Current Challenges in Home Nutrition Services for Frail Older Adults in Japan—A Qualitative Research Study from the Point of View of Care Managers
Abstract
:1. Introduction
2. Method
2.1. Study Participants
| Participant | Age (year) | Sex (F/M) | Career (year) |
|---|---|---|---|
| 1 | 54 | F | 4 |
| 2 | 50 | F | 7 |
| 3 | 48 | F | 2 |
| 4 | 45 | F | 7 |
| 5 | 44 | F | 4 |
| 6 | 43 | M | 3 |
| 7 | 36 | M | 5 |
| 8 | 34 | F | 2 |
| 9 | 32 | M | 6 |
| 10 | 29 | F | 0.4 |
2.2. Data Collection
2.3. Analysis Using the KJ Method
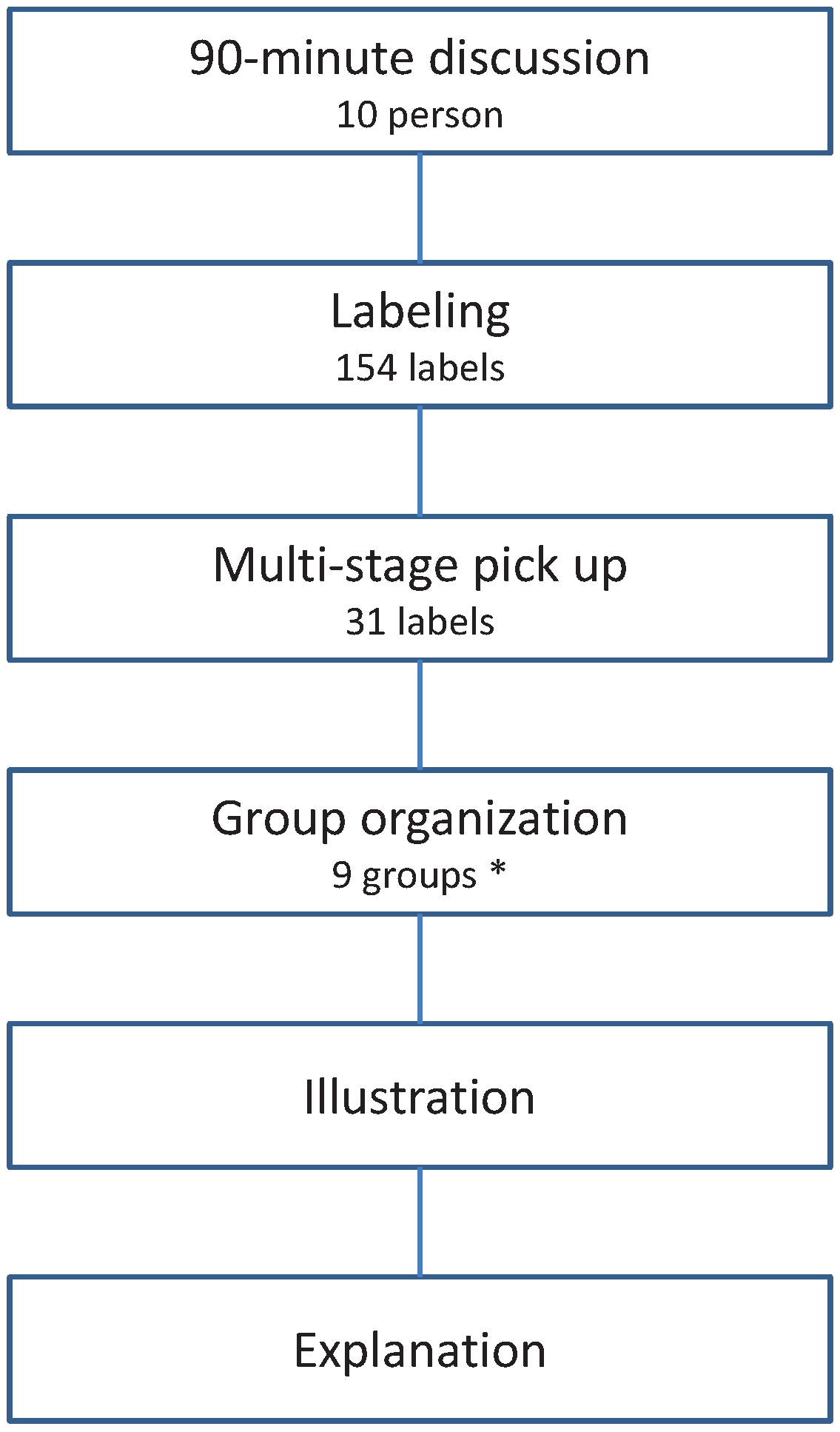
3. Results

3.1. Group Organization
3.2. Illustrated Figure
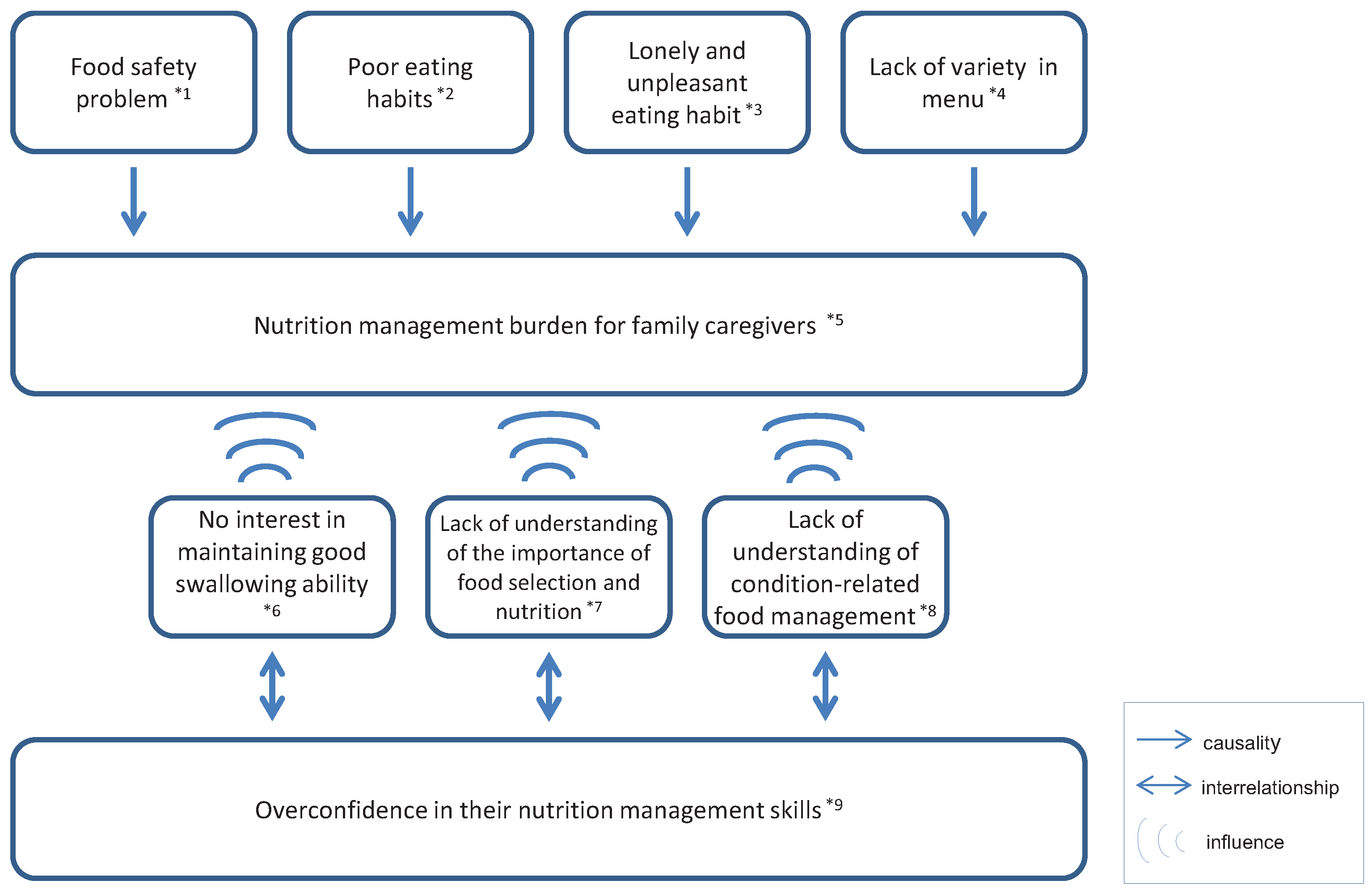
4. Discussion
5. Conclusions
Acknowledgments
Conflicts of Interest
References
- Hirakawa, Y. Palliative care for the elderly: A Japanese perspective. In Contemporary and Innovative Practice in Palliative Care; Esther, C., Amanda, J., Eds.; InTech: Rijeka, Croatia, 2012; pp. 271–290. [Google Scholar]
- Kimura, Y.; Wada, T.; Okumiya, K.; Ishimoto, Y.; Fukutomi, E.; Kasahara, Y.; Chen, W.; Sakamoto, R.; Fujisawa, M.; Otsuka, K.; et al. Eating alone among community-dwelling Japanese elderly: Association with depression and food diversity. J. Nutr. Health Aging 2012, 16, 728–731. [Google Scholar] [CrossRef]
- Endevelt, R.; Werner, P.; Stone, O. Dietitians’ attitudes regarding elderly nutritional factors. J. Nutr. Elder. 2006, 26, 45–58. [Google Scholar] [CrossRef]
- Soini, H.; Routasalo, P.; Lagström, H. Characteristics of the Mini-Nutritional Assessment in elderly home-care patients. Eur. J. Clin. Nutr. 2004, 58, 64–70. [Google Scholar] [CrossRef]
- Sharkey, J.R. The interrelationship of nutritional risk factors, indicators of nutritional risk, and severity of disability among home-delivered meal participants. Gerontologist 2002, 42, 373–380. [Google Scholar] [CrossRef]
- Shatenstein, B.; Kergoat, M.J.; Reid, I.; Chicoine, M.E. Dietary intervention in older adults with early-stage Alzheimer dementia: Early lessons learned. J. Nutr. Health Aging 2013, 17, 142–147. [Google Scholar] [CrossRef]
- Matsuda, S.; Yamamoto, M. Long-term care insurance and integrated care for the aged in Japan. Int. J. Integr. Care 2001, 1, e28. [Google Scholar]
- Hirakawa, Y.; Kuzuya, M.; Enoki, H.; Uemura, K. Information needs and sources of family caregivers of home elderly patients. Arch. Gerontol. Geriat. 2011, 52, 202–205. [Google Scholar] [CrossRef]
- Hirakawa, Y.; Masuda, Y.; Uemura, K.; Naito, M.; Kuzuya, M.; Iguchi, A. Dietitians’ understanding of personalized nutritional guidance—Proposals to increase home visits by dietitians. (in Japanese). Nippon Ronen Igakkai Zasshi 2003, 40, 509–514. [Google Scholar] [CrossRef]
- Mushinkan. Available online: http://mushin-kan.jp/ (accessed on 10 May 2013).
- Raymond, S. The KJ method: A technique for analyzing data derived from Japanese ethnology. Hum. Organ. 1997, 56, 233–237. [Google Scholar]
- Kawakita, J. Abduction(Hassoho); (in Japanese). Chukoshinsho: Tokyo, Japan, 1967. [Google Scholar]
- Silva, P.; Kergoat, M.J.; Shatenstein, B. Challenges in managing the diet of older adults with early-stage Alzheimer dementia: A caregiver perspective. J. Nutr. Health Aging 2008, 12, 461–469. [Google Scholar] [CrossRef]
- Sugiura, K.; Ito, M.; Mikami, H. Family caregiver burden caused by behavioral and psychological symptoms of dementia: Measurement with a new original scale. Nippon Ronen Igakkai Zasshi 2007, 44, 717–725. [Google Scholar] [CrossRef]
- Hafsteinsdóttir, T.B.; Vergunst, M.; Lindeman, E.; Schuurmans, M. Educational needs of patients with a stroke and their caregivers: A systematic review of the literature. Patient Educ. Couns. 2011, 85, 14–25. [Google Scholar] [CrossRef]
- Fairburn, C.G.; Hope, R.A. Changes in eating in dementia. Neurobiol. Aging 1988, 9, 28–29. [Google Scholar] [CrossRef]
- Silver, H.J.; Wellman, N.S. Nutrition education may reduce burden in family caregivers of older adults. J. Nutr. Educ. Behav. 2002, 34, S53–S58. [Google Scholar] [CrossRef]
- Hirakawa, Y.; Enoki, H.; Uemura, K. Proposal concerning personalized nutritional guidance. Nippon Ronen Igakkai Zasshi 2010, 47, 334. [Google Scholar] [CrossRef]
- Krassie, J.; Smart, C.; Roberts, D.C. A review of the nutritional needs of Meals on Wheels consumers and factors associated with the provision of an effective meals on wheels service-an Australian perspective. Eur. J. Clin. Nutr. 2000, 54, 275–280. [Google Scholar] [CrossRef]
- Joung, H.W.; Kim, H.S.; Yuan, J.J.; Huffman, L. Service quality, satisfaction, and behavioral intention in home delivered meals program. Nutr. Res. Pract. 2011, 5, 163–168. [Google Scholar] [CrossRef]
- Nam, S.; Chesla, C.; Stotts, N.A.; Kroon, L.; Janson, S.L. Barriers to diabetes management: Patient and provider factors. Diabetes Res. Clin. Pract. 2011, 93, 1–9. [Google Scholar] [CrossRef]
- Wellman, N.S.; Rosenzweig, L.Y.; Lloyd, J.L. Thirty years of the older Americans Nutrition Program. J. Am. Diet. Assoc. 2002, 102, 348–350. [Google Scholar] [CrossRef]
© 2013 by the authors; licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution license (http://creativecommons.org/licenses/by/3.0/).
Share and Cite
Hirakawa, Y.; Kimata, T.; Uemura, K. Current Challenges in Home Nutrition Services for Frail Older Adults in Japan—A Qualitative Research Study from the Point of View of Care Managers. Healthcare 2013, 1, 53-63. https://doi.org/10.3390/healthcare1010053
Hirakawa Y, Kimata T, Uemura K. Current Challenges in Home Nutrition Services for Frail Older Adults in Japan—A Qualitative Research Study from the Point of View of Care Managers. Healthcare. 2013; 1(1):53-63. https://doi.org/10.3390/healthcare1010053
Chicago/Turabian StyleHirakawa, Yoshihisa, Takaya Kimata, and Kazumasa Uemura. 2013. "Current Challenges in Home Nutrition Services for Frail Older Adults in Japan—A Qualitative Research Study from the Point of View of Care Managers" Healthcare 1, no. 1: 53-63. https://doi.org/10.3390/healthcare1010053




