Quantification of Right and Left Ventricular Function in Cardiac MR Imaging: Comparison of Semiautomatic and Manual Segmentation Algorithms
Abstract
:1. Introduction
2. Materials and Methods
2.1. Study Population
2.2. MR Imaging Protocol
2.3. Image Analysis
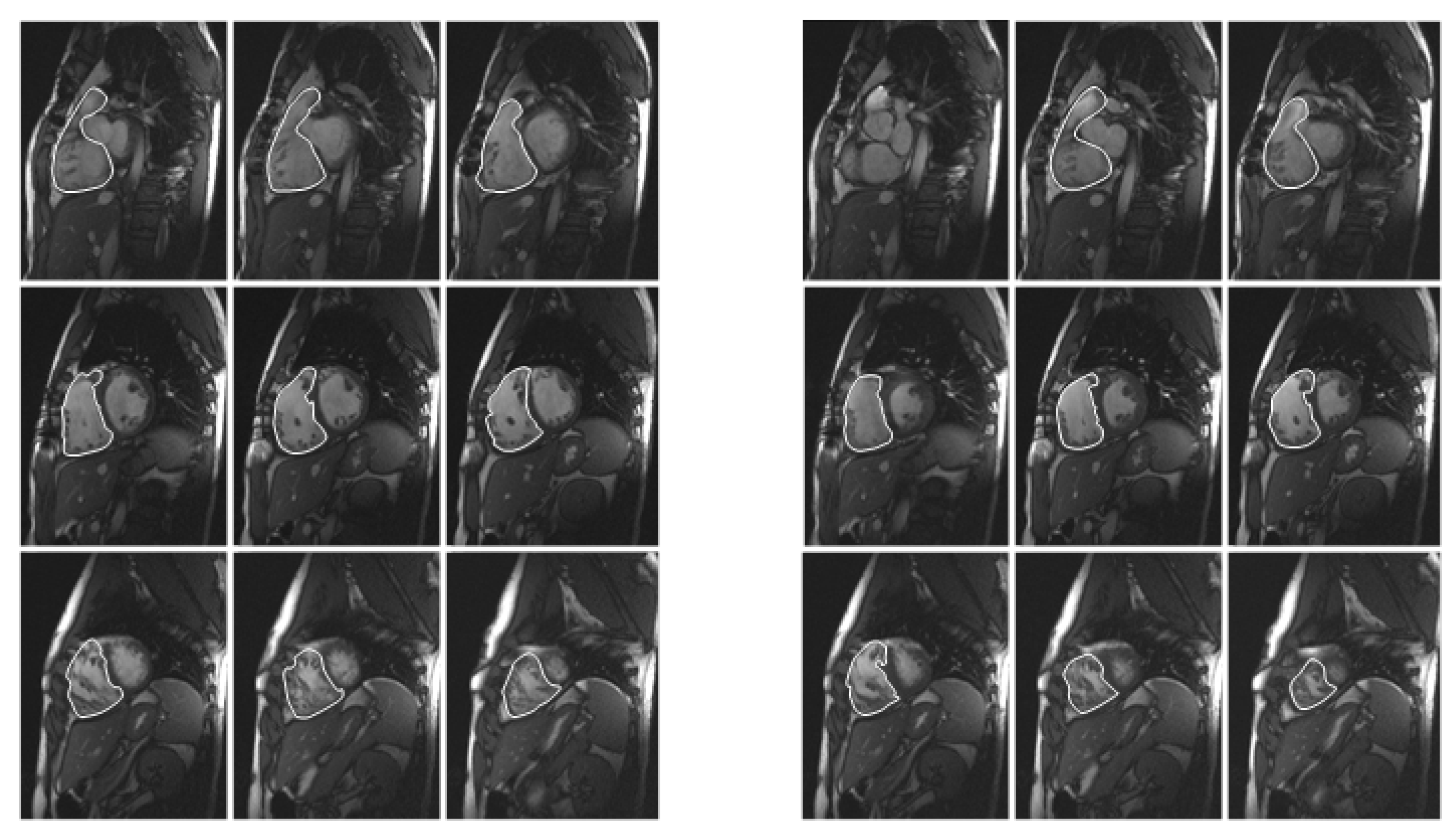
2.4. Manual Method
2.5. Semiautomatic Method

2.6. Statistical Analysis
| Semiautomatic Mean ± SD | Manual Mean ± SD | Semiautomatic vs. Manual r/p * | |
|---|---|---|---|
| EDV (mL) | 149.2 ± 53.4 | 153.2 ± 53.7 | 0.937/0.129 |
| ESV (mL) | 69.9 ± 48.4 | 73.7 ± 48.8 | 0.961/0.051 |
| EF (%) | 56.2 ± 17.7 | 55.2 ± 15.3 | 0.918/0.279 |
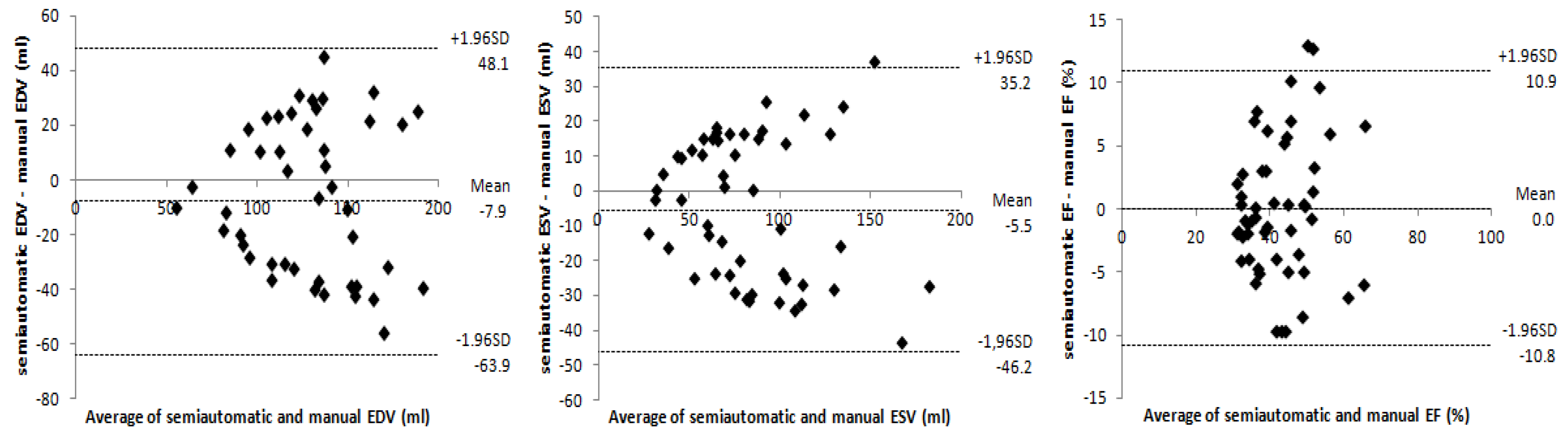
3. Results
3.1. Quantification of LV Parameters

3.2. Quantification of RV Parameters
| Semiautomatic Mean ± SD | Manual Mean ± SD | Semiautomatic vs. Manual r/p * | |
|---|---|---|---|
| EDV (mL) | 142.5 ± 62.5 | 150.4 ± 67.8 | 0.907/0.050 |
| ESV (mL) | 83.5 ± 42.8 | 89.0 ± 48.2 | 0.902/0.061 |
| EF (%) | 42.6 ± 9.6 | 42.5 ± 8.9 | 0.823/0.952 |
Time Efficiency
4. Discussion
Acknowledgements
References
- Becker, M.; Frauenrath, T.; Hezel, F.; Krombach, G.A.; Kremer, U.; Koppers, B.; Butenweg, C.; Goemmel, A.; Utting, J.F.; Schulz-Menger, J.; Niendorf, T. Comparison of left ventricular function assessment using phonocardiogram- and electrocardiogram-triggered 2D SSFP CINE MR imaging at 1.5 T and 3.0 T. Eur. Radiol. 2010, 20, 1344–1355. [Google Scholar] [CrossRef]
- Baldy, C.; Douek, P.; Croisille, P.; Magnin, I.E.; Revel, D.; Amiel, M. Automated myocardial edge detection from breath-hold cine-MR images: Evaluation of left ventricular volumes and mass. Magn. Reson. Imag. 1994, 12, 589–598. [Google Scholar] [CrossRef]
- Bastarrika, G.; Domínguez, P.D.; Azcárate, P.M.; Castaño, S.; Fernández, M.E.; Gavira, J.J. Cuantificación de la función y masa ventricular con secuencias SSFP en tiempo real y respiración libre (in Spanish). Radiología 2008, 50, 67–74. [Google Scholar] [CrossRef]
- Lubbers, D.D.; Willems, T.P.; van der Vleuten, P.A.; Overbosch, J.; Götte, M.J.; van Veldhuisen, D.J.; Oudkerk, M. Assessment of global left ventricular functional parameters: Analysis of every second short-axis magnetic resonance imaging slices is as accurate as analysis of consecutive slices. Int. J. Cardiovasc. Imag. 2008, 24, 185–191. [Google Scholar] [CrossRef]
- Kunz, R.P.; Oellig, F.; Krummenauer, F.; Oberholzer, K.; Romaneehsen, B.; Vomweg, T.W.; Horstick, G.; Hayes, C.; Thelen, M.; Kreitner, K.F. Assessment of left ventricular function by breath-hold cine MR imaging: Comparison of different steady-state free precession sequences. J. Magn. Reson. Imag. 2005, 21, 140–148. [Google Scholar] [CrossRef]
- Holloway, C.J.; Edwards, L.M.; Rider, O.J.; Fast, A.; Clarke, K.; Francis, J.M.; Myerson, S.G.; Neubauer, S. A comparison of visual and quantitative assessment of left ventricular ejection fraction by cardiac magnetic resonance. Int. J. Cardiovasc. Imag. 2011, 27, 563–569. [Google Scholar] [CrossRef]
- Van der Geest, R.J.; Lelieveldt, B.P.; Angelié, E.; Danilouchkine, M.; Swingen, C.; Sonka, M.; Reiber, J.H. Evaluation of a new method for automated detection of left ventricular boundaries in time series of magnetic resonance imaging using an active appearance motion model. J. Cardiovasc. Magn. Reson. 2004, 6, 609–617. [Google Scholar] [CrossRef]
- Hudsmith, L.E.; Petersen, S.E.; Francis, J.M.; Robson, M.D.; Neubauer, S. Normal human left and right ventricular and left atrial dimensions using steady state free precession magnetic resonance imaging. J. Cardiovasc. Magn. Reson. 2005, 7, 775–782. [Google Scholar] [CrossRef]
- Maceira, A.M.; Prasad, S.K.; Khan, M.; Pennell, D.J. Reference right ventricular systolic and diastolic function normalized to age, gender and body surface area from steady-state free precession cardiovascular magnetic resonance. Eur. Heart J. 2006, 27, 2879–2888. [Google Scholar] [CrossRef]
- Geva, T. Repaired tetralogy of Fallot: The roles of cardiovascular magnetic resonance in evaluating pathophysiology and for pulmonary valve replacement decision support. J. Cardiovasc. Magn. Reson. 2011. [Google Scholar] [CrossRef]
- Morcos, P.; Vick, G.W., III; Sahn, D.J.; Jerosch-Herold, M.; Shurman, A.; Sheehan, F.H. Correlation of right ventricular ejection fraction and tricuspid annular plane systolic excursion in tetralogy of Fallot by magnetic resonance imaging. Int. J. Cardiovasc. Imag. 2009, 25, 263–270. [Google Scholar] [CrossRef]
- Sardanelli, F.; Quarenghi, M.; di Leo, G.; Boccaccini, L.; Schiavi, A. Segmentation of cardiac cine MR images of left and right ventricles: Interactive semiautomated methods and manual contouring by two readers with different education and experience. J. Magn. Reson. Imag. 2008, 27, 785–792. [Google Scholar] [CrossRef]
- Petitjean, C.; Dacher, J.N. A review of segmentation methods in short axis cardiac MR images. Med. Image Anal. 2011, 15, 169–184. [Google Scholar] [CrossRef]
- Alfakih, H.; Plein, S.; Thiele, H.; Jones, T.; Ridgway, J.P.; Sivananthan, N. Normal human left and right ventricular dimensions for MRI as assessed by turbo gradient echo and steady-state free precession imaging sequences. J. Magn. Reson. Imag. 2003, 17, 323–329. [Google Scholar] [CrossRef]
- Narayan, G.; Nayak, K.; Pauly, J.; Hu, B. Single-breathhold, four-dimensional, quantitative assessment of LV and RV function using triggered, real time, steady-state free precession MRI in heart failure patients. J. Magn. Reson. Imag. 2005, 22, 59–66. [Google Scholar] [CrossRef]
- Kim, T.H.; Ryu, Y.H.; Hur, J.; Kim, S.J.; Kim, H.S.; Choi, B.W.; Kim, Y.; Kim, H.J. Evaluation of right ventricular volume and mass using retrospective ECG-gated cardiac multidetector computed tomography: Comparison with first-pass radionuclide angiography. Eur. Radiol. 2005, 15, 1987–1993. [Google Scholar] [CrossRef]
- Lötjönen, J.M.; Järvinen, V.M.; Cheong, B.; Wu, E.; Kivistö, S.; Koikkalainen, J.R.; Mattila, J.J.; Kervinen, H.M.; Muthupillai, R.; Sheehan, F.H.; Lauerma, K. Evaluation of cardiac biventricular segmentation from multiaxis MRI data: A multicenter study. J. Magn. Reson. Imag. 2008, 28, 626–636. [Google Scholar] [CrossRef]
- Masip, L.R.; Tahoces, P.G.; Souto, M.; Martínez, A.; Vidal, J.J. Semiautomatic quantification of left and right ventricular functions in magnetic resonance imaging. Comput. Cardiol. 2010, 37, 797–800. [Google Scholar]
- Umbaugh, S.E. Computer Vision and Image Processing: A Practical Approach Using CVIP Tools; Prentice Hall PTR: Upper Saddle River, NJ, USA, 1998. [Google Scholar]
- Bellenger, N.G.; Davies, L.C.; Francis, J.M.; Coats, A.J.; Pennell, D.J. Reduction in sample size for studies of remodeling in heart failure by the use of cardiovascular magnetic resonance. J. Cardiovasc. Magn. Reson. 2000, 2, 271–278. [Google Scholar] [CrossRef]
- Bland, J.M.; Altman, D.G. Statistical methods for assessing agreement between two methods of clinical measurement. Lancet 1986, 1, 307–310. [Google Scholar] [CrossRef]
- Hendel, R.C.; Patel, M.R.; Kramer, C.M.; Poon, M.; Hendel, R.C.; Carr, J.C.; Gerstad, N.A.; Gillam, L.D.; Hodgson, J.M.; Kim, R.J.; et al. ACCF/ACR/SCCT/SCMR/ASNC/NASCI/SCAI/SIR 2006 appropriateness criteria for cardiac computed tomography and cardiac magnetic resonance imaging. J. Am. Coll. Cardiol. 2006, 48, 1475–1497. [Google Scholar] [CrossRef] [Green Version]
- Bastarrika, G.; Arraiza, M.; Pueyo, J.C.; Herraiz, M.J.; Zudaire, B.; Villanueva, A. Quantification of left ventricular function and mass in cardiac Dual-Source CT (DSCT) exams: Comparison of manual and semiautomatic segmentation algorithms. Eur. Radiol. 2008, 18, 939–946. [Google Scholar] [CrossRef]
- Mühlenbruch, G.; Das, M.; Hohl, C.; Wildberger, J.E.; Rinck, D.; Flohr, T.G.; Koos, R.; Knackstedt, C.; Günther, R.W.; Mahnken, A.H. Global left ventricular function in cardiac CT. Evaluation of an automated 3D region-growing segmentation algorithm. Eur. Radiol. 2006, 16, 1117–1123. [Google Scholar] [CrossRef]
- Vogel, M.; Gutberlet, M.; Dittrich, S.; Hosten, N.; Lange, P.E. Comparison of transthoracic three dimensional echocardiography with magnetic resonance imaging in the assessment of right ventricular volume and mass. Heart 1997, 78, 127–130. [Google Scholar] [CrossRef] [PubMed]
- Remy-Jardin, M.; Remy, J. Integrated Cardiothoracic Imaging with MDCT; Springer-Verlag: Berlin, Germany, 2009. [Google Scholar]
- Ho, S.Y.; Nihoyannopoulos, P. Anatomy, echocardiography, and normal right ventricular dimensions. Heart 2006, 92, i2–i13. [Google Scholar] [CrossRef]
- Childs, H.; Ma, L.; Ma, M.; Clarke, J.; Cocker, M.; Green, J.; Strohm, O.; Friedrich, M.G. Comparison of long and short axis quantification of left ventricular volume parameters by cardiovascular magnetic resonance, with ex vivo validation. J. Cardiovasc. Magn. Reson. 2011. [Google Scholar] [CrossRef]
- Catalano, O.; Corsi, C.; Antonaci, S.; Moro, G.; Mussida, M.; Frascaroli, M.; Baldi, M.; Caiani, E.; Lamberti, C.; Cobelli, F. Improved reproducibility of right ventricular volumes and function estimation from cardiac magnetic resonance images using level-set models. Magn. Reson. Med. 2007, 57, 600–605. [Google Scholar] [CrossRef]
- Von Knobelsdorff-Brenkenhoff, F.; Frauenrath, T.; Prothmann, M.; Dieringer, M.A.; Hezel, F.; Renz, W.; Kretschel, K.; Niendorf, T.; Schulz-Menger, J. Cardiac chamber quantification using magnetic resonance imaging at 7 Tesla—A pilot study. Eur. Radiol. 2010, 20, 2844–2852. [Google Scholar] [CrossRef]
- Nassenstein, K.; Eberle, H.; Maderwald, S.; Jensen, C.J.; Heilmaier, C.; Schlosser, T.; Bruder, O. Single breath-hold magnetic resonance cine imaging for fast assessment of global and regional left ventricular function in clinical routine. Eur. Radiol. 2010, 20, 2341–2347. [Google Scholar] [CrossRef]
© 2013 by the authors; licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution license (http://creativecommons.org/licenses/by/3.0/).
Share and Cite
Souto, M.; Masip, L.R.; Couto, M.; Suárez-Cuenca, J.J.; Martínez, A.; Tahoces, P.G.; Carreira, J.M.; Croisille, P. Quantification of Right and Left Ventricular Function in Cardiac MR Imaging: Comparison of Semiautomatic and Manual Segmentation Algorithms. Diagnostics 2013, 3, 271-282. https://doi.org/10.3390/diagnostics3020271
Souto M, Masip LR, Couto M, Suárez-Cuenca JJ, Martínez A, Tahoces PG, Carreira JM, Croisille P. Quantification of Right and Left Ventricular Function in Cardiac MR Imaging: Comparison of Semiautomatic and Manual Segmentation Algorithms. Diagnostics. 2013; 3(2):271-282. https://doi.org/10.3390/diagnostics3020271
Chicago/Turabian StyleSouto, Miguel, Lambert Raul Masip, Miguel Couto, Jorge Juan Suárez-Cuenca, Amparo Martínez, Pablo G. Tahoces, Jose Martin Carreira, and Pierre Croisille. 2013. "Quantification of Right and Left Ventricular Function in Cardiac MR Imaging: Comparison of Semiautomatic and Manual Segmentation Algorithms" Diagnostics 3, no. 2: 271-282. https://doi.org/10.3390/diagnostics3020271




