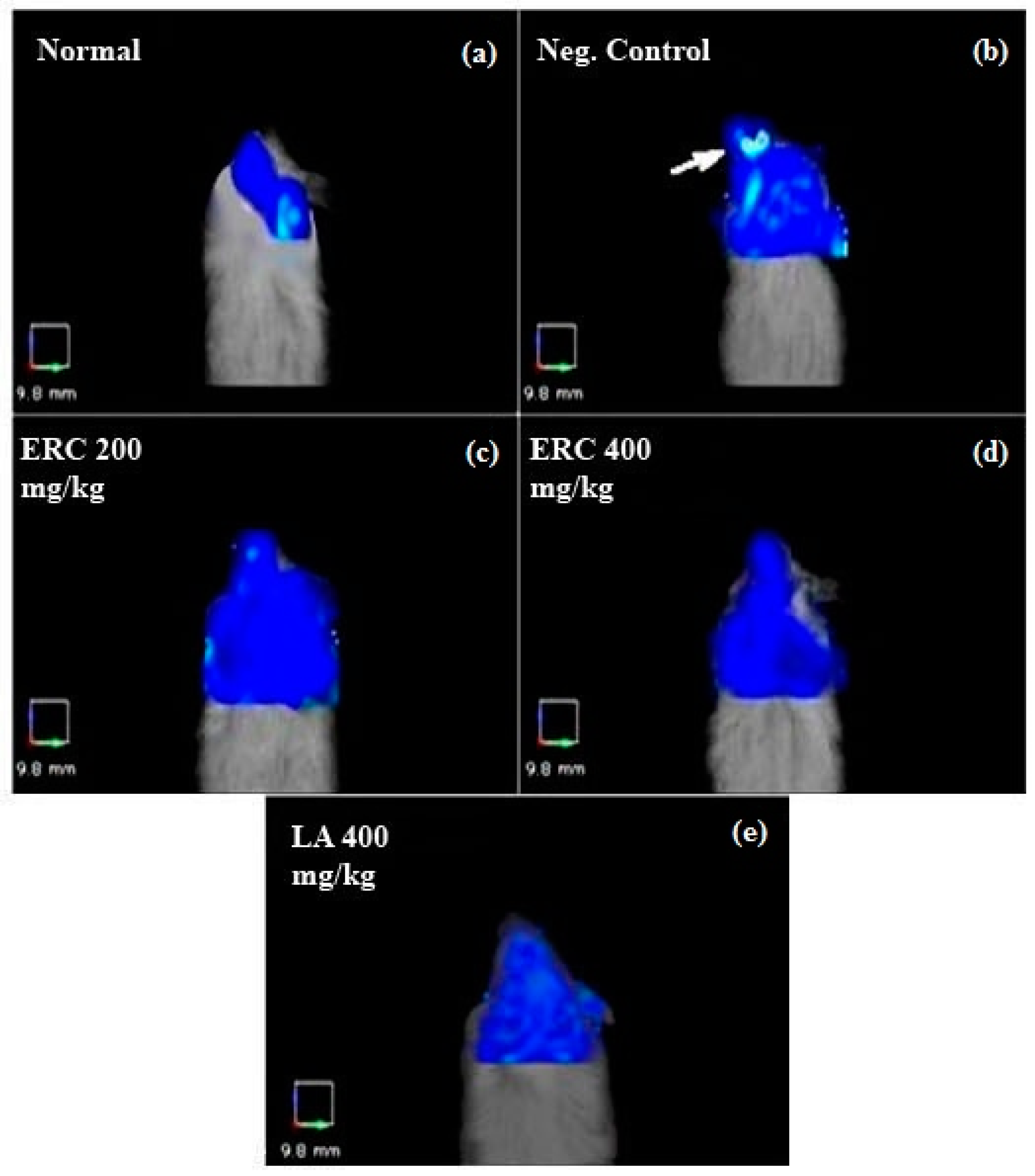
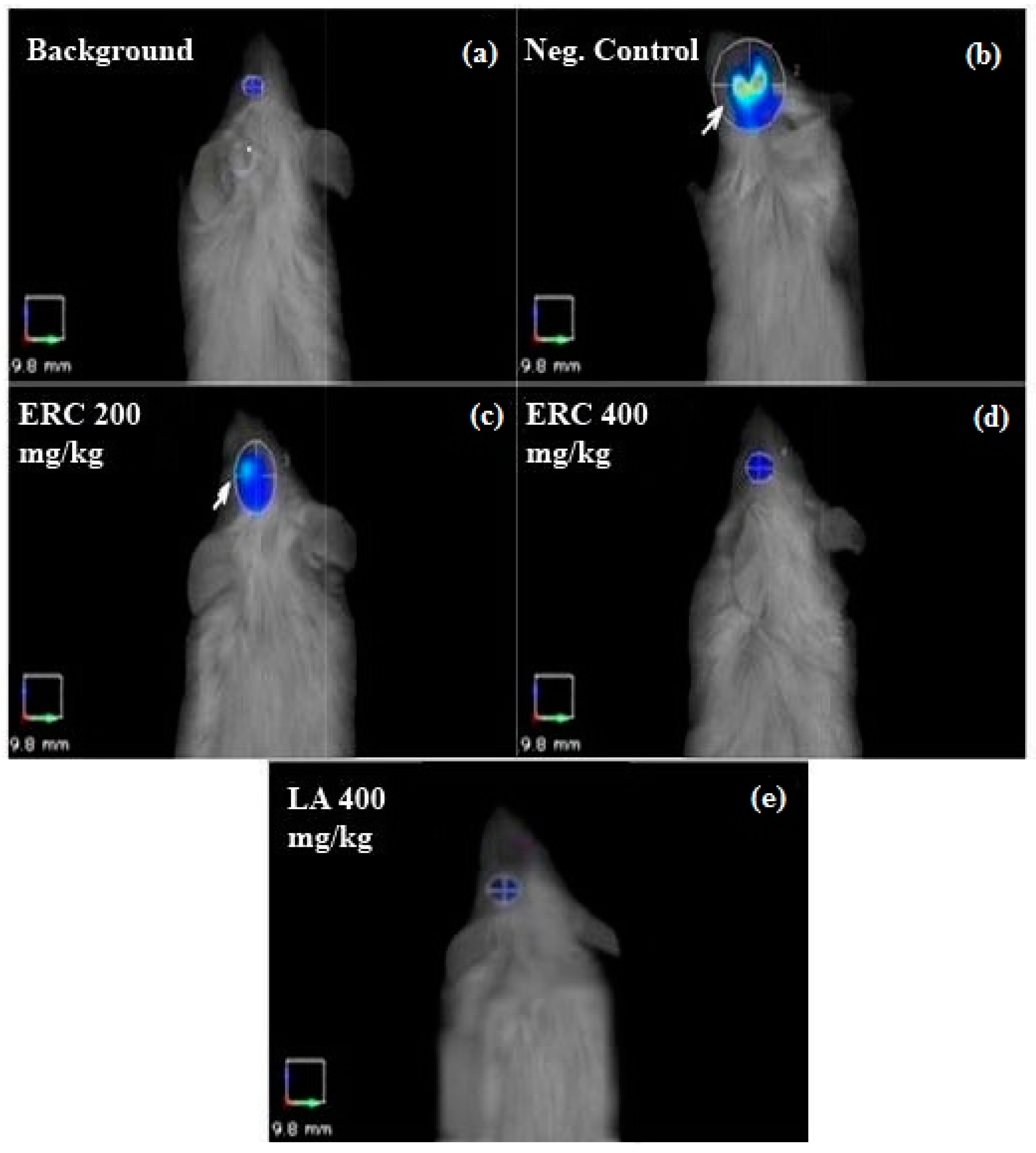
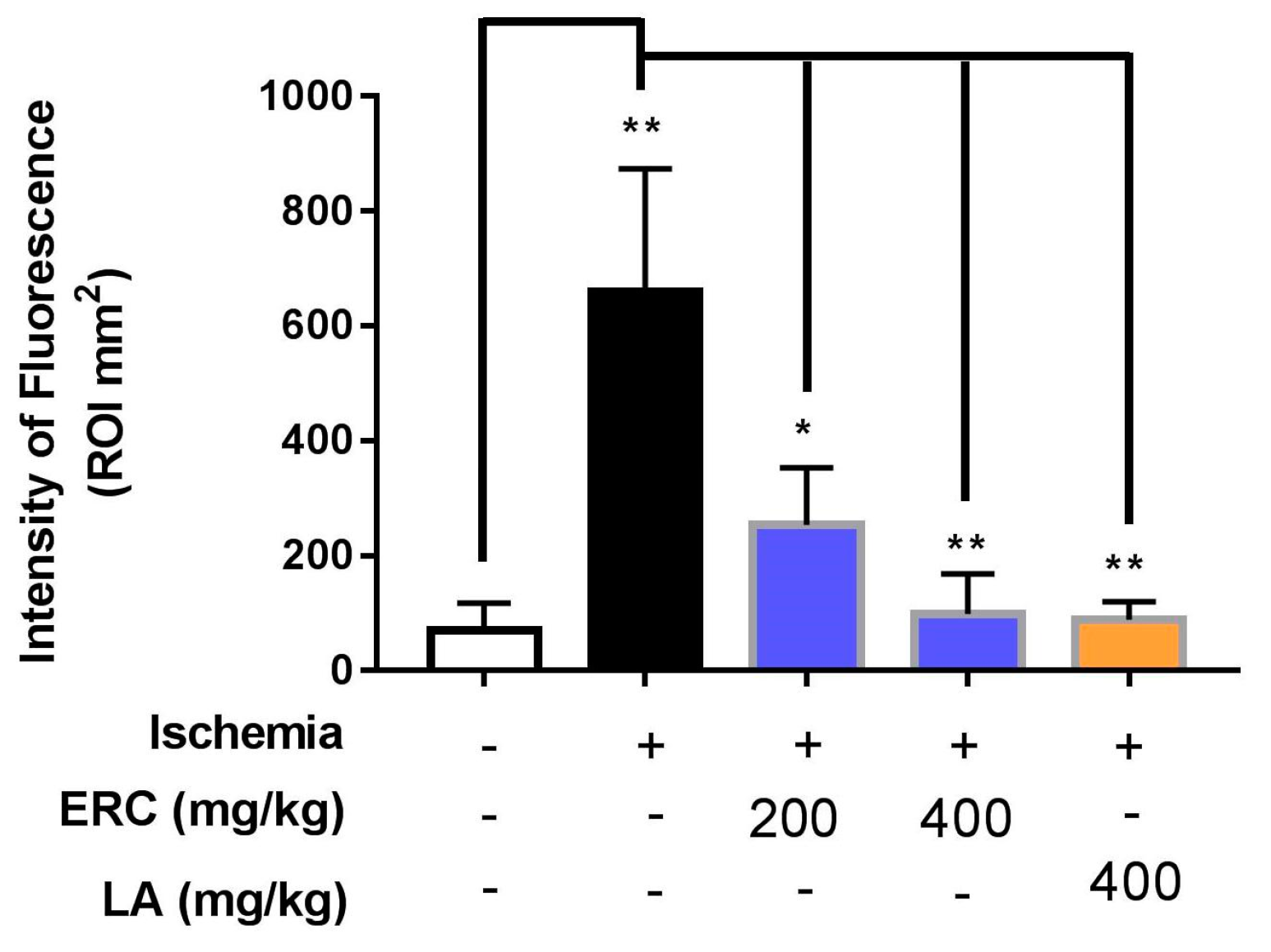
3.6. FMT Imaging
4. Discussion
5. Conclusions
Acknowledgments
Author Contributions
Conflicts of Interest
References
- Khalilpour, S.; Latifi, S.; Behnammanesh, G.; Majid, A.M.S.A.; Majid, A.S.A.; Tamayol, A. Ischemic optic neuropathy as a model of neurodegenerative disorder: A review of pathogenic mechanism of axonal degeneration and the role of neuroprotection. J. Neurol. Sci. 2017, 375, 430–441. [Google Scholar] [CrossRef] [PubMed]
- Biousse, V.; Bousser, M.; Schaison, M. Normal pressure pseudotumor cerebri. J. Neuroophthalmol. 1997, 17, 279–280. [Google Scholar] [CrossRef] [PubMed]
- Levin, L.A.; Gordon, G.L. Retinal ganglion cell disorders: Types of treatement. Exp. Eye Res. 2002, 21, 465–484. [Google Scholar] [CrossRef]
- Jang, S.; Soto, J.; Agostini, B.; Javadov, S. Role of C-jun N-terminal kinase in the mitochondria of ischemia-reperfusion injury of isolated heart (LB648). FASEB J. 2014, 28, LB648. [Google Scholar]
- Khalilpour, S.; Behnammanesh, G.; Majid, A.M.S.A.; Tamayol, A.; Majid, A.S.A. Assessment of neuroprotective properties of Rhus coriaria L. Ethanol extract in an in vitro model of retinal degeneration. J. Herb. Med. 2017, 10, 45–52. [Google Scholar] [CrossRef]
- Conus, S.; Perozzo, R.; Reinheckel, T.; Peters, C.; Scapozza, L.; Yousefi, S.; Simon, H.-U. Caspase-8 is activated by cathepsin D initiating neutrophil apoptosis during the resolution of inflammation. J. Exp. Med. 2008, 205, 685–698. [Google Scholar] [CrossRef] [PubMed]
- Hobson, M.J.; Zingarelli, B. Ischemia-reperfusion injury. In Pediatric Critical Care Medicine; Springer: London, UK, 2014; pp. 251–268. [Google Scholar]
- Osborne, N.N.; Ji, D.; Majid, A.S.A.; Fawcett, R.J.; Sparatore, A.; Del Soldato, P. ACS67, a hydrogen sulfide–releasing derivative of latanoprost acid, attenuates retinal ischemia and oxidative stress to RGC-5 cells in culture. Investig. Ophthalmol. Vis. Sci. 2010, 51, 284–294. [Google Scholar] [CrossRef] [PubMed]
- Majid, A.S.A.; Yin, Z.Q.; Ji, D. Sulphur antioxidants inhibit oxidative stress induced retinal ganglion cell death by scavenging reactive oxygen species but influence nuclear factor (erythroid-derived 2)-like 2 signalling pathway differently. Biol. Pharmaceut. Bull. 2013, 36, 1095–1110. [Google Scholar] [CrossRef]
- Aquilano, K.; Baldelli, S.; Rotilio, G.; Ciriolo, M.R. Role of nitric oxide synthases in parkinson’s disease: A review on the antioxidant and anti-inflammatory activity of polyphenols. Neurochem. Res. 2008, 33, 2416–2426. [Google Scholar] [CrossRef] [PubMed]
- Tabana, Y.M.; Al-Suede, F.S.R.; Ahamed, M.B.K.; Dahham, S.S.; Hassan, L.E.A.; Khalilpour, S.; Taleb-Agha, M.; Sandai, D.; Majid, A.S.A.; Majid, A.M.S.A. Cat’s whiskers (Orthosiphon stamineus) tea modulates arthritis pathogenesis via the angiogenesis and inflammatory cascade. BMC Complement. Altern. Med. 2016, 16, 480. [Google Scholar] [CrossRef] [PubMed]
- Behnammanesh, G.; Khalilpour, S.; Majid, A.S.A.; Majid, A.M.S.A. Pharmacological actions and potential neuroprotective effects of Rhus coriaria L. and Echium amoenum L.: A brief review. WebmedCentral Pharmacol. 2015, 6, WMC005008. [Google Scholar]
- Abu-Reidah, I.M.; Jamous, R.M.; Ali-Shtayeh, M.S. Phytochemistry, pharmacological properties and industrial applications of Rhus coriaria L. (sumac). Jordan J. Biol. Sci. 2014, 7, 233–244. [Google Scholar] [CrossRef]
- Roberta, R.; Nicoletta, P.; Anna, P.; Ananth, P.; MinRice, Y.; Catherine, E. Antioxidant activity applying an improved abts radical cation decolorization assay. Free Radic. Biol. Med. 1999, 26, 1231–1237. [Google Scholar]
- Mensor, L.L.; Menezes, F.S.; Leitão, G.G.; Reis, A.S.; Santos, T.C.D.; Coube, C.S.; Leitão, S.G. Screening of brazilian plant extracts for antioxidant activity by the use of dpph free radical method. Phytother. Res. 2001, 15, 127–130. [Google Scholar] [CrossRef] [PubMed]
- Sun, T.H.; Ho, C.-T. Antioxidant activities of buckwheat extracts. Food Chem. 2005, 90, 743–749. [Google Scholar] [CrossRef]
- Dewanto, V.; Wu, X.; Adom, K.K.; Liu, R.H. Thermal processing enhances the nutritional value of tomatoes by increasing total antioxidant activity. J. Agric. Food Chem. 2002, 50, 3010–3014. [Google Scholar] [CrossRef] [PubMed]
- Wetwitayaklung, P.; Thavanapong, N.; Charoenteeraboon, J. Chemical constituents and antimicrobial activity of essential oil and extracts of heartwood of aquilaria crassna obtained from water distillation and supercritical fluid carbon dioxide extraction. Silpakorn Univ. Sci. Technol. J. 2009, 3, 25–33. [Google Scholar]
- Miyake, K.-I.; Yoshida, M.; Inoue, Y.; Hata, Y. Neuroprotective effect of transcorneal electrical stimulation on the acute phase of optic nerve injury. Investig. Ophthalmol. Vis. Sci. 2007, 48, 2356–2361. [Google Scholar] [CrossRef] [PubMed]
- McCann, C.M.; Waterman, P.; Figueiredo, J.L.; Aikawa, E.; Weissleder, R.; Chen, J.W. Combined magnetic resonance and fluorescence imaging of the living mouse brain reveals glioma response to chemotherapy. Neuroimage 2009, 45, 360–369. [Google Scholar]
- Houghton, P.J.; Raman, A. Laboratory Handbook for the Fractionation of Natural Extracts; Chapman & Hall: London, UK, 1998; pp. 1–7. [Google Scholar]
- Asgarpanah, J.; Saati, S. An overview on phytochemical and pharmacological properties of Rhus coriaria L. Res. J. Pharmacogn. 2014, 1, 47–54. [Google Scholar]
- Ardalani, H.; Hassanpour Moghadam, M.; Hadipanah, A.; Fotovat, F.; Azizi, A.; Soltani, J. Identification and characterization of chemical composition in Rhus coriaria L. J. Herb. Drugs 2015, 6, 93–100. [Google Scholar]
- Murali, H.S.; Mohan, M.S.; Mania, K.S.; Sankaran, R. Polar and nonpolar lipids and their fatty acid composition of a few fusarium species. JAOCS 1993, 70, 1039–1041. [Google Scholar] [CrossRef]
- Kumar, G.P.; Khanum, F. Neuroprotective potential of phytochemicals. Pharmacogn. Rev. 2012, 6, 81–90. [Google Scholar] [CrossRef] [PubMed]
- Botelho, J.R.S.; Medeiros, N.G.; Rodrigues, A.; Araújo, M.E.; Machado, N.T.; Guimarães Santos, A.; Santos, I.R.; Gomes-Leal, W.; Carvalho Junior, R.N. Black sesame (Sesamum Indicum L.) seeds extracts by CO2 supercritical fluid yield, kinetics data, total fatty acids, phytosterols and neuroprotective effects. J. Supercrit. Fluids 2014, 93, 49–55. [Google Scholar] [CrossRef]
- Dratviman-Storobinsky, O.; Hasanreisoglu, M.; Offen, D.; Barhum, Y.; Weinberger, D.; Goldenberg-Cohen, N. Progressive damage along the optic nerve following induction of crush injury or rodent anterior ischemic optic neuropathy in transgenic mice. Mol. Vis. 2008, 14, 2171–2179. [Google Scholar] [PubMed]
- PerkinElmer, I. Perkinelmer for the Better. Available online: http://www.perkinelmer.com/catalog/product/id/nev11171 (accessed on 20 April 2018).
- Conus, S.; Simon, H.U. Cathepsins: Key modulators of cell death and inflammatory responses. Biochem. Pharmacol. 2008, 76, 1374–1382. [Google Scholar] [CrossRef] [PubMed]
- Nguyen, C.T.; Bui, B.V.; Sinclair, A.J.; Vingrys, A.J. Dietary omega 3 fatty acids decrease intraocular pressure with age by increasing aqueous outflow. Investig. Ophthalmol. Vis. Sci. 2007, 48, 756–762. [Google Scholar] [CrossRef] [PubMed]
| Test Sample | Total Phenolics (µg GAE/g) | Total Flavonoids (µg QE/g) |
|---|---|---|
| ERC | 9353 ± 83 | 1393 ± 32 |
| Peak | Compound | Ref | Quality | Peak Height | R.T. Min | % Area | RI |
|---|---|---|---|---|---|---|---|
| a | Tricosane | 114376 | 99 | 1,192,748 | 11.118 | 2.65% | 1408.8 |
| b | Heptacosane | 113306 | 99 | 826,548 | 11.16 | 1.87% | 1496.4 |
| c | Nonacosane | 116666 | 98 | 451,294 | 11.229 | 1.03% | 1632.8 |
| d | Octadecane | 106289 | 95 | 680,873 | 11.514 | 7.85% | 2195 |
| e | Campesterol | 130016 | 97 | 5,389,423 | 11.944 | 9.32% | 2298.8 |
| f | 8,11-Octadecadienoic acid, methyl ester | 136481 | 97 | 607,878 | 12.361 | 1.10% | 2398.4 |
| g | γ-Sitosterol | 136487 | 98 | 6,507,080 | 12.777 | 11.95% | 2497.9 |
| h | 9,12,15-Octadecatrienoic acid, methyl ester | 91035 | 96 | 331,695 | 13.235 | 0.90% | 2599.5 |
| i | Linoleicacid (LA) (9,12-Octadecadienoic acid (Z,Z)-) | 151555 | 99 | 5,171,060 | 13.756 | 12.39% | 2697.9 |
| j | Stigmasta-5,24(28)-dien-3-ol | 158131 | 99 | 2,634,496 | 15.054 | 8.95% | 2945.6 |
| Test | Fluorescenceintensity (mm2) (Mean) | SEM | % Inhibition Ofischemia |
|---|---|---|---|
| Normal control | 69.66 | 48.56 | — |
| Ischemia (negative control) | 659.32 | 123.57 | — |
| ERC 200 mg/kg | 253.56 | 57.64 | 61.54 |
| ERC 400 mg/kg | 99.30 | 40.28 | 84.87 |
| LA 400 mg/kg | 87.20 | 50.12 | 86.71 |
© 2018 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Khalilpour, S.; Behnammanesh, G.; Suede, F.; Ezzat, M.O.; Muniandy, J.; Tabana, Y.; Ahamed, M.B.K.; Tamayol, A.; Majid, A.M.S.; Sangiovanni, E.; et al. Neuroprotective and Anti-Inflammatory Effects of Rhus coriaria Extract in a Mouse Model of Ischemic Optic Neuropathy. Biomedicines 2018, 6, 48. https://doi.org/10.3390/biomedicines6020048
Khalilpour S, Behnammanesh G, Suede F, Ezzat MO, Muniandy J, Tabana Y, Ahamed MBK, Tamayol A, Majid AMS, Sangiovanni E, et al. Neuroprotective and Anti-Inflammatory Effects of Rhus coriaria Extract in a Mouse Model of Ischemic Optic Neuropathy. Biomedicines. 2018; 6(2):48. https://doi.org/10.3390/biomedicines6020048
Chicago/Turabian StyleKhalilpour, Saba, Ghazaleh Behnammanesh, Fouad Suede, Mohammed O. Ezzat, Jayadhisan Muniandy, Yasser Tabana, Mohamed B. K. Ahamed, Ali Tamayol, Amin Malik Shah Majid, Enrico Sangiovanni, and et al. 2018. "Neuroprotective and Anti-Inflammatory Effects of Rhus coriaria Extract in a Mouse Model of Ischemic Optic Neuropathy" Biomedicines 6, no. 2: 48. https://doi.org/10.3390/biomedicines6020048