A Modified Surface on Titanium Deposited by a Blasting Process
Abstract
: Hydroxyapatite (HA) coating of hard tissue implants is widely employed for its biocompatible and osteoconductive properties as well as its improved mechanical properties. Plasma technology is the principal deposition process for coating HA on bioactive metals for this application. However, thermal decomposition of HA can occur during the plasma deposition process, resulting in coating variability in terms of purity, uniformity and crystallinity, which can lead to implant failure caused by aseptic loosening. In this study, CoBlast™, a novel blasting process has been used to successfully modify a titanium (V) substrate with a HA treatment using a dopant/abrasive regime. The impact of a series of apatitic abrasives under the trade name MCD, was investigated to determine the effect of abrasive particle size on the surface properties of both microblast (abrasive only) and CoBlast (HA/abrasive) treatments. The resultant HA treated substrates were compared to substrates treated with abrasive only (microblasted) and an untreated Ti. The HA powder, apatitic abrasives and the treated substrates were characterized for chemical composition, coating coverage, crystallinity and topography including surface roughness. The results show that the surface roughness of the HA blasted modification was affected by the particle size of the apatitic abrasives used. The CoBlast process did not alter the chemistry of the crystalline HA during deposition. Cell proliferation on the HA surface was also assessed, which demonstrated enhanced osteo-viability compared to the microblast and blank Ti. This study demonstrates the ability of the CoBlast process to deposit HA coatings with a range of surface properties onto Ti substrates. The ability of the CoBlast technology to offer diversity in modifying surface topography offers exciting new prospects in tailoring the properties of medical devices for applications ranging from dental to orthopedic settings.1. Introduction
2. Results and Discussion
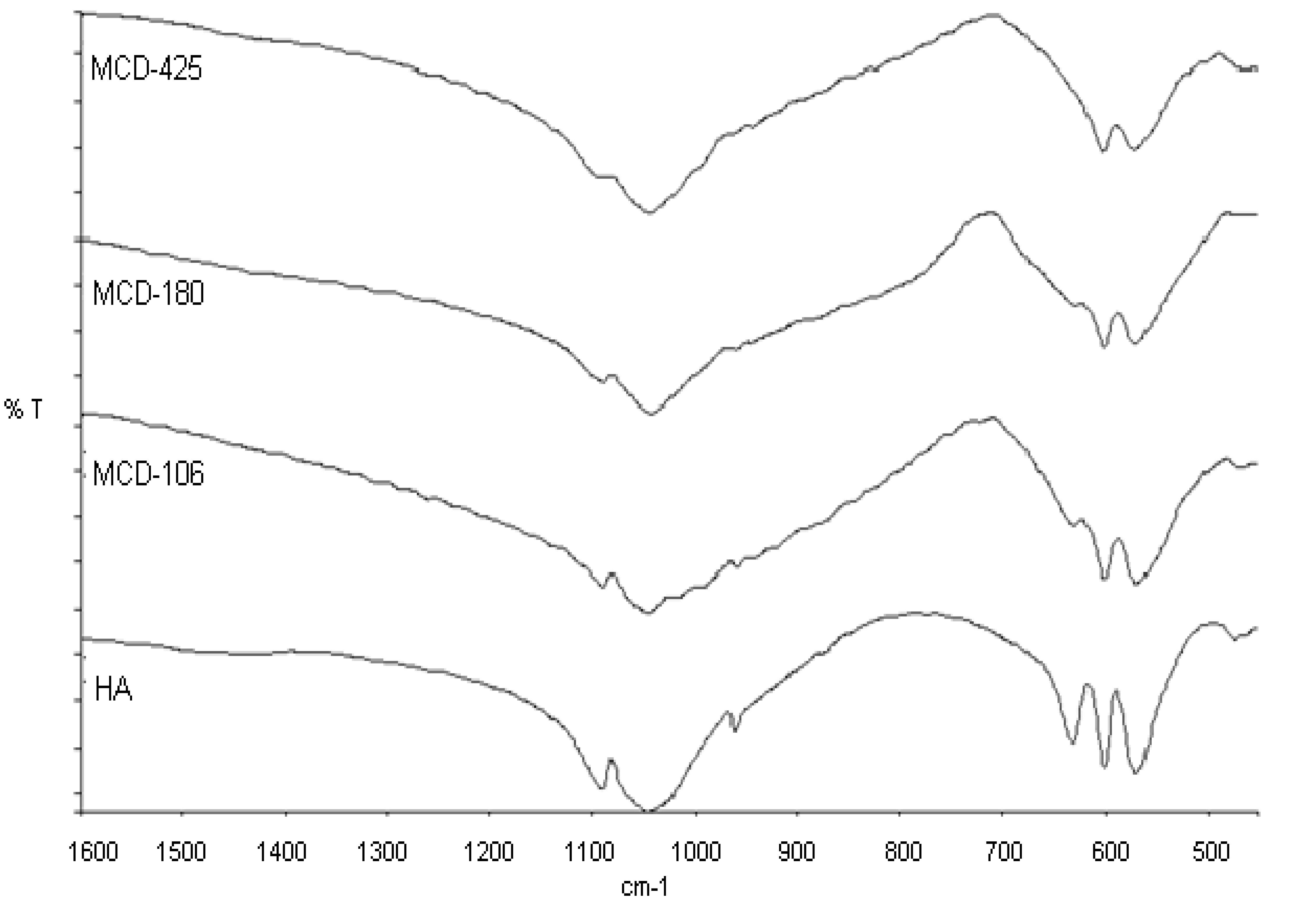
2.1. Chemical Characterization of HA and MCD Abrasive Powders
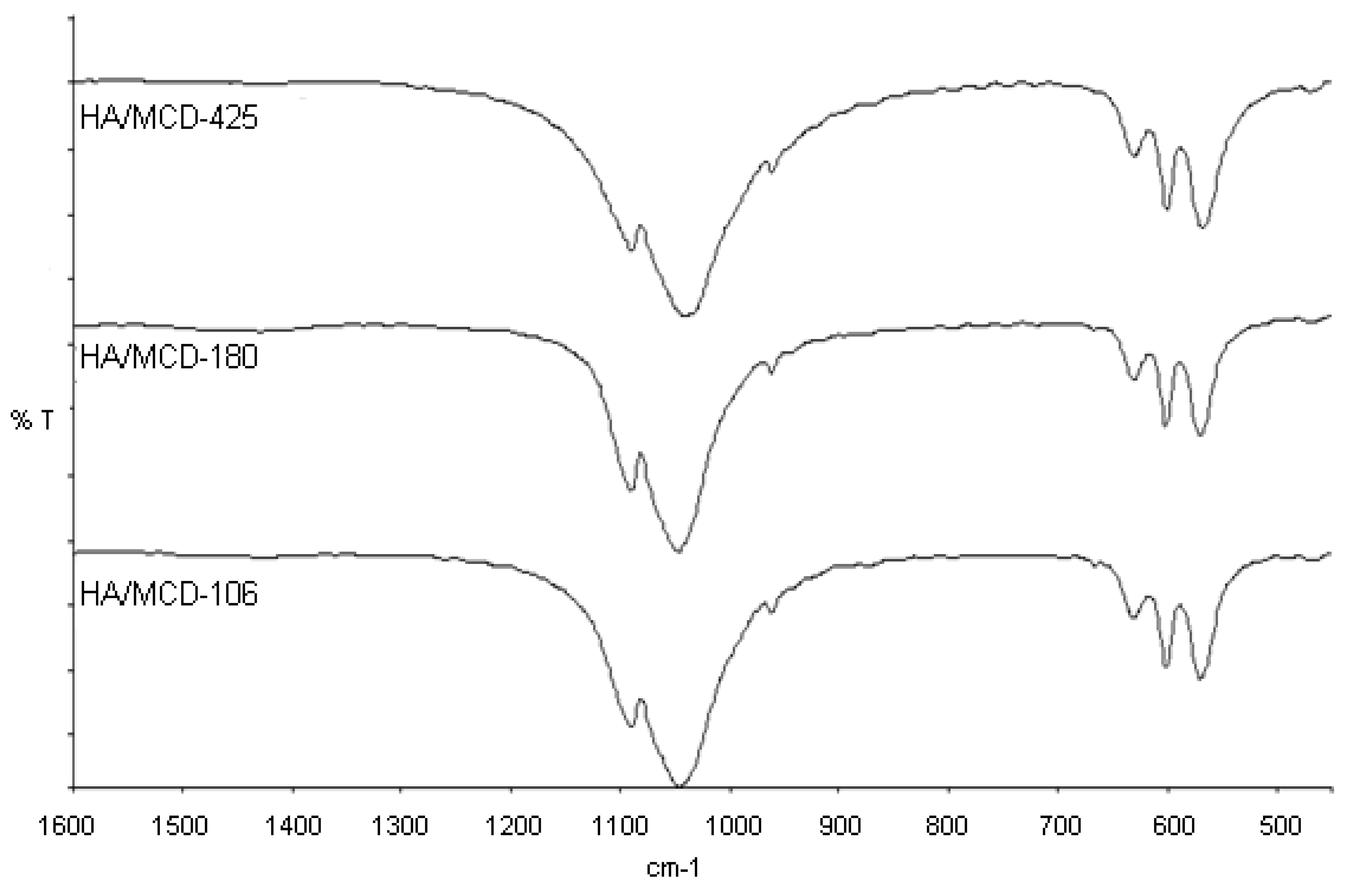
2.2. Characterization of the Modified Titanium Substrates
2.3. Cell Culture Analysis
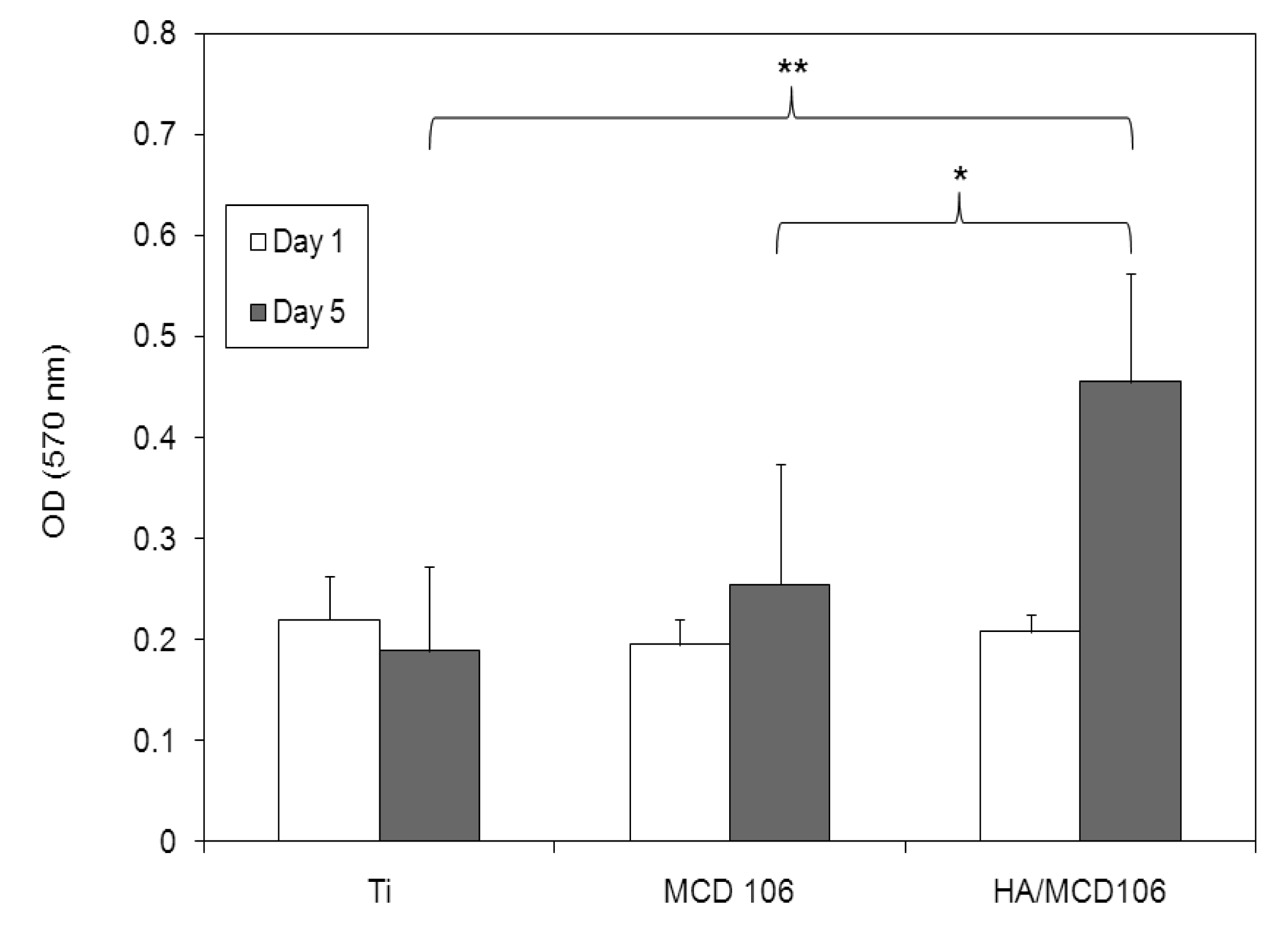
2.3.1. Cell Proliferation
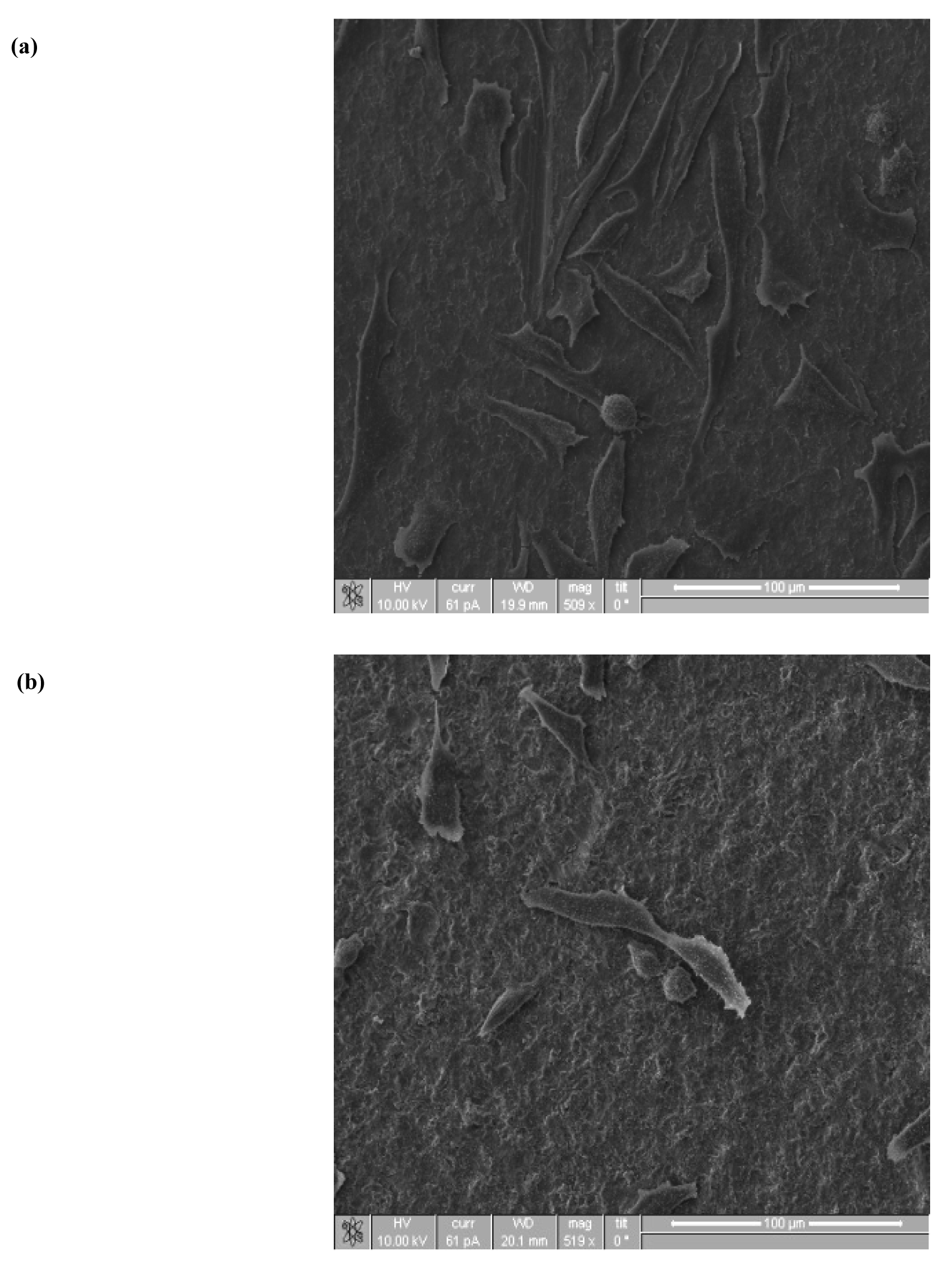
2.3.2. Cell Morphology
3. Experimental Section
3.1. Materials
3.2. Sample Preparation
3.3. Surface Characterisation
3.4. In Vitro Cell Culture
3.4.1. Cell Proliferation
3.4.2. Cell Morphology
4. Conclusions






| Powder | Mean particle Size (μm) | O % atm | Ca % atm | P % atm | Ca/P |
|---|---|---|---|---|---|
| HA | 40 (±4) | 71 | 18 | 11 | 1.66 |
| MCD-106 | 44 (±2) | 72 | 18 | 10 | 1.76 |
| MCD-180 | 124 (±6) | 73 | 17 | 10 | 1.73 |
| MCD-425 | 355 (±6) | 77 | 13 | 10 | 1.29 |
| Modification | O % atm | P % atm | Ca % atm | Ti % atm | Ca/P | Coating Thickness (μm) (2STD) | Coating Mass (mg/cm2) (2STD) | |
|---|---|---|---|---|---|---|---|---|
| Blank | Ti | 23 | - | - | 77 | - | 0 | - |
| Microblast | MCD-106 | 59 | 8 | 12 | 21 | 1.56 | 3 ± 1 | - |
| MCD-180 | 56 | 6 | 10 | 27 | 1.53 | 3 ± 1 | - | |
| MCD-425 | 55 | 7 | 11 | 27 | 1.57 | 3 ± 2 | - | |
| CoBlast | HA/MCD-106 | 63 | 13 | 21 | 2 | 1.59 | 6 ± 3 | 0.48 ± 0.4 |
| HA/MCD-180 | 67 | 12 | 18 | 3 | 1.53 | 6 ± 1 | 0.44 ± 0.4 | |
| HA/MCD-425 | 65 | 12 | 20 | 5 | 1.61 | 7 ± 3 | 0.44 ± 0.3 |
Acknowledgments
References and Notes
- Borsari, V.; Giavaresi, G.; Fini, M.; Torricelli, P.; Salito, A.; Chiesa, R.; Chiusoli, L.; Volpert, A.; Rimondini, L.; Giardino, R. Physical characterization of different-roughness titanium surfaces, with and without hydroxyapatite coating and their effect on human osteoblast-like cells. J. Biomed. Mater. Res. Part B 2005, 75B, 359–368. [Google Scholar]
- Stoch, A.; Jastrze, B.W.; Dlugon, E.; Lejda, W.; Trybalska, B.; Stoch, G.J.; Adamczyk, A. Sol-gel derived hydroxyapatite coatings on titanium and its alloy Ti6Al4V. J. Mol. Struct. 2005, 744, 633–640. [Google Scholar]
- Oh, I.H.; Nomura, N.; Chiba, A. Microstructures and bond strengths of plasma-sprayed hydroxyapatite coatings on porous titanium substrates. J. Mater. Sci. Mater. Med. 2005, 16, 635–640. [Google Scholar]
- Lu, Y.P.; Li, M.S.; Li, S.T.; Wang, Z.G.; Zhu, R.F. Plasma-sprayed hydroxyapatite + titania composite bond coat for hydroxyapatite coating on titanium substrate. Biomaterials 2004, 25, 4393–4403. [Google Scholar]
- Wennerberg, A.; Ektessabi, A.; Albrektsson, T.; Johansson, C.; Andersson, B.A. 1-year follow-up of implants of differing surface roughness placed in rabbit bone. Inter. J. Oral Maxillofac. Implants 1997, 12, 486–494. [Google Scholar]
- Abron, A.; Hopfensperger, M.; Thompson, J.; Cooper, L.F. Evaluation of a predictive model for implant surface topography effects on early osseointegration in the rat tibia model. J. Prosthet. Dent. 2001, 85, 40–46. [Google Scholar]
- Nakada, H.; Sakae, T.; Legeros, R.Z.; Legeros, J.P.; Suwa, T.; Numata, Y.; Kobayashi, K. Early tissue response to modified implant surfaces using back scattered imaging. Implant Dent. 2007, 16, 281–289. [Google Scholar]
- Gil, F.J.; Planell, J.A.; Padros, A.; Aparicio, C. The effect of shot blasting and heat treatment on the fatigue behavior of titanium for dental implant applications. Dent. Mater. 2007, 23, 486–491. [Google Scholar]
- Chen, J.; Wolke, J.G.C.; De Groot, K. Microstructure and crystallinity in hydroxyapatite coatings. Biomaterials 1994, 15, 396–399. [Google Scholar]
- Gross, K.A.; Berndt, C.C.; Herman, H. Amorphous phase formation in plasma-sprayed hydroxyapatite coatings. J. Biomed. Mater. Res. 1998, 39, 407–414. [Google Scholar]
- Gross, K.A.; Berndt, C.C. Thermal processing of hydroxyapatite for coating production. J. Biomed. Mater. Res. 1998, 39, 580–587. [Google Scholar]
- Heimann, R.B.; Wirth, R. Formation and transformation of amorphous calcium phosphates on titanium alloy surfaces during atmospheric plasma spraying and their subsequent in vitro performance. Biomaterials 2006, 27, 823–831. [Google Scholar]
- Weng, J.; Liu, Q.; Wolke, J.G.; Zhang, X.; De Groot, K. Formation and characteristics of the apatite layer on plasma-sprayed hydroxyapatite coatings in simulated body fluid. Biomaterials 1997, 18, 1027–1035. [Google Scholar]
- Li, H.; Li, Z.X.; Li, H.; Wu, Y.Z.; Wei, Q. Characterization of plasma sprayed hydroxyapatite/ZrO2 graded coating. Mater. Design 2009, 30, 3920–3924. [Google Scholar]
- Katto, M.; Kurosawa, K.; Yokotani, A.; Kubodera, S.; Kameyama, A.; Higashiguchi, T.; Nakayama, T.; Tsukamoto, M. Poly-crystallized hydroxyapatite coating deposited by pulsed laser deposition method at room temperature. Appl. Surf. Sci. 2005, 248, 365–368. [Google Scholar]
- Hong, Z.; Luan, L.; Paik, S.E.; Deng, B.; Ellis, D.E.; Ketterson, J.B.; Mello, A.; Eon, J.G.; Terra, J.; Rossi, A. Crystalline hydroxyapatite thin films produced at room temperature—An opposing radio frequency magnetron sputtering approach. Thin Solid Films 2007, 515, 6773–6780. [Google Scholar]
- Stoch, A.; Brozek, A.; Kmita, G.; Stoch, J.; Jastrzebski, W.; Rakowska, A. Electrophoretic coating of hydroxyapatite on titanium implants. J. Mole. Struct. 2001, 596, 191–200. [Google Scholar]
- Mano, T.; Ueyama, Y.; Ishikawa, K.; Matsumura, T.; Suzuki, K. Initial tissue response to a titanium implant coated with apatite at room temperature using a blast coating method. Biomaterials 2002, 23, 1931–1926. [Google Scholar]
- Gbureck, U.; Masten, A.; Probst, J.; Thull, R. Tribochemical structuring and coating of implant metal surfaces with titanium oxide and hydroxyapatite layers. Mater. Sci. Eng. C 2003, 23, 461–465. [Google Scholar]
- Ishikawa, K.; Miyamoto, Y.; Nagayama, M.; Asaoka, K. Blast coating method: New method of coating titanium surface with hydroxyapatite at room temperature. J. Biomed. Mater. Res. 1997, 38, 129–134. [Google Scholar]
- O'Hare, P.; Meenan, B.J.B.; George, A.; Byrne, G.; Dowling, D.; Hunt, J.A. In vitro and in vivo response of hydroxyapatite surfaces deposited via a novel co-incident microblasting technique for improved orthopaedic implant performance. Biomaterials 2010, 31, 515–522. [Google Scholar]
- O'Neill, L.; O'Sullivan, C.; O'Hare, P.; Sexton, L.; Keady, F.; O'Donoghue, J. Deposition of substituted apatites onto titanium surfaces using a novel blasting process. Surf. Coat. Technol. 2009, 204, 484–488. [Google Scholar]
- O'Sullivan, C.; O'Hare, P.; O'Leary, N.D.; Crean, A.M.; Ryan, K.; Dobson, A.D.; O'Neill, L.D. Deposition of substituted apatites with anticolonizing properties onto titanium surfaces using a novel blasting process. J. Biomed. Mater. Res. Part B 2010, 95, 141–149. [Google Scholar]
- Mosmann, T. Rapid colorimetric assay for cellular growth and survival: Application to proliferation and cytotoxicity assays. J. Immunol. Methods 1983, 65, 55–63. [Google Scholar]
- Kim, T.N.; Feng, Q.L.; Kim, J.O.; Wu, J.; Wang, H.; Chen, G.C.; Cui, F.Z. Antimicrobial effects of metal ions (Ag+, Cu2+, Zn2+) in hydroxyapatite. J. Mater. Sci.: Mater. Med. 1998, 9, 129–134. [Google Scholar]
- Fathi, M.H.; Hanifi, A.; Mortazavi, V. Preparation and bioactivity evaluation of bone-like hydroxyapatite nanopowder. J. Mater. Proc. Technol. 2008, 202, 536–542. [Google Scholar]
- Varma, H.K.; Babu, S.S. Synthesis of calcium phosphate bioceramics by citrate gel pyrolysis method. Ceram. Int. 2005, 31, 109–114. [Google Scholar]
- Pleshko, N.; Boskey, A.; Mendelsohn, R. Novel infrared spectroscopic method for the determination of crystallinity of hydroxyapatite minerals. Biophy. J. 1991, 60, 786–793. [Google Scholar]
- Legeros, R.Z.; Daculsi, G.; Orly, I.; Gregoire, M. Substrate surface dissolution and interfacial biological minerals. In The Bone-Biomaterial Interface; Davies, J.E., Ed.; University of Toronto: Toronto, Canada, 1991; pp. 76–88. [Google Scholar]
- Masmoudi, M.; Assoul, M.; Wery, M.; Abdelhedi, R.; El Halouani, F.; Monteil, G. Friction and wear behaviour of cp Ti and Ti6Al4V following nitric acid passivation. Appl. Surf. Sci. 2006, 253, 237–2243. [Google Scholar]
- Anselme, K. Osteoblast adhesion on biomaterials. Biomaterials 2000, 21, 667–681. [Google Scholar]
- Bigerelle, M.; Anselme, K. Statistical correlation between call adhesion and proliferation on biocompatible metallic materials. J. Biomed. Mater. Res. A 2005, 75, 530–540. [Google Scholar]
- Puckett, A.; Pareta, R.; Webster, T.J. Nano rough micron patterned titanium for directing osteoblast morphology and adhesion. Inter. J. Nanomed. 2008, 2, 229–241. [Google Scholar]
- Sun, L.; Berndt, C.C.; Gross, K.A.; Kucuk, A. Material fundamentals and clinical performance of plasma-sprayed hydroxyapatite coatings: A review. J Biomed. Mate. Res. 2001, 58, 570–592. [Google Scholar]
© 2011 by the authors; licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution license (http://creativecommons.org/licenses/by/3.0/).
Share and Cite
O’Sullivan, C.; O’Hare, P.; Byrne, G.; O’Neill, L.; Ryan, K.B.; Crean, A.M. A Modified Surface on Titanium Deposited by a Blasting Process. Coatings 2011, 1, 53-71. https://doi.org/10.3390/coatings1010053
O’Sullivan C, O’Hare P, Byrne G, O’Neill L, Ryan KB, Crean AM. A Modified Surface on Titanium Deposited by a Blasting Process. Coatings. 2011; 1(1):53-71. https://doi.org/10.3390/coatings1010053
Chicago/Turabian StyleO’Sullivan, Caroline, Peter O’Hare, Greg Byrne, Liam O’Neill, Katie B. Ryan, and Abina M. Crean. 2011. "A Modified Surface on Titanium Deposited by a Blasting Process" Coatings 1, no. 1: 53-71. https://doi.org/10.3390/coatings1010053
APA StyleO’Sullivan, C., O’Hare, P., Byrne, G., O’Neill, L., Ryan, K. B., & Crean, A. M. (2011). A Modified Surface on Titanium Deposited by a Blasting Process. Coatings, 1(1), 53-71. https://doi.org/10.3390/coatings1010053





