Detection of Alpha-Methylacyl-CoA Racemase (AMACR), a Biomarker of Prostate Cancer, in Patient Blood Samples Using a Nanoparticle Electrochemical Biosensor
Abstract
:1. Introduction
2. Experimental
2.1. Chemistry and Reaction Mechanisms of Detecting AMACR
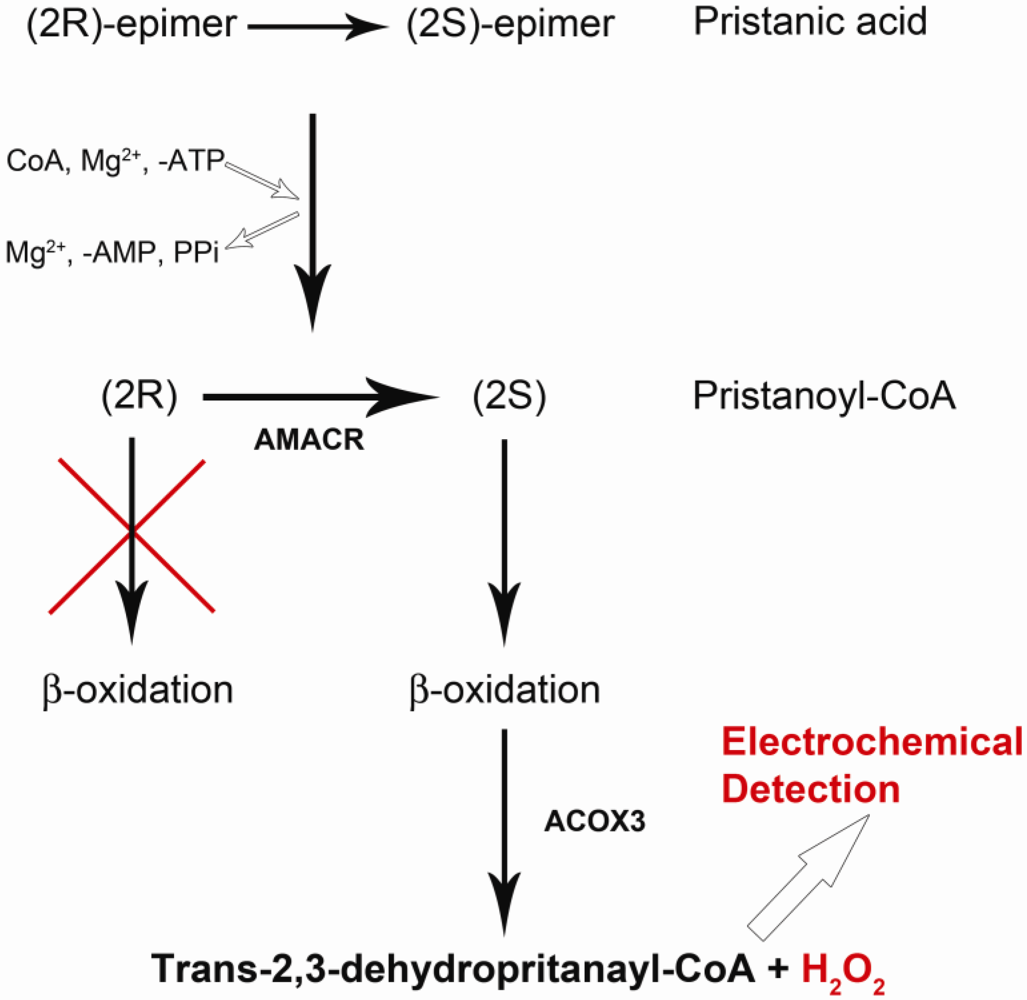
2.2. AMACR Biosensor Fabrication
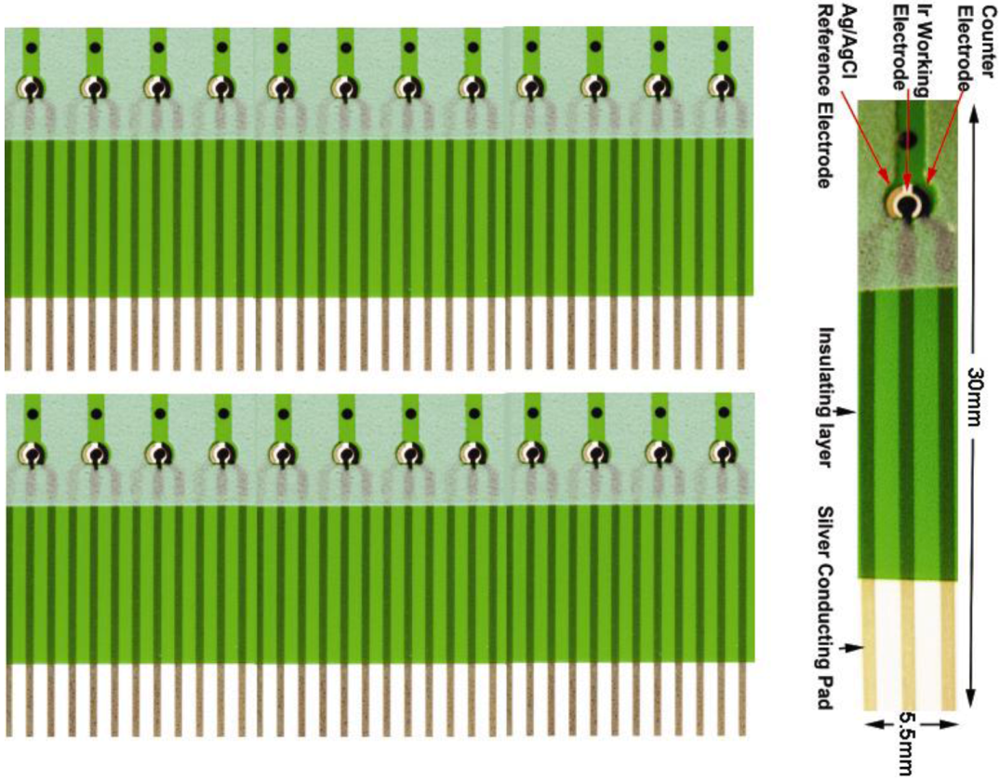
2.3. Calibration of this AMACR Biosensor

3. Results and Discussion
| Healthy Controls (N = 9) | HGPIN (N = 10) | Prostate Cancer Cases (N = 5) | |
|---|---|---|---|
| Gleason score, N (%) | N/A | N/A | |
| Mean (SD) Plasma PSA, ng/mL | 2.31 (1.67) | 18.86 (7.43) | 15.81 (11.43) |
| Mean (SD) Plasma AMACR, µg/µL | 0.005 (0.001) | 0.0004 (0.0005) | 0.077 (0.10) |
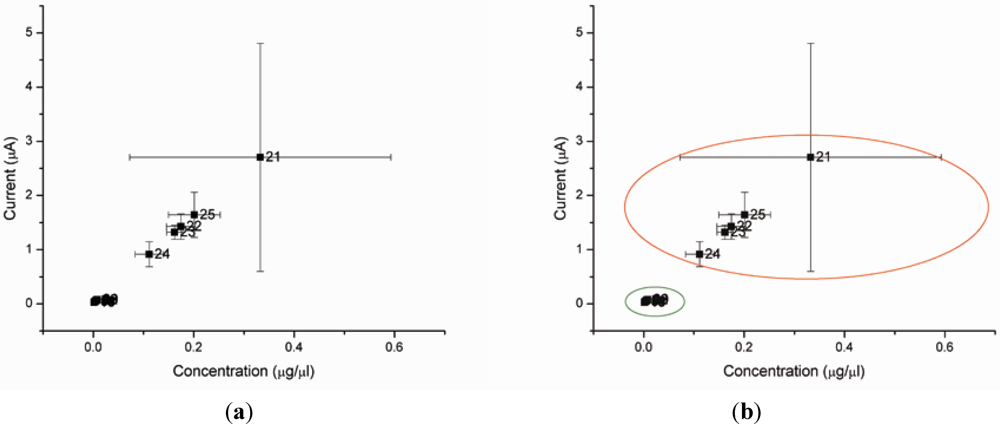
4. Conclusions
Acknowledgements
References
- Jemal, A.; Siegel, R.; Xu, J.; Ward, E. Cancer statistics. CA Cancer J. Clin. 2010, 60, 277–300. [Google Scholar] [CrossRef]
- Siegel, R.; Naishadham, D.; Jemal, A. Cancer statistics. CA Cancer J. Clin. 2012, 62, 10–29. [Google Scholar] [CrossRef]
- Brawer, M.K.; Chetner, M.P.; Beatie, J.; Buchner, D.M.; Vessella, R.L.; Lange, P.H. Screening for prostatic carcinoma with prostate specific antigen. J. Urol. 1992, 147, 841–845. [Google Scholar]
- Catalona, W.J.; Richie, J.P.; Ahmann, F.R.; Hudson, M.A.; Scardino, P.T.; Flanigan, R.C.; de Kernion, J.B.; Ratliff, T.L.; Kavoussi, L.R.; Dalkin, B.L.; et al. Comparison of digital rectal examination and serum prostate specific antigen in the early detection of prostate cancer: Results of a multicenter clinical trial of 6,630 men. J. Urol. 1994, 151, 1283–1290. [Google Scholar]
- Catalona, W.J.; Smith, D.S.; Ornstein, D.K. Prostate cancer detection in men with serum psa concentrations of 2.6 to 4.0 ng/mL and benign prostate examination. Enhancement of specificity with free psa measurements. JAMA 1997, 277, 1452–1455. [Google Scholar] [CrossRef]
- Cooperberg, M.R.; Lubeck, D.P.; Mehta, S.S.; Carroll, P.R. Time trends in clinical risk stratification for prostate cancer: Implications for outcomes (data from capsure). J. Urol. 2003, 170, S21–S25, discussion S26–S27. [Google Scholar] [CrossRef]
- Di Giuseppe, J.A.; Sauvageot, J.; Epstein, J.I. Increasing incidence of minimal residual cancer in radical prostatectomy specimens. Am. J. Surg. Pathol. 1997, 21, 174–178. [Google Scholar] [CrossRef]
- Jemal, A.; Ward, E.; Wu, X.; Martin, H.J.; McLaughlin, C.C.; Thun, M.J. Geographic patterns of prostate cancer mortality and variations in access to medical care in the united states. Cancer Epidemiol. Biomarkers Prev. 2005, 14, 590–595. [Google Scholar] [CrossRef]
- Polascik, T.J.; Oesterling, J.E.; Partin, A.W. Prostate specific antigen: A decade of discovery—What we have learned and where we are going. J. Urol. 1999, 162, 293–306. [Google Scholar] [CrossRef]
- Tosoian, J.; Loeb, S. Psa and beyond: The past, present, and future of investigative biomarkers for prostate cancer. Sci. World J. 2010, 10, 1919–1931. [Google Scholar] [CrossRef]
- Draisma, G.; Etzioni, R.; Tsodikov, A.; Mariotto, A.; Wever, E.; Gulati, R.; Feuer, E.; de Koning, H. Lead time and overdiagnosis in prostate-specific antigen screening: Importance of methods and context. J. Natl. Cancer Inst. 2009, 101, 374–383. [Google Scholar] [CrossRef]
- Esserman, L.; Shieh, Y.; Thompson, I. Rethinking screening for breast cancer and prostate cancer. JAMA 2009, 302, 1685–1692. [Google Scholar] [CrossRef]
- Hakama, M.; Coleman, M.P.; Alexe, D.M.; Auvinen, A. Cancer screening: Evidence and practice in Europe 2008. Eur. J. Cancer 2008, 44, 1404–1413. [Google Scholar] [CrossRef]
- Hasui, Y.; Marutsuka, K.; Asada, Y.; Ide, H.; Nishi, S.; Osada, Y. Relationship between serum prostate specific antigen and histological prostatitis in patients with benign prostatic hyperplasia. Prostate 1994, 25, 91–96. [Google Scholar] [CrossRef]
- Nadler, R.B.; Humphrey, P.A.; Smith, D.S.; Catalona, W.J.; Ratliff, T.L. Effect of inflammation and benign prostatic hyperplasia on elevated serum prostate specific antigen levels. J. Urol. 1995, 154, 407–413. [Google Scholar] [CrossRef]
- Djavan, B.; Zlotta, A.; Remzi, M.; Ghawidel, K.; Basharkhah, A.; Schulman, C.C.; Marberger, M. Optimal predictors of prostate cancer on repeat prostate biopsy: A prospective study of 1,051 men. J. Urol. 2000, 163, 1144–1148, discussion 1148–1149. [Google Scholar] [CrossRef]
- Roberts, R.O.; Bergstralh, E.J.; Besse, J.A.; Lieber, M.M.; Jacobsen, S.J. Trends and risk factors for prostate biopsy complications in the pre-psa and psa eras, 1980 to 1997. Urology 2002, 59, 79–84. [Google Scholar] [CrossRef]
- Wolf, A.M.; Wender, R.C.; Etzioni, R.B.; Thompson, I.M.; D'Amico, A.V.; Volk, R.J.; Brooks, D.D.; Dash, C.; Guessous, I.; Andrews, K.; et al. American cancer society guideline for the early detection of prostate cancer: Update 2010. CA Cancer J. Clin. 2010, 60, 70–98. [Google Scholar] [CrossRef]
- Benson, M.C.; Whang, I.S.; Pantuck, A.; Ring, K.; Kaplan, S.A.; Olsson, C.A.; Cooner, W.H. Prostate specific antigen density: A means of distinguishing benign prostatic hypertrophy and prostate cancer. J. Urol. 1992, 147, 815–816. [Google Scholar]
- Borofsky, M.S.; Makarov, D.V. Prostate cancer: Psa velocity in prostate cancer screening—The debate continues. Nat. Rev. Urol. 2011, 8, 413–414. [Google Scholar] [CrossRef]
- Oesterling, J.E. Prostate specific antigen: A critical assessment of the most useful tumor marker for adenocarcinoma of the prostate. J. Urol. 1991, 145, 907–923. [Google Scholar]
- Ohori, M.; Dunn, J.K.; Scardino, P.T. Is prostate-specific antigen density more useful than prostate-specific antigen levels in the diagnosis of prostate cancer? Urology 1995, 46, 666–671. [Google Scholar] [CrossRef]
- Essink-Bot, M.L.; de Koning, H.J.; Nijs, H.G.; Kirkels, W.J.; van der Maas, P.J.; Schroder, F.H. Short-term effects of population-based screening for prostate cancer on health-related quality of life. J. Natl. Cancer Inst. 1998, 90, 925–931. [Google Scholar]
- Etzioni, R.; Penson, D.F.; Legler, J.M.; di Tommaso, D.; Boer, R.; Gann, P.H.; Feuer, E.J. Overdiagnosis due to prostate-specific antigen screening: Lessons from u.S. Prostate cancer incidence trends. J. Natl. Cancer Inst. 2002, 94, 981–990. [Google Scholar] [CrossRef]
- Fowler, F.J., Jr; Barry, M.J.; Walker-Corkery, B.; Caubet, J.F.; Bates, D.W.; Lee, J.M.; Hauser, A.; McNaughton-Collins, M. The impact of a suspicious prostate biopsy on patients’ psychological, socio-behavioral, and medical care outcomes. J. Gen. Intern. Med. 2006, 21, 715–721. [Google Scholar] [CrossRef]
- Hsieh, C.L.; Oakley-Girvan, I.; Balise, R.R.; Halpern, J.; Gallagher, R.P.; Wu, A.H.; Kolonel, L.N.; O’Brien, L.E.; Lin, I.G.; van Den Berg, D.J.; et al. A genome screen of families with multiple cases of prostate cancer: Evidence of genetic heterogeneity. Am. J. Hum. Genet. 2001, 69, 148–158. [Google Scholar] [CrossRef]
- Wiklund, F.; Gillanders, E.M.; Albertus, J.A.; Bergh, A.; Damber, J.E.; Emanuelsson, M.; Freas-Lutz, D.L.; Gildea, D.E.; Goransson, I.; Jones, M.S.; et al. Genome-wide scan of swedish families with hereditary prostate cancer: Suggestive evidence of linkage at 5q11.2 and 19p13.3. Prostate 2003, 57, 290–297. [Google Scholar] [CrossRef]
- Lloyd, M.D.; Darley, D.J.; Wierzbicki, A.S.; Threadgill, M.D. Alpha-methylacyl-coa racemase—an ‘obscure’ metabolic enzyme takes centre stage. FEBS J. 2008, 275, 1089–1102. [Google Scholar] [CrossRef]
- Mukherji, M.; Schofield, C.J.; Wierzbicki, A.S.; Jansen, G.A.; Wanders, R.J.; Lloyd, M.D. The chemical biology of branched-chain lipid metabolism. Prog. Lipid Res. 2003, 42, 359–376. [Google Scholar] [CrossRef]
- Shen, J.; Dudik, L.; Liu, C.-C. An iridium nanoparticles dispersed carbon based thick film electrochemical biosensor and its application for a single use, disposable glucose biosensor. Sens. Actuator. B Chem. 2007, 125, 106–113. [Google Scholar] [CrossRef]
- Jiang, Z.; Woda, B.A.; Rock, K.L.; Xu, Y.; Savas, L.; Khan, A.; Pihan, G.; Cai, F.; Babcook, J.S.; Rathanaswami, P.; et al. P504s: A new molecular marker for the detection of prostate carcinoma. Am. J. Surg. Pathol. 2001, 25, 1397–1404. [Google Scholar] [CrossRef]
© 2012 by the authors; licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution license (http://creativecommons.org/licenses/by/3.0/).
Share and Cite
Lin, P.-Y.; Cheng, K.-L.; McGuffin-Cawley, J.D.; Shieu, F.-S.; Samia, A.C.; Gupta, S.; Cooney, M.; Thompson, C.L.; Liu, C.C. Detection of Alpha-Methylacyl-CoA Racemase (AMACR), a Biomarker of Prostate Cancer, in Patient Blood Samples Using a Nanoparticle Electrochemical Biosensor. Biosensors 2012, 2, 377-387. https://doi.org/10.3390/bios2040377
Lin P-Y, Cheng K-L, McGuffin-Cawley JD, Shieu F-S, Samia AC, Gupta S, Cooney M, Thompson CL, Liu CC. Detection of Alpha-Methylacyl-CoA Racemase (AMACR), a Biomarker of Prostate Cancer, in Patient Blood Samples Using a Nanoparticle Electrochemical Biosensor. Biosensors. 2012; 2(4):377-387. https://doi.org/10.3390/bios2040377
Chicago/Turabian StyleLin, Po-Yuan, Kai-Lun Cheng, James D. McGuffin-Cawley, Fuh-Sheng Shieu, Anna C. Samia, Sanjay Gupta, Matthew Cooney, Cheryl L. Thompson, and Chung Chiun Liu. 2012. "Detection of Alpha-Methylacyl-CoA Racemase (AMACR), a Biomarker of Prostate Cancer, in Patient Blood Samples Using a Nanoparticle Electrochemical Biosensor" Biosensors 2, no. 4: 377-387. https://doi.org/10.3390/bios2040377
APA StyleLin, P.-Y., Cheng, K.-L., McGuffin-Cawley, J. D., Shieu, F.-S., Samia, A. C., Gupta, S., Cooney, M., Thompson, C. L., & Liu, C. C. (2012). Detection of Alpha-Methylacyl-CoA Racemase (AMACR), a Biomarker of Prostate Cancer, in Patient Blood Samples Using a Nanoparticle Electrochemical Biosensor. Biosensors, 2(4), 377-387. https://doi.org/10.3390/bios2040377







