Climate Change and Infectious Disease Risk in Western Europe: A Survey of Dutch Expert Opinion on Adaptation Responses and Actors
Abstract
:1. Introduction
2. Methodology
2.1. Stakeholder Analysis and Sampling
2.2. Survey Design
2.3. Survey Content
- (a)
- Adaptation responses to climate change-induced infectious disease risk in Western Europe;
- (b)
- The priorities under budgetary constraints for mitigation or adaptation responses to climate change-induced infectious disease risk; and
- (c)
- The willingness and the capacity of potentially relevant actors to respond to climate change-induced infectious disease risk.
| Response | Description |
|---|---|
| Monitoring | Includes both indicator-based surveillance and event-based epidemic intelligence. Indicator-based surveillance refers to data collection, (trend) analysis, and interpretation of data. Indicator-based surveillance is conducted based on data from infectious disease notifications at the European Union level, pharmacy-based monitoring, sentinel surveillance, vector distribution monitoring, real-time surveillance, monitoring cause-specific deaths from infectious diseases, and syndrome surveillance. Event-based epidemic intelligence refers to the early identification of climatic change-induced infectious disease threats, through screening of news media, scientific reports, clinical case reports, and interdisciplinary reporting (such as from related industrial sectors) [3]. |
| Outbreak investigation and response | The diagnosis and investigation of new/emerging infectious diseases, as well as responding effectively to (potential) outbreaks involving the cooperation of multiple sectors. For effective response adequate supplies (such as medication and vaccinations) and distributive infrastructures are required and thus need to be included in this sort of policy option [3]. |
| Dissemination of information, and health education | The communication of information, health education, and health promotion; all relating specifically to human (risk) behavior in the context of work, recreational activities, food handling, but also personal preventive measures for vector control and minimization of exposure [3]. |
| Foster interagency and community partnerships | Fostering interagency and community partnerships, thus establishing partnerships between stakeholders across different sectors, disciplines, and levels (e.g., local community, municipality, national) [3]. |
| Enforce laws and regulations | Enforcing laws and regulations regarding reporting climate change-induced health events, setting up and enforcing conventions relating to e.g., water resources and sanitation, and regulation to e.g., minimize harmful exposures [3]. |
| Access to health care, and prevention | Providing access to health services, prevention of outbreak propagation through treatment of infected patients, and prevention (such as vaccination, prophylaxis, travel medicine) [3]. |
| Strengthen capacity of public health workforce and implement emergency preparedness training | Strengthening of the capacity (in terms of quality and quantity) of public workforce for instance through training focused on diagnosis of specific infectious diseases. In addition, this policy option includes the implementation of emergency preparedness training [3]. |
| Research | Fostering research focused on the relationship between infectious diseases and climate change, risk mapping of climate sensitive vectors and pathogens, development of diagnostic tests and vaccines, burden-of-disease studies, and climate as well as policy scenarios, amongst other related research activities [3]. |
| Environmental management/modification | The practice of using environmental management to reduce the capacity of local habitats to maintain pathogens and/or populations of disease vectors (e.g., reducing reservoir host abundance, removing larval breeding sites), thus resulting in a decrease of spread of a disease to humans/animals [17]. |
| Direct control methods | The use of chemical or biological control methods in order to reduce pathogen or vector abundance. Chemical control methods consist of, for example, the use of insecticides or water treatment chemicals. Biological control methods consist of the utilization of biological toxins and natural enemies include e.g., bacteria and larvivorous fish [17]. |
| Assessment Criterion | Description |
|---|---|
| Potential health gain | The “potential magnitude of the health gain” of the policy option [30] (p.23). |
| Uncertainty of potential health gain | The extent to which the potential health impact (i.e., gain) of the policy option is uncertain. Uncertainty refers to the predictability of the health outcomes that can result from the policy option [30]. |
| Monetary costs | Direct and indirect monetary costs of the policy option [30]. |
| Non-monetary costs | The potential (non-monetary) imposition on the health system and society at large that this policy option can create |
| Positive spill-over effects | The potential that this policy option can bring about positive side-effects for other policy areas, sectors, and/or for society |
| Flexibility | The degree of ease for modification of the policy option should this become necessary in the future [30]. |
| Urgency of implementation | The rapidity at which the policy option needs to be implemented for it to still have an effect, and if it is not to run into any implementation barriers [30]. |
| Regret if climate change does not turn out as expected | The extent that the policy option will still be effective in terms of health gain if climate change trends turn out differently than expected [30]. |
2.4. Survey Analysis
3. Results
3.1. Expert Assessment of the Responses to Climate Change-Induced Infectious Disease Risk
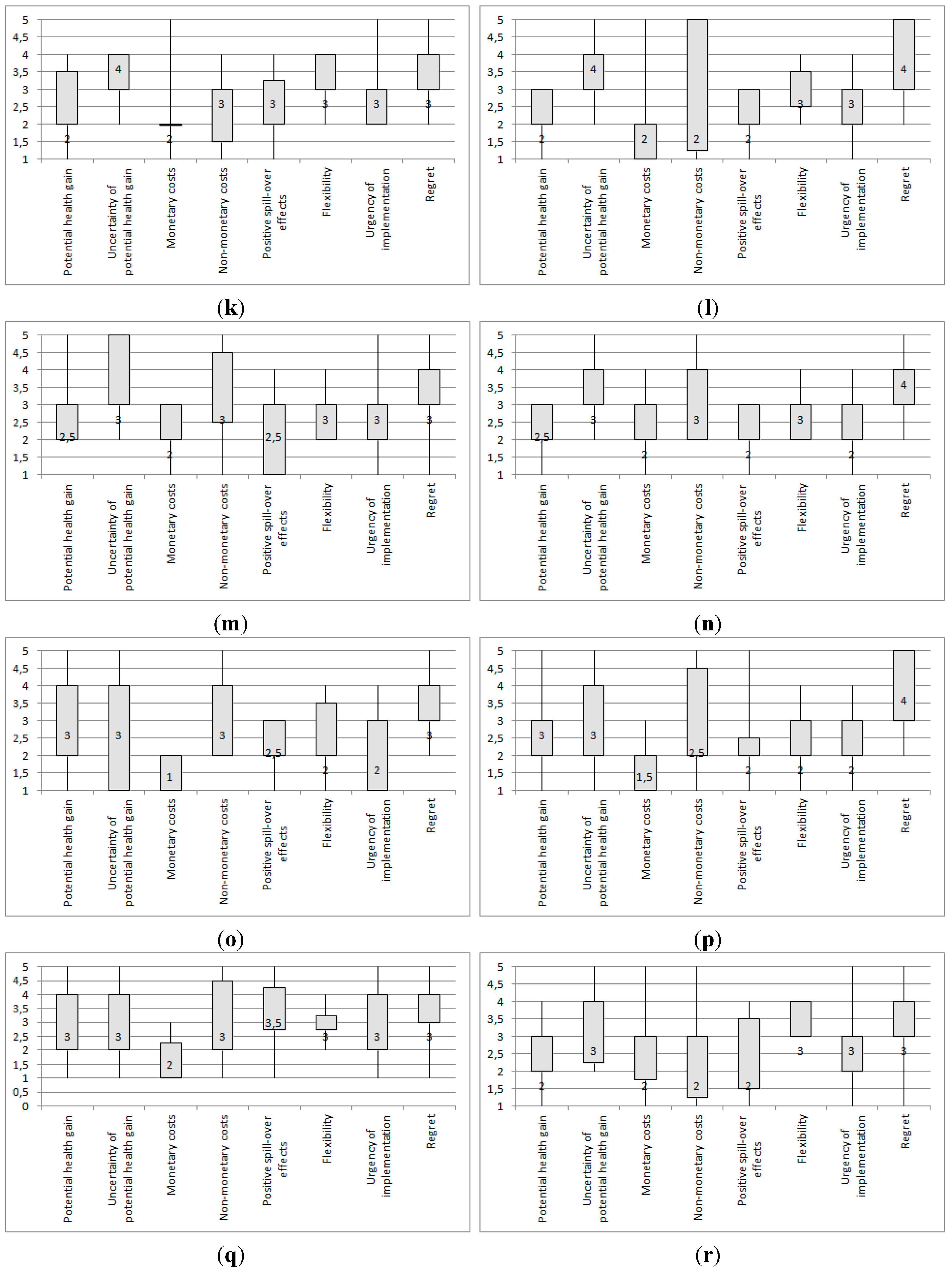

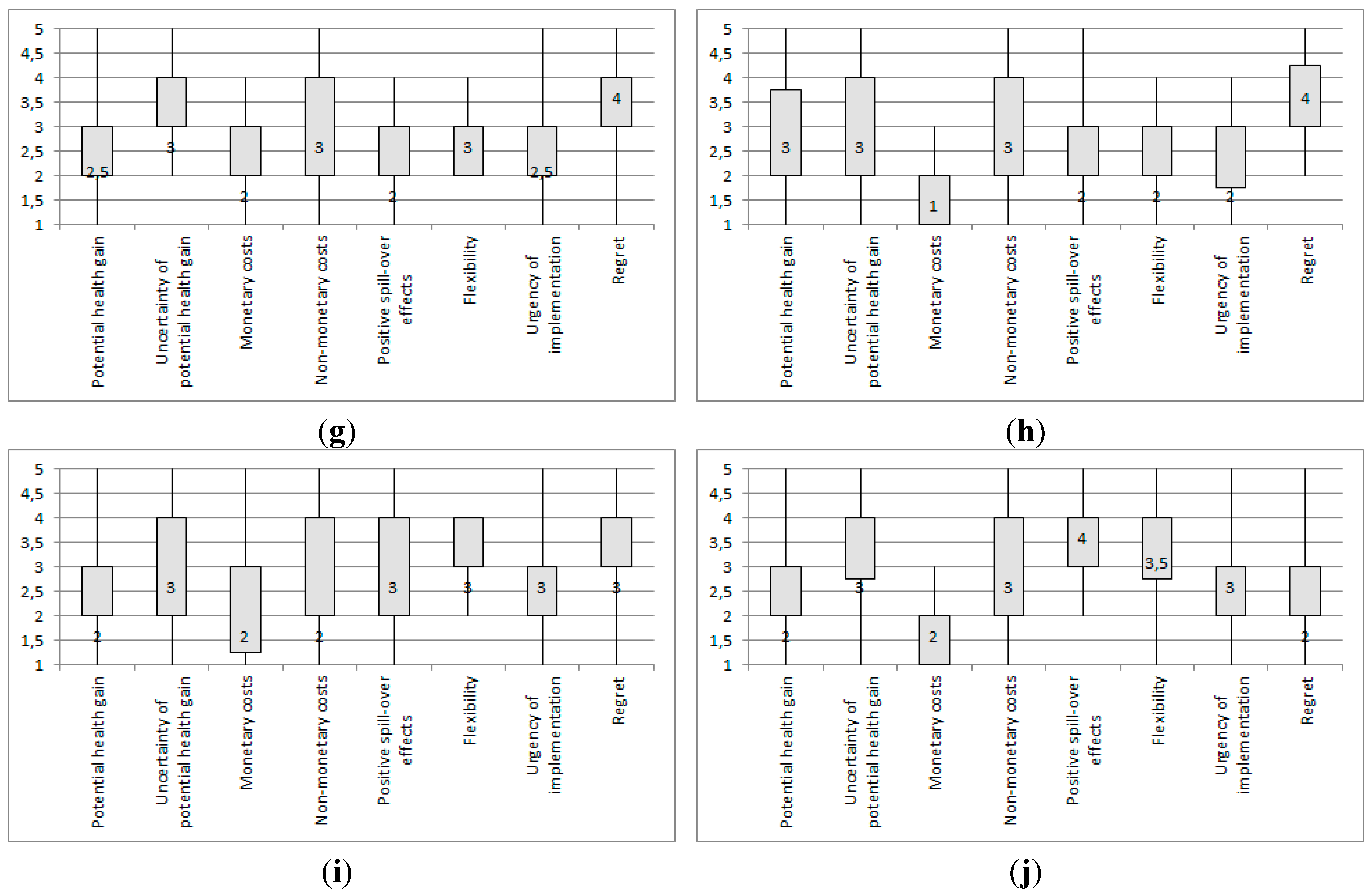



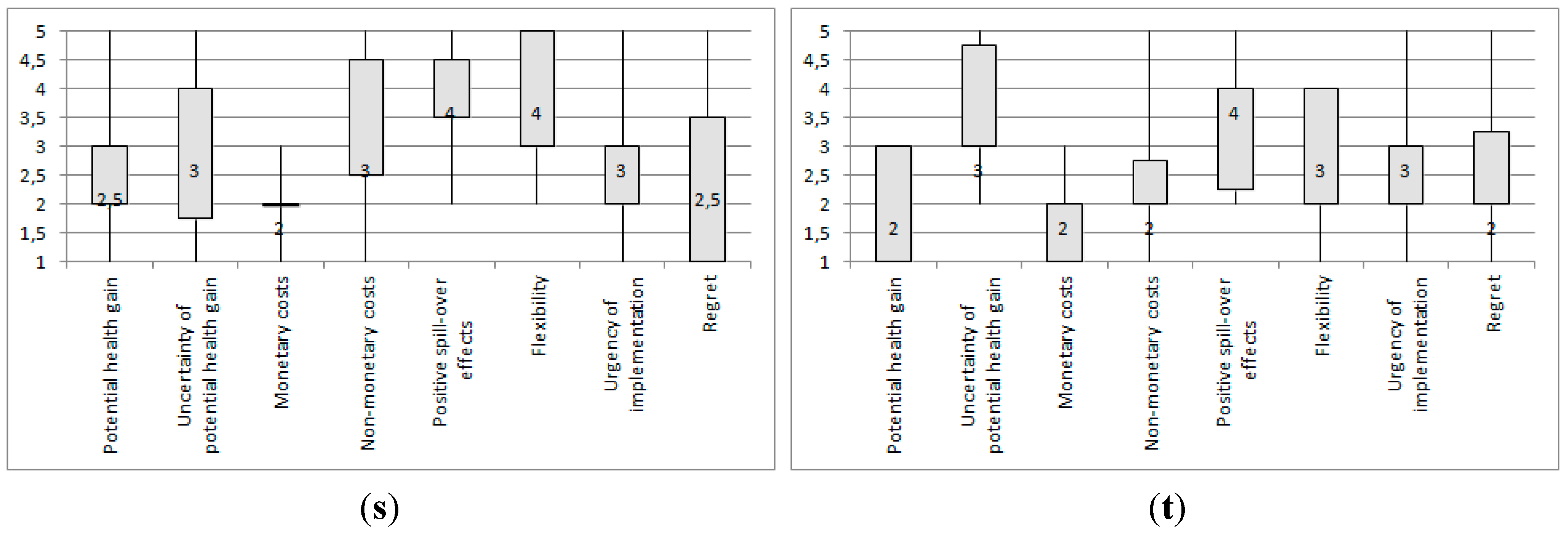
3.2. Expert Prioritization of Mitigation and Adaptation Response Strategies
| Aggregate Sample | Sample Group “Policy” | Sample Group “Science” | ||||
|---|---|---|---|---|---|---|
| Response Strategy | Mean (in %) | Standard Deviation | Mean (in %) | Standard Deviation | Mean (in %) | Standard Deviation |
| Mitigation | 50.52 | 27.37 | 47.92 | 24.63 | 52.35 | 29.75 |
| Adaptation | 49.48 | 27.37 | 52.08 | 24.63 | 47.65 | 29.75 |
3.3. Expert Assessment of Relevant Actors’ Willingness and Capacity to Respond
| Actors | Assessment of Willingness to Respond | |||||
|---|---|---|---|---|---|---|
| Aggregate Sample | Sample Group “Policy” | Sample Group “Science” | ||||
| Median | IQR | Median | IQR | Median | IQR | |
| National government/health authority | 3 | 2 | 3 | 1 | 3 | 2 |
| Local health authority | 3 | 2 | 3 | 2 | 2 | 2 |
| Policy-advice, policy-maker | 3 | 1 | 3 | 0 | 3 | 1 |
| NGO, advocacy, funders, charity | 2 | 1 | 2 | 1 | 2 | 1 |
| Science | 2 | 2 | 2 | 1 | 2 | 1.75 |
| Health care provider/health practitioner | 3 | 2 | 3 | 2 | 3 | 1.25 |
| Veterinary profession | 3 | 2 | 3 | 2 | 3 | 1.75 |
| Pharmaceutical industry | 3 | 1 | 2 | 2 | 4 | 2 |
| Farmer union | 4 | 1 | 4 | 1.5 | 4 | 2 |
| Food supply sector | 4 | 1 | 3 | 1.75 | 4 | 1.5 |
| Environmental management, conservation | 2 | 1 | 2 | 0 | 3 | 1 |
| Trade and tourism sector | 3 | 2 | 2 | 2 | 4 | 1 |
| Other business/private sector actors | 4 | 1 | 3 | 2.5 | 4 | 0 |
| Actors | Assessment of Capacity to Respond | |||||
|---|---|---|---|---|---|---|
| Aggregate Sample | Sample Group “Policy” | Sample Group “Science” | ||||
| Median | IQR | Median | IQR | Median | IQR | |
| National government/health authority | 2 | 1 | 3 | 1 | 2 | 1 |
| Local health authority | 3 | 2 | 3 | 2 | 3 | 1.75 |
| Policyadvice, policy-maker | 3 | 1 | 3 | 2 | 3 | 1 |
| NGO, advocacy, funders, charity | 3 | 1.25 | 4 | 2 | 3 | 1 |
| Science | 3 | 1 | 3 | 1 | 3 | 1 |
| Health care provider/health practitioner | 3 | 2 | 2 | 1 | 3 | 1.75 |
| Veterinary profession | 3 | 2 | 2 | 1.5 | 3 | 1.75 |
| Pharmaceutical industry | 3 | 2 | 3 | 1.25 | 3 | 2 |
| Farmer union | 3 | 2 | 3 | 1 | 3 | 2 |
| Food supply sector | 3 | 2 | 3 | 2 | 3.5 | 1.75 |
| Environmental management, conservation | 3 | 2 | 3 | 2 | 3 | 1 |
| Trade and tourism sector | 3 | 2 | 2 | 1 | 3.5 | 1 |
| Other business/private sector actors | 3 | 1.5 | 4 | 2.25 | 3 | 1.5 |
4. Discussion and Conclusions
Acknowledgments
Author Contributions
Conflicts of Interest
References
- IPCC. Summary for Policymakers; Cambridge University Press: Cambridge, UK; New York, NY, USA, 2013; pp. 1–29. [Google Scholar]
- Kovats, R.S.; Valentini, R.; Bouwers, L.M.; Georgopoulou, E.; Jacob, D.; Martin, E.; Rounsevell, M.; Soussana, J.-F. Europe; The Intergovernmental Panel on Climate Change, Cambridge University Press: Cambridge, UK; New York, NY, USA, 2014; pp. 1267–1326. [Google Scholar]
- Semenza, J.; Menne, B. Climate change and infectious diseases in Europe. Lancet 2009, 9, 365–375. [Google Scholar] [CrossRef] [PubMed]
- WHO-Europe. Climate change and health in Europe: Opportunities for action in partnership. In Protecting Children’s Health in a Changing Environment; Proceedings of the Fifth Ministerial Conference on Environment and Health, Parma, Italy, 10–12 March 2010; WHO Regional Office for Europe: Copenhagen, Denmark, 2010. [Google Scholar]
- Menne, B.; Apfel, F.; Kovats, S.; Racioppi, F. Protecting Health in EUROPE from Climate Change; World Health Organisation Regional Office for Europe: Copenhagen, Denmark, 2008. [Google Scholar]
- European Environment Agency (EEA). Climate Change, Impacts and Vulnerabilty in Europe 2012: An Indicator-Based Report; EEA Report No12/2012; European Environment Agency: Copenhagen, Denmark, 2012. [Google Scholar]
- WHO-Europe. Strategic Objective 1 to Reduce the Health, Social and Economic Burden of Communicable Diseases; WHO Region Office for Europe: Copenhagen, Denmark.
- Climate change in Europe. Available online: http://www.ecdc.europa.eu/en/healthtopics/climate_change/Pages/index.aspx (accessed on 23 April 2013).
- Martens, P.; Chang, C.T.; McEvoy, D. Integrating adaptation and mitigation to climatic changes. Regions 2012, 288, 18–20. [Google Scholar]
- Wardekker, J.A.; de Jong, A.; van Bree, L.; Turkenburg, W.C.; van der Sluijs, J.P. Health risks of climate change: An assessment of uncertainties and its implications for adaptation policies. Environ. Health 2012, 11, 67. [Google Scholar] [CrossRef] [PubMed]
- WHO-Europe. Parma Declaration on Environment and Health; WHO Europe Conference Secretariat: Copenhagen, Denmark, 2010. [Google Scholar]
- European Commission (EC). Adaptation to Climate Change Impacts on Human, Animal and Plant Health; SWD (2013) 136 final; European Commission: Brussels, Belgium, 2013. [Google Scholar]
- European Commission (EC). Adapting to Climate Change: Towards a European Framework for Action; COM (2009) 147 final; European Commission: Brussels, Belgium, 2009. [Google Scholar]
- European Commission (EC). Declaration of the European Commission. In Proceedings of the Fifth Ministerial Conference on Environment and Health, Parma, 10–12 March 2010.
- European Commission (EC). White Paper: Together for Health: A Strategic Approach for the EU 2008–2013; COM (2007) 630 final; European Commission: Brussels, Belgium, 2007. [Google Scholar]
- Smith, K.R.; Woodward, A.; Campbell-Lendrum, D.; Chadee, D.D.; Honda, Y.; Liu, Q.; Olwoch, J.W.; Revich, B.; Sauerborn, R. Human Health: Impacts, Adaptation, and Co-Benefits; Intergovernmental Panel on Climate Change, Cambridge University Press: Cambridge, UK; New York, NY, USA, 2014; pp. 709–754. [Google Scholar]
- MEA. In Ecosystems and Human Well-Being: Policy Responses; Island Press: Washington, DC, USA, 2005.
- McIntyre, K.M.; Setzkorn, C.; Baylis, M.; Waret-Szkuta, A.; Caminade, C.; Morse, A.P.; Akin, S.; Huynen, M.; Martens, P.; Morand, S. Impact of climate change on human and animal health. Vet. Rec. 2010, 167, 586. [Google Scholar] [CrossRef] [PubMed]
- De Ridder, W.; Turnpenny, J.; Nilsson, M.; von Raggamby, A. A framework for tool selection and use in integrated assessment for sustainable development. J. Environ. Assess. Policy Manag. 2007, 9, 423–441. [Google Scholar] [CrossRef]
- Kloprogge, P.; van der Sluijs, J.P. The inclusion of stakeholder knowledge and perspectives in integrated assessment of climate change. Clim. Chang. 2006, 75, 359–389. [Google Scholar] [CrossRef]
- Akin, S.; Martens, P. A survey of Dutch expert opinion on climatic drivers of infectious disease risk in Western Europe. Climate 2014, 2, 310–328. [Google Scholar] [CrossRef]
- Prell, C.; Hubacek, K.; Reed, M. Stakeholder analysis and social network analysis in natural resource management. Soc. Nat. Resour. Int. J. 2013, 22, 501–518. [Google Scholar] [CrossRef]
- Reed, M.S.; Graves, A.; Norman, D.; Posthumus, H.; Hubacek, K.; Morris, J.; Prell, C.; Quinn, C.H.; Stringer, L.C. Who’s in and why? A typology of stakeholder analysis methods for natural resource management. J. Environ. Assess. Policy Manag. 2009, 90, 1933–1949. [Google Scholar] [CrossRef] [PubMed]
- Allen, W.; Kilvington, M. Stakeholder Analysi; Crown Research Institute, Landcare Research Manaaki Whenua: Lincoln, New Zealand, 2003. [Google Scholar]
- Davie, T.; Fenemore, A.; Allen, W.; Phillips, C. Stakeholder Involvement in Integrated Catchment Management—Motueka, New Zealand; Landcare Research: Lincoln, New Zealand, 2006. [Google Scholar]
- Freeman, R.E.; McVea, J. A Stakeholder Approach to Strategic Management, Working Paper No. 01–02; University of Virginia: Charlottesville, VA, USA, 2001. [Google Scholar]
- Cooper, D.R.; Schindler, P.S. Business Research Methods, 8th ed.; McGraw-Hill/Irwin: New York, NY, USA, 2003. [Google Scholar]
- Garson, G.D. Sampling. In Blue Book Series; Statistical Associates Publishing: Raleigh, NC, USA, 2012. [Google Scholar]
- WHO-Europe. Protecting health in an environment challenged by climate change: European regional framework for action. In Contribution of the Climate Change and Health Task Force; WHO Regional Office for Europe: Copenhagen, Denmark, 2010. [Google Scholar]
- WHO-Europe. Climate Change and Health: Policy Options for Climate Change and Health; Report on a joint WHO-PBL technical meeting; WHO Europe: Bonn, Germany, 2010. [Google Scholar]
- IPCC. Appendix I Glossary; Cambridge University Press: Cambridge, UK, 2007; pp. 869–884. [Google Scholar]
- ENHANCE Research Project. Available online: http://www.liv.ac.uk/enhance/ (accessed on 9 June 2015).
- Füssel, H.-M. Adaptation planning for climate change: Concepts, assessment approaches, and key lessons. Sustain. Sci. 2007, 2, 265–275. [Google Scholar] [CrossRef]
- Ebi, K.; Kovats, R.S.; Menne, B. An approach for assessing human health vulnerability and public health interventions to adapt to climate change. Environ. Health Perspect. 2006, 114, 1930–1934. [Google Scholar] [CrossRef] [PubMed]
- WHO. The Global Burden of Disease: 2004 Update; UN World Health Organization: Geneva, Switzerland, 2008. [Google Scholar]
- Nordhaus, W.D. Expert opinion on climatic change. Am. Sci. 1994, 82, 45–51. [Google Scholar]
© 2015 by the authors; licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Akin, S.-M.; Martens, P.; Huynen, M.M.T.E. Climate Change and Infectious Disease Risk in Western Europe: A Survey of Dutch Expert Opinion on Adaptation Responses and Actors. Int. J. Environ. Res. Public Health 2015, 12, 9726-9749. https://doi.org/10.3390/ijerph120809726
Akin S-M, Martens P, Huynen MMTE. Climate Change and Infectious Disease Risk in Western Europe: A Survey of Dutch Expert Opinion on Adaptation Responses and Actors. International Journal of Environmental Research and Public Health. 2015; 12(8):9726-9749. https://doi.org/10.3390/ijerph120809726
Chicago/Turabian StyleAkin, Su-Mia, Pim Martens, and Maud M.T.E. Huynen. 2015. "Climate Change and Infectious Disease Risk in Western Europe: A Survey of Dutch Expert Opinion on Adaptation Responses and Actors" International Journal of Environmental Research and Public Health 12, no. 8: 9726-9749. https://doi.org/10.3390/ijerph120809726





