Environmental Factors Influencing Adoption of Canadian Guidelines on Smoking Cessation in Dental Healthcare Settings in Quebec: A Qualitative Study of Dentists’ Perspectives
Abstract
:1. Introduction
2. Materials and Methods
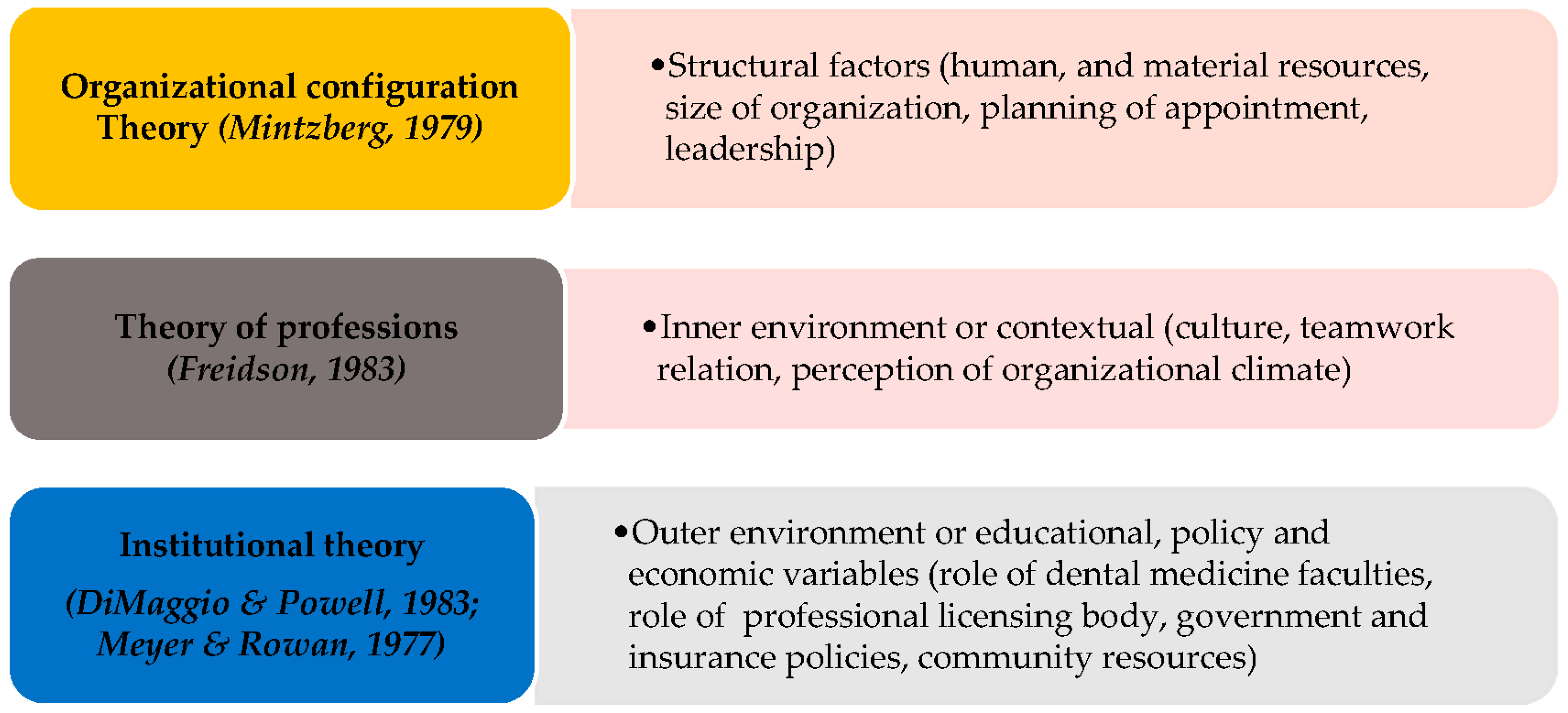
2.1. Conceptual Framework
2.2. Methods
2.2.1. Ethical Considerations
2.2.2. Study Design
2.2.3. Selection of Participants
2.2.4. Process of Data Collection
2.2.5. Data Analysis
3. Results
3.1. Participants and Dental Clinics Characteristics
3.2. Results from the Inductive Analysis Approach
3.2.1. Patient
“If the initiative comes from the patient who has seen a poster or a TV spot in the waiting room, this action can stimulate the practitioner to help smoker for quitting.”
“There are places where tobacco use is a generational issue and disadvantaged settings where smoking is the pleasure of life. Thus, the dentist must consider these aspects when he wants to support a smoker who wants to quit smoking.”
3.2.2. Characteristics of Canadian Smoking Cessation Guideline
“The existence of a specific, clear and concise protocol is a prerequisite for my involvement, as well as reimbursement and the possibility of writing a prescription. If I have to be reimbursed for smoking cessation services and I do not have direct directions to follow, this would take me too long and I do not want to spend extra time on this service, we need a protocol.”
3.2.3. Perception of the Statements of Canadian Smoking Cessation Guidelines
“The dentist does not have the role to monitor the patient during the smoking cessation process, just to raise awareness about the consequences of smoking.”
3.2.4. Structural Factors that Influencing the Implementation of CSCCG in Private Dental Clinics in Connection with Mintzberg’s Organizational Configuration Theory
Receptive Working Environment
“Practice groups with support staff have the opportunity to offer smoking cessation services. If individuals are mandated to do certain tasks, it provides the time to the help the patient and the opportunity for dentists to take more time with the patient.”
“The pamphlet is the most used as a promotional tool, as it helps to start the conversation and the patient can view it in the waiting room in the dental clinic.”
Leadership in Clinical and Administrative Decisions
“Every dentist is responsible for his treatment plan. He is responsible for his patients. We can work with a colleague for some treatment plans, depending on the case, working either in collaboration or consultation.”“Young graduates will move towards a group practice, working as associate dentists. In this case, they are more likely to adhere to the philosophy of the owner of the dental clinic and to follow their guidelines.”
“If a clinic is too loaded with appointments between patients every 30 min, it is certain that the workload will negatively influence the support provided to smokers.”
3.2.5. Factors Related to the Internal Environment Influencing the Implementation of CSCCG in Private Dental Clinics in Connection with Friedson’s Theory of Professions
Professional Duty in the Healthcare Context
“It is difficult for us to survive as a liberal profession in a public context, to find a balance between a profitable practice and the patient’s needs; we are facing a problem of time and efficiency. Thus, the financial issue over the patient’s health is an important issue.”
Culture
“Given this consistency in the messages internally, the patient may be aware of the seriousness of the problem and be reassured of the support if he wants to quit.”
“The dental hygienist is the first person to see the smokers, they are the first contact. However, I see no harm in the dentist adding support to the dental hygienist.”
3.3.6. Factors Related to the Outer Environment in the Implementation of CSCCG in Private Dental Clinics in Connection with Institutional Theory
Complementary Training Organisations: Dental Faculties and the Professional Licensing Body of Dentists in Quebec
“A participant mentioned the relevance for dental faculties to bring the community health course earlier to the undergraduate, to familiarize future dentists with an overall health approach, to give them time to internalize it, and develop the skills and abilities to effectively intervene with smokers.”
Government Policies
“Dentists need to strengthen actions that have been undertaken by the government, the information needs to be conveyed that is out there. Government activities are incentives for practitioners. It is a way to make them understand that the ball is thrown, the train is leaving the station and that everyone should hop on.”
Economic Issues
“You cannot ask for money for all the information and advice given to patients. It’s like checking tissue during an examination for oral cancer, as well as talking about alcohol with patients.”“Yes, it might be recognition of their time that could encourage dentists to become more involved and that their time is not volunteered, this can make a difference if there is a reasonable fee.”
4. Discussion
4.1. Strengths and Limitations
5. Conclusions
Supplementary Materials
Acknowledgments
Author Contributions
Conflicts of Interest
References
- Marteau, T.M.; Johnston, M. Health professionals: A source of variance in health outcomes. Psychol. Health 1991, 5, 47–58. [Google Scholar] [CrossRef]
- Harrison, M.B.; Graham, I.D.; Fervers, B. Adapting knowledge to a local context. In Knowledge Translation in Health Care: Moving from Evidence to Practice; Straus, S., Tetroe, J., Graham, I., Eds.; Blackwell Publishing: Toronto, ON, Canada, 2009; pp. 77–93. [Google Scholar]
- Spallek, H.; Song, M.; Polk, D.E.; Bekhuis, T.; Frantsve-Hawley, J.; Aravamudhan, K. Barriers to Implementing Evidence-Based Clinical Guidelines: A Survey of Early Adopters. J. Évid. Based Dent. Pract. 2010, 10, 195–206. [Google Scholar] [CrossRef] [PubMed]
- CAN-ADAPTT. Lignes Directrices Canadiennes de Pratique Clinique sur le Renoncement au Tabagisme: Énoncés Sommaires. Toronto, Canada: Réseau D’action Canadien Pour L’avancement, la Dissémination et L’adoption de Pratiques en Matière de Traitement du Tabagisme Fondées sur L’expérience Clinique; Centre de Toxicomanie et de Santé Mentale: Toronto, ON, Canada, 2011. [Google Scholar]
- Bergström, J.; Eliasson, S.; Dock, J. Exposure to tobacco smoking and periodontal health. J. Clin. Periodontol. 2000, 27, 61–68. [Google Scholar] [CrossRef] [PubMed]
- Rad, M.; Kakoie, S.; Brojeni, F.; Pourdamghan, N.E. Effect of long-term smoking on whole-mouth salivary flow rate and oral health. J. Dent. Res. Dent. Clin. Dent. Prospect. 2011, 4, 110–114. [Google Scholar]
- McBride, C.M.; Emmons, K.M.; Lipkus, I.M. Understanding the potential of teachable moments: The case of smoking cessation. Health Educ. Res. 2003, 18, 156–170. [Google Scholar] [CrossRef] [PubMed]
- Jannat-Khah, D.P.; McNeely, J.; Pereyra, M.R.; Parish, C.; Pollack, H.A.; Ostroff, J. Dentists’ Self-Perceived Role in Offering Tobacco Cessation Services: Results From a Nationally Representative Survey, United States, 2010–2011. Prev. Chronic Dis. 2014, 11, E196. [Google Scholar] [CrossRef] [PubMed]
- Fiore, M.C.; Jaen, C.R.; Baker, T.B.; Bailey, W.C.; Benowitz, N.L.; Curry, S.J.; Dorfman, S.F.; Froelicher, E.S.; Goldstein, M.G.; Healton, C.G.; et al. Treating Tobacco Use and Dependence: 2008 Update; United States Department of Health and Human Services, Public Health Services: Rockville, MD, USA, 2008.
- Gordon, J.S.; Andrews, J.A.; Lichtenstein, E.; Severson, H.H.; Akers, L. Disseminating a smokeless tobacco cessation intervention model to dental hygienists: A randomized comparison of personalized instruction and self-study methods. Health Psychol. 2005, 24, 447–455. [Google Scholar] [CrossRef] [PubMed]
- Little, S.J.; Hollis, J.F.; Fellows, J.L.; Snyder, J.J.; Dickerson, J.F. Implementing a tobacco assisted referral program in dental practices. J. Public Health Dent. 2009, 69, 149–155. [Google Scholar] [CrossRef] [PubMed]
- Applegate, B.W.; Sheffer, C.E.; Crews, K.M.; Payne, T.J.; Smith, P.O. A survey of tobacco-related knowledge, attitudes and behaviours of primary care providers in Mississippi. J. Eval. Clin. Pract. 2008, 14, 537–544. [Google Scholar] [CrossRef] [PubMed]
- Patel, A.M.; Blanchard, S.B.; Christen, A.G.; Bandy, R.W.; Romito, L.M. A survey of united states periodontists’ knowledge, attitudes, and behaviors related to tobacco-cessation interventions. J. Periodontol. 2011, 82, 367–376. [Google Scholar] [CrossRef] [PubMed]
- Watt, R.; McGlone, P.; Dykes, J.; Smith, M. Barriers limiting dentists’ active involvement in smoking cessation. Oral Health Prev. Dent. 2004, 2, 95–102. [Google Scholar] [PubMed]
- McGlone, P.; Watt, R.; Sheiham, A. Evidence-based dentistry: An overview of the challenges in changing professional practice. Br. Dent. J. 2001, 190, 636–639. [Google Scholar] [CrossRef] [PubMed]
- Estabrooks, C.; Scott, S.; Squires, J.; Stevens, B.; O’Brien-Pallas, L.; Watt-Watson, J.; Profetto-McGrath, J.; McGilton, K.; Golden-Biddle, K.; Lander, J.; et al. Patterns of research utilization on patient care units. Implement. Sci. 2008, 3, 31. [Google Scholar] [CrossRef] [PubMed]
- Amemori, M. Developing Assessment and Promotion of Tobacco Counsellin: A Cluster-Randomised Community Trial among Oral Health Professionals; University of Helsinki: Helsinki, Finland, 2012; p. 32. [Google Scholar]
- Rosseel, J.P.; Jacobs, J.E.; Hilberink, S.R.; Maassen, I.M.; Segaar, D.; Plasschaert, A.J.; Grol, R.P. Experienced barriers and facilitators for integrating smoking cessation advice and support into daily dental practice. A short report. Br. Dent. J. 2011, 210, E10. [Google Scholar] [CrossRef] [PubMed]
- Rosseel, J.P.; Jacobs, J.E.; Hilberink, S.R.; Maassen, I.M.; Allard, R.H.B.; Plasschaert, A.J.; Grol, R.P. What determines the provision of smoking cessation advice and counselling by dental care teams? Br. Dent. J. 2009, 206, E13. [Google Scholar] [CrossRef] [PubMed]
- Warnakulasuriya, S.; Dietrich, T.; Bornstein, M.M.; Casals Peidró, E.; Preshaw, P.M.; Walter, C.; Wennström, J.L.; Bergström, J. Oral health risks of tobacco use and effects of cessation. Int. Dent. J. 2010, 60, 7–30. [Google Scholar] [PubMed]
- Godin, G.; Belanger-Gravel, A.; Eccles, M.; Grimshaw, J. Healthcare professionals’ intentions and behaviours: A systematic review of studies based on social cognitive theories. Implement. Sci. 2008, 3, 36. [Google Scholar] [CrossRef] [PubMed]
- Carr, A.B.; Ebbert, J. Interventions for tobacco cessation in the dental setting. Cochrane Database Syst. Rev. 2012. [Google Scholar] [CrossRef]
- Shelley, D.; Wright, S.; McNeely, J.; Rotrosen, J.; Winitzer, R.F.; Pollack, H.; Abel, S.; Metsch, L. Reimbursing Dentists for Smoking Cessation Treatment: Views From Dental Insurers. Nicotine Tob. Res. 2012, 14, 1180–1186. [Google Scholar] [CrossRef] [PubMed]
- Ebn Ahmady, A.; Khoshnevisan, M.H.; Heidari, N.; Lando, H.A. Dentists’ familiarity with tobacco cessation programs in dental settings in Iran. J. Public Health Dent. 2011, 71, 271–277. [Google Scholar] [CrossRef] [PubMed]
- Prakash, P.; Belek, M.G.; Grimes, B.; Silverstein, S.; Meckstroth, R.; Heckman, B.; Weintraub, J.A.; Gansky, S.A.; Walsh, M.M. Dentists’ attitudes, behaviors, and barriers related to tobacco-use cessation in the dental setting. J. Public Health Dent. 2013, 73, 94–102. [Google Scholar] [CrossRef] [PubMed]
- Tremblay, M.; Cournoyer, D.; O’Loughlin, J. Do the correlates of smoking cessation counseling differ across health professional groups? Nicotine Tob. Res. 2009, 11, 1330–1338. [Google Scholar] [CrossRef] [PubMed]
- Gagnon, M.P. Déterminants Psychosociaux et Organisationnels de L’adoption des Technologies de Télémédecine Dans le RÉSEAU Québécois de Télésanté Élargi (RQTE); Université Laval: Québec, QC, Canada, 2003. [Google Scholar]
- Hannes, K.; Norré, D.; Goedhuys, J.; Naert, I.; Aertgeerts, B. Obstacles to Implementing Evidence-Based Dentistry: A Focus Group-Based Study. J. Dent. Educ. 2008, 72, 736–744. [Google Scholar] [PubMed]
- DiMaggio, P.J.; Powell, W.W. The Iron Cage Revisited: Institutional Isomorphism and Collective Rationality in Organizational Fields. Am. Sociol. Rev. 1983, 48, 147–160. [Google Scholar] [CrossRef]
- Meyer, J.W.; Rowan, B. Institutionalized organizations: Formal structures as myth and ceremony. Am. J. Sociol. 1977, 83, 340–363. [Google Scholar] [CrossRef]
- Mintzberg, H. The Structuring of Organizations: A Synthesis of the Research; Prentice Hall: Englewood Cliffs, NJ, USA, 1979. [Google Scholar]
- Freidson, E. The Theory of Professions: State of the Art. In The Sociology of the Professions; Lewis, R.D.A.P., Ed.; Macmillan: London, UK, 1983. [Google Scholar]
- Stokes, E.; Pine, C.; Harris, R. The promotion of oral health within the Healthy School context in England: A qualitative research study. BMC Oral Health 2009, 9, 3. [Google Scholar] [CrossRef] [PubMed]
- Creswell, J.W. Qualitative procedures. In Research Design: Qualitative, Quantitative, and Mixed Methods Approachs, 3rd ed.; Creswell, J.W., Ed.; Sage Publications: Los Angeles, CA, USA, 2009; pp. 173–202. [Google Scholar]
- Hsieh, H.F.; Shannon, S.E. Three approaches to qualitative content analysis. Qual. Health Res. 2005, 15, 1277–1288. [Google Scholar] [CrossRef] [PubMed]
- Graneheim, U.H.; Lundmanm, B. Qualitative content analysis in nursing research: Concepts, procedures and measures to achieve trustworthiness. Nurse Educ. Today 2004, 24, 105–112. [Google Scholar] [CrossRef] [PubMed]
- ATLAS.ti; The Next Generation of QDA Software; ATLAS.ti Scientific Software Development GmbH: Berlin, Germany, 2015.
- Ministère de l’économie dliede. Portrait Économique des Régions du Québec Édition. Available online: https://www.economie.gouv.qc.ca/fileadmin/contenu/documents_soutien/regions/portraits_regionaux/portrait_socio_econo.pdf (accessed on 5 November 2015).
- Chambers, D.W. The Role of Dentists in Dentistry. J. Dent. Educ. 2001, 65, 1430–1440. [Google Scholar] [PubMed]
- Labelle, H.R. Le professionalisme. J. L’ordre Dent. Québec 2010, 47, 1–10. [Google Scholar]
- Zijlstra-Shaw, S.; Roberts, T.E.; Robinson, P.G. Perceptions of professionalism in dentistry—A qualitative study. Br. Dent. J. 2013, 215, E18. [Google Scholar] [CrossRef] [PubMed]
- Dussault, G. Dental services in Quebec: Issues and changes. Soc. Sci. Méd. 1984, 18, 251–255. [Google Scholar] [CrossRef]
- Morison, S.; McMullan, C. Preparing for the future: Challenges and opportunities for management and leadership skills. Br. Dent. J. 2013, 214, E2–E7. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Greer, S. Medical autonomy: Peeling the onion. J. Health Serv. Res. Policy 2008, 13, 1–2. [Google Scholar] [CrossRef] [PubMed]
- Gordon, J.S.; Severson, H.H. Tobacco cessation through dental office settings. J. Dent. Educ. 2001, 65, 354–363. [Google Scholar] [PubMed]
- Damanpour, F. Organizational Innovation—A Metaanalysis of Effects of Determinants and Moderators. Acad. Manag. J. 1991, 34, 555–590. [Google Scholar] [CrossRef]
- Cohen, S.J.; Stookey, G.K.; Katz, B.P.; Drook, C.A.; Christen, A.G. Helping smokers quit: A randomized controlled trial with private practice dentists. J. Am. Dent. Assoc. 1989, 118, 41–45. [Google Scholar] [CrossRef] [PubMed]
- Estabrooks, C.A.; Squires, J.E.; Hutchinson, A.M.; Scott, S.; Cummings, G.G.; Kang, S.H.; Midodzi, W.K.; Stevens, B. Assessment of variation in the Alberta context tool: The contribution of unit level contextual factors and specialty in Canadian paediatric acute care settings. BMC Health Serv. Res. 2011, 11, 251. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Bergström, A.; Peterson, S.; Namusoko, S.; Waiswa, P.; Wallin, L. Knowledge translation in Uganda: A qualitative study of Ugandan midwives’ and managers’ perceived relevance of the sub-elements of the context cornerstone in the PARIHS framework. Implement. Sci. 2012, 7, 1–13. [Google Scholar] [CrossRef] [PubMed]
- Healthy People 2020. Tobacco Use Objectives Centers for Disease Control and Prevention. 2013 Updated June 2016. Available online: https://www.healthypeople.gov/2020/topics-objectives/topic/tobacco-use (accessed on 20 May 2016).
- Watt, R.G.; Benzian, H.; Binnie, V.; Gafner, C.; Hovius, M.; Newton, T.J.; Mecklenburg, R.E. Public health aspects of tobacco control: Settings the agenda for action by oral health professions across Europe. Oral Health Prev. Dent. 2006, 4, 19–26. [Google Scholar] [PubMed]
- Ibrahim, H.; Norkhafizah, S. Attitudes and practices in smoking cessation counselling among dentists in Kelantan. Arch. Orofac. Sci. 2008, 3, 11–16. [Google Scholar]
- Crews, K.M.; Sheffer, C.E.; Payne, T.J.; Applegate, B.W.; Martin, A.; Sutton, T. A survey of oral and maxillofacial surgeons’ tobacco-use-related knowledge, attitudes and intervention behaviors. J. Am. Dent. Assoc. 2008, 139, 1643–1651. [Google Scholar] [CrossRef] [PubMed]
- O’Shea, R.M. Dentistry as an Organization and Institution. Milbank Meml. Fund Q. 1971, 49, 13–38. [Google Scholar] [CrossRef]
- Aarons, G.A. Measuring Provider Attitudes Toward Evidence-Based Practice: Consideration of Organizational Context and Individual Differences. Child Adolesc. Psychiatr. Clin. N. Am. 2005, 14, 255–271. [Google Scholar] [CrossRef] [PubMed]
- Prasad, A.; Prasad, P. The Coming of Age of Interpretive Organizational Research. Organ. Res. Methods 2002, 5, 4–11. [Google Scholar] [CrossRef]
- Albert, D.A.; Ward, A.; Ahluwalia, K.; Sadowsky, D. Addressing tobacco in managed care: A survey of dentists’ knowledge, attitudes, and behaviors. Am. J. Public Health 2002, 92, 997–1001. [Google Scholar] [CrossRef] [PubMed]
- Rogers, E.M. Diffusion of Innovations, 4th ed.; Free Press: New York, NY, USA, 1995. [Google Scholar]
- Albert, D.A.; Ahluwalia, K.P.; Ward, A.; Sadowsky, D. The use of ‘academic detailing’ to promote tobacco-use cessation counseling in dental offices. J. Am. Dent. Assoc. 2004, 135, 1700–1706. [Google Scholar] [CrossRef] [PubMed]
- Anderson, C.A. Leaders and leadership: Who are they and what is it? Nurs. Outlook 1996, 44, 163. [Google Scholar] [PubMed]
- Hebbal, M.; Ankola, N.; Murugaboopathy, V.; Patel, S.; Patel, N.; Parka, N. Do Dentists Require Leadership Qualities? Can. Méd. Educ. J. 2012, 3, 1–2. [Google Scholar]
- Christen, A.G. Survey of smoking behavior and attitudes of 630 American dentists: Current trends. J. Am. Dent. Assoc. 1984, 109, 271–272. [Google Scholar] [CrossRef] [PubMed]
- Tremblay, M. Le Counseling en Abandon du Tabac: Besoins des Professionnels de la Santé en 2010; Institut national de santé publique du Québec: Quebec, QC, Canada, 2010. [Google Scholar]
- Silverman, S.; Kerr, A.R.; Epstein, J.B. Oral and Pharyngeal Cancer Control and Early Detection. J. Cancer Educ. 2010, 25, 279–281. [Google Scholar] [CrossRef] [PubMed]
- Denzin, N.; Lincoln, Y. Handbook of Qualitative Research; Sage publications: London, UK, 2005. [Google Scholar]
- Pope, C.; Ziebland, S.; Mays, N. Analysing qualitative data. BMJ: Br. Méd. J. 2000, 320, 114–116. [Google Scholar] [CrossRef]
- Burnard, P.; Gill, P.; Stewart, K.; Treasure, E.; Chadwick, B. Analysing and presenting qualitative data. Br. Dent. J. 2008, 204, 429–432. [Google Scholar] [CrossRef] [PubMed]
- Eaton, K.A.; Patel, R.; Garcia, A.; Rincon, V.; Adams, L.; Brooks, J. Factors Influencing Dental Practionner Performance: A Literature Review; National Clinical Assessment Service (NCAS): London, UK, 2011; pp. 1–121. [Google Scholar]
| Variables (n = 20) | Frequency (n) | Range or Percentage (%) | Mean (SD) |
|---|---|---|---|
| Gender | |||
| Female | 9 | 45 | |
| Male | 11 | 55 | |
| Years of experience in the current dental clinic | 10 to 40 years | 11.7 (11.2) | |
| Years of experience in dentistry | 1.5–47 years | 18.7 (14.2) | |
| Previous knowledge of Canadian smoking cessation guidelines before this study | |||
| Yes | 13 | 65 | |
| No | 7 | 35 | |
| Owner of dental clinic | |||
| Yes | 7 | 35 | |
| No | 13 | 65 | |
| Number of dentists in participants’ dental clinics | 1–6 | 3.1 (1.6) | |
| Number of dental hygienists in participants’ dental clinics | 0–18 | 4.7 (3.8) | |
| Type of practice | |||
| Solo | 3 | 15 | |
| Group practice | 17 | 85 | |
| Number of patients seen by week | |||
| 16–29 | 6 | 30 | |
| 30–44 | 4 | 20 | |
| 45 and more | 10 | 50 | |
| Perception of workload | |||
| Heavy | 8 | 40 | |
| Average | 12 | 60 | |
| Having a dental manager or dental coordinator | |||
| Yes No | 13 7 | 65 35 |
© 2016 by the authors; licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC-BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Kengne Talla, P.; Gagnon, M.-P.; Dawson, A. Environmental Factors Influencing Adoption of Canadian Guidelines on Smoking Cessation in Dental Healthcare Settings in Quebec: A Qualitative Study of Dentists’ Perspectives. Dent. J. 2016, 4, 40. https://doi.org/10.3390/dj4040040
Kengne Talla P, Gagnon M-P, Dawson A. Environmental Factors Influencing Adoption of Canadian Guidelines on Smoking Cessation in Dental Healthcare Settings in Quebec: A Qualitative Study of Dentists’ Perspectives. Dentistry Journal. 2016; 4(4):40. https://doi.org/10.3390/dj4040040
Chicago/Turabian StyleKengne Talla, Pascaline, Marie-Pierre Gagnon, and Aimée Dawson. 2016. "Environmental Factors Influencing Adoption of Canadian Guidelines on Smoking Cessation in Dental Healthcare Settings in Quebec: A Qualitative Study of Dentists’ Perspectives" Dentistry Journal 4, no. 4: 40. https://doi.org/10.3390/dj4040040






