Changes in Tobacco Use, Susceptibility to Future Smoking, and Quit Attempts among Canadian Youth over Time: A Comparison of Off-Reserve Aboriginal and Non-Aboriginal Youth
Abstract
:1. Introduction
2. Methods
2.1. Study Design
2.2. Measures
2.3. Survey Protocol
2.4. Analyses
3. Results
3.1. Demographics
3.2. Prevalence of Smoking Behaviour among ORA and Non-Aboriginal Youth Over Time
| 2004 (n = 23,362) | 2006 (n = 34,050) | 2008 (n = 31,249) | |||||||
|---|---|---|---|---|---|---|---|---|---|
| Aboriginal a | Non-Aboriginal a | Chi-Square | Aboriginal a | Non-Aboriginal a | Chi-Square | Aboriginal a | Non-Aboriginal a | Chi-Square | |
| Sex | |||||||||
| Male | 54.2 | 50.9 | Х2 = 4.00 (1), p = 0.05 | 52.9 | 50.9 | Х2 = 4.00 (1), p = 0.05 | 52.4 | 50.7 | Х2 = 2.51 (1), p = 0.11 |
| Female | 45.8 | 49.1 | 47.1 | 49.1 | 47.6 | 49.3 | |||
| Grade | |||||||||
| 6 | 24.7 | 24.0 | Х2 = 22.9 (3), p < 0.001 | 23.4 | 21.8 | Х2 = 8.92 (3), p = 0.03 | 23.1 | 22.9 | Х2 = 5.49 (3), p = 0.14 |
| 7 | 19.8 | 25.6 | 24.8 | 24.7 | 24.8 | 24.7 | |||
| 8 | 24.9 | 25.2 | 23.9 | 26.5 | 23.9 | 25.9 | |||
| 9 | 30.7 | 25.2 | 27.9 | 27.0 | 28.2 | 26.5 | |||
| Weekly | |||||||||
| spending | |||||||||
| money | |||||||||
| $0 | 23.9 | 21.9 | Х2 = 42.9 (3), p < 0.001 | 13.4 | 19.1 | Х2 = 104.4 (3), p < 0.001 | 17.5 | 23.2 | Х2 = 146.75 (3), p < 0.001 |
| $1 to $20 | 37.4 | 46.9 | 50.2 | 49.0 | 40.4 | 44.4 | |||
| $21 or more | 26.7 | 19.3 | 27.6 | 20.8 | 29.3 | 18.9 | |||
| Don’t know | 12.0 | 11.9 | 8.8 | 11.1 | 12.8 | 13.4 | |||
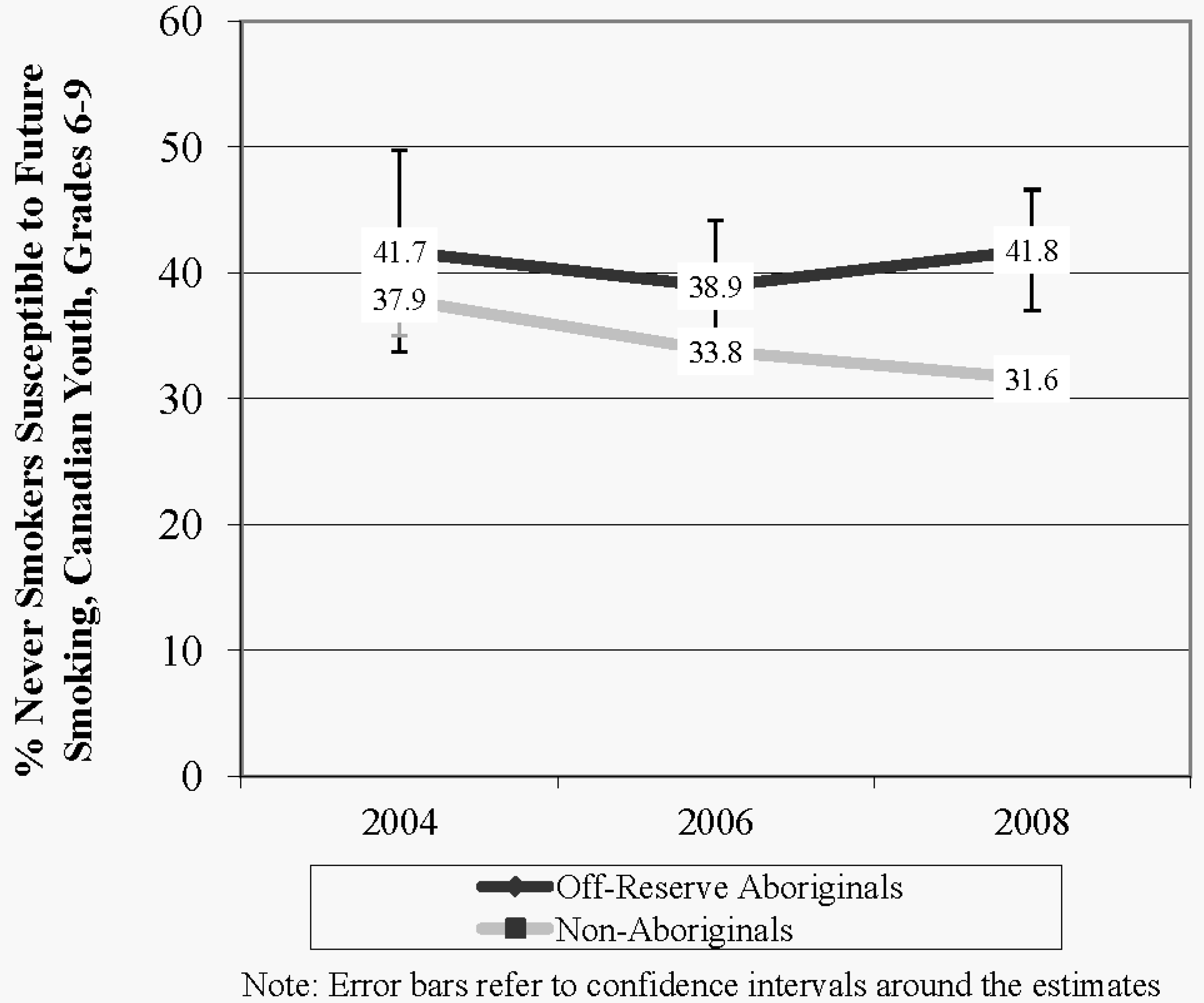
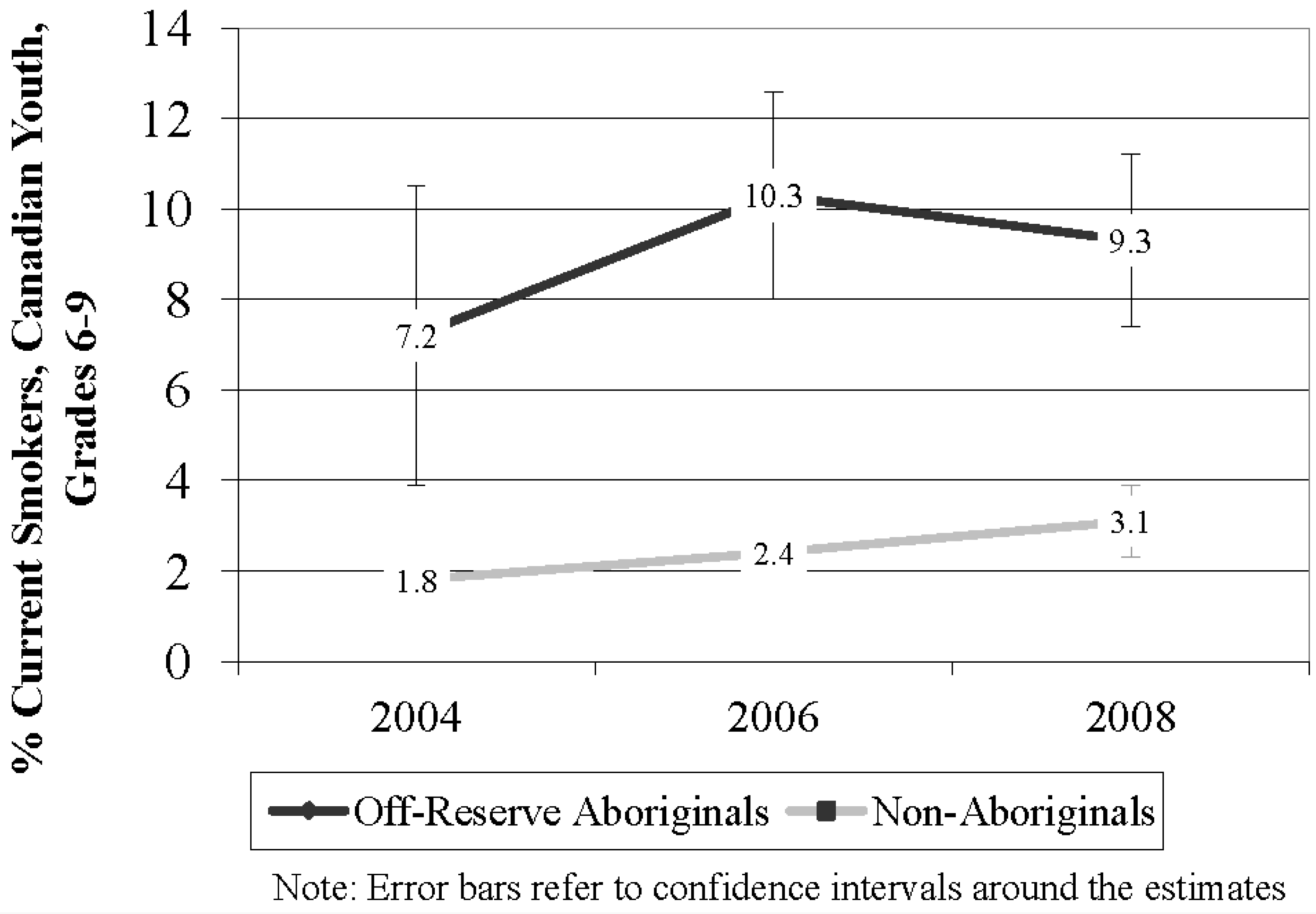

3.3. Testing the Differences in Smoking Behaviour among ORA and Non-Aboriginal Youth
| Adjusted odds ratio* (95% CI) | ||||
|---|---|---|---|---|
| Model 1 | Model 2 | Model 3 | ||
| Parameters | Current smoking vs. Non-smoking | Susceptibility to future smoking vs. Non-Susceptible † | Ever made a quit attempt vs. Never made a quit attempt ‡ | |
| Sex | ||||
| Male | 1.00 | 1.00 | 1.00 | |
| Female | 0.87 (0.80 to 0.95) || | 0.97 (0.94 to 1.01) | 1.91 (1.56 to 2.33) ¶ | |
| Grade | ||||
| 6 | 1.00 | 1.00 | 1.00 | |
| 7 | 5.30 (3.64 to 7.71) ¶ | 1.21 (1.15 to 1.27) ¶ | 1.47 (0.58 to 3.76) | |
| 8 | 12.77 (8.86 to 18.41) ¶ | 1.26 (1.19 to 1.33) ¶ | 1.35 (0.54 to 3.35) | |
| 9 | 22.77 (15.80 to 32.83) ¶ | 1.09 (1.02 to 1.17) § | 1.22 (0.49 to 3.03) | |
| Weekly Spending Money | ||||
| $0 | 1.00 | 1.00 | 1.00 | |
| $1 to $20 | 1.78 (1.52 to 2.09) ¶ | 1.12 (1.08 to 1.17) ¶ | 1.65 (1.15 to 2.37) || | |
| $21 or more | 3.80 (3.25 to 4.44) ¶ | 1.43 (1.35 to 1.51) ¶ | 1.07 (0.75 to 1.52) | |
| Don’t know | 2.05 (1.70 to 2.48) ¶ | 1.08 (1.02 to 1.15) § | 1.63 (1.04 to 2.54) § | |
| Survey Year | ||||
| 2004 | 1.00 | 1.00 | 1.00 | |
| 2006 | 1.24 (0.97 to 1.59) | 0.78 (0.72 to 0.86) ¶ | 0.95 (0.58 to 1.55) | |
| 2008 | 1.54 (1.20 to 1.99) ¶ | 0.79 (0.72 to 0.87) ¶ | 0.91 (0.55 to 1.49) | |
| Aboriginal status | ||||
| Non-Aboriginal | 1.00 | 1.00 | 1.00 | |
| Aboriginal | 3.91 (3.47 to 4.41) ¶ | 1.37 (1.27 to 1.48) ¶ | 0.74 (0.57 to 0.96) § | |
4. Discussion
Limitations
5. Conclusions
Acknowledgements
Conflict of Interest
References
- Information on Global Tobacco Use. Available online: http://www.who.int/tobacco/health_priority/en/index.html (accessed on 26 July 2012).
- World Health Organization. WHO Report on the Global Tobacco Epidemic, 2009: Implementing Smoke-Free Environments. Available online: http://whqlibdoc.who.int/publications/2009/9789241563918_eng_full.pdf (accessed on 26 July 2012).
- King, M. Chronic diseases and mortality in Canadian Aboriginal peoples: Learning from the knowledge. Chron. Dis. Can. 2010, 31, 2–3. [Google Scholar]
- Tjepkema, M.; Wilkins, R.; Senécal, S.; Guimond, É.; Penney, C. Mortality of urban Aboriginal adults in Canada, 1991–2001. Chron. Dis. Can. 2010, 31, 4–21. [Google Scholar]
- Wardman, D.; Khan, N. Smoking-attributable mortality among British Columbia’s first nations populations. Int. J. Circumpol. Health 2004, 63, 81–92. [Google Scholar]
- First Nations Centre. First Nations Regional Longitudinal Health Survey Phase 2 (2008–2010) Preliminary Results. 2010. Available online: http://www.rhs-ers.ca/sites/default/files/RHSPrelimReport.pdf (accessed on 26 July 2012).
- First Nations Centre. First Nations Regional Longitudinal Health Survey 2002/03: Results for Adults, Youth and Children Living in First Nations Communities. Available online: http://www.rhs-ers.ca/english/pdf/rhs2002–03reports/rhs2002–03-technicalreport-afn.pdf (accessed on 10 November 2012).
- Retnakaran, R.; Hanley, A.; Connelly, P.; Harris, S.; Zinman, B. Cigarette smoking and cardiovascular risk factors among aboriginal Canadian youths. Can. Med. Assoc. J. 2005, 173, 885–889. [Google Scholar] [CrossRef]
- US Department of Health and Human Services, The Health Consequences of Smoking; Office on Smoking and Health, Centre for Disease Control and Prevention: Atlanta, GA, USA, 2004.
- Adami, H.O.; Day, N.E.; Trichopoulos, N.E.; Willett, W.C. Primary and secondary prevention in the reduction of cancer morbidity and mortality. Euro. J. Canc. 2001, 37, S118–S127. [Google Scholar]
- Colditz, G.A.; DeJong, W.; Hunter, D.J.; Trichopoulos, D. Harvard report on cancer prevention. Causes of human cancer. Canc. Causes Contr. 1996, 7, S3–S58. [Google Scholar] [CrossRef]
- Young, T.K. Review of research on aboriginal populations in Canada: Relevance to their health needs. Br. Med. J. 2003, 327, 419–422. [Google Scholar]
- Statistics Canada. 2006 Census: Aboriginal Peoples in Canada in 2006: Inuit, Métis and First Nations, 2006 Census. Available online: http://www12.statcan.ca/census-recensement/2006/as-sa/97–558/p16-eng.cfm (accessed on 10 November 2010).
- Hutchinson, P.J.; Richardson, C.G.; Bottorff, J.L. Emergent cigarette smoking, correlations with depression and interest in cessation among Aboriginal adolescents in British Columbia. Can. J. Publ. Health 2008, 99, 418–422. [Google Scholar]
- Johnson, J.L.; Tucker, R.S.; Ratner, P.A.; Bottorff, J.L.; Prkachin, K.M.; Shoveller, J.; Zumbo, B. Socio-demographic correlates of cigarette smoking among high school students: Results from the British Columbia youth survey on smoking and health. Can. J. Publ. Health 2004, 95, 268–271. [Google Scholar]
- Tjepkema, M. The health of the off-reserve Aboriginal population. Health Rep. 2002, 13, 1–16. [Google Scholar]
- Elton-Marshall, T.; Leatherdale, S.; Burkhalter, R. Tobacco, alcohol and illicit drug use among Aboriginal youth living off-reserve: Results from the youth smoking survey. Can. Med. Assoc. J. 2011, 183, E480–E486. [Google Scholar] [CrossRef]
- Elton-Marshall, T.; Leatherdale, S.T.; Manske, S.R.; Wong, K.; Ahmed, R.; Burkhalter, R. Research methods of the Youth Smoking Survey (YSS). Chron. Dis. Can. 2011, 32, 47–54. [Google Scholar]
- Health Canada. Terminology. Available online: http://www.hc-sc.gc.ca/hc-ps/tobac-tabac/research-recherche/stat/survey-sondage_term-eng.php (accessed on 26 July 2012).
- Pierce, J.P.; Choi, W.S.; Gilpin, E.A.; Farkas, A.J.; Merritt, R.K. Validation of susceptibility as a predictor of which adolescents take up smoking in the United States. Health Psychol. 1996, 15, 355–361. [Google Scholar] [CrossRef]
- Substance Abuse and Mental Health Services Administration, Center for Behavioral Health Statistics and Quality; The NSDUH Report for Substance Use among American Indian or Alaska Native Adolescents: Rockville, MD, USA, 4 October 2011.
- Substance Use among Aboriginal and Torres Strait Islander People; Australian Institute of Health and Welfare: Canberra, Australia, 2011.
- Thomas, D.P. Changes in smoking intensity among Aboriginal and Torres Strait Islander people, 1994–2008. Med. J. Aust. 2012, 197, 503–506. [Google Scholar] [CrossRef]
- Conigrave, K.; Lee, K. Smoking or alcohol dependence among indigenous Australians: Treatment may be needed, not just education. Heart Lung Circul. 2012, 21, 626–631. [Google Scholar] [CrossRef]
- Kirmayer, L.J.; Brass, G.M.; Tait, C.L. The mental health of aboriginal peoples: Transformations of identity and community. Can. J. Psychiatr. 2000, 45, 607–616. [Google Scholar]
- Schinke, S.P.; Singer, B.; Cole, K.; Contento, I.R. Reducing cancer risk among native American adolescents. Prev. Med. 1996, 25, 146–155. [Google Scholar]
- Carson, K.V.; Brinn, M.P.; Labiszewski, N.A.; Peters, M.; Chang, A.B.; Veale, A.; Esterman, A.J.; Smith, B.J. Interventions for tobacco use prevention in indigenous youth. Cochrane Database Syst. Rev. 2012, 8. [Google Scholar] [CrossRef]
- Ivers, R.G. A review of tobacco interventions for indigenous Australians. Aust. New Zeal. J. Publ. Health 2003, 27, 294–299. [Google Scholar] [CrossRef]
- Statistics Canada. 2006 Census: Aboriginal Peoples in Canada in 2006: Inuit, Métis and First Nations, 2006 Census. Aboriginal people surpass the one-million mark 2006. Available online: http://www12.statcan.ca/census-recensement/2006/as-sa/97-558/p2-eng.cfm (accessed on 4 February 2010).
- Fiore, M.C.; Jaén, C.R.; Baker, T.B.; Bailey, W.C.; Benowitz, N.L.; Curry, S.J. Treating Tobacco Use and Dependence: 2008 Update. Clinical Practice Guideline; U.S. Department of Health and Human Services Public Health Service: Washington, DC, USA, 2008. [Google Scholar]
- Stead, L.; Bergson, G.; Lancaster, T. Physician advice for smoking cessation. Cochrane Database Syst. Rev. 2004, 18. [Google Scholar] [CrossRef]
© 2013 by the authors; licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution license (http://creativecommons.org/licenses/by/3.0/).
Share and Cite
Elton-Marshall, T.; Leatherdale, S.T.; Burkhalter, R.; Brown, K.S. Changes in Tobacco Use, Susceptibility to Future Smoking, and Quit Attempts among Canadian Youth over Time: A Comparison of Off-Reserve Aboriginal and Non-Aboriginal Youth. Int. J. Environ. Res. Public Health 2013, 10, 729-741. https://doi.org/10.3390/ijerph10020729
Elton-Marshall T, Leatherdale ST, Burkhalter R, Brown KS. Changes in Tobacco Use, Susceptibility to Future Smoking, and Quit Attempts among Canadian Youth over Time: A Comparison of Off-Reserve Aboriginal and Non-Aboriginal Youth. International Journal of Environmental Research and Public Health. 2013; 10(2):729-741. https://doi.org/10.3390/ijerph10020729
Chicago/Turabian StyleElton-Marshall, Tara, Scott T. Leatherdale, Robin Burkhalter, and K. Stephen Brown. 2013. "Changes in Tobacco Use, Susceptibility to Future Smoking, and Quit Attempts among Canadian Youth over Time: A Comparison of Off-Reserve Aboriginal and Non-Aboriginal Youth" International Journal of Environmental Research and Public Health 10, no. 2: 729-741. https://doi.org/10.3390/ijerph10020729





