Development and in Vitro Characterization of Photochemically Crosslinked Polyvinylpyrrolidone Coatings for Drug-Coated Balloons
Abstract
:1. Introduction
2. Experimental Section
2.1. Materials
2.2. Coating
2.2.1. Coating of Glass Cover Slips with PVP and/or PTX
2.2.2. Coating of Balloon Catheters
2.2.3. Crosslinking Conditions
2.2.4. Incorporation of PTX via Pipetting
2.3. Characterization
2.3.1. Scanning Electron Microscopy
2.3.2. Coating Stability after Crosslinking
2.3.3. Oven-Based Karl Fischer (KF) Titration
2.3.4. PTX Recovery after Crosslinking
2.3.5. PTX Wash off, Transfer, Residual and Total Load
2.3.6. Simulated Use
2.3.7. Analysis of PTX Wash off and Transfer during Simulated Use
2.3.8. HPLC Parameter
3. Results and Discussion
3.1. Development and in Vitro Characterization of PVP-Coated DCB in Dependence of Crosslinking Conditions

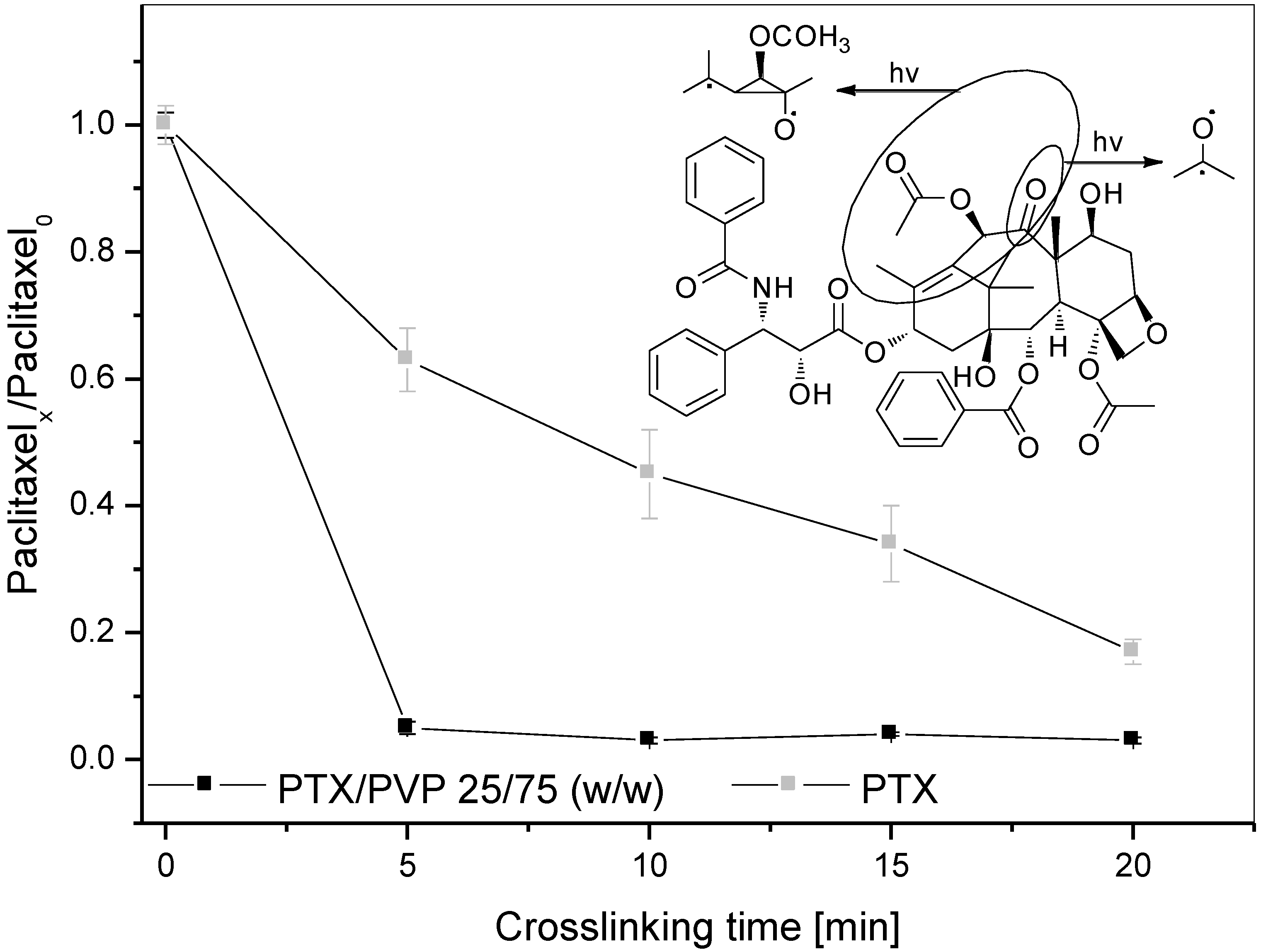

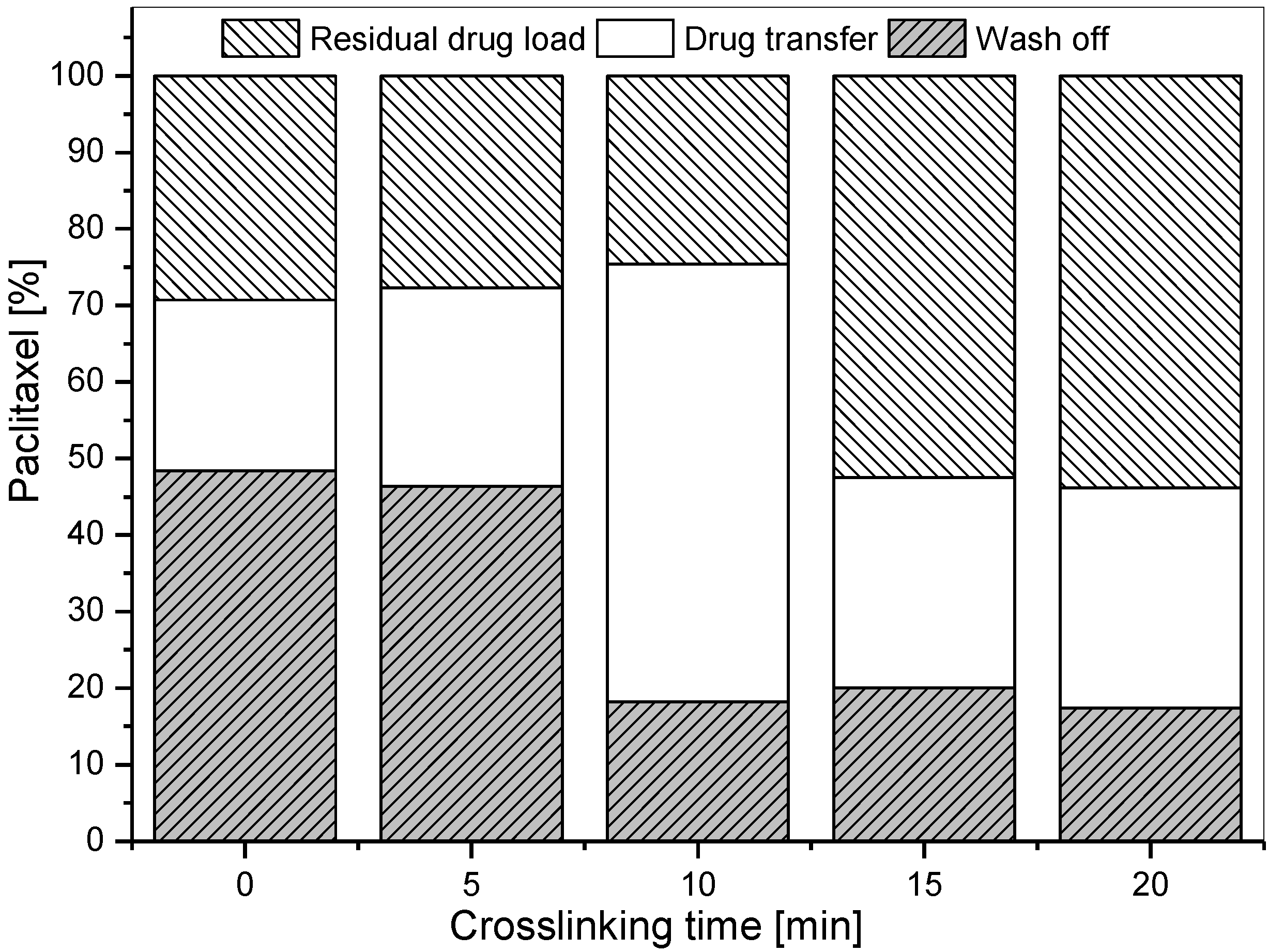
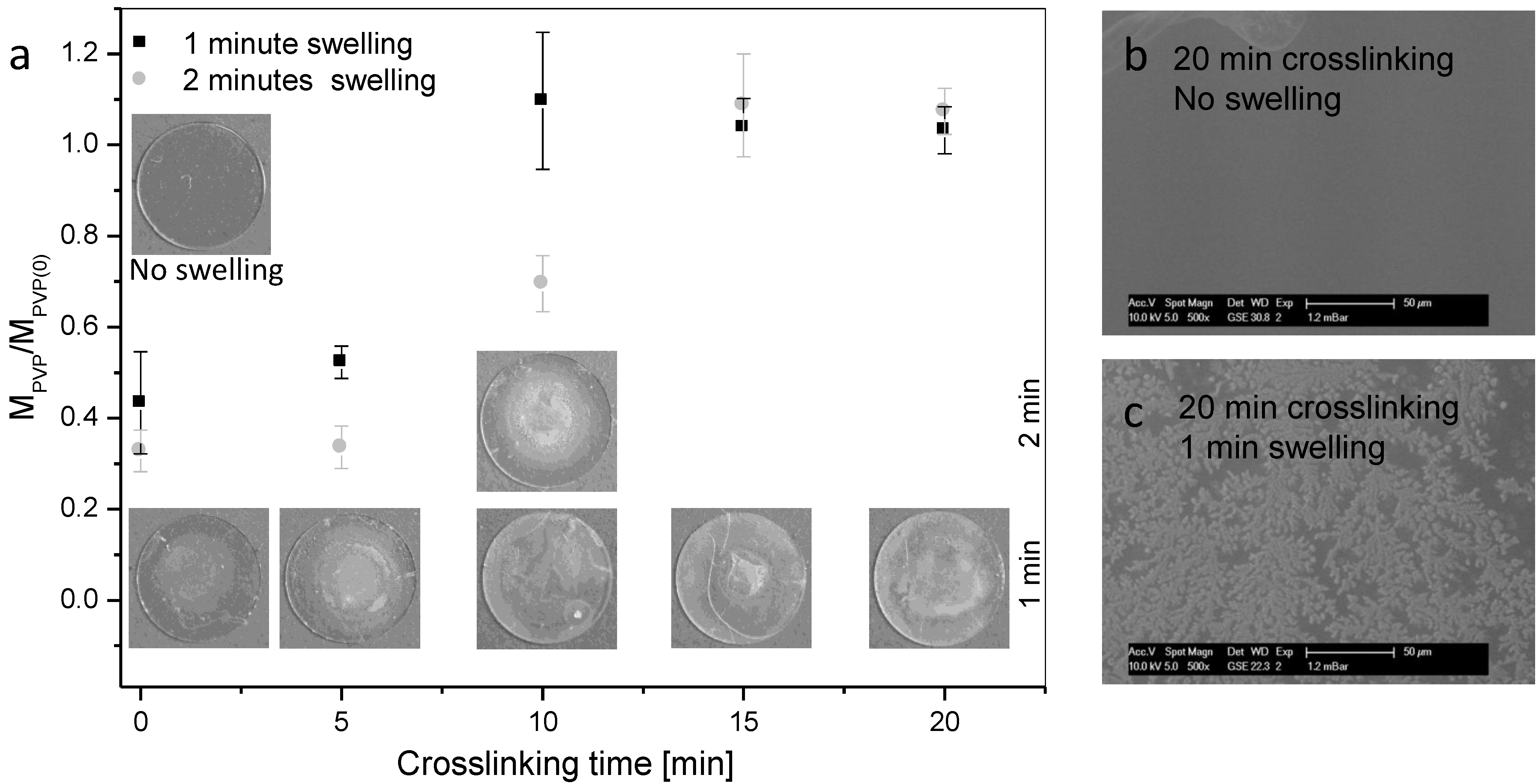
| Crosslinking time (min) | 1 min immersion | 2 min immersion |
|---|---|---|
| 0 | 3.83 ± 0.30 | 3.65 ± 0.46 |
| 5 | 3.47 ± 0.41 | 6.17 ± 0.57 |
| 10 | 7.46 ± 1.42 | 12.22 ± 4.36 |
| 15 | 6.85 ± 1.74 | 16.59 ± 2.36 |
| 20 | 6.56 ± 1.74 | 16.53 ± 1.29 |
3.2. Simulated Use of PVP-Coated DCB
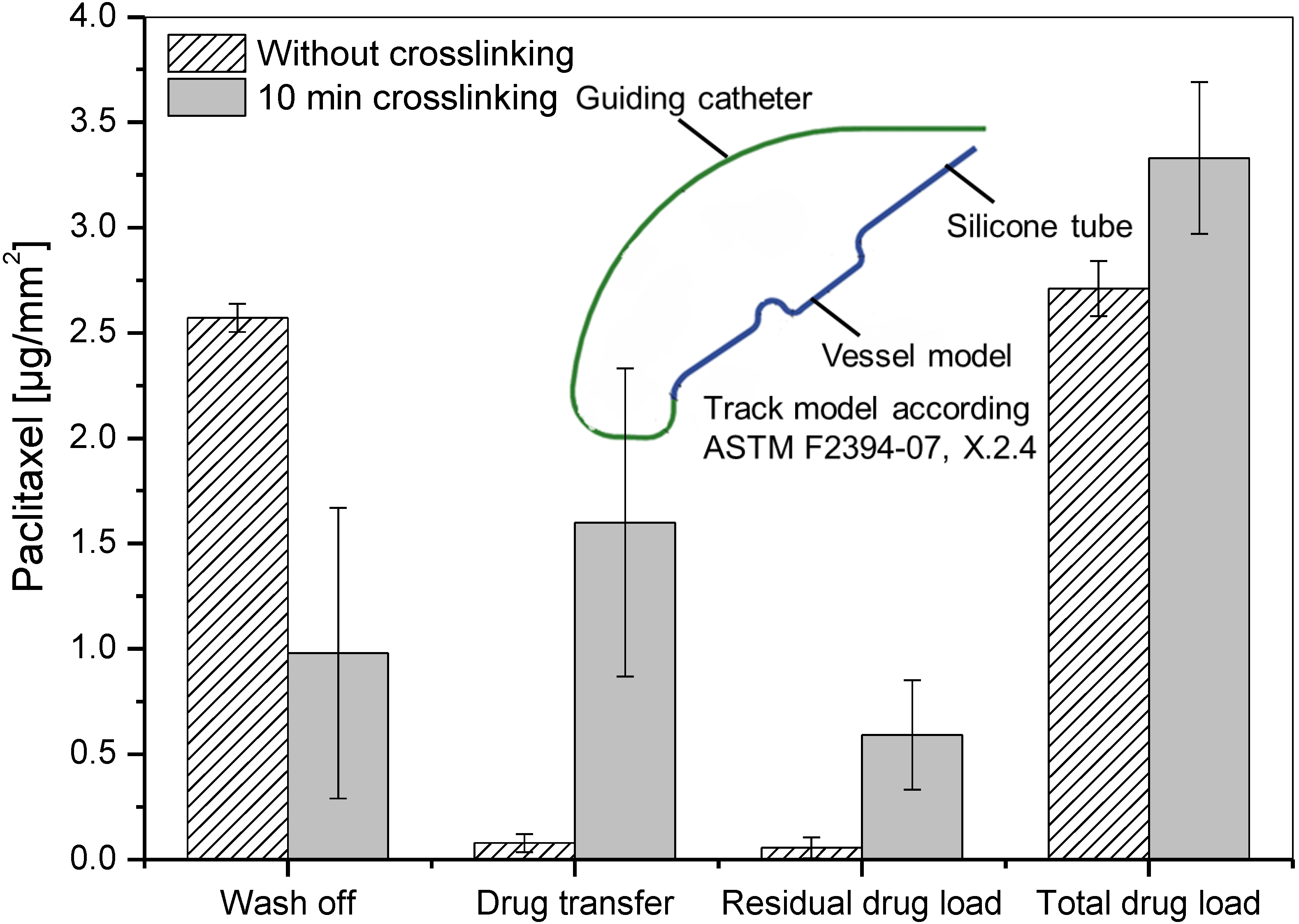
4. Conclusions
Acknowledgments
Conflicts of Interest
References
- Deloose, K.; Lauwers, K.; Callaert, J.; Maene, L.; Keirse, K.; Verbist, J.; Peeters, P.; Bosiers, M. Drug-eluting technologies in femoral artery lesions. J. Cardiovasc. Surg. 2013, 54, 217–224. [Google Scholar]
- Buechel, R.; Stirnimann, A.; Zimmer, R.; Keo, H.; Groechenig, E. Drug-eluting stents and drug-coated balloons in peripheral artery disease. VASA 2012, 41, 248–261. [Google Scholar] [CrossRef]
- De Labriolle, A.; Pakala, R.; Bonello, L.; Lemesle, G.; Scheinowitz, M.; Waksman, R. Paclitaxel-eluting balloon: From bench to bed. Catheter. Cardiovasc. Interv. 2009, 73, 643–652. [Google Scholar] [CrossRef]
- Waksman, R.; Pakala, R. Drug-eluting balloon: The comeback kid? Circ. Cardiovasc. Interv. 2009, 2, 352–358. [Google Scholar] [CrossRef]
- Baumbach, A.; Herdeg, C.; Kluge, M.; Oberhoff, M.; Lerch, M.; Haase, K.K.; Wolter, C.; Schröder, S.; Karsch, K.R. Local drug delivery: Impact of pressure, substance characteristics, and stenting on drug transfer into the arterial wall. Catheter. Cardiovasc. Interv. 1999, 47, 102–106. [Google Scholar] [CrossRef]
- Scheller, B.; Speck, U.; Romeike, B.; Schmitt, A.; Sovak, M.; Böhm, M.; Stoll, H.-P. Contrast media as carriers for local drug delivery successful inhibition of neointimal proliferation in the porcine coronary stent model. Eur. Heart. J. 2003, 24, 1462–1467. [Google Scholar] [CrossRef]
- Cremers, B.; Clever, Y.; Schaffner, S.; Speck, U.; Böhm, M.; Scheller, B. Treatment of coronary in-stent restenosis with a novel paclitaxel urea coated balloon. Minerva Cardioangiol. 2010, 58, 583–588. [Google Scholar]
- Joner, M.; Byrne, R.A.; Lapointe, J.-M.; Radke, P.W.; Bayer, G.; Steigerwald, K.; Wittchow, E. Comparative assessment of drug-eluting balloons in an advanced porcine model of coronary restenosis. Thromb. Haemost. 2011, 105, 864–872. [Google Scholar] [CrossRef]
- Cortese, B.; Bertoletti, A. Paclitaxel coated balloons for coronary artery interventions: A comprehensive review of preclinical and clinical data. Int. J. Cardiol. 2012, 161, 4–12. [Google Scholar] [CrossRef]
- Sternberg, K.; Grabow, N.; Petersen, S.; Weitschies, W.; Harder, C.; Ince, H.; Kroemer, H.K.; Schmitz, K.-P. Advances in coronary stent technology—Active drug-loaded stent surfaces for prevention of restenosis and improvement of biocompatibility. Curr. Pharm. Biotechnol. 2013, 14, 76–90. [Google Scholar]
- Kelsch, B.; Scheller, B.; Biedermann, M.; Clever, Y.P.; Schaffner, S.; Mahnkopf, D.; Speck, U.; Cremers, B. Dose response to Paclitaxel-coated balloon catheters in the porcine coronary overstretch and stent implantation model. Invest. Radiol. 2011, 46, 255–263. [Google Scholar] [CrossRef]
- Berg, M.C.; Kolodziej, H.; Cremers, B.; Gershony, G.; Speck, U. Drug-coated angioplasty balloon catheters: Coating compositions and methods. Adv. Eng. Mater. 2012, 14, B45–B50. [Google Scholar] [CrossRef]
- Kallmes, D.F.; McGraw, J.K.; Evans, A.J.; Mathis, J.M.; Hergenrother, R.W.; Jensen, M.E.; Cloft, H.J.; Lopes, M.; Dion, J.E. Thrombogenicity of hydrophilic and nonhydrophilic microcatheters and guiding catheters. AJNR Am. J. Neuroradiol. 1997, 18, 1243–1251. [Google Scholar]
- Nagaoka, S.; Akashi, R. Low-friction hydrophilic surface for medical devices. Biomaterials 1990, 11, 419–424. [Google Scholar] [CrossRef]
- Babcock, D.E.; Hergenrother, R.W.; Craig, D.A.; Kolodgie, F.D.; Virmani, R. In vivo distribution of particulate matter from coated angioplasty balloon catheters. Biomaterials 2013, 34, 3196–3205. [Google Scholar] [CrossRef]
- Robinson, B.V. PVP: A Critical Review of the Kinetics and Toxicology of Polyvinylprrolidone (Povidone); Taylor & Francis: London, UK, 1990. [Google Scholar]
- Barros, J.A.G.; Fechine, G.J.M.; Alcantara, M.R.; Catalani, L.H. Poly(N-vinyl-2-pyrrolidone) hydrogels produced by Fenton reaction. Polymer 2006, 47, 8414–8419. [Google Scholar] [CrossRef]
- Rosiak, J.; Olejniczak, J.; Pȩkala, W. Fast reaction of irradiated polymers—I. Crosslinking and degradation of polyvinylpyrrolidone. Int. J. Radiat. Appl. Instrum. C 1990, 36, 747–755. [Google Scholar]
- Henglein, A. Crosslinking of polymers in solution under the influence of gamma radiation. J. Phys. Chem. 1959, 63, 1852–1858. [Google Scholar] [CrossRef]
- Lopérgolo, L.C.; Lugão, A.B.; Catalani, L.H. Direct UV photocrosslinking of poly(N-vinyl-2-pyrrolidone) (PVP) to produce hydrogels. Polymer 2003, 44, 6217–6222. [Google Scholar] [CrossRef]
- Speck, U.; Scheller, B.; Abramjuk, C.; Breitwieser, C.; Dobberstein, J.; Boehm, M.; Hamm, B. Neointima inhibition: Comparison of effectiveness of non–stent-based local drug delivery and a drug-eluting stent in porcine coronary arteries1. Radiology 2006, 240, 411–418. [Google Scholar] [CrossRef]
- Scheller, B.; Hehrlein, C.; Bocksch, W.; Rutsch, W.; Haghi, D.; Dietz, U.; Böhm, M.; Speck, U. Treatment of coronary in-stent restenosis with a paclitaxel-coated balloon catheter. N. Engl. J. Med. 2006, 355, 2113–2124. [Google Scholar] [CrossRef]
- Scheller, B.; Hehrlein, C.; Bocksch, W.; Rutsch, W.; Haghi, D.; Dietz, U.; Böhm, M.; Speck, U. Two year follow-up after treatment of coronary in-stent restenosis with a paclitaxel-coated balloon catheter. Clin. Res. Cardiol. 2008, 97, 773–781. [Google Scholar] [CrossRef]
- Schmidt, W.; Lanzer, P. Instrumentation. In Catheter-Based Cardiovascular Interventions; Lanzer, P., Ed.; Springer: Berlin/Heidelberg, Germany, 2013; pp. 445–472. [Google Scholar]
- Tønnesen, H.H. The Photostability of Drugs and Drug Formulations; Taylor & Francis: London, UK, 1996. [Google Scholar]
- Chen, S.-H.; Farina, V.; Huang, S.; Gao, Q.; Golik, J.; Doyle, T.W. Studies on the photochemistry of taxol®. Tetrahedron 1994, 50, 8633–8650. [Google Scholar] [CrossRef]
- Petersen, S.; Kaule, S.; Stein, F.; Minrath, I.; Schmitz, K.-P.; Kragl, U.; Sternberg, K. Novel paclitaxel-coated angioplasty balloon catheter based on cetylpyridinium salicylate: Preparation, characterization and simulated use in an in vitro vessel model. Mater. Sci. Eng. C 2013, 33, 4244–4250. [Google Scholar] [CrossRef]
- Petersen, S.; Kaule, S.; Teske, M.; Minrath, I.; Schmitz, K.-P.; Sternberg, K. Development and in vitro characterization of hyaluronic acid-based coatings for implant-associated local drug delivery systems. J. Chem. 2013, 2013, 587875:1–587875:11. [Google Scholar]
- Hoffman, A.S. Hydrogels for biomedical applications. Adv. Drug Deliv. Rev. 2012, 64, S18–S23. [Google Scholar] [CrossRef]
- Scheller, B.; Speck, U.; Abramjuk, C.; Bernhardt, U.; Böhm, M.; Nickenig, G. Paclitaxel balloon coating, a novel method for prevention and therapy of restenosis. Circulation 2004, 110, 810–814. [Google Scholar] [CrossRef]
© 2013 by the authors; licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution license (http://creativecommons.org/licenses/by/3.0/).
Share and Cite
Petersen, S.; Minrath, I.; Kaule, S.; Köcher, J.; Schmitz, K.-P.; Sternberg, K. Development and in Vitro Characterization of Photochemically Crosslinked Polyvinylpyrrolidone Coatings for Drug-Coated Balloons. Coatings 2013, 3, 253-267. https://doi.org/10.3390/coatings3040253
Petersen S, Minrath I, Kaule S, Köcher J, Schmitz K-P, Sternberg K. Development and in Vitro Characterization of Photochemically Crosslinked Polyvinylpyrrolidone Coatings for Drug-Coated Balloons. Coatings. 2013; 3(4):253-267. https://doi.org/10.3390/coatings3040253
Chicago/Turabian StylePetersen, Svea, Ingo Minrath, Sebastian Kaule, Jürgen Köcher, Klaus-Peter Schmitz, and Katrin Sternberg. 2013. "Development and in Vitro Characterization of Photochemically Crosslinked Polyvinylpyrrolidone Coatings for Drug-Coated Balloons" Coatings 3, no. 4: 253-267. https://doi.org/10.3390/coatings3040253




