Public Health Adaptation to Climate Change in OECD Countries
Abstract
:1. Introduction
Role of National Governments in Public Health Adaptation
2. Materials and Methods
2.1. Sample
2.2. Data Collection
2.3. Indicators
2.4. Tracking Reporting of Adaptation
3. Results
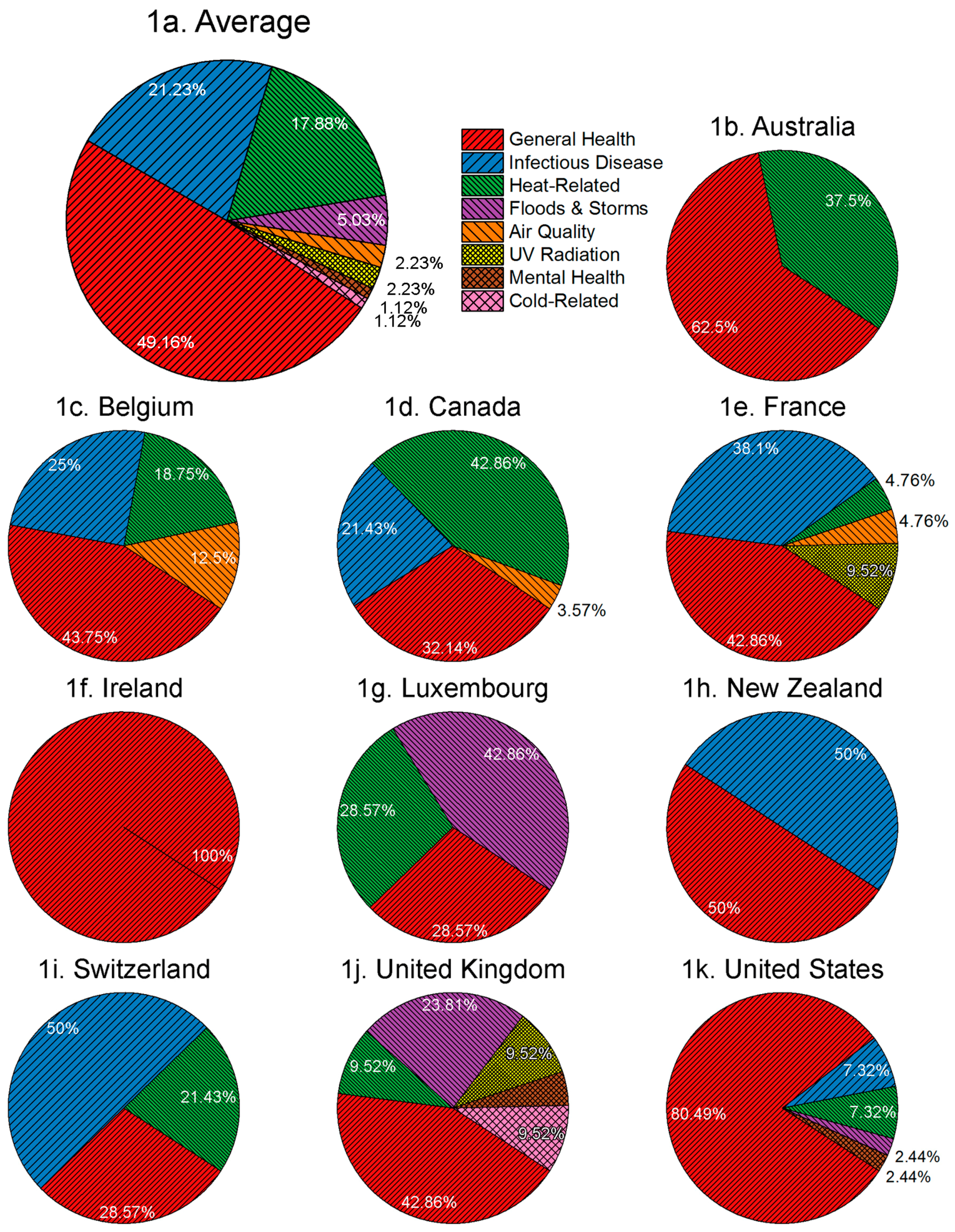
3.1. National Adaptation Planning Typically Does Not Target Specific Health Risks
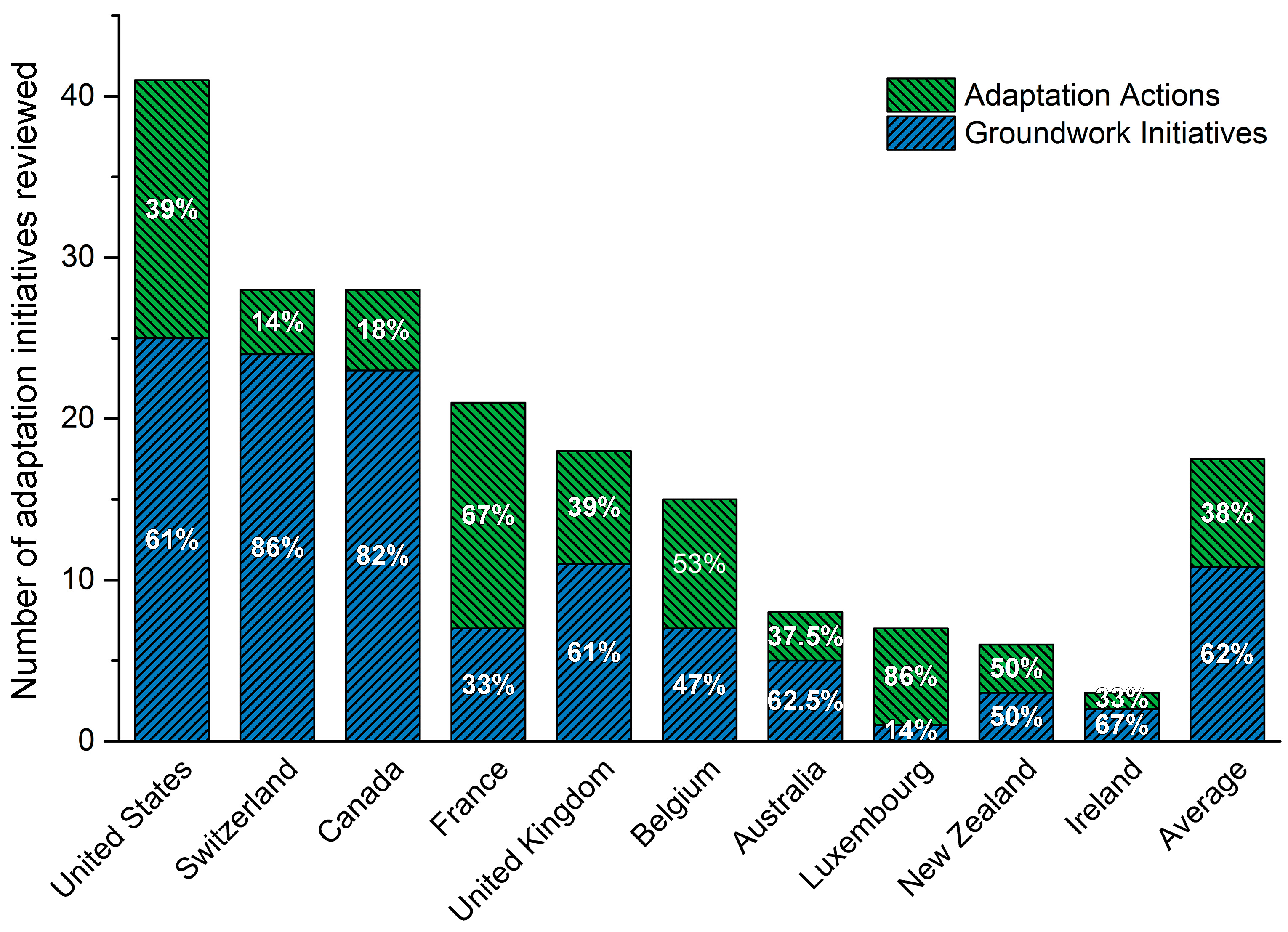
3.2. National Governments Report Planning or Implementing Primarily Groundwork Adaptation Initiatives
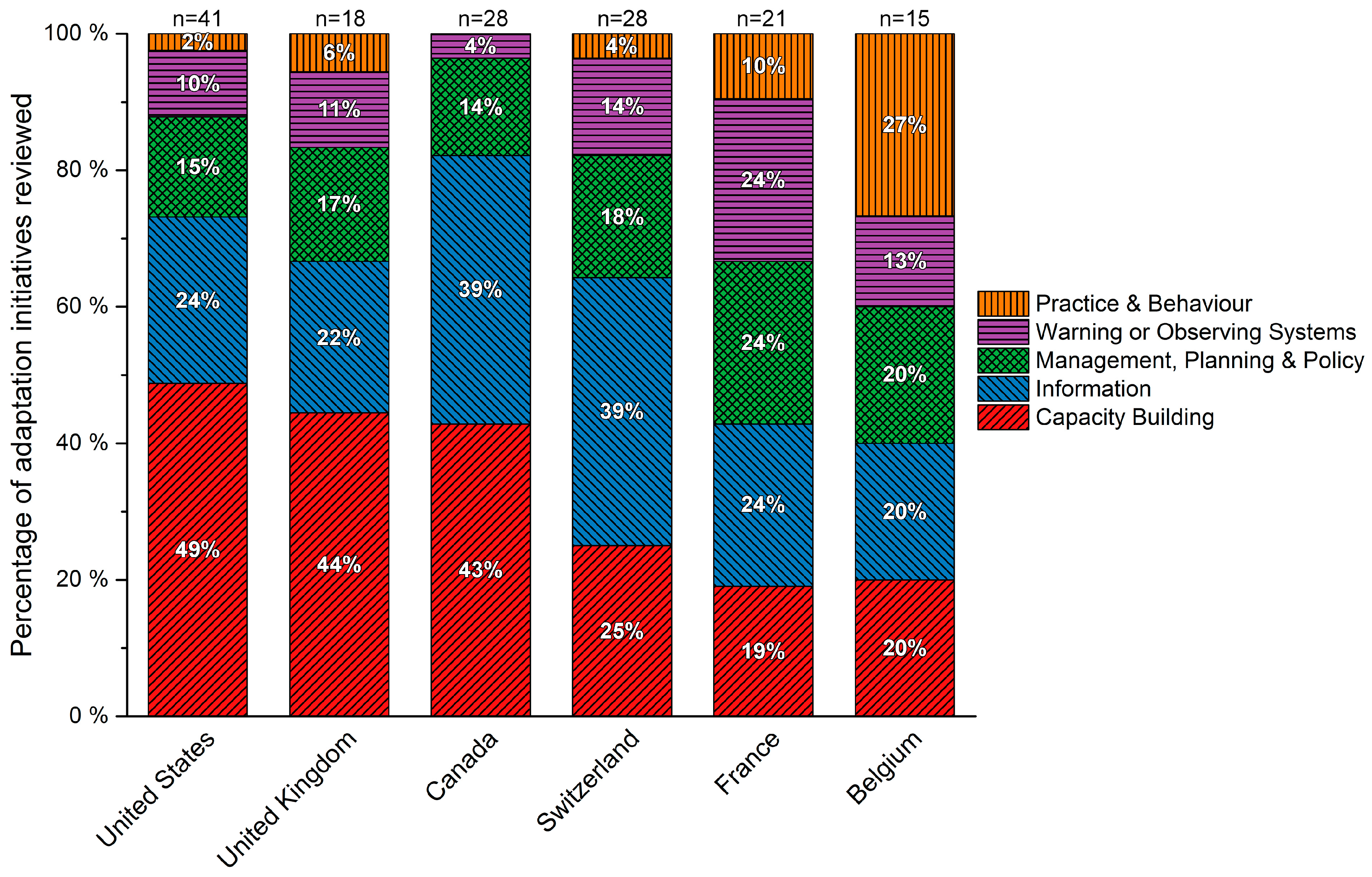
3.3. The Role of Inter-Sectoral Adaptation Planning Varies across Countries
3.4. National Adaptation Frameworks Provide Important Reference Points for Strategic Action
4. Discussion
4.1. Governing Structure and National Governments’ Roles in Public Health Adaptation
4.2. Options for Cross-Sectoral Collaboration, Vertical Coordination and National Health Adaptation Planning
4.3. Limitations
5. Conclusions
Supplementary Materials
Acknowledgments
Author Contributions
Conflicts of Interest
References
- IPCC. Climate Change 2014: Impacts, Adaptation, and Vulnerability. Part B: Regional Aspects. Contribution of Working Group II to the Fifth Assessment Report of the Intergovernmental Panel on Climate Change; Barros, V.R., Field, C.B., Dokken, D.J., Mastrandrea, M.D., Mach, K.J., Bilir, T.E., Chatterjee, M., Ebi, K.L., Estrada, Y.O., Genova, R.C., et al., Eds.; Cambridge University Press: Cambridge, UK; New York, NY, USA, 2014; p. 688. [Google Scholar]
- Adler, N.E.; Boyce, T.; Chesney, M.A.; Cohen, S.; Folkman, S.; Kahn, R.L.; Syme, S.L. Socioeconomic status and health: The challenge of the gradient. Am. Psychol. 1994, 49, 15–24. [Google Scholar] [CrossRef] [PubMed]
- Marmot, M. Social determinants of health inequalities. Lancet 2005, 365, 1099–1104. [Google Scholar] [CrossRef]
- Bowen, K.J.; Friel, S.; Ebi, K.; Butler, C.D.; Miller, F.; McMichael, A.J. Governing for a healthy population: Towards an understanding of how decision-making will determine our global health in a changing climate. Int. J. Environ. Res. Public Health 2011, 9, 55–72. [Google Scholar] [CrossRef] [PubMed]
- Page, L.A.; Howard, L. The impact of climate change on mental health (but will mental health be discussed at copenhagen?). Psychol. Med. 2010, 40, 177–180. [Google Scholar] [CrossRef] [PubMed]
- British Medical Association. Climate Change. Available online: http://bma.org.uk/working-for-change/international-affairs/climate-change (accessed on 7 August 2015).
- Canadian Medical Association. Climate Change and Human Health; Canadian Medical Association: Ottawa, ON, Canada, 2010. [Google Scholar]
- American Medical Association. H-135.938 Global Climate Change and Human Health; American Medical Association: Chicago, IL, USA, 2008. [Google Scholar]
- American Public Health Association. A Declaration on Climate Change and Health; American Public Health Association: Washington, DC, USA, 2014. [Google Scholar]
- Costello, A.; Abbas, M.; Allen, A.; Ball, S.; Bell, S.; Bellamy, R.; Friel, S.; Groce, N.; Johnson, A.; Kett, M.; et al. Managing the health effects of climate change: Lancet and university college london institute for global health commission. Lancet 2009, 373, 1693–1733. [Google Scholar] [CrossRef]
- Chan, M. Achieving a cleaner, more sustainable, and healthier future. Lancet 2015, 386, e27–e28. [Google Scholar] [CrossRef]
- Watts, N.; Adger, W.N.; Agnolucci, P.; Blackstock, J.; Byass, P.; Cai, W.; Chaytor, S.; Colbourn, T.; Collins, M.; Cooper, A.; et al. Health and climate change: Policy responses to protect public health. Lancet 2015, 386, 1861–1914. [Google Scholar] [CrossRef]
- IPCC. Annex II: Glossary [Agard, J., Schipper, E.L.F., Birkmann, J., Campos, M., Dubeux, C., Nojiri, Y., Olsson, L., Osman-Elasha, B., Pelling, M., Prather, M.J., et al., eds.]. In Climate Change 2014: Impacts, Adaptation, and Vulnerability. Part B: Regional Aspects. Contribution of Working Group II to the Fifth Assessment Report of the Intergovernmental Panel on Climate Change; Barros, V.R., Field, C.B., Dokken, D.J., Mastrandrea, M.D., Mach, K.J., Bilir, T.E., Chatterjee, M., Ebi, K.L., Estrada, Y.O., Genova, R.C., et al., Eds.; Cambridge University Press: Cambridge, UK; New York, NY, USA, 2014; pp. 1757–1776. [Google Scholar]
- Ford, J.D.; Willox, A.C.; Chatwood, S.; Furgal, C.; Harper, S.; Mauro, I.; Pearce, T. Adapting to the effects of climate change on inuit health. Am. J. Public Health 2014, 104, e9–e17. [Google Scholar] [CrossRef] [PubMed]
- Ebi, K.L.; Semenza, J.C. Community-based adaptation to the health impacts of climate change. Am. J. Prev. Med. 2008, 35, 501–507. [Google Scholar] [CrossRef] [PubMed]
- Frumkin, H.; Hess, J.; Luber, G.; Malilay, J.; McGeehin, M. Climate change: The public health response. Am. J. Public Health 2008, 98, 435–445. [Google Scholar] [CrossRef] [PubMed]
- Magnan, A.K.; Ribera, T. Global adaptation after Paris. Science 2016, 352, 1280–1282. [Google Scholar] [CrossRef] [PubMed]
- Ford, J.D.; Berrang-Ford, L. The 4cs of adaptation tracking: Consistency, comparability, comprehensiveness, coherency. Mitig. Adapt. Strateg. Glob. Chang. 2015. [Google Scholar] [CrossRef]
- Ford, J.D.; Berrang-Ford, L.; Lesnikowski, A.; Barrera, M.; Heymann, S.J. How to track adaptation to climate change: A typology of approaches for national-level application. Ecol. Soc. 2013, 18, 40. [Google Scholar] [CrossRef]
- Magnan, A.K. Climate change: Metrics needed to track adaptation. Nature 2016, 530, 160. [Google Scholar] [CrossRef] [PubMed]
- Massey, E.; Biesbroek, R.; Huitema, D.; Jordan, A. Climate policy innovation: The adoption and diffusion of adaptation policies across europe. Glob. Environ. Chang. 2014, 29, 434–443. [Google Scholar] [CrossRef]
- Biesbroek, G.R.; Swart, R.J.; Carter, T.R.; Cowan, C.; Henrichs, T.; Mela, H.; Morecroft, M.D.; Rey, D. Europe adapts to climate change: Comparing national adaptation strategies. Glob. Environ. Chang. 2010, 20, 440–450. [Google Scholar] [CrossRef]
- Bauer, A.; Feichtinger, J.; Steurer, R. The governance of climate change adaptation in 10 OECD countries: Challenges and approaches. J. Environ. Policy Plan. 2012, 14, 279–304. [Google Scholar] [CrossRef]
- Lesnikowski, A.; Ford, J.; Berrang-Ford, L.; Paterson, J.; Barrera, M.; Heymann, S. Adapting to health impacts of climate change: A study of UNFCCC Annex I parties. Environ. Res. Lett. 2011, 6, 4. [Google Scholar] [CrossRef]
- Bowen, K.J.; Ebi, K.L. Governing the health risks of climate change: Towards multi-sector responses. Curr. Opin. Environ. Sustain. 2015, 12, 80–85. [Google Scholar] [CrossRef]
- Amundsen, H.; Berglund, F.; Westskogô, H. Overcoming barriers to climate change adaptation—A question of multilevel governance? Environ. Plan. C Gov. Policy 2010, 28, 276–289. [Google Scholar] [CrossRef]
- Glaas, E.; Jonsson, A.; Hjerpe, M.; Andersson-Sköld, Y. Managing climate change vulnerabilities: Formal institutions and knowledge use as determinants of adaptive capacity at the local level in Sweden. Local Environ. 2010, 15, 525–539. [Google Scholar] [CrossRef]
- Austin, S.E.; Ford, J.D.; Berrang-Ford, L.; Araos, M.; Parker, S.; Fleury, M.D. Public health adaptation to climate change in Canadian jurisdictions. Int. J. Environ. Res. Public Health 2015, 12, 623–651. [Google Scholar] [CrossRef] [PubMed]
- Department of the Environment Community and Local Government. National Climate Change Adaptation Framework; Department of the Environment Community and Local Government: Dublin, Ireland, 2012.
- Panic, M.; Ford, J.D. A review of national-level adaptation planning with regards to the risks posed by climate change on infectious diseases in 14 OECD nations. Int. J. Environ. Res. Public Health 2013, 10, 7083–7109. [Google Scholar] [CrossRef] [PubMed]
- Burton, I. Adaptation to climate change: Context, status, and prospects. In Climate Change Adaptation in Developed Nations; Ford, J.D., Berrang-Ford, L., Eds.; Springer: Dordrecht, The Netherlands, 2011; pp. 477–483. [Google Scholar]
- Pielke, R.; Prins, G.; Rayner, S.; Sarewitz, D. Climate change 2007: Lifting the taboo on adaptation. Nature 2007, 445, 597–598. [Google Scholar] [CrossRef] [PubMed]
- Nalau, J.; Preston, B.L.; Maloney, M.C. Is adaptation a local responsibility? Environ. Sci. Policy 2015, 48, 89–98. [Google Scholar] [CrossRef]
- Measham, T.; Preston, B.; Smith, T.; Brooke, C.; Gorddard, R.; Withycombe, G.; Morrison, C. Adapting to climate change through local municipal planning: Barriers and challenges. Mitig. Adapt. Strateg. Glob. Chang. 2011, 16, 889–909. [Google Scholar] [CrossRef]
- O’Neill, M.S.; Jackman, D.K.; Wyman, M.; Manarolla, X.; Gronlund, C.J.; Brown, D.G.; Brines, S.J.; Schwartz, J.; Diez-Roux, A.V. US local action on heat and health: Are we prepared for climate change? Int. J. Public Health 2010, 55, 105–112. [Google Scholar] [CrossRef] [PubMed]
- Hanssen, G.S.; Mydske, P.K.; Dahle, E. Multi-level coordination of climate change adaptation: By national hierarchical steering or by regional network governance? Local Environ. 2013, 18, 869–887. [Google Scholar] [CrossRef]
- Paterson, J.A.; Ford, J.D.; Ford, L.B.; Lesnikowski, A.; Berry, P.; Henderson, J.; Heymann, J. Adaptation to climate change in the ontario public health sector. BMC Public Health 2012, 12, 452. [Google Scholar] [CrossRef] [PubMed]
- Urwin, K.; Jordan, A. Does public policy support or undermine climate change adaptation? Exploring policy interplay across different scales of governance. Glob. Environ. Chang. 2008, 18, 180–191. [Google Scholar] [CrossRef]
- Bauer, A.; Steurer, R. Multi-level governance of climate change adaptation through regional partnerships in Canada and England. Geoforum 2014, 51, 121–129. [Google Scholar] [CrossRef]
- Mimura, N.; Pulwarty, R.S.; Duc, D.M.; Elshinnawy, I.; Redsteer, M.H.; Huang, H.Q.; Nkem, J.N.; Rodriguez, R.A.S. Adaptation planning and implementation. In Climate Change 2014: Impacts, Adaptation, and Vulnerability. Part A: Global and Sectoral Aspects. Contribution of Working Group II to the Fifth Assessment Report of the Intergovernmental Panel of Climate Change; Field, C.B., Barros, V.R., Dokken, D.J., Mach, K.J., Mastrandrea, M.D., Bilir, T.E., Chatterjee, M., Ebi, K.L., Estrada, Y.O., Genova, R.C., et al., Eds.; Cambridge University Press: Cambridge, UK; New York, NY, USA, 2014; pp. 869–898. [Google Scholar]
- Fidelman, P.I.J.; Leitch, A.M.; Nelson, D.R. Unpacking multilevel adaptation to climate change in the great barrier reef, Australia. Glob. Environ. Chang. Hum. Policy Dimens. 2013, 23, 800–812. [Google Scholar] [CrossRef]
- Keskitalo, E.C.H. Introduction—Adaptation to climate change in europe: Theoretical framework and study design. In Developing Adaptation Policy and Practice in Europe: Multi-Level Governance of Climate Change; Keskitalo, E.C.H., Ed.; Springer: Umeå, Sweden, 2010. [Google Scholar]
- Huang, C.; Vaneckova, P.; Wang, X.; FitzGerald, G.; Guo, Y.; Tong, S. Constraints and barriers to public health adaptation to climate change: A review of the literature. Am. J. Prev. Med. 2011, 40, 183–190. [Google Scholar] [CrossRef] [PubMed]
- Burton, I. Adapt and thrive: Options for reducing the climate change adaptation deficit. Policy Opt. 2005, 27, 33–38. [Google Scholar]
- Dickinson, T.; Burton, I. Adaptation to climate change in Canada: A multi-level mosaic. In Climate Change Adaptation in Developed Nations; Ford, J.D., Berrang-Ford, L., Eds.; Springer: Dordrecht, The Netherlands, 2011; pp. 103–117. [Google Scholar]
- Lijphart, A. Patterns of Democracy: Government Forms and Performance in Thirty-Six Countries; Yale University Press: New Haven, CT, USA, 2012. [Google Scholar]
- Glicksman, R.L. Climate change adaptation: A collective action perspective on federalism considerations. Environ. Law 2010, 40, 1159. [Google Scholar]
- Hess, J.J.; McDowell, J.Z.; Luber, G. Integrating climate change adaptation into public health practice: Using adaptive management to increase adaptive capacity and build resilience. Environ. Health Perspect. 2012, 120, 171–179. [Google Scholar] [CrossRef] [PubMed]
- Ebi, K.L.; Balbus, J.; Kinney, P.L.; Lipp, E.; Mills, D.; O’Neill, M.S.; Wilson, M.L. US funding is insufficient to address the human health impacts of and public health responses to climate variability and change. Environ. Health Perspect. 2009, 117, 857–862. [Google Scholar] [CrossRef] [PubMed]
- Gosselin, P.; Bélanger, D.; Lapaige, V.; Labbé, Y. The burgeoning field of transdisciplinary adaptation research in Quebec (1998–): A climate change-related public health narrative. J. Multidiscip. Healthc. 2011, 4, 337–348. [Google Scholar] [CrossRef] [PubMed]
- Bowen, K.J.; Ebi, K.; Friel, S.; McMichael, A.J. A multi-layered governance framework for incorporating social science insights into adapting to the health impacts of climate change. Glob. Health Action 2013, 6. [Google Scholar] [CrossRef] [PubMed]
- Corfee-Morlot, J.; Cochran, I.; Hallegatte, S.; Teasdale, P.-J. Multilevel risk governance and urban adaptation policy. Clim. Chang. 2011, 104, 169–197. [Google Scholar] [CrossRef]
- Preston, B.L.; Westaway, R.M.; Yuen, E.J. Climate adaptation planning in practice: An evaluation of adaptation plans from three developed nations. Mitig. Adapt. Strateg. Glob. Chang. 2011, 16, 407–438. [Google Scholar] [CrossRef]
- Jordan, A.; Huitema, D. Policy innovation in a changing climate: Sources, patterns and effects. Glob. Environ. Chang. 2014, 29, 387–394. [Google Scholar] [CrossRef]
- Smith, J.B.; Vogel, J.M.; Cromwell, J.E., III. An architecture for government action on adaptation to climate change. An editorial comment. Clim. Chang. 2009, 95, 53–61. [Google Scholar] [CrossRef]
- Magnan, A.K.; Schipper, E.L.F.; Burkett, M.; Bharwani, S.; Burton, I.; Eriksen, S.; Gemenne, F.; Schaar, J.; Ziervogel, G. Addressing the risk of maladaptation to climate change. Wiley Interdiscip. Rev. Clim. Chang. 2016, 7, 646–665. [Google Scholar] [CrossRef]
- Araos, M.; Austin, S.E.; Berrang-Ford, L.; Ford, J.D. Public health adaptation to climate change in large cities: A global baseline. Int. J. Health Serv. 2016, 46, 53–78. [Google Scholar] [CrossRef] [PubMed]
- Lesnikowski, A.; Ford, J.D.; Berrang-Ford, L.; Barrera, M.; Berry, P.; Henderson, J.; Heymann, S. National-level factors affecting planned, public adaptation to health impacts of climate change. Glob. Environ. Chang. 2013, 23, 1153–1163. [Google Scholar] [CrossRef]
- Berrang-Ford, L.; Pearce, T.; Ford, J. Systematic review approaches for climate change adaptation research. Reg. Environ. Chang. 2015, 15, 755–769. [Google Scholar] [CrossRef]
- Ford, J.D.; Berrang-Ford, L.; Biesbroek, R.; Araos, M.; Austin, S.; Lesnikowski, A. Adaptation tracking for a post-2015 climate agreement. Nat. Clim. Chang. 2015, 5, 967–969. [Google Scholar] [CrossRef]
- Boyd, E.; Street, R.; Gawith, M.; Lonsdale, K.; Newton, L.; Johnstone, K.; Metcalf, G. Leading the UK adaptation agenda: A landscape of stakeholders and networked organizations for adaptation to climate change. In Climate Change Adaptation in Developed Nations; Ford, J.D., Berrang-Ford, L., Eds.; Springer Netherlands: Dordrecht, The Netherlands, 2011; Volume 42, pp. 85–102. [Google Scholar]
- Araos, M.; Berrang-Ford, L.; Ford, J.D.; Austin, S.E.; Biesbroek, R. Climate change adaptation in large cities: A systematic global assessment. Environ. Sci. Policy 2016. [Google Scholar] [CrossRef]
- Lesnikowski, A.; Ford, J.; Biesbroek, R.; Berrang-Ford, L.; Heymann, S.J. National-level progress on adaptation. Nat. Clim. Chang. 2016, 6, 261–264. [Google Scholar] [CrossRef]
- Lesnikowski, A.; Ford, J.D.; Berrang-Ford, L.; Barrera, M.; Heymann, J. How are we adapting to climate change? A global assessment. Mitig. Adapt. Strateg. Glob. Chang. 2013. [Google Scholar] [CrossRef]
- Hay, I. Qualitative Research Methods in Human Geography; Oxford University Press: South Melbourne, Australia, 2005. [Google Scholar]
- Walliman, N. Research Methods: The Basics; Routledge: New York, NY, USA, 2010. [Google Scholar]
- Fallon, D.S.M.; Sullivan, C.A. Are we there yet? NSW local governments’ progress on climate change. Aust. Geogr. 2014, 45, 221–238. [Google Scholar] [CrossRef]
- Lundqvist, L.J. Planning for climate change adaptation in a multi-level context: The Gothenburg metropolitan area. Eur. Plan. Stud. 2016, 24, 1–20. [Google Scholar] [CrossRef]
- IPCC. Climate Change 2014: Impacts, Adaptation, and Vulnerability. Part A: Global and Sectoral Aspects. Contribution of Working Group II to the Fifth Assessment Report of the Intergovernmental Panel on Climate Change; Field, C.B., Barros, V.R., Dokken, D.J., Mastrandrea, M.D., Mach, K.J., Bilir, T.E., Chatterjee, M., Ebi, K.L., Estrada, Y.O., Genova, R.C., et al., Eds.; Cambridge University Press: Cambridge, UK; New York, NY, USA, 2014; p. 1132. [Google Scholar]
- Biagini, B.; Bierbaum, R.; Stults, M.; Dobardzic, S.; McNeeley, S.M. A typology of adaptation actions: A global look at climate adaptation actions financed through the global environment facility. Glob. Environ. Chang. 2014, 25, 97–108. [Google Scholar] [CrossRef]
- Smith, K.R.; Woodward, A.; Campbell-Lendrum, D.; Chadee, D.D.; Honda, Y.; Liu, Q.; Olwoch, J.M.; Revich, B.; Sauerborn, R. Human health: Impacts, adaptation, and co-benefits. In Climate Change 2014: Impacts, Adaptation, and Vulnerability. Part A: Global and Sectoral Aspects. Contribution of Working Group II to the Fifth Assessment Report of the Intergovernmental Panel of Climate Change; Field, C.B., Barros, V.R., Dokken, D.J., Mach, K.J., Mastrandrea, M.D., Bilir, T.E., Chatterjee, M., Ebi, K.L., Estrada, Y.O., Genova, R.C., et al., Eds.; Cambridge University Press: Cambridge, UK; New York, NY, USA, 2014; pp. 709–754. [Google Scholar]
- Stott, C.; Huq, S. Knowledge flows in climate change adaptation: Exploring friction between scales. Clim. Dev. 2014, 6, 382–387. [Google Scholar] [CrossRef]
- Williams, C.; Fenton, A.; Huq, S. Knowledge and adaptive capacity. Nat. Clim. Chang. 2015, 5, 82–83. [Google Scholar] [CrossRef]
- Earle, A.; Mokomane, Z.; Heymann, J. International perspectives on work-family policies: Lessons from the world’s most competitive economies. Future Child. 2011, 21, 191–210. [Google Scholar] [CrossRef] [PubMed]
- Heymann, J.; Raub, A.; Earle, A. Creating and using new data sources to analyze the relationship between social policy and global health: The case of maternal leave. Public Health Rep. 2011, 126, 127–134. [Google Scholar] [PubMed]
- Health Protection Agency. Health Effects of Climate Change in the UK 2012: Current Evidence, Recommendations and Research Gaps; Health Protection Agency: Chilton, UK, 2012.
- World Bank. Population, Total; World Bank: Washington, DC, USA, 2016. [Google Scholar]
- World Bank. World Development Indicators; World Bank: Washington, DC, USA, 2014. [Google Scholar]
- Adger, W.N.; Arnell, N.W.; Tompkins, E.L. Successful adaptation to climate change across scales. Glob. Environ. Chang. 2005, 15, 77–86. [Google Scholar] [CrossRef]
- Greer, A.; Ng, V.; Fisman, D. Climate change and infectious diseases in North America: The road ahead. Can. Med. Assoc. J. 2008, 178, 715–722. [Google Scholar]
- Bennett, H.; Jones, R.; Keating, G.; Woodward, A.; Hales, S.; Metcalfe, S. Health and equity impacts of climate change in Aotearoa-New Zealand, and health gains from climate action. N. Z. Med. J. (Online) 2014, 127, 16–31. [Google Scholar]
- Bourque, F.; Willox, A.C. Climate change: The next challenge for public mental health? Int. Rev. Psychiatry 2014, 26, 415–422. [Google Scholar] [CrossRef] [PubMed]
- Swiss Confederation. Adaptation Aux Changements Climatiques en Suisse: Plan D’action 2014–2019—Deuxième volet de la Stratégie du Conseil Fédéral; Swiss Confederation: Bern, Switzerland, 2014. [Google Scholar]
- Government of Canada. Federal Adaptation Policy Framework; Environment Canada, Ed.; Government of Canada: Gatineau, QC, Canada, 2011.
- Department of Health. Department of Health Statement of Strategy 2015–2017; Department of Health: Dublin, Ireland, 2014.
- Australian Government. Adapting to Climate Change in Australia—An Australian Government Position Paper; Department of Climate Change, Ed.; Australian Government: Canberra, Australia, 2010.
- European Environment Agency. National Adaptation Policy Processes in European Countries—2014; European Environment Agency: Copenhagen, Denmark, 2014. [Google Scholar]
- Ford, J.D.; King, D. Coverage and framing of climate change adaptation in the media: A review of influential North American newspapers during 1993–2013. Environ. Sci. Policy 2015, 48, 137–146. [Google Scholar] [CrossRef]
- Deleon, P.; deLeon, L. What ever happened to policy implementation? An alternative approach. J. Public Adm. Res. Theory J-PART 2002, 12, 467–492. [Google Scholar] [CrossRef]
- Sénat de Belgique. Projet de loi portant assentiment à l’accord de coopération entre l’état fédéral, la région flamande, la région wallonne et la région de bruxelles-capitale relatif à l’établissement, l’exécution et le suivi d’un plan national climat, ainsi que l’établissement de rapports, dans le cadre de la convention-cadre des nations unies sur les changements climatiques et du protocole de kyoto, conclu à bruxelles le 14 novembre 2002. In Doc 50 2376/001; Chambre des Représentants de Belgique: Bruxelles, Belgium, 2003. [Google Scholar]
- Commission Nationale Climat. Belgian National Climate Change Aadptation Strategy; Flemish Environment Nature and Energy Department: Brussels, Belgium, 2010. [Google Scholar]
- L’Assemblée Fédérale de la Confédération Suisse. Loi Fédérale sur la Réduction des Émissions de CO2 (loi sur le CO2); L’Assemblée fédérale de la Confédération suisse: Bern, Switzerland, 2013. [Google Scholar]
- Office Fédérale de l’Environnement. Adaptation aux Changements Climatiques dans les Villes Suisses [Adaptation to Climatic Changes in Swiss Cities]; Section Climat: Bern, Switzerland, 2012. [Google Scholar]
- Service Public Fédéral Belge. Projet de Plan Fédéral ‘Adaptation aux Changements Climatiques’; Santé Publique, Sécurité de la Chaine Alimentaire et Environnement: Brussels, Belgium, 2013. [Google Scholar]
- Hess, J.J.; Schramm, P.J.; Luber, G. Public health and climate change adaptation at the federal level: One agency’s response to Executive Order 13514. Am. J. Public Health 2014, 104, e22–e30. [Google Scholar] [CrossRef] [PubMed]
- Department of Health and Human Services. Hhs Climate Adaptation Plan; Department of Health and Human Services: Washington, DC, USA, 2014.
- Hess, J.J.; Marinucci, G.; Schramm, P.J.; Manangan, A.; Luber, G. Management of climate change adaptation at the united states centers for disease control and prevention. In Global Climate Change and Public Health; Springer: New York, NY, USA, 2014; pp. 341–360. [Google Scholar]
- Séguin, J. Human Health in a Changing Climate: A Canadian Assessment of Vulnerabilities and Adaptive Capacity; Health Canada: Ottawa, ON, Canada, 2008. [Google Scholar]
- Warren, F.J.; Lemmen, D.S. Canada in a Changing Climate: Sector Perspectives on Impacts and Adaptation; Government of Canada: Ottawa, ON, Canada, 2014; p. 286.
- Health Canada. Heat Alert and Response Systems to Protect Health: Best Practices Guidebook; Healthy Environments and Consumer Safety Branch: Ottawa, ON, Canada, 2012. [Google Scholar]
- Health Canada. Extreme Heat Events Guidelines: Technical Guide for Health Care Workers; Health Canada: Ottawa, ON, Canada, 2011. [Google Scholar]
- Health Canada. Extreme Heat Events Guidelines: User Guide for Health Care Workers and Health Administrators; Health Canada: Ottawa, ON, Canada, 2011. [Google Scholar]
- HM Government. The National Adaptation Programme: Making the Country Resilient to a Changing Climate; Department for Environment Food & Rural Affairs: London, UK, 2013.
- MEDDTL. Plan National D’adaptation de la France aux Effets du Changement Climatique; Ministère de l’Écologie du Développement durable des Transports et du Logement: Paris, France, 2011.
- Institut de Veille Sanitaire. Impacts Sanitaires du Changement Climatique en France: Quels Enjeux Pour L’InVS? Institut de Veille Sanitaire: Saint-Maurice, France, 2010. [Google Scholar]
- Ebi, K.L.; Smith, J.; Burton, I.; Scheraga, J. Some lessons learned from public health on the process of adaptation. Mitig. Adapt. Strateg. Glob. Chang. 2006, 11, 607–620. [Google Scholar] [CrossRef]
- Peters, B.G. Managing horizontal government: The politics of coordination. Public Adm. 1998, 76, 295–311. [Google Scholar] [CrossRef]
- Candel, J.J.; Biesbroek, R. Toward a processual understanding of policy integration. Policy Sci. 2016, 49, 211–231. [Google Scholar] [CrossRef]
- Keskitalo, E.C.H.; Juhola, S.; Westerhoff, L. Climate change as governmentality: Technologies of government for adaptation in three European countries. J. Environ. Plan. Manag. 2012, 55, 435–452. [Google Scholar] [CrossRef]
- Centers for Disease Control and Prevention. CDC’s Climate-Ready States and Cities Initiative. Available online: http://www.cdc.gov/climateandhealth/climate_ready.htm (accessed on 10 June 2014).
- Commission Nationale Climat. Belgium’s Sixth National Communication: Under the United Nations Framework Convention on Climate Change; Federal Public Service Health, Food Chain Safety and Environment: Brussels, Belgium, 2013. [Google Scholar]
- Dupuis, J.; Biesbroek, R. Comparing apples and oranges: The dependent variable problem in comparing and evaluating climate change adaptation policies. Glob. Environ. Chang. 2013, 23, 1476–1487. [Google Scholar] [CrossRef]
- Keskitalo, E.C.H. Developing Adaptation Policy and Practice in Europe: Multi-Level Governance of Climate Change; Springer: Dordrecht, The Netherlands, 2010. [Google Scholar]
| Adaptation Category | Description | Examples of Initiatives in Category |
|---|---|---|
| Capacity Building | Developing human resources, institutions, and communities, equipping them with the capability to adapt to climate change. |
|
| Management, Planning and Policy | Incorporating understanding of climate science, impacts, and vulnerability and risk into government and institutional planning, management, policies and regulations. |
|
| Practice and Behaviour | Revisions or expansion of practices and on the ground behaviour that are directly related to building resilience. |
|
| Information | Systems for communicating climate information to help build resilience towards climate impacts (other than communication for early warning systems). |
|
| Warning or Observing Systems | Implementation of new or enhanced tools and technologies for communicating weather and climate risks, and for monitoring changes in the climate system. |
|
| Country Name | Population Size (2015) [77] | GDP (Billion USD) (2014) [78] | GDP/Capita (PPP Adjusted) (2015) [78] | Governing Structure [46] | Number of Health Adaptation Initiatives Reviewed |
|---|---|---|---|---|---|
| Australia | 23,490,736 | 1454.7 | 45,514.2 | Federal and decentralized | 8 |
| Belgium | 11,225,207 | 531.2 | 43,991.6 | Federal and decentralized | 15 |
| Canada | 35,540,419 | 1783.8 | 44,310.1 | Federal and decentralized | 28 |
| France | 66,206,930 | 2829.2 | 39,678.0 | Unitary and centralized | 21 |
| Ireland | 4,612,719 | 250.8 | 54,654.4 | Unitary and centralized | 3 |
| Luxembourg | 556,074 | 64.9 | 101,926.4 | Unitary and centralized | 7 |
| New Zealand | 4,509,700 | 200.1 | 36,982.3 | Unitary and centralized | 6 |
| Switzerland | 8,190,229 | 701.0 | 60,535.2 | Federal and decentralized | 28 |
| United Kingdom | 64,510,376 | 2990.2 | 41,324.6 | Unitary and centralized | 18 |
| United States | 318,857,056 | 17,348.1 | 55,836.8 | Federal and decentralized | 41 |
© 2016 by the authors; licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC-BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Austin, S.E.; Biesbroek, R.; Berrang-Ford, L.; Ford, J.D.; Parker, S.; Fleury, M.D. Public Health Adaptation to Climate Change in OECD Countries. Int. J. Environ. Res. Public Health 2016, 13, 889. https://doi.org/10.3390/ijerph13090889
Austin SE, Biesbroek R, Berrang-Ford L, Ford JD, Parker S, Fleury MD. Public Health Adaptation to Climate Change in OECD Countries. International Journal of Environmental Research and Public Health. 2016; 13(9):889. https://doi.org/10.3390/ijerph13090889
Chicago/Turabian StyleAustin, Stephanie E., Robbert Biesbroek, Lea Berrang-Ford, James D. Ford, Stephen Parker, and Manon D. Fleury. 2016. "Public Health Adaptation to Climate Change in OECD Countries" International Journal of Environmental Research and Public Health 13, no. 9: 889. https://doi.org/10.3390/ijerph13090889
APA StyleAustin, S. E., Biesbroek, R., Berrang-Ford, L., Ford, J. D., Parker, S., & Fleury, M. D. (2016). Public Health Adaptation to Climate Change in OECD Countries. International Journal of Environmental Research and Public Health, 13(9), 889. https://doi.org/10.3390/ijerph13090889






