Risk of Suboptimal Iodine Intake in Pregnant Norwegian Women
Abstract
:1. Introduction
2. Materials and Methods
2.1. Population and Study Sample
2.2. Dietary Information
2.3. Other Variables
2.4. Statistical Methods
3. Results
| All | Iodine containing supplement user | ||||||
|---|---|---|---|---|---|---|---|
| No | Yes | ||||||
| n (%) | 61,904 | 42,329 (68.4) | 19,575 (31.6) | ||||
| Iodine intake, μg/day | n | % | Cum% | n | Cum% | n | Cum% |
| <50 | 674 | 1.1 | 1.1 | 667 | 1.6 | 7 | 0.0 |
| 50–70 | 2272 | 3.7 | 4.8 | 2208 | 6.8 | 64 | 0.4 |
| 70–100 | 7006 | 11.3 | 16.1 | 6658 | 22.5 | 348 | 2.1 |
| 100–150 | 16,061 | 25.9 | 42.0 | 14,267 | 56.2 | 1794 | 11.3 |
| 150–175 | 7572 | 12.2 | 54.3 | 6044 | 70.5 | 1528 | 19.1 |
| 175–250 | 14,886 | 24.0 | 78.3 | 8970 | 91.7 | 5916 | 49.3 |
| 250–500 | 12,663 | 20.5 | 98.8 | 3463 | 99.9 | 9200 | 96.3 |
| ≥500 | 770 | 1.2 | 100 | 52 | 100 | 718 | 100 |
| Iodine from food | Total iodine | |||||
|---|---|---|---|---|---|---|
| n (%) | Median (P5, P95) | p-Value * | Median (P5, P95) | p-Value * | ||
| μg/day | μg/day | |||||
| All | 61,904 | 141 (65, 280) | 166 (71, 369) | |||
| Maternal age | ||||||
| <25 years | 6880 (11.1) | 141 (61, 305) | 0.406 | 164 (65, 389) | 0.207 | |
| 25–29 years | 20,926 (38.3) | 141 (64, 282) | 167 (70, 373) | |||
| 30–34 years | 23,554 (38.0) | 141 (66, 274) | 165 (73, 362) | |||
| ≥35 years | 10,544 (17.0) | 141 (67, 275) | 166 (74, 367) | |||
| Parity | ||||||
| Nulliparous | 32,053 (51.8) | 139 (64, 280) | <0.001 | 169 (71, 381) | ||
| Primiparous | 19,262 (31.1) | 141 (65, 279) | 162 (70, 357) | <0.001 | ||
| Multiparous | 10,589 (17.1) | 147 (67, 284) | 164 (72, 356) | |||
| Maternal education | ||||||
| ≤12 years | 19,809 (32.0) | 140 (60, 295) | 0.607 | 163 (65, 372) | <0.001 | |
| 13–16 years | 26,612 (43.0) | 141 (66, 276) | 167 (73, 369) | |||
| ≥17 years | 15,484 (25.0) | 141 (70, 267) | 167 (76, 366) | |||
| Marital status | ||||||
| Married/cohabiting | 59,726 (96.5) | 141 (65, 279) | 0.083 | 166 (71, 368) | 0.246 | |
| Not married/cohabiting | 2178 (3.5) | 143 (61, 302) | 168 (67, 388) | |||
| Smoking prior to pregnancy | ||||||
| Non smoker | 44,005 (71.1) | 142 (66, 277) | 0.026 | 166 (72, 367) | 0.015 | |
| Occasional smoker | 6376 (10.3) | 140 (66, 276) | 165 (72, 368) | |||
| Daily smoker | 11,523 (18.6) | 139 (61, 294) | 164 (66, 377) | |||
| Pre-pregnancy BMI | ||||||
| <18.5 kg/m2 | 1809 (2.9) | 140 (62, 271) | <0.001 | 168 (71, 376) | <0.001 | |
| 18.5–24.9 kg/m2 | 40,457 (65.4) | 142 (67, 278) | 167 (74, 368) | |||
| 25–29.9 kg/m2 | 13,604 (22.0) | 140 (62, 285) | 163 (67, 372) | |||
| ≥30 kg/m2 | 6034 (9.7) | 137 (58, 288) | 160 (63, 372) | |||
| Income | ||||||
| Both <300,000 NOK | 18,929 (30.6) | 143 (63, 291) | <0.001 | 167 (69, 371) | 0.073 | |
| One ≥300,000 NOK | 26,419 (42.7) | 142 (65, 283) | 166 (71, 371) | |||
| Both ≥300,000 NOK | 16,556 (26.7) | 138 (67, 260) | 164 (74, 363) | |||
| Milk and yogurt intake | ||||||
| <200 mL/day | 17,187 (27,8) | 88 (49, 141) | <0.001 | 102 (53, 262) | <0.001 | |
| 200–399 mL/day | 13,378 (21.6) | 122 (84, 175) | 137 (88, 296) | |||
| ≥400 mL/day | 31,339 (50.6) | 183 (123, 320) | 209 (129, 410) | |||
| Fish and seafood intake | ||||||
| <20 g/day | 14,195 (22.9) | 117 (49, 252) | <0.001 | 141 (54, 346) | <0.001 | |
| ≥20 g/day | 47,709 (77.1) | 148 (74, 286) | 172 (79, 376) | |||
| Egg intake | ||||||
| <8 g/day | 19,921 (32.2) | 129 (56, 269) | <0.001 | 153 (61, 357) | <0.001 | |
| ≥8 g/day | 41,983 (67.8) | 146 (71, 283) | 171 (77, 375 ) | |||
| Iodine from supplements | ||||||
| No | 42,329 (68.4) | 141 (65, 279) | <0.001 | 141 (65, 279) | <0.001 | |
| Yes | 19,575 (31.6) | 141 (65, 282) | 252 (122, 466) | |||
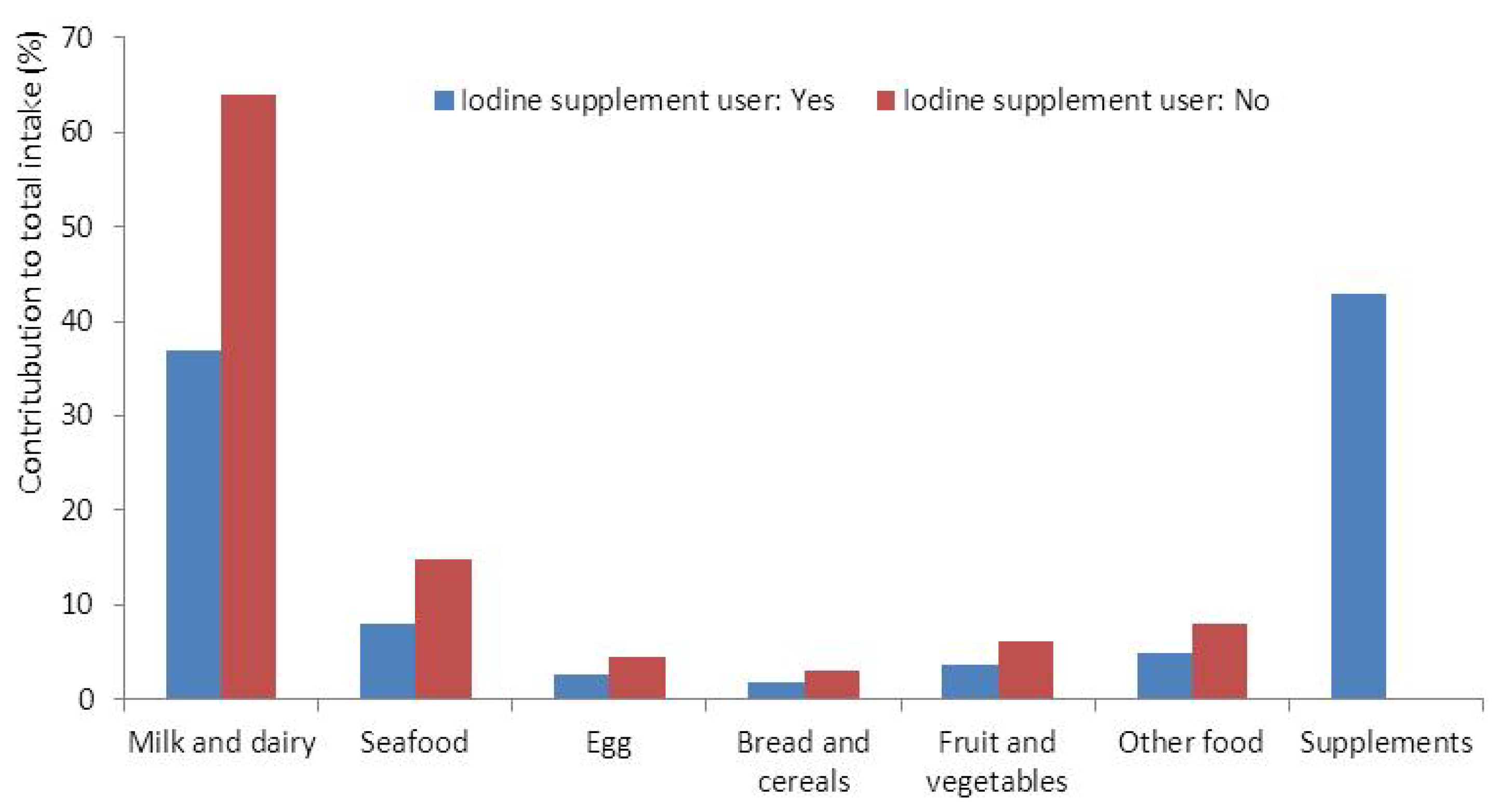


| Iodine < 100 μg/day | Unadjusted model | Adjusted model 1 | ||
|---|---|---|---|---|
| n (%) | OR (95% CI) | OR (95% CI) | ||
| Iodine from supplements | ||||
| Yes | 419 (2.1) | 1 | 1 | |
| No | 9533 (22.5) | 13.3 (12.0, 14.7) | 58.6 (52.0, 66.2) | |
| Low milk/yoghurt intake | ||||
| No: ≥200 mL/day | 1723 (3.9) | 1 | 1 | |
| Yes: <200 mL/day | 8229 (47.9) | 22.9 (21.7, 24.3) | 42.2 (39.4, 45.7) | |
| Low fish and seafood intake | ||||
| No: ≥20 g/day | 6093 (12.8) | 1 | 1 | |
| Yes: <20 g/day | 3859 (27.2) | 2.6 (2.4, 2.7) | 3.8 (3.5, 4.1) | |
| Low egg intake | ||||
| No: ≥8 g/day | 5584 (13.3) | 1 | 1 | |
| Yes: <8 g/day | 4368 (21.9) | 1.8 (1.7, 1.9) | 1.5 (1.4, 1.6) | |
| Year | 2002 | 2003 | 2004 | 2005 | 2006 | 2007 | 2008 |
|---|---|---|---|---|---|---|---|
| Number of women | 3997 | 10,552 | 11,020 | 11,286 | 11,921 | 10,246 | 2882 |
| Iodine <100 μg/day (%) | 14.8 | 15.6 | 16.2 | 15.9 | 15.7 | 16.3 | 17.1 |
| Iodine supplement use (%) | 26.5 | 25.8 | 31.6 | 34.5 | 34.7 | 32.9 | 31.5 |
| Iodine from food, median μg/day | 147 | 144 | 141 | 141 | 140 | 138 | 137 |
| Iodine from milk and yogurt, median μg/day | 75 | 74 | 72 | 73 | 70 | 68 | 66 |
| Iodine from other dairy products, median μg/day | 14 | 14 | 14 | 14 | 14 | 14 | 14 |
| Iodine contributed by seafood, median μg/day | 23 | 22 | 21 | 20 | 20 | 19 | 19 |
| Milk and yogurt, median mL/day | 413 | 409 | 402 | 408 | 400 | 381 | 363 |
| Seafood, median g/day | 35 | 34 | 33 | 33 | 33 | 33 | 32 |

4. Discussion
5. Conclusions
Acknowledgments
Conflict of Interest
References
- Delange, F. Iodine deficiency in Europe and its consequences: An update. Eur. J. Nucl. Med. Mol. Imaging 2002, 29, S404–S416. [Google Scholar] [CrossRef]
- Andersson, M.; Karumbunathan, V.; Zimmermann, M.B. Global iodine status in 2011 and trends over the past decade. J. Nutr. 2012, 142, 744–750. [Google Scholar]
- Zimmermann, M.B.; Andersson, M. Assessment of iodine nutrition in populations: Past, present, and future. Nutr. Rev. 2012, 70, 553–570. [Google Scholar] [CrossRef]
- Skeaff, S.A. Iodine deficiency in pregnancy: The effect on neurodevelopment in the child. Nutrients 2011, 3, 265–273. [Google Scholar]
- Andersson, M.; de Benoist, B.; Delange, F.; Zupan, J. Prevention and control of iodine deficiency in pregnant and lactating women and in children less than 2-years-old: Conclusions and recommendations of the Technical Consultation. Public Health Nutr. 2007, 10, 1606–1611. [Google Scholar]
- Li, M.; Eastman, C.J. The changing epidemiology of iodine deficiency. Nat. Rev. Endocrinol. 2012, 8, 434–440. [Google Scholar]
- Dahl, L.; Meltzer, H.M. The Iodine Content of Foods and Diets: Norwegian Perspectives. In Comprehensive Handbook of Iodine; Preedy, V.R., Burrow, G.N., Watson, R.R., Eds.; Academic Press: London, UK, 2009; pp. 345–352. [Google Scholar]
- Frey, H.; Rosenlund, B.; Try, K.; Theodorsen, L. Urinary excretion of iodine in Norway. In Iodine Deficiency in Europe; Delange, F., Ed.; Plenum Press: New York, NY, USA, 1993; pp. 297–300. [Google Scholar]
- Phillips, D.I. Iodine, milk, and the elimination of endemic goitre in Britain: The story of an accidental public health triumph. J. Epidemiol. Community Health 1997, 51, 391–393. [Google Scholar] [CrossRef]
- Zimmermann, M.B.; Andersson, M. Update on iodine status worldwide. Curr. Opin. Endocrinol. Diabetes Obes. 2012, 19, 382–387. [Google Scholar]
- Zimmermann, M.B. The effects of iodine deficiency in pregnancy and infancy. Paediatr. Perinat. Epidemiol. 2012, 26, 108–117. [Google Scholar] [CrossRef]
- Zimmermann, M.B. Iodine deficiency in pregnancy and the effects of maternal iodine supplementation on the offspring: A review. Am. J. Clin. Nutr. 2009, 89, 668S–672S. [Google Scholar]
- NNR Project Group, Iodine. In Nordic Nutrition Recommendations 2004, Integrating Nutrition and Physical Activity, 4th; Becker, W.; Alexander, J.; Andersen, S.; Aro, A.; Fogelholm, M.; Lyhne, N. (Eds.) Nordic Council of Ministers: Copenhagen, Denmark, 2004; pp. 389–396.
- World Health OrganizationUnited Nations Children’s FundInternational Council for Control of Iodine Deficiency DisordersAssessment of Iodine Deficiency Disorders and Monitoring Their Elimination: A Guide for Programme Managers; World Health Organization: Geneva, Switzerland, 2007.
- Zimmermann, M.B.; Jooste, P.L.; Pandav, C.S. Iodine-deficiency disorders. Lancet 2008, 372, 1251–1262. [Google Scholar]
- Glinoer, D. The importance of iodine nutrition during pregnancy. Public Health Nutr. 2007, 10, 1542–1546. [Google Scholar]
- Brantsæter, A.L.; Haugen, M.; Julshamn, K.; Alexander, J.; Meltzer, H.M. Evaluation of urinary iodine excretion as a biomarker for intake of milk and dairy products in pregnant women in the Norwegian Mother and Child Cohort Study (MoBa). Eur. J. Clin. Nutr. 2009, 63, 347–354. [Google Scholar] [CrossRef]
- Brantsæter, A.L.; Haugen, M.; Hagve, T.A.; Aksnes, L.; Rasmussen, S.E.; Julshamn, K.; Alexander, J.; Meltzer, H.M. Self-reported dietary supplement use is confirmed by biological markers in the Norwegian Mother and Child Cohort Study (MoBa). Ann. Nutr. Metab. 2007, 51, 146–154. [Google Scholar]
- Haugen, M.; Brantsæter, A.L.; Alexander, J.; Meltzer, H.M. Dietary supplements contribute substantially to the total nutrient intake in pregnant Norwegian women. Ann. Nutr. Metab. 2008, 52, 272–280. [Google Scholar] [CrossRef]
- Magnus, P.; Irgens, L.M.; Haug, K.; Nystad, W.; Skjaerven, R.; Stoltenberg, C. Cohort profile: The Norwegian Mother and Child Cohort Study (MoBa). Int. J. Epidemiol. 2006, 35, 1146–1150. [Google Scholar]
- Irgens, L.M. The medical birth registry of Norway. Epidemiological research and surveillance throughout 30 years. Acta Obstet. Gynecol. Scand. 2000, 79, 435–439. [Google Scholar] [CrossRef]
- Meltzer, H.M.; Brantsæter, A.L.; Ydersbond, T.A.; Alexander, J.; Haugen, M. Methodological challenges when monitoring the diet of pregnant women in a large study: Experiences from the Norwegian Mother and Child Cohort Study (MoBa). Matern. Child. Nutr. 2008, 4, 14–27. [Google Scholar]
- Norwegian Institute of Public Health website. MoBa Food Frequency Questionnaire. Available online: http://www.fhi.no/dokumenter/253304bd64.pdf (accessed on 20 August 2012).
- FoodCalc. Available online: http://www.ibt.ku.dk/jesper/foodcalc (accessed on 1 February 2005).
- Norwegian Food Safety Authority. Norwegian Directorate of Health, Department of Nutrition-University of Oslo. Matvaretabellen 2006. Available online: http://www.matportalen.no (accessed on 1 October 2008).
- Dahl, L.; Opsahl, J.A.; Meltzer, H.M.; Julshamn, K. Iodine concentration in Norwegian milk and dairy products. Br. J. Nutr. 2003, 90, 679–685. [Google Scholar] [CrossRef]
- Dahl, L.; Johansson, L.; Julshamn, K.; Meltzer, H.M. The iodine content of Norwegian foods and diets. Public Health Nutr. 2004, 7, 569–576. [Google Scholar]
- Brantsæter, A.L.; Haugen, M.; Alexander, J.; Meltzer, H.M. Validity of a new food frequency questionnaire for pregnant women in the Norwegian Mother and Child Cohort Study (MoBa). Matern. Child. Nutr. 2008, 4, 28–43. [Google Scholar]
- Brantsæter, A.L.; Haugen, M.; Thomassen, Y.; Ellingsen, D.G.; Ydersbond, T.A.; Hagve, T.A.; Alexander, J.; Meltzer, H.M. Exploration of biomarkers for total fish intake in pregnant Norwegian women. Public Health Nutr. 2010, 13, 54–62. [Google Scholar]
- Dahl, L.; Meltzer, H.M.; Opsahl, J.A.; Julshamn, K. Iodine intake and status in two groups of Norwegians. Scand. J. Nutr. 2003, 47, 170–178. [Google Scholar] [CrossRef]
- Rasmussen, L.B.; Ovesen, L.; Bulow, I.; Jorgensen, T.; Knudsen, N.; Laurberg, P.; Pertild, H. Dietary iodine intake and urinary iodine excretion in a Danish population: Effect of geography, supplements and food choice. Br. J. Nutr. 2002, 87, 61–69. [Google Scholar] [CrossRef]
- Brussaard, J.H.; Brants, H.A.; Hulshof, K.F.; Kistemaker, C.; Lowik, M.R. Iodine intake and urinary excretion among adults in the Netherlands. Eur. J. Clin. Nutr. 1997, 51, S59–S62. [Google Scholar]
- Kibirige, M.S.; Hutchison, S.; Owen, C.J.; Delves, H.T. Prevalence of maternal dietary iodine insufficiency in the north east of England: Implications for the fetus. Arch. Dis. Child. Fetal. Neonatal. Ed. 2004, 89, F436–F439. [Google Scholar] [CrossRef]
- Limbert, E.; Prazeres, S.; Sao, P.M.; Madureira, D.; Miranda, A.; Ribeiro, M.; Jacome de Castro, J.; Carrilho, F.; Oliveira, M.J.; Reguengo, H.; et al. Iodine intake in Portuguese pregnant women: Results of a countrywide study. Eur. J. Endocrinol. 2010, 163, 631–635. [Google Scholar]
- Andersson, M.; Aeberli, I.; Wust, N.; Piacenza, A.M.; Bucher, T.; Henschen, I.; Haldimann, M.; Zimmermann, M.B. The Swiss iodized salt program provides adequate iodine for school children and pregnant women, but weaning infants not receiving iodine-containing complementary foods as well as their mothers are iodine deficient. J. Clin. Endocrinol. Metab. 2010, 95, 5217–5124. [Google Scholar]
- Lazarus, J.H.; Smyth, P.P. Iodine deficiency in the UK and Ireland. Lancet 2008, 372, 888. [Google Scholar]
- Zimmermann, M.; Delange, F. Iodine supplementation of pregnant women in Europe: A review and recommendations. Eur. J. Clin. Nutr. 2004, 58, 979–984. [Google Scholar]
- Vitti, P.; Rago, T.; Aghini-Lombardi, F.; Pinchera, A. Iodine deficiency disorders in Europe. Public Health Nutr. 2001, 4, 529–535. [Google Scholar]
- Pettigrew-Porter, A.; Skeaff, S.; Gray, A.; Thomson, C.; Croxson, M. Are pregnant women in New Zealand iodine deficient? A cross-sectional survey. Aust. N. Z. J. Obstet. Gynaecol. 2011, 51, 464–467. [Google Scholar] [CrossRef]
- Travers, C.A.; Guttikonda, K.; Norton, C.A.; Lewis, P.R.; Mollart, L.J.; Wiley, V.; Wilcken, B.; Eastman, C.J.; Boyages, S.C. Iodine status in pregnant women and their newborns: Are our babies at risk of iodine deficiency? Med. J. Aust. 2006, 184, 617–620. [Google Scholar]
- Caldwell, K.L.; Makhmudov, A.; Ely, E.; Jones, R.L.; Wang, R.Y. Iodine status of the U.S. population, National Health and Nutrition Examination Survey, 2005–2006 and 2007–2008. Thyroid 2011, 21, 419–427. [Google Scholar] [CrossRef]
- Gunnarsdottir, I.; Dahl, L. Iodine intake in human nutrition: A systematic literature review. Food Nutr. Res. 2012, 56. [Google Scholar] [CrossRef]
- Choudhury, N.; Gorman, K.S. Subclinical prenatal iodine deficiency negatively affects infant development in Northern China. J. Nutr. 2003, 133, 3162–3165. [Google Scholar]
- Oken, E.; Braverman, L.E.; Platek, D.; Mitchell, M.L.; Lee, S.L.; Pearce, E.N. Neonatal thyroxine, maternal thyroid function, and child cognition. J. Clin. Endocrinol. Metab. 2009, 94, 497–503. [Google Scholar] [CrossRef]
- Velasco, I.; Carreira, M.; Santiago, P.; Muela, J.A.; Garcia-Fuentes, E.; Sanchez-Munoz, B.; Garriga, M.J.; Gonzalez-Fernandez, M.C.; Rodriguez, A.; Caballero, F.F.; et al. Effect of iodine prophylaxis during pregnancy on neurocognitive development of children during the first two years of life. J. Clin. Endocrinol. Metab. 2009, 94, 3234–3241. [Google Scholar]
- Vermiglio, F.; Lo Presti, V.P.; Moleti, M.; Sidoti, M.; Tortorella, G.; Scaffidi, G.; Castagna, M.G.; Mattina, F.; Violi, M.A.; Crisa, A.; et al. Attention deficit and hyperactivity disorders in the offspring of mothers exposed to mild-moderate iodine deficiency: A possible novel iodine deficiency disorder in developed countries. J. Clin. Endocrinol. Metab. 2004, 89, 6054–6060. [Google Scholar] [CrossRef]
- Van Mil, N.H.; Tiemeier, H.; Bongers-Schokking, J.J.; Ghabassian, A.; Hofman, A.; Hooijkaas, H.; Jaddoe, V.W.; de Muinck Keizer-Schrama, S.M.; Steegers, E.A.; Visser, T.J.; et al. Low urinary iodine excretion during early pregnancy is associated with alterations in executive functioning in children. J. Nutr. 2012, 142, 2167–2174. [Google Scholar] [CrossRef]
- Nilsen, R.M.; Vollset, S.E.; Gjessing, H.K.; Skjaerven, R.; Melve, K.K.; Schreuder, P.; Alsaker, E.R.; Haug, K.; Daltveit, A.K.; Magnus, P. Self-selection and bias in a large prospective pregnancy cohort in Norway. Paediatr. Perinat. Epidemiol. 2009, 23, 597–608. [Google Scholar]
- Skeaff, S.A. Assessing iodine intakes in pregnancy and strategies for improvement. J. Trace Elem. Med. Biol. 2012, 26, 141–144. [Google Scholar]
- Julshamn, K.; Dahl, L.; Eckhoff, K. Determination of iodine in seafood by inductively coupled plasma/mass spectrometry. J. AOAC Int. 2001, 84, 1976–1983. [Google Scholar]
- Norwegian Scientific Committee for Food Safety Ad Hoc Group, A Comprehensive Assessment of Fish and Other Seafood in the Norwegian Diet; Norwegian Scientific Committee for Food Safety (VKM): Oslo, Norway, 2007.
- Gunnarsdottir, I.; Gustavsdottir, A.G.; Steingrimsdottir, L.; Maage, A.; Johannesson, A.J.; Thorsdottir, I. Iodine status of pregnant women in a population changing from high to lower fish and milk consumption. Public Health Nutr. 2013, 16, 325–329. [Google Scholar]
- Rasmussen, L.B.; Carle, A.; Jorgensen, T.; Knudsen, N.; Laurberg, P.; Pedersen, I.B.; Perrild, H.; Vejbjerg, P.; Ovesen, L. Iodine intake before and after mandatory iodization in Denmark: Results from the Danish Investigation of Iodine Intake and Thyroid Diseases (DanThyr) study. Br. J. Nutr. 2008, 100, 166–173. [Google Scholar]
- Lamberg, B.A. Endemic goitre in Finland and changes during 30 years of iodine prophylaxis. Endocrinol. Exp. 1986, 20, 35–47. [Google Scholar]
- Hess, S.Y.; Zimmermann, M.B.; Torresani, T.; Burgi, H.; Hurrell, R.F. Monitoring the adequacy of salt iodization in Switzerland: A national study of school children and pregnant women. Eur. J. Clin. Nutr. 2001, 55, 162–166. [Google Scholar]
© 2013 by the authors; licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution license (http://creativecommons.org/licenses/by/3.0/).
Share and Cite
Brantsæter, A.L.; Abel, M.H.; Haugen, M.; Meltzer, H.M. Risk of Suboptimal Iodine Intake in Pregnant Norwegian Women. Nutrients 2013, 5, 424-440. https://doi.org/10.3390/nu5020424
Brantsæter AL, Abel MH, Haugen M, Meltzer HM. Risk of Suboptimal Iodine Intake in Pregnant Norwegian Women. Nutrients. 2013; 5(2):424-440. https://doi.org/10.3390/nu5020424
Chicago/Turabian StyleBrantsæter, Anne Lise, Marianne Hope Abel, Margaretha Haugen, and Helle Margrete Meltzer. 2013. "Risk of Suboptimal Iodine Intake in Pregnant Norwegian Women" Nutrients 5, no. 2: 424-440. https://doi.org/10.3390/nu5020424
APA StyleBrantsæter, A. L., Abel, M. H., Haugen, M., & Meltzer, H. M. (2013). Risk of Suboptimal Iodine Intake in Pregnant Norwegian Women. Nutrients, 5(2), 424-440. https://doi.org/10.3390/nu5020424






