Cerebral Metastases from Malignant Melanoma: Current Treatment Strategies, Advances in Novel Therapeutics and Future Directions
Abstract
:1. Introduction
2. Clinicopathological Characteristics
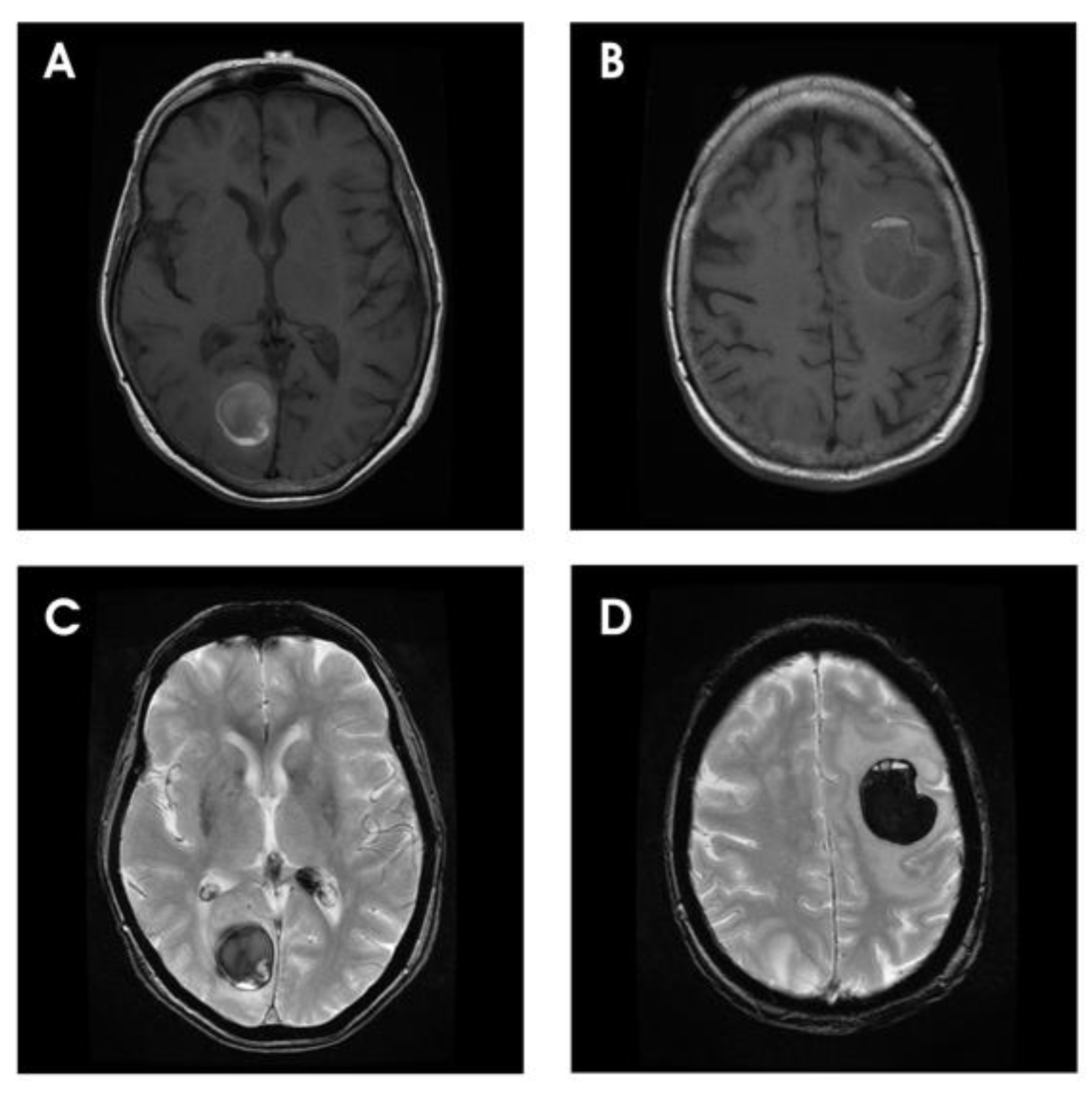
3. Radiotherapy
4. Surgery
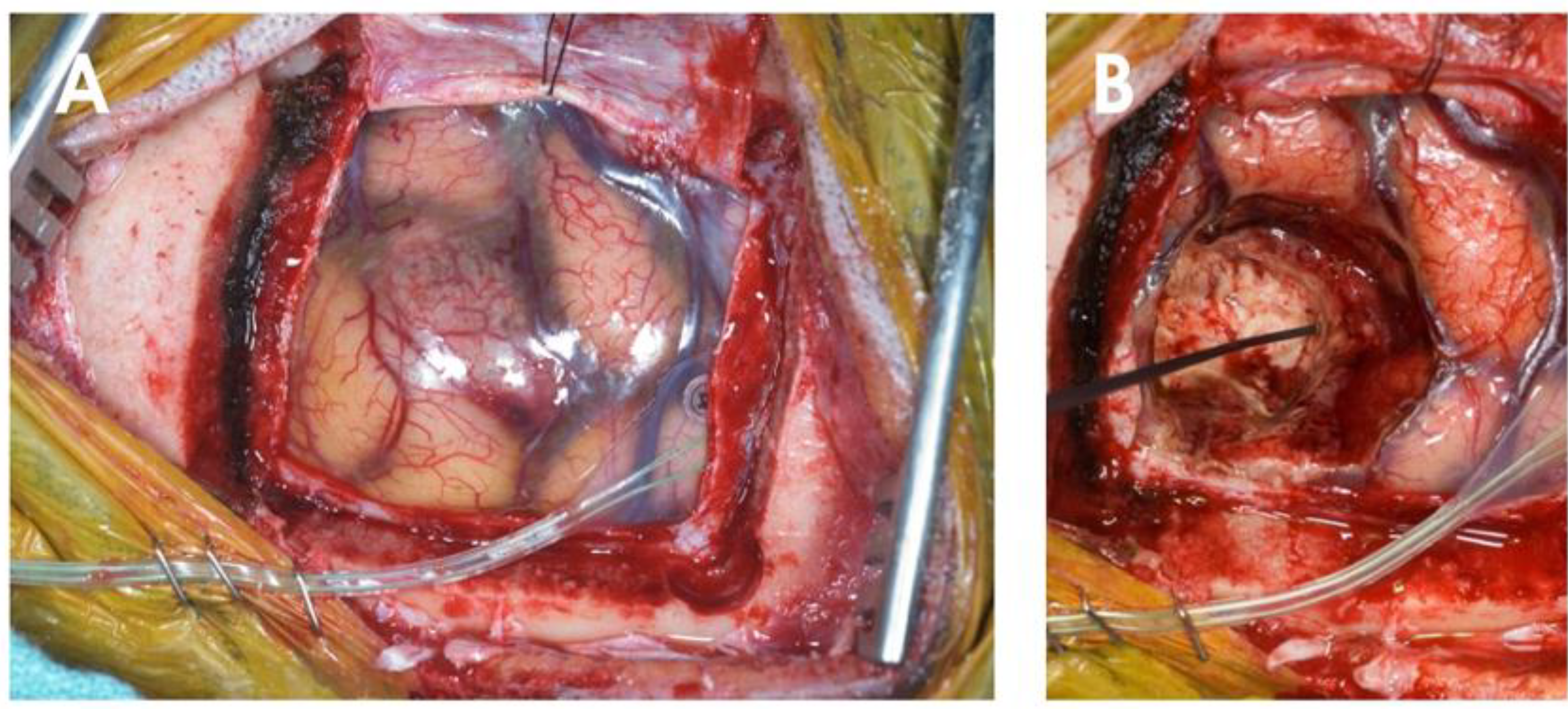
5. Stereotactic Radiosurgery
6. Chemotherapy
7. Targeted Molecular Therapy
8. Conclusions and Future Directions
References
- Horner, M.J.R.L.; Krapcho, M.; Neyman, N.; Aminou, R.; Howlader, N.; Altekruse, S.F.; Feuer, E.J.; Huang, L.; Mariotto, A.; Miller, B.A.; Lewis, D.R.; Eisner, M.P.; Stinchcomb, D.G.; Edwards, B.K. SEER Cancer Statistics Review, 1975–2006; National Cancer Institute: Bethesda, MD, USA, 2009. [Google Scholar]
- Amer, M.H.; Al-Sarraf, M.; Baker, L.H.; Vaitkevicius, V.K. Malignant melanoma and central nervous system metastases: Incidence, diagnosis, treatment and survival. Cancer 1978, 42, 660–668. [Google Scholar] [CrossRef]
- Barnholtz-Sloan, J.S.; Sloan, A.E.; Davis, F.G.; Vigneau, F.D.; Lai, P.; Sawaya, R.E. Incidence proportions of brain metastases in patients diagnosed (1973 to 2001) in the Metropolitan Detroit Cancer Surveillance System. J. Clin. Oncol. 2004, 22, 2865–2872. [Google Scholar] [CrossRef]
- Budman, D.R.; Camacho, E.; Wittes, R.E. The current causes of death in patients with malignant melanoma. Eur. J. Cancer 1978, 14, 327–330. [Google Scholar]
- Bullard, D.E.; Cox, E.B.; Seigler, H.F. Central nervous system metastases in malignant melanoma. Neurosurgery 1981, 8, 263. [Google Scholar]
- Hofmann, M.A.; Coll, S.H.; Kuchler, I.; Kiecker, F.; Wurm, R.; Sterry, W.; Trefzer, U. Prognostic factors and impact of treatment in melanoma brain metastases: Better prognosis for women? Dermatology 2007, 215, 10–16. [Google Scholar] [CrossRef]
- Sampson, J.H.; Carter, J.H., Jr.; Friedman, A.H.; Seigler, H.F. Demographics, prognosis, and therapy in 702 patients with brain metastases from malignant melanoma. J. Neurosurg. 1998, 88, 11–20. [Google Scholar]
- Sloan, A.E.; Nock, C.J.; Einstein, D.B. Diagnosis and treatment of melanoma brain metastasis: A literature review. Cancer Contr. 2009, 16, 248–255. [Google Scholar]
- Peacock, K.H.; Lesser, G.J. Current therapeutic approaches in patients with brain metastases. Curr. Treat. Options. Oncol. 2006, 7, 479–489. [Google Scholar]
- Barranco, S.C.; Romsdahl, M.M.; Humphrey, R.M. The radiation response of human malignant melanoma cells grown in vitro. Cancer Res. 1971, 31, 830–833. [Google Scholar]
- Komarnicky, L.T.; Phillips, T.L.; Martz, K.; Asbell, S.; Isaacson, S.; Urtasun, R. A randomized phase III protocol for the evaluation of misonidazole combined with radiation in the treatment of patients with brain metastases (RTOG-7916). Int. J. Radiat. Oncol. Biol. Phys. 1991, 20, 53–58. [Google Scholar] [CrossRef]
- Phillips, T.L.; Scott, C.B.; Leibel, S.A.; Rotman, M.; Weigensberg, I.J. Results of a randomized comparison of radiotherapy and bromodeoxyuridine with radiotherapy alone for brain metastases: report of RTOG trial 890–5. Int. J. Radiat. Oncol. Biol. Phys. 1995, 33, 339–348. [Google Scholar] [CrossRef]
- Sause, W.T.; Crowley, J.J.; Morantz, R.; Rotman, M.; Mowry, P.A.; Bouzaglou, A.; Borst, J.R.; Selin, H. Solitary brain metastasis: Results of an RTOG/SWOG protocol evaluation surgery + RT versus RT alone. Am. J. Clin. Oncol. 1990, 13, 427–432. [Google Scholar] [CrossRef]
- Carella, R.J.; Gelber, R.; Hendrickson, F.; Berry, H.C.; Cooper, J.S. Value of radiation therapy in the management of patients with cerebral metastases from malignant melanoma: Radiation therapy oncology group brain metastases study I and II. Cancer 1980, 45, 679–683. [Google Scholar]
- Cooper, J.S.; Carella, R. Radiotherapy of intracerebral metastatic malignant melanoma. Radiology 1980, 134, 735–738. [Google Scholar]
- Ellerhorst, J.; Strom, E.; Nardone, E.; McCutcheon, I. Whole brain irradiation for patients with metastatic melanoma: A review of 87 cases. Int. J. Radiat. Oncol. Biol. Phys. 2001, 49, 93–97. [Google Scholar]
- Stridsklev, I.C.; Hagen, S.; Klepp, O. Radiation therapy for brain metastases from malignant melanoma. Acta Radiol. Oncol. 1984, 23, 231–235. [Google Scholar] [CrossRef]
- Chang, E.L.; Wefel, J.S.; Hess, K.R.; Allen, P.K.; Lang, F.F.; Kornguth, D.G.; Arbuckle, R.B.; Swint, J.M.; Shiu, A.S.; Maor, M.H.; Meyers, C.A. Neurocognition in patients with brain metastases treated with radiosurgery or radiosurgery plus whole-brain irradiation: A randomised controlled trial. Lancet Oncol. 2009, 10, 1037–1044. [Google Scholar] [CrossRef]
- Hart, M.G.; Grant, R.; Walker, M.; Dickinson, H. Surgical resection and whole brain radiation therapy versus whole brain radiation therapy alone for single brain metastases. Cochrane Database Syst. Rev. 2005, CD003292. [Google Scholar]
- Mintz, A.H.; Kestle, J.; Rathbone, M.P.; Gaspar, L.; Hugenholtz, H.; Fisher, B.; Duncan, G.; Skingley, P.; Foster, G.; Levine, M. A randomized trial to assess the efficacy of surgery in addition to radiotherapy in patients with a single cerebral metastasis. Cancer 1996, 78, 1470–1476. [Google Scholar]
- Patchell, R.A.; Tibbs, P.A.; Walsh, J.W.; Dempsey, R.J.; Maruyama, Y.; Kryscio, R.J.; Markesbery, W.R.; Macdonald, J.S.; Young, B. A randomized trial of surgery in the treatment of single metastases to the brain. N. Engl. J. Med. 1990, 322, 494–500. [Google Scholar]
- Vecht, C.J.; Haaxma-Reiche, H.; Noordijk, E.M.; Padberg, G.W.; Voormolen, J.H.; Hoekstra, F.H.; Tans, J.T.; Lambooij, N.; Metsaars, J.A.; Wattendorff, A.R.; et al. Treatment of single brain metastasis: radiotherapy alone or combined with neurosurgery? Ann. Neurol. 1993, 33, 583–590. [Google Scholar] [CrossRef]
- Chang, S.D.; Adler, J.R., Jr. Current treatment of patients with multiple brain metastases. Neurosurg. Focus 2000, 9, e5. [Google Scholar]
- Paek, S.H.; Audu, P.B.; Sperling, M.R.; Cho, J.; Andrews, D.W. Reevaluation of surgery for the treatment of brain metastases: Review of 208 patients with single or multiple brain metastases treated at one institution with modern neurosurgical techniques. Neurosurgery 2005, 56, 1021–1034. [Google Scholar]
- Suki, D.; Abouassi, H.; Patel, A.J.; Sawaya, R.; Weinberg, J.S.; Groves, M.D. Comparative risk of leptomeningeal disease after resection or stereotactic radiosurgery for solid tumor metastasis to the posterior fossa. J. Neurosurg. 2008, 108, 248–257. [Google Scholar] [CrossRef]
- Suki, D.; Hatiboglu, M.A.; Patel, A.J.; Weinberg, J.S.; Groves, M.D.; Mahajan, A.; Sawaya, R. Comparative risk of leptomeningeal dissemination of cancer after surgery or stereotactic radiosurgery for a single supratentorial solid tumor metastasis. Neurosurgery 2009, 64, 664–674. [Google Scholar]
- Niranjan, A.; Gobbel, G.T.; Kondziolka, D.; Flickinger, J.C.; Lunsford, L.D. Experimental radiobiological investigations into radiosurgery: present understanding and future directions. Neurosurgery 2004, 55, 495–504. [Google Scholar] [CrossRef]
- Mehta, M.P.; Rozental, J.M.; Levin, A.B.; Mackie, T.R.; Kubsad, S.S.; Gehring, M.A.; Kinsella, T.J. Defining the role of radiosurgery in the management of brain metastases. Int. J. Radiat. Oncol. Biol. Phys. 1992, 24, 619–625. [Google Scholar] [CrossRef]
- Brown, P.D.; Brown, C.A.; Pollock, B.E.; Gorman, D.A.; Foote, R.L. Stereotactic radiosurgery for patients with "radioresistant" brain metastases. Neurosurgery 2002, 51, 656–665. [Google Scholar]
- Mathieu, D.; Kondziolka, D.; Cooper, P.B.; Flickinger, J.C.; Niranjan, A.; Agarwala, S.; Kirkwood, J.; Lunsford, L.D. Gamma knife radiosurgery in the management of malignant melanoma brain metastases. Neurosurgery 2007, 60, 471–481. [Google Scholar]
- Mingione, V.; Oliveira, M.; Prasad, D.; Steiner, M.; Steiner, L. Gamma surgery for melanoma metastases in the brain. J. Neurosurg. 2002, 96, 544–551. [Google Scholar] [CrossRef]
- Selek, U.; Chang, E.L.; Hassenbusch, S.J., 3rd; Shiu, A.S.; Lang, F.F.; Allen, P.; Weinberg, J.; Sawaya, R.; Maor, M.H. Stereotactic radiosurgical treatment in 103 patients for 153 cerebral melanoma metastases. Int. J. Radiat. Oncol. Biol. Phys. 2004, 59, 1097–1106. [Google Scholar] [CrossRef]
- Fife, K.M.; Colman, M.H.; Stevens, G.N.; Firth, I.C.; Moon, D.; Shannon, K.F.; Harman, R.; Petersen-Schaefer, K.; Zacest, A.C.; Besser, M.; Milton, G.W.; McCarthy, W.H.; Thompson, J.F. Determinants of outcome in melanoma patients with cerebral metastases. J. Clin. Oncol. 2004, 22, 1293–1300. [Google Scholar] [CrossRef]
- Wronski, M.; Arbit, E. Surgical treatment of brain metastases from melanoma: A retrospective study of 91 patients. J. Neurosurg. 2000, 93, 9–18. [Google Scholar] [CrossRef]
- Zacest, A.C.; Besser, M.; Stevens, G.; Thompson, J.F.; McCarthy, W.H.; Culjak, G. Surgical management of cerebral metastases from melanoma: outcome in 147 patients treated at a single institution over two decades. J. Neurosurg. 2002, 96, 552–558. [Google Scholar] [CrossRef]
- Muacevic, A.; Wowra, B.; Siefert, A.; Tonn, J.C.; Steiger, H.J.; Kreth, F.W. Microsurgery plus whole brain irradiation versus Gamma Knife surgery alone for treatment of single metastases to the brain: a randomized controlled multicentre phase III trial. J. Neurooncol. 2008, 87, 299–307. [Google Scholar] [CrossRef]
- Smith, M.L.; Lee, J.Y. Stereotactic radiosurgery in the management of brain metastasis. Neurosurg. Focus. 2007, 22, E5. [Google Scholar]
- Delattre, J.Y.; Krol, G.; Thaler, H.T.; Posner, J.B. Distribution of brain metastases. Arch. Neurol. 1988, 45, 741–744. [Google Scholar] [CrossRef]
- Aoyama, H.; Shirato, H.; Tago, M.; Nakagawa, K.; Toyoda, T.; Hatano, K.; Kenjyo, M.; Oya, N.; Hirota, S.; Shioura, H.; Kunieda, E.; Inomata, T.; Hayakawa, K.; Katoh, N.; Kobashi, G. Stereotactic radiosurgery plus whole-brain radiation therapy vs. stereotactic radiosurgery alone for treatment of brain metastases: a randomized controlled trial. JAMA 2006, 295, 2483–2491. [Google Scholar] [CrossRef]
- Patchell, R.A.; Tibbs, P.A.; Regine, W.F.; Dempsey, R.J.; Mohiuddin, M.; Kryscio, R.J.; Markesbery, W.R.; Foon, K.A.; Young, B. Postoperative radiotherapy in the treatment of single metastases to the brain: a randomized trial. JAMA 1998, 280, 1485–1489. [Google Scholar] [CrossRef]
- Jagannathan, J.; Yen, C.P.; Ray, D.K.; Schlesinger, D.; Oskouian, R.J.; Pouratian, N.; Shaffrey, M.E.; Larner, J.; Sheehan, J.P. Gamma Knife radiosurgery to the surgical cavity following resection of brain metastases. J. Neurosurg. 2009, 111, 431–438. [Google Scholar] [CrossRef]
- Mathieu, D.; Kondziolka, D.; Flickinger, J.C.; Fortin, D.; Kenny, B.; Michaud, K.; Mongia, S.; Niranjan, A.; Lunsford, L.D. Tumor bed radiosurgery after resection of cerebral metastases. Neurosurgery 2008, 62, 817–823. [Google Scholar]
- Franciosi, V.; Cocconi, G.; Michiara, M.; Di Costanzo, F.; Fosser, V.; Tonato, M.; Carlini, P.; Boni, C.; Di Sarra, S. Front-line chemotherapy with cisplatin and etoposide for patients with brain metastases from breast carcinoma, nonsmall cell lung carcinoma or malignant melanoma: A prospective study. Cancer 1999, 85, 1599–1605. [Google Scholar] [CrossRef]
- Madajewicz, S.; Karakousis, C.; West, C.R.; Caracandas, J.; Avellanosa, A.M. Malignant melanoma brain metastases. review of roswell park memorial institute experience. Cancer 1984, 53, 2550–2552. [Google Scholar] [CrossRef]
- Agarwala, S.S.; Kirkwood, J.M.; Gore, M.; Dreno, B.; Thatcher, N.; Czarnetski, B.; Atkins, M.; Buzaid, A.; Skarlos, D.; Rankin, E.M. Temozolomide for the treatment of brain metastases associated with metastatic melanoma: a phase II study. J. Clin. Oncol. 2004, 22, 2101–2107. [Google Scholar] [CrossRef]
- Atkins, M.B.; Sosman, J.A.; Agarwala, S.; Logan, T.; Clark, J.I.; Ernstoff, M.S.; Lawson, D.; Dutcher, J.P.; Weiss, G.; Curti, B.; Margolin, K.A. Temozolomide, thalidomide, and whole brain radiation therapy for patients with brain metastasis from metastatic melanoma: A phase II cytokine working group study. Cancer 2008, 113, 2139–2245. [Google Scholar] [CrossRef]
- Denkins, Y.; Reiland, J.; Roy, M.; Sinnappah-Kang, N.D.; Galjour, J.; Murry, B.P.; Blust, J.; Aucoin, R.; Marchetti, D. Brain metastases in melanoma: Roles of neurotrophins. Neuro. Oncol. 2004, 6, 154–165. [Google Scholar] [CrossRef]
- Perides, G.; Zhuge, Y.; Lin, T.; Stins, M.F.; Bronson, R.T.; Wu, J.K. The fibrinolytic system facilitates tumor cell migration across the blood-brain barrier in experimental melanoma brain metastasis. BMC Cancer 2006, 6, 56. [Google Scholar] [CrossRef]
- Rolland, Y.; Demeule, M.; Fenart, L.; Beliveau, R. Inhibition of melanoma brain metastasis by targeting melanotransferrin at the cell surface. Pigment Cell Melanoma Res. 2009, 22, 86–98. [Google Scholar] [CrossRef]
- Xie, T.X.; Huang, F.J.; Aldape, K.D.; Kang, S.H.; Liu, M.; Gershenwald, J.E.; Xie, K.; Sawaya, R.; Huang, S. Activation of stat3 in human melanoma promotes brain metastasis. Cancer Res. 2006, 66, 3188–3196. [Google Scholar]
- Devarajan, E.; Huang, S. STAT3 as a central regulator of tumor metastases. Curr. Mol. Med. 2009, 9, 626–633. [Google Scholar] [CrossRef]
- Zhang, R.D.; Price, J.E.; Schackert, G.; Itoh, K.; Fidler, I.J. Malignant potential of cells isolated from lymph node or brain metastases of melanoma patients and implications for prognosis. Cancer Res. 1991, 51, 2029–2035. [Google Scholar]
- Huang, F.J.; Steeg, P.S.; Price, J.E.; Chiu, W.T.; Chou, P.C.; Xie, K.; Sawaya, R.; Huang, S. Molecular basis for the critical role of suppressor of cytokine signaling-1 in melanoma brain metastasis. Cancer Res. 2008, 68, 9634–9642. [Google Scholar] [CrossRef]
- Levy, D.E.; Lee, C.K. What does Stat3 do? J. Clin. Invest. 2002, 109, 1143–1148. [Google Scholar]
© 2010 by the authors; licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution license (http://creativecommons.org/licenses/by/3.0/).
Share and Cite
Siu, T.L.; Huang, S. Cerebral Metastases from Malignant Melanoma: Current Treatment Strategies, Advances in Novel Therapeutics and Future Directions. Cancers 2010, 2, 364-375. https://doi.org/10.3390/cancers2020364
Siu TL, Huang S. Cerebral Metastases from Malignant Melanoma: Current Treatment Strategies, Advances in Novel Therapeutics and Future Directions. Cancers. 2010; 2(2):364-375. https://doi.org/10.3390/cancers2020364
Chicago/Turabian StyleSiu, Timothy L., and Suyun Huang. 2010. "Cerebral Metastases from Malignant Melanoma: Current Treatment Strategies, Advances in Novel Therapeutics and Future Directions" Cancers 2, no. 2: 364-375. https://doi.org/10.3390/cancers2020364
APA StyleSiu, T. L., & Huang, S. (2010). Cerebral Metastases from Malignant Melanoma: Current Treatment Strategies, Advances in Novel Therapeutics and Future Directions. Cancers, 2(2), 364-375. https://doi.org/10.3390/cancers2020364



