Ethnopharmacology and Therapeutic Value of Bridelia micrantha (Hochst.) Baill. in Tropical Africa: A Comprehensive Review
Abstract
:1. Introduction
2. Research Methodology
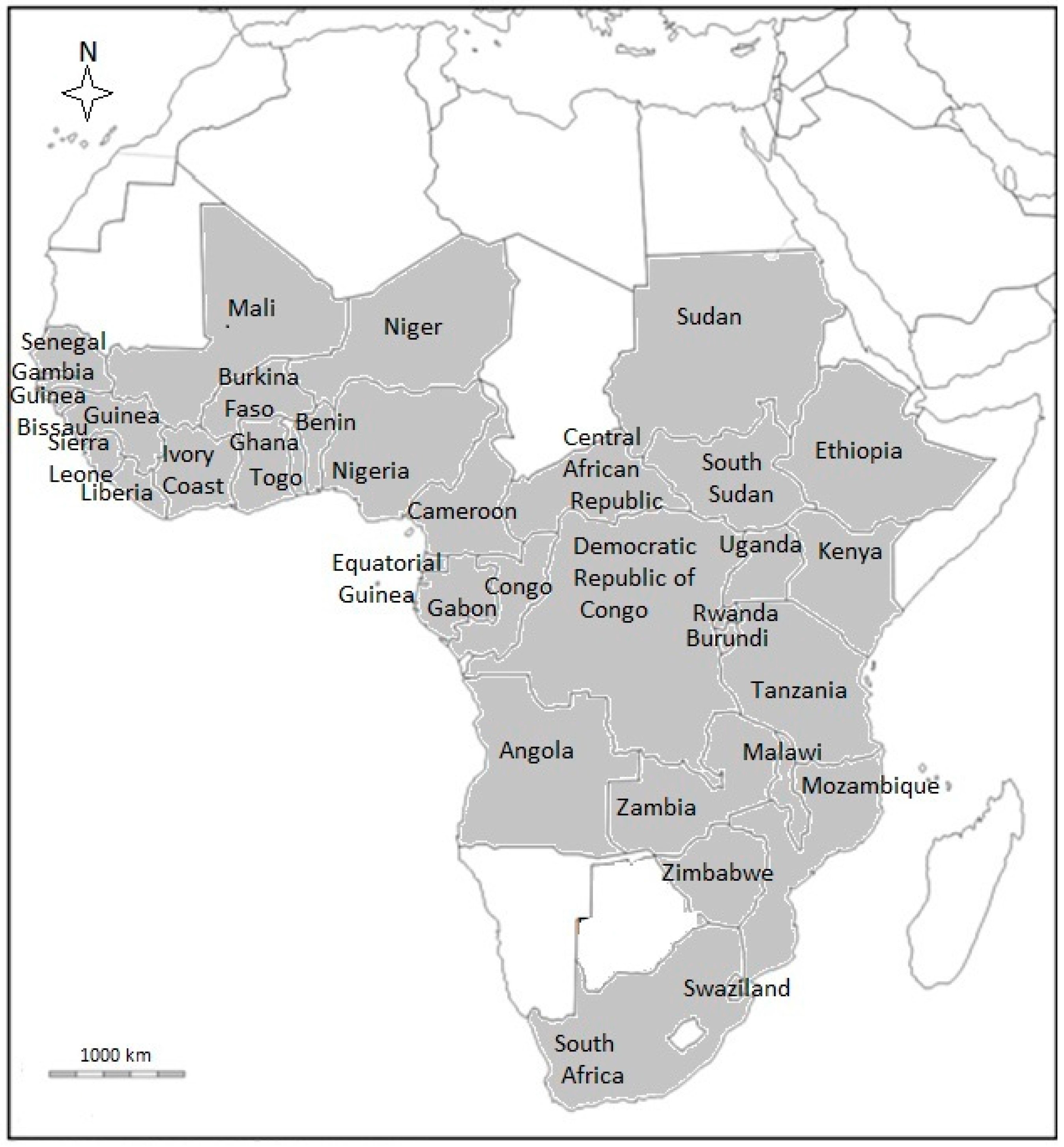
3. Occurrence, Distribution and Botanical Description
4. Ethnomedicinal Uses of B. micrantha
5. Phytochemical Constituents of B. micrantha
6. Pharmacological Properties of B. micrantha
6.1. Anthelmintic
6.2. Antibacterial
6.3. Anticonvulsant and Sedative
6.4. Antidiabetic
6.5. Antidiarrhoeal
6.6. Antifungal
6.7. Anti-Helicobacter pylori
6.8. Antimycobacterial
6.9. Antinociceptive
6.10. Antioxidant
6.11. Antiplasmodial
6.12. Antischistosomal
6.13. Antiviral
6.14. Hepatoprotective
6.15. Insecticidal
6.16. β-Lactamase Inhibitory
6.17. Toxicity and Cytotoxicity
7. Conclusions
Acknowledgments
Conflicts of Interest
References
- Bosch, C.H. Bridelia micrantha (Hochst.) Baill. In Plant Resources of Tropical Africa 7(2). Timbers 2; Lemmens, R.H.M.J., Louppe, D., Oteng-Amoako, A.A., Eds.; PROTA Foundation: Wageningen, The Netherlands, 2012; pp. 169–171. [Google Scholar]
- Schmidt, E.; Lotter, M.; McCleland, W. Trees and Shrubs of Mpumalanga and Kruger National Park; Jacana Publishers: Johannesburg, South Africa, 2002. [Google Scholar]
- Radcliffe-Smith, A. Euphorbiaceae (Part 1). In Flora of Tropical East Africa; Polhill, P.M., Ed.; A.A Balkema: Rotterdam, The Netherlands, 1987; pp. 1–407. [Google Scholar]
- Ngueyem, T.A.; Brusotti, G.; Caccialanza, G.; Finzi, P.V. The genus Bridelia: A phytochemical and ethnopharmacological review. J. Ethnopharmacol. 2009, 12, 339–349. [Google Scholar] [CrossRef] [PubMed]
- Van Wyk, B.; Gericke, N. People’s Plants: A Guide to Useful Plants of Southern Africa; Briza Publications: Pretoria, South Africa, 2000. [Google Scholar]
- Walsh, M. The use of wild and cultivated plants as famine foods on Pemba Island, Zanzibar. Études Océan Indien 2012, 42–43, 217–241. Available online: http://oceanindien.revues.org/793 (accessed on 10 July 2017). [CrossRef]
- Van Wyk, B.-E. The potential of South African plants in the development of new food and beverage products. S. Afr. J. Bot. 2011, 77, 857–868. [Google Scholar] [CrossRef]
- Maghembe, J.A.; Prins, H. Performance of multipurpose trees for agroforestry two years after planting at Makoka, Malawi. For. Ecol. Manag. 1994, 64, 171–182. [Google Scholar] [CrossRef]
- Kideghesho, J.R.; Msuya, T.S. Gender and socio-economic factors influencing domestication of indigenous medicinal plants in the West Usambara Mountains, northern Tanzania. Int. J. Biodivers. Sci. Ecosyst. Serv. Manag. 2010, 6, 3–12. [Google Scholar] [CrossRef]
- Ingram, V.; Schure, J. Review of Non Timber Forest Products (NTFPs) in Central Africa: Cameroon; Center for International Forestry Research (CIFOR): Yaounde, Cameroon, 2010. [Google Scholar]
- Meke, G.S.; Mumba, R.F.E.; Bwanali, R.J.; Williams, V.L. The trade and marketing of traditional medicines in southern and central Malawi. Int. J. Sustain. Dev. World Ecol. 2017, 24, 73–87. [Google Scholar] [CrossRef]
- Oluwalana, E.O.A.; Adekunle, M.F.; Ayeni, A.A. Sales of medicinal forest tree barks in Abeokuta, Ogun State Nigeria. Afr. Res. Rev. 2007, 1, 57–64. [Google Scholar] [CrossRef]
- Williams, V.L.; Balkwill, K.; Witkowski, E.T.F. A lexicon of plants traded in the Witwatersrand umuthi shops, South Africa. Bothalia 2001, 31, 71–98. [Google Scholar] [CrossRef]
- Chekole, G.; Asfaw, Z.; Kelbessa, E. Ethnobotanical study of medicinal plants in the environs of Tara-gedam and Amba remnant forests of Libo Kemkem District, northwest Ethiopia. J. Ethnobiol. Ethnomed. 2015, 11, 4. [Google Scholar] [CrossRef] [PubMed]
- Hamill, F.A.; Apio, S.; Mubiru, N.K.; Bukenya-Ziraba, R.; Mosango, M.; Maganyi, O.W.; Soejarto, D.D. Traditional herbal drugs of southern Uganda, II: Literature analysis and antimicrobial assays. J. Ethnopharmacol. 2003, 84, 57–78. [Google Scholar] [CrossRef]
- Mbayo, K.M.; Kalonda, M.E.; Tshisand, T.P.; Kisimba, K.E.; Mulamba, M.; Richard, M.K.; Sangwa, K.G.; Mbayo, K.G.; Maseho, M.F.; Bakari, S.; et al. Contribution to ethnobotanical knowledge of some Euphorbiaceae used in traditional medicine in Lubumbashi and its surroundings (DRC). J. Adv. Bot. Zool. 2016, 4, 1–16. [Google Scholar]
- Arnold, H.-J.; Gulumian, M. Pharmacopoeia of traditional medicine in Venda. J. Ethnopharmacol. 1984, 12, 35–74. [Google Scholar] [CrossRef]
- Gelfand, M.; Mavi, S.; Drummond, R.B.; Ndemera, B. The Traditional Medical Practitioners in Zimbabwe: His Principles of Practice and Pharmacopoeia; Mambo Press: Gweru, Zimbabwe, 1985. [Google Scholar]
- Steenkamp, V.; Fernandes, A.C.; van Rensburg, C.E. Antibacterial activity of Venda medicinal plants. Fitoterapia 2007, 78, 561–564. [Google Scholar] [CrossRef] [PubMed]
- Moshi, M.J.; Otieno, D.F.; Weisheit, A. Ethnomedicine of the Kagera region, north western Tanzania. Part 3: Plants used in traditional medicine in Kikuku village, Muleba district. J. Ethnobiol. Ethnomed. 2012, 8, 14. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Betti, J.L. An ethnobotanical study of medicinal plants among the Baka pygmies in the Dja Biosphere reserve, Cameroon. Afr. Study Monogr. 2004, 25, 1–27. [Google Scholar]
- Latham, P. Useful Plants of Bas-Congo Province, Democratic Republic of Congo; Department of International Development (DFID): London, UK, 2004.
- Mabogo, E.E.N. The Ethnobotany of the Vhavenda; MSc dissertation, University of Pretoria: Pretoria, South Africa, 1990. [Google Scholar]
- Venter, F.; Venter, J.-A. Making the Most of Indigenous Trees; Briza Publications: Pretoria, South Africa, 1996. [Google Scholar]
- Lin, J.; Puckree, T.; Mvelase, T.P. Anti-diarrheal evaluation of some medicinal plants used by Zulu traditional healers. J. Ethnopharmacol. 2002, 79, 53–56. [Google Scholar] [CrossRef]
- Munayi, R.R. Phytochemical Investigation of Bridelia micrantha and Tabernaemontana ventricosa for Cytotoxic Principles against Drug Sensitive Leukemia Cell Lines. Master’s Thesis, University of Nairobi, Nairobi, Kenya, 2016. [Google Scholar]
- Ochwang’I, D.O.; Kimwele, C.N.; Oduma, J.A.; Gathumbi, P.K.; Mbaria, J.M.; Kiama, S.G. Medicinal plants used in treatment and management of cancer in Kakamega County, Kenya. J. Ethnopharmacol. 2014, 151, 1040–1055. [Google Scholar] [CrossRef] [PubMed]
- Focho, D.A.; Ndam, W.T.; Fonge, B.A. Medicinal plants of Aguambu—Bamumbu in the Lebialem highlands, southwest province of Cameroon. Afr. J. Pharm. Pharmacol. 2009, 3, 1–13. [Google Scholar]
- Jiofack, T.; Fokunang, C.; Guedje, N.; Kemeuze, V.; Fongnzossie, E.; Nkongmeneck, B.A.; Mapongmetsem, P.M.; Tsabang, N. Ethnobotanical uses of medicinal plants of two ethnoecological regions of Cameroon. Int. J. Med. Med. Sci. 2010, 2, 60–79. [Google Scholar]
- Madge, C. Therapeutic landscapes of the Jola, The Gambia, West Africa. Health Place 1998, 4, 293–311. [Google Scholar] [CrossRef]
- Koné, M.; Atindehou, K.K. Ethnobotanical inventory of medicinal plants used in traditional veterinary medicine in Northern Côte d’Ivoire (West Africa). S. Afr. J. Bot. 2008, 74, 76–84. [Google Scholar] [CrossRef]
- Gangoué-Piéboji, J.; Eze, N.; Djintchui, A.N.; Ngameni, B.; Tsabang, N.; Pegnyemb, D.E.; Biyiti, L.; Ngassam, P.; Koulla-Shiro, S.; Galleni, M. The in vitro antimicrobial activity of some traditionally used medicinal plants against beta-lactam-resistant bacteria. J. Infect. Dev. Ctries. 2009, 3, 671–680. [Google Scholar] [CrossRef] [PubMed]
- Idu, M.; Erhabor, J.O.; Ovuakporie-Uvo, O. Ethnomedicinal plants used by the Idoma people-Benue State, Nigeria. Am. J. Ethnomed. 2014, 1, 72–88. [Google Scholar]
- Abo, K.A.; Fred-Jaiyesimi, A.A.; Jaiyesimi, A.E.A. Ethnobotanical studies of medicinal plants used in the management of diabetes mellitus in South Western Nigeria. J. Ethnopharmacol. 2008, 115, 67–71. [Google Scholar] [CrossRef] [PubMed]
- Gbolade, A.A. Inventory of antidiabetic plants in selected districts of Lagos State, Nigeria. J. Ethnopharmacol. 2009, 121, 135–139. [Google Scholar] [CrossRef] [PubMed]
- Mabeku, L.B.K.; Roger, K.J.; Louis, O.E.J. Screening of some plants used in the Cameroonian folk medicine for the treatment of infectious diseases. Int. J. Biol. 2011, 3, 13–21. [Google Scholar]
- Diallo, A.; Traore, M.S.; Keita, S.M.; Balde, M.A.; Keita, A.; Camara, M.; van Miert, S.; Pieters, L.; Balde, A.M. Management of diabetes in Guinean traditional medicine: An ethnobotanical investigation in the coastal lowlands. J. Ethnopharmacol. 2012, 144, 353–361. [Google Scholar] [CrossRef] [PubMed]
- Kokwaro, J.O. Medicinal Plants of East Africa; Kenya Literature Bureau: Nairobi, Kenya, 1993. [Google Scholar]
- Bessong, P.O.; Obi, C.L.; Igumbor, E.; Andreola, M.-L.; Litvak, S. In vitro activity of three selected South African medicinal plants against human immunodeficiency virus type 1 reverse transcriptase. Afr. J. Biotechnol. 2004, 3, 555–559. [Google Scholar]
- Bessong, P.O.; Rojas, L.B.; Obi, L.C.; Tshisikawe, P.M.I.; Eunice, O. Further screening of Venda medicinal plants for activity against HIV type 1 reverse transcriptase and Integrase. Afr. J. Biotechnol. 2006, 5, 526–528. [Google Scholar]
- Ita, P.B.; Offiong, E.E. Medicinal plants used in traditional medicine by rural communities in Cross River State, Nigeria. J. Health Med. Nurs. 2013, 1, 23–29. [Google Scholar]
- Hallam, G.M. Medicinal Uses of Flowering Plants in the Gambia; Department of Forestry: Yundum, Gambia, 1979.
- Nzigidahera, B. Assessment of Socio-Cultural, Economic Characteristics and Livelihood of Riparian Population of the Kibira National Park (Rukoma-Mutana Locality). 2006. Available online: https://www.google.co.za/url?sa=t&rct=j&q=&esrc=s&source=web&cd=1&cad=rja&uact=8&ved=0ahUKEwjTsbeE9JHWAhWFKMAKHYmCApgQFgglMAA&url=http%3A%2F%2Fbi.chm-cbd.net%2Frestored%2Fbiodiversity%2Fbiodiversite-du-burundi%2Fetudes-et-publications%2Ffol494566%2FEtude_socio_Kibira_Anglais1.pdf%2Fdownload%2Fen%2F1%2FEtude_socio_Kibira_Anglais1.pdf&usg=AFQjCNFdr0Q_BDN7ipaIsJG0SMCubGIpJg (accessed on 10 June 2017).
- Hutchings, A.; Scott, A.H.; Lewis, G.; Cunningham, A. Zulu Medicinal Plants. An Inventory; University of Natal Press: Scottsville, South Africa, 1996. [Google Scholar]
- Watt, J.M.; Breyer-Brandwijk, M.G. The Medicinal and Poisonous Plants of Southern and Eastern Africa; E. and S. Livingstone: London, UK, 1962. [Google Scholar]
- Shelembe, B.G. Phytochemical and Elemental Studies of Two Indigenous Medicinal Plants of South Africa, Bridelia micrantha and Sideroxylon inerme. Master’s Thesis, University of KwaZulu Natal, Durban, South Africa, 2014. [Google Scholar]
- Catarino, L.; Havik, P.J.; Romeiras, M.M. Medicinal plants of Guinea-Bissau: Therapeutic applications, ethnic diversity and knowledge transfer. J. Ethnopharmacol. 2016, 183, 71–94. [Google Scholar] [CrossRef] [PubMed]
- Frazão-Moreira, A. The symbolic efficacy of medicinal plants: Practices, knowledge, and religious beliefs amongst the Nalu healers of Guinea-Bissau. J. Ethnobiol. Ethnomed. 2016, 12, 24. [Google Scholar] [CrossRef] [PubMed]
- Ariwaodo, J.O.; Chukwuma, E.C.; Adeniji, K.A. Some medicinal plant species of Asamagbe stream bank vegetation, Forestry Research Institute of Nigeria, Ibadan. Ethnobot. Res. Appl. 2012, 10, 541–549. [Google Scholar]
- Chukwuma, E.C.; Soladoye, M.O.; Feyisola, R.T. Traditional medicine and the future of medicinal Plants in Nigeria. J. Med. Plants 2015, 3, 23–29. [Google Scholar]
- Amri, E.; Kisangau, D.P. Ethnomedicinal study of plants used in villages around Kimboza forest reserve in Morogoro, Tanzania. J. Ethnobiol. Ethnomed. 2012, 8, 1. [Google Scholar] [CrossRef] [PubMed]
- Njoroge, G.N.; Bussmann, R.W. Ethnotherapeutic management of sexually transmitted diseases (STDs) and reproductive health conditions in central province of Kenya. Indian J. Tradit. Knowl. 2009, 8, 255–261. [Google Scholar]
- Verger, P.F. Ewe: The Use of Plants in Yoruba Society; Editoria Schwarcz: Sao Paulo, Brazil, 1995. [Google Scholar]
- Palmer, E.; Pitman, P. Trees of Southern Africa Covering all Known Indigenous Species in the Republic of South Africa, South West Africa, Botswana, Lesotho and Swaziland; A.A. Balkema: Cape Town, South Africa, 1972. [Google Scholar]
- Nole, T.; Lionel, T.D.W.; Cedrix, T.F.S.; Gabriel, A.A. Ethnomedical and ethnopharmacological study of plants used for potential treatments of diabetes and arterial hypertension by indigenous people in three phytogeographic regions of Cameroon. Diabetes Case Rep. 2016, 1, 110. [Google Scholar] [CrossRef]
- Nguta, J.M.; Mbaria, J.M.; Gakuya, D.W.; Gathumbi, P.K.; Kiama, S.G. Traditional antimalarial phytotherapy remedies used by the South Coast community, Kenya. J. Ethnopharmacol. 2010, 131, 256–267. [Google Scholar] [CrossRef] [PubMed]
- Traore, M.S.; Baldé, M.A.; Diallo, M.S.T.; Baldé, E.S.; Diané, S.; Camara, A.; Diallo, A.; Balde, A.; Keïta, A.; Keita, S.M.; et al. Ethnobotanical survey on medicinal plants used by Guinean traditional healers in the treatment of malaria. J. Ethnopharmacol. 2013, 150, 1145–1153. [Google Scholar] [CrossRef] [PubMed]
- Malan, D.F.; Neuba, D.F.R.; Kouakou, K.L. Medicinal plants and traditional healing practices in ehotile people, around the aby lagoon (eastern littoral of Côte d’Ivoire). J. Ethnobiol. Ethnomed. 2015, 11, 21. [Google Scholar] [CrossRef] [PubMed]
- Nondo, R.S.O.; Zofou, D.; Moshi, M.J.; Erasto, P.; Wanji, S.; Ngemenya, M.N.; Titanji, V.P.K.; Kidukuli, A.W.; Masimba, P.J. Ethnobotanical survey and in vitro antiplasmodial activity of medicinal plants used to treat malaria in Kagera and Lindi regions, Tanzania. J. Med. Plants Res. 2015, 9, 179–192. [Google Scholar]
- Jeruto, P.; Mutai, C.; Ouma, G.; Lukhoba, C.; Nyamaka, R.L.; Manani, S.D. Ethnobotanical survey and propagation of some endangered medicinal plants from south Nandi district of Kenya. J. Anim. Plant Sci. 2010, 8, 1016–1043. [Google Scholar]
- Ssegawa, P.; Kasenene, J.M. Medicinal plant diversity and uses in the Sango Bay area, southern Uganda. J. Ethnopharmacol. 2007, 113, 521–540. [Google Scholar] [CrossRef] [PubMed]
- Okello, S.V.; Nyunja, R.O.; Netondo, G.W.; Onyango, J.C. Ethnobotanical study of medicinal plants used by Sabaots of Mt. Elgon Kenya. Afr. J. Tradit. Complement. Altern. Med. 2010, 7, 1–10. [Google Scholar] [CrossRef]
- Jeruto, P.; Too, E.; Mwamburi, L.A.; Amuka, O. An inventory of medicinal plants used to treat gynaecological obstetric-urino-genital disorders in South Nandi Sub County in Kenya. J. Nat. Sci. Res. 2015, 5, 136–152. [Google Scholar]
- Zenebe, G.; Zerihun, M.; Solomon, Z. An ethnobotanical study of medicinal plants in Asgede Tsimbila district, northwestern Tigray, northern Ethiopia. Ethnobot. Res. Appl. 2012, 10, 305–320. [Google Scholar] [CrossRef]
- Lebbie, A.R.; Guries, R.P. Ethnobotanical value and conservation of sacred groves of the Kpaa Mende in Sierra Leone. Econ. Bot. 1995, 49, 297–308. [Google Scholar] [CrossRef]
- Chifundera, K. Livestock diseases and the traditional medicine in the Bushi area, Kivu province, Democratic Republic of Congo. Afr. Study Monogr. 1998, 19, 13–33. [Google Scholar]
- Wasswa, P.; Olila, D. The in vitro ascaricidal activity of selected indigenous medicinal plants used in ethno veterinary practices in Uganda. Afr. J. Tradit. Complement. Altern. Med. 2006, 3, 94–103. [Google Scholar]
- Kabore, A.; Traore, A.; Pare, S.; Sawadogo, B.C.; Kalkoumdo, G.; Tamboura, H.H.; Belem, A.M.G. Ethno-medicinal study of plants used in ectoparasites infections of ruminant livestock in Sahelian region of Burkina Faso, West Africa. J. Nat. Prod. Plant Resour. 2012, 2, 611–616. [Google Scholar]
- Pegel, K.H.; Rogers, C.B. Constituents of Bridelia micrantha. Phytochemistry 1968, 7, 655–656. [Google Scholar] [CrossRef]
- Okeleye, B.I.; Bessong, P.O.; Ndip, R.N. Preliminary phytochemical screening and in vitro anti-Helicobacter pylori activity of extracts of the stem bark of Bridelia micrantha (Hochst.) Baill. Euphorbiaceae). Molecules 2011, 16, 6193–6205. [Google Scholar] [CrossRef] [PubMed]
- Waiganjo, N.; Ochanda, H.; Yole, D. Phytochemical analysis of the selected five plant extracts. Chem. Mater. Res. 2013, 3, 12–17. [Google Scholar]
- Akinyeye, R.O.; Olatunya, A.M. Phytochemical screening and mineral composition of the bark of some medicinal trees in Ondo State, Nigeria. Med. Aromat. Plant Res. J. 2014, 2, 44–49. [Google Scholar]
- Ejikeme, C.M.; Ezeonu, C.S.; Eboatu, A.N. Determination of physical and phytochemical constituents of some tropical timbers indigenous to Niger Delta area of Nigeria. Eur. Sci. J. 2014, 10, 247–270. [Google Scholar]
- Douglas, K.; Gitonga, A. Antimicrobial activity of Bridelia micrantha and Grewia plagiophylla leaf extracts. Br. J. Pharm. Res. 2016, 12, 1–7. [Google Scholar] [CrossRef]
- Mburu, C.; Kareru, P.G.; Kipyegon, C.; Madivoli, E.S.; Maina, E.G.; Kairigo, P.K.; Kimani, P.K.; Marikah, D.M. Phytochemical Screening of Crude Extracts of Bridelia micrantha. Eur. J. Med. Plants 2016, 16, 1–7. [Google Scholar] [CrossRef]
- Ochwang’I, D.O.; Kimwele, C.N.; Oduma, J.A.; Gathumbi, P.K.; Kiama, S.G.; Efferth, T. Phytochemical screening of medicinal plants of the Kakamega county, Kenya commonly used against cancer. Med. Aromat. Plants 2016, 5, 277. [Google Scholar]
- Shelembe, B.G.; Moodley, R.; Jonnalagadda, S.B. Secondary metabolites isolated from two medicinal plant species, Bridelia micrantha and Sideroxylon inerme and their antioxidant activities. Acta Pol. Pharm. Drug Res. 2016, 73, 1249–1257. [Google Scholar]
- Green, E.; Obi, L.C.; Samie, A.; Bessong, P.O.; Ndip, R.N. Characterization of n-hexane subfraction of Bridelia micrantha (Berth) and its antimycobacterium activity. BMC Complement. Altern. Med. 2011, 11, 28. [Google Scholar] [CrossRef] [PubMed]
- Waterman, C.; Smith, R.A.; Pontiggia, L.; DerMarderosian, A. Anthelmintic screening of sub-Saharan African plants used in traditional medicine. J. Ethnopharmacol. 2010, 127, 755–759. [Google Scholar] [CrossRef] [PubMed]
- Samie, A.; Obi, C.L.; Bessong, P.O.; Namrita, L. Activity profiles of fourteen selected medicinal plants from rural Venda communities in South Africa against fifteen clinical bacterial species. Afr. J. Biotechnol. 2005, 4, 1443–1451. [Google Scholar]
- Adefuye, A.O.; Samie, A.; Ndip, R.N. In Vitro evaluation of the antimicrobial activity of extracts of Bridelia micrantha on selected bacterial pathogens. J. Med. Plants Res. 2011, 5, 5116–5122. [Google Scholar]
- Adefuye, A.; Ndip, R.N. Phytochemical analysis and antibacterial evaluation of the ethyl acetate extract of the stem bark of Bridelia micrantha. Pharmacogn. Mag. 2013, 9, 45–50. [Google Scholar] [PubMed]
- Traoré, M.S.; Baldé, M.A.; Camara, A.; Baldé, E.S.; Diané, S.; Diallo, M.S.T.; Keita, A.; Cos, P.; Maes, L.; Pieters, L.; Baldé, A.M. The malaria co-infection challenge: An investigation into the antimicrobial activity of selected Guinean medicinal plants. J. Ethnopharmacol. 2015, 174, 576–581. [Google Scholar] [CrossRef] [PubMed]
- Bum, E.N.; Ngah, E.; Mune, R.M.N.; Minkoulou, D.M.Z.; Talla, E.; Moto, F.C.O.; Ngoupaye, G.T.; Taiwe, G.S.; Rakotonirina, A.; Rakotonirina, S.V. Decoctions of Bridelia micrantha and Croton macrostachyus may have anticonvulsant and sedative effects. Epilepsy Behav. 2012, 24, 319–323. [Google Scholar]
- Adika, O.A.; Madubunyi, I.I.; Asuzu, I.U. Antidiabetic and antioxidant effects of the methanol extract of Bridelia micrantha (Hochst.) Baill. (Euphorbiaceae) leaves on alloxan-induced diabetic Albino mice. Comp. Clin. Pathol. 2012, 21, 945–951. [Google Scholar] [CrossRef]
- Green, E.; Samie, A.; Obi, C.L.; Bessong, P.O.; Ndip, R.N. Inhibitory properties of selected South African medicinal plants against Mycobacterium tuberculosis. J. Ethnopharmacol. 2010, 130, 151–157. [Google Scholar] [CrossRef] [PubMed]
- Onoja, S.; Ukwueze, C.; Ezeja, M.; Udeh, N. Antinociceptive and antioxidant effects of hydromethanolic extract of Bridelia micrantha stem bark. J. Exp. Integr. Med. 2014, 4, 273. [Google Scholar] [CrossRef]
- Nwaehujor, C.O.; Udeh, N.E. Screening of ethyl acetate extract of Bridelia micrantha for hepatoprotective and antioxidant activities on Wistar rats. Asian Pac. J. Trop. Med. 2011, 4, 796–798. [Google Scholar] [CrossRef]
- Nwaehujor, C.O.; Igile, G.O.; Akande, M.G. In vitro antioxidant potentials of some herbal plants from southern Nigeria. J. Med. Sci. 2013, 13, 56–61. [Google Scholar] [CrossRef]
- Clarkson, C.; Maharaj, V.J.; Crouch, N.R.; Grace, O.M.; Pillay, P.; Matsabisa, M.G.; Bhagwandin, N.; Smith, P.J.; Folb, P.I. In vitro antiplasmodial activity of medicinal plants native to or naturalised in South Africa. J. Ethnopharmacol. 2004, 92, 177–191. [Google Scholar] [CrossRef] [PubMed]
- Ajaiyeoba, E.; Ashidi, J.; Abiodun, O.; Okpako, L.; Ogbole, O.; Akinboye, D.; Falade, C.; Bolaji, O.; Gbotosho, G.; Falade, M.; et al. Antimalarial Ethnobotany: In vitro antiplasmodial activity of seven plants identified in the Nigerian Middle Belt. Pharm. Biol. 2005, 42, 588–591. [Google Scholar] [CrossRef]
- Waiganjo, N.; Yole, D.; Ochanda, H. Anti-schistosomal activity of five plant extracts on Swiss white mice infected with Schistosoma mansoni. J. Pharm. Biol. Sci. 2014, 9, 49–53. [Google Scholar]
- Adesina, J.M.; Ileke, K.D.; Yallappa, R.; Ofuya, T.I. Insecticidal evaluation of Bridelia micrantha and Dalbergia lactea aqueous extracts for the control of Podagrica uniforma (Jacoby) and Nisotra dilecta (Jacoby) (Coleoptera: Chysomelidae) infestation on okra. Agrivita J. Agric. Sci. 2016, 38, 269–274. [Google Scholar] [CrossRef]
- Gangoué-Piéboji, J.; Baurin, S.; Frère, J.M.; Ngassam, P.; Ngameni, B.; Azebaze, A.; Pegnyemb, D.E.; Watchueng, J.; Goffin, C.; Galleni, M. Screening of some medicinal plants from Cameroon for ß-Lactamase inhibitory activity. Phytother. Res. 2007, 21, 284–287. [Google Scholar] [CrossRef] [PubMed]
- Ajaiyeoba, E.O.; Abiodun, O.; Falade, M.O.; Ogbole, N.O.; Ashidi, J.S.; Happi, C.T.; Akinboye, D.O. In vitro cytotoxicity studies of 20 plants used in Nigerian antimalarial ethnomedicine. Phytomedicine 2006, 13, 295–298. [Google Scholar] [CrossRef] [PubMed]
- Steenkamp, V.; Mokoele, T.L.; van Rensburg, C.E.J. Toxicity testing of two medicinal plants, Bridelia micrantha and Antidesma venosum. Open Toxicol. J. 2009, 3, 35–38. [Google Scholar] [CrossRef]
- Moshi, M.J.; Innocent, E.; Magadula, J.J.; Otieno, D.J.; Weisheit, A.; Mbabazi, P.K.; Nondo, R.S.O. Brine shrimp toxicity of some plants used as traditional medicines in Kagera Region, north western Tanzania. Tanzan. J. Health Res. 2010, 12, 63–70. [Google Scholar] [CrossRef] [PubMed]
- Omosa, L.K.; Midiwo, J.O.; Masila, V.M.; Gisacho, B.M.; Munayi, R.; Francisca-Kamakama; Chemutai, K.P.; Elhaboob, G.; Saeed, M.E.M.; Hamdoun, S.; et al. Cytotoxicity of 91 Kenyan indigenous medicinal plants towards human CCRF-CEM leukemia cells. J. Ethnopharmacol. 2016, 179, 177–196. [Google Scholar] [CrossRef] [PubMed]
- Osebe, T.; Mbaria, J.; Yole, D.; Odongo, D.; Nderitu, J.; Ochanda, H. Bioactivity and toxicity of Bridelia micrantha, Chenopodium ambrosoides and Ocimum americanum plant extracts. Int. J. Basic Clin. Pharmacol. 2017, 6, 5–11. [Google Scholar] [CrossRef]
- Ndhlala, A.R.; Mupure, C.; Chitindingu, K.; Benhura, M.A.; Muchuweti, M. Antioxidant potentials and degrees of polymerization of six wild fruits. Sci. Res. Essay 2006, 1, 87–92. [Google Scholar]
- Verdcourt, B.; Trump, E.C. Common Poisonous Plants of East Africa; Collins: London, UK, 1969. [Google Scholar]

| Use | Plant Parts Used | Country Practiced | References |
|---|---|---|---|
| Abdominal pain | Bark, leaf and root decoction taken orally | DRC, Uganda | [15,16] |
| Abortifacient | Bark decoction taken orally | South Africa, Zimbabwe | [5,17,18,19] |
| Amenorrea | Root decoction taken orally | Tanzania | [20] |
| Amoebic dysentery | Bark decoction taken orally | Cameroon | [21] |
| Anaemia | Bark, leaf or root decoction taken orally | DRC | [16,22] |
| Anaesthetic | Root decoction taken orally mixed with roots of Vangueria infausta Burch. (Rubiaceae) and Dichrostachys cinerea (L.) Wight & Arn. (Fabaceae) | South Africa | [2] |
| Burns | Bark decoction applied on affected body part | South Africa | [2,23,24,25] |
| Cancer | Bark decoction taken orally | Kenya | [26] |
| Cervical, breast, skin colorectal cancer | Leaves, roots and stem bark taken orally | Kenya | [27] |
| Chest complaints | Bark decoction taken orally mixed with Pittosporum viridiflorum Sims (Pittosporaceae) | Cameroon | [28] |
| Conjunctivitis | Bark, leaf or root decoction applied to eyes | Cameroon, DRC | [16,29] |
| Constipation | Bark, leaf or root decoction taken orally | DRC, Gambia, Ivory Coast | [16,30,31] |
| Cough | Bark, leaf or root decoction taken orally | Cameroon, DRC, Zimbabwe | [16,18,21,22,32] |
| Cough | Bark decoction taken orally mixed with P. viridiflorum | Cameroon | [28] |
| Cough | Bark mixed with Capsicum frutescens L. (Solanaceae) | Nigeria | [33] |
| Dermatitis | Bark, leaf or root decoction applied to affected body part | Cameroon | [29] |
| Diabetes mellitus | Bark decoction taken orally | Cameroon, Guinea, Nigeria | [34,35,36,37] |
| Diarrhoea | Bark, leaf or root decoction taken orally | Cameroon, DRC, Kenya, Nigeria, South Africa, Tanzania | [2,9,16,22,25,32,36,38,39,40,41] |
| Dysentery | Bark, leaf or root decoction taken orally | Burundi, Cameroon, DRC, Gambia | [16,36,42,43] |
| Dysentery | Bark taken orally mixed with Antrocaryon klaineanum Pierre (Anacardiaceae) and Treculia africana Decne. ex Trécul (Moraceae) | Nigeria | [33] |
| Dysmenorrhea | Root decoction taken orally | Tanzania | [20] |
| Emetic | Bark infusion taken orally | South Africa | [44] |
| Epigastric pain | Root decoction taken orally | Tanzania | [45] |
| Eye diseases | Bark decoction applied to the eyes | Cameroon | [32] |
| Fever | Bark, leaf or root decoction taken orally | DRC, South Africa | [16,23] |
| Gastric ulcers | Bark, leaf or root decoction taken orally | Cameroon, DRC, South Africa | [16,32,46] |
| Gastro-Intestinal ailments | Bark decoction taken orally | South Africa | [25] |
| Guinea worm | Leaf decoction taken orally | Ghana | [34] |
| Haemorrhoids | Bark, leaf or root decoction taken orally | DRC, Guinea-Bissau | [16,22,47,48] |
| Headache | Bark, leaf or root decoction sometimes with oil or butter rubbed into scalp | DRC, Nigeria, South Africa, Tanzania | [9,16,23,45,49,50] |
| Hernia | Leaf or bark decoction taken orally | Tanzania | [51] |
| HIV/AIDs | Bark decoction taken orally | Kenya | [52] |
| Induce labour pains | Bark decoction taken orally | Nigeria | [53] |
| Infertility | Bark decoction taken orally | Cameroon | [36] |
| Infertility | Root decoction taken orally mixed with roots of P. africanum Sond. and Ochna spp. (Ochnaceae) | South Africa | [54] |
| Insomnia | Bark decoction taken orally | Cameroon | [55] |
| Malaria | Bark, leaf or root decoction taken orally | Guinea, Ivory Coast, Kenya, South Africa, Tanzania | [20,23,56,57,58,59] |
| Migraine | Bark, leaves or root decoction taken orally | Nigeria | [49,50] |
| Muscle pain | Bark decoction rubbed on painful muscles | Cameroon | [55] |
| Numbness of feet | Bark decoction rubbed on feet | Cameroon | [55] |
| Painful joints | Bark decoction rubbed on painful joints | Kenya, South Africa | [25,60] |
| Pain killer | Roots taken orally mixed with roots of V. infausta and D. cinerea | South Africa | [54] |
| Paralysis | Bark decoction taken orally | South Africa | [25] |
| Physical weakness | Bark decoction taken orally | Cameroon | [55] |
| Pre-Hepatic jaundice | Bark decoction taken orally | Uganda | [61] |
| Purgative for poisoning | Leaf decoction taken orally | Ivory Coast | [31] |
| Rheumatism | Bark, leaf or root decoction taken orally | Cameroon, Tanzania | [29,51] |
| Sexual weakness | Bark decoction taken orally | Cameroon | [55] |
| Skin eruption | Bark or leaf decoction applied to affected body part | Kenya, Tanzania | [51,62] |
| Spleen enlargement | Bark or leaf decoction taken orally | Tanzania | [51] |
| Sexually transmitted diseases (STDs) | Bark, leaf or root decoction taken orally | Guinea-Bissau, Kenya | [47,60,63] |
| Scorpion bite | Bark decoction applied to affected body part | Ethiopia | [64] |
| Sore eyes | Bark, leaf sap or leaf decoction applied on eyes | South Africa, Tanzania | [2,23,39,45,46] |
| Stomach ache | Bark, leaf or root decoction taken orally | Guinea-Bissau, Kenya, Nigeria, South Africa, Tanzania | [38,39,40,41,47,48,51,60] |
| Syphilis | Bark decoction taken orally mixed with Mangifera indica L. (Anacardiaceae) | Sierra Leone | [65] |
| Syphilis | Bark or leaf decoction taken orally | Uganda | [61] |
| Tape worms | Bark or leaf decoction taken orally | Cameroon, Kenya, Nigeria, South Africa, Tanzania, Uganda | [2,9,15,25,32,38,41,60] |
| Toothache | Bark decoction applied to affected teeth | DRC, South Africa | [2,22,23,25] |
| Tumor | Stem bark decoction taken orally | Kenya | [26] |
| Venereal diseases | Bark or leaf decoction taken orally | Kenya, South Africa | [2,23,25,38] |
| Wounds | Bark, leaf or root decoction applied to affected body part | DRC, Sierra Leone, South Africa | [2,16,23,24,25,65] |
| Yellow fever | Root decoction taken orally | Tanzania | [20] |
| Ethnoveterinary medicine | Burkina Faso, DRC, Ethiopia, Kenya, Uganda | [14,60,66,67,68] |
| Nutritional Composition | Values | Dietary Reference Intake (DRI) (mg/day) | References | |
|---|---|---|---|---|
| Recommended Dietary Allowance (RDA) | Tolerable Upper Intake Level (UL) | |||
| Ash | 3.2 ± 0.46 g/100 g | - | - | [46] |
| Carbohydrate | 1.7 g/100 g | - | - | [46] |
| Ca | 543 µg g−1 | 1000–1300 | 2500 | [46] |
| Co | 6.8 µg g−1 | - | - | [46] |
| Cr | 3 µg g−1 | 0.024–0.035 | 1000 | [46] |
| Cu | 9 µg g−1 | 0.9 | 8.0 | [46] |
| Cyanogenic glycosides | 810 mg/100 g | - | - | [73] |
| Fe | 166 µg g−1 | 8–15 | 45.0 | [46] |
| K | 87.94 mg/100 g | 3000 | 3000 | [72] |
| Mg | 859 µg g−1 | 310–320 | 350 | [46] |
| Mn | 414 µg g−1 | 1.6–3.0 | 9.0 | [46] |
| Moisture content | 90.1 ± 0.60 g/100 g | - | - | [46] |
| Na | 254.8 mg/100 g | 2300 | 2300 | [72] |
| Ni | 3 µg g−1 | - | - | [46] |
| Oil | 0.9 ± 0.01 g/100 g | - | - | [46] |
| Oxalate | 5.84 g/100 g | - | - | [73] |
| P | 2545.4 mg/100 g | - | - | [72] |
| Pb | 1 µg g−1 | - | - | [46] |
| Phytic acid | 0.5% | - | - | [72] |
| Protein | 4.1 ± 0.13 g/100 g | - | - | [46] |
| Saponin | 10.6% | - | - | [73] |
| Tannin | 1160 mg/100 g | - | - | [73] |
| Zn | 226 µg g−1 | 8–11 | 34.0 | [46] |
| Phytochemical Compounds | Plant Parts | Method of Compound Characterization | References |
|---|---|---|---|
| Alkaloid | |||
| Stigmast-8(14)-en-3-ol | Fruits | Gas chromatography-mass spectrometry (GC-MC) | [46,77] |
| Anthocyanidin | |||
| Delphinidin | Bark | Thin-Layer chromatography (TLC) | [69] |
| Essential oil | |||
| N(β)-Benzyl-14-(carboxymethyl) | Bark | GC-MS | [78] |
| Benzene, 1.3-bis (3-phenoxyphenoxy) | Bark | GC-MS | [78] |
| 2-Phenyl-2-tipyl-acenapthenone | Bark | GC-MS | [78] |
| α-Pinene | Bark | GC-MS | [78] |
| Camphene | Bark | GC-MS | [78] |
| 1,8-Cineole | Bark | GC-MS | [78] |
| Camphor | Bark | GC-MS | [78] |
| endo-Borneol | Bark | GC-MS | [78] |
| Linalool | Bark | GC-MS | [78] |
| 1-α-Terpineol | Bark | GC-MS | [78] |
| α-Caryophyllene oxide | Bark | GC-MS | [78] |
| Nopol | Bark | GC-MS | [78] |
| 2-Pinen-4-one | Bark | GC-MS | [78] |
| (−)−Bornyl acetate | Bark | GC-MS | [78] |
| 1-Tetradecanol (fatty alcohol) | Bark | GC-MS | [78] |
| 5-Octadecene | Bark | GC-MS | [78] |
| Hexadecanoic acid methyl ester | Bark | GC-MS | [78] |
| Palmitic acid | Bark | GC-MS | [78] |
| 17-Pentatriacontene | Bark | GC-MS | [78] |
| Tritetracontane | Bark | GC-MS | [78] |
| 5β-Pregn-11-ene | Bark | GC-MS | [78] |
| 4-Imidozolidinone | Bark | GC-MS | [78] |
| Naphthalene | Bark | GC-MS | [78] |
| Quinoline | Bark | GC-MS | [78] |
| Flavonoids | |||
| Caffeic acid | Leaves | TLC | [69] |
| Quercetin | Bark, leaves | GC-MC, nuclear magnetic resonance NMR | [46,77] |
| Quercetin-3-O-glucoside | Bark, leaves | GC-MC, NMR | [46,77] |
| Phenolic | |||
| trans-Triacontyl-4-hydroxy-3-methoxycinnamate | Bark | NMR | [26] |
| Polyol | |||
| Phytic acid | Bark | [72] | |
| Sterols | |||
| Ergosterol | Fruits | GC-MC | [46,77] |
| 5β,6β-Epoxy-7-bromocholestan-3-one | Fruits | GC-MC | [46] |
| Tannins | |||
| Ellagic acid | Bark | TLC | [69] |
| Gallic acid | Bark | TLC | [69] |
| Triterpenes | |||
| Acacic acid lactone | Bark, leaves | GC-MC, NMR | [46,77] |
| Betulinic acid | Bark | NMR | [26] |
| Catechin | Bark | NMR | [26] |
| Cycloartenol | Fruits | GC-MC | [46,77] |
| Cycloartenol acetate | Fruits | GC-MC | [46,77] |
| Epifriedelinol | Bark | TLC | [69] |
| Friedeline | Bark | NMR, TLC | [26,69] |
| Oleanolic acid | Bark, leaves | GC-MC, NMR | [46,77] |
| Taraxerole | Bark | TLC | [69] |
| Taraxerone | Bark | TLC | [69] |
© 2017 by the author. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Maroyi, A. Ethnopharmacology and Therapeutic Value of Bridelia micrantha (Hochst.) Baill. in Tropical Africa: A Comprehensive Review. Molecules 2017, 22, 1493. https://doi.org/10.3390/molecules22091493
Maroyi A. Ethnopharmacology and Therapeutic Value of Bridelia micrantha (Hochst.) Baill. in Tropical Africa: A Comprehensive Review. Molecules. 2017; 22(9):1493. https://doi.org/10.3390/molecules22091493
Chicago/Turabian StyleMaroyi, Alfred. 2017. "Ethnopharmacology and Therapeutic Value of Bridelia micrantha (Hochst.) Baill. in Tropical Africa: A Comprehensive Review" Molecules 22, no. 9: 1493. https://doi.org/10.3390/molecules22091493





