Ethnic Variation in Breastfeeding and Complimentary Feeding in the Republic of Ireland
Abstract
:1. Introduction
2. Methods
2.1. Study Design and Sample
2.2. Questionnaires and Measurements
2.3. Statistical Analysis and Dependent Variable
2.4. Definition of Covariates
2.5. Missing Data
3. Results
3.1. Characteristics of the Study Cohort
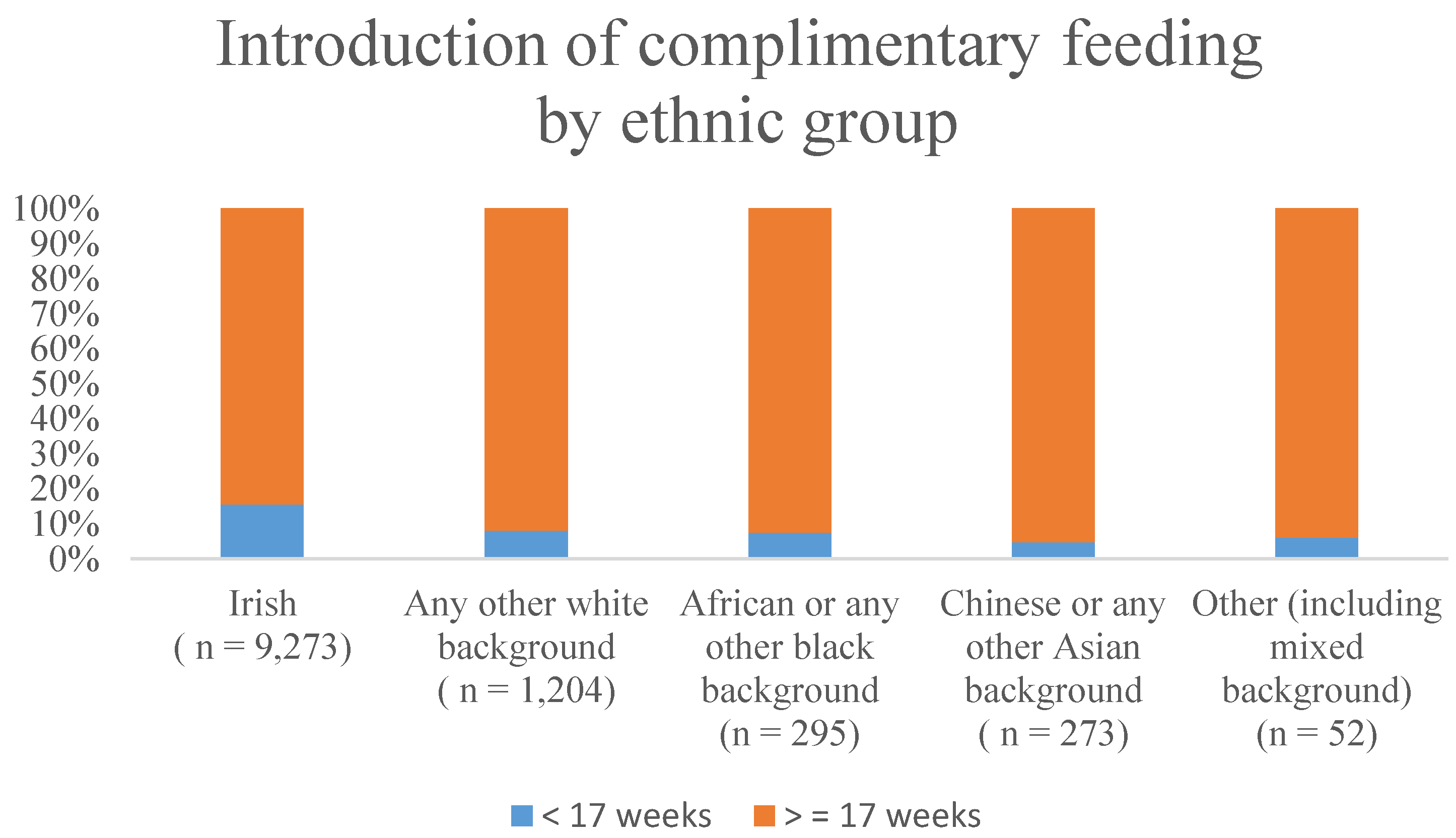
3.2. Percentage of Infants’ Breastfed and the Introduction of Complimentary Feeding in the <17 Weeks and ≥17 Weeks Categories Classified by Ethnic Group

| Characteristic | Primary Caregiver | Irish | Non-Irish | ||||
|---|---|---|---|---|---|---|---|
| Sample (n *) | Mean or % † | SD | Sample (n *) | Mean or % † | SD | ||
| Mean age | 31.7 | 5.3 | 30.9 | 5.4 | |||
| BMI primary carer kg/m2 | Underweight (less than 18.5) | 9275 | 2.5 | 1859 | 3.7 | ||
| Normal weight (18.5–24.9) | 50.5 | 51.1 | |||||
| Overweight (25–29.9) | 30.1 | 28.5 | |||||
| Obese (≥30) | 16.8 | 16.7 | |||||
| Having ever breastfed | Yes | 9273 | 49.5 | 1859 | 88.1 | ||
| No | 50.5 | 11.9 | |||||
| Having exclusively breastfed ‡ | Yes | 4592 | 39.3 | 1634 | 66.5 | ||
| No | 10.2 | 21.4 | |||||
| Mean duration of any breastfeeding (days) ‡ | 4019 | 71.1 | 66.4 | 1153 | 95.8 | 69.2 | |
| Mean duration of exclusive breastfeeding (days) ‡ | 3556 | 74.7 | 62 | 1158 | 95.9 | 63.2 | |
| Introduction of complimentary feeding | <17 weeks | 9151 | 15.5 | 1755 | 7.6 | ||
| ≥17 weeks | 84.5 | 92.4 | |||||
3.3. Predictors of Early Complimentary Feeding
3.4. Effects of Acculturation on Breastfeeding Initiation and Early Complimentary Feeding

| Characteristics | Complimentary Feeding Introduction * | |||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Total | <17 Weeks | ≥17 Weeks | Unadjusted † | Adjusted ‡ | ||||||||
| n | % γ | n | % η | n | % η | OR | p § | OR | 95% CI | p δ | ||
| Primary caregiver age (years) | ||||||||||||
| ≥35 | 3467 | 31.8 | 426 | 12.3 | 3041 | 87.7 | 0.467 | 0.606 | 0.494 | 0.744 | <0.001 | |
| 25–34 | 6119 | 56.1 | 823 | 13.4 | 5296 | 86.6 | 0.519 | 0.664 | 0.555 | 0.794 | <0.001 | |
| ≤24 | 1321 | 12.1 | 304 | 23 | 1017 | 77 | 1.0 $ | <0.001 | 1.0 $ | <0.001 | ||
| Maternal education | ||||||||||||
| Third level education | 5330 | 48.9 | 557 | 10.5 | 4773 | 89.5 | 0.534 | 0.82 | 0.602 | 1.117 | 0.208 | |
| Secondary level education | 5189 | 47.6 | 926 | 17.8 | 4263 | 82.2 | 0.994 | 1.031 | 0.773 | 1.374 | 0.835 | |
| No formal or primary education | 378 | 3.5 | 68 | 18 | 310 | 82 | 1.0$ | <0.001 | 1.0 $ | 0.004 | ||
| Household class | ||||||||||||
| Professional, managerial and technical workers | 5228 | 47.9 | 578 | 11.1 | 4650 | 88.9 | 1.0 $ | 1.0 $ | 0.001 | |||
| Non-manual | 1983 | 18.2 | 332 | 16.7 | 1651 | 83.3 | 1.62 | 1.179 | 1.001 | 1.387 | 0.048 | |
| Skilled and semi-skilled manual | 2428 | 22.3 | 377 | 15.5 | 2051 | 84.5 | 1.478 | 1.111 | 0.941 | 1.311 | 0.214 | |
| Unskilled and all other gainfully occupied and unknown | 283 | 2.6 | 66 | 23.3 | 217 | 76.7 | 2.43 | 1.85 | 1.346 | 2.544 | <0.001 | |
| Never worked at all | 985 | 9 | 200 | 20.3 | 785 | 79.7 | 2.051 | <0.001 | 0.972 | 0.752 | 1.258 | 0.83 |
| Household type | ||||||||||||
| One parent one child under 18 years | 799 | 7.3 | 177 | 22.2 | 622 | 77.8 | 1.042 | 0.925 | 0.72 | 1.189 | 0.545 | |
| One parent two or more children under 18 years | 831 | 7.6 | 178 | 21.4 | 653 | 78.6 | 1.0$ | 1.0 $ | <0.001 | |||
| Two parents one child under 18 years | 3536 | 32.4 | 385 | 10.9 | 3151 | 89.1 | 0.447 | 0.614 | 0.479 | 0.788 | <0.001 | |
| Two parents two or more children under 18 years | 5740 | 52.6 | 813 | 14.2 | 4927 | 85.8 | 0.604 | <0.001 | 0.827 | 0.659 | 1.038 | 0.101 |
| BMI primary carer | ||||||||||||
| Underweight (less than 18.5 kg/m2) | 298 | 2.7 | 43 | 14.4 | 255 | 85.6 | 1.132 | 0.903 | 0.639 | 1.274 | 0.569 | |
| Normal weight (18.5–24.9 kg/m2) | 5519 | 50.6 | 714 | 12.9 | 4805 | 87.1 | 1.0 $ | 1.0 $ | 0.001 | |||
| Overweight (25–29.9 kg/m2) | 3264 | 29.9 | 456 | 14 | 2808 | 86 | 1.093 | 1.074 | 0.942 | 1.224 | 0.284 | |
| Obese (≥30 kg/m2) | 1825 | 16.7 | 340 | 18.6 | 1485 | 81.4 | 1.542 | <0.001 | 1.336 | 1.151 | 1.551 | <0.001 |
| Primary carer ethnicity&length of stay in the ROI | ||||||||||||
| Irish | 9188 | 84.2 | 1424 | 15.5 | 7764 | 84.5 | 1.0 $ | 1.0 $ | 0.001 | |||
| Non-Irish arrived within the last year-5 years ago | 964 | 8.8 | 62 | 6.4 | 902 | 93.6 | 0.374 | 0.493 | 0.371 | 0.656 | <0.001 | |
| Non-Irish arrived 6–10 years ago | 570 | 5.2 | 44 | 7.7 | 526 | 92.3 | 0.456 | 0.566 | 0.408 | 0.785 | 0.001 | |
| Non-Irish arrived 11–>20 years ago | 184 | 1.7 | 23 | 12.5 | 161 | 87.5 | 0.784 | <0.001 | 0.969 | 0.613 | 1.532 | 0.893 |
| Exclusive breastfeeding duration | ||||||||||||
| 0–30 days | 1579 | 14.5 | 241 | 15.3 | 1338 | 84.7 | 0.818 | 0.954 | 0.776 | 1.172 | 0.652 | |
| >30–60 days | 770 | 7.1 | 101 | 13.1 | 669 | 86.9 | 0.687 | 0.864 | 0.665 | 1.122 | 0.272 | |
| >60–90 days | 549 | 5 | 69 | 12.6 | 480 | 87.4 | 0.652 | 0.813 | 0.604 | 1.094 | 0.172 | |
| >90 days | 1782 | 16.3 | 17 | 1 | 1765 | 99 | 0.044 | 0.061 | 0.037 | 0.101 | <0.001 | |
| No exclusive breastfeeding | 6227 | 57.1 | 1125 | 18.1 | 5102 | 81.9 | 1.0 $ | <0.001 | 1.0 $ | <0.001 | ||
4. Discussion
5. Strengths and Limitations
6. Conclusions
Acknowledgments
Author Contributions
Conflicts of Interest
References
- Lanigan, J.; Singhal, A. Early nutrition and long-term health: A practical approach. Proc. Nutr. Soc. 2009, 68, 422–429. [Google Scholar] [CrossRef]
- Koletzko, B.; Brands, B.; Poston, L.; Godfrey, K.; Demmelmair, H. Early nutrition programming of long-term health. Proc. Nutr. Soc. 2012, 71, 371–378. [Google Scholar] [CrossRef]
- Singhal, A.; Lucas, A. Early origins of cardiovascular disease: Is there a unifying hypothesis? Lancet 2004, 363, 1642–1645. [Google Scholar] [CrossRef]
- Complementary Feeding: Report of the Global Consultation, and Summary of Guiding Principles for Complementary Feeding of the Breastfed Child. Available online: http://www.who.int/maternal_child_adolescent/documents/924154614X/en/ (accessed on the 9 February 2014).
- Agostoni, C.; Decsi, T.; Fewtrell, M.; Goulet, O.; Kolacek, S.; Koletzko, B.; Michaelsen, K.F.; Moreno, L.; Puntis, J.; Rigo, J.; et al. Complementary feeding: A commentary by the ESPGHAN Committee on Nutrition. J. Pediatr. Gastroenterol. Nutr. 2008, 46, 99–110. [Google Scholar] [CrossRef]
- Wilson, A.C.; Forsyth, J.S.; Greene, S.A.; Irvine, L.; Hau, C.; Howie, P.W. Relation of infant diet to childhood health: Seven year follow up of cohort of children in Dundee infant feeding study. BMJ 1998, 316. [Google Scholar] [CrossRef]
- Huh, S.Y.; Rifas-Shiman, S.L.; Taveras, E.M.; Oken, E.; Gillman, M.W. Timing of solid food introduction and risk of obesity in preschool-aged children. Pediatrics 2011, 127, e544–e551. [Google Scholar] [CrossRef]
- Mihrshahi, S.; Battistutta, D.; Magarey, A.; Daniels, L.A. Determinants of rapid weight gain during infancy: Baseline results from the NOURISH randomised controlled trial. BMC Pediatr. 2011, 11. [Google Scholar] [CrossRef] [Green Version]
- Schack-Nielsen, L.; Sorensen, T.; Mortensen, E.L.; Michaelsen, K.F. Late introduction of complementary feeding, rather than duration of breastfeeding, may protect against adult overweight. Am. J. Clin. Nutr. 2010, 91, 619–627. [Google Scholar] [CrossRef]
- Cooke, L. The importance of exposure for healthy eating in childhood: A review. J. Hum. Nutr. Diet. 2007, 20, 294–301. [Google Scholar] [CrossRef]
- Nicklaus, S.; Boggio, V.; Chabanet, C.; Issanchou, S. A prospective study of food variety seeking in childhood, adolescence and early adult life. Appetite 2005, 44, 289–297. [Google Scholar] [CrossRef]
- Nicklaus, S. Children’s acceptance of new foods at weaning. Role of practices of weaning and of food sensory properties. Appetite 2011, 57, 812–815. [Google Scholar] [CrossRef]
- Grote, V.; Theurich, M.; Koletzko, B. Do complementary feeding practices predict the later risk of obesity? Curr. Opin. Clin. Nutr. Metab. Care. 2012, 15, 293–297. [Google Scholar] [CrossRef]
- Schiess, S.; Grote, V.; Scaglioni, S.; Luque, V.; Martin, F.; Stolarczyk, A.; Vecchi, F.; Koletzko, B. Introduction of complementary feeding in 5 European countries. J. Pediatr. Gastroenterol. Nutr. 2010, 50, 92–98. [Google Scholar] [CrossRef]
- Tarrant, R.C.; Younger, K.M.; Sheridan-Pereira, M.; White, M.J.; Kearney, J.M. Factors associated with weaning practices in term infants: A prospective observational study in Ireland. Br. J. Nutr. 2010, 104, 1544–1554. [Google Scholar] [CrossRef]
- Clayton, H.B.; Li, R.; Perrine, C.G.; Scanlon, K.S. Prevalence and reasons for introducing infants early to solid foods: Variations by milk feeding type. Pediatrics 2013, 131, e1108–e1114. [Google Scholar] [CrossRef]
- Avery, M.; Duckett, L.; Dodgson, J.; Savik, K.; Henly, S.J. Factors associated with very early weaning among primiparas intending to breastfeed. Matern. Child Health J. 1998, 2, 167–179. [Google Scholar] [CrossRef]
- Wijndaele, K.; Lakshman, R.; Landsbaugh, J.R.; Ong, K.K.; Ogilvie, D. Determinants of early weaning and use of unmodified cow’s milk in infants: A systematic review. J. Am. Diet. Assoc. 2009, 109, 2017–2028. [Google Scholar] [CrossRef]
- Department of Health and Children. Policy Change in Breastfeeding Guidelines; Department of Health and Children: Dublin, Ireland, 2003.
- FSAI. Scientific Recommendations for a National Infant Feeding Policy, 2nd ed.Food Safety Authority of Ireland: Dublin, Ireland, 2011.
- Euro-Peristat Project with SCPE and EUROCAT. European Perinatal Health Report. The Health and Care of Pregnant Women and Babies in Europe in 2010. Available online: www.europeristat.com (accessed on the 24 April 2014).
- McSweeney, M.; Kevany, J. A national survey of infant feeding practices in Ireland 1981: A preliminary report. Ir. Med. J. 1982, 75, 452–455. [Google Scholar]
- Brick, A.; Nolan, A. Explaining the increase in breastfeeding at hospital discharge in Ireland, 2004–2010. Ir. J. Med. Sci. 2013. [Google Scholar] [CrossRef]
- Department of Health and Children. A National Breastfeeding Policy for Ireland; Department of Health and Children: Dublin, Ireland, 1994.
- Department of Health and Children. Breastfeeding in Ireland: A Five Year Strategic Action Plan; Department of Health and Children: Dublin, Ireland, 2005.
- Tarrant, R.C.; Younger, K.M.; Sheridan-Pereira, M.; White, M.J.; Kearney, J.M. The prevalence and determinants of breast-feeding initiation and duration in a sample of women in Ireland. Public Health Nutr. 2010, 13, 760–770. [Google Scholar] [CrossRef]
- Begley, C.; Gallagher, L.; Clarke, M.; Carroll, M.; Millar, S. National Infant Feeding Survey 2008; Trinity College Dublin: Dublin, Ireland, 2009. [Google Scholar]
- Quail, A.; Williams, J.; McCrory, C.; Murray, A.; Thornton, M. Summary Guide to Wave 1 of the Infant Cohort (at 9 months) of Growing Up in Ireland. Available online: www.ucd.ie/issda/static/documentation/esri/GUI-SummaryGuideInfants.pdf (accessed on the 10 February 2014).
- Quail, A.; Williams, J.; McCrory, C.; Murray, A.; Thornton, M. Questionnaires for Wave 1 of the Infant Cohort [at nine months] of Growing Up in Ireland. Available online: http://www.ucd.ie/issda/static/documentation/esri/GUI-QuestionnairesInfants.pdf (accessed on the 10 February 2014).
- Kramer, M.S.; Kakuma, R. Optimal Duration of Exclusive Breastfeeding. Available online: www.who.int/rhl/reviews/CD003517.pdf (accessed on 24 April 2014).
- Department of Health and Children. Perinatal Statistics Report; Economic and Social Research Institute: Dublin, Ireland, 2012. [Google Scholar]
- Oakley, L.L.; Renfrew, M.J.; Kurinczuk, J.J.; Quigley, M.A. Factors associated with breastfeeding in England: an analysis by primary care trust. BMJ Open 2013, 3. [Google Scholar] [CrossRef]
- Parker, M.; Burnham, L.; Cook, J.; Sanchez, E.; Philipp, B.L.; Merewood, A. 10 Years after baby-friendly designation: Breastfeeding rates continue to increase in a US neonatal intensive care unit. J. Hum. Lact. 2013, 29, 354–358. [Google Scholar]
- Norris, S.; Collin, S.M.; Ingram, J. Breastfeeding practices among the old order Mennonites in Ontario, Canada: A multiple methods study. J. Hum. Lact. 2013, 29, 605–610. [Google Scholar]
- Belanoff, C.M.; McManus, B.M.; Carle, A.C.; McCormick, M.C.; Subramanian, S.V. Racial/ethnic variation in breastfeeding across the US: A multilevel analysis from the National Survey of Children’s Health, 2007. Matern. Child Health J. 2012, 16, S14–S26. [Google Scholar] [CrossRef]
- Bulk-Bunschoten, A.M.; Pasker-de Jong, P.C.; van Wouwe, J.P.; de Groot, C.J. Ethnic variation in infant-feeding practices in the Netherlands and weight gain at 4 months. J. Hum. Lact. 2008, 24, 42–49. [Google Scholar] [CrossRef]
- Ahluwalia, I.B.; Morrow, B.; D’Angelo, D.; Li, R. Maternity care practices and breastfeeding experiences of women in different racial and ethnic groups: Pregnancy Risk Assessment and Monitoring System [PRAMS]. Matern. Child Health J. 2012, 16, 1672–1678. [Google Scholar]
- Sparks, P.J. Racial/ethnic differences in breastfeeding duration among WIC-eligible families. Womens Health Issues 2011, 21, 374–382. [Google Scholar]
- Kelly, Y.J.; Watt, R.G.; Nazroo, J.Y. Racial/ethnic differences in breastfeeding initiation and continuation in the United Kingdom and comparison with findings in the United States. Pediatrics 2006, 118, e1428–e1435. [Google Scholar] [CrossRef]
- Ahluwalia, I.B.; D’Angelo, D.; Morrow, B.; McDonald, J.A. Association between acculturation and breastfeeding among Hispanic women: Data from the Pregnancy Risk Assessment and Monitoring System. J. Hum. Lact. 2012, 28, 167–173. [Google Scholar] [CrossRef]
- Chapman, D.J.; Perez-Escamilla, R. Acculturative type is associated with breastfeeding duration among low-income Latinas. Matern. Child Nutr. 2013, 9, 188–198. [Google Scholar]
- Haughton, J.; Gregorio, D.; Perez-Escamilla, R. Factors associated with breastfeeding duration among Connecticut Special Supplemental Nutrition Program for Women, Infants, and Children [WIC] participants. J. Hum. Lact. 2010, 26, 266–273. [Google Scholar] [CrossRef]
- Singh, G.K.; Kogan, M.D.; Dee, D.L. Nativity/immigrant status, race/ethnicity, and socioeconomic determinants of breastfeeding initiation and duration in the United States, 2003. Pediatrics 2007, 119, S38–S46. [Google Scholar] [CrossRef]
- Chen, S.; Binns, C.W.; Zhao, Y.; Maycock, B.; Liu, Y. Breastfeeding by Chinese mothers in Australia and China: The healthy migrant effect. J. Hum. Lact. 2013, 29, 246–252. [Google Scholar] [CrossRef]
- Zhou, Q.; Younger, K.M.; Kearney, J.M. An exploration of the knowledge and attitudes towards breastfeeding among a sample of Chinese mothers in Ireland. BMC Public Health 2010, 10. [Google Scholar] [CrossRef] [Green Version]
- Department of Health Australian Government. Available online: http://www.health.gov.au/breastfeeding (accessed on 24 April 2014).
- Mehta, U.J.; Siega-Riz, A.M.; Herring, A.H.; Adair, L.S.; Bentley, M.E. Pregravid body mass index is associated with early introduction of complementary foods. J. Acad. Nutr. Diet. 2012, 112, 1374–1379. [Google Scholar] [CrossRef]
- Children’s Physical Growth from Birth to Age 3. Available online: http://www.growingup.ie/index.php?id=61 (accessed on 24 April 2014).
- Van Rossem, L.; Kiefte-de Jong, J.C.; Looman, C.W.; Jaddoe, V.W.; Hofman, A.; Hokken-Koelega, A.C.; Mackenbach, J.P.; Moll, H.A.; Raat, H. Weight change before and after the introduction of solids: Results from a longitudinal birth cohort. Br. J. Nutr. 2013, 109, 370–375. [Google Scholar] [CrossRef]
- Griffiths, L.J.; Smeeth, L.; Hawkins, S.S.; Cole, T.J.; Dezateux, C. Effects of infant feeding practice on weight gain from birth to 3 years. Arch. Dis. Child. 2009, 94, 577–582. [Google Scholar] [CrossRef]
- Moorcroft, K.E.; Marshall, J.L.; McCormick, F.M. Association between timing of introducing solid foods and obesity in infancy and childhood: A systematic review. Matern. Child Nutr. 2011, 7, 3–26. [Google Scholar] [CrossRef]
- Woo, J.G.; Guerrero, M.L.; Ruiz-Palacios, G.M.; Peng, Y.M.; Herbers, P.M.; Yao, W.; Ortega, H.; Davidson, B.S.; McMahon, R.J.; Morrow, A.L. Specific infant feeding practices do not consistently explain variation in anthropometry at age 1 year in urban United States, Mexico, and China cohorts. J. Nutr. 2013, 143, 166–174. [Google Scholar] [CrossRef]
- Baker, J.L.; Michaelsen, K.F.; Sorensen, T.I.; Rasmussen, K.M. High prepregnant body mass index is associated with early termination of full and any breastfeeding in Danish women. Am. J. Clin. Nutr. 2007, 86, 404–411. [Google Scholar]
- Hilson, J.A.; Rasmussen, K.M.; Kjolhede, C.L. High prepregnant body mass index is associated with poor lactation outcomes among white, rural women independent of psychosocial and demographic correlates. J. Hum. Lact. 2004, 20, 18–29. [Google Scholar] [CrossRef]
- Li, R.; Jewell, S.; Grummer-Strawn, L. Maternal obesity and breast-feeding practices. Am. J. Clin. Nutr. 2003, 77, 931–936. [Google Scholar]
- Neville, M.C.; Morton, J. Physiology and endocrine changes underlying human lactogenesis II. J. Nutr. 2001, 131, 3005S–3008S. [Google Scholar]
© 2014 by the authors; licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution license (http://creativecommons.org/licenses/by/3.0/).
Share and Cite
Castro, P.D.; Layte, R.; Kearney, J. Ethnic Variation in Breastfeeding and Complimentary Feeding in the Republic of Ireland. Nutrients 2014, 6, 1832-1849. https://doi.org/10.3390/nu6051832
Castro PD, Layte R, Kearney J. Ethnic Variation in Breastfeeding and Complimentary Feeding in the Republic of Ireland. Nutrients. 2014; 6(5):1832-1849. https://doi.org/10.3390/nu6051832
Chicago/Turabian StyleCastro, Patricia Dominguez, Richard Layte, and John Kearney. 2014. "Ethnic Variation in Breastfeeding and Complimentary Feeding in the Republic of Ireland" Nutrients 6, no. 5: 1832-1849. https://doi.org/10.3390/nu6051832




