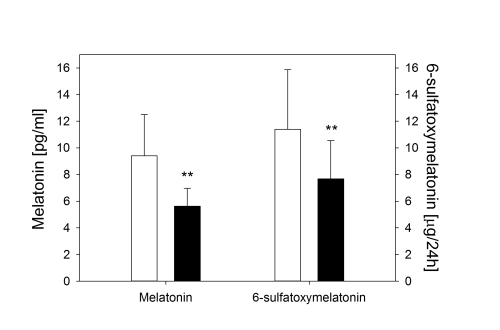
Does Melatonin Homeostasis Play a Role in Continuous Epigastric Pain Syndrome?
Abstract
:1. Introduction
2. Results and Discussion
3. Experimental Section
3.1. Patients
3.2. Study Design and Procedures
3.3. Ethics
3.4. Statistical Analysis
4. Conclusions
Conflict of Interest
References
- Bubenik, G.A.; Hacker, R.R.; Brown, G.M.; Bartos, L. Melatonin concentrations in the luminal fluid, mucosa, and muscularis of the bovine and porcine gastrointestinal tract. J. Pineal Res 1999, 26, 56–63. [Google Scholar]
- Bubenik, G.A. Localization, physiological significance and possible clinical implication of gastrointestinal melatonin. Biol. Signals Recept 2001, 10, 350–366. [Google Scholar]
- Huether, G. Melatonin synthesis in the gastrointestinal tract and the impact of nutritional factors on circulating melatonin. Ann. N. Y. Acad. Sci 1994, 31, 146–158. [Google Scholar]
- Lane, E.A.; Moss, H.B. Pharmacokinetics of melatonin in man: First pass hepatic metabolism. J. Clin. Endocrinol. Metab 1985, 61, 1214–1216. [Google Scholar]
- Messner, M.; Huether, G.; Lorf, T.; Ramadori, G.; Schwörer, H. Presence of melatonin in the human hepatobiliary-gastrointestinal tract. Life Sci 2001, 69, 543–551. [Google Scholar]
- Arendt, J.; Bojkowski, C.; Franey, C.; Wright, J.; Marks, V. Immunoassay of 6-hydroxymelatonin sulfate in human plasma and urine: Abolition of the urinary 24-hour rhythm with atenolol. J. Clin. Endocrinol. Metab 1985, 60, 1166–1173. [Google Scholar]
- Baskett, J.J.; Cockrem, J.F.; Antunovich, T.A. Sulphatoxymelatonin excretion in older people: Relationship to plasma melatonin and renal function. J. Pineal Res 1998, 24, 58–61. [Google Scholar]
- Chojnacki, C.; Wiśniewska-Jarosińska, M.; Kulig, G.; Majsterek, J.; Reiter, R.J.; Chojnacki, J. Evaluation of enterochromaffin cells and melatonin secretion exponents in patirnts with acute phase of ulcerative colitis. World J. Gastroenterol. 2012, in press. [Google Scholar]
- Lee, P.P.; Pang, S.F. Melatonin and its receptors in the gastrointestinal tract. Biol. Signals 1993, 2, 181–193. [Google Scholar]
- Brzeziński, A. Melatonin in humans. N. Engl. J. Med 1997, 336, 186–192. [Google Scholar]
- Konturek, P.C.; Konturek, S.J.; Majka, J.; Zembala, M.; Hahn, E.G. Melatonin affords protection against gastric lesions induced by ischemia-reperfusion possibly due to its antioxidant and mucosal microcirculatory effects. Eur. J. Pharmacol 1997, 322, 73–77. [Google Scholar]
- Sener-Muratoğlu, G.; Paskaloğlu, K.; Arbak, S.; Hürdağ, C.; Ayanoğlu-Dülger, G. Protective effect of famotidine, omeprazole, and melatonin against acetylsalicylic acid-induced gastric damage in rats. Dig. Dis. Sci 2001, 46, 318–330. [Google Scholar]
- Bilici, D.; Süleyman, H.; Banoğlu, Z.N.; Kiziltunç, A.; Avci, B.; Ciftçioğlu, A.; Bilici, S. Melatonin prevents ethanol-induced gastric mucosal damage possibly due to its antioxidant effect. Dig. Dis. Sci 2002, 47, 856–861. [Google Scholar]
- Klupińska, G.; Wiśniewska-Jarosińska, M.; Harasiuk, A.; Chojnacki, C.; Stec-Michalska, K.; Błasiak, J.; Reiter, R.J.; Chojnacki, J. Nocturnal secretion of melatonin in patients with upper digestive tract disorders. J. Physiol. Pharmacol 2006, 5, 41–50. [Google Scholar]
- Chojnacki, C.; Poplawski, T.; Klupinska, G.; Blasiak, J.; Chojnacki, J.; Reiter, R.J. Secretion of melatonin and 6-sulfatoxymelatonin urinary excretion in functional dyspepsia. World J. Gastroenterol 2011, 17, 2646–2651. [Google Scholar]
- Konturek, S.J.; Konturek, P.C.; Brzozowski, T.; Bubenik, G.A. Role of melatonin in upper gastrointestinal tract. J. Physiol. Pharmacol 2007, 6, 23–52. [Google Scholar]
- Mozaffari, S.; Rahimi, R.; Abdollahi, M. Implications of melatonin therapy in irritable bowel syndrome: A systematic review. Curr. Pharm. Des 2010, 16, 3646–3655. [Google Scholar]
- Pozo, M.J.; Gomez-Pinilla, P.J.; Camello-Almaraz, C.; Martin-Cano, F.E.; Pascua, P.; Rol, M.A.; Acuña-Castroviejo, D.; Camello, P.J. Melatonin, a potential therapeutic agent for smooth muscle-related pathological conditions and aging. Curr. Med. Chem 2010, 7, 4150–4165. [Google Scholar]
- Drossman, D.A. The functional gastrointestinal disorders and the Rome III process. Gastroenterology 2006, 130, 1377–1390. [Google Scholar]
- Tack, J.; Talley, N.J.; Camilleri, M.; Holtmann, G.; Hu, P.; Malagelada, J.R.; Stanghellini, V. Functional gastroduodenal disorders. Gastroenterology 2006, 130, 1466–1479. [Google Scholar]
- Cremonini, F.; Delgado-Aros, S.; Talley, N.J. Functional dyspepsia: Drugs for new (and old) therapeutic targets. Best Pract. Res. Clin. Gastroenterol 2004, 18, 717–733. [Google Scholar]
- Moayyedi, P.; Delaney, B.C.; Vakil, N.; Forman, D.; Talley, N.J. The efficacy of proton pump inhibitors in nonulcer dyspepsia: A systematic review and economic analysis. Gastroenterology 2004, 127, 1329–1337. [Google Scholar]
- Klupińska, G.; Poplawski, T.; Drzewoski, J.; Harasiuk, A.; Reiter, R.J.; Blasiak, J.; Chojnacki, J. Therapeutic effect of melatonin in patients with functional dyspepsia. Clin. Gastroenterol 2007, 41, 270–274. [Google Scholar]
- Reiter, R.J.; Tan, D.X.; Mayo, J.C.; Sainz, R.M.; Leon, J.; Czarnocki, Z. Melatonin as an antioxidant: Biochemical mechanisms and pathophysiological implications in humans. Acta Biochim. Pol 2003, 50, 1129–1146. [Google Scholar]
- Reiter, R.J.; Tan, D.X.; Mayo, J.C. Neurally-mediated and neurally-independent beneficial actions of melatonin in the gastrointestinal tract. J. Physiol. Pharmacol 2003, 54, 113–125. [Google Scholar]
- Klupińska, G.; Popławski, T.; Smigielski, J.; Błasiak, J.; Chojnacki, J. The effect of melatonin on oxidative DNA damage in gastric mucosa cells of patients with functional dyspepsia. Pol. Merkur. Lek 2009, 26, 366–369. [Google Scholar]
- Kato, K.; Murai, I.; Asai, S.; Takahashi, Y.; Matsuno, Y.; Komuro, S.; Kurosaka, H.; Iwasaki, A.; Ishikawa, K.; Arakawa, Y. Central nervous system action of melatonin on gastric acid and pepsin secretion in pylorus-ligated rats. Neuroreport 1998, 9, 3989–3992. [Google Scholar]
- Sjöblom, M.; Flemström, G. Melatonin in the duodenal lumen is a potent stimulant of mucosal bicarbonate secretion. J. Pineal Res 2003, 34, 288–293. [Google Scholar]
- Brzozowska, I.; Konturek, P.C.; Brzozowski, T.; Konturek, S.J.; Kwiecień, S.; Pajdo, R.; Drozdowicz, D.; Pawlik, M.; Ptak, A.; Hahn, E.G. Role of prostaglandins, nitric oxide, sensory nerves and gastrin in acceleration of ulcer healing by melatonin and its precursor, l-tryptophan. J. Pineal Res 2002, 32, 149–162. [Google Scholar]
- Mei, Q.; Yu, J.P.; Xu, J.M.; Wei, W.; Xiang, L.; Yue, L. Melatonin reduces colon immunological injury in rats by regulating activity of macrophages. Acta Pharmacol. Sin 2002, 23, 882–886. [Google Scholar]
- Pentney, P.T.; Bubenik, G.A. Melatonin reduces the severity of dextran-induced colitis in mice. J. Pineal Res 1995, 19, 31–39. [Google Scholar]
- Carrillo-Vico, A.; Guerrero, J.M.; Lardone, P.J.; Reiter, R.J. A review of the multiple actions of melatonin on the immune system. Endocrine 2005, 27, 189–200. [Google Scholar]
- Guerrero, J.M.; Reiter, R.J. Melatonin-immune system relationships. Curr. Top. Med. Chem 2002, 2, 167–179. [Google Scholar]
- Reyes-Vázquez, C.; Naranjo-Rodríguez, E.B.; García-Segoviano, J.A.; Trujillo-Santana, J.T.; Prieto-Gómez, B. Apamin blocks the direct relaxant effect of melatonin on rat ileal smooth muscle. J. Pineal Res 1997, 22, 1–8. [Google Scholar]
- Forster, E.R.; Green, T.; Elliot, M.; Bremner, A.; Dockray, G.J. Gastric emptying in rats: Role of afferent neurons and cholecystokinin. Am. J. Physiol 1990, 258, 552–556. [Google Scholar]
- Barajas-López, C.; Peres, A.L.; Espinosa-Luna, R.; Reyes-Vázquez, C.; Prieto-Gómez, B. Melatonin modulates cholinergic transmission by blocking nicotinic channels in the guinea-pig submucous plexus. Eur. J. Pharmacol 1996, 312, 319–325. [Google Scholar]
- Bonouali-Pellissier, S. Melatonin is involved in cholecystokinin-induced changes of ileal motility in rats. J. Pineal Res 1994, 17, 79–85. [Google Scholar]
- Bubenik, G.A. The effect of serotonin, N-acetylserotonin, and melatonin on spontaneous contractions of isolated rat intestine. J. Pineal Res 1986, 3, 41–54. [Google Scholar]
- Harlow, H.J.; Weekley, B.L. Effect of melatonin on the force of spontaneous contractions of in vitro rat small and large intestine. J. Pineal Res 1986, 3, 277–284. [Google Scholar]
- De Souza Pereira, R. Regression of gastroesophageal reflux disease symptoms using dietary supplementation with melatonin, vitamins and minoacids:comparison with omeprazole. J. Pineal Res 2006, 41, 195–200. [Google Scholar]
- Werbach, M.R. Melatonin for the treatment of gastroesophageal reflux disease. Altern. Ther. Health Med 2008, 14, 54–58. [Google Scholar]
- Kandil, T.S.; Mousa, A.A.; El-Gendy, A.A.; Abbas, A.M. The potential therapeutic effect of melatonin in Gastro-Esophageal Reflux Disease. BMC Gastroenterol 2010, 18, 10–17. [Google Scholar]
- Rapoport, S.I.; Raĭkhlin, N.T.; Malinovskaia, N.K.; Lakshin, A.A. Ultrastructural changes in cells of the antral gastric mucosa in patients with duodenal ulcers treated with melatonin. Ter. Arkh 2003, 75, 10–14. [Google Scholar]
- Song, G.H.; Leng, P.H.; Gwee, K.A.; Moochhala, S.M.; Ho, K.Y. Melatonin improves abdominal pain in irritable bowel syndrome patients who have sleep disturbances: A randomised, double blind, placebo controlled study. Gut 2005, 54, 1402–1407. [Google Scholar]
- Lu, W.Z.; Gwee, K.A.; Moochhalla, S.; Ho, K.Y. Melatonin improves bowel symptoms in female patients with irritable bowel syndrome: A double-blind placebo-controlled study. Aliment. Pharmacol. Ther 2005, 22, 927–934. [Google Scholar]
- Saha, L.; Malhotra, S.; Rana, S.; Bhasin, D.; Pandhi, P. A preliminary study of melatonin in irritable bowel syndrome. J. Clin. Gastroenterol 2007, 41, 29–32. [Google Scholar]
- Chojnacki, C.; Wisniewska-Jarosinska, M.; Walecka-Kapica, E.; Klupinska, G.; Jaworek, J.; Chojnacki, J. Evaluation of melatonin effectiveness in the adjuvant treatment of ulcerative colitis. J. Physiol. Pharmacol 2011, 62, 327–334. [Google Scholar]
- Terry, P.D.; Villinger, F.; Bubenik, G.A.; Sitaraman, S.V. Melatonin and ulcerative colitis: Evidence, biological mechanisms, and future research. Inflamm. Bowel Dis 2009, 15, 134–140. [Google Scholar]
- Mickle, A.; Sood, M.; Shahmohammadi, G.; Sengupta, J.N.; Miranda, A. Antinociceptive effects of melatonin in a rat model of post-inflammatory visceral hyperalgesia: A centrally mediated process. Pain 2010, 149, 555–564. [Google Scholar]
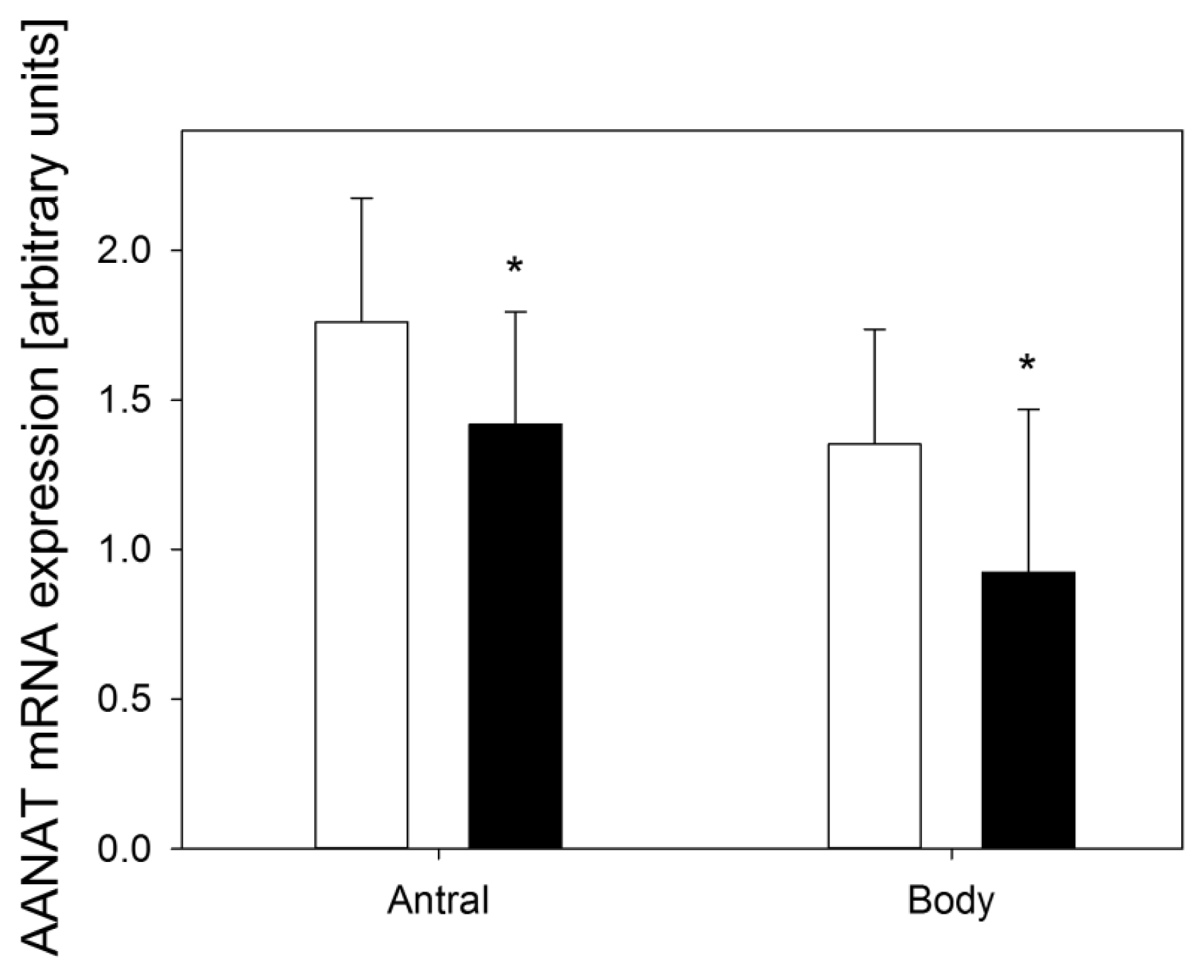
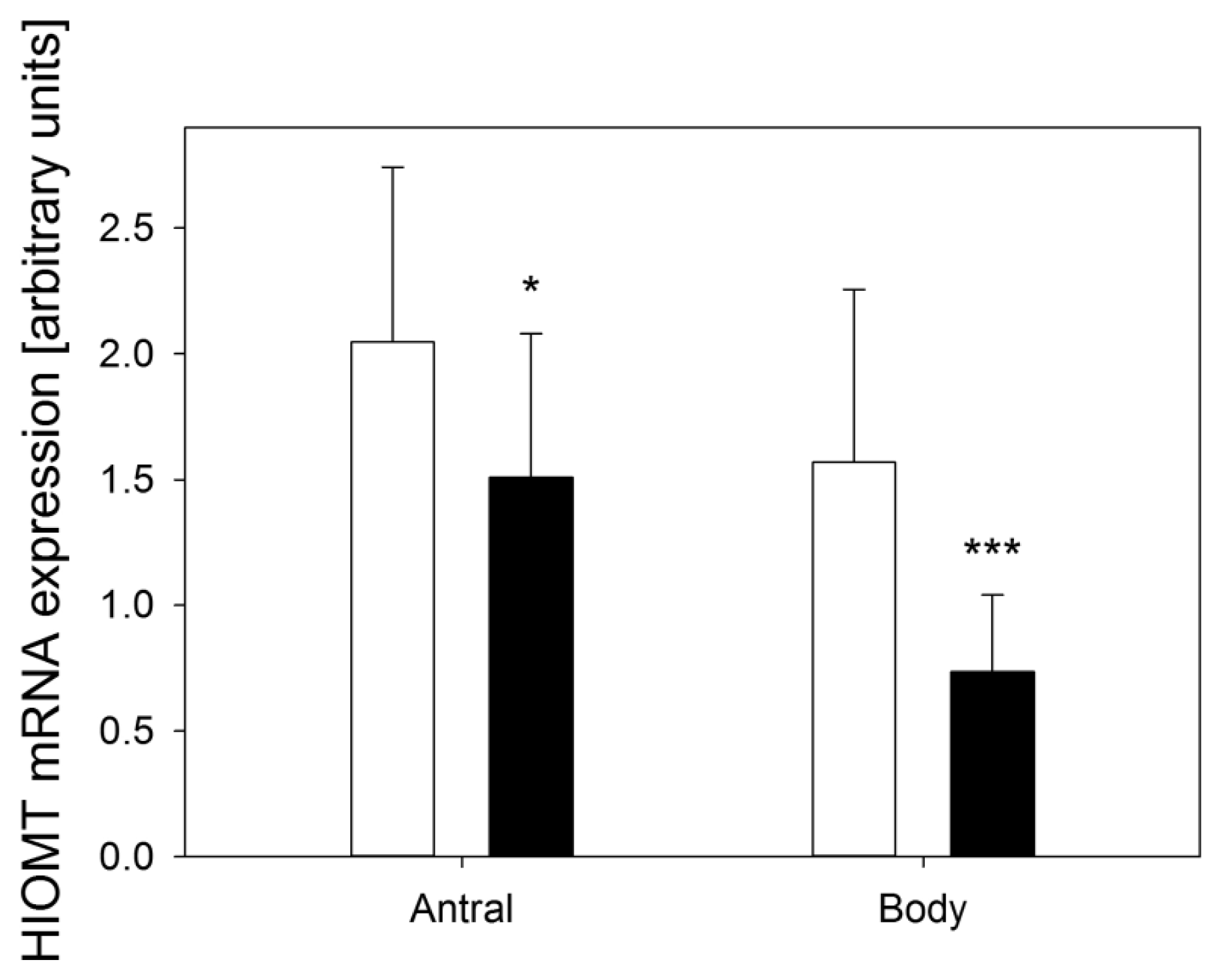

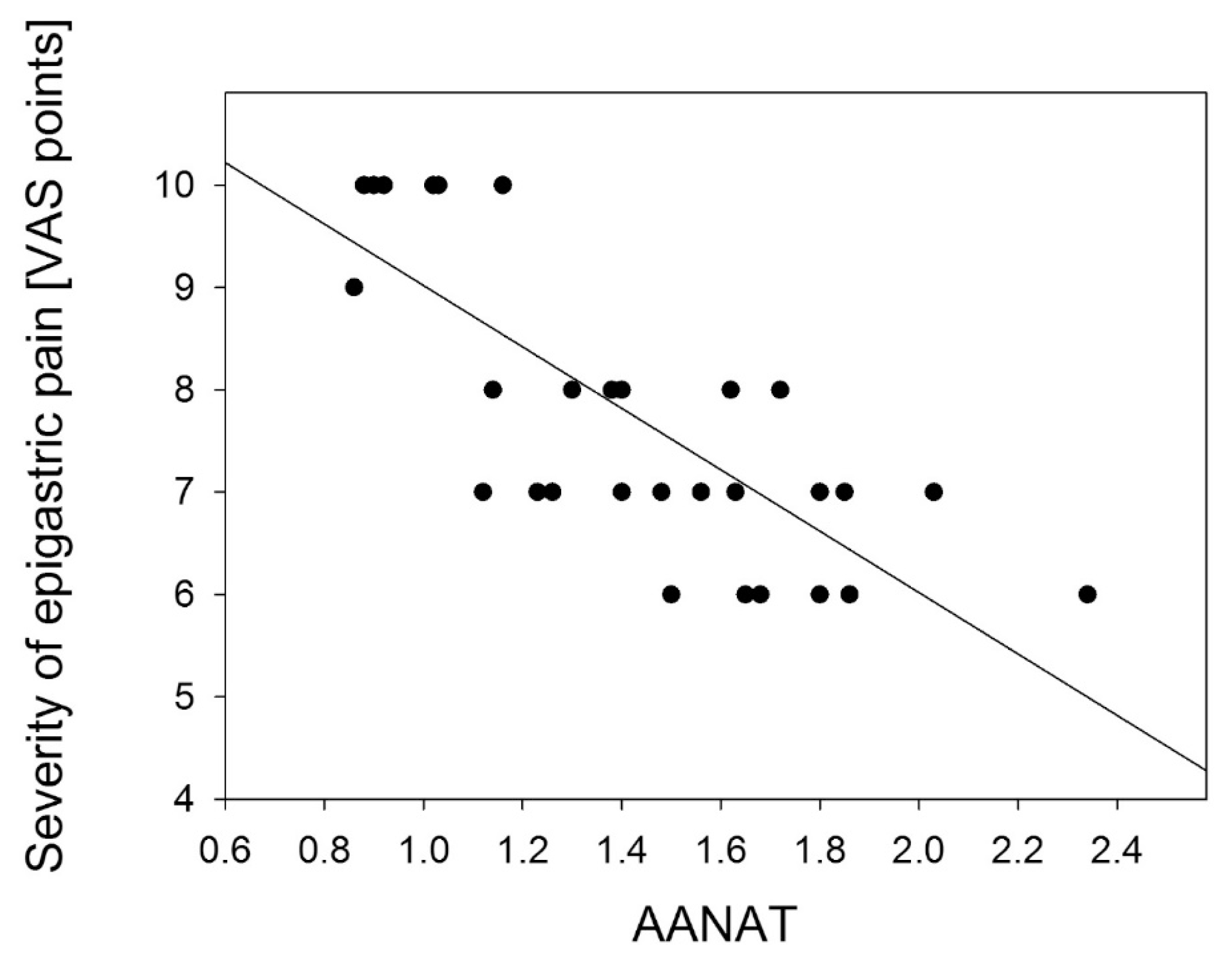
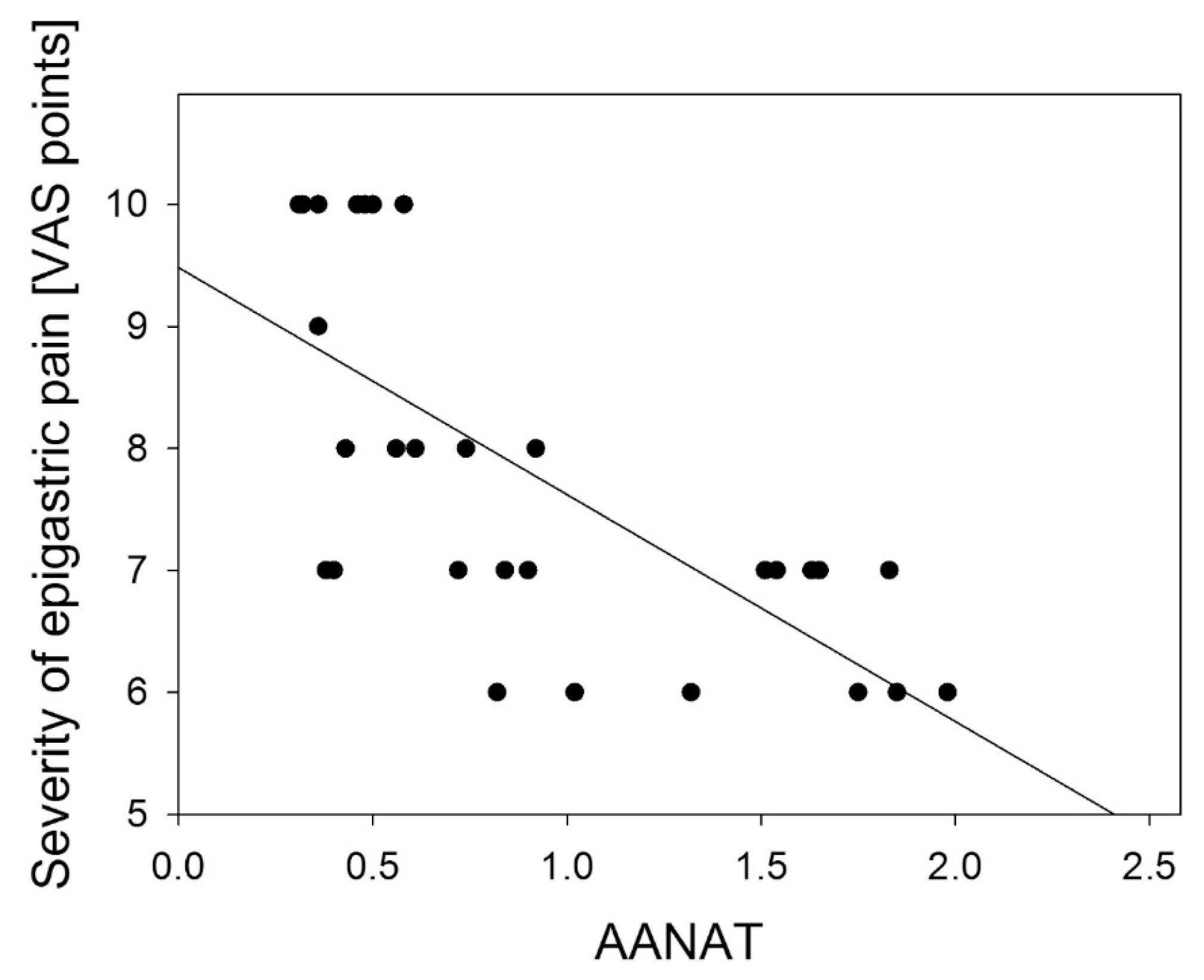
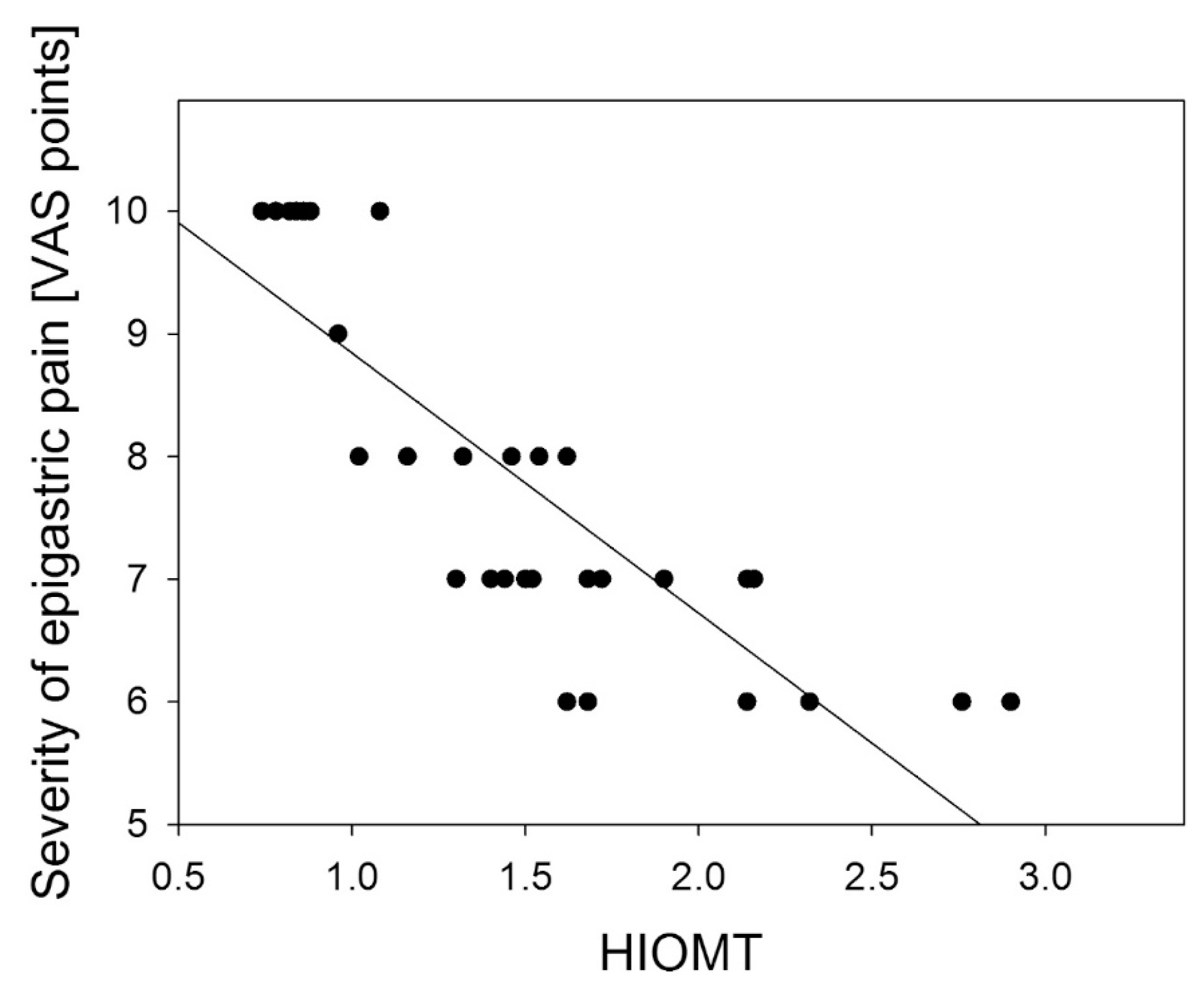
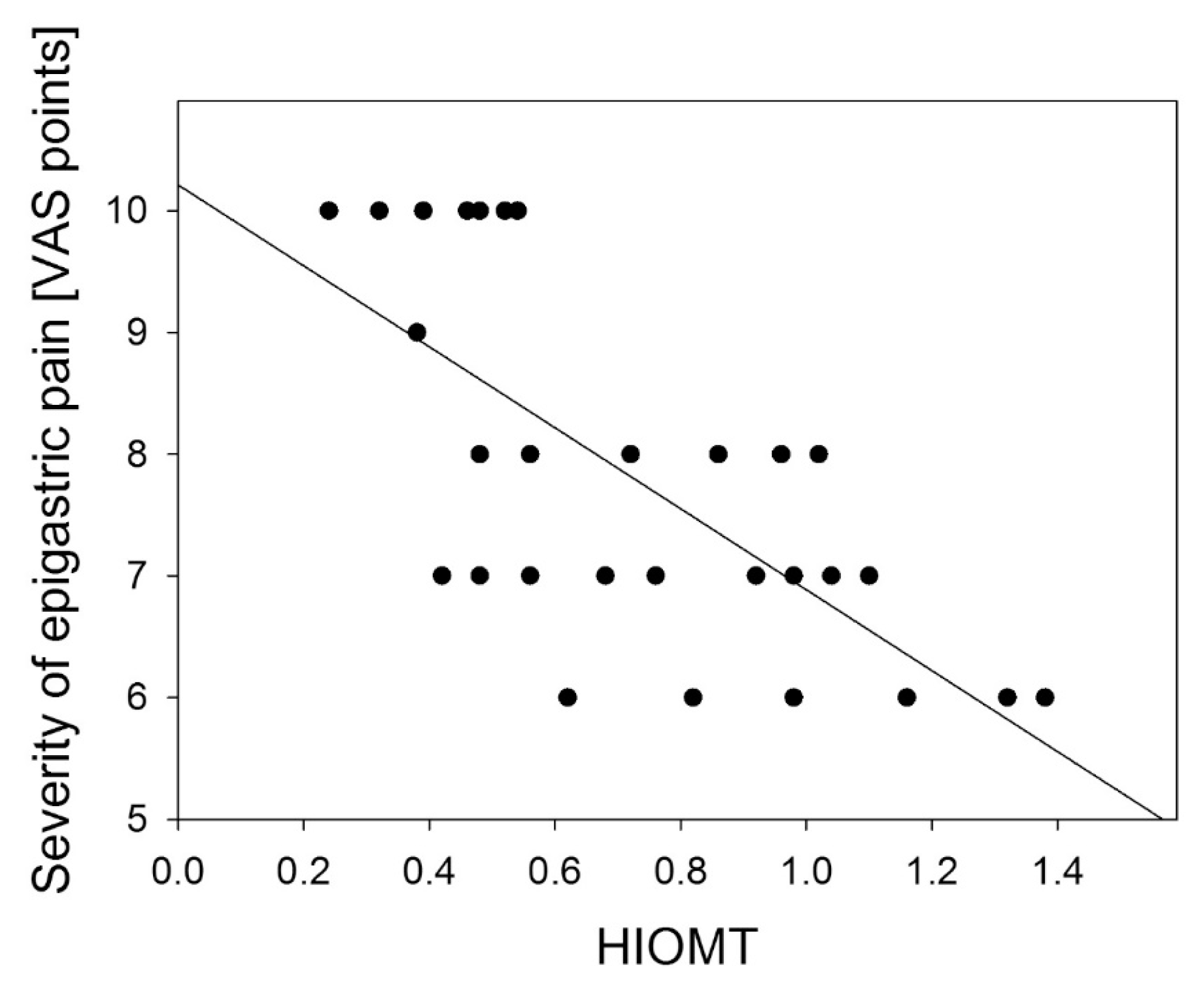
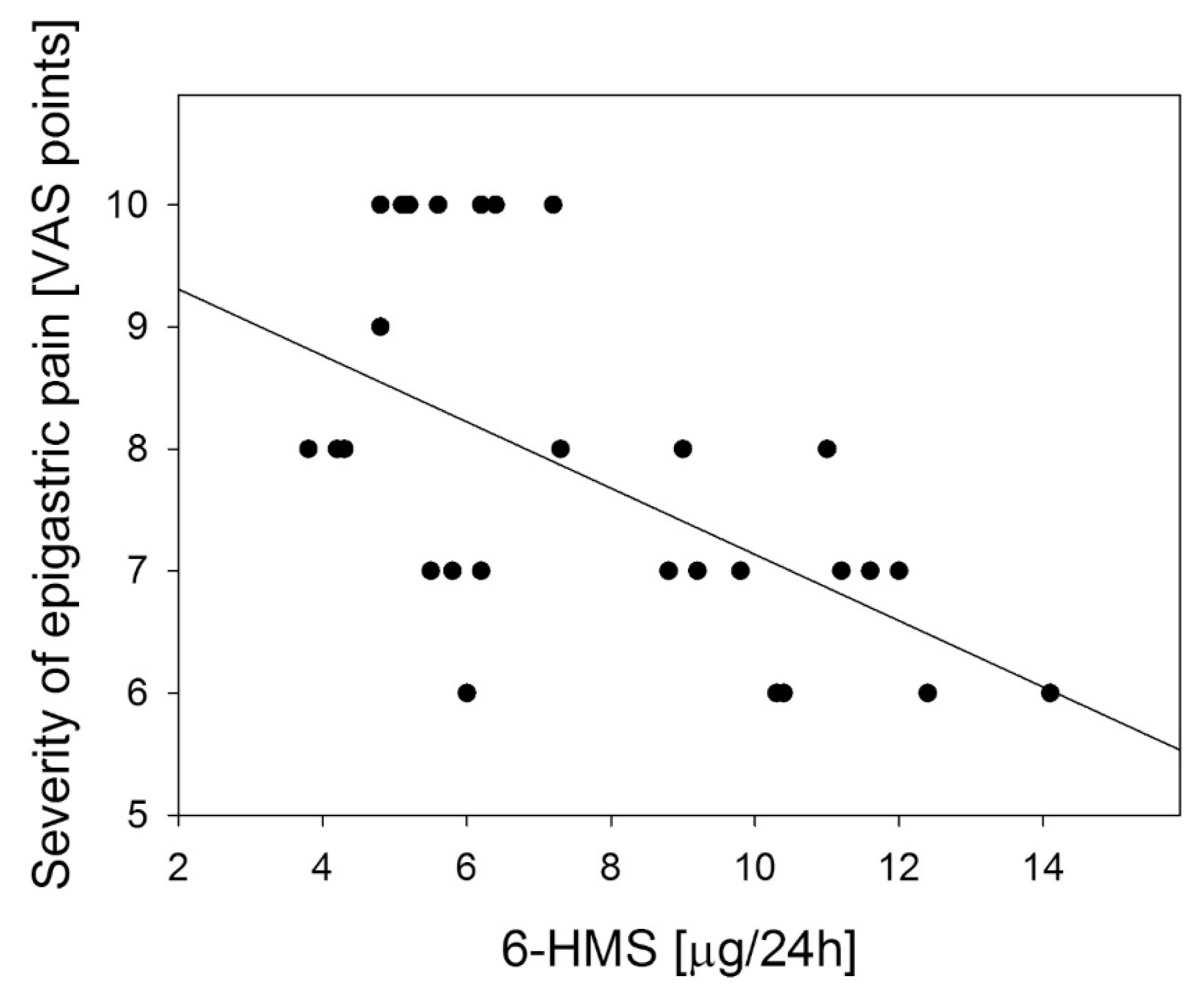

© 2013 by the authors; licensee MDPI, Basel, Switzerland This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution license ( http://creativecommons.org/licenses/by/3.0/).
Share and Cite
Chojnacki, C.; Poplawski, T.; Blasiak, J.; Chojnacki, J.; Klupinska, G. Does Melatonin Homeostasis Play a Role in Continuous Epigastric Pain Syndrome? Int. J. Mol. Sci. 2013, 14, 12550-12562. https://doi.org/10.3390/ijms140612550
Chojnacki C, Poplawski T, Blasiak J, Chojnacki J, Klupinska G. Does Melatonin Homeostasis Play a Role in Continuous Epigastric Pain Syndrome? International Journal of Molecular Sciences. 2013; 14(6):12550-12562. https://doi.org/10.3390/ijms140612550
Chicago/Turabian StyleChojnacki, Cezary, Tomasz Poplawski, Janusz Blasiak, Jan Chojnacki, and Grazyna Klupinska. 2013. "Does Melatonin Homeostasis Play a Role in Continuous Epigastric Pain Syndrome?" International Journal of Molecular Sciences 14, no. 6: 12550-12562. https://doi.org/10.3390/ijms140612550